Objective: Although studies have linked childhood trauma to depression resembling the atypical subtype, a majority of these studies did not use DSM-IV criteria for atypical features nor assess trauma both before and after depression onset. This study examined the relationship between atypical depression and lifetime trauma with the hypothesis that atypically depressed patients would report a higher number of trauma exposures than nonatypically depressed patients.
Method: Raters blind to depressive subtype investigated trauma history by reviewing the Structured Clinical Interview for DSM-IV-TR Axis I Disorders-Patient Edition (SCID-I/P) posttraumatic stress disorder modules and social history sections in charts of depressed outpatients who had participated in treatment studies between 1985 and 2010. Rates of trauma both before and after depression onset were compared for 292 depressed patients with and without DSM-IV-defined atypical features using χ2 tests and binary logistic regressions. This chart review was conducted from 2009 to 2011.
Results: Lifetime trauma was reported significantly more often by depressed patients with atypical features than by those without (P < .001). Patients with atypical features reported significantly more traumatic experiences both prior to (P = .012) and following (P = .015) depression onset. When sex and age at onset or duration of depression were used as covariates, depressive subtype was a significant predictor of reported trauma both prior to (P = .028) and following (P = .011) depression onset.
Conclusions: These results suggest that a relationship exists between atypical depression and lifetime trauma that may be more complex than the etiologic pathways outlined in prior research. Rather, trauma and atypical depression may be interrelated throughout life.
J Clin Psychiatry 2013;74(5):500-506
© Copyright 2013 Physicians Postgraduate Press, Inc.
Submitted: April 27, 2012; accepted December 19, 2012(doi:10.4088/JCP.12m07870).
Corresponding author: Amy C. Withers, MA, 1051 Riverside Drive #3300, New York, NY 10032 ([email protected]).
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
ABSTRACT
Objective: Although studies have linked childhood trauma to depression resembling the atypical subtype, a majority of these studies did not use DSM-IV criteria for atypical features nor assess trauma both before and after depression onset. This study examined the relationship between atypical depression and lifetime trauma with the hypothesis that atypically depressed patients would report a higher number of trauma exposures than nonatypically depressed patients.
Method: Raters blind to depressive subtype investigated trauma history by reviewing the Structured Clinical Interview for DSM-IV-TR Axis I Disorders-Patient Edition (SCID-I/P) posttraumatic stress disorder modules and social history sections in charts of depressed outpatients who had participated in treatment studies between 1985 and 2010. Rates of trauma both before and after depression onset were compared for 292 depressed patients with and without DSM-IV-defined atypical features using χ2 tests and binary logistic regressions. This chart review was conducted from 2009 to 2011.
Results: Lifetime trauma was reported significantly more often by depressed patients with atypical features than by those without (P < .001). Patients with atypical features reported significantly more traumatic experiences both prior to (P = .012) and following (P = .015) depression onset. When sex and age at onset or duration of depression were used as covariates, depressive subtype was a significant predictor of reported trauma both prior to (P = .028) and following (P = .011) depression onset.
Conclusions: These results suggest that a relationship exists between atypical depression and lifetime trauma that may be more complex than the etiologic pathways outlined in prior research. Rather, trauma and atypical depression may be interrelated throughout life.
J Clin Psychiatry 2013;74(5):500-506
© Copyright 2013 Physicians Postgraduate Press, Inc.
Submitted: April 27, 2012; accepted December 19, 2012(doi:10.4088/JCP.12m07870).
Corresponding author: Amy C. Withers, MA, 1051 Riverside Drive #3300, New York, NY 10032 ([email protected]).
