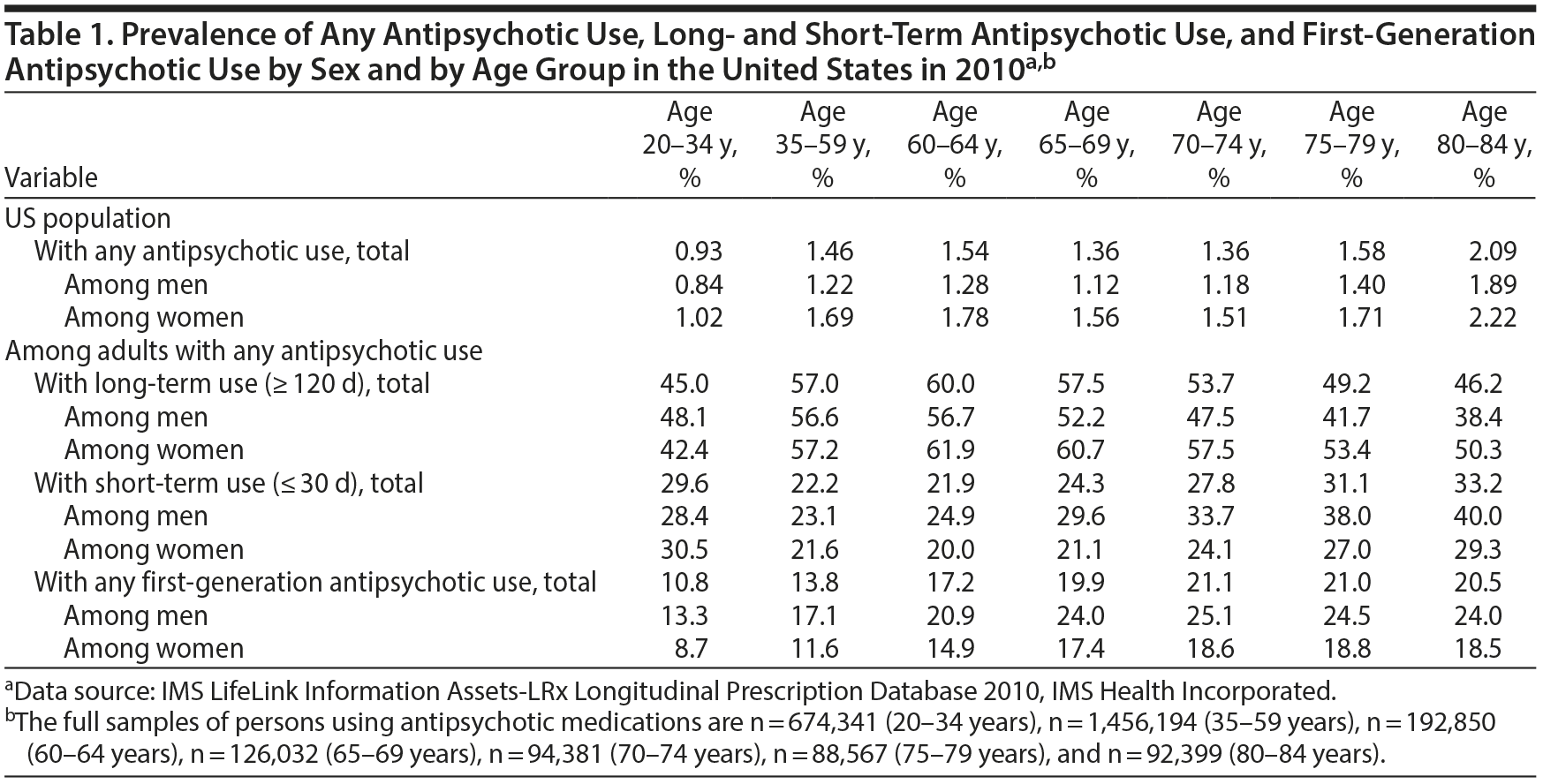Objective: Despite safety risks associated with antipsychotic medications, little is known about their use in older adults. This article describes patterns of antipsychotic treatment of older and younger adults in the United States.
Method: The IMS LifeLink LRx Longitudinal Prescription database was analyzed retrospectively, focusing on adults who filled antipsychotic prescriptions. The database was searched for the years 2006 and 2008-2010. Denominators were adjusted to generalize annual antipsychotic use percentages by sex and single year of age to the US population. Among adults with any antipsychotic use, percentages with short-term (≤ 30 days) and long-term (≥ 120 days) use, prescriptions from psychiatrists, use of other psychotropic medication classes, and ICD-9 clinical diagnoses were also evaluated.
Results: The percentages of US adults by age group who used antipsychotics in 2010 were 0.93% (20-34 years), 1.46% (35-59 years), 1.54% (60-64 years), 1.36% (65-69 years), 1.36% (70-74 years), 1.58% (75-79 years), and 2.09% (80-84 years). Women were consistently more likely than men to use antipsychotics. The percentages of antipsychotic-treated older adults with long-term use were 53.7% (70-74 years), 49.2% (75-79 years), and 46.2% (80-84 years). Among adults with any antipsychotic use, percentages with prescriptions from psychiatrists decreased with age from 66.2% (20-34 years) to 20.6% (80-84 years). Dementia was commonly diagnosed among antipsychotic-treated adults aged 75-79 years (37.2%) and 80-84 years (47.8%) who had any mental disorder or dementia diagnoses.
Conclusions: Despite concerns over the safety of antipsychotic treatment of older adults, long-term use is common. Key challenges for clinical research and practice include development and implementation of management strategies for older adults that are safer than antipsychotic medications.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
ABSTRACT
Objective: Despite safety risks associated with antipsychotic medications, little is known about their use in older adults. This article describes patterns of antipsychotic treatment of older and younger adults in the United States.
Method: The IMS LifeLink LRx Longitudinal Prescription database was analyzed retrospectively, focusing on adults who filled antipsychotic prescriptions. The database was searched for the years 2006 and 2008-2010. Denominators were adjusted to generalize annual antipsychotic use percentages by sex and single year of age to the US population. Among adults with any antipsychotic use, percentages with short-term (≤ 30 days) and long-term (≥ 120 days) use, prescriptions from psychiatrists, use of other psychotropic medication classes, and ICD-9 clinical diagnoses were also evaluated.
