ABSTRACT
Objective: To examine the incremental mental health care resource utilization (MHRU) and barriers to receiving mental health services among adults with a major depressive episode (MDE) and suicidal ideation or behavior with intent.
Methods: Data from adult participants in the 2017 National Survey on Drug Use and Health were used to identify 3 cohorts: MDE (determined by Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition [DSM-5] criteria) with suicidal ideation or behavior with intent (MDSI), MDE, and non-MDE. MHRU and barriers to receiving mental health services were compared among cohorts using logistic regression models.
Results: The MDSI cohort had significantly higher odds (adjusted odds ratio [95% confidence interval]) of receiving mental health–related inpatient care, outpatient care, prescription medications, and any treatment versus the MDE cohort (10.2 [7.1–14.6], 2.4 [1.7–3.4], 2.4 [1.8–3.3], and 2.6 [1.8–3.7], respectively) and the non-MDE cohort (40.3 [27.3–59.5], 20.0 [14.5–27.7], 17.2 [12.9–22.9], and 19.6 [14.1–27.1], respectively). Compared to the MDE cohort, the MDSI cohort was significantly more likely to report barriers to receiving mental health services (2.6 [2.0–3.4]), with the largest differences between cohorts related to fear of negative impact (3.9 [2.8–5.4]). Additionally, 30.6% of the MDSI cohort and 47.0% of the MDE cohort did not receive any mental health treatment in the past year.
Conclusions: Although respondents in the MDSI cohort reported substantially higher MHRU across all categories, they also reported greater barriers to receiving care than those in the MDE cohort. This study documents the extensive burden and unmet need in the MDSI population
J Clin Psychiatry 2021;82(6):20m13842
To cite: Voelker J, Cai Q, Kuvadia H, et al. Mental health care resource utilization and barriers to receiving mental health services among US adults with a major depressive episode and suicidal ideation or behavior with intent. J Clin Psychiatry. 2021;82(6):20m13842.
To share: https://doi.org/10.4088/JCP.20m13842
© Copyright 2021 Physicians Postgraduate Press, Inc.
aJanssen Scientific Affairs, LLC, Titusville, New Jersey
bJanssen Research & Development, LLC, Titusville, New Jersey
cDepartment of Psychiatry, Yale School of Medicine, New Haven, Connecticut
*Corresponding author: Jennifer Voelker, PharmD, MS, Janssen Scientific Affairs, LLC, 1125 Trenton-Harbourton Rd, Titusville, NJ 08560 ([email protected]).
Mood disorders are among the most prevalent mental health conditions, with depression considered the leading cause of disability globally according to the World Health Organization.1,2 In 2018 alone, an estimated 17.7 million adults in the United States (US) had at least 1 major depressive episode (MDE) in the past year, representing approximately 7.2% of the adult population; further, 11.5 million adults had an MDE with severe impairment.3 Some patients with an MDE may have particularly severe symptoms, including suicidal thoughts and behaviors, which increases risk of poor outcomes.4
Depressive symptoms increase the risk of suicide,5 and between 1999 and 2016 the rate of suicide increased in almost every US state.6 The presence of major depressive disorder (MDD) incurs substantial economic burden, a portion of which is attributed to suicide-related costs.7–9 The incremental economic burden of adults with MDD in the US was estimated to be $210.5 billion in 2010, representing an increase of 21.5% from 2005.9 Further, direct medical costs for individuals with MDD were $98.9 billion in 2010, with the majority attributable to outpatient and inpatient medical services ($38.2 and $20.6 billion, respectively) and pharmacy costs ($28.1 billion).9 In the same study, suicide-related costs for individuals with MDD were estimated at $9.7 billion.9
Individuals with severe depression symptoms may not receive mental health treatment.10,11 Barriers to adequate diagnosis and treatment exist worldwide and range from difficulty of access to negative perceptions and fear of community stigma.12–15 Previous studies have found that patients with an MDE and comorbid mental disorders, such as substance use disorders, perceive more unmet need for mental health services than those without such comorbidities.16,17 Additionally, literature supports that patients with an MDE and suicidal ideation may experience additional barriers to mental health treatment, including reluctance to seek treatment because of perceived stigma and associated personal, social, and/or professional discrimination,18,19 and incur greater health care resource use versus their counterparts with an MDE but without suicidal ideation or those without either condition.8,20,21 However, there is no large study in the overall US population that has assessed the perceived barriers to care in MDE with suicidal ideation or behavior with intent or MDE.
Given that the suicide rate has increased nearly 35% in the US during the past 20 years,22 a greater understanding of mental health care resource utilization (MHRU) and barriers to care may facilitate improved access for this vulnerable population. This study aimed to compare MHRU and barriers to receiving mental health services among 3 mutually exclusive cohorts: (1) MDE with suicidal ideation or behavior with intent (MDSI), (2) MDE but without suicidal ideation or behavior, and (3) non-MDE.
