ABSTRACT
Objective: To prospectively investigate the predictive value of diagnosis, suicidal behavior, and subjectively experienced depressed mood for imminent risk of suicide death.
Methods: This prospective study included a representative and diagnostically mixed sample of 7,000 acutely hospitalized psychiatric patients between May 2005 and July 2014 in a Norwegian catchment area of 400,000 inhabitants. Suicide deaths were registered at 1 and 2 weeks and at 1, 6, and 12 months following admission. Survival and hazard functions were estimated, and Cox regression was used to estimate the predictive values of suicidal ideation, suicide attempts, a diagnosis of depressive disorder, and severely depressed mood. Assessments were conducted at admission and included ICD-10 diagnosis, clinical interview in the form of the Health of the Nation Outcome Scales, and qualitative assessments of suicidal ideation and suicide attempts during the past week.
Results: During 1-year follow-up, 101 patients (1.4%) died by suicide, of whom almost 70% were men. Only severely depressed mood, including inappropriate self-blame and guilt, predicted suicide within the first week after admission (hazard ratio [HR] = 7.3; 95% confidence interval [CI], 1.4–37.1; P = .01). Suicidal ideation predicted death by suicide at 2 weeks (HR = 3.8; 95% CI, 1.2–12.8; P = .02) and all follow-up time points after, whereas a recent suicide attempt predicted suicide from the 1-month follow-up (HR = 7.3; 95% CI, 2.2–23.7; P < .001) onward.
Conclusions: We recommend thoroughly examining severity of depressed mood during assessment of imminent suicide risk.
J Clin Psychiatry 2023;84(1):22m14460
To cite: Fredriksen KJ, Bartz-Johannessen C, Schoeyen HK, et al. Imminent and short-term risk of death by suicide in 7,000 acutely admitted psychiatric inpatients. J Clin Psychiatry. 2023;84(1):22m14460.
To share: https://doi.org/10.4088/JCP.22m14460
© 2022 The Authors. Published by Physicians Postgraduate Press, Inc. This is an open access article under the CC BY-NC-ND license.
aClinic for Adult Mental Health Care, Stavanger University Hospital, Stavanger, Norway
bTIPS Centre for Clinical Research in Psychosis, Clinic for Adult Mental Health Care, Stavanger University Hospital, Stavanger, Norway
cFaculty of Health Sciences, University of Stavanger, Stavanger, Norway
dResearch Department, Division of Psychiatry, Haukeland University Hospital, Bergen, Norway
eDepartment of Østmarka, St Olavs Hospital, Trondheim, Norway.
fDepartment of Mental Health, Norwegian University of Science and Technology, Trondheim, Norway.
gNational Centre for Suicide Research and Prevention, Institute of Clinical Medicine, University of Oslo, Oslo, Norway
hFaculty of Social Sciences, University of Stavanger, Stavanger, Norway
*Corresponding author: Kristin Joerstad Fredriksen, MD, Clinic of Adult Psychiatry, Stavanger University Hospital, Armauer Hansens vei 20, 4011 Stavanger, Norway ([email protected]).
Although suicide risk assessments dominate clinical practice in emergency psychiatric settings,1 clinically relevant evidence to guide precautions and decision making in these settings is scarce.2 Suicide rates for 1 week following discharge from psychiatric hospitalization have, in a meta-analysis,3 been estimated at approximately 3,000 suicides per 100,000 person years (95% CI, 1,740 to 5,000; I2 = 88), about 200–300 times above the global suicide rate.
Accepted risk factors predominantly stem from longer-term follow-up studies and include a diagnosis of depressive disorder4–6 increasing in strength with episode severity,6–9 previous suicide attempts,2,6,7,9 male sex,6,7,9,10 and suicidal ideation.11–14 The usability in acute and emergency psychiatry of these longer-term risk factors is unclear,10,15 and our ability to identify imminent risk remains close to chance.10,15 This is problematic because suicide risk is at its highest during, and shortly after, psychiatric hospitalization.5,8,10,13,16–19
Some efforts at identifying short-term suicide risk have been made. These have, however, been hampered by several methodological challenges. First, most studies have been either cross-sectional or limited to chart reviews. A chart review20 of 381 suicides among US veterans found that suicidal ideation, psychotic symptoms, and sleep problems were associated with suicide within 1 week after contact. However, no charts of survivors were reviewed for comparison. A large registry-based study21 on more than 500,000 primary and mental health care patient records of the Patient Health Questionnaire suicidal ideation item found a risk of suicide within 7 days of only 0.01% among persons reporting having SI “nearly every day.” On the other hand, a large Swedish registry-based study14 including 18,684 patients found suicidal ideation and suicidal behavior as measured by the Columbia Suicide Severity Rating Scale to be significantly associated with completed suicide within 1 week after assessment.
Further, existing studies from psychiatric emergency departments have used small, non-representative samples and thus lack statistical power and generalizability.16 One example included a chart review22 of 76 inpatient or shortly post-discharge suicides and found extreme anxiety and/or agitation in 79% of suicide victims. This study also did not include survivors. A literature overview16 of existing studies on hospitalized patients found depressive symptoms to be associated with inpatient suicides in some case-control studies, but uncovered a need for larger and more representative, prospective studies tracing clinical predictors such as hopelessness and depressive symptoms. Findings of robust suicide predictors in acute psychiatry for the very short term thus seem lacking.2,10
Thus, although there is a growing literature investigating imminent and short-term risk factors for attempted suicide and ideation,23 a paucity of representative cohort studies of completed suicide, ie, death by suicide, in hospitalized or recently discharged patients remains.
