ABSTRACT
Objective: Frailty is a clinical phenotype that predicts negative health outcomes, including mortality, and is increasingly used for risk stratification in geriatric medicine. Similar to frailty, late-life depression is also associated with increased mortality rates. Therefore, we examined whether frailty and frailty-related biomarkers predict mortality among depressed older patients.
Methods: In our study of 378 older patients aged ≥ 60 years with a depressive disorder (DSM-IV criteria), we examined whether frailty predicts time-to-death during a 6-year follow-up using Cox proportional hazard regression analyses adjusted for confounders. Baseline data were collected from 2007 to September 2010. Frailty was defined according to the Fried Frailty Phenotype criteria (muscle weakness, slowness, exhaustion, low activity level, unintended weight loss). Similarly, we examined the predictive value of 3 inflammatory markers, vitamin D level, and leukocyte telomere length and whether these effects were independent of the frailty phenotype.
Results: During follow-up, 27 (26.2%) of 103 frail depressed patients died compared with 35 (12.7%) of 275 non-frail depressed patients (P < .001). Adjusted for confounders, the number of frailty components was associated with an increased mortality rate (hazard ratio = 1.38 [95% CI, 1.06–1.78], P = .015). All biomarkers except for interleukin 6 were prospectively associated with mortality, but only higher levels of high-sensitivity C-reactive protein and lower levels of vitamin D were independent of frailty associated with mortality.
Conclusions: In late-life depression, frailty identifies older patients at increased risk of adverse negative health outcomes. Therefore, among frail depressed patients, treatment models that include frailty-specific interventions might reduce mortality rates.
J Clin Psychiatry 2021;82(3):20m13277
To cite: Arts MHL, van den Berg KS, Marijnissen RM, et al. Frailty as a predictor of mortality in late-life depression: a prospective clinical cohort study. J Clin Psychiatry. 2021;82(3):20m13277.
To share: https://doi.org/10.4088/JCP.20m13277
© Copyright 2021 Physicians Postgraduate Press, Inc.
aUniversity of Groningen, University Medical Center Groningen, University Center for Psychiatry, Groningen, Netherlands
bMental Health Center (GGZ) Westelijk Noord-Brabant, Department of Old Age Psychiatry, Halsteren, Netherlands
cNow with Tranzo, School of Social and Behavioural Sciences, Tilburg University, Tilburg, Netherlands
dSt Antonius Hospital, Department of Psychiatry, Nieuwegein, Netherlands
eMental Health Centre, Pro Persona, Department of Old Age Psychiatry, Wolfheze, Netherlands
fUniversity Medical Centre St Radboud, Department of Psychiatry, Nijmegen, Netherlands
gVU University Medical Center/GGZinGeest, Department of Psychiatry/EMGO Institute for Health and Care Research, Amsterdam, Netherlands
hDepartment and Institute of Psychiatry, Faculty of Medicine, University of São Paulo, São Paulo, Brazil
iGGNet, Department of Old Age Psychiatry, Apeldoorn, Netherlands
*Corresponding author: Matheus H. L. Arts, MD, MSc, GGZ Westelijk Noord-Brabant, Hoofdlaan 8, 4661 AA, Halsteren, The Netherlands ([email protected]).
Depressive disorder is increasingly recognized as a disorder of accelerated aging based on its association with many physiologic and cellular markers of aging.1 In line with this theory, meta-analyses2,3 have shown that depression is associated with excess mortality that cannot be explained by suicide. A reassessment3 of 293 studies included in 15 systematic reviews, however, found evidence for pronounced publication bias in favor of positive findings, bias due to preselection on medical conditions, and insufficient control for confounders, especially comorbidity and lifestyle. Furthermore, most studies in these reviews had assessed depression with depressive symptom severity scales instead of formal diagnostic criteria of the DSM or ICD.3 Self-report depressive symptom scales may be falsely inflated by the presence of comorbid chronic somatic diseases4 and thereby confound the association between depression and mortality. The 4 studies that had assessed depressive disorders according to DSM criteria yielded a pooled hazard ratio (HR) of 1.2 (95% CI, 0.8–1.6) for mortality, which was no longer statistically significant.3 More well-controlled studies of excess mortality in depressed patients according to DSM criteria are needed to explore which characteristics may explain the potential relationship between depression and mortality.
Frailty is characterized by cumulative declines in multiple physiologic systems, accompanied by an increased vulnerability to stressors.5 In geriatric medicine, frailty is increasingly used for risk stratification to identify patients at increased risk of adverse health outcomes, including mortality, and to deliver patient-centered care.6 Frailty might be a pathway that may explain excess mortality in depression. In a population-based cohort study7 of men aged 75 years and older, the crude mortality hazard ratio of 4.3 for a DSM-IV–defined depressive disorder dropped to 1.8 after additional correction for frailty. The other way around, the prospective association of frailty with mortality differs between disease clusters and seems smallest for patients with neuropsychiatric disorders.8 To our knowledge, prospective association between frailty and mortality has never been examined in clinically depressed patients, which is relevant as frailty and depression have a complex relationship. Firstly, depression and frailty share many risk factors and consequences.9 Secondly, at a population level, frailty and depression often identify the same subgroup of persons, especially older persons with high levels of depressive symptoms.9 Thirdly, many operationalizations of the frailty concept include criteria that may overlap with a depressive disorder, like psychomotor retardation, fatigue, weight loss, and feelings of exhaustion. A meta-analysis10 estimated that 40.4% of depressed older persons are frail and that 38.6% of frail persons are depressed. Furthermore, longitudinal studies showing a bidirectional association between depression and frailty are scarse.10 Nonetheless, only 4 studies in this meta-analysis assessed depression according to formal diagnostic criteria. In the Netherlands Study of Depression in Older persons (NESDO),11 we showed that only 27.2% of the patients suffering from a DSM-IV–defined depressive disorder were physically frail.
