Objective: This large-scale population-based prospective study examined the association between depressive symptoms and cognitive performance at baseline with later functioning in middle-aged adults.
Methods: The Center for Epidemiologic Studies Depression Scale, the Digit Symbol Substitution Test (DSST), the Trail Making Test B (TMT-B), and the Semantic Verbal Fluency test (SVF) were completed at baseline by 7,426 participants aged ≥ 45 years from February 2012 to December 2013. Role limitations and social functioning were later assessed with the second version of the 12-Item Short Form Health Survey. The association between depressive symptoms and cognitive performance at baseline with functioning at follow-up was examined using general linear models and mediation analyses including sex, age, education, alcohol intake, and cannabis use as covariates.
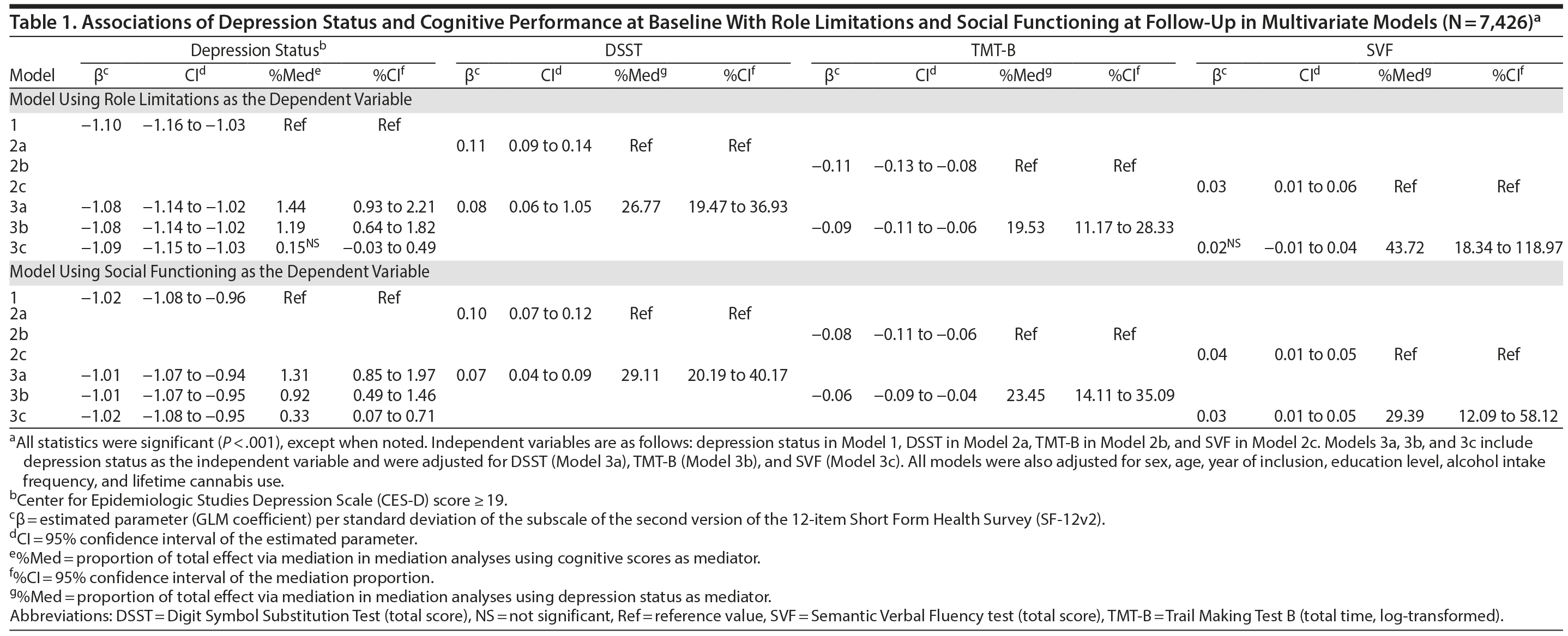
Results: Altered functioning at follow-up was predicted by depressive symptoms (β per standard deviation [95% confidence intervals]: −1.10 [−1.16 to −1.03] and −1.02 [−1.08, −0.96] for role limitations and social functioning, respectively) and DSST, TMT-B, and SVF performance (for role limitations: 0.11 [0.09 to 0.14], −0.11 [−0.13 to −0.08], and 0.03 [0.01 to 0.06], respectively; for social functioning: 0.10 [0.07 to 0.12], −0.08 [−0.11 to −0.06], and 0.04 [0.01 to 0.05], respectively) at baseline. Depressive symptoms were associated with poorer cognitive performance at baseline (−0.19 [−0.25 to −0.13], 0.15 [0.08 to 0.21], and −0.11 [−0.17 to −0.04], respectively). Cognitive performance accounted for only 0.3%-1.4% of the relationship between depressive symptoms and functioning. In contrast, depressive symptoms accounted for 19.5%-43.7% of the association between cognitive performance and functioning.
Conclusions: In middle-aged adults from the general population, cognitive impairment is unlikely to substantially explain the association between depressive symptoms and later role limitations and social functioning.
This work may not be copied, distributed, displayed, published, reproduced, transmitted, modified, posted, sold, licensed, or used for commercial purposes. By downloading this file, you are agreeing to the publisher’s Terms & Conditions.

Depression, Cognitive Functions, and Impaired Functioning in Middle-Aged Adults From the CONSTANCES Cohort

ABSTRACT
Objective: This large-scale population-based prospective study examined the association between depressive symptoms and cognitive performance at baseline with later functioning in middle-aged adults.
Methods: The Center for Epidemiologic Studies Depression Scale, the Digit Symbol Substitution Test (DSST), the Trail Making Test B (TMT-B), and the Semantic Verbal Fluency test (SVF) were completed at baseline by 7,426 participants aged ≥ 45 years from February 2012 to December 2013. Role limitations and social functioning were later assessed with the second version of the 12-Item Short Form Health Survey. The association between depressive symptoms and cognitive performance at baseline with functioning at follow-up was examined using general linear models and mediation analyses including sex, age, education, alcohol intake, and cannabis use as covariates.
