ABSTRACT
Objective: Suicidal ideation or behavior (SIB) is a symptom of major depressive disorder (MDD). This study evaluated health care resource utilization (HRU) and costs of commercially insured adults who had diagnosed MDD with acute SIB (MDSI).
Methods: Adults with MDSI (index date: first SIB claim) and controls without MDD or suicide-related claims (random index date) were identified using International Classification of Diseases, Clinical Modification, 10th Revision codes in the OptumHealth Care Solutions, Inc. database (October 2014 to March 2017). Adults with < 12 months of plan enrollment pre-index and/or selected psychiatric comorbidities were excluded. MDSI and control cohorts were matched 1:1 on demographics and comorbidities. HRU and costs were compared between matched cohorts during up to 1 and 12 months post-index (inclusive) using regressions adjusted for baseline costs.
Results: Among patients with MDSI (n = 1,576, mean age = 34 years, 55.6% female), most index events occurred in emergency department (ED; 50.7%) and inpatient (45.2%) settings. The MDSI cohort, compared with the control cohort within 1 and 12 months post-index, respectively, had 157.7 and 28.0 times more inpatient admissions, 16.4 and 5.4 times more ED visits, and 4.9 and 3.2 times more outpatient visits (all P < .01). Incremental health care costs per patient per month in the MDSI compared with the control cohort within 1 and 12 months were $7,839 and $2,757, respectively (both P values < .01). Inpatient and ED costs constituted 70.6% and 16.5% of the total incremental costs, respectively, within the first month of follow-up.
Conclusions: Among commercially insured adults, MDSI was associated with significant economic burden; inpatient and ED services drove incremental costs of the condition. Further assessment of treatment options for this vulnerable patient population is warranted.
J Clin Psychiatry 2022;83(3):21m14090
To cite: Pilon D, Neslusan C, Zhdanava M, et al. Economic burden of commercially insured patients with major depressive disorder and acute suicidal ideation or behavior in the United States. J Clin Psychiatry. 2022;83(3):21m14090.
To share: https://doi.org/10.4088/JCP.21m14090
© Copyright 2022 Physicians Postgraduate Press, Inc.
aAnalyses Group, Inc., Montréal, QC, Canada
bJanssen Scientific Affairs, LLC, Titusville, New Jersey
cAnalysis Group, Inc., Boston, Massachusetts
*Corresponding author: Masha (Maryia) Zhdanava, MA, Analysis Group, Inc, 1190 avenue des Canadiens-de-Montréal, Deloitte Tower, Ste 1500, Montreal, QC, H3B 0G7 ([email protected]).
Major depressive disorder (MDD) is a recurrent psychiatric illness with an estimated 12-month prevalence of 7.8% in 2019.1 MDD has detrimental consequences on the lives of affected individuals, with approximately 80% of them experiencing difficulties with work, home activities, or social activities as a result of the condition.2,3 In 2016, MDD was the second leading condition contributing to years lived with disability and the ninth leading condition contributing to disability-adjusted life-years in the US.4
MDD is a risk factor for suicide.5 Approximately half of those who attempt suicide have an MDD diagnosis,6 and nearly a third of suicide decedents exhibit depressive symptoms.7 The risk of suicide attempt is particularly high during major depressive episodes (MDEs): there is a 21-fold increase in the risk of suicide during MDEs relative to periods of remission.8 Among adults with an MDE in the past year, based on self-report, 32.1% had suicidal ideation, 11.8% made suicide plans, and 4.3% attempted suicide according to the 2019 National Survey on Drug Use and Health.1
The national cost of officially reported suicide and suicide attempt was estimated at $58.4 billion in 2013, and this figure increased to $93.5 billion after adjusting for suicide event underreporting.9 Acute suicidal ideation or behavior (SIB) that accompanies MDD may be associated with a substantial economic burden. However, limited data exist on the health care resource utilization (HRU) and costs of patients diagnosed with MDD and with acute SIB (MDSI). To understand the unmet needs and to improve care for this vulnerable population, an analysis of the economic burden of the condition is warranted. As the majority of the US population (68.0%) has commercial insurance,10 and SIB has a high prevalence and is increasing rapidly among younger adults,1,11–13 our study sought to compare HRU and costs in commercially insured adult employees and family beneficiaries with MDSI versus those without either MDD or SIB.
