Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
In the care of psychiatric patients, many of whom will require prolonged medication treatment and monitoring, the pharmacotherapy visit is one place where “the rubber meets the road.” Complex clinical and administrative needs must be addressed, often with incomplete clinical information during encounters that are abbreviated due to packed schedules and late arrivals. Clinician engagement is undermined by growing caseloads, increasing documentation requirements, coverage limitations, and the need to keep abreast of a growing body of knowledge that defines evidence-based practices.
This work may not be copied, distributed, displayed, published, reproduced, transmitted, modified, posted, sold, licensed, or used for commercial purposes. By downloading this file, you are agreeing to the publisher’s Terms & Conditions.

In the care of psychiatric patients, many of whom will require prolonged medication treatment and monitoring, the pharmacotherapy visit is one place where “the rubber meets the road.” Complex clinical and administrative needs must be addressed, often with incomplete clinical information during encounters that are abbreviated due to packed schedules and late arrivals. Clinician engagement is undermined by growing caseloads, increasing documentation requirements, coverage limitations, and the need to keep abreast of a growing body of knowledge that defines evidence-based practices. The challenge of performing a valid diagnostic assessment, making optimal treatment decisions, answering patients’ questions, and communicating with caregivers and other treatment providers is an increasingly formidable one.
Knowledge of the pharmacology of psychiatric medications is necessary but not sufficient for the delivery of appropriate, ethical, and high-quality care—to be more specific, care that is “safe, effective, patient-centered, efficient, timely, and equitable.”1(p3) Excellent resources are available to update clinicians on the properties of medications, but careful attention must also be paid to the framework and conduct of a pharmacotherapy visit.
Current opinion on the conduct of a pharmacotherapy visit is addressed in several texts2,3 as well as in an ASCP Model Psychopharmacology Curriculum statement.4 A recent paper5 on “reconceptualizing medication management” includes, in addition, an assessment tool for measuring clinician competency. The present article complements those sources by describing our view of how to provide long-term medication and focused psychotherapeutic management that incorporates both patients and their caregivers, including the core pharmacotherapy visit tasks. We will discuss initial evaluation and follow-up visits, recommending a systematic approach that prompts thoroughness and reinforces the crucial pharmacotherapeutic alliance.
The Initial Consultation
Before the first meeting, we often ask patients and caregivers to complete a comprehensive form (Table 1). This information helps the evaluating clinician to complete both an individual descriptive diagnostic assessment and a biopsychosocial formulation that provides a richer context for appreciating the identified patient’s concerns. In the office, a HIPAA privacy notice is signed, preliminary information is reviewed, and the patient’s target symptoms are discussed. The clinician asks about past and current psychiatric medication use, including benefits, adverse reactions, and allergies. Past psychotherapy experience is noted. An objective scale for rating symptoms and drug responses will provide baseline information for later comparison. Additional questions address the medical history including the presence or absence of relevant symptoms, disorders, and treatments as well as past or present recreational substance use. The evaluator learns about the patient’s understanding of his or her illness, motivation for treatment, and expectations or fears. A key issue is for patients, clinicians, and caregivers to agree on goals, including what can and cannot be achieved with medications.6
The Patient-Caregiver-Prescriber Alliance
Prime objectives of the initial visit are to obtain information, move toward an agreement about goals, and formulate a treatment approach. To accomplish these goals, the clinician must build an alliance with the patient and, often, caregivers.6 Caregiver involvement may help promote treatment adherence and decrease risk, but it requires valid patient consent. The alliance with caregivers has special importance in the care of patients with psychotic or neurocognitive disorders, whose communication and processing difficulties, whether transient or more persistent, may undermine treatment success.7
Toward the end of the initial evaluation, personalized psychoeducation is provided. The clinician elicits and responds to the patient’s questions about symptoms, diagnosis, prognosis, short- and long-term goals, treatment choices, and side effects. This interaction increases adherence and strengthens the treatment alliance. When appropriate, and with valid consent, information may be shared with caregivers and their questions or concerns can be discussed. Permission is also obtained for contacting other prior and current treatment providers, to coordinate care and to learn about previous treatment successes and problems that may recur in a new treatment relationship.
Before Each Follow-Up Visit
For expedient use of time, the patient and caregivers, as well as the treating clinician, should arrive at the follow-up visit aware of the preceding visit’s content and follow-up plan. The clinician should have in hand, and should have reviewed, new test results, including laboratory reports. These might include hematologic measures supporting clozapine treatment or neuropsychological tests assessing cognitive status. Relevant communications from other treatment team members such as a psychotherapist or caregiver should be available for discussion and for inclusion in further treatment planning as appropriate. Interim history includes an update on treatment adherence, benefits and adverse effects of medications, and new circumstances affecting the patient’s symptoms. When appropriate, and we consider this a standard practice rather than special case, patients and their caregivers and families should know the diagnoses and treatment plans.