Results: Altered functioning at follow-up was predicted by depressive symptoms (β per standard deviation [95% confidence intervals]: −1.10 [−1.16 to −1.03] and −1.02 [−1.08, −0.96] for role limitations and social functioning, respectively) and DSST, TMT-B, and SVF performance (for role limitations: 0.11 [0.09 to 0.14], −0.11 [−0.13 to −0.08], and 0.03 [0.01 to 0.06], respectively; for social functioning: 0.10 [0.07 to 0.12], −0.08 [−0.11 to −0.06], and 0.04 [0.01 to 0.05], respectively) at baseline. Depressive symptoms were associated with poorer cognitive performance at baseline (−0.19 [−0.25 to −0.13], 0.15 [0.08 to 0.21], and −0.11 [−0.17 to −0.04], respectively). Cognitive performance accounted for only 0.3%-1.4% of the relationship between depressive symptoms and functioning. In contrast, depressive symptoms accounted for 19.5%-43.7% of the association between cognitive performance and functioning.
Conclusions: In middle-aged adults from the general population, cognitive impairment is unlikely to substantially explain the association between depressive symptoms and later role limitations and social functioning.
J Clin Psychiatry 2018;79(6):17m12003
To cite: Vulser H, Wiernik E, Hoertel N, et al. Depression, cognitive functions, and impaired functioning in middle-aged adults from the CONSTANCES cohort. J Clin Psychiatry. 2018;79(6):17m12003.
To share: https://doi.org/10.4088/JCP.17m12003
© Copyright 2018 Physicians Postgraduate Press, Inc.
aParis Descartes University, Sorbonne Paris Cité, Faculty of Medicine, Paris, France
bAP-HP, West Paris University Hospitals, Department of Psychiatry, Paris, France
cINSERM, Population-based Epidemiological Cohorts Unit, UMS 011, Villejuif, France
dINSERM U894, Psychiatry and Neurosciences Center, Paris, France
eINSERM, UMR_S 1136, Pierre Louis Institute of Epidemiology and Public Health, Department of Social Epidemiology, Paris, France
fSorbonne Universités, UPMC Univ Paris 06, UMR-S 1136, Pierre Louis Institute of Epidemiology and Public Health, Department of Social Epidemiology, F-75013 Paris, France
gINSERM, U1061, Neuropsychiatry: Epidemiological and Clinical Research, Montpellier, France
hMontpellier University Hospital, Montpellier University, Montpellier, France
iAP-HP, Pitié-Salpêtriרre Hospital, Department of Psychiatry, Paris, France
jINSERM U 1127, CNRS UMR 7225, Sorbonne Universités, UPMC Univ Paris 06, UMR S 1127, Institut du Cerveau et de la Moelle, ICM, Social and Affective Neuroscience (SAN) Laboratory, Paris, France
*Corresponding author: Hélרne Vulser, MD, PhD, Unité de Psychologie et Psychiatrie de liaison et d’ urgence, H×´pital Européen Georges Pompidou, 20 rue Leblanc, 75908 Paris Cedex 15, France ([email protected]).
Depression affects 350 million people worldwide and is a major contributor to the overall global burden of disease.1 Depression is strongly associated with functional impairment,2 which has been found to be comparable to or worse than that associated with several major chronic medical conditions (eg, diabetes, arthritis, angina).3 Impaired subjective performance has been reported in widespread domains of functioning, such as household; work; relationships with partners, family members, and friends; and leisure activities.4,5 These impairments in functioning are strongly associated with the severity of depressive symptoms6,7 and reduced quality of life.8 In addition, depression may contribute to objective social damage, such as work absenteeism, presenteeism, and unemployment.7,9 Several studies have reported a significant positive effect of antidepressant treatments on quality of life and on social and work functioning,10 although residual functional impairment is frequent in patients who achieved remission.11 However, the mechanisms underlying the association between depression and functioning remain largely unknown. In recent decades, it has been suggested that cognitive dysfunctions associated with depression might mediate its impact on functioning.12,13 Indeed, a broad range of cognitive domains may be affected in depressed patients, such as information processing speed, verbal fluency, working memory, attentional control, and cognitive inhibition.14,15 Such cognitive impairments, which all relate to some extent to executive function, have even been found in patients during their first depressive episode.16,17 While cognitive function may improve after pharmacologic treatment of depression,18,19 deficits can still be detected in euthymic patients,20,21 which might explain persistent functional impairment in remission.
Several studies have reported an association between objectively assessed cognitive dysfunction and functional impairment in patients with depression.12,13 For example, Jaeger et al22 reported that several cognitive measures were associated with disability 6 months following hospitalization for a major depressive episode in 48 patients; in addition, 6-month cognitive performance was strongly associated with self-reported functioning after adjusting for residual depression. In 21 adults treated for depression, Naismith et al23 found a moderate relationship between objectively measured psychomotor speed and physical disability, even after adjusting for depression severity. In 52 inpatients with depression, Withall et al24 found that poor event-based prospective memory and more perseverative errors on the shortened Wisconsin Card Sorting Test at admission predicted worse social and occupational outcomes at a 3-month follow-up. Considering occupational status, Baune et al25 reported that, among 70 patients with depression, those who were unemployed had poorer results on neuropsychological tests than those who were employed. Finally, in 483 currently non-depressed patients with major depressive disorder receiving selective serotonin reuptake inhibitors, improvements in cognitive performance were found to predict improvements in functioning.26
Overall, these studies are consistent with the hypothesis that cognitive impairment may account for a substantial part of functional limitation in patients with depression. However, in contrast with more severe mental disorders such as schizophrenia or bipolar disorder,27 the evidence supporting this hypothesis remains weak. Most of the aforementioned studies were based on relatively small, highly selected samples; few had a longitudinal design; and none performed formal mediation analyses.12,28,29 In a cross-sectional survey including 21,425 adults from 6 European countries, Buist-Bouwman et al30 reported that more than 25% of the association of depression with role functioning was directly attributable to self-reported cognitive complaints (ie, concentration, attention, and memory problems). However, that large-scale study did not use objective measures of cognitive function or have a longitudinal design. Besides, due to its associations with both impaired cognition and altered functioning, depression is a plausible confounding factor that may partly explain the association between cognitive and functional impairment.
In this study, we used data from CONSTANCES, a French large-scale population-based study, to investigate the prospective associations between depressive symptoms and cognitive functions with later functioning in middle-aged adults.