METHODS
Study Design and Data Source
Data from the 2017 National Survey on Drug Use and Health (NSDUH) public-use files were used to compare MHRU and barriers to receiving mental health services among study cohorts.23,24 The NSDUH is a nationally representative annual survey sponsored by the Substance Abuse and Mental Health Services Administration that is administered to the civilian non-institutionalized population of the US using computer-assisted interviewing methods. It provides information on alcohol, tobacco, and drug use; mental health; and other health-related issues and includes select questions based on the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5),25 which allows diagnostic criteria to be applied. Households and interview respondents for the NSDUH are randomly selected from each state based on multistage area probability sample design.26 All patient data contained in the NSDUH were deidentified and in compliance with the Health Insurance Portability and Accountability Act. Because this study consisted of secondary data analyses of deidentified patient records, the study was exempt from institutional review board approval.
Study Cohorts
Adult (≥ 18 years of age) survey respondents were categorized into 3 mutually exclusive cohorts (MDSI, MDE, and non-MDE) based on their response to questions in the NSDUH (additional details in Supplementary Table 1). Respondents who reported experiencing at least 5 of the 9 core DSM-525 symptoms of MDD in the prior 12 months, in which at least 1 of these symptoms was depressed mood or loss of interest or pleasure in daily activities, were classified as having experienced past-year MDE.
All adult respondents were asked the first suicide-related question: “Did you seriously think about trying to kill yourself?”; only respondents who responded “yes” were asked 2 additional questions: “Did you make any plans to kill yourself?” (ie, suicide plan) and “Did you try to kill yourself?” (ie, suicide attempt). Respondents who met MDE criteria and responded “yes” to suicide plan and/or suicide attempt were categorized as the MDSI cohort. The MDE cohort consisted of respondents who met criteria for MDE but answered “no” to the first suicide-related question. The non-MDE cohort was defined as respondents who did not meet criteria for MDE and answered “no” to the first suicide-related question.
Outcome Measures
Outcome measures included sociodemographic characteristics, MHRU, and barriers to receiving mental health services. MHRU was measured by responses to yes-or-no questions on receiving any mental health–related inpatient care, outpatient care, and prescription medications. Additionally, receipt of any mental health treatment was a recoded composite variable; respondents were coded as having received any mental health treatment if they had answered “yes” to any of the 3 categories previously described (ie, mental health–related inpatient care, outpatient care, and prescription medications). Barriers to receiving mental health services were derived from respondents who answered “yes” to the question: “During the past 12 months, was there any time when you needed mental health treatment or counseling for yourself but didn’t get it?” Those who answered “yes” were then instructed to select among a list of reasons that explained why they did not receive the mental health treatment or counseling they needed. Barriers to receiving mental health services were evaluated for the 2 cohorts of patients with MDE; the 15 response options were grouped into the following 6 categories: cost, fear of negative impact, minimization of problems, low expectation of treatment benefit, structural barriers, and other reasons.27
Statistical Analysis
Sociodemographic characteristics, MHRU, and barriers to receiving mental health services were estimated based on past-year reports and extrapolated to the US adult population, taking survey sampling weights into account. Sociodemographic characteristics and MHRU were compared for the MDSI cohort versus the MDE cohort and versus the non-MDE cohort. Barriers were compared between the MDSI and MDE cohorts.
Several exploratory and hypothesis-generating analyses were also conducted. As the definition of past-year MDE does not distinguish symptomatic depression versus depression diagnosed by a clinician, a subgroup analysis was conducted to evaluate the rates of MHRU among those who reported that they saw or talked to a mental health professional about their depression. Additionally, in the barriers portion of the NSDUH, the question was structured such that the respondent was asked in a single question if his/her barrier was related to the fear of being committed to a psychiatric hospital or having to take a medication, preventing the ability to determine which specific component was the cause of barrier. To explore which component might be driving the response to this question, a subgroup analysis of MHRU was conducted among those who responded “yes” to this question.
Logistic regressions, using survey logistic procedure, were conducted to assess the impact of MDSI on MHRU and on barriers to receiving mental health services; crude odds ratios (ORs) and adjusted ORs (aORs; adjusted for age, sex, and race) with 95% confidence intervals (CIs) were reported. All analyses were conducted using survey logistic procedures in SAS, version 9.4 (SAS Institute Inc; Cary, North Carolina), while taking into account the complex survey designs of the NSDUH, sampling weights, and clustering effects; differences were considered significant if the P value was less than .05.