The Follow-Up Visit
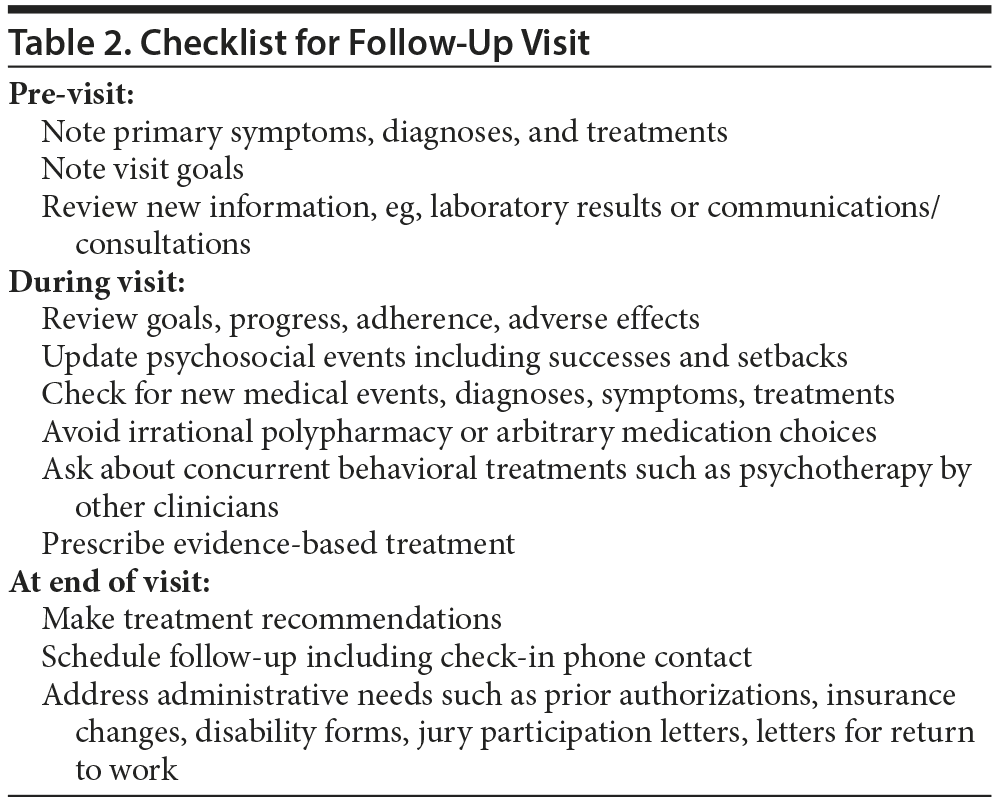
The overriding objective of follow-up visits is to deliver quality care that includes thorough assessment of the patient’s needs, appropriate interventions, adequate risk management, and compliance with regulatory needs. Table 2 shows a checklist for use in follow-up visits. We supplement office visits as needed with phone calls that are documented in the patient’s medical records. Medication reconciliation, eliciting of new concerns or new concurrent treatments, and a review of medication effects on target symptoms are essential. As appropriate, the pharmacotherapist may offer adjunctive psychotherapy that is focused and problem-oriented rather than exploratory. We encourage patients to call between sessions, at no additional charge, if urgent concerns arise. Various forms of asynchronous communication and data-gathering smartphone apps, providing additional data via secure forms of Internet-based messaging, are likely to enhance patient/clinician interaction in the future.
For familiar and stable patients, a visit of 20 to 30 minutes may be adequate. Those with severe or rapidly shifting symptoms should not be managed in sessions of inadequate length. When hospitalization is necessary, the clinician needs to devote adequate time for communicating treatment needs with a receiving institution. We oppose a 15-minute visit standard as excessively brief for many patients, but some individuals develop over time an ability to manage their symptoms and a strong treatment alliance that persists even during symptomatic exacerbations. Shortening visits too early in treatment, however, requires the clinician to rely on inadequate information and an impressionistic assessment, resulting possibly in misjudgment of a patient’s needs.
