Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
To the Editor: Suicide stands in the top 3 causes of death among youth worldwide, and attempts are 20-40 times higher than completed suicide. The objective of this study was to find out whether those who attempted suicide and recovered perceived if their suicide attempt could have been prevented. Aims of the study were to know the degree of intent of the attempt, warning signs, and the risk factors.
Risk Factors, Warning Signs, and Intent in Referred Patients of Suicide Attempt After Recovery
To the Editor: Suicide stands in the top 3 causes of death among youth worldwide, and attempts are 20-40 times higher than completed suicide.1,2 The objective of this study was to find out whether those who attempted suicide and recovered perceived if their suicide attempt could have been prevented. Aims of the study were to know the degree of intent of the attempt, warning signs, and the risk factors.
Method. The study included 69 patients who had attempted suicide and were referred to the psychiatry department from other departments of Government Medical College, Udaipur, India. After obtaining patient consent, clinician-structured proforma was used to record risk factors and warning signs for attempt. Beck’s Scale for Suicide Ideation3 was used to assess the level of intent by understanding the severity of the attempt. SPSS version 19 (IBM Corp, Armonk, NY) was used for statistical analysis.
Results. Of the study participants, 57% (n = 39) of attempters were females and 39% (n = 27) were between 21 and 30 years of age, 30% (n = 21) were between 10 and 20 years of age, and 23% (n = 16) were > 40 years of age. There were 57% (n = 39) from a rural area, and 83% (n = 57) were from nuclear families.
For the 62 patients who provided more detailed information, 48% (n = 30) expressed medium intent, 24% (n = 15) expressed high intent, and 27% (n = 17) expressed low intent. Most had no premeditation (61% [n = 38]), ie, their attempt was an impulsive act, and 29% (n = 18) contemplated suicide for > 3 hours prior to the attempt. The primary purpose of the attempt for 48% (n = 30) was to escape or surcease or solve their problems; 37% (n = 23) wanted to manipulate or get attention or revenge through the attempt. After the attempt, 74%, (n = 46) felt sorry or were ashamed in reaction to their attempt, and 8% (n = 5) had regrets in the failure of attempt.
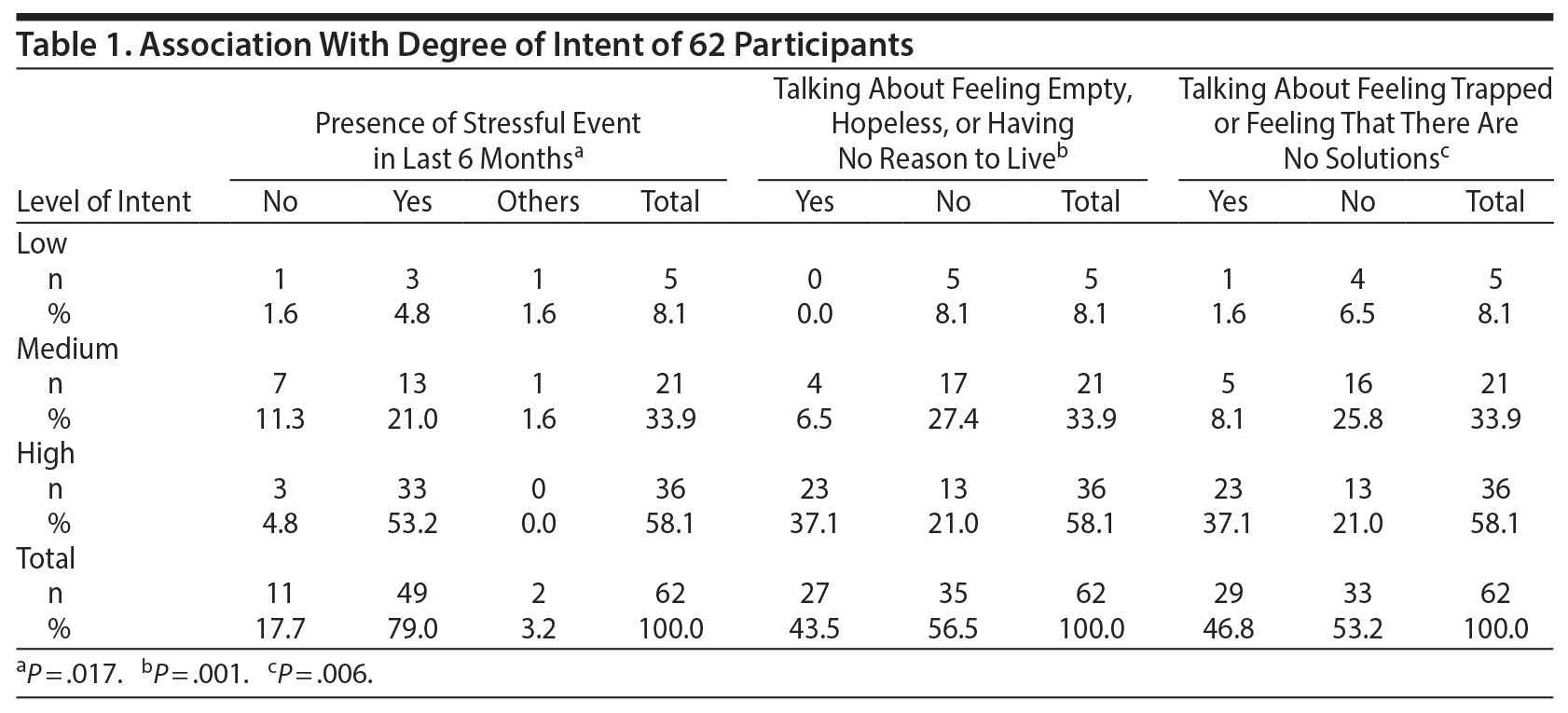
Intent was high in 53% (n = 33) in the presence of stressful events, with significant association between stressful events in the last 6 months (P = .017). Srivastava et al4 also observed significant association between stressful events. A significant association (P = .001) was observed between talking about feeling empty, hopeless, or having no reason to live and degree of intent: high intent was seen in 37% (n = 23). Association was also observed between talking about feeling trapped or feeling that there are no solutions and degree of intent: intent was high (P = .006) in 37% (n = 23) (Table 1).