METHODS
Data Source
The OptumHealth Care Solutions, Inc. insurance claims database was used (data from October 1, 2014, to March 31, 2017). This database contains information on 19.9 million commercially insured beneficiaries nationwide, including claimant demographics, insurance eligibility, and medical and prescription drug claims. Beneficiaries are employees or dependents covered by select Fortune 500 self-insured private payers. The data are available from OptumHealth Care Solutions, Inc., but restrictions apply to the availability of these data, which were used under license for the current study and are not publicly available. The database contains only deidentified information and fully complies with the patient confidentiality requirements of the Health Insurance Portability and Affordability Act (HIPAA). No ethics board review was required.
Study Design
A retrospective matched cohort study design was used. Two cohorts of patients were analyzed: the MDSI cohort and the cohort of patients without either an MDD or an SIB diagnosis (non-MDD cohort).
The study period spanned from October 1, 2014 (12 months before the beginning of the index window), to March 31, 2017 (end of available data). The index window was set to begin on October 1, 2015, the date of the introduction of the International Classification of Diseases, 10th Revision, Clinical Modification (ICD-10-CM) coding system, since relative to its predecessor, the ICD-9-CM coding system, it permits a more accurate identification of nonfatal suicide attempts and intentional self-harm in claims data.14 Furthermore, ICD-9-CM codes identify SIB events exclusively by external cause codes, but in ICD-10-CM some SIB events have diagnosis codes, required by federal mandates for claims reimbursement.14
For those included in the MDSI cohort, the index date was defined as the date of the first claim with a code for suicide attempt or a code for suicidal ideation. For those included in the non-MDD cohort, the index date was randomly generated to mimic the distribution of time from the study period start to the index date in the MDSI cohort. Patient characteristics were evaluated during the 12-month baseline period preceding the index date. The follow-up period spanned from the index date until the end of continuous eligibility or data availability, and outcomes were described and compared during (1) up to 1 month and (2) up to 12 months of follow-up to evaluate both the short-term/acute and longer-term outcomes associated with the SIB event.
Study Population
Patients were included in the MDSI cohort if they met the following criteria: (1) ≥ 1 claim with a diagnosis of MDD (ICD-9-CM: 296.2, 296.3; ICD-10-CM: F32 [excluding F32.8], F33 [excluding F33.8]) during the study period (October 1, 2014, to March 31, 2017); (2) ≥ 1 claim with a code for a suicidal ideation or attempt; the latter was defined based on the guidance from the Centers for Disease Control and Prevention,14 with an added criterion that patients with an intentional self-harm code must have an accompanying suicidal ideation code (ICD-10-CM: R45.851) within 30 days (see Table 1 for the list of codes); (3) ≥ 1 claim with a diagnosis of depression (ICD-9-CM: 296.2, 296.3, 300.4, 311, 309.0, 309.1; ICD-10-CM: F32, F33, F34.1, F43.21) during the baseline period or on the index date. Patients were included in the non-MDD cohort if they had (1) no claims with a diagnosis of MDD and (2) no claims with a code for SIB during the study period.
Besides the aforementioned criteria, patients included in the MDSI and non-MDD cohorts were additionally required to meet the following criteria: (1) no claims with a diagnosis of specific psychiatric comorbidities, including bipolar disorder and related conditions, cluster B personality disorder, dementia, intellectual disability, schizophrenia and other non-mood psychotic disorders, and substance-induced mood disorder (see Supplementary Table 1 for the list of codes); (2) no Medicare coverage during continuous insurance eligibility; (3) ≥ 12 months of continuous insurance eligibility prior to the index date; and (4) 18–64 years of age at the index date. Given the fluidity of mental health diagnoses and shared symptoms across psychiatric conditions, patients with certain psychiatric conditions were excluded from the study to minimize the possibility of MDD misidentification. This study focused on commercially insured adults of working age; private payer costs of adults aged 65 and older may be incomplete due to Medicare’s covering service costs.
Outcome Measures
Use of MDD-related therapies and evaluations was reported and included use of antidepressants, antidepressant augmentation therapy (ie, anticonvulsants, buspirone, lithium, psychostimulants, select atypical antipsychotics and thyroid hormones [T3]), psychotherapy, and psychiatric diagnostic evaluations.
