How Successful Are Physicians in Eliciting the Truth From Their Patients? A Large-Scale Internet Survey From Patients’ Perspectives

ABSTRACT
Objective: How honestly patients report their symptoms and medication adherence to their physicians has not been adequately addressed in patients with depression. We therefore conducted a large-scale Internet survey in an effort to discover how successful physicians are in eliciting the truth from their patients and also to examine reasons for patients’ truth-concealing behaviors.
Method: 2,354 participants who had received treatment for depression within the past year and had been diagnosed with depression by Patient Health Questionaire were identified from 323,226 registrants at the Macromill database through screening procedures. Participants were asked to complete a questionnaire regarding their treatment for depression with a special focus on patient-physician relationship. This study was conducted from December 7 to 13, 2010, in Japan.
Results: 2,020 participants successfully completed the questionnaire. Overall, 70.2% of responders reported that they had withheld the truth from their physicians. A logistic regression model found significant associations of such a behavior with female sex (95% CI, 1.15-1.74; P = .001), younger age (95% CI, 0.49-0.97; P = .030), and a lower degree of satisfaction in mutual communication (95% CI, 3.17-6.58; P < .001). 69.2% and 52.6% of the participants refrained from telling about their “daily activities” and “symptoms,” respectively. Female participants were more likely to hide the facts concerning “adherence to prescribed medication” and “figures such as body temperature and weight.” 31.9% of participants had discontinued the treatment without consulting their physician, which was again more frequent in females, younger persons, and those who were not satisfied with communication with their physician.
Conclusions: While the findings obtained herein need to be replicated in other patient populations, a majority of patients with depression were reluctant to uncover the truth, which emphasizes the need for more fine-tuned suspicion among physicians about symptoms and medication adherence.
J Clin Psychiatry 2012;73(3):311-317
© Copyright 2012 Physicians Postgraduate Press, Inc.
Submitted: April 18, 2011; accepted August 16, 2011(doi:10.4088/JCP.11m07078).
Corresponding author: Norifusa Sawada, MD, Department of Psychiatry, Oizumi Hospital, 6-9-1 Oizumigauencho, Nerima-ku, Tokyo, 178-0061, Japan ([email protected]).
Depression is a chronic, recurrent, and debilitating illness, and approximately one-half of all patients are reported to relapse within 6 months if they discontinue antidepressant drugs immediately after achieving remission.1 On the other hand, if they continue taking antidepressants, the relapse rate can be lowered to 10%-25%.1,2 However, one of the major obstacles that hamper therapeutic effects in reality is patients’ suboptimal adherence to these drugs. We previously investigated persistence and compliance to antidepressant drugs in 367 patients with major depressive disorder in clinical outpatient settings and found that only 44.3% of patients continued antidepressant treatment for 6 months.3 Moreover, 63.1% of patients who discontinued their initial antidepressant drug did so without consulting their psychiatrists, which clearly indicates a lack of sufficient mutual communication between patients and their psychiatrists. Furthermore, the rate of patients who were compliant to the antidepressant treatment, defined as a medication possession rate of ≥ 0.8, was as low as 55.6%, which also underscores substantial room for improvement toward a successful treatment. Thus, enhancing communication and sharing information between patients and their psychiatrists would be indispensable for providing appropriate treatment for depression.
However, another major obstacle is that patients may have a tendency to conceal the truth from their physicians. To our knowledge, there is only 1 survey that investigated this issue; this cross-sectional survey that was conducted in Japan (N = 1,074) revealed that 28% of patients with a physical illness who visited a general practitioner reported that they had not told the truth to their physicians at least once.4 Furthermore, 24% of these patients did not honestly disclose the truth about their symptoms, and neither did another 24% of patients about adherence to medications. Given that determination of psychiatric diagnoses and assessment of treatment response heavily depend on the subjective information provided by patients, it is critically important to evaluate how truthfully patients report their symptoms and concerns to their psychiatrists. However, this important issue has not been addressed in patients with psychiatric disorders, including depression.
To thoroughly evaluate such patients’ truth-telling behaviors toward physicians, a sufficient number in the sample is desirable. Surveys using the Internet have successfully been conducted for this purpose.5 Furthermore, since anonymous participation is guaranteed and participants are less likely to feel any pressure from physicians or research staff under this particular system, we could extract more practical information that may more precisely mirror the everyday life of patients. Using a large-scale Internet survey from patients’ perspectives, this study addressed how successful psychiatrists are in eliciting the truth from their patients with depression.
METHOD
This Internet-based survey was conducted from December 7 to 13, 2010, in Japan. A total of 2,027 participants were selected through the following steps.