RESULTS
Sociodemographic Characteristics
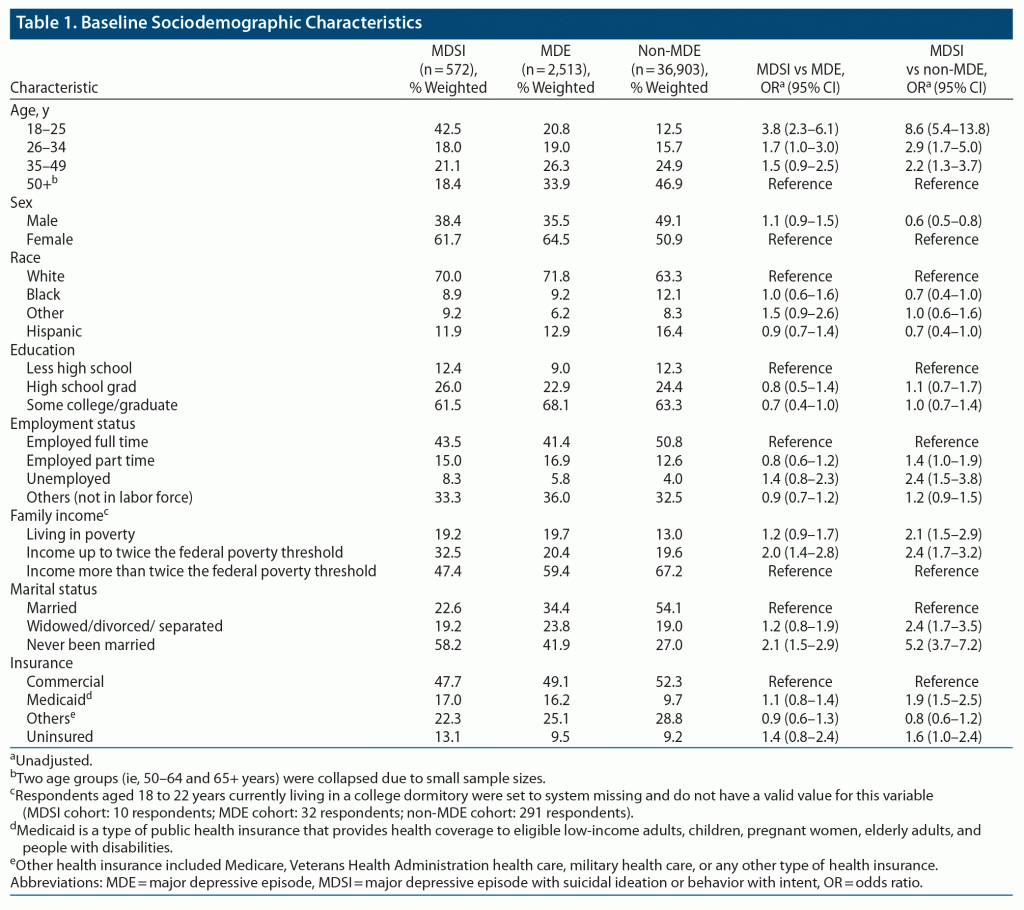
A total of 572 respondents in the MDSI cohort (weighted n = 2,032,663), 2,513 in the MDE cohort (weighted n = 12,053,975), and 36,903 in the non-MDE cohort (weighted n = 221,452,230) were included. Baseline characteristics for the 3 cohorts are presented in Table 1. Respondents in the MDSI cohort were more likely to be younger adults (aged 18–25 years) and never married compared to those in the other 2 cohorts. Those in the MDSI cohort were also more likely to report being unemployed, living in or slightly above the federal poverty threshold, and having Medicaid insurance (a type of public health insurance that provides health coverage to eligible low-income adults, children, pregnant women, elderly adults, and people with disabilities) compared with those in the MDE cohort.
Mental Health Care Resource Utilization
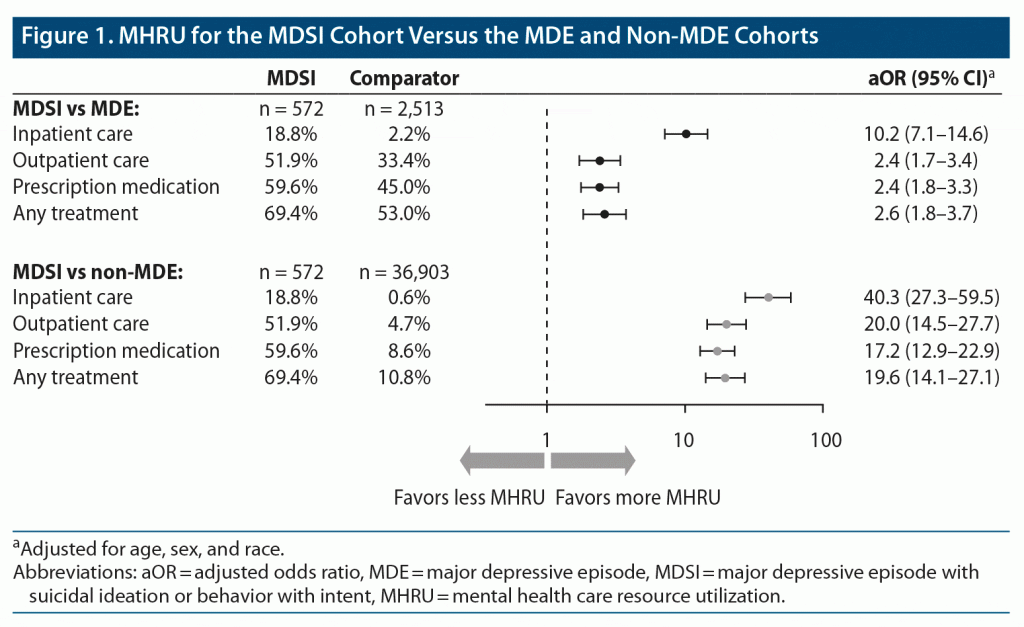
Receipt of any mental health treatment in the past year was more commonly reported among respondents in the MDSI cohort (69.4%) than among those in the MDE cohort (53.0%) and least common among those in the non-MDE cohort (10.8%). After adjusting for age, sex, and race, respondents in the MDSI cohort reported increased odds of using all categories of mental health treatment compared with those in the MDE cohort, including inpatient care (aOR = 10.2; 95% CI, 7.1–14.6), outpatient care (aOR = 2.4; 95% CI, 1.7–3.4), prescription medications (aOR = 2.4; 95% CI, 1.8–3.3), and any mental health treatment (aOR = 2.6; 95% CI, 1.8–3.7; Figure 1). As expected, respondents in the MDSI cohort reported increased odds of MHRU in every category compared with those in the non-MDE cohort, including inpatient