Another challenge concerns group level, statistical risk factors and their limited applicability on the individual level. Rudd24 has proposed warning signs of imminent suicide. These include being in a mental state of hopelessness, rage, feeling trapped, anxiety, and agitation. Other studies have indicated similar signs and symptoms in the final day(s) before a suicidal event,24 such as anxiety and agitation,22,25 sleep problems,25–27 psychosis,20,28 impulsivity,29 and intense affective states3,22,24,28,30,31 including depressive symptoms.16,32 More recently, Galynker33 proposed a pre-suicidal mental state called the Suicidal Crisis Syndrome (SCS), which includes an aroused negative affective state, a deep feeling of entrapment, excessive rumination, panic, fear of dying, and emotional pain. SCS has thus far been tested against only proxy variables for suicide death such as ideation, attempts, and behavior and not completed suicide.23,34 In sum, risk factors such as a diagnosis of depressive disorder, suicidal ideation, and suicide attempts the first months to years after assessment have been studied extensively, while clinically useful data on imminent risk still appear to be lacking.
Aims of the Study
The aims of this study were to use clinical data from a prospectively followed representative cohort of 7,000 acutely hospitalized psychiatric patients to (1) study the relevance of known risk factors for imminent risk of suicide, (2) investigate the importance of a negative affective state clinically assessed as severely depressed mood, and (3) investigate imminent compared to longer-term risk.
METHODS
Participants
This study was part of the prospective cohort study Suicidality in Psychiatric Emergency Admissions run by the Department of Psychiatry, Haukeland University Hospital, Bergen, Norway.35,36 The Norwegian psychiatric health care system is catchment area based and publicly funded. There are no privately run acute inpatient facilities. Haukeland University Hospital covers a population of approximately 400,000. The study has established a database consisting of all consecutively admitted patients to the psychiatric acute ward between May 2005 and July 2014, constituting a mixed diagnostic sample of 7,000 patients, of whom 6,823 had complete data and thus were included in the prospective analyses. Over one-third (38.5%) were committed under the Norwegian Mental Health Act. In patients with several admissions during the study period, we used data from the most recent admission.
Assessments
Clinicians and trained research assistants collected and coded demographic and clinical data on admission. Clinicians who were involved in the assessment of patients at admission underwent training in the rating scales used. Clinical diagnoses were assessed according to ICD-1037 at admission. Experienced clinicians made qualitative assessments of current suicidal behavior over the past week using a standardized rating form in which only one of the following items (the most severe) could be rated positive: no suicidal ideation, passive death wishes, suicidal ideation, suicide plans made, self-harm without suicidal intent, and suicide attempt. All available information was used to complete this form, including the patient’s self-report, information from referring physicians, and information from any recent known somatic hospital admissions for suicide attempts or self-harm.
Mental health status and depressed mood were assessed using the Health of the Nation Outcome Scales (HoNOS),38 an instrument widely used in clinical practice and research for over 20 years.39 HoNOS covers mental health status and social functioning and was administered by clinicians on the admission day. It consists of 12 items, recording information about the last 14 days including admission day. Each item is scored on a 5-point scale representing maximum severity over the rating period (0 = no problem; 1 = minor problem requiring no action; 2 = mild problem but definitely present; 3 = moderately severe problem; 4 = severe to very severe problem). HoNOS item 7, “problems with depressed mood,” was used as a measure of affective state, and a cutoff score of 3 was chosen to indicate “severely depressed mood.” These scores are as follows40: a score of 3 indicates “Depression with inappropriate self-blame; preoccupation with feelings of guilt,” and a score of 4 indicates “Severe or very severe depression, with guilt or self-accusation.”
Suicide as Primary Outcome
We obtained suicide data by linking each patient’s 11-digit birth number to the Norwegian Cause of Death Registry (CDR) up to December 31, 2015. The CDR contains information about Norwegian residents regardless of geographic location of death and is > 98% complete.41 We defined suicide outcome within 1 week post-hospital admission as imminent and from 2 weeks to 1 year as short-term.
Statistical Analyses
Descriptive analyses were used to describe clinical and demographic characteristics at admission. A Kaplan-Meier survival curve was estimated to show the survival probability within the first year after admission. Patients were censored if they died of reasons other than suicide. Cox regression models (missing data on 177 subjects; n = 6,823 with complete data) were fitted with time to suicide as outcome. This method of analysis was chosen to allow data on patients who dropped out of the study or died of causes other than suicide before day 31 to still contribute to the model. Predictors in the first model, based on hypotheses, were a diagnosis of depressive disorder within the F30–F39 chapter of the ICD-10 (see Supplementary Appendix 1), suicidal ideation, and suicide attempts. Because suicide is a low-frequency incident (completed suicide: 10 after 7 days, 18 after 14 days, and 30 after 31 days), the number of predictors per model had to be limited to 3. These 3 were assessed across 5 time points, constituting 15 tests per model not independent of one another. Thus, a Bonferroni correction is not indicated. The second model included the predictor from our second research aim: severely depressed mood, suicidal ideation, and suicide attempt last week. A diagnosis of depressive disorder was excluded, as it did not contribute to model 1. To conclude, we conducted a new Cox regression with only diagnosis of depression and HoNOS item 7 (model 3). Analyses were repeated for the imminent (within 1 week) and short-term (2 weeks, 1 month, 6 months, and up to 1 year post admission) follow-ups. At the 1-year follow-up, we added sex as predictor variable to adjust for sex, as male sex is a well-established risk factor for suicide during inpatient stay and shortly after discharge.4–6,16,17,36 All tests were 2-tailed, and a P value < .05 was considered statistically significant. We used the statistical software R42 for all analyses.
Ethics
The Regional Committee for Medical Research Ethics (REK 2009/1057) and the Norwegian Social Science Data Service approved the study (NSD 11237). The Norwegian Directorate of Health Care authorized the use of patient information (SHDIR 07/2558). The study was exempted by these boards from requiring written or oral informed consent, because the collected data were part of standard assessments on admission to inpatient psychiatric care. The data were collected on the basis of person identifiers; however, after collection, they were anonymized, with identifiable data substituted by number tags.