Trauma and depression are highly associated.1-5 However, few studies have examined the relationship between trauma and DSM-IV depressive subtypes, such as depression with atypical features, which is defined by mood reactivity and at least 2 of the following: significant weight gain or increased appetite, hypersomnia, leaden paralysis, and interpersonal rejection sensitivity. Atypical depression has been differentiated from other forms of depression in terms of its biology,6-8 treatment,9-11 and family history.12
Research has shown a possible link between trauma and atypical depression. Although 1 study associated severe childhood adversity with endogenous depression13 resembling the melancholic or nonatypical depression subtype, most have connected trauma with nonendogenous depression14,15 resembling the atypical depression subtype.16,17 Specifically, depression with reversed neurovegetative features (oversleeping and overeating) was more strongly associated with childhood abuse than both depression without reversed neurovegetative features16,17 and normal controls.16 Trauma has also been associated with early onset of depression,4,18 chronicity of depression,3,19,20 and increased comorbidity.4,21 Since atypical depression is characterized by reversed neurovegetative features,6,12 early onset,12,22-24 chronicity,12,22,24 and increased comorbidity,6,23 it seems plausible that increased trauma may also be associated with this depressive subtype.
A second possible link between trauma and atypical depression comes from reports25,26 that both exhibit down-regulation of the hypothalamic-pituitary-adrenal (HPA) axis due to chronic stress. Cortisol levels are lowered in posttraumatic stress disorder (PTSD)27 and hypersuppressed in childhood sexual abuse victims28 and depressed trauma survivors.29 Similarly, in atypical depressive patients, cortisol levels are lowered relative to both melancholic depressive patients30 and healthy controls31 and hypersuppressed relative to healthy controls,32 especially for early-onset, chronic atypical depression.8 Thus, a hypoactive HPA axis characterizes trauma victims and atypical depression patients in contrast to the hyperactive HPA axis in melancholic depression.33,34
Nevertheless, gaps remain in research linking atypical depression and trauma. First, prior studies16,17 did not use DSM-IV criteria for atypical depression but instead used reversed neurovegetative symptoms to infer atypical subtype. Second, the majority of studies required the presence of childhood maltreatment16,17,25 or PTSD rather than trauma in general.16,35 Though some studies take trauma events at any age into account, they still limit their purview to those that occurred prior to depression onset,14 assuming that early trauma predisposes one to later development of atypical depression.16,17 If trauma causes atypical depression, there should be increased trauma prior to depression onset but not necessarily once depression has occurred. Alternatively, association of trauma and atypical depression before and after depression onset would not disprove a causal connection but would indicate the possibility of a more complex relationship and require the consideration of additional factors.

- History of trauma appears more likely in patients with atypical depression than other depressive subtypes.
- Patients with atypical depression report more traumatic experiences both prior to and following depression onset.
- Individual symptoms of atypical depression do not appear to be associated with trauma history; the association may be present only when multiple symptoms co-occur to form the distinct syndrome of atypical depression.
We sought to answer the following questions: (1) Does a relationship exist between trauma and DSM-IV-defined atypical depression? (2) Do rates of trauma differ before and after onset of depression? and (3) Are any individual atypical features associated with trauma?
We hypothesized that atypical depression patients would report more lifetime traumatic experiences than nonatypical depression patients. We also predicted that certain characteristic features of atypical depression, particularly mood reactivity and rejection sensitivity, might mediate the relationship between reported trauma and atypical depression, perhaps by making individuals more sensitive to negative events.
METHOD
Description
A chart review of depressed patients was conducted between 2009 and 2011 to assess presence or absence of trauma, with particular focus on the timing of any reported trauma. This research was approved by the Institutional Review Board (IRB) of the New York State Psychiatric Institute.
Participants
Patients who had participated in various psychopharmacologic research studies at the Depression Evaluation Service of the New York State Psychiatric Institute from 1985 to 2010 were randomly selected from a pool of several thousand Depression Evaluation Service patients until a sample of 300 patients was obtained. Criteria for inclusion were current diagnosis of a unipolar mood disorder (ie, major depressive disorder, dysthymic disorder, or depressive disorder not otherwise specified) and determination of presence or absence of both atypical features and trauma history. There was insufficient documentation of trauma history for 6 patients and depressive diagnosis for 2 patients, so 8 were removed from the analysis, resulting in 292 patients. Because of exclusion criteria from prior Depression Evaluation Service studies, no participant had a history of psychosis, current substance abuse or dependence, and/or other medical conditions or medications that were known to induce psychiatric disorders at the time of intake. Most Depression Evaluation Service studies excluded individuals with histories of bulimia or anorexia nervosa because of antidepressant-associated seizure risk. Informed consent was obtained for the initial Depression Evaluation Service studies and the New York State Psychiatric Institute IRB granted a waiver of consent for the present research.