care (aOR = 40.3; 95% CI, 27.3–59.5), outpatient care (aOR = 20.0; 95% CI, 14.5–27.7), prescription medications (aOR = 17.2; 95% CI, 12.9–22.9), and any mental health treatment (aOR = 19.6; 95% CI, 14.1–27.1). Unadjusted comparisons for MHRU are reported in Supplementary Table 2.
Notably, although respondents in the MDSI cohort reported increased odds of MHRU compared with respondents in the other cohorts, 30.6% reported not receiving any mental health treatment at all.
In a subgroup analysis of respondents in the MDSI cohort who had seen or spoken with a mental health professional about their depression in the past year (n = 307), MHRU was reported as follows: 28.7% inpatient care, 78.8% outpatient care, 78.3% prescription medication, and 93.3% any mental health treatment.
Barriers to Receiving Mental Health Services
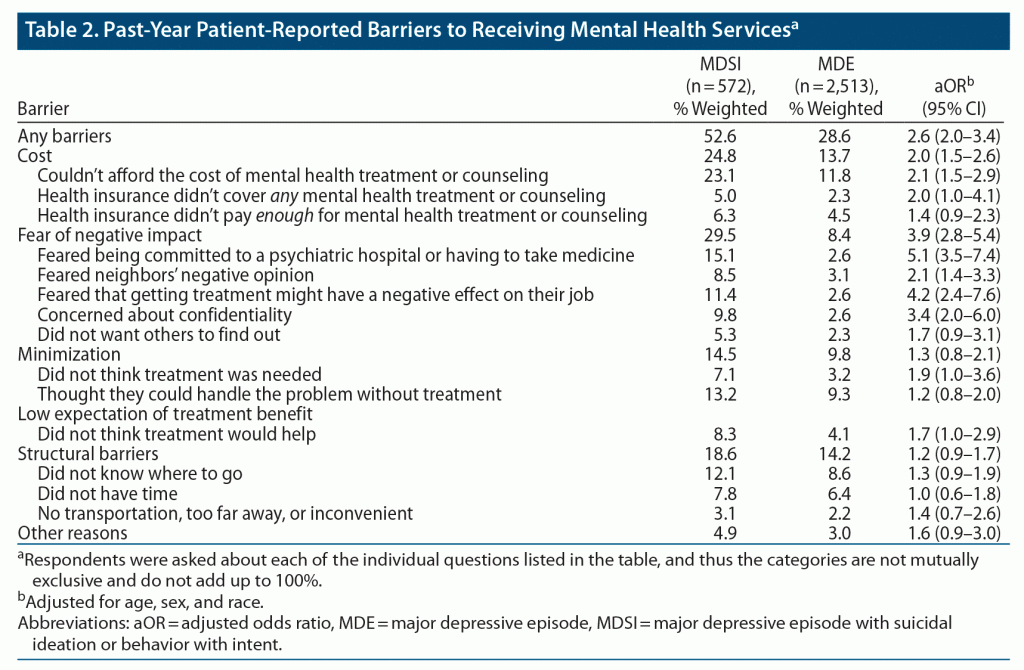
Compared with respondents in the MDE cohort, those in the MDSI cohort were 2.6 times more likely to report experiencing treatment barriers of any category after adjusting for age, sex, and race (Table 2). The largest difference between cohorts was noted in treatment barriers related to fear of negative impact (29.5% vs 8.4%), followed by cost (24.8% vs 13.7%) and low expectation of treatment benefit (8.3% vs 4.1%). Among the 15 individual barriers assessed, the 3 at the greatest increased likelihood all fell in the category of fear of negative impact: fear of being committed to a psychiatric hospital or having to take medicine (aOR = 5.1; 95% CI, 3.5–7.4), fear that getting treatment might have a negative effect on their job (aOR = 4.2; 95% CI, 2.4–7.6), and concerns about confidentiality (aOR = 3.4; 95% CI, 2.0–6.0). Unadjusted ORs are presented in Supplementary Table 3.