RESULTS
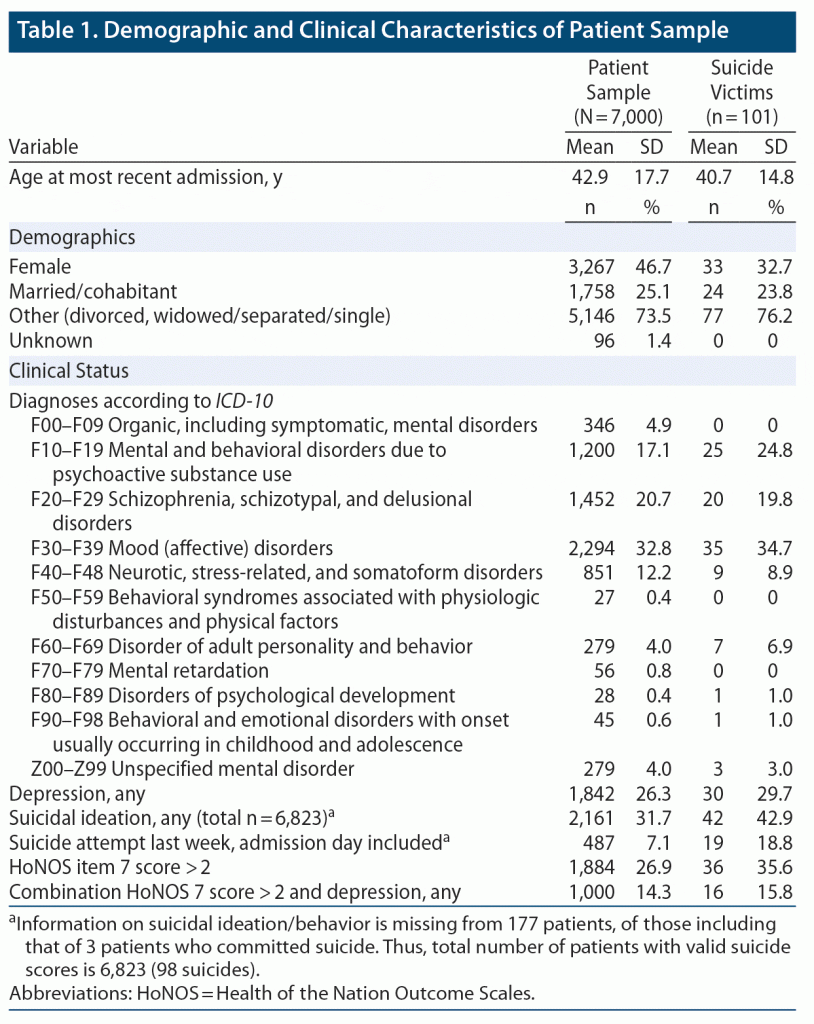
Sample characteristics (N = 7,000) are detailed in Table 1. A total of 101 patients (1.44%) had died by suicide by the 1-year follow-up. Among these were 30 patients with a diagnosis of depressive disorder Thirty-one percent of patients reported suicidal ideation at admission. A total of 7.1% reported having attempted suicide in the last week, admission day included. One thousand patients (14.3%) had a high score (3 or 4) on HoNOS item 7 in addition to a diagnosis of depression. Of the suicide decedents, 35.6% had a high score on HoNOS item 7, while 15.8% had both a diagnosis of depression and a high HoNOS item 7 score.
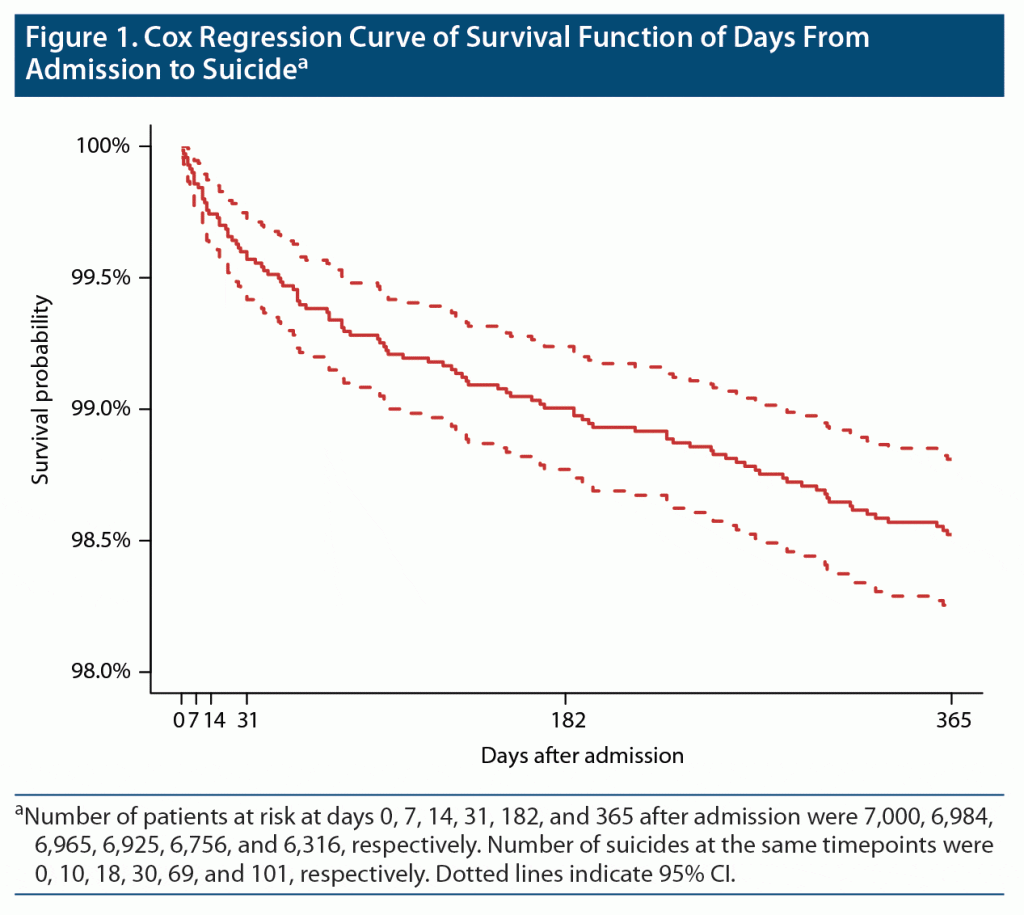
Figure 1 illustrates the Kaplan-Meier survival curve, showing the cumulative incidence of completed suicide over time for the 6,823 patients with complete data sets. After 1 week, 10 patients had died by suicide; after 1 month, 30 had done so; after 6 months, 69 had done so; and after 1 year, 101 patients had died by suicide.