Diagnosis
At intake, a research psychiatrist completed an interview including the Structured Clinical Interview for DSM-IV-TR Axis I Disorders-Patient Edition (SCID-I/P)36 and a written social history, with particular focus on depressive subtype. For this study, all diagnoses past and present were taken into account and patients were grouped into those who had experienced an atypical episode and those who had not.
Sources of Trauma Information
The SCID-I PTSD module was reviewed for any traumas listed, followed by the written social history for any additional traumas.
Types of Trauma
Trauma was defined as in DSM-IV as physical abuse, sexual abuse, experiencing a serious accident or disaster, witnessing severe violence, and experiences that threatened death, serious injury, or threat to the physical integrity of self or others. We considered severe verbal/emotional abuse by a caregiver toward a dependent child to be a threat to physical integrity, but vague statements, such as “the patient had a traumatic home environment” or “the patient’s mother would yell at him,” were not included as trauma.
Trauma Raters
Two raters (J.M.T. and A.C.W.) blind to depressive subtype documented all potentially traumatic events (213) from intake records. Both raters then judged each event as either fitting or not fitting the definition of trauma above, achieving high interrater reliability (κ = 0.75). All discrepancies (11) between judges were resolved by consensus with a third judge (J.W.S.). Thirty-six events were deemed nontraumatic, resulting in 177 traumatic events. Patients were then coded for whether they experienced trauma throughout their lifespan (“lifetime trauma”). Following completion of trauma coding, presence and dates of traumas were merged with a database that included demographics, Axis I diagnoses, depressive subtype, and age at depression onset.
Timing of Trauma
When documented, age at each traumatic event was recorded. For discrete events (eg, witnessing violence), a single age was recorded. For ongoing or chronic events (eg, abuse throughout childhood), ages at both onset and offset of the event were recorded. By using the ages at which the traumatic events occurred and the age at first depression onset, each patient was identified as having experienced trauma prior to depression onset, following depression onset, or both. Some patients provided the life period (eg, childhood, adolescence, adulthood) when the trauma occurred rather than a specific age. When it was possible to determine the order of events, the before and after depression onset trauma categories were coded. For example, someone who was sexually abused “throughout early childhood,” became depressed “after college,” and then was attacked at knifepoint “during middle age” would be coded as having trauma both before and after depression onset. However, if both depression onset and trauma occurred “in childhood,” the relative order could not be determined. Likewise, because depression chronology and trauma history were probed separately, events that occurred at the same age or co-occurred were not assigned a relative order, and such traumas were captured only under the lifetime trauma category. Twenty-nine patients had trauma history that could not be established as occurring before or after depression onset and therefore were included in analyses of lifetime trauma but not of onset-relative trauma.
Statistics
Analyses of variance were used to compare atypical depression and nonatypical depression diagnostic groups on age at intake, age at earliest depression onset, age at earliest trauma, and number of years from first depression onset. Sex ratio, comorbidity, and lifetime trauma rates between diagnostic groups were compared between diagnostic groups with 2 ×— 2 χ2 tests. We expected to find that female patients would have higher rates of both atypical depression23,24,37 and trauma,38 so an additional 2 ×— 2 ×— 2 χ2 test compared lifetime trauma rates by sex and diagnostic group.