Results: The percentages of US adults by age group who used antipsychotics in 2010 were 0.93% (20-34 years), 1.46% (35-59 years), 1.54% (60-64 years), 1.36% (65-69 years), 1.36% (70-74 years), 1.58% (75-79 years), and 2.09% (80-84 years). Women were consistently more likely than men to use antipsychotics. The percentages of antipsychotic-treated older adults with long-term use were 53.7% (70-74 years), 49.2% (75-79 years), and 46.2% (80-84 years). Among adults with any antipsychotic use, percentages with prescriptions from psychiatrists decreased with age from 66.2% (20-34 years) to 20.6% (80-84 years). Dementia was commonly diagnosed among antipsychotic-treated adults aged 75-79 years (37.2%) and 80-84 years (47.8%) who had any mental disorder or dementia diagnoses.
Conclusions: Despite concerns over the safety of antipsychotic treatment of older adults, long-term use is common. Key challenges for clinical research and practice include development and implementation of management strategies for older adults that are safer than antipsychotic medications.
J Clin Psychiatry 2015;76(10):1346-1353
dx.doi.org/10.4088/JCP.15m09863
© Copyright 2015 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, College of Physicians and Surgeons, Columbia University and New York State Psychiatric Institute, New York, New York
bYale University, School of Management, New Haven, Connecticut
cOffice of the Science Policy, Planning and Evaluation, National Institute of Mental Health, National Institutes of Health, Bethesda, Maryland
*Corresponding author: Mark Olfson, MD, MPH, New York State Psychiatric Institute/Department of Psychiatry, College of Physicians and Surgeons of Columbia University, 1051 Riverside Drive, New York, NY 10032 ([email protected]).
Antipsychotics are one of the most commonly prescribed classes of medications in the United States.1 In adults, they have been approved by the US Food and Drug Administration (FDA) as a primary treatment for schizophrenia,2 bipolar disorder,3 and Tourette’s disorder (haloperidol and pimozide) as well as an adjunctive treatment for major depressive disorder (aripiprazole and olanzapine).4 Yet in office-based practice only about half (45%) of antipsychotic prescriptions to adults 18 to 64 years of age and approximately one-quarter (26%) of such prescriptions to adults aged 65 years and older are to patients who have been diagnosed with one of these FDA-approved indications.5 Similar results have been reported from Medicaid administrative data in which a smaller percentage of antipsychotic-treated adults aged over 65 years (35%) than similarly treated adults aged 21 to 64 years (51%) received a clinical diagnoses for one of the FDA-approved indications.6
In the care of older adults, there are safety concerns over the off-label use of antipsychotics to manage aggression, agitation, delusions, and other neuropsychiatric symptoms in Alzheimer’s disease and dementia.7 In older adults, antipsychotic use has been associated with an increased risk of cerebrovascular events,8 fractures,9 acute kidney injury,10 and premature mortality.11 All antipsychotics include a boxed warning from the FDA concerning an increased risk of mortality in adults with dementia.12
Characterizing patterns of antipsychotic use among adults, including older adults especially, can provide clinicians and policy makers with insights into the distribution of antipsychotic treatment and help focus attention on populations at risk for potentially excessive antipsychotic use. Previous research on adult antipsychotic treatment patterns in the United States has been largely limited to specific payers, including Medicaid,13 Medicare,14 the US Department of Veterans Affairs,15 or private insurance,16 or to specific treatment settings, such as nursing homes16 or office-based practice.5 Most antipsychotic treatment among older adults in the United States occurs among community residents rather than nursing home residents.17 A paucity of information on national patterns of antipsychotic use among adults, especially among older adults, across payers and treatment settings hinders clinical and policy planning.
We present results from an analysis of a large US prescription database that includes all payers and permits estimation of national percentages of antipsychotic use among adults by sex and single year of age, duration of use, specialty of prescribing physician, and coprescribed psychotropic medications. Clinical diagnostic information was also available on a subset of the antipsychotic-treated adults.
METHOD
We conducted a population-level, retrospective observational study of antipsychotic use among adults in the United States with data from the IMS LifeLink LRx Longitudinal Prescription database and the Medical Expenditure Panel Survey (MEPS).18 The LifeLink data contain deidentified individual prescriptions from approximately 33,000 retailers including approximately 3,000 pharmacies in long-term care facilities such as nursing homes and nursing home providers. In 2010, IMS data captured 63% of all retail prescriptions in the United States and were nationally representative with respect to age, sex, and health insurance. Because the following analyses rely exclusively on deidentified data, they were exempted from human subjects review by the institutional review boards of Yale University and New York State Psychiatric Institute.
From IMS Health, we obtained data from filled prescriptions for all antipsychotics in 2006, 2008, 2009, and 2010 by sex and age, as well as the total population covered by the dataset by sex and age. Prescriptions for other psychotropic medications were also available in 2008. Only individuals filling a prescription at a retail outlet, including mail order, are captured in the database. To generalize our prevalence estimates of antipsychotic use to the entire US population of adults, including individuals who did not fill a prescription during the study period, we adjusted the denominators using data from the MEPS. This adjustment permits estimation of antipsychotic use by age and by sex to all civilians aged 20 to 84 years in the United States. The age and sex composition of the IMS population that filled at least 1 prescription of any kind closely resembled the composition of the corresponding population from the nationally representative MEPS. The original datasets are available from IMS Health, New York, New York, and from the MEPS website (http://meps.ahrq.gov/mepsweb/).

- Although antipsychotics are strongly contraindicated for the treatment of older adults with dementia, little is known about antipsychotic community prescribing practices.
- Antipsychotic treatment rates increase with advancing adult age, and among older, antipsychotic-treated patients, dementia is the most commonly diagnosed mental disorder.
- There is a critical need to increase access to alternative interventions for this patient population.
In addition to the age and sex of the patient, the IMS data included the name of the medication for which the prescription was written, the days of supply, the specialty of the prescriber, and prescriptions for other psychotropic medications (in 2008). Among adults with any antipsychotic use, we determined the percentages of those who within the year had short-term antipsychotic use (≤ 30 days), had long-term antipsychotic use (≥ 120 days), had all of their antipsychotic prescriptions written by a nonpsychiatrist physician, had at least 1 prescription for a first-generation antipsychotic medication, and had at least 1 prescription for an antidepressant, anxiolytic, or mood stabilizer. The analyses were stratified by men and women and by age group, with a particular focus on older aged adults (20-34, 35-59, 60-64, 65-69, 70-74, 75-79, and 80-84 years).