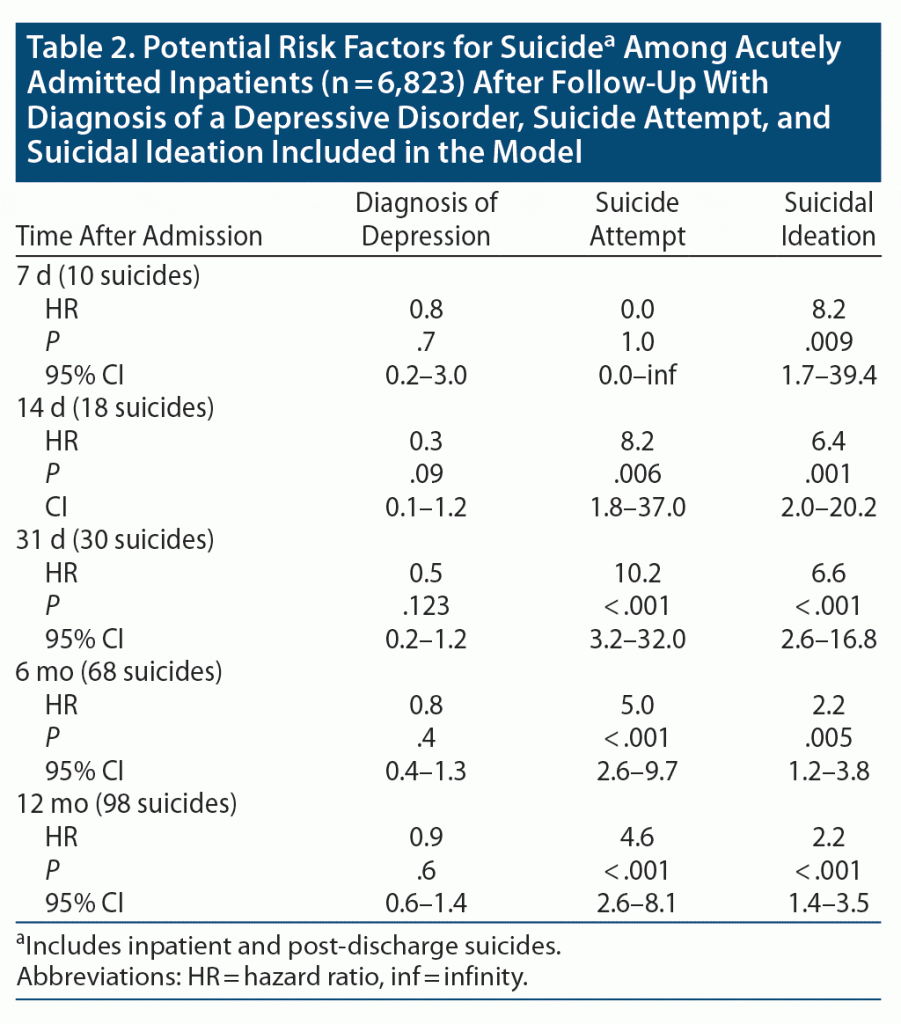
In the first Cox regression model, with a diagnosis of depression, suicidal ideation, and suicide attempt as predictors, only suicidal ideation significantly added to the model concerning the first 7 days following admission, though with a wide confidence interval (Table 2). It continued to be statistically significant at every subsequent follow-up, with narrowing confidence intervals. Suicide attempt was a significant predictor from 14 days and onward. A diagnosis of depression did not contribute significantly to the model for any of the follow-up time points.