HRU and costs were stratified into all-cause, behavioral and mental health–related, and depression-related. Behavioral and mental health–related HRU and costs were identified based on claims with an ICD-10-CM diagnosis between F01 and F99. Depression-related HRU and costs were defined as claims with an ICD-10-CM diagnosis code among F32.xx, F33.xx, F34.1x, and F43.21.
The following types of health care services were reported: inpatient, outpatient, emergency department (ED), and other services. Total health care costs consisted of medical and pharmacy costs; medical costs included inpatient, outpatient, ED, and other services costs. HRU and cost outcomes were reported per patient per month (PPPM). Costs were expressed in 2017 US dollars and were measured from the payer’s perspective.
Statistical Analysis
Patients in the MDSI cohort were matched 1:1 to patients in the non-MDD cohort using propensity scores. The propensity score was defined as the probability of being in the MDSI cohort and was estimated for each patient using a logistic regression model with the following baseline characteristics as independent variables: age, sex, year of the index date, geographic region, type of health care plan, and score on the Quan-Charlson Comorbidity Index (Quan-CCI), which provides a composite score of mortality risk calculated using diagnosis codes in claims data.15 The balance of baseline characteristics between cohorts after matching was assessed with standardized differences (< 10% indicated balance).16
HRU and cost outcomes during the follow-up period were compared between matched cohorts using regression models adjusted for baseline total health care costs. HRU outcomes were compared using generalized estimating equations (GEEs), to account for matched pairs, with Poisson or binomial distribution. Mean cost differences were estimated using GEEs with normal distribution. Given that cost data do not follow normal distribution (ie, they contain only positive values and a large proportion of zeros), 95% confidence intervals (CIs) and P values were obtained from nonparametric bootstrap procedures with 500 replications.
RESULTS
Baseline Characteristics
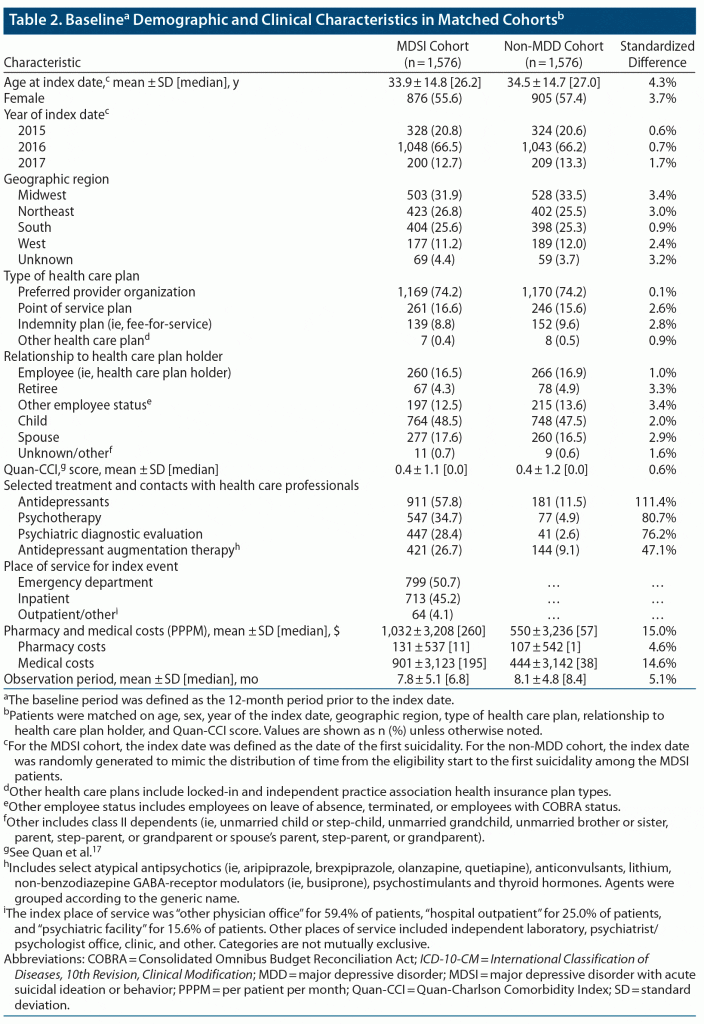
A total of 1,576 patients were included in the MDSI cohort; all were matched 1:1 to the non-MDD cohort (Supplementary Figure 1). The MDSI and non-MDD cohorts were generally well-balanced on demographic characteristics and Quan-CCI scores after matching (Table 2). In the MDSI cohort, mean age was 33.9 years, and 55.6% of patients were female. Almost all index events (95.9%) were identified in a hospital setting (ED: 50.7%; inpatient: 45.2%), and 4.1% were identified in an outpatient setting. During the baseline period, relative to non-MDD controls, more patients in the MDSI cohort received psychiatric diagnostic evaluations (28.4% vs 2.6%), psychotherapy (34.7% vs 4.9%), antidepressants (57.8% vs 11.5%), and antidepressant augmentation therapy (26.7% vs 9.1%). Patients in the MDSI cohort exhibited higher total health care costs than those in the non-MDD cohort (mean: $1,032 vs $550).