The 2009 IMS Medical Claims Database, which includes over 16 million service claims per month from over 100,000 unique physicians across all 50 US states, was merged with pharmacy claims from patients common to the 2009 LRx database. The merged 2009 IMS Medical Claims Database and 2009 IMS LifeLink LRx Longitudinal Prescription database included 257,616 antipsychotic-treated patients aged 20 to 84 years with service claims. Among this group, we first examined the percentage who received 1 or more claim for a mental disorder or dementia. Among the antipsychotic-treated group with at least 1 mental disorder or dementia claim, we examined by age group and sex the percentage with 1 or more service claims with a diagnosis of schizophrenia (ICD-9 codes: 295.xx), bipolar disorder (ICD-9 codes: 296.0x, 296.1x, 296.4x, 296.5x, 296.6x, 296.7x, 296.8x), depression (ICD-9 codes: 296.2x, 296.3x, 296.82, 298.0, 300.4, 311), pervasive developmental disorder or mental retardation (ICD-9 codes: 299.xx, 317.xx, 318.xx, 319.xx), dementia (ICD-9 codes: 290.0, 290.1x, 290.2x, 290.3, 290.4x, 291.2, 294.10, 294.11, 294.21, 331.0, 331.1, 331.2, 331.7, 331.82, 331.89, 331.9), or other mental disorders (ICD-9 codes: 290-319, not otherwise defined).
RESULTS
Age and Sex Patterns of Antipsychotic Use
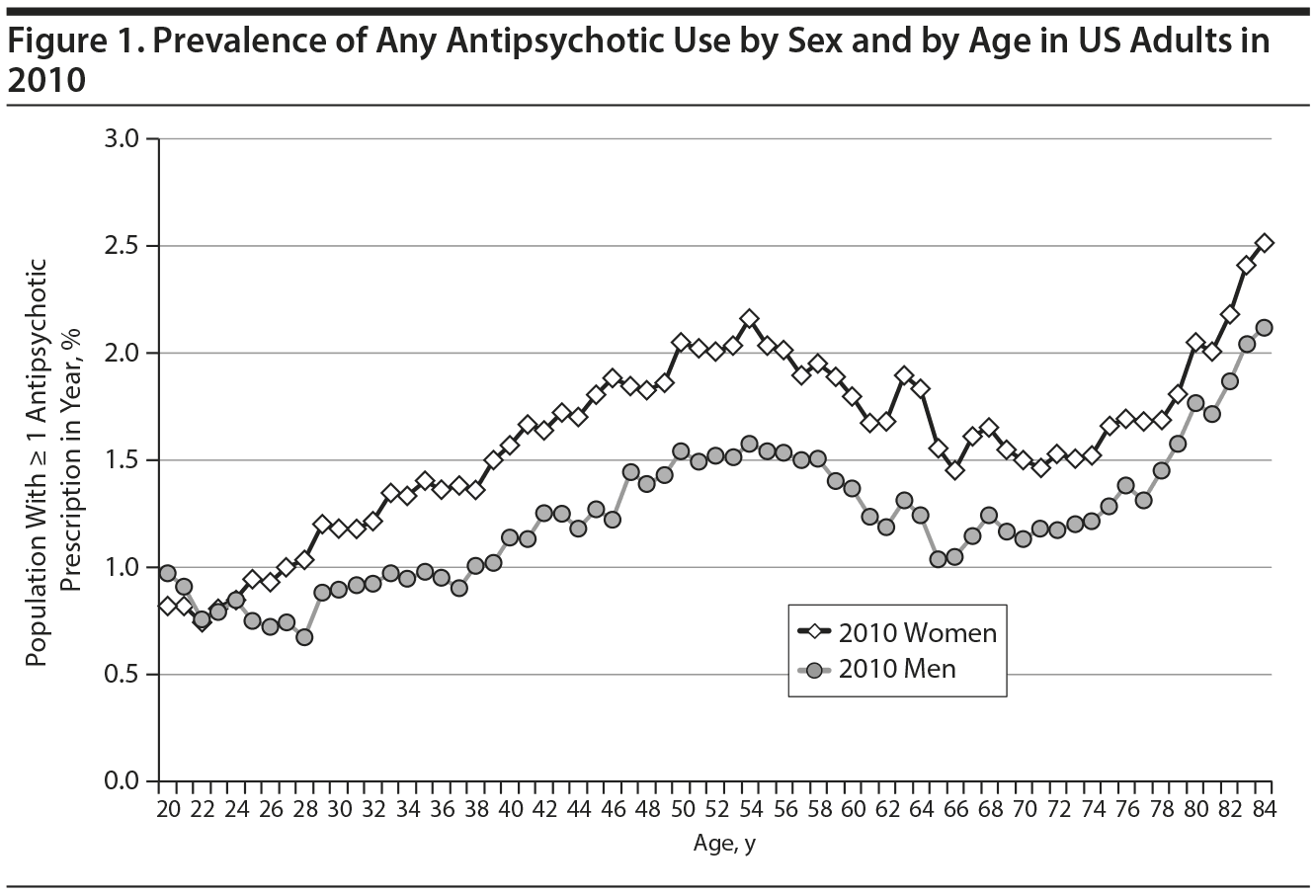
The percentage of adults with any antipsychotic use in 2010 was determined by single year of age (20 to 84) for men and women (Figure 1). Each year between ages 25 and 84 years, women had a higher rate of antipsychotic use than men. The percentages of women and men who used antipsychotics tended to increase starting when patients were in their early 20s until they reached age 54 years, then decrease until they reached age 66 years, and then increase to age 84. Similar patterns were observed in 2006 and 2008 (see Supplementary eFigures 1A and 1B at Psychiatrist.com). In 2010, approximately 2.5% of women and 2.1% of men 84 years of age received ≥ 1 antipsychotic prescription.
Among adults with any antipsychotic use, the percentage with long-term use varied by age group from 45.0% (20-34 years) to 60.0% (60-64 years). Older women who were treated with antipsychotics were more likely than corresponding older men to have long-term use and less likely to have short-term use. The percentage of antipsychotic-treated adults that received first-generation agents was higher among older than middle-aged or younger adults and among men than women (Table 1).