Recruitment Procedures
Selection of participants. A total of 323,226 people had already registered with the Internet Web site monitor system (the Macromill research monitor, http://www.macromill.com/global/index.html) and agreed to participate in health-related surveys on registration. Of these people, 26,007 persons were categorized as panel registrants who had suffered depression. Those registrants were invited to participate in this survey by e-mail. In this e-mail, details of this survey were first described; if participants agreed to participate in this survey and provided informed consent by clicking a corresponding button, a screening survey started. Of the 26,007 registrants, 13,527 persons agreed to participate in this survey, and 2,354 patients were identified that met the following criteria: age 20 to 69 years, having been diagnosed with major depressive disorder by a psychiatrist within the past year, having received treatment for depression within the past year, and having not been diagnosed with bipolar disorder. In addition, participants were requested to complete the 9 items of Patient Health Questionnaire (PHQ-9).6,7 The PHQ is a self-administered questionnaire for determining criterion-based diagnoses of various psychiatric disorders that are common in primary care. In this study, major depression diagnosis was corroborated when 5 or more of the 9 depressive symptoms in the criteria had been present at least “more than half the days” over the last 2 weeks, and 1 of the symptoms was depressed mood or anhedonia. In total, 2,027 participants fulfilled our inclusion criteria.
- Among responders with depression, about 70% reported that they had withheld the truth from their physicians.
- A logistic regression model found significant associations of such behavior with female sex, younger age, and a lower degree of satisfaction in patient-physician communication.
- Female patients were less likely than male patients to disclose the facts concerning “adherence to prescribed medication” and “figures such as body temperature and weight.”
- A good patient-physician alliance is needed to gather relevant information toward successful depression treatment.
Collected information. These 2,027 participants were asked to complete questionnaires. The information collected included sex, age, family structure, occupation, academic background, and annual income. Participants were then asked 39 questions about their experiences when they received treatment for depression, which included communication with their physician with a special focus on whether they had not frankly disclosed the truth (see eAppendix 1, available at PSYCHIATRIST.COM).
Statistical Analyses
Statistical analyses were carried out using SPSS version 18.0 for Windows (IBM, Armonk, New York). Logistic regression analysis was employed to identify predictors of participants’ behavior of not telling the truth to their physician among the following variables: age in decade, sex, physicians’ sex, whether participants thought their physicians were older than they were or not, participants’ satisfaction with communication with their physician (ie, satisfied [very much satisfied or satisfied], not satisfied nor dissatisfied, or dissatisfied [dissatisfied or very much dissatisfied]), highest academic qualification (ie, junior high school, high school, carrier college, 2-year college, or university/graduate school), and income (ie, less than Â¥4 million [equivalent to approximately US $48,780], Â¥4 million and more). We conducted another logistic regression analysis to examine predictors of treatment discontinuation or predictors of antidepressant discontinuation, using the same variables described above. Differences of interest between groups were compared with a χ2 test. A P value of < .05 was considered statistically significant (2-tailed).
The present study was carried out in accordance with the latest version of the Declaration of Helsinki and approved by the Institutional Review Board at Oizumi Hospital, Tokyo, Japan. All participants provided informed consent online after a complete description of the study.
RESULTS
Demographic and Clinical Characteristics of Participants
A total of 2,027 participants completed the questionnaire. Of these, 7 were excluded because they did not follow the instructions. Thus, the data from 2,020 participants were included, and all participants provided necessary data for statistical analyses. Their mean ± SD age was 39.1 ± 8.56 years, and 45.0% (n = 909) were men. More than four-fifths of the participants were currently receiving treatment for depression, and 83.1% of the participants (n = 1,678) reported that their psychiatrist was male.
Factors and Reasons Associated With Participants’ Not Telling the Truth
Overall, 70.2% of responders reported that they had, at least once, not told the truth to their psychiatrists (Table 1). The logistic regression model found significant associations of such a behavior with female sex, younger age, and a lower degree of satisfaction in the communication with their physicians. On the other hand, no effect was found for their income, academic background, physicians’ sex, and physicians’ estimated age.