Patients were followed for a mean of 7.8 months after the index date in the MDSI cohort and 8.1 months in the non-MDD cohort.
Health Care Resource Utilization
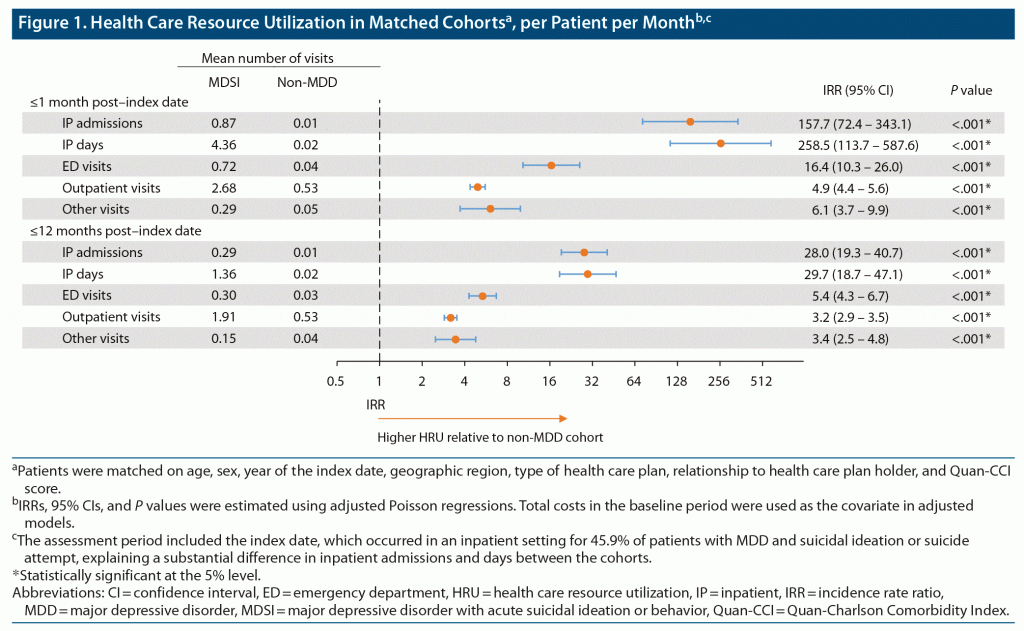
Within the first month post–index date, patients in the MDSI cohort had 157.7 times more inpatient admissions, 258.5 times more inpatient days, 16.4 times more ED visits, 4.9 times more outpatient visits, and 6.1 times more other visits than matched non-MDD controls (all P < .001; Figure 1). The odds of having ≥ 1 all-cause inpatient admission were 472.3 times higher, ≥1 ED visit 45.1 times higher, and ≥ 1 outpatient visit 7.1 times higher among patients with MDSI than among controls without MDD (all P < .001; Supplementary Figure 2A). There were 145 (9.2%) and 1,127 (71.5%) patients in the MDSI and non-MDD cohorts without any inpatient admissions or outpatient visits, respectively (OR [95% CI] = 0.04 [0.03–0.05], P < .001). Similar trends were observed for behavioral and mental health–related HRU and depression-related HRU (Supplementary Table 2).