Antipsychotic Prescriptions From Psychiatrists
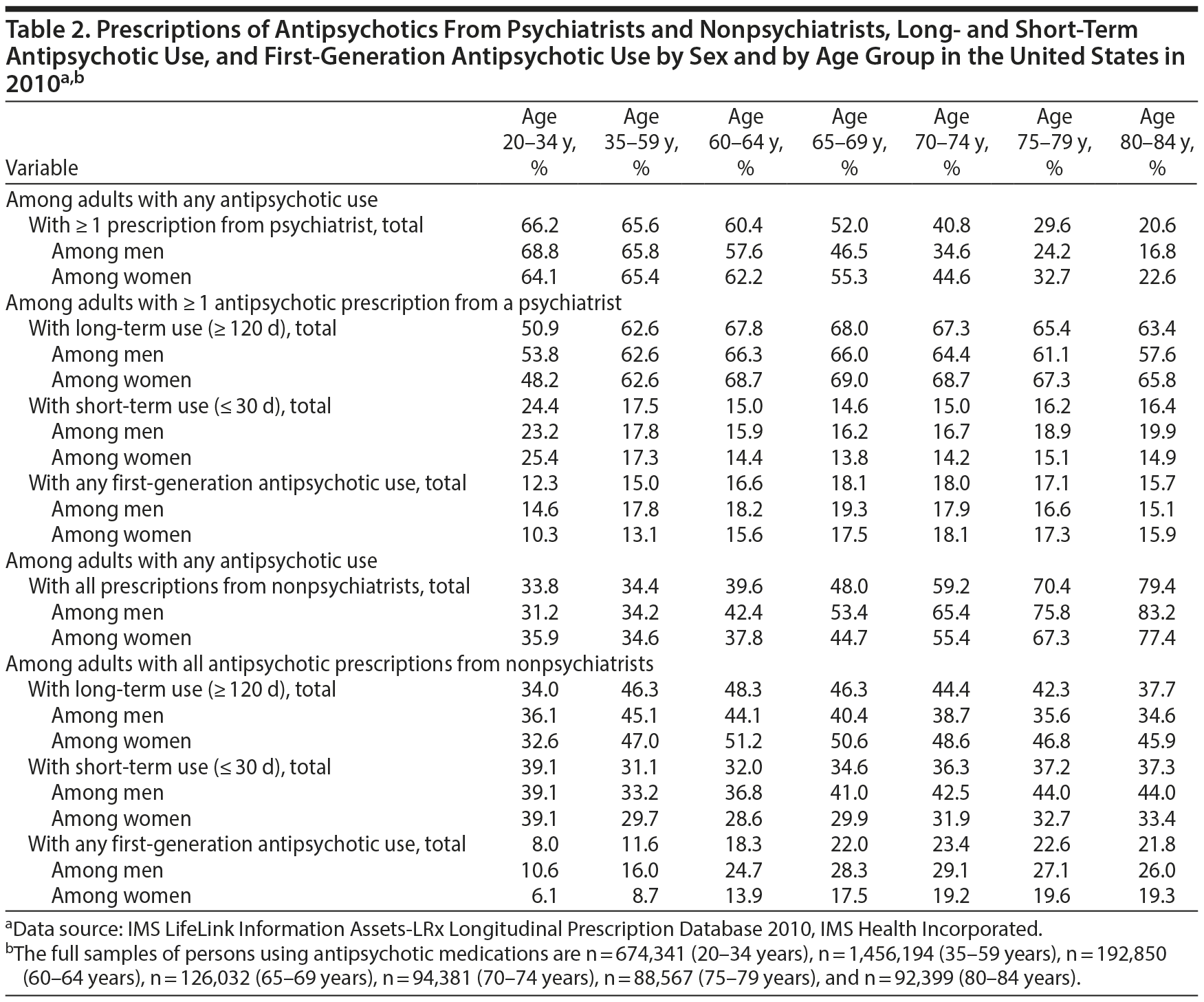
Among adults with any antipsychotic use in 2010, the proportion that filled ≥ 1 prescription written by a psychiatrist declined with patient age from 66.2% (20-34 years) to 20.6% (80-84 years). This pattern was especially evident for men; 16.8% of antipsychotic-treated men aged 80 to 84 years filled a prescription from a psychiatrist (Table 2).
Long-term antipsychotic treatment was considerably more common among adults of all ages who received at least some of their prescriptions from psychiatrists than among those who received all of their prescriptions from nonpsychiatrist physicians. By contrast, short-term use at all ages was proportionately less common among adults who received at least some of their antipsychotics from psychiatrists than among adults who received all antipsychotics from nonpsychiatrist physicians. As compared with older adults who received antipsychotics from nonpsychiatrists, those who received them from psychiatrists were also less likely to be treated with first-generation agents (Table 2).
Other Classes of Psychotropic Medications
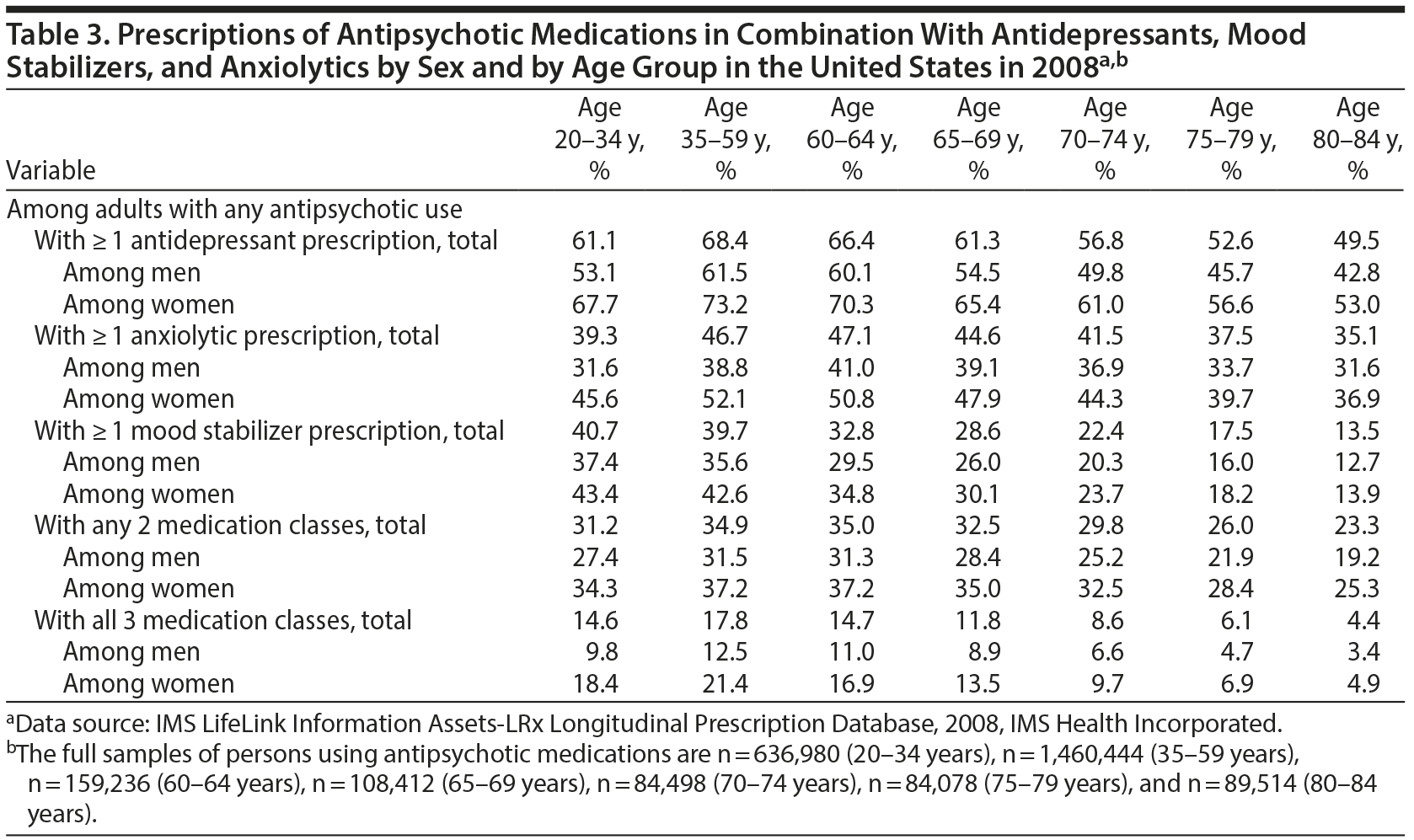
During 2008, most adults who were treated with antipsychotic medications were also treated with other classes of psychotropic medications. Across all 7 age groups, antidepressants were the most commonly prescribed other class of psychotropic medication, with women proportionately more likely than men to receive both classes of medications. Anxiolytics, which were the second