Many aging-related biomarkers are associated with both frailty and depressive disorder. Whether these biomarkers represent common pathophysiology or mediate the prospective association from frailty to depression (or vice versa) needs further study. In NESDO, we did not find consistent associations between late-life depression and low-grade inflammatory markers12 or leukocyte telomere length (LTL),13 whereas we found that lower vitamin D levels were only cross-sectionally but not prospectively associated with late-life depression.14,15 Consistent with the literature on frailty, we also found that physical frailty was associated with low-grade inflammation,16 a shorter LTL,17 and lower vitamin D levels.18 Collectively, these NESDO results may point to frailty as a moderating factor to adverse outcomes like death among depressed older adults.
To our knowledge, only 1 study19 has examined whether frailty predicts mortality in psychiatric patients. In that study of a mixed group of 120 older psychiatric inpatients, among which 41 were depressed patients, frailty predicted mortality within 5 years. This effect was independent of chronological age, somatic disease burden, functional status, and neuropsychiatric symptoms.19 The present study, embedded in NESDO, examines the prospective association of the physical frailty phenotype and associated biomarkers with mortality in 378 clinically depressed older patients. We hypothesize that physical frailty as well as physiologic and cellular biomarkers of aging are prospectively associated with the 6-year mortality rate.
METHODS
Study Population
The present NESDO-embedded study included 378 depressed subjects aged ≥ 60 years who meet the criteria for a DSM-IV depressive disorder using the Composite International Diagnostic Interview (CIDI)20 version 2.1. Of these 378 patients, 95% had a major depressive disorder diagnosis within the previous 6 months, 26.5% a dysthymia diagnosis within the previous 6 months, and 5.6% a minor depression diagnosis within the previous month (numbers do not add up to 100% as 26.5% had 2 depressive disorders). Exclusion criteria were an established or suspected diagnosis of a neurocognitive disorder, a Mini-Mental State Examination (MMSE)21 score < 18, a history of a psychotic disorder, and insufficient mastery of the Dutch language. Since a severe depressive disorder may interfere with cognitive testing, we accepted an MMSE score as low as 18 in case the patient was neither diagnosed with nor suspected to have an underlying neurocognitive disorder.
The overall aim of NESDO is to examine the course and consequences of depressive disorders in older persons. All participants underwent a baseline examination at 1 of the 5 research locations or at their homes. This baseline examination included a structured psychiatric diagnostic interview (CIDI 2.1),20 cognitive testing, physical examination, blood collection, and several observer-rated and self-report questionnaires. Baseline data collection started in 2007 and was finished in September 2010. This assessment was repeated at 2-year and 6-year follow-up for all baseline characteristics amenable to change. In between, every 6 months, up to 6 years, postal questionnaires were sent to monitor depressive symptom severity (among other measures). Reasons for dropout (including mortality) were explored and registered at 6-month intervals parallel to postal questionnaires and site vistis.22
The ethical review boards of all participating study centers approved the NESDO-study protocol, and all participants provided written informed consent.20,22
Physical Frailty Phenotype
The physical frailty phenotype was assessed according to the Fried Frailty Phenotype criteria,11,23 also known as the Fried Frailty Index (FFI), and patients were classified as frail when at least 3 of the 5 criteria were present, including weight loss, weakness, exhaustion, slowness, and low physical activity.
Weakness was defined as the maximum handgrip strength (as measured by 2 squeezes of the dominant hand on a hand grip dynamometer) below a cutoff stratified by sex and body mass index (BMI). Slowness was defined as a time ≥ 8 seconds for men ≥ 173 cm tall or women ≥ 159 cm tall, or ≥ 9 seconds for men < 173 cm tall or women < 159 cm tall, on a 6-meter walking test. Exhaustion was defined as scoring positive (with a score of 2 or 3) on 1 of the 2 items regarding energy level and exhaustion of the Center for Epidemiologic Studies Depression (CES-D) scale.24 Low physical activity was defined as doing no daily activities, such as walking or gardening, and the performance of sports less than once a week, as assessed with the International Physical Activity Questionnaire.25 Finally, unintended weight loss was defined as a positive answer to the CIDI question about unintended weight loss (≥ 1 kg/wk for ≥ 2 consecutive weeks) or a BMI < 18.5 kg/m2.
Aging and Frailty Biomarkers
Fasting blood samples were obtained at baseline in the morning around 8 am and kept at −80 °C for subsequent analyses of biomarkers. On the basis of availability in the NESDO study, we have chosen to explore the following biomarkers:
Low-grade inflammation: We assessed plasma levels of C-reactive protein (CRP), interleukin 6 (IL-6), and neutrophil gelatinase-associated lipocalin (lipocalin-2 or NGAL). High-sensitivity plasma levels of CRP (hsCRP) were measured in duplicate by an immunoturbidimetric assay (Tina-quant CRP–HS, Roche Diagnostics). Intra- and interassay coefficients of variation were 2% and 2%, respectively. Plasma IL-6 levels were measured in duplicate by a high-sensitivity enzyme-linked immunosorbent assay (ELISA) kit (PeliKine Compact ELISA, Sanquin). Intra- and interassay coefficients of variation were 8% and 12%, respectively. Finally, the plasma lipocalin-2 levels (ng/mL) were measured in duplicate using a lipocalin 2/NGAL ELISA kit (R&D Systems).26 The intra- and interassay coefficients of variation were 2% and 5%, respectively. Lipocalin-2 is a 25-kDa protein of the lipocalin superfamily and a critical component of innate immunity to bacterial infection. It has recently been identified as a neuroinflammatory marker in depressed or cognitively impaired patients.26 Lipocalin-2 expression is triggered by TNF receptor 1 signaling and is able to induce a proapoptotic signaling cascade by attenuating Akt phosphorylation of the protein kinase B (Akt) pathway.