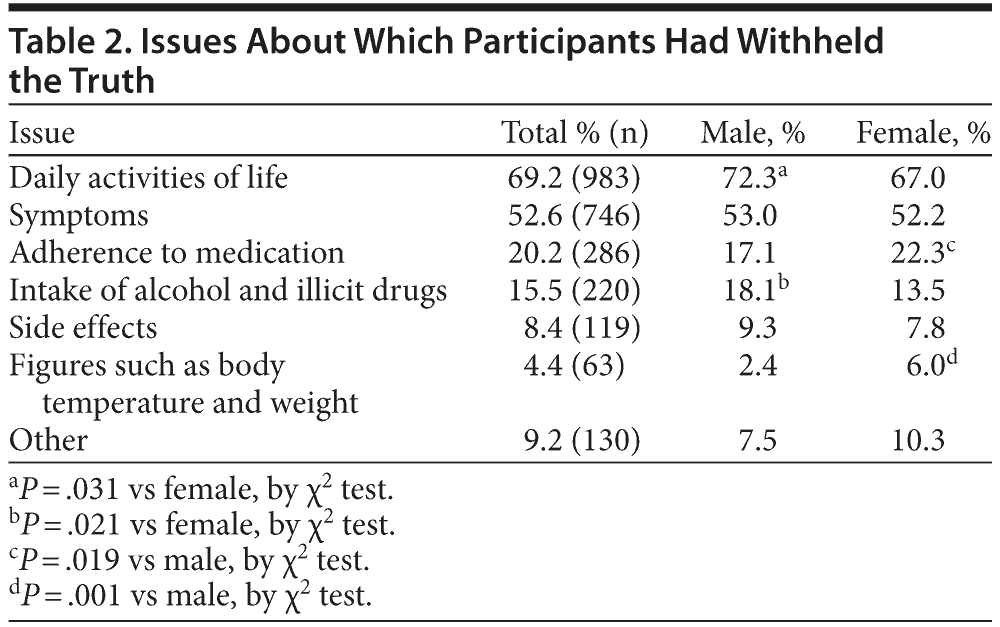
Issues about which participants hid the truth are summarized in Table 2. More than two-thirds of the participants who concealed the truth reported that they did so about their daily activities, and more than half did not accurately report their symptoms on purpose. Male sex was significantly associated with not frankly disclosing the truth about “daily activities” (P = .031) and “intake of alcohol and illicit drugs” (P = .021). In contrast, “adherence to prescribed medication” and “figures such as body temperature and weight” were not honestly reported more frequently in females (P = .019 and P = .001, respectively).
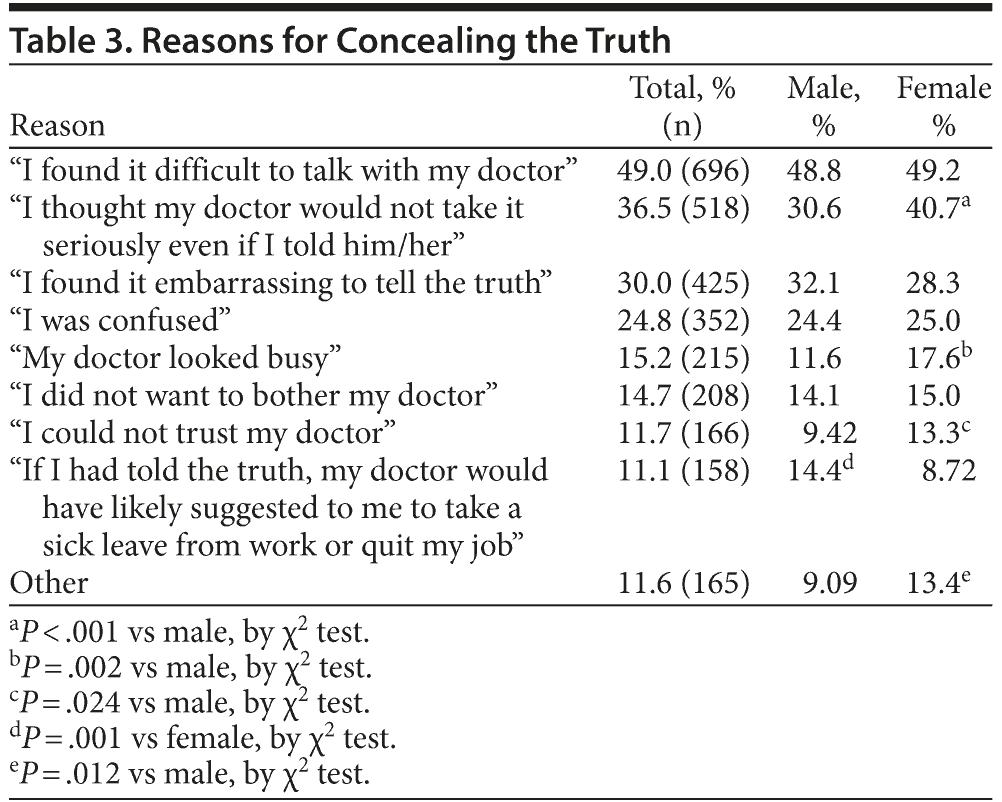
The most frequent reason the participants did not tell the truth was “I found it difficult to talk with my doctor” (49.0%), followed by “I thought my doctor would not take it seriously even if I told him/her” (36.5%) and “I found it embarrassing to tell the truth” (30.0%). Other reasons are summarized in Table 3. Female sex was significantly associated with not frankly disclosing the truth because “I thought my doctor would not take it seriously even if I told him/her” (P < .001), “My doctor looked busy” (P = .002), and “I could not trust my doctor” (P = .024). In contrast, “If I had told the truth, my doctor would have likely suggested to me to take a sick leave from work or quit my job” was the reason for withholding the truth in males (P = .001).