To account for the fact that there is more opportunity for trauma to occur over longer periods of time, all time-relative trauma rates (ie, trauma before and after depression onset) were assessed by using binary logistic regressions covaried for the duration of the time period in years. This method corrects for potential effects of expected differences in age at onset between the 2 diagnostic groups. The duration of the period before depression onset was measured as the age at first depression onset. The duration of the period after depression onset was measured as the difference between the current age at intake and the age at first depression onset. Binary logistic regressions were run for each time period, with trauma presence as the categorical dependent variable, sex and depressive subtype as categorical predictors, and duration of time period as a continuous predictor. Thus, while it was expected that female gender and longer duration would both be significantly associated with increased trauma rates in each time period, the question of interest was whether atypical depression remained a significant predictor of higher trauma rates while sex and duration were included as covariates. This analysis was meant to confirm the hypothesis that atypical depression is associated with increased trauma rates in the period preceding first depression onset and to test whether atypical depression patients have similar or different trauma rates in the period following depression onset.
To examine whether individual atypical depression features account for any atypical depression-trauma associations, similar binary logistic regressions were run for each life period using all 5 atypical depression features as simultaneous categorical predictors in place of depressive subtype.
RESULTS
Demographic Characteristics
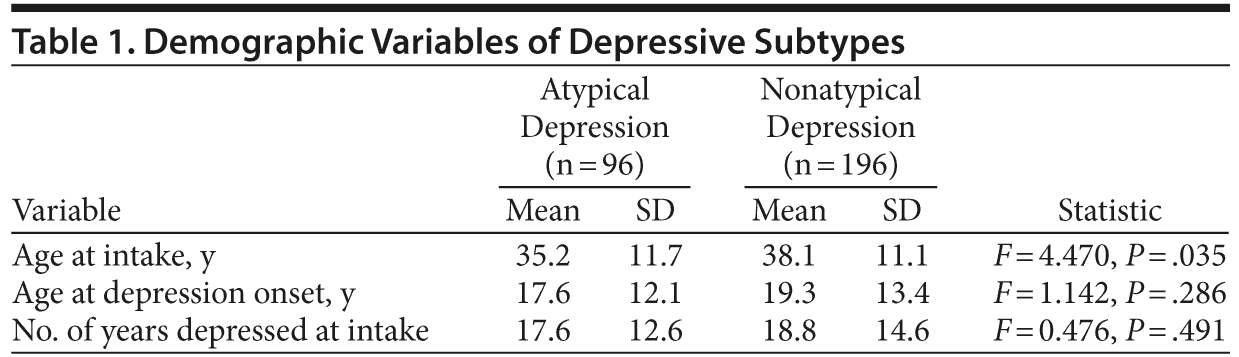
The sample of 292 depressed individuals consisted of 96 (32.9%) atypical depression and 196 (67.1%) nonatypical depression patients, with 169 (57.9%) female and 123 (42.1%) male patients. Mean age at intake was 37.2 years (SD = 11.4) and at earliest depression onset was 18.7 years (SD = 13.0). Mean number of years from earliest depression onset was 18.4 (SD = 14.0). Of the 292 patients, 283 (96.9%) had sufficient data to determine lifetime psychiatric comorbidity. Specifically, criteria were met for substance dependence (past only) by 10.6%, PTSD by 7.1%, other anxiety disorders by 33.6%, somatoform disorders by 5.7%, and eating disorders (primarily binge eating disorder) by 8.2%. Overall, 135 patients (47.7%) met diagnostic criteria for at least 1 comorbid disorder.
Demographic data are shown by diagnostic group (Table 1). At intake, atypical depression patients were significantly younger than nonatypical depression patients (P = .035). No significant difference was found between atypical depression and nonatypical depression patients in terms of number of years depressed (P = .491) and age at onset (P = .286), an unexpected result since atypical depression has been associated with an earlier age at onset relative to depressive subtypes.12,22-24 Although age at onset was not significantly different, atypical depression patients in our sample still had an earlier onset, so this discrepancy appears to result from an earlier than usual onset for nonatypical depression patients versus prior literature.