most commonly prescribed other class of psychotropic medication, were also proportionately more commonly prescribed to antipsychotic-treated women than men. The percentage of adults prescribed antipsychotics who were also prescribed mood stabilizers declined with age. Similar declines with age were observed for antipsychotic-treated men and women who were prescribed any 2 or all 3 of the other psychotropic medication classes during the study year (Table 3).
Clinical Diagnoses
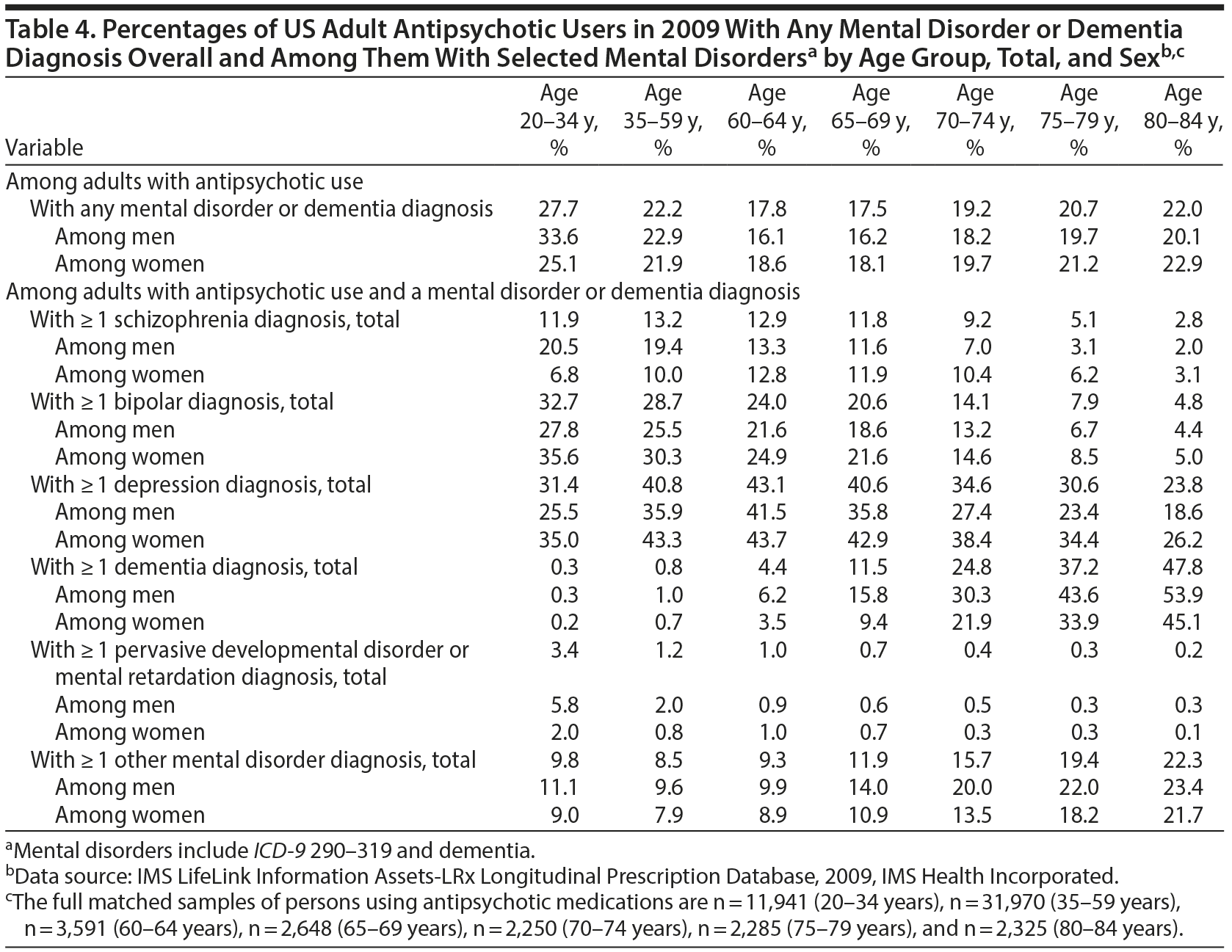
In the merged 2009 medical claims and LRx sample, most antipsychotic-treated adults in each age group and both sexes had no outpatient or inpatient claim that included a mental disorder diagnosis or dementia diagnosis. Among antipsychotic-treated adults with ≥ 1 claim for a mental disorder or dementia, depression and bipolar disorder were the most common diagnoses in young (20-34 years) and middle-aged (35-59 years) adults. Across all age groups, schizophrenia was diagnosed in less than one-quarter of antipsychotic-treated adults with any mental disorder or dementia diagnoses. Among the 2 oldest age groups, dementia was the most common diagnosis, particularly among men. Dementia was diagnosed in over half (53.9%) of the antipsychotic-treated men in the 80- to 84-year age subgroup with any mental disorder or dementia diagnoses (Table 4). In post hoc analyses of antipsychotic-treated adults with dementia, 67.4% of persons aged 75 to 79 years and 69.5% of persons aged 80 to 84 years received long-term antipsychotic treatment (data not shown).