When the participants were asked, “What do you think would make patients feel free to tell the truth to their doctors during the treatment?” the most frequent response was “doctors spend more time with each patient” (68.4%), followed by “providing an environment where patients and doctors can freely discuss issues” (33.5%) and “communication and explanation, using letters or memos” (29.8%).
Frequency of Discontinuing Therapy for Depression
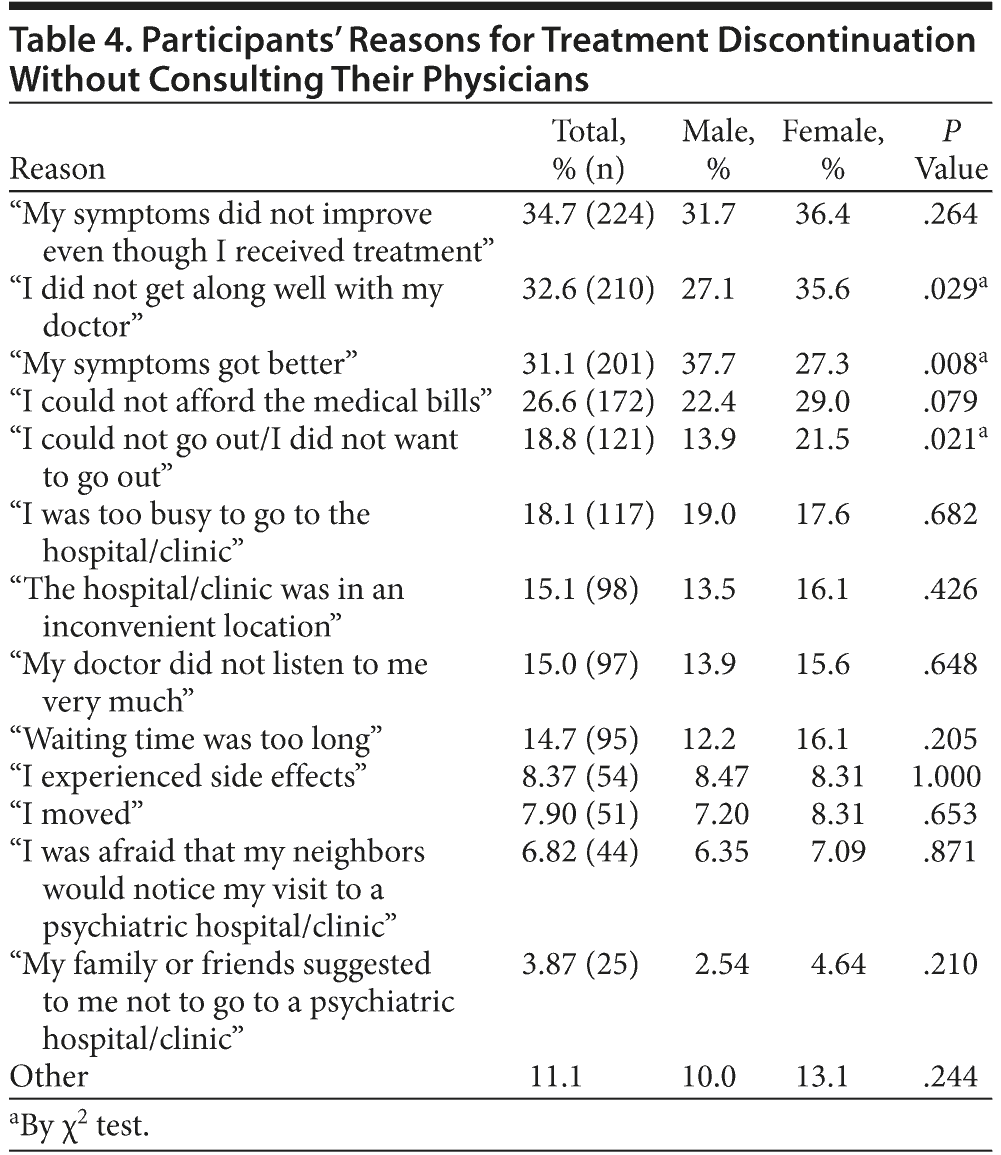
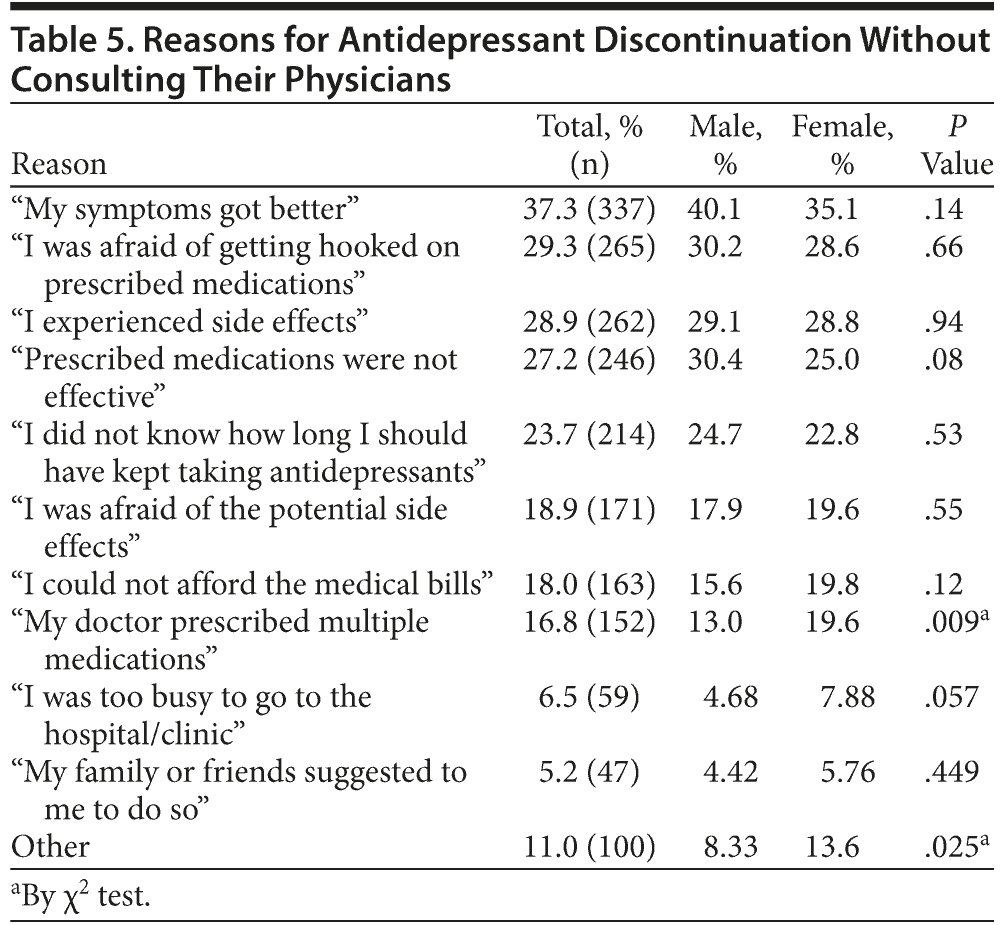
Among 2,020 participants, 31.9% discontinued any form of their treatment for depression, including nondrug therapies such as psychotherapies, without consulting their physicians (Table 1). The logistic regression model found significant associations for such a behavior with female sex, younger age, and a lower degree of satisfaction in the communication with their physicians, while no effect was found in their income or academic background. Participants’ frequently endorsed reasons for discontinuing treatment without consulting their physicians are shown in Table 4. Among the total sample, 44.7% quit taking antidepressant drugs without consulting their physicians (Table 1). The logistic regression model found significant associations for such a behavior with physicians’ estimated age and a lower degree of satisfaction with the communication with their physicians, while no effect was found for their sex, age, income, academic background, or physicians’ sex. Frequent reasons for such a discontinuation are shown in Table 5.
Patients’ Need for the Treatment of Depression