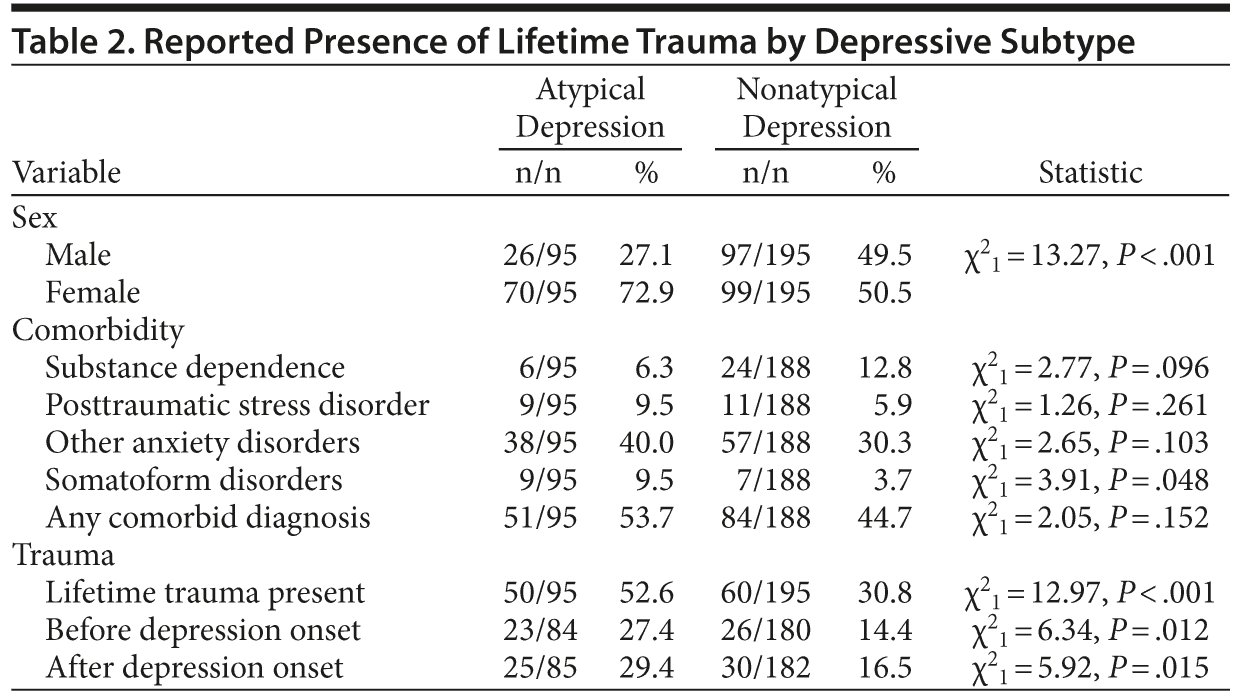
Sex and comorbidity are compared by diagnostic group (Table 2). Significantly more female patients were in the atypical depression group than in the nonatypical depression group (P < .001). No significant difference was shown in any comorbid disorder (P = .152), comorbid PTSD (P = .261), other anxiety disorders (P = .103), or substance dependence (P = .096), but significantly more comorbid somatoform disorders were in atypical depression than in nonatypical depression patients (P = .048) (Table 2).
Trauma Rates
Basic trauma rates were compared with χ2 tests (Table 2). Atypical depression patients reported significantly more traumatic experiences than nonatypical depression patients for the lifetime (P < .001), before depression onset (P = .012), and after depression onset (P = .015) periods.
