Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
To the Editor: Recent studies demonstrate that cognitive remediation therapy (CRT) improves cognition and psychosocial functioning in people with depression. However, none of these studies appeared to include people with psychotic major depressive disorder, which from early episodes is associated with greater cognitive impairment than other mood disorders. Here, we present a case of first-episode psychotic major depressive disorder treated with CRT.
Cognitive Remediation Therapy for Psychotic Major Depressive Disorder
To the Editor: Recent studies1 demonstrate that cognitive remediation therapy (CRT) improves cognition and psychosocial functioning in people with depression. However, none of these studies1 appeared to include people with psychotic major depressive disorder, which from early episodes is associated with greater cognitive impairment than other mood disorders.2 Here, we present a case of first-episode psychotic major depressive disorder treated with CRT.
Case report. Following a 4-day admission to an acute ward, Ms A, a 27-year-old, female physician, was referred to CAMEO Early Intervention in Psychosis Service in Cambridge, United Kingdom, with a DSM-5 diagnosis of major depressive disorder with psychotic features. Despite treatment with quetiapine XL 600 mg and venlafaxine XL 225 mg, Ms A still suffered from occasional auditory hallucinations, and her mood remained low for several months after discharge. The patient received 8 sessions of cognitive-behavioral therapy for psychosis over 4 months but continued to complain of difficulties in planning tasks and lack of concentration that impeded her return to work. She was offered CRT as part of a training case for a therapist (S.A.), who was part of a team of investigators conducting a randomized controlled trial of CRT in nonaffective first-episode psychosis.3 The therapist was supervised by a CRT specialist senior clinical psychologist (M.C.).
Ms A attended 15 sessions over 3 months for a total of 18 hours including homework. She set the following CRT goals: to appraise and present a journal article as part of her research, plan routine tasks in optimal order, and improve mental arithmetic. She had no difficulties with these tasks premorbidly. Approximately half of the sessions involved completing tasks on a computer program,4 focusing on cognitive strategies and how to apply these to daily activities; the other half was devoted to in-vivo tasks. All of these activities were supported by the therapist.
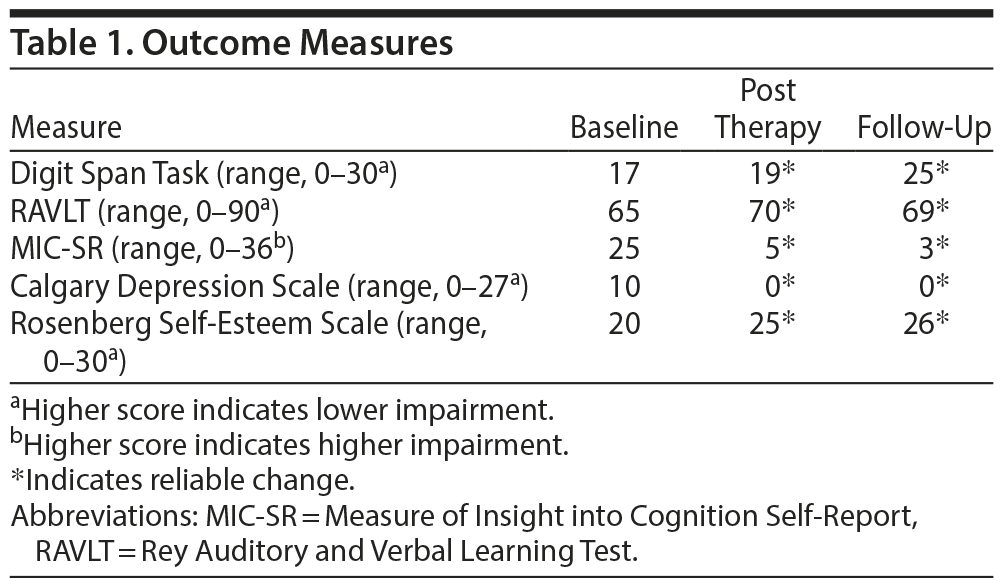
Measures of goals (Goal Attainment Scale5), cognition (Wechsler Digit Span Task,6 Rey Auditory and Verbal Learning Test7 part 1, and Measure of Insight into Cognition Self-Report8), and symptoms (Calgary Depression Scale9 and Rosenberg Self-Esteem Scale10) were obtained at baseline, after the last session, and 4 months after the end of therapy. All outcome measures demonstrated clinically reliable improvement11 sustained over time (Table 1). Ms A achieved all of her CRT goals and returned to work 11 months after her referral to the psychosis service. She is now near successful completion of her training program.
Ms A completed the Negative Incidents and Effects of Psychological Treatment Scale12 and a feedback form. No negative effects were reported, except mildly unpleasant memories of being bullied when she found tasks difficult. She reported that CRT helped her break down tasks to make their cognitive demand more manageable and felt that CRT was instrumental in rebuilding her confidence.