Within the first 12 months post–index date, patients in the MDSI cohort had 28.0 times more inpatient admissions, 29.7 times more inpatient days, 5.4 times more ED visits, 3.2 times more outpatient visits, and 3.4 times more other visits than matched non-MDD controls (all P < .001; Figure 1). Relative to non-MDD controls, patients in the MDSI cohort had 3.6 times higher odds of having ≥ 1 all-cause outpatient visit, 80.2 times higher odds of having ≥ 1 all-cause inpatient admission, and 10.1 times higher odds of having ≥ 1 ED visit (all P < .001; Supplementary Figure 2B). There were 69 (4.4%) and 523 (33.2%) patients in the MDSI and non-MDD cohorts without any inpatient admissions or outpatient visits, respectively (OR [95% CI] = 0.10 [0.08–0.13], P < .001). These trends were preserved when evaluating behavioral and mental health–related HRU and depression-related HRU (Supplementary Table 2).
Health Care Costs
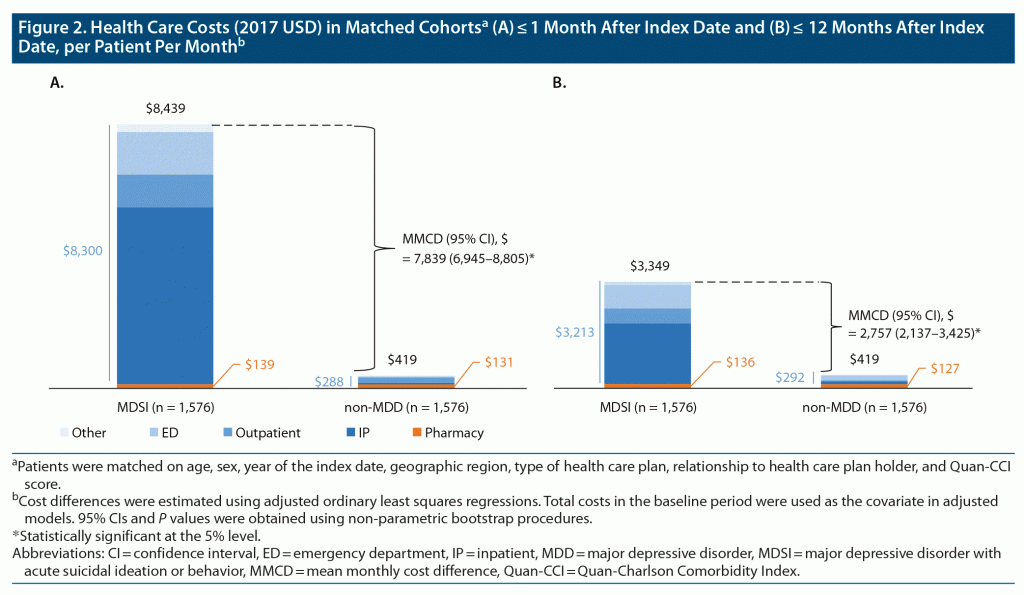
Within the first month of follow-up, patients with MDSI relative to controls incurred $7,839 higher health care costs PPPM (P < .001; Figure 2A). This difference was predominantly driven by higher inpatient (cost difference = $5,532) and ED (cost difference = $1,292; all P < .001) costs.
Within the first 12 months of follow-up, patients with MDSI relative to controls incurred $2,757 higher health care costs PPPM (P < .001; Figure 2B). The main drivers of this cost difference were greater inpatient (mean cost difference = $1,750), outpatient (mean cost difference = $512), and ED (mean cost difference = $434; all P < .001) costs.
Mean monthly behavioral and mental health–related costs constituted 66.6% and 53.3% of the mean monthly total health care costs of patients with MDSI within the first month and within the first 12 months. Mean monthly depression-related costs constituted 52.8% and 39.5%, respectively (Supplementary Table 3).
Use of MDD-Related Therapies
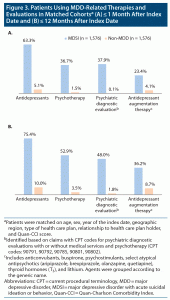
Within the first month and within the first 12 months post-index, respectively, 63.3% and 75.4% of patients in the MDSI cohort used antidepressants, 36.7% and 52.9% received psychotherapy, 37.9% and 48.0% received psychiatric diagnostic evaluation, and 23.4% and 36.2% used antidepressant augmentation therapy (Figure 3). The use of MDD-related therapies and evaluations, as expected, was consistently lower in the non-MDD cohort.