METHODS
Participants
All participants were recruited from the CONSTANCES cohort (www.constances.fr). This project aims at providing a general prospective cohort of a large sample of the French population aged 18-69 years.31,32 Participants were recruited since 2012 among people affiliated to the main national health insurance provider, which covers more than 85% of the French population. The cohort was designed to be representative of the target population according to age, sex, employment status, and occupational class. A random sample from the target population was invited by mail to join the cohort. Those who agreed had to fill out self-administrated questionnaires dealing with lifestyle, health, physical limitations, and social and personal characteristics. They were invited to go to one of the 21 participating Health Screening Centers throughout France to benefit from an extensive health examination (medical and paraclinical examinations, blood tests). In addition, cognitive tests were performed for those aged 45 years or older. A follow-up self-administered questionnaire was then completed annually by the participants at home, using either paper or web-based questionnaires.

- Depression is associated with both cognitive and functional impairment.
- In middle-aged adults from the general population with depressive symptoms, cognitive impairment is unlikely to substantially explain altered functioning.
- Interventions aimed at reducing the functional impairment associated with depression should primarily target depressive symptoms themselves; such interventions are likely to improve cognitive functioning at the same time.
In the present study, we used data from the participants aged 45 years or older included from February 21, 2012, to December 31, 2013. Eligibility criteria were being able to fill out the study questionnaires, ability to speak French, and having no missing data for selected variables, including assessment of functioning at follow-up in 2014 (Supplementary Figure 1).
All confidentiality, safety, and security procedures were approved by the French legal authorities. In accordance with French regulations, the CONSTANCES cohort project obtained the authorization of the National Data Protection Authority (Commission Nationale de l’ Informatique et des Libertés). Written informed consent was obtained from all participants.
Assessment of Depressive Symptoms at Baseline
Depressive symptoms were measured at baseline with the French version of the Center for Epidemiologic Studies Depression Scale (CES-D).33,34 The total score ranged from 0 (no depressive symptom) to 60. We used a cutoff score of 19 (CES-D score ≥ 19 versus < 19) to define depression status34 (Appendix 1).
Assessment of Cognitive Functions at Baseline
Cognitive functions were assessed at baseline using objective neuropsychological tests for which impaired performance has been previously reported in patients with major depression15: Digit Symbol Substitution Test (DSST),35 Trail Making Test part B (TMT-B),36 and Semantic Verbal Fluency test (SVF)37 (Appendix 1). TMT-B score was log transformed to achieve a close-to-normal distribution. All of these tests engage executive function to some extent.
Assessment of Functioning at Follow-Up
The second version of the Short-Form-12 Health Survey (SF-12v2)38-40 was part of the annual follow-up questionnaire sent in 2014 to all participants (Appendix 1). Mean (SD) duration between baseline assessments and reception of the 2014 follow-up questionnaire was 497 (157) days. Because we were interested in functional impairment associated with depression specifically, we decided a priori to use 2 subscales as primary outcomes, as Spijker et al41 did: role limitations due to emotional problems, henceforth referred to as “role limitations” (score range, 2-10), and social functioning (score range, 1-5). For both scales, a higher score corresponds with better functioning.
Other Covariates
Other covariates included age at baseline, sex, year of inclusion, education level (no diploma, lower secondary education, professional education, upper secondary education, bachelor, fourth-year university level, master’s degree or higher, other), alcohol intake frequency (never, once or less than once in a month, 2 or 3 times in a month, once or more in a week), and lifetime cannabis use. Education level, alcohol intake frequency, and lifetime cannabis use were assessed at baseline.
Statistical Analysis
Cognitive and functioning scores were z-transformed. The relationships between variables were assessed within the framework of generalized linear models (GLMs) using R software (http://cran.r-project.org, version 3.3.1). First, analyses were conducted including role limitations and social functioning at follow-up as the dependent variables and depression status at baseline as the independent variable. Sex, age, year of inclusion, education level, alcohol intake frequency, and lifetime cannabis use at baseline were entered as covariates. The association between depression status (as a binary variable) and each cognitive score at baseline was also assessed. Then, each of the 3 cognitive scores (DSST, TMT-B, SVF) was entered as the independent variable instead of depression status in 3 separate models. Finally, both depression status and cognitive scores were entered in the 3 separate models. GLM coefficients were presented per standard deviation of the SF-12v2 subscale.
To examine whether changes in regression coefficients across the aforementioned models were statistically significant, formal mediation analyses were conducted with functioning scores as the dependent variable based on algorithms devised by Imai et al.42 Sex, age, year of inclusion, education level, alcohol intake frequency, and lifetime cannabis use at baseline were entered as covariates. First, depression status at baseline was considered as the independent variable, and cognitive scores at baseline (DSST, TMT-B, and SVF separately) as the “mediator” variables between depression status at baseline and functioning at follow-up. Then, each cognitive score was entered as the independent variable with depression status at baseline as the “mediator” variable between each cognitive score at baseline and functioning at follow-up. These mediation models were fit with GLM, and output objects were bootstrapped 500 times with replacement using a parametric mediational analysis. In mediation analysis, a significant mediating effect is defined by a 95% confidence interval (CI) of the regression coefficient that does not include zero.42
To examine the robustness of our findings, we also carried out sensitivity analyses. We performed similar analyses (1) using CES-D as a continuous score, taking the interval between the 25th and the 75th percentile as the unit to provide clinically meaningful regression coefficients; and (2) using a more restricted definition for depression requiring both CES-D score ≥ 19 and self-reported limitation at inclusion. Self-reported limitation at inclusion was defined as having answered “yes” to “Have you been limited, for at least 6 months, in your routine activities by a health problem?” and then having answered “depressive state” to “If yes, for what reasons?”
RESULTS
The final study population consisted of 7,426 participants (3,551 men, 47.82%) with a mean (SD) age of 57.79 (7.20) years. Study population selection is described in Supplementary Figure 1. The mean (SD) CES-D score was 9.88 (8.35) (range, 0-53); 13.24% of participants (n = 983) were depressed at baseline (CES-D score ≥ 19) (Supplementary Table 1). Characteristics of participants lost to follow-up and comparisons with the study population are displayed in Supplementary Table 2.