Vitamin D: Serum 25-hydroxy vitamin D levels were measured at baseline using isotope dilution–online solid-phase extraction liquid chromatography–tandem mass spectrometry, as described previously.14
Leukocyte telomere length (LTL): LTL was determined by Telomere Diagnostics. Quantitative polymerase chain reaction was used to compare the telomere sequence copy number (T) in each patient’s sample to a single-copy gene copy number (S), relative to a reference sample. The intraassay coefficient of variation (CV) was 5.1%, and the interassay CV was 4.6%. The resulting T/S ratio was proportional to mean telomere length. The T/S ratio was converted to base pairs (bp) by the following formula: bp = 3274 + 2413 × ([T/S – 0.0545]/1.16).27
Covariates
For covariates, we included the most important determinants of mortality, ie, sociodemographic data (age, sex, years of education, partner status), lifestyle characteristics, somatic disease burden, and depressive symptom severity at baseline.
Lifestyle characteristics included smoking (yes/no), number of alcoholic drinks per day based on the Alcohol Use Disorder Identification Test,28 physical activity in metabolic-equivalent-of-task–minutes based on the International Physical Activity Questionnaire,25 and body mass index (BMI) in kg/m2.
The somatic disease burden was quantified as the number of chronic somatic diseases under treatment and the number of prescribed medications. The total number of self-reported chronic diseases was determined by well-validated algorithms29 and included lung disease, cardiovascular disease, diabetes, osteoarthritis or rheumatic disease, cancer, ulcer, intestinal problems, liver disease, epilepsy, and thyroid gland disease. To calculate the number of medications, all drugs with a unique Anatomic Therapeutical Chemical (ATC) Classification System code at a 3-digit level were counted. Dermatologic preparations, medications without an ATC code, medications used less than half of the week (except drugs for which nondaily use is common, ie, bisphosphonates, methotrexate), and medications for use “if necessary” were excluded. Data on drug use were collected at the interviews (and checked by reviewing medication containers). In addition, analyses were also adjusted for insomnia and depressive symptom severity because depression and sleep duration have both been associated with death. Depressive symptom severity was measured by the well-validated 30-item self-rating Inventory for Depressive Symptomatology.30 Additionally, sleep was measured with the self-report 5-item Insomnia Rating Scale.30
Finally, models including vitamin D levels were additionally adjusted for the astronomical season when blood samples were collected.
Data Analysis
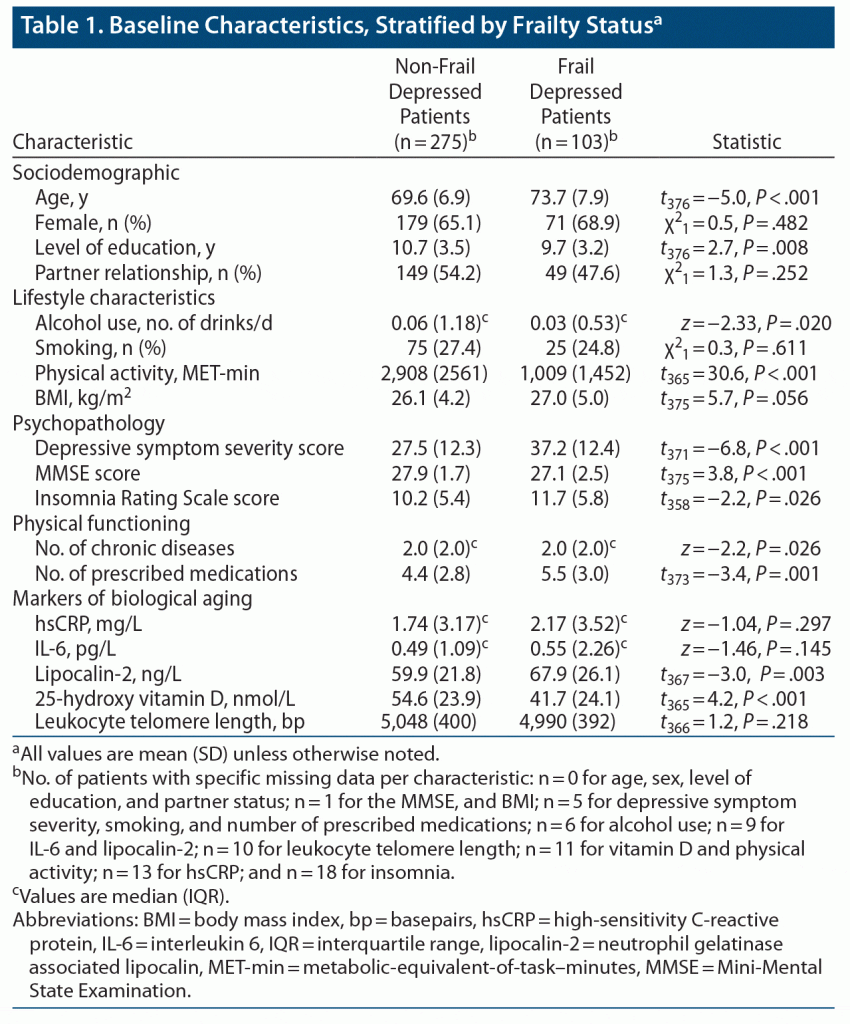
Baseline characteristics are presented stratified for frail and non-frail depressed patients and tested by Student t tests or Mann-Whitney U tests for continuous variables and by χ2 tests for categorical variables.