DISCUSSION
In the United States, the rate, specialty of the prescribing physician, and clinical diagnoses associated with antipsychotic medication use varied across the adult lifespan. The population-based rate of antipsychotic use rose slowly during early and middle adulthood, peaked around age 55 years, and then declined over the following decade before increasing again after age 65 years. From ages 25 to 84 years, women had consistently higher rates of antipsychotic use than men. With advancing age, adults treated with antipsychotic medications were more likely to receive their prescriptions from nonpsychiatrist physicians than psychiatrists. At all ages, a great majority of antipsychotic-treated adults had no evidence of clinically diagnosed mental disorders or dementia in their claims records. When these diagnoses did appear in the claims record, antipsychotic treatment was commonly related to depression and bipolar disorder in young and middle aged adults and to dementia in older adults.
These national patterns in antipsychotic use provide a window into the antipsychotic treatment of adults across the lifespan. The single year of age patterns of antipsychotic use refine earlier population-based antipsychotic use estimates from Italy,19 Canada,20 and the United Kingdom21 that involved multiyear age categories. Consistent with these reports, rates of antipsychotic use in the United States increased in older age, with an abrupt rise starting in adults in their midseventies. This increase most likely reflects an increase in the underlying prevalence of dementia during this age period. In a large, US epidemiologic study,22 dementia was present in 5% of adults aged 71 to 79 years and 24% in those aged 80 to 89 years.
The rate of antipsychotic use gradually declined between ages 55 and 65 years. It is possible that changes in the prevalence or course of major mood disorders during this period of life contribute to this decline. The likelihood of having major depressive disorder, dysthymia, or bipolar disorder declines between ages 55 and 65 years for men and women.23 In some clinical studies, there is also evidence that older as compared to younger adults with bipolar disorder tend to have fewer manic symptoms,24 less often have psychotic symptoms,25 and have lower rates of treatment with antipsychotic medications.25 Other studies, however, have reported few differences in the acute presentation of bipolar disorder in older and younger adults.26 Nevertheless, it is noteworthy that starting around age 60 years and continuing into older age there was a decline in the percentage of antipsychotic-treated adults who were also treated with mood stabilizers.
Across the adult lifespan, women had higher rates of antipsychotic use than men. This difference, which has been previously reported outside of the United States,19-21 may be related to the higher prevalence of major depressive disorder in women than in men.27 Although the community prevalence of bipolar disorder is similar in men and women,28 treatment seeking and adherence may be greater in women.29 There is also evidence from some,30 but not all,22 epidemiologic studies of older adults that dementia is more prevalent in women than men.
Long-term antipsychotic treatment was common across all of the age groups. The pattern of clinical diagnoses, however, suggests that only a small proportion of older adults who are treated with antipsychotics have disorders for which long-term or maintenance antipsychotic treatment is generally indicated. Although strong evidence supports long-term antipsychotic treatment for schizophrenia,31 only a small percentage of antipsychotic-treated adults within each age group were diagnosed with schizophrenia. Several antipsychotics (olanzapine, quetiapine, aripiprazole, long-acting risperidone, and ziprasidone) also have an established role in the maintenance treatment of bipolar disorder.32 Again, however, only a small percentage of older antipsychotic-treated adults were diagnosed with bipolar disorder.
Depression and dementia diagnoses were common among antipsychotic-treated older adults. Yet there is only limited evidence to support the efficacy of long-term antipsychotic adjuvant treatment of major depressive disorder and little available evidence on long-term safety of antipsychotic medications in this patient population.33 Uncertainty over effectiveness should be considered with the risks of serious adverse events that are a strong contraindication to long-term antipsychotic treatment of dementia.34 In a randomized placebo-controlled trial35 of adults with Alzheimer’s disease, the 12-month cumulative probability of survival of subjects assigned to continue antipsychotics (70%) was significantly lower than those assigned to placebo (77%). Because antipsychotic use in older adults with clinically diagnosed dementia was often long-term, the present findings raise concerns over the safety of this community prescribing practice.
In contrast to the antipsychotic treatment of younger adults, which usually involved prescriptions from psychiatrists, antipsychotic treatment of older adults was predominantly provided exclusively by nonpsychiatrist physicians. This pattern is part of a broader tendency for older adults to receive their mental health care within the general medical rather than specialty mental sector.36 Good assessment and management of behavioral and psychological symptoms of dementia involve tailoring interventions by (1) accurately describing the symptoms and the contexts in which they occur; (2) investigating possible underlying and modifiable causes; (3) creating and implementing a treatment plan that employs pharmacologic, behavioral, or environmental interventions that target the most distressing symptoms; and (4) evaluating whether the recommended interventions were implemented and effective.37
The FDA issued a black box warning in 200538 concerning increased risk of death among patients with dementia-related psychosis treated with atypical antipsychotics that was subsequently extended to conventional antipsychotics in 2008.39 Although prior research indicated that between 2005 and 2008 there was a decrease in antipsychotic use among older adults with dementia and among individuals of all ages that was temporally linked to the first FDA warning,40 we found no evidence of an overall reduction in antipsychotic use among older adults between 2006 and 2010.
This analysis has several limitations. First, the IMS prescription data capture medicines purchased rather than used. Second, clinical diagnoses were available on only a subset of patients in the larger database, and the clinical intent of antipsychotic treatment may not align with diagnoses in the claims record. Third, no measures were available for neuropsychiatric symptoms, which are core features of Alzheimer’s disease and commonly manifest in early stage and prodromal phases. Fourth, although the population denominator was adjusted for the percentage of the population by age and sex who reported not filling a prescription medication within the year, it is not possible to estimate the precision of the derived estimates. Finally, the primary analyses are based on 2010 dispensing patterns. Since that time, community antipsychotic prescribing practices may have changed.
