The Fall 2019 ASCP Psychopharmacology Update in New York included a debate by the authors on the controversial topic of whether, and when, antidepressants are appropriate in bipolar disorder. Our mutual goal was to suggest that the current state of knowledge precludes absolute recommendations for or against the use of traditional monoaminergic antidepressants. Rather, clinicians should have a clear rationale in mind when deciding whether to use or avoid antidepressants in any given patient with bipolar disorder. Herein we recap the concepts we consider of greatest relevance for decision-making on this relentlessly contentious topic, focusing on which patients may fare better or worse with antidepressants.
The controversy surrounding antidepressant use in bipolar disorder arose from initial observations in the 1970s and 1980s, mainly with tricyclic antidepressants, that some depressed bipolar patients may develop a next manic episode sooner than expected following antidepressant exposure and/or incur more frequent subsequent episodes as an iatrogenic phenomenon. Some clinicians refer to adverse outcomes as antidepressant “misadventures”; however, we discourage use of this term because it fosters automatic assumptions that antidepressants expectably cause poor outcomes. Problematic is how to differentiate polarity switches or cycle accelerations that “clearly” result from antidepressant exposure versus mood episodes that simply reflect the natural course of illness. The seminal NIMH Systematic Treatment Enhancement Program for Bipolar Disorder (STEP-BD) failed to identify either an acute benefit or mood destabilization in a large group of depressed bipolar patients taking a mood stabilizer with versus without an antidepressant1—failing to discriminate switches due to antidepressants versus natural illness course. Longer-term data on the purported hazard for antidepressants to hasten mania relapse long-term come mainly from older data comparing lithium or imipramine,2 with almost no studies exploring longitudinal course with versus without modern antidepressants.
The largest meta-analysis to date examining acute risk of polarity switch in acute bipolar depression (encompassing over 10,000 subjects from 51 trials) reveals a risk ratio of about 12% when considering only randomized data (about 14% with all prospective studies, and as high as 31% with only retrospective trials).3 The 12% switch rate from prospective studies is not much different from the STEP-BD-observed 10.7% risk of switch from depression to mania/hypomania using only a mood stabilizer.3 Sidor and MacQueen4 identify a very high number needed to harm (NNH) of 200 with respect to antidepressant-associated polarity switch. Their meta-analysis also showed underwhelming