In a subgroup analysis of respondents in the MDSI cohort who reported fear of being committed to a psychiatric hospital or having to take medicine, the proportion who reported taking prescription medications (61.4%) was much higher than the proportion who reported past-year inpatient mental health care (16.5%).
DISCUSSION
According to nationally representative data from the NSDUH, respondents in the MDSI cohort reported significantly higher levels of MHRU than those in the MDE cohort. This study underscores the substantial MHRU burden and barriers to receiving mental health services among adult patients with MDSIestablished that not only do these patients incur greater MHRU compared with those with an MDE alone, but their current level of care often does not adequately meet their needs. These findings are further strengthened by the national-level data and ability to evaluate resource use among both individuals with insurance who are interacting with the health care system and those without insurance and who may not routinely receive medical care.
Most notably, respondents in the MDSI cohort were approximately 10 times more likely to report use of inpatient mental health services than those in the MDE cohort after adjusting for age, sex, and race. Similar findings were shown in previous literature in populations outside the US. A cross-European observational study8 showed that, among patients with MDD, those reporting suicidal ideation had higher numbers of health care professional visits, general/family practitioner visits, hospitalizations, and emergency department visits compared to patients with MDD but without suicidal ideation. The present study is unique in that the database captured the reported experience of those who may not be interacting with the health care system in a large representative sample of the US population, in contrast to much of the available literature, which examines the experience of patients when they present to the emergency department or other hospital locations.28–34
In the present study, approximately one-third of respondents in the MDSI cohort did not receive any mental health treatment in the past year and approximately 50% reported at least 1 barrier to receiving mental health services. Other studies have corroborated that a large proportion of patients with an MDE or suicidal ideation do not receive adequate treatment. Similar to the current findings, a prior study analyzing national NSDUH data from 2008 to 201211 reported that more than 30% of participants who made suicide plans and/or attempted suicide received no mental health treatment before or after planning or attempting suicide. Another study35 reported that individuals who perceive that they have an unmet need for mental health services have a greater likelihood of reporting suicidal ideation and suicide attempt. These findings reiterate the need to make adjustments to the health care system such that these unmet needs may be better addressed.
Coupled with greater MHRU, respondents in the MDSI cohort were nearly 3 times more likely to report barriers to receiving mental health services compared with respondents in the MDE cohort. The most prevalently reported barriers among patients in the MDSI cohort were in the categories of fear of negative impact and cost (reported by 29.5% and 24.8% of respondents, respectively). In addition to being the most commonly reported category of barrier in the MDSI cohort, fear of negative impact was also the most likely to occur in the MDSI versus MDE cohorts (aOR = 3.9). The most impactful barriers associated with MDSI were found among this category and were the following: fear of being committed to a psychiatric hospital or having to take medicine, fear that getting treatment might have a negative effect on their job, and concerns about confidentiality. In a recently published study, Richards et al36 used health record data from Kaiser Permanente Washington to identify patients with a suicide attempt who had not previously reported suicidal ideation; these patients said they did not report it at the time due to fears of stigma, health care provider overreaction and potential loss of confidentially, and loss of autonomy in the form of psychiatric hospitalization. Similarly, in the NSDUH, “fear of being committed to a psychiatric hospital or having to take medicine” represented the barrier at greatest increased likelihood in the MDSI cohort compared with the MDE cohort (aOR = 5.1). Among respondents in the MDSI cohort who endorsed this barrier, prescription use was much more common than inpatient care (61.4% reported taking prescription medications vs 16.5% reported receiving inpatient mental health care in the past year), which suggests concerns over psychiatric hospitalization disproportionately drive this barrier. Future iterations of the NSDUH could consider splitting this topic into 2 questions so researchers could better ascertain the reasons behind unmet need. Further, the NSDUH does not currently differentiate between voluntary or involuntary prior hospitalization. Because patient perspective can be strongly influenced by their prior experience and the nature of prior hospitalization,37,38 future iterations of the NSDUH should consider evaluating this distinction.
The use of a nationally representative database ensures the inclusion of people in the US regardless of insurance status and allows broad implications to be drawn from this study. In most cases, the most significant barrier to seeking care was fear of negative impact and stigma associated with MHRU; cost was the next most significant barrier. These barriers were more highly endorsed among vulnerable populations within the MDSI cohort, which may indicate a greater reluctance to seek treatment and explain why the suicide rate was higher among those who reported living in poverty, being unemployed, and having Medicaid.