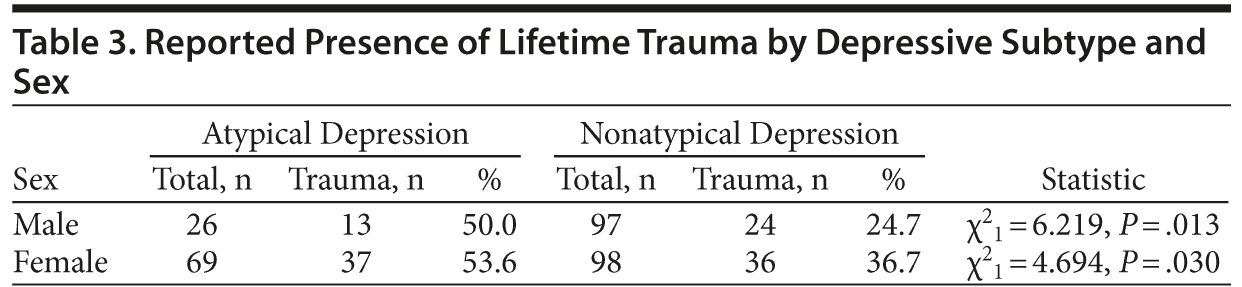
Lifetime trauma was reported significantly more often by 43.7% of female patients (73/167) versus 30.1% of male patients (37/123) (χ21 = 3.11, P = .009). A 2 ×— 2 ×— 2 χ2 test confirmed that atypical depression was associated with lifetime trauma, regardless of sex (male patients: P = .013; female patients: P = .030) (Table 3).
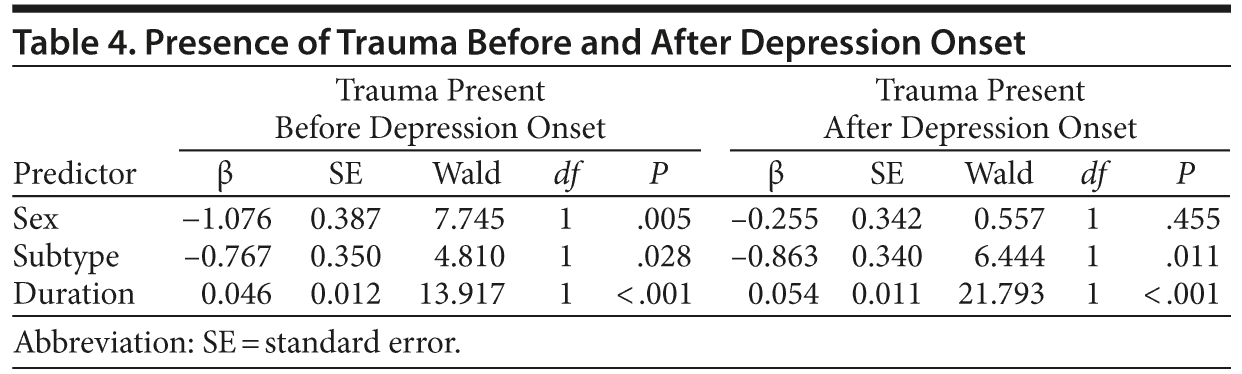
In the binary logistic regressions for the period before depression onset, sex (P = .005), subtype (P = .028), and duration (ie, age at onset) (P < .001) were all significant predictors of reported trauma, such that female gender, atypical depression, and longer duration were all associated with more frequent reports of trauma before depression onset (Table 4). For the period after depression onset, subtype (P = .011) and duration (ie, age − age at onset) (P < .001) were significant predictors, such that atypical depression and longer duration were associated with more frequent reports of trauma after depression onset; however, sex was not a significant predictor of trauma rates after depression onset (P = .455) (Table 4).
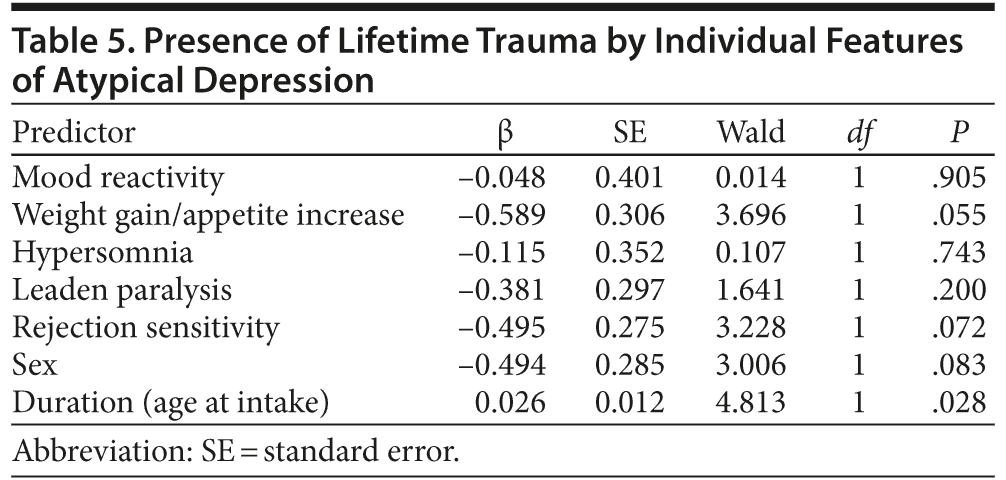
In the binary logistic regressions with the 5 atypical depression features, sex, and duration as simultaneous predictors of trauma presence, no atypical depression features were significant predictors of reported lifetime trauma (Table 5).