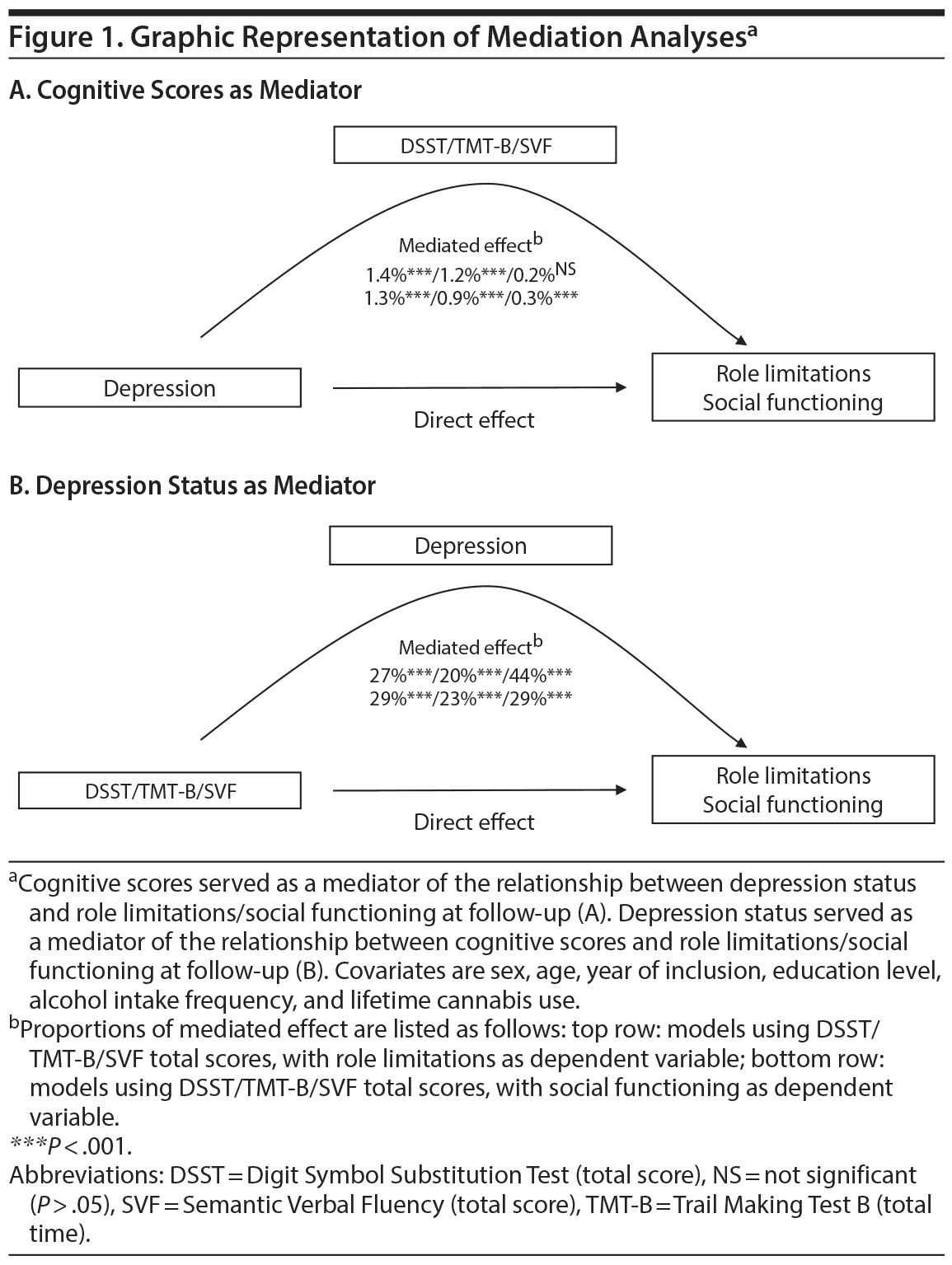
First, after adjustment for covariates, depression status was significantly associated with each of the 3 cognitive scores at baseline as expected (DSST: β = −0.19; 95% CI, −0.25 to −0.13; P < .001; TMT-B: β = 0.15; 95% CI, 0.08 to 0.21; P < .001; SVF: β = −0.11; 95% CI, −0.17 to −0.04; P = .001) and with both functioning scores (role limitations and social functioning) at follow-up (Table 1). Second, each of the 3 cognitive scores at baseline was significantly associated with the 2 functioning scores at follow-up as expected (Table 1). Third, after further adjustment for each cognitive score, the relationship between depression status and functioning remained virtually unchanged, and mediation analyses showed that cognitive scores at baseline accounted for only 0.3%-1.4% of the relationship between depression status at baseline and functioning at follow-up (Table 1, Figure 1). In contrast, depression status at baseline accounted for 19.5%-43.7% of the relationship between cognitive at baseline and functioning scores at follow-up (Table 1, Figure 1).

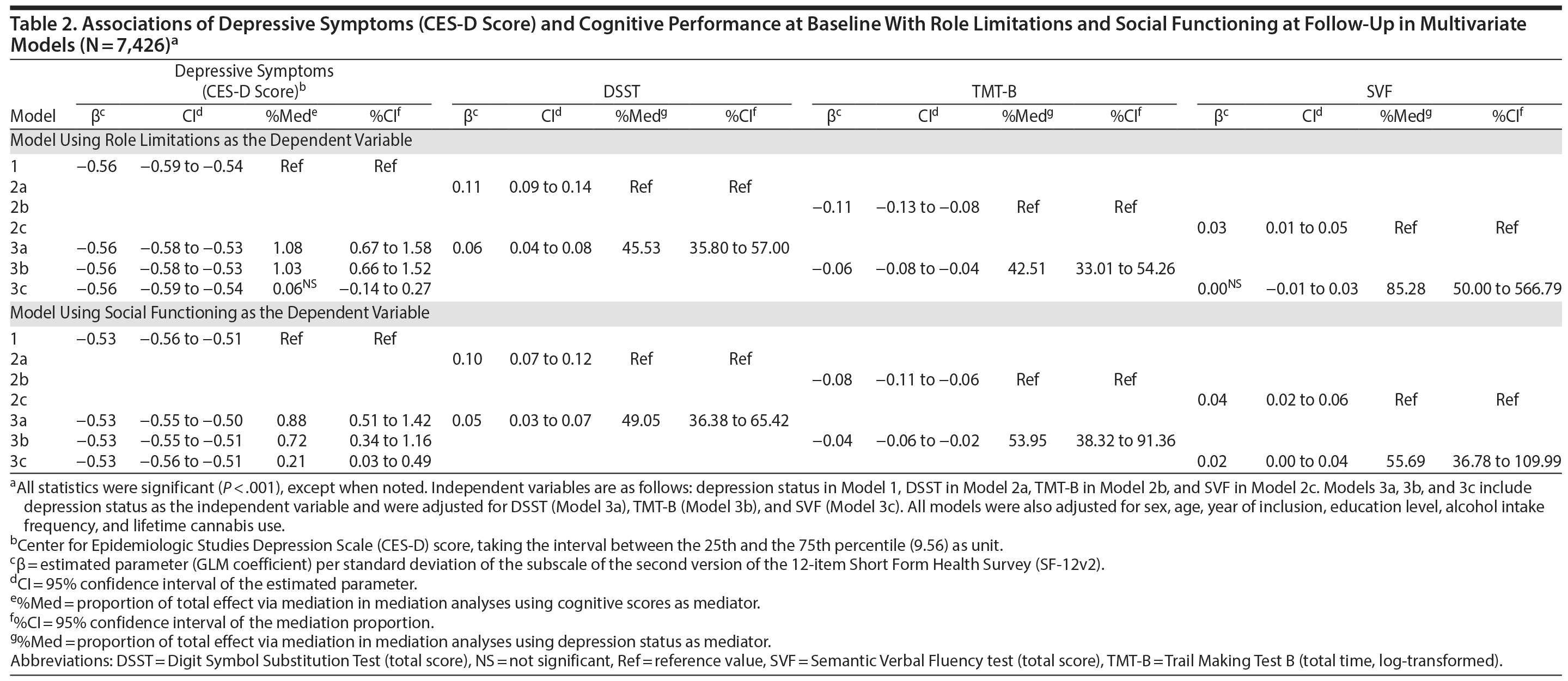