Cox proportional hazard regression models were used to investigate the effect of frailty on time-to-attrition due to death. Survival time ranged from baseline till either death (outcome) or censorship at time of study dropout or end of the follow-up (at 6 years). The presence of frailty (yes/no) and the number of frailty components present (range, 0–5) were the primary variables of interest. To explore the impact of frailty in more depth, we also examined the impact of specific frailty components, ie, (1) the impact of each of the 5 Fried frailty criteria (yes/no); (2) gait speed and handgrip strength as continuous, unidimensional proxies for frailty; and (3) 2 frailty dimensions based on the principal components analysis with direct oblimin rotation on the 5 components of the Fried Frailty Phenotype23 as described before.15 The Cox proportional hazard assumption was checked by visual inspection of the survival curves for patients with and without meeting the frailty criteria. Hazard ratios are presented bivariate as well as adjusted for age, sex, level of education, smoking, alcohol use, physical activity, insomnia, depressive symptom severity, cognitive functioning, number of chronic somatic diseases, and number of prescribed medications.
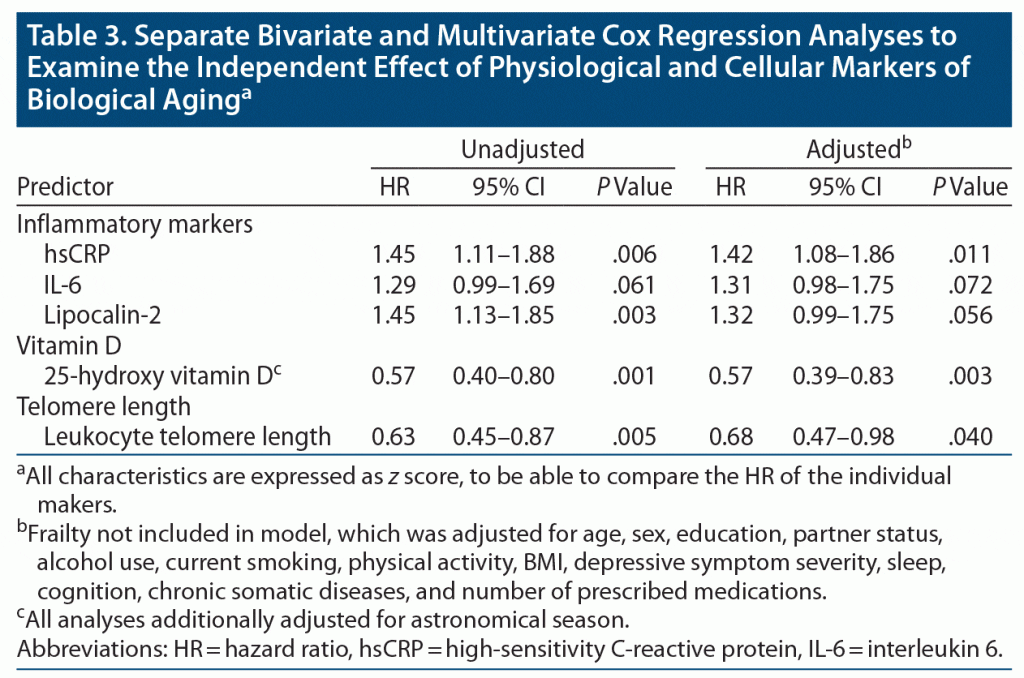
Next, we examined whether the 3 inflammatory markers, vitamin D level, and LTL (independently) were prospectively associated with mortality using separate bivariate and multivariate Cox regression models with time-to-death as the dependent variable (similarly built and checked as the frailty models, but excluding frailty characteristics). Analyses of vitamin D levels were additionally adjusted for season of blood collection. To be able to compare the effect size of the different underlying mechanisms, we calculated z scores for each variable. Before calculating z scores, gait speed, handgrip strength, hsCRP, and IL-6 were log-transformed to achieve a normal distribution. For lipocalin-2, 3 outliers were trimmed at 3 times the standard deviation to achieve a normal distribution.
Finally, clinically significant inflammatory markers, vitamin D levels, and/or LTL were added simultaneously with frailty in a final model to examine whether the results were independent or could be explained by shared variance.
All P values < .05 were considered statistically significant. Analyses were conducted using SPSS Statistics version 25 (IBM Corp).
RESULTS
Sample
The baseline characteristics of the study sample (n = 378) are presented in Table 1, stratified by the presence of frailty. The number of patients with missing data varied between none (for age, sex, level of education) and 6 (for alcohol use). Compared with non-frail patients, frail patients were significantly older, less educated, more severely depressed, drank less alcohol, and had more chronic somatic diseases. The two groups did not differ with respect to sex and smoking status.