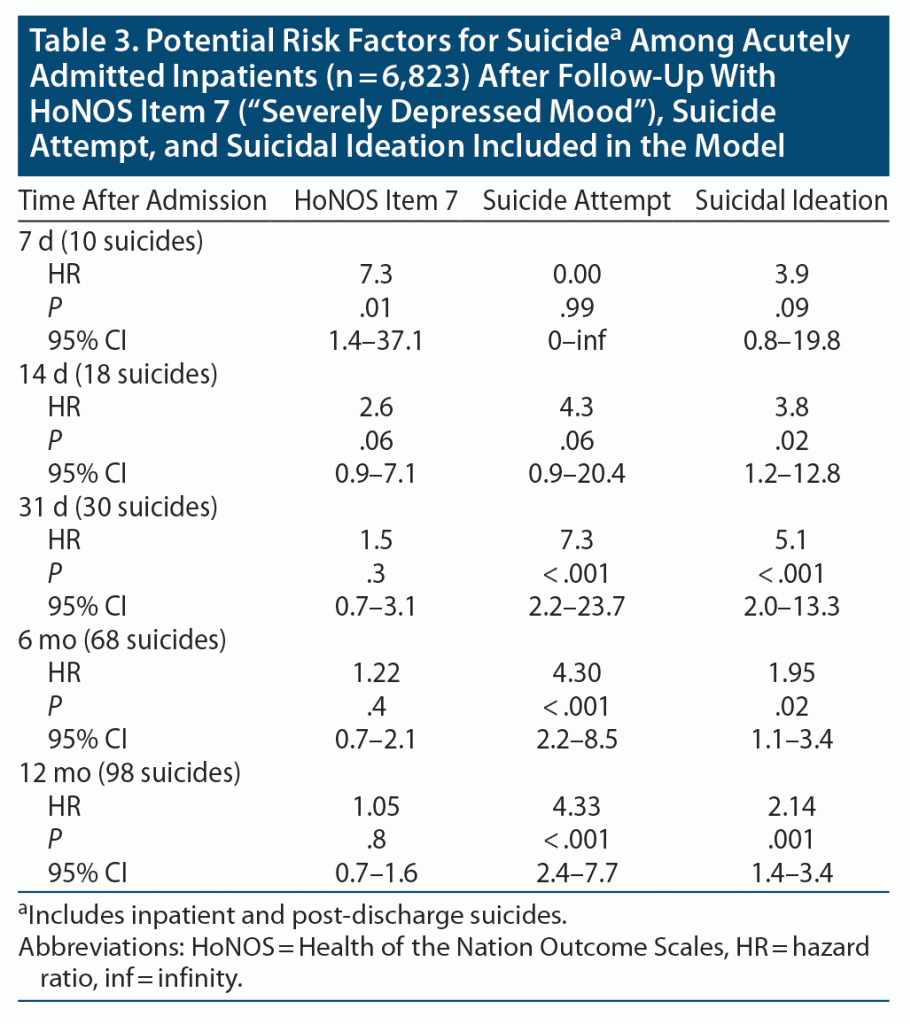
The following analysis (Table 3) included mental status as expressed by the HoNOS item 7 “severely depressed mood,” suicidal ideation, and suicide attempt as a predictor variables. A high score (3 or 4) on HoNOS item 7 was the only statistically significant predictor of imminent suicide risk, ie, death by suicide within the first 7 days following admission, though with a wide confidence interval. Between 7 and 14 days following hospital admission, suicidal ideation was the only statistically significant predictor, while HoNOS item 7 “severely depressed mood” and suicide attempt did not contribute significantly to the model. Suicidal ideation and suicide attempt had significant effects on suicide risk after 1, 6, and 12 months.
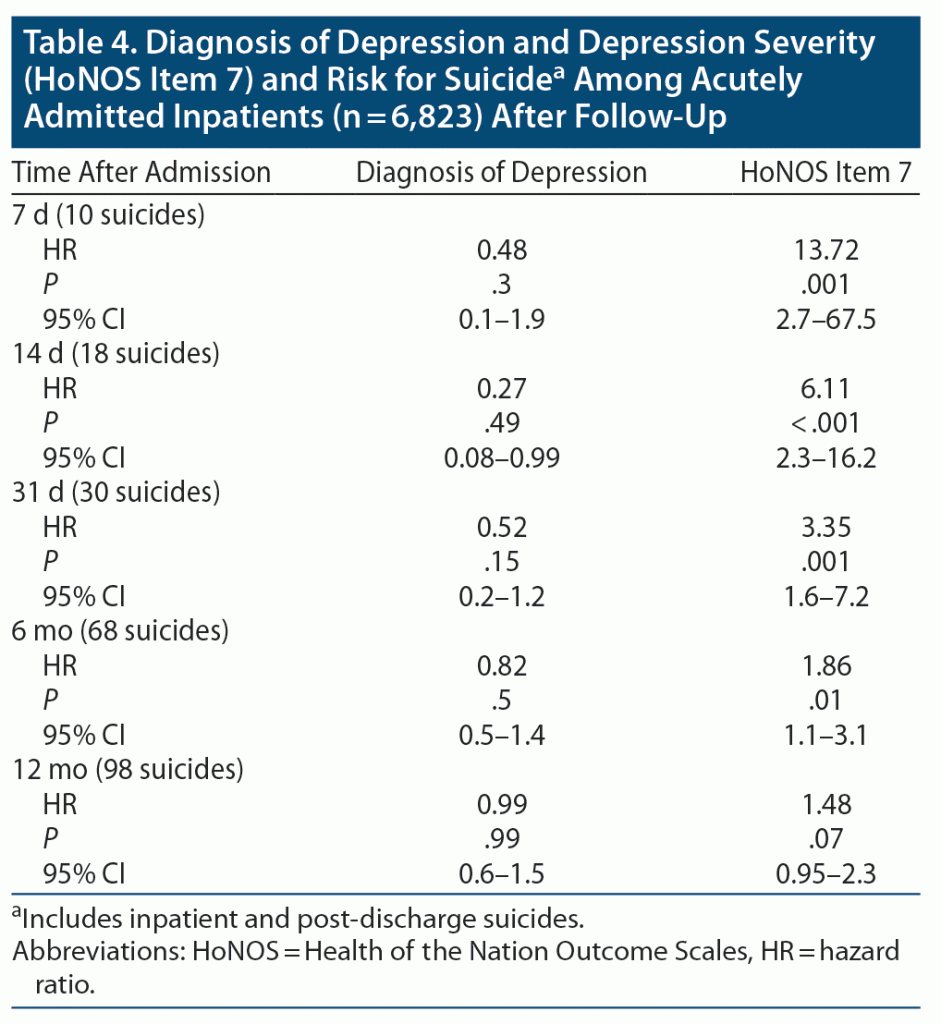
As a follow-up post hoc analysis, a model was tested using only a diagnosis of depressive disorder and HoNOS item 7 “severely depressed mood” (Table 4). This analysis was done to explore the relative significance of a diagnosis of depression compared to severity of depressed mood. The latter significantly predicted suicide at every follow-up time point (Table 4), whereas a diagnosis of depression did not at any time point.