In sensitivity analyses based on continuous CES-D scores, depressive symptoms were also associated with each of the 3 cognitive scores (DSST: β = −0.10; 95% CI, −0.12 to −0.07; P < .001; TMT-B: β = .09; 95% CI, 0.07 to 0.12; P < .001; SVF: β = −0.06; 95% CI, −0.08 to −0.03; P < .001) and with both functioning scores (Table 2). The association between depressive symptoms and the 2 functioning scores remained virtually unchanged after further adjustment for each cognitive score, which accounted for only 0.2%-1.1% of this relationship (P < .001 considering DSST and TMT-B, not significant for SVF) (Table 2). In contrast, continuous CES-D scores accounted for 42.5%-85.3% of the relationship between cognitive and functioning scores (all P < .001) (Table 2).
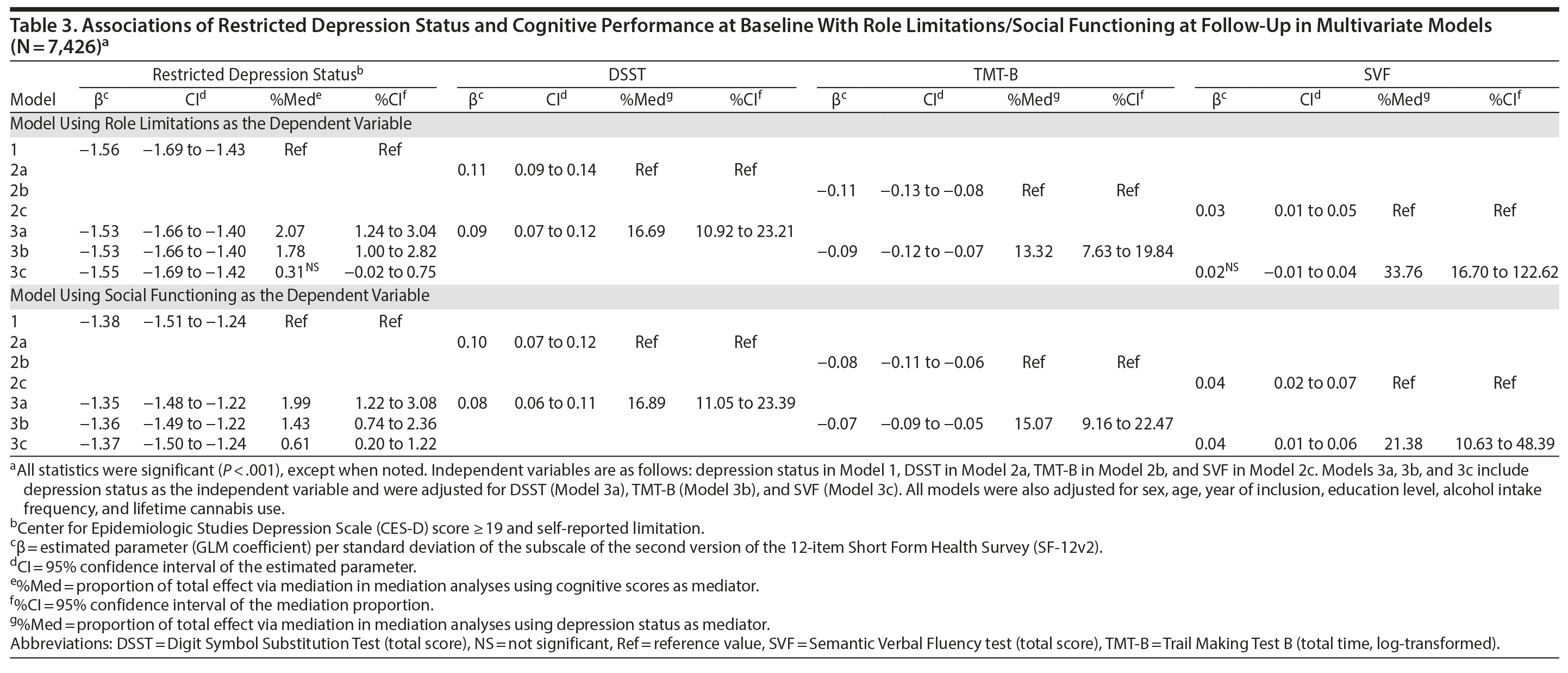
When a more restricted definition of depression status is used, combining both CES-D score ≥ 19 and self-reported limitation (n = 205, ie, 2.76% of the total sample), the association of depression status with each of the cognitive scores (DSST: β = −0.34; 95% CI, −0.47 to −0.22; P < .001; TMT-B: β = .29; 95% CI, 0.16 to 0.42; P < .001; SVF: β = −0.25; 95% CI, −0.38 to −0.11; P < .001) and with both functioning scores (Table 3) strengthened. However, cognitive scores accounted for only 0.6%-2.1% of the relationship between CES-D scores and functioning, whereas depression status still explained 13.3%-33.8% of the relationship between cognitive and functioning scores (all P < .001) (Table 3).