When the participants were asked for factors that could influence their subjective preference of antidepressants, they gave the highest priority to good balance between efficacy and tolerability (48.2%), followed by strong efficacy (19.5%), fewer side effects (15.7%), rapid onset of action (7.4%), and low cost (2.3%).
DISCUSSION
Using a large-scale Internet survey from patients’ perspectives, this study addressed how successful physicians are in eliciting the truth from their patients with depression. To our knowledge, this is the first study to investigate this question. The results are somewhat disappointing in that the rate of patients with depression who had not told the truth was as high as 70.2%, and withholding disclosure was found to be influenced by female sex, younger age, and a lower degree of satisfaction in mutual communication with their physicians.
Approximately two-thirds of the participants with depression had hidden the truth from their psychiatrists; this rate was much higher than that found in patients with physical illness (28%).4 In addition, while the most frequent issues about which patients with physical illness did not tell the truth were “symptoms” (24%) and “adherence to medication” (24%),4 the most frequent issue in patients with depression was “daily activities of life” (69.2%), which is of a high clinical relevance as well as a significant concern for the treatment of depression. Depression is not only characterized by psychopathological depressive symptoms but also accompanied by consequences derived from those symptoms, such as impaired daily social functioning.8 In this context, a possible discrepancy between subjectively reported versus objectively evaluated daily activities and functioning needs to be carefully ascertained.