Suicidal ideation and suicide attempt were still significant at the 1-year follow-up after adjusting for sex. Women were less likely to die by suicide than men (hazard ratio = 0.62; P < .02; 95% CI, 0.4–0.93).
DISCUSSION
The main findings of this study were as follows: First, severely depressed mood was the strongest predictor of imminent suicide risk in a sample in which 6,823 of 7,000 consecutively admitted patients in an acute psychiatric ward in Norway were analyzed using complete data sets. A high score on the severely depressed mood item 7 of Health of the Nation Outcome Scales (ie, HoNOS item 7) was associated with an increased risk of suicide within 7 days after hospital admission by a hazard ratio of more than 7. Second, a diagnosis of depressive disorder in and of itself did not indicate increased risk of suicide either imminently or longer-term. Third, suicidal ideation predicted suicide throughout the follow-up period except for the first week, when the model was adjusted for severely depressed mood. Finally, a suicide attempt the last week prior to admission also predicted suicide at, and after, 1 month, when the model was adjusted for severely depressed mood.
Severely depressed mood may be viewed as an intense affective state.30 It is compatible with elements of the proposed Suicide Crisis Syndrome (SCS), including excessive rumination and emotional pain, and predicted suicide within 7 days. SCS has been linked to pre-suicidal states, but appears to be independent of expressed suicidal ideation in previous studies33,34,43 as well as in the current study. This study underscores the importance of addressing discrepancies between “what a person says and what a person does”24 and placing more emphasis on clinically assessed depth of depressed mood. Severely depressed mood may be a modifiable factor over the course of an admission and after discharge and as such may be relevant for choosing interventions and for future risk assessment tools.16
Contrary to expectation, a diagnosis of depressive disorder did not significantly predict risk of suicide at any follow-up points. Findings are in line with those of a systematic review and meta-analysis13 reporting that discharged patients with mood disorders did not have a significantly elevated suicide rate compared to other diagnostic groups. One explanation may be that approximately 20% of suicide decedents had high scores on HoNOS item 7 but no diagnosis of depressive disorder. Further, the diagnostic category of depression is very broad, from mild to severe. A mild depression does not confer the same severity of distress or affective disturbance as a severe one,6–9 and “severely depressed mood” arguably represents the more severe end of the category. For instance, HoNOS item 7’s description includes overvalued psychosis-like ideas of self-blame. Researchers in other studies have hypothesized that paranoid and psychotic processes may transform suicidal thoughts into suicidal acts.44–46 Similarly, our research group previously found psychotic as opposed to non-psychotic depression to be a significant predictor of suicide.36 Psychotic delusions were also closely related to serious suicide attempts in a previously published qualitative study.44 In that study, persecutory delusions or delusions about shame and guilt accompanied by extreme fear and anxiety were reported by several patients as having driven them toward suicidal behavior.
Recent suicide attempts are known and robust predictors of suicide.2,6,7,9,16 Our data did not replicate this for suicide within the first 2 weeks after admission. However, this finding may be due to study subjects’ having been admitted to psychiatric care, and a suicide attempt would in many of the cases warrant admittance under the mental health act. These patients would then stay in a secured hospital setting for at least 10 days, often longer, reducing risk. Of note, statistical power was low due to few recent suicide attempts in the sample.
Our findings replicate male sex as a robust statistical predictor,4–6,16,17,36 as almost 70% of patients dead by suicide after 1 year were men.
In conclusion, our findings should not be taken as an argument against placing value on a diagnosis of depressive disorder when assessing imminent suicide risk, as this diagnosis may elicit suicide-preventive treatment47,48 and safety precautions. Rather, it is an argument in favor of also considering the more transdiagnostic phenomenon of intense affective states as expressed by subjectively experienced severely depressed mood. Denial of suicidal ideation alone may mislead the clinician to wrongly assess risk as low.
Strengths and Limitations
A 1-year follow-up study of completed suicides at 1 and 2 weeks and 1, 6, and 12 months after admission has, to our knowledge, never before been conducted. Strengths include a clinically representative population of acutely admitted patients not selected by presence of suicidal ideation or behavior and a prospective design. Also, the study has a very low rate of missing registered suicidal behavior (177 of 7,000, 2.5%). Systematic assessment of suicidal behavior at admission (suicidal/ideation/plans, passive death wishes, self-harm, and suicide attempt) combined with clinical data on depressive symptoms in all consecutively admitted acute ward patients has, to our knowledge, never previously been conducted in a prospective study. Including diagnosis, depressive symptoms, and suicidal behavior (suicidal ideation and suicide attempts) in the same study is a strength and a novelty. Finally, the completeness of the Norwegian Cause of Death Registry is a strength.
One limitation is a low base rate of suicides in absolute terms, notably not in this sample compared to other similar samples, but nevertheless resulting in wide confidence intervals. This low base rate prevented inclusion of potential confounders and other candidate predictors, or interaction effects. In addition, our study evaluated suicidal behavior at admission, and patients may have reported more suicidal thoughts/behaviors later. Also, data concerning hospitalization status at time of death were not available for inclusion in the study, meaning that some patients might have died by suicide during, and others (shortly) after, their hospital stay. Caution in generalizing to other non-acute, longer-term settings is warranted. Finally, interrater reliability for diagnosis and HoNOS was not established due to the practical limitations given by a large, naturalistic sample in psychiatric clinical practice.
Submitted: March 17, 2022; accepted August 11, 2022.
Published online: December 12, 2022.
Author contributions: Drs Fredriksen, Walby, Schoeyen, and Vaaler planned the study. Mr Bartz-Johannessen, Dr Hegelstad, and Dr Fredriksen as well as Liv Mellesdal, PhD (deceased), conducted the statistical analyses. Drs Fredriksen and Hegelstad interpreted the results and wrote the first draft of the manuscript. Dr Mellesdal was principal investigator and organized assessments, trainings, and data collection. Drs Schoeyen, Vaaler, and Walby provided feedback and co-wrote the manuscript.