DISCUSSION
To our knowledge, this is the first study utilizing DSM-IV criteria for atypical depression while measuring trauma in the life periods both before and after depression onset. These results confirm the hypothesis that atypical depression patients report more traumatic experiences than nonatypical depression patients. Moreover, our findings are in line with prior studies14-17 that associated depression resembling atypical depression with early trauma. The data go further, however, in demonstrating that increased trauma also occurs after depression onset.
Various possibilities could explain this relationship between trauma and atypical depression. First, the findings could be coincidental, so they require replication. Second, it is possible that atypical depression patients may not actually incur more traumatic events than nonatypical depression patients, but they may report events differently. Compared to melancholic nonatypical depression patients, atypical depression patients are characterized by a mood state that may make them more likely to initially experience an event as traumatic. Also, research has shown that mood state affects both encoding and recall of memories.39-42 Amygdala activity during emotional arousal causes increased memory consolidation in the hippocampus, leading to sustained memory enhancement over time.43,44 This observation suggests that the emotional tone of an event might influence later recall of whether the event occurred at all. It is also possible that the various depressive subtypes include presentations that cue interviewers to probe differently, resulting in varying reports of trauma history.
Third, a possible explanation for the observed relationship to atypical depression patients actually incurring more traumatic events than nonatypical depression patients. It remains possible that early trauma has a causal influence on later development of atypical depression. However, this does not explain increased trauma following depression onset. Alternatively, other factors, such as a chaotic environment, anxious-ambivalent attachment styles,45 and personality pathology, determining poor relationship choices and interpersonal problems could be associated with both increased trauma and depressive illness. It is also possible that trauma and atypical depression have a complex and potentially bidirectional relationship. For instance, trauma may induce atypical depression features through adaptive responses of the central nervous system,8,25-32 chromosomal changes,46,47 and interplay with genes,48-50 while atypical depression may make one more prone to trauma through its characteristic mood state. Any of these possibilities would be consistent with findings that victims of trauma are more likely than nonvictims to experience subsequent traumas.35,51
Although we predicted that rejection sensitivity and mood reactivity would partially mediate the relationship between trauma and atypical depression, this was not the case in our sample. It seems that the 5 atypical depression features combine into a phenomenologically distinct disorder that accounts for more variance in trauma reporting than any of the features alone. This finding should be replicated with more detailed documentation of trauma. For example, it is possible that certain atypical depression features are associated with particular types of trauma, such as those that are interpersonal in nature.
There are some limitations of this study that merit consideration. The type of patient who presents for participation in free medication studies may represent 1 subtype of depressed individuals, in terms of both exclusion criteria imposed by the researchers and motivation for treatment. For instance, few patients had bulimia or anorexia nervosa and none had bipolar disorder in our sample, which helps control potentially confounding variables52-55 but also limits the generalizability of our findings. Further, personality disorders are associated with both trauma56,57 and atypical depression,58,59 but their influence could not be examined, as they are not assessed at the Depression Evaluation Service. However, we found an association of somatoform diagnoses with atypical depression, which confirms prior findings of high rates of somatization disorder in atypical depression.60 Although somatoform disorders have been associated with trauma,61,62 they were found in only 5.7% of our sample, so it is unlikely that this variable accounts for our main finding. Nevertheless, larger and more inclusive samples are needed to fully examine the role of comorbidity in the relationship between trauma and atypical depression and to generalize our findings to a broader population of depressed individuals.