The allocation of time in a follow-up visit is tailored to specific needs, clinical or administrative, that may arise. In the absence of unexpected needs, one general strategy is to divide the available time (whether 5, 15, 30, 45, or 60 minutes) into 3 parts. The first, usually about one-fifth of the visit, is for inquiring about treatment adherence, response, and relevant new data. Medication reconciliation can be accomplished by asking the patient to list all the medications he or she is taking and describe any problems.8 Measurement-based care, increasingly recognized as a treatment enhancement, has become more common and can be accomplished efficiently by asking a patient to respond to paper or computerized questionnaires before the visit.9 We always inquire about use of recreational substances. We ask whether patients are actively taking their medications as prescribed and review any side effects. Patients often appreciate a frank discussion of the relative risks and benefits of pharmacotherapy, since side effects accompany most treatments.
The second portion of the visit, usually more than half the allotted time, focuses on global outcome in the context of the patient’s life in the community. This inquiry varies depending on the patient’s disorder and functional level. Areas to cover include work or school, family and other significant relationships, and quality of life. How patients appear in the office matters, but how they function and feel elsewhere is even more important. Clinicians must avoid shortcuts in treatment monitoring, even when based on a prolonged treatment relationship. Complacency or discouragement may cloud a clinician’s perception of important shifts in clinical status.
The last part of the visit, which is briefer, is devoted to reviewing the visit. The treatment plan must be agreed upon. In some cases, informed consent for a treatment intervention such as an antipsychotic may be required. We often ask patients and/or caregivers to take notes on our discussion of the treatment plan. We look for further psychoeducational needs and offer appropriate encouragement. The visit ends with a specific follow-up plan and scheduling of a subsequent visit.
Summary
In our suggestions, we have focused on the process and core elements of an effective pharmacotherapy evaluation and follow-up visit in the context of the patient’s life. Implementation of evidence-based care and measurement-based outcome management, keeping up to date with new medications and their risks or benefits, adapting to insurance-related constraints on time and medication access, and incorporating new initiatives related to integration of behavioral with primary medical care are important issues beyond the scope of this discussion but worthy of attention. Providing service as we have described is not simple, but this approach covers the critical bases and improves the odds of offering effective care.
Author affiliations: Department of Psychiatry and Behavioral Sciences, Stanford University School of Medicine, Stanford, California (Dr Glick); and Department of Psychiatry, Harvard Medical School, and McLean Hospital, Belmont, Massachusetts (Dr Ellison).
Potential conflicts of interest: None reported.
Funding/support: None reported.
Acknowledgments: The authors thank Donald Klein, MD, for suggestions and review.
Corresponding author: Ira D. Glick, MD, Department of Psychiatry and Behavioral Sciences, Stanford University School of Medicine, 401 Quarry Rd, Stanford, CA 94305 ([email protected]).
References
1. Scott KW, Jha AK. Putting quality on the global health agenda. N Engl J Med. 2014;371(1):3-5. PubMed doi:10.1056/NEJMp1402157
2. Klein DF. Diagnosis and Drug Treatment of Psychiatric Disorders: Adults and Children. 2nd ed. Baltimore, MD: Williams & Wilkins; 1980:1-25.
3. Schatzberg A, Cole JO, DeBattista C. Manual of Clinical Psychopharmacology. 7th ed. Washington, DC: American Psychiatric Press; 2010:3-13.
4. Glick ID, Zisook S, Balon R, et al. The ASCP Model Psychopharmacology Curriculum for Psychiatric Residency Programs, Training Directors and Teachers. 8th ed. Brentwood, TN: ASCP Inc; 2014:13-20.
5. Young JQ, Nelson JC. Reconceptualizing medication management: implications for training and clinical practice. J Clin Psychiatry. 2009;70(12):1722-1723. PubMed doi:10.4088/JCP.09ac05828whi
6. Srivastava R. Complicated lives—taking the social history. N Engl J Med. 2011;365(7):587-589. PubMed doi:10.1056/NEJMp1106985
7. Glick ID. Adding psychotherapy to pharmacotherapy: data, benefits, and guidelines for integration. Am J Psychother. 2004;58(2):186-208. PubMed
8. Pizzo P. Dean talks about physician communication. Stanford Medical Staff Update. 2011;35(6):3. http://med.stanford.edu/shs/update/archives/AUG2011/dean_talks.htm. Updated August 2011. Accessed April 10, 2015.
9. Harding KJ, Rush AJ, Arbuckle M, et al. Measurement-based care in psychiatric practice: a policy framework for implementation. J Clin Psychiatry. 2011;72(8):1136-1143. PubMed doi:10.4088/JCP.10r06282whi
J Clin Psychiatry 2015;76(6):735-736 (doi:10.4088/JCP.15ac10034).
© Copyright 2015 Physicians Postgraduate Press, Inc.
ASCP Corner offerings are not peer reviewed by the Journal but are peer reviewed by the ASCP. The information contained herein represents the opinion of the author.
Visit the Society Web site at www.ascpp.org
This PDF is free for all visitors!