DISCUSSION
This prospective large-scale population-based study aimed to investigate the association of depressive symptoms and cognitive performance at baseline with both role limitations and social functioning at follow-up in adults aged 45 years or older. We found that the association between depressive symptoms and later functioning was not substantially explained by cognitive performance, regardless of the definition of depression (ie, binary or continuous), the cognitive test (ie, DSST, TMT-B or SVF), or the functioning variable (ie, role limitations or social functioning). In contrast, depression explained a substantial proportion of the association between cognition at baseline and functioning at follow-up.
Strengths of the study are the large size, the population-based sample, the prospective design, and the use of objective measures of cognitive functions. Thanks to a sufficient statistical power and standardized neuropsychological tests, our results were consistent with decades of literature linking depressive symptoms with both cognitive14,15 and functional2-6,8-11 impairment. However, it is noteworthy that this literature did not examine the contribution of cognitive function or functional impairment associated with depression. To our knowledge, our study might indeed be the first to explore this issue in a large prospective sample.
Some limitations should also be acknowledged. First, the population study is not representative of the general population and was confined to participants aged 45 to 69 years. Thus, our results cannot be generalized to younger or older adults. Second, the duration of the follow-up was short. However, the majority of the studies on this topic have been cross-sectional. Third, the diagnosis of depression was based on a self-report scale rather than on a standardized interview. However, sensitivity analyses using CES-D as a continuous score or a more restricted definition of depression status (including both CES-D score ≥ 19 and self-reported limitation at baseline) yielded similar results. Fourth, as in other studies on this topic,40 functioning was measured with a self-administered questionnaire (ie, the SF-12v2). In particular, one may argue that the items that were selected a priori from the SF-12v2 are intrinsically connected to depressive symptoms so that there might be little room for a mediating effect of objective cognitive functioning. However, it should be noted that not only depressive symptoms but also cognitive functions were associated with the 2 SF-12v2 subscales, suggesting that these measures were sensitive enough to capture relevant effects. Furthermore, depressive symptoms did account for a substantial part of the association between cognitive functions and these 2 subscales. Therefore, the lack of mediation effect by cognitive functions is unlikely to be explained by the subjective versus objective nature of the measures. Finally, our analyses did not control for intelligence quotient (IQ). Future studies would benefit in reproducing our results while additionally adjusting for IQ, particularly for cognitive tests that are closely related to IQ. For example, in older adults, TMT score has been found to be more strongly associated with IQ than education level.43 However, IQ may also be considered as the composite of neurobehavioral abilities assessed in neurocognitive tests.44 In this study, analyses were adjusted for education level, which has been found to be positively associated with both IQ and neuropsychological test performance.45 For example, a recent study46 reported a positive association between education level and cognitive scores, especially on more cognitively complex tests such as the TMT-B or the DSST, in contrast with more simple tests such as the TMT-A. Thus, schooling may foster the development of cognitive processes that underpin performance on IQ.
This study confirms results from previous ones2-6,8-11 of a strong association between depression and later altered functioning. We found that both social functioning and role limitations were significantly altered up to 24 months after depression assessment. The strength of these associations was similar to the figures obtained by Spijker et al41 with the 36-item Short Form Health Survey in individuals with major depression. Furthermore, we found a significant negative association between CES-D scores as a continuous measure and later functioning, suggesting that, as previously reported,6 these impairments in functioning were associated with the severity of depressive symptoms.
This study also confirms and extends in a general population sample the previously well-described associations between cognitive impairment (as measured by 3 cognitive tests) and both depression14-17 and altered functioning12,13,22-26 (as measured by 2 functioning scores). However, despite these findings, this large population-based study did not support the hypothesis that cognitive dysfunction could substantially explain the association between depression and functioning. This negative result could be explained by the population-based design of our study, which excluded severely depressed participants. However, we found similar results with a more stringent definition of depression. Thus, these analyses did not provide additional evidence for a mediation effect of cognitive impairment. To our knowledge, only 1 large-scale study30 found support for this hypothesis by formally testing the mediation. However, that study relied on subjective cognitive complaints that are poorly correlated with objective cognitive functions such as those measured by standardized neuropsychological tests.47 Some studies12,13 have reported an association between objectively assessed cognitive function and functional impairment in individuals with depression, thus providing preliminary evidence for a mediating role of cognitive function, but such mediation effect was not reported. Furthermore, since depression is associated with both cognitive and functional impairment, the association between objectively assessed cognitive function and functional impairment could have been confounded by depression itself.
Consistent with this alternative hypothesis, and contrasting with the lack of evidence for a mediating role of cognitive function, the mediation analyses suggested that depression could explain up to 44% of the relationship between cognitive deficits and altered functioning. Our results suggest that depression and cognitive impairment are strongly interrelated and both negatively impact functioning. However, depression without cognitive impairment may alter functioning to a greater extent than cognitive impairment without depression in a general population sample. Another plausible interpretation of this result is that depression might cause both cognitive and functional impairment. For instance, depression may result in both cognitive and functional impairment through altered motivation or decreased self-efficacy. Depression may also simultaneously affect cognitive and functional impairment, but by different mechanisms. For instance, ruminative thoughts associated with depression may reduce cognitive resources during performance of externally oriented cognitive tasks,48 whereas poor self-esteem and embarrassment may have detrimental impact on social functioning.30 However, these findings are controversial. For example, in 117 remitted patients with major depressive disorder, no association was found between residual symptoms such as self-blaming, feeling worthless, or hopeless and impaired cognition.49 As mediation and confounding are identical statistically, they can be distinguished only on conceptual grounds, even in longitudinal studies.50 Therefore, strictly speaking, our results are also consistent with the hypothesis that depression could mediate, rather than confound, the association between cognitive and functional impairment. For instance, the DSST, TMT-B, and SVF outcomes might result from impaired cognitive control, which is also involved in poor emotion regulation and thus vulnerability to depression.48 Although these 2 hypotheses (ie, confusion versus mediation) are not mutually exclusive, they both imply that the impact of depression on functional impairment is independent of cognitive impairment.
In adults aged 45 years or older from the general population, the association between depression at baseline and role limitations and social functioning at follow-up could not be explained by lower scores on cognitive tests. Although the management of cognitive impairment associated with depression is central to the treatment of depression, it may not be sufficient to improve the functioning beyond what is expected from the improvement of depression per se at the general population level. Further studies based on more ecological cognitive tests (eg, tests involving social cognition or integration of cognitive tests in social context), but also using objective measures of functioning (eg, absenteeism), are needed to further refine our understanding of the mechanisms explaining why depression is one of the most disabling conditions worldwide.51
Submitted: November 6, 2017; accepted May 14, 2018.
Published online: November 13, 2018.