Relevant financial relationships: The authors declare that they have no conflict of interest.
Funding/support: The study was funded by the Haukeland University Hospital and Stavanger University Hospital and Western Norway Regional Health Authority (Grant numbers: 911209/HV and 911671/HV).
Role of the sponsor: Funding agencies were not involved in design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication.
Acknowledgements: We thank all participants of the study and the clinicians at the Department of Psychiatry, Bergen University Hospital, Norway, who conducted the clinical assessments. We honor Liv Mellesdal PhD (deceased), former principal investigator in Suicidality in Psychiatric Emergency Admissions (SIPEA), for valuable input in the whole research process. We thank Igor Galynker, PhD, and Lisa Janet Cohen, PhD, at Icahn School of Medicine at Mount Sinai hospital, New York for invaluable feedback and intellectual input. Drs Galynker and Cohen have no financial relationships relevant to the subject of this article.
Data availability statement: Data sharing is not applicable due to limitations of data sharing as restricted in the approval from the Regional Committee for Medical and Health Research Ethics and the Norwegian Social Science Data Service.
Supplementary material: Available at Psychiatrist.com.
Clinical Points
- Severely depressed mood, including overvalued ideas and delusions of self-blame and guilt, predicted imminent suicide risk in a large representative sample of persons acutely hospitalized in mental health care.
- Suicidal ideation and a recent suicide attempt at admission also conferred an elevated risk, though not for the first week after admission.
- A diagnosis of depressive disorder in and of itself did not predict suicide death during the first year after hospital admission.
References (48)

- Bolton JM, Gunnell D, Turecki G. Suicide risk assessment and intervention in people with mental illness. BMJ. 2015;351:h4978. PubMed CrossRef
- Glenn CR, Nock MK. Improving the short-term prediction of suicidal behavior. Am J Prev Med. 2014;47(suppl 2):S176–S180. PubMed CrossRef
- Chung D, Hadzi-Pavlovic D, Wang M, et al. Meta-analysis of suicide rates in the first week and the first month after psychiatric hospitalisation. BMJ Open. 2019;9(3):e023883. PubMed CrossRef
- Leadholm AK, Rothschild AJ, Nielsen J, et al. Risk factors for suicide among 34,671 patients with psychotic and non-psychotic severe depression. J Affect Disord. 2014;156:119–125. PubMed CrossRef
- Olfson M, Wall M, Wang S, et al. Short-term suicide risk after psychiatric hospital discharge. JAMA Psychiatry. 2016;73(11):1119–1126. PubMed CrossRef
- Isometsä ET. Suicides in mood disorders in psychiatric settings in nordic national register-based studies. Front Psychiatry. 2020;11:721. PubMed CrossRef
- Hawton K, Casañas I, Comabella C, Haw C, et al. Risk factors for suicide in individuals with depression: a systematic review. J Affect Disord. 2013;147(1–3):17–28. PubMed CrossRef
- Deisenhammer EA, Behrndt E-M, Kemmler G, et al. Suicide risk factors in patients recently discharged from a psychiatric hospital: a case-control study. J Clin Psychiatry. 2019;80(5):18m12702. PubMed CrossRef
- Aaltonen KI, Isometsä E, Sund R, et al. Risk factors for suicide in depression in Finland: first-hospitalized patients followed up to 24 years. Acta Psychiatr Scand. 2019;139(2):154–163. PubMed CrossRef
- Franklin JC, Ribeiro JD, Fox KR, et al. Risk factors for suicidal thoughts and behaviors: a meta-analysis of 50 years of research. Psychol Bull. 2017;143(2):187–232. PubMed CrossRef
- McHugh CM, Corderoy A, Ryan CJ, et al. Association between suicidal ideation and suicide: meta-analyses of odds ratios, sensitivity, specificity and positive predictive value. BJPsych Open. 2019;5(2):e18. PubMed CrossRef
- Hubers AAM, Moaddine S, Peersmann SHM, et al. Suicidal ideation and subsequent completed suicide in both psychiatric and non-psychiatric populations: a meta-analysis. Epidemiol Psychiatr Sci. 2018;27(2):186–198. PubMed CrossRef
- Chung DT, Ryan CJ, Hadzi-Pavlovic D, et al. Suicide rates after discharge from psychiatric facilities: a systematic review and meta-analysis. JAMA Psychiatry. 2017;74(7):694–702. PubMed CrossRef
- Bjureberg J, Dahlin M, Carlborg A, et al. Columbia-Suicide Severity Rating Scale Screen Version: initial screening for suicide risk in a psychiatric emergency department. Psychol Med. 2021;1–9. PubMed CrossRef
- Bolton JM. Suicide risk assessment in the emergency department: out of the darkness. Depress Anxiety. 2015;32(2):73–75. PubMed CrossRef
- Madsen T, Erlangsen A, Nordentoft M. Risk estimates and risk factors related to psychiatric inpatient suicide—an overview. Int J Environ Res Public Health. 2017;14(3):253. PubMed CrossRef
- Madsen T, Erlangsen A, Hjorthøj C, et al. High suicide rates during psychiatric inpatient stay and shortly after discharge. Acta Psychiatr Scand. 2020;142(5):355–365. PubMed CrossRef
- Walsh G, Sara G, Ryan CJ, et al. Meta-analysis of suicide rates among psychiatric in-patients. Acta Psychiatr Scand. 2015;131(3):174–184. PubMed CrossRef