antidepressant efficacy in bipolar depression, with a rather high number needed to treat of 29.4 From one perspective, the collective database argues that antidepressants are, on average, neither helpful nor harmful—that is, they are most likely a waste of time for the majority of depressed bipolar patients. The fact that clinicians nevertheless tend to favor their use (both short- and long-term) over FDA-approved treatment options (ie, olanzapine-fluoxetine combination, quetiapine, lurasidone, or cariprazine) defies evidence-based medicine.
On a deeper level, though, the sheer presence of a bipolar diagnosis alone may not convey sufficient information for deciding whether to use an antidepressant. Simply “having a bipolar diagnosis” may be tantamount to having a diagnosis of cancer (how is an appropriate antineoplastic drug then chosen?), an upper respiratory infection (is an antibiotic appropriate? Which one? Or an antifungal drug? Or tincture of time?), or a headache (when and how do we decide the appropriateness of nonsteroidal antiinflammatories, steroids, opiates, antimigraine drugs, or a therapeutic lumbar puncture?). Identifiable bipolar subgroups have empirically been shown to fare better with antidepressants, including those with bipolar II (rather than bipolar I) depression, non-rapid cyclers, patients with pure (non-mixed) depressed phase episodes, and those lacking a history of alcohol or substance use disorders, among other characteristics.5 Long-term antidepressant use appears to be a wiser proposition mainly (if not only) when it initially produces a marked acute response (rather than an incomplete or nonresponse).6
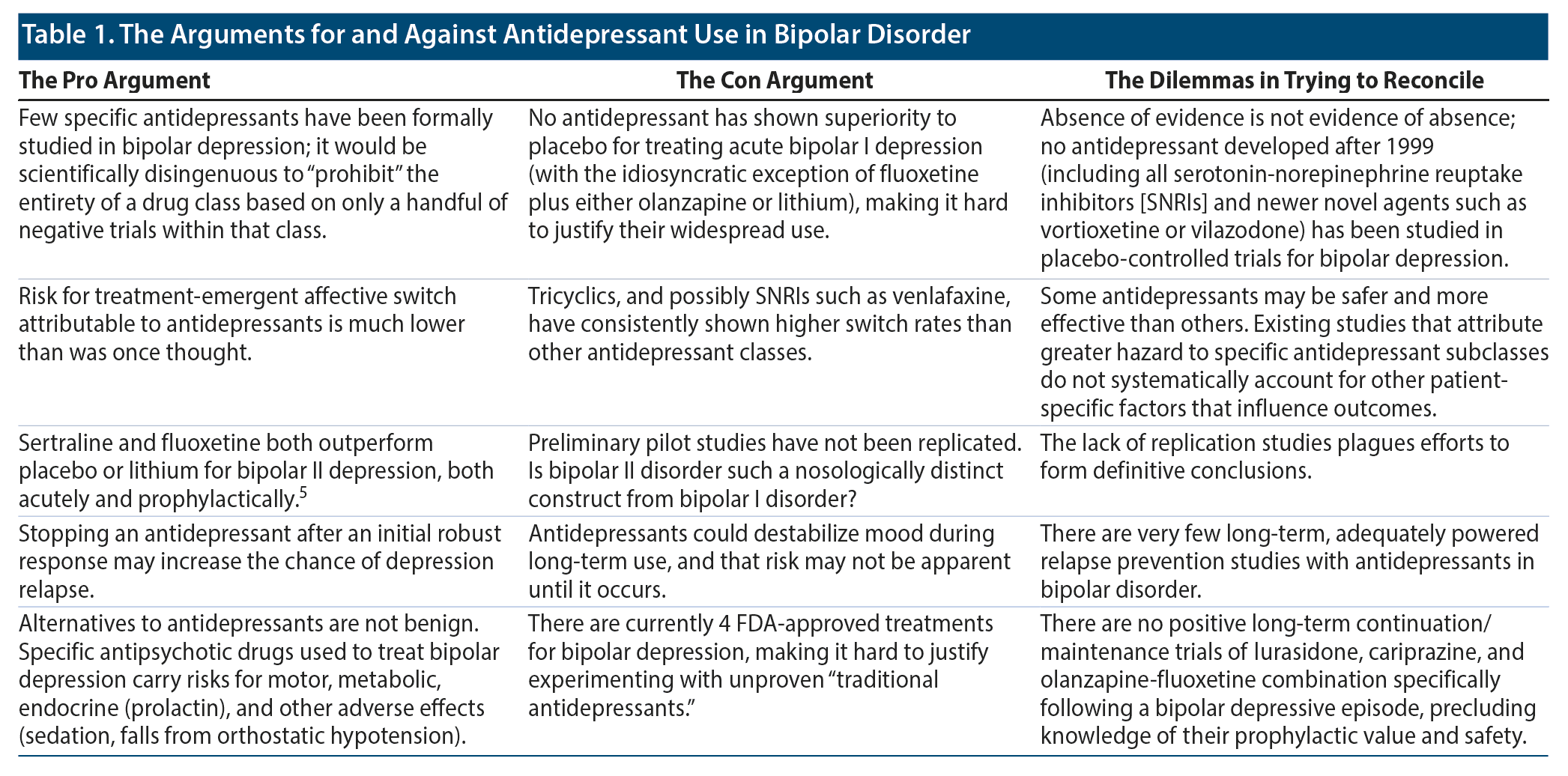
Table 1 presents the core challenges one must consider when deciding on the wisdom or lack thereof in using antidepressants for a given patient with bipolar disorder.
Perhaps the most solemn “takeaway” from this debate was the sense of frustration felt by many clinicians who want clear and simple guidance on “what to do” for bipolar depression, when no such simplicity exists. Having a rationale first requires appreciating that (a) lack of efficacy, more than risk for acute mood destabilization, appears to be the greatest challenge when using antidepressants, but (b) the paucity of large, replicated empirical trials (particularly with more modern agents) makes it hard to form generalizations about whether antidepressants as a class are helpful, harmful, or neither. Devising a strategy—whether that involves a monoaminergic antidepressant, one of the 4 FDA-approved antidepressant antipsychotic preparations, or a novel intervention (such as ketamine, lamotrigine ± lithium or quetiapine, or pramipexole, among others)—depends on the unique clinical profile of a given patient.