Although 19% of respondents with MDSI had an inpatient stay in the last year, many more likely had such experiences in previous years.38 Studies have shown that perceived coercion into psychiatric hospitalization may be associated with poor outcomes following discharge, including suicide attempts37; thus, efforts to improve quality of care and mitigate the stigma and repercussions around seeking and using care are critical for this vulnerable population.
The current study findings echo previous data18,39 indicating that fear of employers finding out is a leading barrier to seeking help for those with MDSI. Some employer groups have become increasingly interested in providing better mental health care for employees.40,41 Findings from this study suggest that employers can work to remove the stigma or fear of negative impact associated with seeking treatment for MDE, improve confidentiality, and make treatment options more affordable. Likewise, private insurance and government policymakers could make treatments more affordable by reducing cost share burden and out-of-pocket expenses. Additionally, they could implement additional quality measures and reimbursement incentives among providers to screen for depression in primary care settings and provide more educational resources to their members about where and how to receive mental health care. These steps would continue to build on existing mental health parity laws aiming to improve the care of those with serious mental illness.
Results of this study should be interpreted cautiously given some limitations. Data are self-reported and do not contain comprehensive details such as diagnosis or procedure codes. Specifically, the analysis did not differentiate which respondents were diagnosed with an MDE by a health care professional, as the survey included all those who met DSM-5 criteria for an MDE. The accuracy of data collected depends on respondents’ memory and how they interpreted the questions as they pertained to their specific experience and health literacy, so the data are subject to misclassification and recall bias. However, the anonymous computerized survey method may allow for honest reporting by reducing worries about the perceived stigma associated with patients’ conditions. This is an important strength of this study, as suicidal thoughts and behavior are often underreported.42,43 Barriers to receiving mental health services are unlikely to be inclusive of all possible reasons for barriers because respondents were limited by the structured questionnaire. Additionally, the database lacked information on how often and how many times the reported barrier prevented patients from seeking care; thus, the size of the unmet treatment need is unknown, and ultimately the majority of patients with MDSI did receive some form of mental health care. Further, the NSDUH does not include questions that would allow DSM-5 diagnostic criteria to categorize respondents with other mental health conditions, such as anxiety disorder, schizophrenia, and personality disorders. Thus, although we cannot ascertain the prevalence of other types of mental health disorders among the non-MDE cohort, presumably some respondents had mental health conditions, as 10.8% reported receiving mental health treatment (Supplementary Table 2).
The strengths of this study include its use of a nationally representative database instead of traditional health care databases, which may contain only insurance claims or rely on diagnosis codes for suicidal ideation and suicidal behavior. Use of this database afforded the ability to capture co-occurring MDE and suicidal behavior with intent and to include participants regardless of insurance status and health care access. An analysis of the national survey data ensures the inclusion of people in the US regardless of their insurance status and contributes to a generalizable view of barriers among individuals inside and outside the health care system.
CONCLUSION
Respondents in the MDSI cohort reported significantly higher MHRU than those in the MDE cohort, but in turn were nearly 3 times as likely to report barriers to mental health services, particularly related to stigma or fear of negative impact. These results underscore the substantial unmet health care needs that exist for individuals with an MDE and suicidal ideation and behaviors with intent.
Submitted: January 8, 2021; accepted April 4, 2021.
Published online: September 14, 2021.
Potential conflicts of interest: Drs Voelker, Daly, Pesa, and Sheehan and Mss Cai, Kuvadia, and Connolly are employees of Janssen and may be stockholders in Johnson & Johnson. Dr Wilkinson has received funding for the conduct of clinical trials administered through Yale University from Janssen, Sage Therapeutics, and Oui Therapeutics and has also received consulting fees from Janssen, Biohaven, Sage Therapeutics, and Oui Therapeutics.
Funding/support: This study was sponsored by Janssen Scientific Affairs, LLC, Titusville, NJ.
Role of the sponsor: The sponsor was involved in the study design; management, analysis, and interpretation of the data; and preparation, review, and approval of the manuscript.
Previous presentation: Presented, in part, at the 32nd Annual Psych Congress; October 3–6, 2019; San Diego, California • American Society of Clinical Psychopharmacology (ASCP) 2020 Annual Meeting; May 29–30, 2020 (virtual conference).
Acknowledgments: Medical writing support was provided by Courtney St. Amour, PhD, of Cello Health Communications/MedErgy, and was funded by Janssen Scientific Affairs, LLC.
Supplementary material: Available at Psychiatrist.com.
Clinical Points
- Mental health care resource utilization (MHRU) and barriers to receiving mental health services among adults with a major depressive episode (MDE) and suicidal ideation or behaviors with intent (MDSI) are understudied.
- MHRU and barriers to care were higher for patients with MDSI compared with the MDE cohort.