- Walby FA, Myhre MO, Kildahl AT. Contact with mental health services prior to suicide: a systematic review and meta-analysis. Psychiatr Serv. 2018;69(7):751–759. PubMed CrossRef
- Britton PC, Ilgen MA, Rudd MD, et al. Warning signs for suicide within a week of healthcare contact in veteran decedents. Psychiatry Res. 2012;200(2–3):395–399. PubMed CrossRef
- Simon GE, Coleman KJ, Rossom RC, et al. Risk of suicide attempt and suicide death following completion of the Patient Health Questionnaire depression module in community practice. J Clin Psychiatry. 2016;77(2):221–227. PubMed CrossRef
- Busch KA, Fawcett J, Jacobs DG. Clinical correlates of inpatient suicide. J Clin Psychiatry. 2003;64(1):14–19. PubMed CrossRef
- Bloch-Elkouby S, Barzilay S, Gorman BS, et al. The revised Suicide Crisis Inventory (SCI-2): Validation and assessment of prospective suicidal outcomes at one month follow-up. J Affect Disord. 2021;295:1280–1291. PubMed CrossRef
- Rudd MD. Suicide warning signs in clinical practice. Curr Psychiatry Rep. 2008;10(1):87–90. PubMed CrossRef
- Berman AL. Risk factors proximate to suicide and suicide risk assessment in the context of denied suicide ideation. Suicide Life Threat Behav. 2018;48(3):340–352. PubMed CrossRef
- Pigeon WR, Pinquart M, Conner K. Meta-analysis of sleep disturbance and suicidal thoughts and behaviors. J Clin Psychiatry. 2012;73(9):e1160–e1167. PubMed CrossRef
- Bernert RA, Kim JS, Iwata NG, et al. Sleep disturbances as an evidence-based suicide risk factor. Curr Psychiatry Rep. 2015;17(3):554. PubMed CrossRef
- Sani G, Tondo L, Koukopoulos A, et al. Suicide in a large population of former psychiatric inpatients. Psychiatry Clin Neurosci. 2011;65(3):286–295. PubMed CrossRef
- Gvion Y, Apter A. Aggression, impulsivity, and suicide behavior: a review of the literature. Arch Suicide Res. 2011;15(2):93–112. PubMed CrossRef
- Fawcett J, Scheftner WA, Fogg L, et al. Time-related predictors of suicide in major affective disorder. Am J Psychiatry. 1990;147(9):1189–1194. PubMed CrossRef
- Hendin H, Maltsberger JT, Szanto K. The role of intense affective states in signaling a suicide crisis. J Nerv Ment Dis. 2007;195(5):363–368. PubMed CrossRef
- Large M, Smith G, Sharma S, et al. Systematic review and meta-analysis of the clinical factors associated with the suicide of psychiatric in-patients. Acta Psychiatr Scand. 2011;124(1):18–29. PubMed CrossRef
- Galynker I. The Suicidal Crisis: Clinical Guide to the Assessment of Imminent Suicide Risk. Oxford University Press; 2017.
- Rogers ML, Vespa A, Bloch-Elkouby S, et al. Validity of the modular assessment of risk for imminent suicide in predicting short-term suicidality. Acta Psychiatr Scand. 2021;144(6):563–577. PubMed CrossRef
- Strømme MF, Mellesdal LS, Bartz-Johannesen C, et al. Mortality and non-use of antipsychotic drugs after acute admission in schizophrenia: a prospective total-cohort study. Schizophr Res. 2021;235:29–35. PubMed CrossRef
- Fredriksen KJ, Gjestad R, Walby FA, et al. High scores on the MADRS depression rating scale and psychotic symptoms predict suicide: a prospective cohort study of psychiatric acute ward patients. J Clin Psychiatry. 2022;83(5):21m14018. PubMed CrossRef
- World Health Organization. The ICD-10 Classification of Mental and Behavioural Disorders: Clinical Descriptions and Diagnostic Guidelines. World Health Organization; 1992.
- Wing J, Curtis R, Beevor A. ‘Health of the Nation’: measuring mental health outcomes. Psychol Bull. 1994;18(11):690–691. CrossRef
- James M, Painter J, Buckingham B, et al. A review and update of the Health of the Nation Outcome Scales (HoNOS). BJPsych Bull. 2018;42(2):63–68. PubMed CrossRef
- Wing J, Curtis RH, Beevor A. Health of the Nation Outcome Scales (HoNOS): glossary for HoNOS score sheet. Br J Psychiatry. 1999;174(5):432–434. PubMed CrossRef
- Pedersen AG, Ellingsen CL. Data quality in the causes of death registry. Tidsskr Nor Laegeforen. 2015;135(8):768–770. PubMed CrossRef
- R Core Team. (2021). R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. R Project website. http://www.r-project.org.
- Schuck A, Calati R, Barzilay S, et al. Suicide Crisis Syndrome: A review of supporting evidence for a new suicide-specific diagnosis. Behav Sci Law. 2019;37(3):223–239. PubMed CrossRef
- Fredriksen KJ, Schoeyen HK, Johannessen JO, et al. Psychotic depression and suicidal behavior. Psychiatry. 2017;80(1):17–29. PubMed CrossRef
- Roose SP, Glassman AH, Walsh BT, et al. Depression, delusions, and suicide. Am J Psychiatry. 1983;140(9):1159–1162. PubMed CrossRef
- Yates K, Lång U, Cederlöf M, et al. Association of psychotic experiences with subsequent risk of suicidal ideation, suicide attempts, and suicide deaths: a systematic review and meta-analysis of longitudinal population studies. JAMA Psychiatry. 2019;76(2):180–189. PubMed CrossRef
- Brent DA, Oquendo MA, Reynolds CF 3rd. Caring for suicidal patients. JAMA Psychiatry. 2019;76(8):862–863. PubMed CrossRef
- Mann JJ, Michel CA, Auerbach RP. Improving suicide prevention through evidence-based strategies: a systematic review. Am J Psychiatry. 2021;178(7):611–624. PubMed CrossRef
This PDF is free for all visitors!