Stressful events from the past were present in 78% (n = 50/64), psychiatric illness was present in 70% (n = 47/67), history of substance abuse was seen in 34% (n = 22/64), history of family violence including physical and sexual abuse was present in 23% (n = 15/64), and previous attempts and family history of attempt or completed suicide were present in 13% (n = 8/62) and 6% (n = 4/67), respectively.
Among the 66 patients with psychiatric illnesses, depression were present in 33% (n = 22/66) and schizophrenia or psychotic disorder in 15% (n = 10/66), with other disorders (eg, bipolar affective disorder, personality disorder) occurring in smaller numbers. The immediate cause of the attempt was mental illness in 50% (n = 32/64), interpersonal problems in 30% (n = 19/64), and love affair failure in 8% (n = 5/64). The main method used in an attempt was poisoning in 80% (n = 51/64). Changes in patient behavior was evident prior to the attempts, with 86% (n = 54/63) acting anxious or agitated, 65% (n = 41/63) having mood swings, 64% (n = 40/63) experiencing changes in eating/sleeping, and 56% (n = 35/63) often talking or thinking about death.
Discussion. The majority of attempters were aged < 30 years (70% [n = 48]). Similar observation was seen by Kodali and Kilaru.5 Female preponderance in this study (57% [n = 39]) is similar to the finding by Ramanathan et al6; however, male preponderance is observed by Ponnudurai et al7 and Narang et al.8
Low intent of 27%, medium of 48%, and high of 24% in our group is comparable in low to medium intents found by Ramanathan et al6 where low, medium, and high intent was 64%, 16%, and 20%, respectively.
The present study compares its finding with other distant geographical areas within the country, making it of interest for other populations. A substantial percentage of attempters had medium to high intent and also had underlying psychiatric disorder, which signifies that prompt identification and proper treatment of psychiatric illness will help in preventing an attempt. Attempts may also be prevented if family members and friends carefully observe the warning signs and risk factors and intervene appropriately.
References
1. Mental health, Suicide Prevention. World Health Organization. WHO website. http://www.who.int/mental_health/prevention/suicide/suicideprevent/en/. Accessed March 31, 2018.
2. Schmidtke A, Bille-Brahe U, DeLeo D, et al. Attempted suicide in Europe: rates, trends and sociodemographic characteristics of suicide attempters during the period 1989-1992: results of the WHO/EURO multicentre study on parasuicide. Acta Psychiatr Scand. 1996;93(5):327-338. PubMed CrossRef
3. Beck AT, Kovacs M, Weissman A. Assessment of suicidal intention: the Scale for Suicide Ideation. J Consult Clin Psychol. 1979;47(2):343-352. PubMed CrossRef
4. Srivastava MK, Sahoo RN, Ghotekar LH, et al. Risk factors associated with attempted suicide: a case control study. Indian J Psychiatry. 2004;46(1):33-38. PubMed
5. Kodali M, Kilaru K. Psychiatric morbidity of attempted suicide patients admitted to a general hospital in rural area of South India. IOSR Journal of Dental and Medical Science. 2013;4(3):46-50. CrossRef
6. Ramanathan R, Ramachandran AS, Periasamy K, et al. Assessment of suicidal intent. Indian J Psychol Med. 2016;38(6):529-532. PubMed CrossRef
7. Ponnudurai R, Jeyakar J, Saraswathy M. Attempted suicides in Madras. Indian J Psychiatry. 1986;28(1):59-62. PubMed
8. Narang RL, Mishra BP, Nitesh M. Attempted suicide in ludhiana. Indian J Psychiatry. 2000;42(1):83-87. PubMed
aDepartment of Psychiatry, RNT Medical College, Udaipur, Raj, India
Potential conflicts of interest: None.
Funding/support: None.
Previous presentation: The results of this study were presented at the World Congress of Mental Health organized by World Federation for Mental Health; November 2-5, 2017; at New Delhi, India.
Published online: February 7, 2019.
Prim Care Companion CNS Disord 2019;21(1):18l02313
To cite: Sharma S, Kherada S, Gocher S, et al. Risk factors, warning signs, and intent in referred patients of suicide attempt after recovery. Prim Care Companion CNS Disord. 2019;21(1):18l02313.
To share: https://doi.org/10.4088/PCC.18l02313
© Copyright 2019 Physicians Postgraduate Press, Inc.
Enjoy this premium PDF as part of your membership benefits!