High rates of antipsychotic use among older adults paired with common diagnoses of dementia raise critical quality-of-care challenges for research and practice. Consistent with a recent report from the US Government Accountability Office,41 clinical policymakers have opportunities to improve the quality and safety of the management of adults with behavioral and psychological symptoms of dementia in all treatment settings. Although geriatric psychiatrists may be best suited to manage these symptoms in older adults, there is a national shortage of geriatric psychiatrists.42 Within nursing homes, staff training and support interventions focused on behavioral management alternatives to drug treatment may lower antipsychotic use in patients with dementia without worsening behavioral symptoms.43 Within primary care, collaborative care models have demonstrated significant improvement in behavioral and psychological symptoms of dementia without increasing antipsychotic use.44 As the US elderly population increases, the number of adults with dementia will grow and the quality of their behavioral health management will become an increasingly important public health priority.
Submitted: February 5, 2015; accepted April 13, 2015.
Drug names: aripiprazole (Abilify and others), haloperidol (Haldol and others), olanzapine (Zyprexa and others), pimozide (Orap), quetiapine (Seroquel and others), risperidone (Risperdal and others), ziprasidone (Geodon and others).
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Financial disclosure: Drs Olfson, King, and Schoenbaum have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: This research was funded by contracts from the National Institutes of Health to Yale University (Dr King) and Columbia University (Dr Olfson). Dr Olfson is also supported by the New York State Psychiatric Institute.
Role of the sponsor: The sponsors had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; and preparation, review, or approval of the manuscript.
Disclaimer: This article does not necessarily reflect the views of the National Institute of Mental Health, the National Institutes of Health, or the US Federal Government.
Additional information: The IMS database is available for purchase from IMS. Readers can register to receive information about purchasing the IMS databases at https://websolutions.imshealth.com/EB2/User/Validate_UserID.aspx?TARGET=$SM$http://customerportal.imshealth.com/portal/site/imsportal. Information on how to access the MEPS database can be found at http://meps.ahrq.gov/mepsweb/data_stats/download_data_files.jsp.
Supplementary material: Available at PSYCHIATRIST.COM.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
REFERENCES
1. IMS Institute for Healthcare Informatics. The use of medicines in the United States: review of 2011. IMS Health Web site. http://www.imshealth.com/ims/Global/Content/Insights/IMS Institute for Healthcare Informatics/IHII_Medicines_in_U.S_Report_2011.pdf. Updated April 2012. Accessed August 8, 2015.
2. Leucht S, Heres S, Kissling W, et al. Evidence-based pharmacotherapy of schizophrenia. Int J Neuropsychopharmacol. 2011;14(2):269-284. PubMed doi:10.1017/S1461145710001380
3. Pfeifer JC, Kowatch RA, DelBello MP. Pharmacotherapy of bipolar disorder in children and adolescents: recent progress. CNS Drugs. 2010;24(7):575-593. PubMed doi:10.2165/11533110-000000000-00000
4. Pae CU, Forbes A, Patkar AA. Aripiprazole as adjunctive therapy for patients with major depressive disorder: overview and implications of clinical trial data. CNS Drugs. 2011;25(2):109-127. PubMed doi:10.2165/11538980-000000000-00000
5. Alexander GC, Gallagher SA, Mascola A, et al. Increasing off-label use of antipsychotic medications in the United States, 1995-2008. Pharmacoepidemiol Drug Saf. 2011;20(2):177-184. PubMed doi:10.1002/pds.2082
6. Leslie DL, Rosenheck R. Off-label use of antipsychotic medications in Medicaid. Am J Manag Care. 2012;18(3):e109-e117. PubMed
7. Schulze J, Glaeske G, van den Bussche H, et al. Prescribing of antipsychotic drugs in patients with dementia: a comparison with age-matched and sex-matched non-demented controls. Pharmacoepidemiol Drug Saf. 2013;22(12):1308-1316. PubMed doi:10.1002/pds.3527
8. Kleijer BC, van Marum RJ, Egberts AC, et al. Risk of cerebrovascular events in elderly users of antipsychotics. J Psychopharmacol. 2009;23(8):909-914. PubMed doi:10.1177/0269881108093583
9. Rigler SK, Shireman TI, Cook-Wiens GJ, et al. Fracture risk in nursing home residents initiating antipsychotic medications. J Am Geriatr Soc. 2013;61(5):715-722. PubMed doi:10.1111/jgs.12216
10. Hwang YJ, Dixon SN, Reiss JP, et al. Atypical antipsychotic drugs and the risk for acute kidney injury and other adverse outcomes in older adults: a population-based cohort study. Ann Intern Med. 2014;161(4):242-248. PubMed doi:10.7326/M13-2796
11. Schneider LS, Dagerman KS, Insel P. Risk of death with atypical antipsychotic drug treatment for dementia: meta-analysis of randomized placebo-controlled trials. JAMA. 2005;294(15):1934-1943. PubMed doi:10.1001/jama.294.15.1934
12. Kales HC, Zivin K, Kim HM, et al. Trends in antipsychotic use in dementia 1999-2007. Arch Gen Psychiatry. 2011;68(2):190-197. PubMed doi:10.1001/archgenpsychiatry.2010.200
13. Pathak P, West D, Martin BC, et al. Evidence-based use of second-generation antipsychotics in a state Medicaid pediatric population, 2001-2005. Psychiatr Serv. 2010;61(2):123-129. PubMed doi:10.1176/ps.2010.61.2.123
14. Simoni-Wastila L, Ryder PT, Qian J, et al. Association of antipsychotic use with hospital events and mortality among medicare beneficiaries residing in long-term care facilities. Am J Geriatr Psychiatry. 2009;17(5):417-427. PubMed doi:10.1097/JGP.0b013e31819b8936
15. Yang M, Barner JC, Lawson KA, et al. Antipsychotic medication utilization trends among Texas veterans: 1997-2002. Ann Pharmacother. 2008;42(9):1229-1238. PubMed doi:10.1345/aph.1L155
16. Crystal S, Olfson M, Huang C, et al. Broadened use of atypical antipsychotics: safety, effectiveness, and policy challenges. Health Aff. 2009;28(5):w770-w781. doi:10.1377/hlthaff.28.5.w770
17. Gellad WF, Aspinall SL, Handler SM, et al. Use of antipsychotics among older residents in VA nursing homes. Med Care. 2012;50(11):954-960. PubMed doi:10.1097/MLR.0b013e31825fb21d
18. MEPS-HC panel design and data collection process. Agency for Healthcare Research and Quality Web site. http://meps.ahrq.gov/survey_comp/hc_data_collection.jsp. Accessed August 8, 2015.