- This study documents the extensive burden and unmet need among the MDSI population.
References (43)

- GBD 2017 Disease and Injury Incidence and Prevalence Collaborators. Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet. 2018;392(10159):1789–1858. PubMed CrossRef
- World Health Organization. Depression and Other Common Mental Disorders. Global Health Estimates. Geneva, Switzerland: WHO Document Production Services; 2017.
- Key Substance Use and Mental Health Indicators in the United States: Results from the 2018 National Survey on Drug Use and Health. 2019. HHS Publication No. PEP19-5068, NSDUH Series H-54. Center for Behavioral Health Statistics and Quality, Substance Abuse and Mental Health Services Administration. Accessed August 10, 2020. https://www.samhsa.gov/data/sites/default/files/cbhsq-reports/NSDUHNationalFindingsReport2018/NSDUHNationalFindingsReport2018.pdf
- Nock MK, Borges G, Bromet EJ, et al. Suicide and suicidal behavior. Epidemiol Rev. 2008;30(1):133–154. PubMed CrossRef
- Sokero TP, Melartin TK, Rytsälä HJ, et al. Prospective study of risk factors for attempted suicide among patients with DSM-IV major depressive disorder. Br J Psychiatry. 2005;186(4):314–318. PubMed CrossRef
- Suicide rising across the US. CDC Vital Signs. June 2018. Accessed August 16, 2020. https://www.cdc.gov/vitalsigns/pdf/vs-0618-suicide-H.pdf
- Gauthier G, Guérin A, Zhdanava M, et al. Treatment patterns, healthcare resource utilization, and costs following first-line antidepressant treatment in major depressive disorder: a retrospective US claims database analysis. BMC Psychiatry. 2017;17(1):222. PubMed CrossRef
- Jaffe DH, Rive B, Denee TR. The burden of suicidal ideation across Europe: a cross-sectional survey in five countries. Neuropsychiatr Dis Treat. 2019;15:2257–2271. PubMed CrossRef
- Greenberg PE, Fournier AA, Sisitsky T, et al. The economic burden of adults with major depressive disorder in the United States (2005 and 2010). J Clin Psychiatry. 2015;76(2):155–162. PubMed CrossRef
- Thornicroft G, Chatterji S, Evans-Lacko S, et al. Undertreatment of people with major depressive disorder in 21 countries. Br J Psychiatry. 2017;210(2):119–124. PubMed CrossRef
- Choi NG, DiNitto DM, Marti CN. Mental health treatment use and perceived treatment need among suicide planners and attempters in the United States: between and within group differences. BMC Res Notes. 2015;8(1):305. PubMed CrossRef
- Sun Y, Chen G, Wang L, et al. Perception of stigma and its associated factors among patients with major depressive disorder: a multicenter survey from an Asian population. Front Psychiatry. 2019;10:321. PubMed CrossRef
- Beaulieu T, Ti L, Milloy MJ, et al. Major depressive disorder and access to health services among people who use illicit drugs in Vancouver, Canada. Subst Abuse Treat Prev Policy. 2018;13(1):3. PubMed CrossRef
- Yucel A, Essien EJ, Sanyal S, et al. Racial/ethnic differences in the treatment of adolescent major depressive disorders (MDD) across healthcare providers participating in the Medicaid program. J Affect Disord. 2018;235:155–161. PubMed CrossRef
- Unützer J, Park M. Strategies to improve the management of depression in primary care. Prim Care. 2012;39(2):415–431. PubMed CrossRef
- Chen LY, Crum RM, Martins SS, et al. Service use and barriers to mental health care among adults with major depression and comorbid substance dependence. Psychiatr Serv. 2013;64(9):863–870. PubMed CrossRef
- Urbanoski KA, Cairney J, Bassani DG, et al. Perceived unmet need for mental health care for Canadians with co-occurring mental and substance use disorders. Psychiatr Serv. 2008;59(3):283–289. PubMed CrossRef
- Sheehan L, Dubke R, Corrigan PW. The specificity of public stigma: a comparison of suicide and depression-related stigma. Psychiatry Res. 2017;256:40–45. PubMed CrossRef
- Wimsatt LA, Schwenk TL, Sen A. Predictors of depression stigma in medical students: potential targets for prevention and education. Am J Prev Med. 2015;49(5):703–714. PubMed CrossRef
- Stringer B, van Meijel B, Eikelenboom M, et al. Perceived need for care and health care utilization among depressed and anxious patients with and without suicidal ideation. Crisis. 2013;34(3):192–199. PubMed CrossRef
- Benson C, Singer D, Carpinella CM, et al. The health-related quality of life, work productivity, healthcare resource utilization, and economic burden associated with levels of suicidal ideation among patients self-reporting moderately severe or severe major depressive disorder in a national survey. Neuropsychiatr Dis Treat. 2021;17:111–123. PubMed CrossRef
- Hedegaard H, Curtin SC, Warner M. Increase in suicide mortality in the United States, 1999–2018. NCHS Data Brief. 2020;(362):1–8. PubMed
- Substance Abuse and Mental Health Data Archive. Substance Abuse and Mental Health Services Administration. Accessed August 16, 2020. https://www.samhsa.gov/data/
- Center for Behavioral Health Statistics and Quality. 2017 National Survey on Drug Use and Health Public Use File Codebook. Substance Abuse and Mental Health Services Administration. Accessed August 10, 2020. https://samhda.s3-us-gov-west-1.amazonaws.com/s3fs-public/field-uploads-protected/studies/NSDUH-2017/NSDUH-2017-datasets/NSDUH-2017-DS0001/NSDUH-2017-DS0001-info/NSDUH-2017-DS0001-info-codebook.pdf
- American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fifth Edition. Washington, DC: American Pychiatric Association; 2013.