The results showed that female participants tended to conceal the truth more frequently, and they did so especially about “adherence to prescribed medications” and “figures such as body temperature and weight.” This sex difference is consistent with the finding in patients with physical illness in the literature.4 Although potential mechanisms underlying the sex differences remain unclear, this aspect should be taken into account in an adherence evaluation that frequently relies upon subjective confession. Among the participants, 83.1% reported that their psychiatrist was male; this rate is comparable to those of male physicians in Japan (81.9%)9 and the United States (82.2%).10
We also found that older participants were more likely to tell the truth and were less likely to discontinue their treatment; this finding is consistent with the literature.3,11 For example, Harman et al12 reported that younger patients with depression were less likely to receive any treatment, less likely to fill an adequate number of prescriptions, and less likely to receive an adequate number of counseling sessions. Minamisawa et al13 also found that being younger in patients with psychiatric illness was associated with a lower degree of trust toward their psychiatrists. These findings collectively suggest that younger patients may be less likely to establish a good therapeutic relationship with their psychiatrists. More than two-thirds of the participants in the present study thought that they would feel ready to tell the truth to their physicians if their doctors spent more time with them. However, the actual impact of the time spent with each patient has not been systematically investigated in this study, leaving a question as to how much time spent with a patient is optimal.
Another pertinent finding is that one-third of the participants had discontinued their treatment without consulting their physicians, and the most frequently endorsed reason for doing so was “my symptoms did not improve even though I received treatment.” This finding argues for the fact that currently available antidepressants do not necessarily meet the need of many patients with depression. In fact, the STAR*D study14 demonstrated that only 28% of depressed patients achieved remission with a first-line selective serotonin reuptake inhibitor. Pigott et al15 reanalyzed the data from STAR*D and found that the results of STAR*D may be even worse than previously appreciated. Furthermore, as Fournier et al16 claimed, the magnitude of benefit of antidepressant medication compared with a placebo may be minimal or nonexistent in patients with mild or moderate symptoms. The second most common reason participants gave for discontinuing their treatment was “I did not get along well with my doctor,” plausibly suggesting that a better therapeutic alliance should be targeted, which in turn would be expected to enhance treatment adherence and outcomes.
Approximately half the participants discontinued their antidepressant drugs without consulting their physicians, and the most common reason for doing so was “my symptoms got better.” This sounds reasonable but actually represents a major clinical concern in light of established therapeutic effects of antidepressant drugs for the maintenance phase.1,2,17 Bull et al18 reported that, whereas 72% of physicians said they usually tell patients to continue using antidepressants for at least 6 months, only 34% of patients reported being told so. Furthermore, more than half of patients reported not being told about the expected duration of antidepressant treatment needed. The second and third most frequent reasons were “I was afraid of getting hooked on prescribed medications” and “I experienced side effects,” respectively, which is consistent with the findings by Melartin et al,19 who found that premature discontinuation of an antidepressant treatment was associated with a fear of dependence or side effects of antidepressants. Goethe et al20 reported that experiencing side effects could double the risk of treatment discontinuation. Previous studies have demonstrated that sufficiently discussing potential side effects could result in a greater degree of adherence to medications.18 Therefore, physicians should be encouraged to discuss side effects of medications to reduce unwanted discontinuation of the treatment.
A lower degree of satisfaction in communication with physicians was found to be significantly associated with not disclosing the truth. Moreover, participants who were not satisfied with communication with their doctors were also found to be more likely to discontinue their antidepressant treatment. Effective physician-patient communication can increase the likelihood of a favorable health outcome,21 and encouraging patients to take an active role in their health care can lead to treatment success.22 To achieve this, introducing shared decision-making may improve communication between patients with depression and physicians as well as patients’ satisfaction.17,23 Moreover, such active participation in the treatment process can also improve treatment adherence and clinical outcome.24
There are several limitations in the present study. First, although we systematically used the PHQ-9 as a validated diagnostic tool for depression, the diagnosis was solely based on participants’ self-report, which could be associated with either overdiagnosis or underdiagnosis. Second, we were not able to detect the frequency and duration (ie, stability or consistency) of participants’ behavior of withholding the truth as well as depression severity. Moreover, the frequency of visits would have varied across patients, but this was not investigated herein. Furthermore, adherence and other issues as a function of frequency of visits to the psychiatrists should be carefully considered.25 Third, female participants in our study were less likely to tell the truth than males. Another possibility here is that they might be more likely to acknowledge their dishonesty than males. Fourth, differences in cultural background could affect doctor-patient relationships. More than 99% of Japanese citizens are from a single ethnic group and communicate in Japanese, which may, in part, limit the extrapolation of our results to societies with multiethnic cultures and emphasizes the need for further investigations in other cultural settings. Fifth, the participants who agreed to participate in this type of study may be more cooperative than the general patient population, and our findings may therefore overestimate a proportion of people who communicate well with their physician to some extent. Furthermore, limiting the participants to those who had an Internet access would have rendered our study sample relatively younger.26 Indeed, the mean age of the study participants was younger than the Japanese population by about 4 years (39.1 vs 43.3 years). Rather, despite this potential selection bias, it is surprising to find that more than 70% of the participants withheld the truth, and this type of survey will add to a clinical challenge of eliciting issues in patients. Sixth, the severity of illness, actual antidepressant in use, and side effects, which were not systematically evaluated in the present study, could have confounded the results. Finally, and most importantly, cross-sectional surveys cannot address long-term treatment outcomes, and only fixed responses were available to participants. These limitations are inevitably associated with Internet surveys and therefore have to be carefully acknowledged.