19. Mirandola M, Andretta M, Corbari L, et al. Prevalence, incidence and persistence of antipsychotic drug prescribing in the Italian general population: retrospective database analysis, 1999-2002. Pharmacoepidemiol Drug Saf. 2006;15(6):412-420. PubMed doi:10.1002/pds.1162
20. Alessi-Severini S, Biscontri RG, Collins DM, et al. Utilization and costs of antipsychotic agents: a Canadian population-based study, 1996-2006. Psychiatr Serv. 2008;59(5):547-553. PubMed
21. Kaye JA, Bradbury BD, Jick H. Changes in antipsychotic drug prescribing by general practitioners in the United Kingdom from 1991 to 2000: a population-based observational study. Br J Clin Pharmacol. 2003;56(5):569-575. PubMed doi:10.1046/j.1365-2125.2003.01905.x
22. Plassman BL, Langa KM, Fisher GG, et al. Prevalence of dementia in the United States: the aging, demographics, and memory study. Neuroepidemiology. 2007;29(1-2):125-132. PubMed doi:10.1159/000109998
23. Byers AL, Yaffe K, Covinsky KE, et al. High occurrence of mood and anxiety disorders among older adults: the National Comorbidity Survey Replication. Arch Gen Psychiatry. 2010;67(5):489-496. PubMed doi:10.1001/archgenpsychiatry.2010.35
24. Young RC, Kiosses D, Heo M, et al. Age and ratings of manic psychopathology. Bipolar Disord. 2007;9(3):301-304. PubMed doi:10.1111/j.1399-5618.2007.00393.x
25. Oostervink F, Boomsma MM, Nolen WA; EMBLEM Advisory Board. Bipolar disorder in the elderly; different effects of age and of age of onset. J Affect Disord. 2009;116(3):176-183. PubMed doi:10.1016/j.jad.2008.11.012
26. Al Jurdi RK, Nguyen QX, Petersen NJ, et al. Acute bipolar I affective episode presentation across life span. J Geriatr Psychiatry Neurol. 2012;25(1):6-14. PubMed doi:10.1177/0891988712436686
27. Hasin DS, Goodwin RD, Stinson FS, et al. Epidemiology of major depressive disorder: results from the National Epidemiologic Survey on Alcoholism and Related Conditions. Arch Gen Psychiatry. 2005;62(10):1097-1106. PubMed doi:10.1001/archpsyc.62.10.1097
28. Weissman MM, Bland RC, Canino GJ, et al. Cross-national epidemiology of major depression and bipolar disorder. JAMA. 1996;276(4):293-299. PubMed doi:10.1001/jama.1996.03540040037030
29. Leclerc E, Mansur RB, Brietzke E. Determinants of adherence to treatment in bipolar disorder: a comprehensive review. J Affect Disord. 2013;149(1-3):247-252. PubMed doi:10.1016/j.jad.2013.01.036
30. Launer LJ, Andersen K, Dewey ME, et al. Rates and risk factors for dementia and Alzheimer’s disease: results from EURODEM pooled analyses. EURODEM Incidence Research Group and Work Groups. European Studies of Dementia. Neurology. 1999;52(1):78-84. PubMed doi:10.1212/WNL.52.1.78
31. Buchanan RW, Kreyenbuhl J, Kelly DL, et al; Schizophrenia Patient Outcomes Research Team (PORT). The 2009 schizophrenia PORT psychopharmacological treatment recommendations and summary statements. Schizophr Bull. 2010;36(1):71-93. PubMed doi:10.1093/schbul/sbp116
32. Vieta E, Valentí M. Pharmacological management of bipolar depression: acute treatment, maintenance, and prophylaxis. CNS Drugs. 2013;27(7):515-529. PubMed doi:10.1007/s40263-013-0073-y
33. Wright BM, Eiland EH 3rd, Lorenz R. Augmentation with atypical antipsychotics for depression: a review of evidence-based support from the medical literature. Pharmacotherapy. 2013;33(3):344-359. PubMed doi:10.1002/phar.1204
34. Gareri P, De Fazio P, Manfredi VG, et al. Use and safety of antipsychotics in behavioral disorders in elderly people with dementia. J Clin Psychopharmacol. 2014;34(1):109-123. PubMed doi:10.1097/JCP.0b013e3182a6096e
35. Ballard C, Hanney ML, Theodoulou M, et al; DART-AD investigators. The dementia antipsychotic withdrawal trial (DART-AD): long-term follow-up of a randomised placebo-controlled trial. Lancet Neurol. 2009;8(2):151-157. PubMed doi:10.1016/S1474-4422(08)70295-3
36. Wang PS, Lane M, Olfson M, et al. Twelve-month use of mental health services in the United States: results from the National Comorbidity Survey Replication. Arch Gen Psychiatry. 2005;62(6):629-640. PubMed doi:10.1001/archpsyc.62.6.629
37. Kales HC, Gitlin LN, Lyketsos CG. Assessment and management of behavioral and psychological symptoms of dementia. BMJ. 2015;350(7):h369. PubMed doi:10.1136/bmj.h369
38. US Food and Drug Administration. Public health advisory: deaths with antipsychotics in elderly patients with behavioral disturbances. http://www.fda.gov/Drugs/DrugSafety/PostmarketDrugSafetyInformationfor
PatientsandProviders/ucm053171.htm. Published April 11, 2005. Accessed August 26, 2015.
39. US Food and Drug Administration. FDA requests boxed warnings on older class of antipsychotic drugs. http://www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/2008/ucm116912.htm. Published June 16, 2008. Accessed August 26, 2015.
40. Dorsey ER, Rabbani A, Gallagher SA, et al. Impact of FDA black box advisory on antipsychotic medication use. Arch Intern Med. 2010;170(1):96-103. PubMed doi:10.1001/archinternmed.2009.456
41. United States Government Accountability Office. Antipsychotic drug use: HHS has initiatives to reduce use among older adults in nursing homes, but should expand efforts to other settings. http://www.gao.gov/assets/670/668221.pdf. Updated January 2015. Accessed August 8, 2015.
42. Abrams RC, Young RC. Crisis in access to care: geriatric psychiatry services unobtainable at any price. Public Health Rep. 2006;121(6):646-649. PubMed
43. Fossey J, Ballard C, Juszczak E, et al. Effect of enhanced psychosocial care on antipsychotic use in nursing home residents with severe dementia: cluster randomised trial. BMJ. 2006;332(7544):756-761. PubMed doi:10.1136/bmj.38782.575868.7C
44. Callahan CM, Boustani MA, Unverzagt FW, et al. Effectiveness of collaborative care for older adults with Alzheimer disease in primary care: a randomized controlled trial. JAMA. 2006;295(18):2148-2157. PubMed doi:10.1001/jama.295.18.2148