- 2017 National Survey on Drug Use and Health: Methodological Summary and Definitions. Substance Abuse and Mental Health Services Administration. 2018. Accessed March 7, 2021. https://www.samhsa.gov/data/sites/default/files/cbhsq-reports/NSDUHMethodSummDefs2017/NSDUHMethodSummDefs2017.htm
- Alang SM. Sociodemographic disparities associated with perceived causes of unmet need for mental health care. Psychiatr Rehabil J. 2015;38(4):293–299. PubMed CrossRef
- Betz ME, Wintersteen M, Boudreaux ED, et al. Reducing suicide risk: challenges and opportunities in the emergency department. Ann Emerg Med. 2016;68(6):758–765. PubMed CrossRef
- Bridge JA, Olfson M, Caterino JM, et al. Emergency department management of deliberate self-harm: a national survey. JAMA Psychiatry. 2019;76(6):652–654. PubMed CrossRef
- Canner JK, Giuliano K, Selvarajah S, et al. Emergency department visits for attempted suicide and self harm in the USA: 2006–2013. Epidemiol Psychiatr Sci. 2018;27(1):94–102. PubMed CrossRef
- Chang BP, Tezanos K, Gratch I, et al. Depressed and suicidal patients in the emergency department: an evidence-based approach. Emerg Med Pract. 2019;21(5):1–24. PubMed
- Dold M, Bartova L, Fugger G, et al. Major depression and the degree of suicidality: results of the European Group for the Study of Resistant Depression (GSRD). Int J Neuropsychopharmacol. 2018;21(6):539–549. PubMed CrossRef
- Doshi A, Boudreaux ED, Wang N, et al. National study of US emergency department visits for attempted suicide and self-inflicted injury, 1997–2001. Ann Emerg Med. 2005;46(4):369–375. PubMed CrossRef
- Goldberg JF, Ernst CL, Bird S. Predicting hospitalization versus discharge of suicidal patients presenting to a psychiatric emergency service. Psychiatr Serv. 2007;58(4):561–565. PubMed CrossRef
- Ali MM, Lackey S, Mutter R, et al. The relationship between perceived unmet mental health care needs and suicidal ideation and attempt. Adm Policy Ment Health. 2018;45(5):709–715. PubMed CrossRef
- Richards JE, Whiteside U, Ludman EJ, et al. Understanding why patients may not report suicidal ideation at a health care visit prior to a suicide attempt: a qualitative study. Psychiatr Serv. 2019;70(1):40–45. PubMed CrossRef
- Jordan JT, McNiel DE. Perceived coercion during admission into psychiatric hospitalization increases risk of suicide attempts after discharge. Suicide Life Threat Behav. 2020;50(1):180–188. PubMed CrossRef
- Mitchell AM, Garand L, Dean D, et al. Suicide assessment in hospital emergency departments: implications for patient satisfaction and compliance. Top Emerg Med. 2005;27(4):302–312. PubMed
- Schwenk TL, Davis L, Wimsatt LA. Depression, stigma, and suicidal ideation in medical students. JAMA. 2010;304(11):1181–1190. PubMed CrossRef
- Psychologically healthy workplace awards 2019. American Psychological Association. Accessed March 9, 2021. https://www.apa.org/applied-psychology/psychologically-healthy-workplaces-2019.pdf
- TiER1 Performance Solutions. American Psychiatric Association, Center for Workplace Mental Health. Accessed March 9, 2021. https://workplacementalhealth.org/Case-Studies/Tier1PerformanceSolutions
- Anestis MD, Mohn RS, Dorminey JW, et al. Detecting potential underreporting of suicide ideation among US military personnel. Suicide Life Threat Behav. 2019;49(1):210–220. PubMed CrossRef
- Pritchard C, Hansen L. Examining undetermined and accidental deaths as source of ‘under-reported-suicide’ by age and sex in twenty Western countries. Community Ment Health J. 2015;51(3):365–376. PubMed CrossRef
This PDF is free for all visitors!