CONCLUSION
The fact that more than 70% of patients with depression do not disclose the truth to their physicians emphasizes the need for clinical suspicion as well as more objective assessment of their symptoms and medication adherence. Furthermore, when communication between patients and their physician is suboptimal, patients’ status and behavior should be monitored with more objective vigilance in an effort to avoid undesirable premature withdrawal from antidepressants. This also underscores the critical importance of a good patient-physician alliance to gather relevant information toward a successful treatment.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Author affiliations: Department of Psychiatry, Oizumi Hospital, Tokyo (Dr Sawada); Department of Neuropsychiatry, Keio University School of Medicine, Tokyo (all authors), Japan; Geriatric Mental Health Program, Centre for Addiction and Mental Health, Toronto, Ontario, Canada (Dr Uchida); Division of Molecular Imaging and Neuropathology, Columbia University, New York, New York (Dr Kikuchi); and Department of Psychiatry, Inokashira Hospital, Tokyo, Japan (Dr Suzuki).
Financial disclosure: Dr Sawada has received speaker’s honoraria or manuscript fees from Pfizer, Otsuka, Dainippon Sumitomo, and Janssen within the past 2 years. Dr Uchida has received grants, speaker’s honoraria, or manuscript fees from the Pfizer Health Research Foundation, GlaxoSmithKline, Otsuka, Dainippon Sumitomo, Janssen, and Pfizer within the past 2 years. Dr Watanabe has received grants or consultant fees from Dainippon Sumitomo, Eli Lilly, GlaxoSmithKline, Janssen, and Pfizer and received speaker’s honoraria from Astellas, Dainippon Sumitomo, Eli Lilly, GlaxoSmithKline, Janssen, Meiji, Otsuka, Pfizer, and Yoshitomiyakuhin within the past 2 years. Dr Kikuchi has received a research grant from GlaxoSmithKline within the past 2 years. Dr Suzuki has received fellowship grants from the Japanese Society of Clinical Neuropsychopharmacology, the Government of Canada Post-Doctoral Research Fellowships, Kanae Foundation, and Mochida Memorial Foundation and received manuscript fees from Kyowa Hakko Kirin and Dainippon Sumitomo within the past 2 years. Drs Kashima and Mimura have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: Funding for this study was provided by Pfizer.
Disclaimer: Pfizer had no further role in study design; in the collection, analysis, and interpretation of data; in the writing of the report; and in the decision to submit the paper for publication.
Previous presentation: Some of these data were presented at the 24th Congress of the European College of Neuropsychopharmacology; September 3-7, 2011; Paris, France.
Supplementary material: eAppendix 1 is available at PSYCHIATRIST.COM.
REFERENCES
1. American Psychiatric Association. Practice Guideline for the Treatment of Patients With Major Depressive Disorder (revision). American Psychiatric Association. Am J Psychiatry. 2000;157(suppl):1-45. PubMed
2. Geddes JR, Carney SM, Davies C, et al. Relapse prevention with antidepressant drug treatment in depressive disorders: a systematic review. Lancet. 2003;361(9358):653-661. PubMed doi:10.1016/S0140-6736(03)12599-8
3. Sawada N, Uchida H, Suzuki T, et al. Persistence and compliance to antidepressant treatment in patients with depression: a chart review. BMC Psychiatry. 2009;9:38. PubMed doi:10.1186/1471-244X-9-38
4. QLife I. Do patients tell lies? [published online] http://www.qlife.jp/square/pdf/square_anq_20100331.pdf (in Japanese). Updated March 31, 2010. Accessed April 18, 2011.