Frailty as Determinant of Mortality
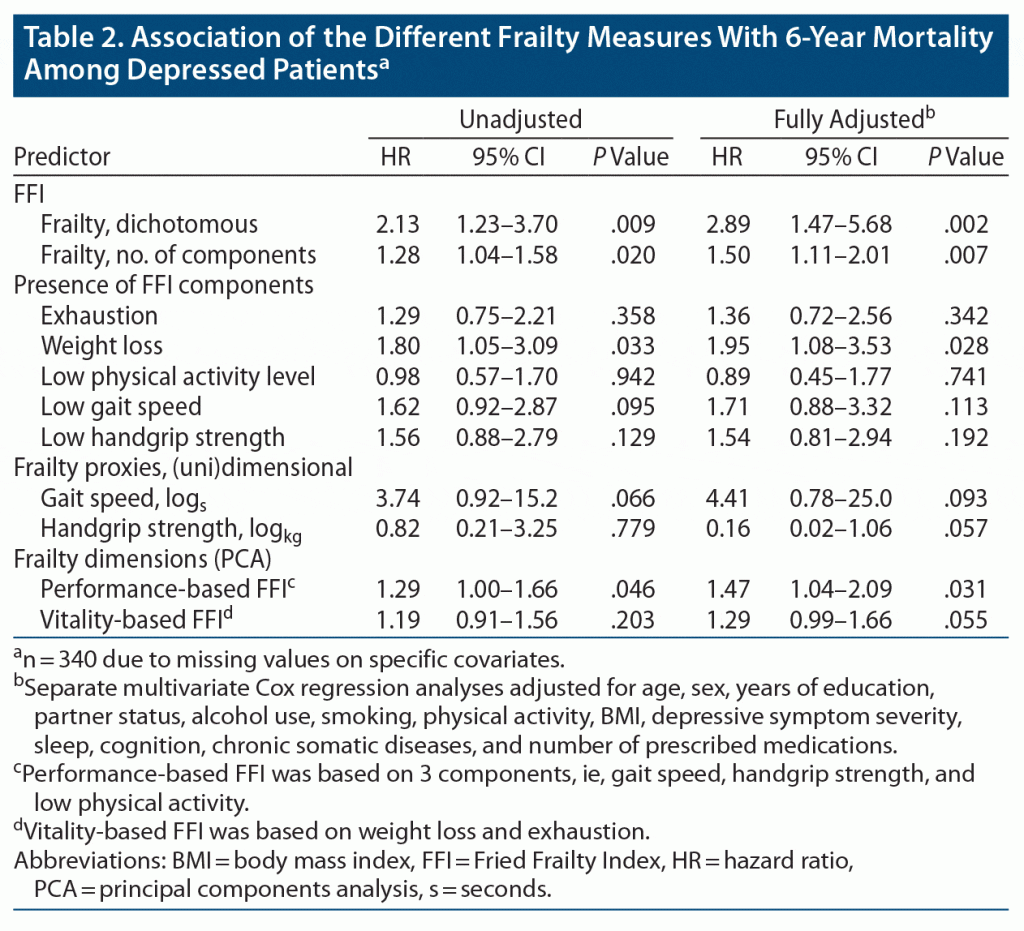
During the 6-year follow-up, a total of 27 (26.2%) of 103 frail depressed patients died compared with 35 (12.7%) of 275 non-frail depressed patients (χ21 = 9.9, P = .002). Adjusted for covariates, the HR of frailty was 2.43 (95% CI, 1.33–4.43), P = .004.
Table 2 presents the unadjusted and adjusted prospective association between frailty and mortality. As shown, frailty is associated with an increased mortality risk, irrespective of being classified as present/absent or by the number of frailty components met. Regarding the individual frailty components, only weight loss reached statistical significance, and regarding frailty dimensions, only performance-based physical frailty reached significance (see Table 2).
Biomarkers as Determinants of Mortality
Except for the level of IL-6, all biomarkers were significantly associated with the mortality rate, although the impact of lipocalin-2 lost statistical significance in the fully adjusted model. Higher hsCRP levels were prospectively associated with increased mortality rates, whereas higher vitamin D levels and LTL were protective (see Table 3).
Subsequently, we included the 3 significant biomarkers (hsCRP, LTL, vitamin D) in the fully adjusted frailty models. The HR of the presence of frailty remained significant (HR = 2.85 [95% CI, 1.40–5.77], P = .004) as did the HR of the sum score (HR = 1.29 [95% CI, 0.98–1.68], P = .065). In these models, LTL lost significance, whereas hsCRP and vitamin D remained significant independently of frailty associated with mortality (in the dichotomous frailty model, HR of hsCRP: [HR = 1.37 (95% CI, 1.04–1.81), P = .026]; HR of vitamin D: [HR = 0.59 (95% CI, 0.41–0.86), P = .005]).
DISCUSSION
In line with a recent meta-analysis32,33 on the relationship between frailty and mortality, we found a prospective association between physical frailty and mortality over a 6-year follow-up among patients suffering from late-life depression. This association remained significant even when adjusted for depression severity, lifestyle characteristics, and somatic morbidity. Moreover, the impact of frailty on mortality in late-life depression was independent of inflammatory markers, leukocyte telomere length, and vitamin D, whereas hsCRP and vitamin D were also prospectively associated with mortality independent of frailty.34
The concept of frailty has been introduced to describe (and identify) older persons at increased risk for disability and death. Demonstrating a prospective association between a specific frailty model and mortality is generally regarded as the ultimate validation of these models. A meta-analysis33 of 19 longitudinal studies demonstrated that the Fried Frailty Index, which is based on the deficit accumulation model, consistently predicts mortality. The deficits accumulation model postulates that the proportion of at least 30 aging-related health deficits reflects biological age on top of chronological age.35 Nonetheless, this model can be criticized to be merely a model of multimorbidity, as chronic diseases as well disease severity states are included as health deficits.35 Currently, many studies have shown that the Fried Frailty Phenotype23 is also associated with increased mortality rates,36 although a meta-analysis is not available. Within the UK biobank, comprising data from 493,737 persons, the Fried Frailty Phenotype predicted mortality independent of multimorbidity.36 The authors of these studies argue for more research on the impact of frailty across different disease contexts. This research may be especially important for a mental health context, as the impact of the frailty phenotype is less in patients with neuropsychiatric diseases compared with those with other chronic disease clusters,8 which might be explained by overlapping criteria between frailty and (neuro)psychiatric disorders.8 To our knowledge, our study is the first to evaluate the impact of frailty in a homogeneous sample of psychiatric patients. Moreover, in contrast to previous studies, we adjusted for multimorbidity as well as for lifestyle characteristics. We found most robust results for the original operationalization of the Fried Frailty Phenotype, showing that frailty is more than the sum of its components.