Potential conflicts of interest: Pr Fossati received consulting and speaker honoraria from Janssen and Lundbeck and grant support from Servier. Pr Limosin received consulting and speaker honoraria from AstraZeneca, Euthérapie/Servier, Janssen, Lundbeck, Otsuka, and Roche. Pr Lemogne reports grants, personal fees, and non-financial support from Lundbeck; personal fees from Daiichi-Sankyo, Janssen, and Servier; and non-financial support from Otsuka, outside of this work. Drs Vulser, Wiernik, Hoertel, Melchior, Thibault, Olekhnovitch, Goldberg, and Zins have no conflict of interest to disclose.
Funding/support: The CONSTANCES cohort study was supported and funded by the Caisse nationale d’ assurance maladie des travailleurs salariés (CNAMTS). The CONSTANCES cohort study is an “Infrastructure nationale en Biologie et Santé” and benefits from a grant from Agence nationale de la recherche (ANR-11-INBS-0002). CONSTANCES is also partly funded by Merck Sharpe & Dohme, AstraZeneca, and Lundbeck.
Role of the sponsor: Funding sources had no role in the conduct or publication of the study.
Acknowledgments: The authors thank the CNAMTS and the “Centres d’ examens de santé” of the French Social Security, which collected a large part of the data, as well as the “Caisse nationale d’ assurance vieillesse,” ClinSearch, Asqualab, and Eurocell, which are in charge of the data quality control.
Supplementary material: Available at PSYCHIATRIST.COM.
REFERENCES
1. World Health Organization. Depression. WHO website. http://www.who.int/mediacentre/factsheets/fs369/en/ Accessed March 3, 2017.
2. Broadhead WE, Blazer DG, George LK, et al. Depression, disability days, and days lost from work in a prospective epidemiologic survey. JAMA. 1990;264(19):2524-2528. PubMed CrossRef
3. Wells KB, Stewart A, Hays RD, et al. The functioning and well-being of depressed patients: results from the Medical Outcomes Study. JAMA. 1989;262(7):914-919. PubMed CrossRef
4. Adler DA, McLaughlin TJ, Rogers WH, et al. Job performance deficits due to depression. Am J Psychiatry. 2006;163(9):1569-1576. PubMed CrossRef
5. Weinstock LM, Keitner GI, Ryan CE, et al. Family functioning and mood disorders: a comparison between patients with major depressive disorder and bipolar I disorder. J Consult Clin Psychol. 2006;74(6):1192-1202. PubMed CrossRef
6. Reed C, Monz BU, Perahia DGS, et al. Quality of life outcomes among patients with depression after 6 months of starting treatment: results from FINDER. J Affect Disord. 2009;113(3):296-302. PubMed CrossRef
7. Kim JM, Chalem Y, di Nicola S, et al. A cross-sectional study of functional disabilities and perceived cognitive dysfunction in patients with major depressive disorder in South Korea: the PERFORM-K study. Psychiatry Res. 2016;239:353-361. PubMed CrossRef
8. Strine TW, Kroenke K, Dhingra S, et al. The associations between depression, health-related quality of life, social support, life satisfaction, and disability in community-dwelling US adults. J Nerv Ment Dis. 2009;197(1):61-64. PubMed CrossRef
9. Rizvi SJ, Cyriac A, Grima E, et al. Depression and employment status in primary and tertiary care settings. Can J Psychiatry. 2015;60(1):14-22. PubMed CrossRef
10. Soares CN, Kornstein SG, Thase ME, et al. Assessing the efficacy of desvenlafaxine for improving functioning and well-being outcome measures in patients with major depressive disorder: a pooled analysis of 9 double-blind, placebo-controlled, 8-week clinical trials. J Clin Psychiatry. 2009;70(10):1365-1371. PubMed CrossRef
11. Kennedy N, Foy K, Sherazi R, et al. Long-term social functioning after depression treated by psychiatrists: a review. Bipolar Disord. 2007;9(1-2):25-37. PubMed CrossRef
12. Evans VC, Iverson GL, Yatham LN, et al. The relationship between neurocognitive and psychosocial functioning in major depressive disorder: a systematic review. J Clin Psychiatry. 2014;75(12):1359-1370. PubMed CrossRef
13. Lam RW, Kennedy SH, Mclntyre RS, et al. Cognitive dysfunction in major depressive disorder: effects on psychosocial functioning and implications for treatment. Can J Psychiatry. 2014;59(12):649-654. PubMed CrossRef
14. McDermott LM, Ebmeier KP. A meta-analysis of depression severity and cognitive function. J Affect Disord. 2009;119(1-3):1-8. PubMed CrossRef
15. Snyder HR. Major depressive disorder is associated with broad impairments on neuropsychological measures of executive function: a meta-analysis and review. Psychol Bull. 2013;139(1):81-132. PubMed CrossRef
16. Lee RSC, Hermens DF, Porter MA, et al. A meta-analysis of cognitive deficits in first-episode major depressive disorder. J Affect Disord. 2012;140(2):113-124. PubMed CrossRef
17. Ahern E, Semkovska M. Cognitive functioning in the first-episode of major depressive disorder: a systematic review and meta-analysis. Neuropsychology. 2017;31(1):52-72. PubMed CrossRef
18. Mahableshwarkar AR, Zajecka J, Jacobson W, et al. A randomized, placebo-controlled, active-reference, double-blind, flexible-dose study of the efficacy of vortioxetine on cognitive function in major depressive disorder. Neuropsychopharmacology. 2015;40(8):2025-2037. PubMed CrossRef
19. Rosenblat JD, Kakar R, McIntyre RS. The cognitive effects of antidepressants in major depressive disorder: a systematic review and meta-analysis of randomized clinical trials. Int J Neuropsychopharmacol. 2015;19(2):pyv0852. PubMed
20. Bora E, Harrison BJ, Yücel M, et al. Cognitive impairment in euthymic major depressive disorder: a meta-analysis. Psychol Med. 2013;43(10):2017-2026. PubMed CrossRef
21. Rock PL, Roiser JP, Riedel WJ, et al. Cognitive impairment in depression: a systematic review and meta-analysis. Psychol Med. 2014;44(10):2029-2040. PubMed CrossRef
22. Jaeger J, Berns S, Uzelac S, et al. Neurocognitive deficits and disability in major depressive disorder. Psychiatry Res. 2006;145(1):39-48. PubMed CrossRef