Within the first month post-index, there were 264 (16.8%) and 1,408 (89.3%) patients in the MDSI and non-MDD cohorts, respectively, without pharmacologic or non-pharmacologic therapy or mental health evaluations (ie, none of these treatment modalities). Within the first 12 months, these numbers were 172 (10.9%) and 1,252 (79.4%) in the MDSI and non-MDD cohorts, respectively.
DISCUSSION
To the best of our knowledge, this study is the first to evaluate the economic burden of patients with MDSI. In this study, most index events occurred in a hospital setting, reflecting acute care required for patients at imminent risk of suicide. Given this finding, substantially higher health care costs incurred in the MDSI cohort relative to the non-MDD cohort, particularly in the first month after the SIB event, are not surprising. Nonetheless, these costs are important to quantify and discuss. In the year preceding the SIB event, nearly half of the MDSI cohort had no evidence of antidepressant use and almost two-thirds no evidence of psychotherapy. Coupled with the fact that the economic burden is concentrated in the provision of acute care, this finding highlights the need for better strategies for the timely identification and treatment of patients with MDD whose symptoms are escalating, as at least in some cases a crisis may be avoided with personalized pharmacologic and non-pharmacologic therapy. Substantial economic burden associated with MDSI persisted in the year following the SIB event. Patients with MDSI incurred total health care costs of $3,349 PPPM during this time. Although this study did not have a control cohort of patients with MDD and without SIB, the aforementioned estimate can be contrasted with an estimate from the literature of $816 PPPM (2015 USD) among a population of patients with MDD initiated on antidepressants.18 This contrast suggests that the majority of the incremental burden associated with MDSI may be attributable to SIB as opposed to MDD.
This study is timely given the emerging evidence of negative effects of the COVID-19 outbreak and the associated social isolation and economic consequences on psychological health.19,20 The situation of at-risk patients could be further exacerbated by the disruption of face-to-face health care.21 As a result, SIB may increase among vulnerable groups22 and strategies for suicide prevention need urgent consideration. While the social stigma related to talking about depression and suicidal ideation is less than in the past, it still exists. Primary health care providers should strive to integrate basic mental health services into outpatient primary care, proactively engage patients in discussions about their mental health, and, as needed, be prepared to screen for and directly discuss suicide risk. Doing so could improve the early identification of at-risk patients and provide an opportunity to propose available treatment options before symptoms escalate and patients present to an inpatient or ED setting for an SIB event. Continuity of care is also critical. In the year following the SIB event, nearly one-quarter of patients with MDSI had no evidence of antidepressant use while nearly half had no evidence of psychotherapy. While the reasons treatment may not have been received are unknown, physicians should strive to implement strategies to ensure patients are periodically reevaluated, treatment options are discussed, and personalized treatment plans are created to mitigate poor outcomes in this complex patient population.
Among adults with an MDE in the past year, based on self-report, 32.1% had suicidal ideation, 11.8% made suicide plans, and 4.3% attempted suicide,1 while in our study, 2% of patients with MDD had a claim for SIB. This gap in reported prevalence of SIB among MDD patients likely supports the assumption that a risk of underreporting of SIB in claims data exists due to stigma, perception of accidental injury, liability concerns, or billing guidelines. Furthermore, our study looked exclusively at beneficiaries with commercial insurance, while the prevalence of SIB may be higher among vulnerable populations, including the uninsured or Medicaid beneficiaries.11 Future studies should assess outcomes among patients with MDD and acute SIB with Medicaid coverage.
Tools, such as the Suicide Intent Scale,23 can be used to measure the seriousness of the intent to die and predict the risk of subsequent suicidal behavior.24 However, this information is not available in health insurance claims, which made it challenging to identify if self-inflicted harm was carried out with an intent to die. This potential limitation was, however, mitigated by requiring that patients with codes of intentional self-harm alone were included only if they had an accompanying diagnosis of suicidal ideation.
The health care costs captured in the present study reflect the private payer’s perspective and do not include patient out-of-pocket and societal costs, such as work productivity loss and costs of caregivers. As the overall economic burden of patients with MDSI extends beyond the direct health care costs reported in the current study, further research is warranted to provide a comprehensive assessment of these additional costs.