Previously, we reported that, within the NESDO-study, the mortality rate was significantly higher among depressed patients compared with the non-depressed comparison group.22 However, when adjusted for demographic, lifestyle, and somatic comorbidity, this difference lost significance.18 This latter finding points to the importance of adequate adjustment for confounders. Previous studies on the association between depression and mortality have been criticized for incomplete correction for potential confounders.3
Frailty is a clinical phenotype that is supposed to result from many different pathophysiologic mechanisms.34 Studies on the biology of frailty are now booming, and a large number of frailty-related biomarkers have been proposed; in particular, those representing inflammatory, endocrine, and metabolic pathways.34,37 In this study, we have focused on immunosenescence, vitamin D deficiency, and shortened LTL. Of the 3 inflammatory markers, IL-6 and lipocalin-2 (NAGAL) became nonsignificant due to shared variance with frailty, whereas increased hsCRP remained independently associated with mortality. Immunosenescence manifests itself by a decline of B-cell and T-cell function and an impaired response to chronic antigenic stimuli.38 Paradoxically, it creates a condition of chronic low-level inflammation, also called “inflamm-ageing,”38 and is characterized by elevated levels of the inflammatory cytokine IL-6 and the nonspecific acute-phase reactant CRP.39 Both frailty and depression have been associated with higher serum levels of CRP and IL-6,40 albeit frailty more consistently when compared with depression.41 Previously, we have shown that physical frailty is associated with low-grade inflammation in late-life depression.16
We found that shorter LTL was associated with mortality in our sample, independent of lifestyle and somatic disease burden. Telomere length, as a marker of cellular aging, has been associated with increased mortality rates and the onset of various age-related diseases.3 With each cell division some telomeric DNA is lost, leading to apoptosis when a critical length is reached. Next to replication, endogenous factors may also cause telomere shortening, including inflammation, metabolic dysregulation, and oxidative stress.42 These mechanisms become more prominent with chronological aging. Shortened LTL is also consistently associated with depression earlier in life,1 but the association seems to be lost in older age samples.27 Thus far, the limited studies reported only a weak association between telomere length and frailty.17 Nonetheless, LTL and frailty share variance in explaining mortality in our sample.
In our study, higher vitamin D levels were protective for death. One of the key features of frailty, and a potential link with vitamin D deficiency, is the loss of skeletal muscle, or sarcopenia.23 In older persons, a consistent relationship between hypovitaminosis D and muscle dysfunction has been demonstrated, as well as a positive effect of vitamin D supplementation on balance and muscle strength.43 A recent dose-response meta-analysis44 showed an association between low-levels of vitamin D and higher risk for frailty. Although frailty experts consider vitamin D supplements useful for frail persons who are vitamin D deficient,45 intervention studies into the effect of vitamin D supplementation on frailty are currently lacking.46 Previously, we have shown that physical frailty in late-life depression is associated with low vitamin D levels.18 Moreover, low vitamin D levels are consistently associated with (late-life) depression,18 although causality has been questioned and such levels are seen merely as a marker of poor health.15 We found that lower vitamin D has a strong association with mortality in late-life depression, independent of depressive symptom severity and independent of frailty. This finding suggests that randomized controlled trials of vitamin D supplementation in late-life depression may also include mortality as an endpoint in addition to improvement of depressive symptoms.
For proper interpretation, some methodological issues need to be addressed. Strengths of this study include the relatively large sample of patients with a confirmed depressive disorder as well as the comprehensive assessment of depression characteristics and confounding factors. However, some limitations should also be acknowledged. Firstly, the Fried Frailty Phenotype23 has been criticized for taking little account of variables such as cognitive and emotional domains in the older adult. However, using the Fried criteria for studying frailty in a psychiatric sample enables us to disentangle mental disorders, cognitive aging, and physical frailty. Moreover, the frailty phenotype is a well-validated instrument widely used in frailty research.47 Secondly, we did not have access to causes of death. On the one hand, inclusion in the sensitivity analyses of only older adults who deceased from frailty-related causes would have led to more accuracy. On the other hand, even if causes of death are known, it is arbitrary which causes of death should be considered frailty related. Moreover, our sample size was too small to conduct subgroup analyses for patients with specific somatic comorbidity patterns. Therefore, we adjusted all analyses for the number of chronic somatic conditions as a dimensional indicator of multimorbidity and for the number of prescribed drugs as a severity marker of comorbid chronic diseases. Finally, we adjusted only for covariates at baseline, while fluctuations in covariates over time, for example in depressive symptom severity, may additionally impact mortality.
The management of frailty is an important clinical priority, especially for health professionals working with middle-aged and older persons. While frailty has been largely neglected in mental health care, future studies should focus on the clinical implications of frailty across different psychiatric disorders to facilitate the development of interventions to modify frailty and ameliorate its effects in these vulnerable patients. In light of the many mechanisms underlying frailty, we should adopt a wider range of interventions when targeting frailty in late-life depression. Of the mechanisms explored in the present study, shared variance with leukocyte telomere length seems relevant regarding mortality, whereas inflammation and vitamin D seem to have independent effects on the risk of mortality. While the effectiveness of vitamin D supplementation in the treatment of depression is still debated,45,46 one may hypothesize that vitamin D supplementation in late-life depression might be able to prevent adverse health effects like mortality. A recent network analysis48 on interventions for frailty pointed to the importance of physical activity interventions, with nutritional supplementation as most promising.
Since frailty is identifiable in depressed older adults and prospectively associated with mortality independently of the extent of multimorbidity, sociodemographic, and lifestyle characteristics, we hope that our findings will contribute to the evolution of mental health care services to better meet the needs of our increasingly complex patient populations.
Submitted: January 29, 2020; accepted August 24, 2020.
Published online: March 30, 2021.
Potential conflicts of interest: None.
Funding/support: The infrastructure of the Netherlands Study of Depression in Older persons (NESDO) is funded through the Fonds NutsOhra, Stichting tot Steun VCVGZ, NARSAD, The Brain and Behaviour Research Fund, and the participating universities and mental health care organizations (VU University Medical Center, Leiden University Medical Center, University Medical Center Groningen, University Medical Center St Radboud, GGZinGeest, GGNet, GGZ Nijmegen, GGZ Rivierduinen, Lentis, and Parnassia). Assessment of leucocyte telomere length was supported through a ZonMW VICI grant awarded to B.W.H. Penninx, who contributed to the larger NESDO study in which the present study is embedded.