Every patient is an “N of 1” experiment, making someone’s personal history of response to a specific drug the most influential datapoint to guide that one patient’s further care. Absent such a personal history, one might weigh pros and cons of specific antidepressants based on the patient’s unique characteristics. Antidepressants appear inappropriate when current manic or hypomanic symptoms exist, and they should be deprescribed once lack of efficacy has been judged. Newer antidepressants lack data altogether, and, if chosen, their status as “unstudied entities” should be disclosed to patients. Perhaps most important of all is systematic and careful symptom monitoring, including recognition of manic symptoms in all depressed patients, when using any intervention for a condition as dynamic as bipolar depression; whether circumstances improve or worsen, resulting either from or despite an intervention, clinicians should be astute to the protean nature of bipolar disorder and be prepared to modify a treatment plan as dictated by changing symptoms and the observable consequences of any treatment, good or bad, antidepressant or otherwise.
Published online: January 19, 2021.
REFERENCES
1.Sachs GS, Nierenberg AA, Calabrese JR, et al. Effectiveness of adjunctive antidepressant treatment for bipolar depression. N Engl J Med. 2007;356(17):1711-1722. PubMed CrossRef
2.Prien RF, Kupfer DJ, Mansky PA, et al. Drug therapy in the prevention of recurrences in unipolar and bipolar affective disorders: report of the NIMH Collaborative Study Group comparing lithium carbonate, imipramine, and a lithium carbonate-imipramine combination. Arch Gen Psychiatry. 1984;41(11):1096-1104. PubMed CrossRef
3.Fornaro M, Anastasia A, Novello S, et al. Incidence, prevalence and clinical correlates of antidepressant-emergent mania in bipolar depression: a systematic review and meta-analysis. Bipolar Disord. 2018;20(3):195-227. PubMed CrossRef
4.Sidor MM, MacQueen GM. Antidepressants for the acute treatment of bipolar depression: a systematic review and meta-analysis. J Clin Psychiatry. 2011;72(2):156-167. PubMed CrossRef
5.Goldberg JF. Determining patient candidacy for antidepressant use in bipolar disorder. Psychiatr Ann. 2019;49(9):386-391. CrossRef
6.Altshuler LL, Post RM, Hellemann G, et al. Impact of antidepressant continuation after acute positive or partial treatment response for bipolar depression: a blinded, randomized study. J Clin Psychiatry. 2009;70(4):450-457. PubMed CrossRef
aDepartment of Psychiatry, Icahn School of Medicine at Mount Sinai, New York, New York
bDauten Family Center for Bipolar Treatment Innovation, Massachusetts General Hospital, Boston, Massachusetts
cHarvard Medical School, Boston, Massachusetts
dDepartment of Psychiatry, NYU Langone Health, New York, New York
eClinical Research Division, Nathan Kline Institute for Psychiatric Research, Orangeburg, New York
*Corresponding author: Joseph F. Goldberg, MD, 128 East Ave, Norwalk, CT 06851 ([email protected]).
J Clin Psychiatry 2021;82(1):19ac13181
To cite: Goldberg JF, Nierenberg AA, Iosifescu DV. Wrestling with antidepressant use in bipolar disorder: the ongoing debate. J Clin Psychiatry. 2021;82(1):19ac13181.
To share: https://doi.org/10.4088/JCP.19ac13181
© Copyright 2021 Physicians Postgraduate Press, Inc.
The ASCP Corner is a collection of brief peer-reviewed, evidence-based articles, authored by American Society of Clinical Psychopharmacology members, that examine the practice of psychopharmacology through the lens of clinical experience. The information contained herein only represents the opinion of the author(s).
See more ASCP Corner articles along with abstracts and updates from the last annual ASCP meeting at Psychiatrist.com/ASCP.
This PDF is free for all visitors!