Limitations
The present study is subject to some limitations. The study population included patients with commercial insurance, and results may not be generalized to patients with other types of insurance (eg, Medicaid) or the uninsured, who may be more vulnerable and at risk of SIB. Among commercially insured patients, there may be underinsured patients with insufficient funds to cover out-of-pocket costs or copay. Their access to pharmacologic and non-pharmacologic interventions may be limited, contributing to the high share of acute care in the economic burden of MDSI. The study period was narrow, driven by the end of data availability in 2017; future studies with more recent data, including data during the COVID-19 global pandemic, and a broader study population are warranted to confirm and detail our findings. Pharmacy claims data do not account for medication dispensed being taken as prescribed and do not include medications purchased over-the-counter or obtained as samples; thus, the use of MDD-related pharmacologic therapies may be misestimated. Lastly, despite the use of matching and multivariable adjustments, the observational nature of the study makes results vulnerable to unmeasured confounders.
CONCLUSIONS
Acute SIB in patients with MDD carries a significant HRU and cost burden. This burden is driven by acute care for the suicide-related event and persists for up to a year after it. Strategies are needed to improve treatment options and quality of care for patients with MDD whose symptoms escalate.
Submitted: May 14, 2021; accepted January 6, 2022.
Published online: April 4, 2022.
Relevant financial relationships: Mr Pilon, Ms Zhdanava, Ms Morrison, Dr Rossi, Mr Lefebvre, and Mr Greenberg are employees of Analysis Group, Inc., a consulting company that has provided paid consulting services to Janssen Scientific Affairs, LLC (JSA), which funded the development and conduct of this study and manuscript. Drs Neslusan and Sheehan and Ms Joshi are employees of JSA and stockholders of Johnson & Johnson.
Funding/support: This study was funded by Janssen Scientific Affairs, LLC (JSA); Titusville, New Jersey.
Role of the sponsor: JSA participated in designing the study and reviewed the manuscript. Interpretation of the data, drafting of the manuscript, and the decision to submit the manuscript for publication were done by the authors, some of whom are employees of JSA.
Previous presentation: Part of the material in this manuscript was presented at the Academy of Managed Care Pharmacy (AMCP) Nexus 2019 meeting; October 29–November 1, 2019; Gaylord National Harbor, National Harbor, Maryland.
Supplementary material: Available at Psychiatrist.com.
CLINICAL POINTS
- The economic burden of commercially insured patients with major depressive disorder and acute suicidal ideation or behavior (MDSI) is not well documented.
- In this study, patients with MDSI incurred greater health care costs than patients without major depressive disorder; acute care for the suicide-related event drove the incremental costs between cohorts.
- Strategies are needed to identify at-risk patients whose symptoms escalate, as at least in some cases a crisis may be avoided with personalized pharmacologic and non-pharmacologic therapy.
References (24)

- Kaiser Family Foundation. A View from the States: Key Medicaid Policy Changes. KFF website. https://www.kff.org/report-section/a-view-from-the-states-key-medicaid-policy-changes-methods/. 2019. Accessed December 10, 2019.
- National Institute of Mental Health. Major Depression. NIH website. https://www.nimh.nih.gov/health/statistics/major-depression.shtml. Accessed May 13, 2019.
- Centers for Disease Control and Prevention (CDC). Prevalence of Depression Among Adults Aged 20 and Over: United States, 2013–2016. 2018; CDC website. https://www.cdc.gov/nchs/products/databriefs/db303.htm. Accessed May 13, 2019.
- Mokdad AH, Ballestros K, Echko M, et al; US Burden of Disease Collaborators. The state of US health, 1990–2016: burden of diseases, injuries, and risk factors among US states. JAMA. 2018;319(14):1444–1472. PubMed CrossRef
- American Psychiatric Association (APA). Practice Guidelines for the Assessment and Treatment of Patients With Suicidal Behaviors. Psychiatry Online website. https://psychiatryonline.org/pb/assets/raw/sitewide/practice_guidelines/guidelines/suicide.pdf. 2010. Accessed December 13, 2019.