Role of the sponsor: The supporters had no role in the design, analysis, interpretation, or publication of this study.
Clinical Points:
- Physical frailty is increasingly recognized as an important concept for risk stratification in somatic medicine, but largely neglected in mental health care.
- Frailty is associated with increased mortality rates in depressed patients, independent of somatic comorbidity and lifestyle.
- The pathophysiology of frailty may guide development of treatment strategies to lower excess mortality associated with psychiatric disorders.
References (48)

- Verhoeven JE, Révész D, Epel ES, et al. Major depressive disorder and accelerated cellular aging: results from a large psychiatric cohort study. Mol Psychiatry. 2014;19(8):895–901. PubMed CrossRef NLM
- Cuijpers P, Vogelzangs N, Twisk J, et al. Comprehensive meta-analysis of excess mortality in depression in the general community versus patients with specific illnesses. Am J Psychiatry. 2014;171(4):453–462. PubMed CrossRef NLM
- Miloyan B, Fried E. A reassessment of the relationship between depression and all-cause mortality in 3,604,005 participants from 293 studies. World Psychiatry. 2017;16(2):219–220. PubMed CrossRef NLM
- Thombs BD, Ziegelstein RC, Pilote L, et al. Somatic symptom overlap in Beck Depression Inventory-II scores following myocardial infarction. Br J Psychiatry. 2010;197(1):61–66. PubMed CrossRef NLM
- Hoogendijk EO, Afilalo J, Ensrud KE, et al. Frailty: implications for clinical practice and public health. Lancet. 2019;394(10206):1365–1375. PubMed CrossRef NLM
- Dent E, Martin FC, Bergman H, et al. Management of frailty: opportunities, challenges, and future directions. Lancet. 2019;394(10206):1376–1386. PubMed CrossRef NLM
- Almeida OP, Hankey GJ, Yeap BB, et al. Depression, frailty, and all-cause mortality: a cohort study of men older than 75 years. J Am Med Dir Assoc. 2015;16(4):296–300. PubMed CrossRef NLM
- Nguyen QD, Wu C, Odden MC, et al. Multimorbidity patterns, frailty, and survival in community-dwelling older adults. J Gerontol A Biol Sci Med Sci. 2019;74(8):1265–1270. PubMed CrossRef NLM
- Mezuk B, Edwards L, Lohman M, et al. Depression and frailty in later life: a synthetic review. Int J Geriatr Psychiatry. 2012;27(9):879–892. PubMed CrossRef NLM
- Soysal P, Veronese N, Thompson T, et al. Relationship between depression and frailty in older adults: a systematic review and meta-analysis. Ageing Res Rev. 2017;36:78–87. PubMed CrossRef NLM
- Collard RM, Comijs HC, Naarding P, et al. Physical frailty: vulnerability of patients suffering from late-life depression. Aging Ment Health. 2014;18(5):570–578. PubMed CrossRef NLM
- Rozing MP, Veerhuis R, Westendorp RGJ, et al. Inflammation in older subjects with early- and late-onset depression in the NESDO study: a cross-sectional and longitudinal case-only design. Psychoneuroendocrinology. 2019;99:20–27. PubMed CrossRef NLM
- Révész D, Milaneschi Y, Verhoeven JE, et al. Telomere length as a marker of cellular aging is associated with prevalence and progression of metabolic syndrome. J Clin Endocrinol Metab. 2014;99(12):4607–4615. PubMed CrossRef NLM
- Oude Voshaar RC, Derks WJ, Comijs HC, et al. Antidepressants differentially related to 1,25-(OH)2 vitamin D3 and 25-(OH) vitamin D3 in late-life depression. Transl Psychiatry. 2014;4(4):e383. PubMed CrossRef NLM
- van den Berg KS, Marijnissen RM, van den Brink RH, et al. Vitamin D deficiency, depression course and mortality: longitudinal results from the Netherlands Study on Depression in Older persons (NESDO). J Psychosom Res. 2016;83:50–56. PubMed CrossRef NLM
- Arts MHL, Collard RM, Comijs HC, et al. Relationship between physical frailty and low-grade inflammation in late-life depression. J Am Geriatr Soc. 2015;63(8):1652–1657. PubMed CrossRef NLM
- Arts MHL, Collard RM, Comijs HC, et al. Leucocyte telomere length is no molecular marker of physical frailty in late-life depression. Exp Gerontol. 2018;111:229–234. PubMed CrossRef NLM
- van den Berg KS, Arts MHL, van den Brink R, et al. Vitamin D deficiency and course of frailty in a depressed older population. Aging Ment Health. 2018;15:1–7. PubMed NLM
- Benraad CEM, Haaksma ML, Karlietis MHJ, et al. Frailty as a predictor of mortality in older adults within 5 years of psychiatric admission. Int J Geriatr Psychiatry. 2020;35(6):617–625. PubMed CrossRef NLM
- Comijs HC, van Marwijk HW, van der Mast RC, et al. The Netherlands study of depression in older persons (NESDO); a prospective cohort study. BMC Res Notes. 2011;4(1):524. PubMed CrossRef NLM
- Folstein MF, Folstein SE, McHugh PR. “Mini-mental state”: a practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975;12(3):189–198. PubMed CrossRef NLM
- Jeuring HW, Stek ML, Huisman M, et al. A six-year prospective study of the prognosis and predictors in patients with late-life depression. Am J Geriatr Psychiatry. 2018;26(9):985–997. PubMed CrossRef NLM
- Fried LP, Tangen CM, Walston J, et al; Cardiovascular Health Study Collaborative Research Group. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci. 2001;56(3):M146–M156. PubMed CrossRef NLM
- Radloff L. The CES-D scale: A self-report depression scale for research in the general population. Appl Psychol Meas 1977;1:385–401.