23. Naismith SL, Longley WA, Scott EM, et al. Disability in major depression related to self-rated and objectively-measured cognitive deficits: a preliminary study. BMC Psychiatry. 2007;7(1):32. PubMed CrossRef
24. Withall A, Harris LM, Cumming SR. The relationship between cognitive function and clinical and functional outcomes in major depressive disorder. Psychol Med. 2009;39(3):393-402. PubMed CrossRef
25. Baune BT, Miller R, McAfoose J, et al. The role of cognitive impairment in general functioning in major depression. Psychiatry Res. 2010;176(2-3):183-189. PubMed CrossRef
26. Rothschild AJ, Raskin J, Wang CN, et al. The relationship between change in apathy and changes in cognition and functional outcomes in currently non-depressed SSRI-treated patients with major depressive disorder. Compr Psychiatry. 2014;55(1):1-10. PubMed CrossRef
27. Bowie CR, Depp C, McGrath JA, et al. Prediction of real-world functional disability in chronic mental disorders: a comparison of schizophrenia and bipolar disorder. Am J Psychiatry. 2010;167(9):1116-1124. PubMed CrossRef
28. McIntyre RS, Cha DS, Soczynska JK, et al. Cognitive deficits and functional outcomes in major depressive disorder: determinants, substrates, and treatment interventions. Depress Anxiety. 2013;30(6):515-527. PubMed CrossRef
29. Woo YS, Rosenblat JD, Kakar R, et al. Cognitive deficits as a mediator of poor occupational function in remitted major depressive disorder patients. Clin Psychopharmacol Neurosci. 2016;14(1):1-16. PubMed CrossRef
30. Buist-Bouwman MA, Ormel J, de Graaf R, et al; ESEMeD/MHEDEA 2000 investigators. Mediators of the association between depression and role functioning. Acta Psychiatr Scand. 2008;118(6):451-458. PubMed CrossRef
31. Zins M, Bonenfant S, Carton M, et al. The CONSTANCES cohort: an open epidemiological laboratory. BMC Public Health. 2010;10(1):479. PubMed CrossRef
32. Zins M, Goldberg M; CONSTANCES team. The French CONSTANCES population-based cohort: design, inclusion and follow-up. Eur J Epidemiol. 2015;30(12):1317-1328. PubMed CrossRef
33. Radloff LS. The CES-D Scale: a self-report depression scale for research in the general population. Appl Psychol Meas. 1977;1(3):385-401. CrossRef
34. Morin AJS, Moullec G, Maׯano C, et al. Psychometric properties of the Center for Epidemiologic Studies Depression Scale (CES-D) in French clinical and nonclinical adults. Rev Epidemiol Sante Publique. 2011;59(5):327-340. PubMed CrossRef
35. Wechsler D. WAIS-R, Wechsler Adult Intelligence Scale- Revised, Manual. New York, NY: Psychological Corporation; 1981.
36. Gaudino EA, Geisler MW, Squires NK. Construct validity in the Trail Making Test: what makes Part B harder? J Clin Exp Neuropsychol. 1995;17(4):529-535. PubMed CrossRef
37. Borkowski JG, Benton AL, Spreen O. Word fluency and brain damage. Neuropsychologia. 1967;5(2):135-140. CrossRef
38. Ware J Jr, Kosinski M, Keller SDA. A 12-Item Short-Form Health Survey: construction of scales and preliminary tests of reliability and validity. Med Care. 1996;34(3):220-233. PubMed CrossRef
39. Ware JE; QualityMetric Incorporated, New England Medical Center Hospital; Health Assessment Lab. How to Score Version 2 of the SF-12 Health Survey (With a Supplement Documenting Version 1). Lincoln, RI: Health Assessment Lab; Boston, MA: QualityMetric Inc; 2005.
40. Cheak-Zamora NC, Wyrwich KW, McBride TD. Reliability and validity of the SF-12v2 in the medical expenditure panel survey. Qual Life Res. 2009;18(6):727-735. PubMed CrossRef
41. Spijker J, Graaf R, Bijl RV, et al. Functional disability and depression in the general population: results from the Netherlands Mental Health Survey and Incidence Study (NEMESIS). Acta Psychiatr Scand. 2004;110(3):208-214. PubMed CrossRef
42. Imai K, Keele L, Tingley D. A general approach to causal mediation analysis. Psychol Methods. 2010;15(4):309-334. PubMed CrossRef
43. Steinberg BA, Bieliauskas LA, Smith GE, et al. Mayo’s Older Americans Normative Studies: Age- and IQ-Adjusted Norms for the Trail-Making Test, the Stroop Test, and MAE Controlled Oral Word Association Test. Clin Neuropsychol. 2005;19(3-4):329-377. PubMed CrossRef
44. Larrabee GJ. Association between IQ and neuropsychological test performance: commentary on Tremont, Hoffman, Scott, and Adams (1998). Clin Neuropsychol. 2000;14(1):139-145. PubMed CrossRef
45. Ceci SJ. How much does schooling influence general intelligence and its cognitive components? a reassessment of the evidence. Dev Psychol. 1991;27(5):703-722. CrossRef
46. Guerra-Carrillo B, Katovich K, Bunge SA. Does higher education hone cognitive functioning and learning efficacy? findings from a large and diverse sample. PLoS One. 2017;12(8):e0182276. PubMed CrossRef
47. Burmester B, Leathem J, Merrick P. Subjective cognitive complaints and objective cognitive function in aging: a systematic review and meta-analysis of recent cross-sectional findings. Neuropsychol Rev. 2016;26(4):376-393. PubMed CrossRef
48. Nejad AB, Fossati P, Lemogne C. Self-referential processing, rumination, and cortical midline structures in major depression. Front Hum Neurosci. 2013;7:666. PubMed CrossRef
49. Pedrelli P, Baer L, Losifescu DV, et al. Relationship between residual symptoms of depression and self-reported cognitive impairment. CNS Spectr. 2010;15(1):46-51. PubMed CrossRef
50. MacKinnon DP, Krull JL, Lockwood CM. Equivalence of the mediation, confounding and suppression effect. Prev Sci. 2000;1(4):173-181. PubMed CrossRef
51. Baldessarini RJ, Forte A, Selle V, et al. Morbidity in depressive disorders. Psychother Psychosom. 2017;86(2):65-72. PubMed CrossRef
Editor’s Note: We encourage authors to submit papers for consideration as a part of our Early Career Psychiatrists section. Please contact Erika F. H. Saunders, MD, at [email protected].
This PDF is free for all visitors!