5. Kikuchi T, Uchida H, Suzuki T, et al. Patients’ attitudes toward side effects of antidepressants: an Internet survey. Eur Arch Psychiatry Clin Neurosci. 2011;261(2):103-109. PubMed doi:10.1007/s00406-010-0124-z
6. Spitzer RL, Kroenke K, Williams JB. Validation and utility of a self-report version of PRIME-MD: the PHQ primary care study. Primary Care Evaluation of Mental Disorders. Patient Health Questionnaire. JAMA. 1999;282(18):1737-1744. PubMed doi:10.1001/jama.282.18.1737
7. Muramatsu K, Miyaoka H, Kamijima K, et al. The Patient Health Questionnaire, Japanese version: validity according to the Mini-International Neuropsychiatric Interview-plus. Psychol Rep. 2007;101(3, Pt 1):952-960. PubMed
8. Hirschfeld RM, Montgomery SA, Keller MB, et al. Social functioning in depression: a review. J Clin Psychiatry. 2000;61(4):268-275. PubMed doi:10.4088/JCP.v61n0405
9. Numbers of doctors in medical site in Japan, 2008 Edition. Ministry of Health, Labor, and Welfare Web site. http://www.mhlw.go.jp/toukei/saikin/hw/ishi/08/dl/gaikyo1.pdf (in Japanese). Accessed August 3, 2011.
10. Minority Affairs Section. Physician Statistics. American Medical Association Web site. http://www.ama-assn.org/ama/pub/about-ama/our-people/member-groups-sections/minority-affairs-consortium/physician-statistics.page Accessed August 3, 2011.
11. Warden D, Rush AJ, Wisniewski SR, et al. What predicts attrition in second step medication treatments for depression? a STAR*D Report. Int J Neuropsychopharmacol. 2009;12(4):459-473. PubMed doi:10.1017/S1461145708009073
12. Harman JS, Edlund MJ, Fortney JC. Disparities in the adequacy of depression treatment in the United States. Psychiatr Serv. 2004;55(12):1379-1385. PubMed doi:10.1176/appi.ps.55.12.1379
13. Minamisawa A, Suzuki T, Watanabe K, et al. Patient’s trust in their psychiatrist: a cross-sectional survey. [published online ahead of print March 3, 2011]. Eur Arch Psychiatry Clin Neurosci. 2011;261(8):603-608. doi:10.1007/s00406-011-0199-1 PubMed.
14. Trivedi MH, Rush AJ, Wisniewski SR, et al; STAR*D Study Team. Evaluation of outcomes with citalopram for depression using measurement-based care in STAR*D: implications for clinical practice. Am J Psychiatry. 2006;163(1):28-40. PubMed doi:10.1176/appi.ajp.163.1.28
15. Pigott HE, Leventhal AM, Alter GS, et al. Efficacy and effectiveness of antidepressants: current status of research. Psychother Psychosom. 2010;79(5):267-279. PubMed doi:10.1159/000318293
16. Fournier JC, DeRubeis RJ, Hollon SD, et al. Antidepressant drug effects and depression severity: a patient-level meta-analysis. JAMA.2010;303(1):47-53. PubMed
17. Simon D, Loh A, Wills CE, et al. Depressed patients’ perceptions of depression treatment decision-making. Health Expect. 2007;10(1):62-74. PubMed doi:10.1111/j.1369-7625.2006.00424.x
18. Bull SA, Hu XH, Hunkeler EM, et al. Discontinuation of use and switching of antidepressants: influence of patient-physician communication. JAMA. 2002;288(11):1403-1409. PubMed doi:10.1001/jama.288.11.1403
19. Melartin TK, Rytsפlפ HJ, Leskelפ US, et al. Continuity is the main challenge in treating major depressive disorder in psychiatric care. J Clin Psychiatry. 2005;66(2):220-227. PubMed doi:10.4088/JCP.v66n0210
20. Goethe JW, Woolley SB, Cardoni AA, et al. Selective serotonin reuptake inhibitor discontinuation: side effects and other factors that influence medication adherence. J Clin Psychopharmacol. 2007;27(5):451-458. PubMed doi:10.1097/jcp.0b013e31815152a5
21. Stewart MA. Effective physician-patient communication and health outcomes: a review. CMAJ. 1995;152(9):1423-1433. PubMed
22. Speedling EJ, Rose DN. Building an effective doctor-patient relationship: from patient satisfaction to patient participation. Soc Sci Med. 1985;21(2):115-120. PubMed doi:10.1016/0277-9536(85)90079-6
23. Loh A, Simon D, Wills CE, et al. The effects of a shared decision-making intervention in primary care of depression: a cluster-randomized controlled trial. Patient Educ Couns. 2007;67(3):324-332. PubMed doi:10.1016/j.pec.2007.03.023
24. Loh A, Leonhart R, Wills CE, et al. The impact of patient participation on adherence and clinical outcome in primary care of depression. Patient Educ Couns. 2007;65(1):69-78. PubMed doi:10.1016/j.pec.2006.05.007
25. Mitchell AJ, Selmes T. Why don’ t patients take their medicine? reasons and solution in psychiatry. Adv Psychiatr Treat. 2007;13(5):336-346. doi:10.1192/apt.bp.106.003194
26. Rhodes SD, Bowie DA, Hergenrather KC. Collecting behavioural data using the World Wide Web: considerations for researchers. J Epidemiol Community Health. 2003;57(1):68-73. PubMed doi:10.1136/jech.57.1.68