- Nock MK, Kessler RC. Prevalence of and risk factors for suicide attempts versus suicide gestures: analysis of the National Comorbidity Survey. J Abnorm Psychol. 2006;115(3):616–623. PubMed CrossRef
- Kung HC, Pearson JL, Liu X. Risk factors for male and female suicide decedents ages 15-64 in the United States. results from the 1993 National Mortality Followback Survey. Soc Psychiatry Psychiatr Epidemiol. 2003;38(8):419–426. PubMed CrossRef
- Holma KM, Melartin TK, Haukka J, et al. Incidence and predictors of suicide attempts in DSM-IV major depressive disorder: a five-year prospective study. Am J Psychiatry. 2010;167(7):801–808. PubMed CrossRef
- Shepard DS, Gurewich D, Lwin AK, et al. Suicide and suicidal attempts in the United States: costs and policy implications. Suicide Life Threat Behav. 2016;46(3):352–362. PubMed CrossRef
- Keisler-Starkey K, Bunch LN. Health Insurance Coverage in the United States: 2019. US Census Bureau website. https://www.census.gov/library/publications/2020/demo/p60-271.html. 2020. Accessed July 23, 2021.
- Voelker J, Kuvadia H, Cai Q, et al. United States national trends in prevalence of major depressive episode and co-occurring suicidal ideation and treatment resistance among adults. J Affect Disord Rep. 2021;5:100172. CrossRef
- Neslusan C, Voelker J, Lingohr-Smith M, et al. Characteristics of hospital encounters and associated economic burden of patients with major depressive disorder and acute suicidal ideation or behavior. Hosp Pract (1995). 2021;49(3):176–183. PubMed CrossRef
- Benson C, Singer D, Carpinella CM, et al. The health-related quality of life, work productivity, healthcare resource utilization, and economic burden associated with levels of suicidal ideation among patients self-reporting moderately severe or severe major depressive disorder in a national survey. Neuropsychiatr Dis Treat. 2021;17:111–123. PubMed CrossRef
- Hedegaard H, Schoenbaum M, Claassen C, et al. Issues in developing a surveillance case definition for nonfatal suicide attempt and intentional self-harm using International Classification of Diseases, Tenth Revision, Clinical Modification (ICD-10-CM) coded data. Natl Health Stat Rep. 2018;(108):1–19. PubMed
- Quan H, Li B, Couris CM, et al. Updating and validating the Charlson comorbidity index and score for risk adjustment in hospital discharge abstracts using data from 6 countries. Am J Epidemiol. 2011;173(6):676–682. PubMed CrossRef
- Austin PC. Using the standardized difference to compare the prevalence of a binary variable between two groups in observational research. Commun Stat Simul Comput. 2009;38(6):1228–1234. CrossRef
- Quan H, Sundararajan V, Halfon P, et al. Coding algorithms for defining comorbidities in ICD-9-CM and ICD-10 administrative data. Med Care. 2005;43(11):1130–1139. PubMed CrossRef
- Amos TB, Tandon N, Lefebvre P, et al. Direct and indirect cost burden and change of employment status in treatment-resistant depression: a matched-cohort study using a us commercial claims database. J Clin Psychiatry. 2018;79(2):24–32. PubMed CrossRef
- Ornell F, Schuch JB, Sordi AO, et al. “Pandemic fear” and COVID-19: mental health burden and strategies. Br J Psychiatry. 2020;42(3):232–235. PubMed CrossRef
- Cascella M, Rajnik M, Aleem A, et al. Features, Evaluation, and Treatment of Coronavirus (COVID-19). StatPearls; 2021.
- Porras-Segovia A, Baca-García E, Courtet P, et al. If suicide were CoViD-19: a neglected cause of premature death. J Clin Psychiatry. 2021;82(2):20l13702. PubMed CrossRef
- Gunnell D, Appleby L, Arensman E, et al; COVID-19 Suicide Prevention Research Collaboration. Suicide risk and prevention during the COVID-19 pandemic. Lancet Psychiatry. 2020;7(6):468–471. PubMed CrossRef
- Beck AT, Schuyler D, Herman I. Development of Suicidal Intent Scales. The Prediction of Suicide. In: Beck AT, Resnik HL, Lettieri DJ, eds. Oxford, England: Charles Press Publishers; 1974:xii, 249–xii, 249.
- Harriss L, Hawton K, Zahl D. Value of measuring suicidal intent in the assessment of people attending hospital following self-poisoning or self-injury. Br J Psychiatry. 2005;186(1):60–66. PubMed CrossRef
This PDF is free for all visitors!