- Craig CL, Marshall AL, Sjöström M, et al. International physical activity questionnaire: 12-country reliability and validity. Med Sci Sports Exerc. 2003;35(8):1381–1395. PubMed CrossRef NLM
- Naudé PJ, Eisel UL, Comijs HC, et al. Neutrophil gelatinase-associated lipocalin: a novel inflammatory marker associated with late-life depression. J Psychosom Res. 2013;75(5):444–450. PubMed CrossRef NLM
- Schaakxs R, Verhoeven JE, Oude Voshaar RC, et al. Leukocyte telomere length and late-life depression. Am J Geriatr Psychiatry. 2015;23(4):423–432. PubMed CrossRef NLM
- Babor TF, Kranzler HR, Lauerman RJ. Early detection of harmful alcohol consumption: comparison of clinical, laboratory, and self-report screening procedures. Addict Behav. 1989;14(2):139–157. PubMed CrossRef NLM
- Kriegsman DM, Penninx BW, van Eijk JT, et al. Self-reports and general practitioner information on the presence of chronic diseases in community dwelling elderly. A study on the accuracy of patients’ self-reports and on determinants of inaccuracy. J Clin Epidemiol. 1996;49(12):1407–1417. PubMed CrossRef NLM
- Rush AJ, Giles DE, Schlesser MA, et al. The inventory for depressive symptomatology (IDS): preliminary findings. Psychiatry Res. 1986;18(1):65–87. PubMed CrossRef NLM
- Rush AJ, Gullion CM, Basco MR, et al. The Inventory of Depressive Symptomatology (IDS): psychometric properties. Psychol Med. 1996;26(3):477–486. PubMed CrossRef NLM
- Vermeiren S, Vella-Azzopardi R, Beckwée D, et al; Gerontopole Brussels Study group. Frailty and the Prediction of Negative Health Outcomes: A Meta-Analysis. J Am Med Dir Assoc. 2016;17(12):1163.e1–1163.e17. PubMed CrossRef NLM
- Kojima G, Iliffe S, Walters K. Frailty index as a predictor of mortality: a systematic review and meta-analysis. Age Ageing. 2018;47(2):193–200. PubMed CrossRef NLM
- Cardoso AL, Fernandes A, Aguilar-Pimentel JA, et al. Towards frailty biomarkers: candidates from genes and pathways regulated in aging and age-related diseases. Ageing Res Rev. 2018;47:214–277. PubMed CrossRef NLM
- Searle SD, Mitnitski A, Gahbauer EA, et al. A standard procedure for creating a frailty index. BMC Geriatr. 2008;8(1):24. PubMed CrossRef NLM
- Hanlon P, Nicholl BI, Jani BD, et al. Frailty and pre-frailty in middle-aged and older adults and its association with multimorbidity and mortality: a prospective analysis of 493 737 UK Biobank participants. Lancet Public Health. 2018;3(7):e323–e332. PubMed CrossRef NLM
- Gross AL, Carlson MC, Chu NM, et al. Derivation of a measure of physiological multisystem dysregulation: results from WHAS and health ABC. Mech Ageing Dev. 2020;188:111258. PubMed CrossRef NLM
- Grolleau-Julius A, Ray D, Yung RL. The role of epigenetics in aging and autoimmunity. Clin Rev Allergy Immunol. 2010;39(1):42–50. PubMed CrossRef NLM
- Moshage H. Cytokines and the hepatic acute phase response. J Pathol. 1997;181(3):257–266. PubMed CrossRef NLM
- Howren MB, Lamkin DM, Suls J. Associations of depression with C-reactive protein, IL-1, and IL-6: a meta-analysis. Psychosom Med. 2009;71(2):171–186. PubMed CrossRef NLM
- Soysal P, Stubbs B, Lucato P, et al. Inflammation and frailty in the elderly: a systematic review and meta-analysis. Ageing Res Rev. 2016;31:1–8. PubMed CrossRef NLM
- Garcia-Rizo C, Fernandez-Egea E, Miller BJ, et al. Abnormal glucose tolerance, white blood cell count, and telomere length in newly diagnosed, antidepressant-naïve patients with depression. Brain Behav Immun. 2013;28:49–53. PubMed CrossRef NLM
- Muir SW, Montero-Odasso M. Effect of vitamin D supplementation on muscle strength, gait and balance in older adults: a systematic review and meta-analysis. J Am Geriatr Soc. 2011;59(12):2291–2300. PubMed CrossRef NLM
- Ju SY, Lee JY, Kim DH. Low 25-hydroxyvitamin D levels and the risk of frailty syndrome: a systematic review and dose-response meta-analysis. BMC Geriatr. 2018;18(1):206. PubMed CrossRef NLM
- Morley JE, Vellas B, van Kan GA, et al. Frailty consensus: a call to action. J Am Med Dir Assoc. 2013;14(6):392–397. PubMed CrossRef NLM
- Bruyère O, Cavalier E, Buckinx F, et al. Relevance of vitamin D in the pathogenesis and therapy of frailty. Curr Opin Clin Nutr Metab Care. 2017;20(1):26–29. PubMed CrossRef PubMed CrossRef NLM
- Buta BJ, Walston JD, Godino JG, et al. Frailty assessment instruments: systematic characterization of the uses and contexts of highly-cited instruments. Ageing Res Rev. 2016;26:53–61. PubMed CrossRef NLM
- Negm AM, Kennedy CC, Thabane L, et al. Management of frailty: a systematic review and network meta-analysis of randomized controlled trials. J Am Med Dir Assoc. 2019;20(10):1190–1198. PubMed NLM
This PDF is free for all visitors!