Ms A improved with a CRT program for nonaffective psychosis. However, she required fewer therapy hours (18) than that previously reported for people with schizophrenia (approximately 32).13 This need for fewer therapy hours may partly be due to milder cognitive impairment, higher levels of motivation, cognitive reserve, or premorbid functioning in psychotic major depressive disorder. Thus, there may be some scope to tailor CRT for this specific disorder. Additionally, given that psychotic major depressive disorder may be recurrent, maintenance sessions might be recommended.
This case study indicates that CRT can be effective and well tolerated in psychotic major depressive disorder. CRT could potentially be used to treat people with this condition in clinical settings such as early intervention in psychosis services. Further studies are required to confirm this finding.
References
1. Motter JN, Pimontel MA, Rindskopf D, et al. Computerized cognitive training and functional recovery in major depressive disorder: a meta-analysis. J Affect Disord. 2016;189:184-191. PubMed CrossRef
2. Zanelli J, Reichenberg A, Morgan K, et al. Specific and generalized neuropsychological deficits: a comparison of patients with various first-episode psychosis presentations. Am J Psychiatry. 2010;167(1):78-85. PubMed CrossRef
3. ISRCTN registry. ECLIPSE Study 9: Building resilience and recovery through enhancing cognition and quality. ISRCTN Regist. http://www.isrctn.com/ISRCTN14678860. Accessed June 5, 2018. CrossRef http://www.isrctn.com/ISRCTN14678860
4. Reeder C, Pile V, Crawford P, et al. The feasibility and acceptability to service users of CIRCuiTS, a computerized cognitive remediation therapy program for schizophrenia. Behav Cogn Psychother. 2016;44(3):288-305. PubMed CrossRef
5. Kiresuk TJ, Sherman RE. Goal attainment scaling: a general method for evaluating comprehensive community mental health programs. Community Ment Health J. 1968;4(6):443-453. PubMed CrossRef
6. Wechsler D. Manual for the Wechsler Adult Intelligence Scale. New York, NY: Psychological Incorporation; 1955.
7. Schmidt M. Rey Auditory and Verbal Learning Test: A Handbook. Los Angeles, CA: Western Psychological Association; 1996.
8. Medalia A, Thysen J, Freilich B. Do people with schizophrenia who have objective cognitive impairment identify cognitive deficits on a self-report measure? Schizophr Res. 2008;105(1-3):156-164. PubMed CrossRef
9. Addington D, Addington J, Maticka-Tyndale E, et al. Reliability and validity of a depression rating scale for schizophrenics. Schizophr Res. 1992;6(3):201-208. PubMed CrossRef
10. Rosenberg M. Society and the Adolescent Self-Image. Princeton, NJ: Princeton University Press; 1965.
11. Morley S, Dowzer CN. Manual for the Leeds Reliable Change Indicator: Simple Excel(tm) Applications for the Analysis of Individual Patient and Group Data. Leeds, United Kingdom: University of Leeds; 2014.
12. Rozental A, Kottorp A, Boettcher J, et al. Negative effects of psychological treatments: an exploratory factor analysis of the negative effects questionnaire for monitoring and reporting adverse and unwanted events. PLoS One. 2016;11(6):e0157503. PubMed CrossRef
13. Wykes T, Huddy V, Cellard C, et al. A meta-analysis of cognitive remediation for schizophrenia: methodology and effect sizes. Am J Psychiatry. 2011;168(5):472-485. PubMed CrossRef
aCambridgeshire and Peterborough NHS Foundation Trust, Cambridge, United Kingdom
bDepartment of Psychology, Institute of Psychiatry, Psychology, and Neuroscience, King’s College London, London, United Kingdom
cSouth London and Maudsley NHS Foundation Trust, London, United Kingdom
dDepartment of Psychiatry, University of Cambridge, United Kingdom
eNorwich Medical School, University of East Anglia, United Kingdom
fDepartment of Neuroscience, Instituto de Investigacion Biomedica de Salamanca (IBSAL), University of Salamanca, Spain
Potential conflicts of interest: None.
Funding/support: The authors acknowledge funding support from the National Institute for Health Research Programme Grant for Applied Research (NIHR PGfAR) RP-PG-0612-20002: "Building Resilience and Recovery through Enhancing Cognition and quality of LIfe in the early PSychosEs (ECLIPSE)." Dr Wykes acknowledges the support of the NIHR Biomedical Research Centre for Mental Health at the South London and Maudsley NHS Foundation Trust and King’s College London as well as the support of her NIHR Senior Investigator award. Dr Perez acknowledges support from the NIHR PGfAR RP-PG-0606-1335.
Role of the sponsor: The NIHR had no further role in the study design; the collection, analysis, and interpretation of data; the writing of the report; or the decision to submit the paper for publication.
Patient consent: Permission was received from the patient to publish this case, and information has been de-identified to protect anonymity.
Published online: June 14, 2018.
Prim Care Companion CNS Disord 2018;20(3):17l02180
To cite: Allan S, Cella M, Wykes T, et al. Cognitive remediation therapy for psychotic major depressive disorder. Prim Care Companion CNS Disord. 2018;20(3):17l02180.
To share: https://doi.org/10.4088/PCC.17l02180
© Copyright 2018 Physicians Postgraduate Press, Inc.
Enjoy this premium PDF as part of your membership benefits!