Further, an important limitation is that although each patient was systematically asked about trauma history during administration of the SCID-I and social history interview, a comprehensive list of specific event types was not consistently probed for. This unstandardized assessment of trauma made it difficult to evaluate trauma in terms of type, severity, and duration, any of which could be important, so future studies should utilize validated trauma scales.
Finally, self-reported trauma history that relied on retrospective recall makes it possible that subjectivity and recall bias were more pronounced in atypical depression patients than nonatypical depression patients. It may be helpful to attain independent corroboration of traumatic events to minimize recall bias.
Because of these limitations, our results can speak only to differences in reporting of trauma during interviews; however, reporting of trauma may be a critically important variable itself, as it can be an indicator of a patient’s own life experience. Indeed, corroboration of reported events is often unavailable to clinicians. Therefore, the unstandardized collection of trauma history used in this study may reflect clinical practice better than more sophisticated measures. Thus, when clinicians encounter depressed patients who also report both atypical features and histories of trauma, we suggest (1) keeping in mind the possible effects of mood on the initial experience of events, recall bias, and reporting of events; (2) considering traumatic events throughout the lifespan; and (3) maximizing the standardization of information collection between varying types of patients by using validated, self-rated trauma history questionnaires.
Despite several limitations, our study confirms a link between lifetime trauma and atypical depression and thus justifies the need for further research into this observed relationship. Our findings suggest that the relationship may be more complex than previously accounted for and that studies limiting trauma inquiries to childhood or life periods before depression may be leaving out half of the picture.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Author affiliations: Depression Evaluation Service, New York State Psychiatric Institute (all authors); and Department of Clinical Psychiatry, Columbia University, College of Physicians and Surgeons (Dr Stewart), New York, New York.
Author contributions: Mss Withers and Tarasoff are equally contributing co-first authors.
Financial disclosure: Dr Stewart has received honoraria from Bristol-Myers Squibb, Forest, Organon, Shire, and Somerset; has received consulting fees from Biovail, Merck, Organon, and Wyeth; has received research funding from Eli Lilly, GlaxoSmithKline, Organon, and Pfizer; has received study medication from GlaxoSmithKline and Forest; has given speaking engagements paid for by Eli Lilly, GlaxoSmithKline, Organon, and Pfizer; has been informed he will receive money from Biovail in consideration of their intent to file a patent based on work done by him and colleagues; has received other funding support from New York State Office of Mental Health, Research Foundation for Mental Hygiene (New York State), NARSAD, and the National Institute of Mental Health; and owns mutual funds and other managed accounts which own stock in pharmaceutical companies. Mss Withers and Tarasoff report no financial or other relationships relevant to the subject of this article.
Funding/support: The current study was not supported by grants or other financial resources.
REFERENCES
1. Bifulco A, Brown GW, Adler Z. Early sexual abuse and clinical depression in adult life. Br J Psychiatry. 1991;159(1):115-122. PubMed doi:10.1192/bjp.159.1.115
2. Kessler RC, Davis CG, Kendler KS. Childhood adversity and adult psychiatric disorder in the US National Comorbidity Survey. Psychol Med. 1997;27(5):1101-1119. PubMed doi:10.1017/S0033291797005588
3. Zlotnick C, Warshaw M, Shea MT, et al. Trauma and chronic depression among patients with anxiety disorders. J Consult Clin Psychol. 1997;65(2):333-336. PubMed doi:10.1037/0022-006X.65.2.333
4. Bernet CZ, Stein MB. Relationship of childhood maltreatment to the onset and course of major depression in adulthood. Depress Anxiety. 1999;9(4):169-174. PubMed doi:10.1002/(SICI)1520-6394(1999)9:4<169::AID-DA4>3.0.CO;2-2
5. Brown J, Cohen P, Johnson JG, et al. Childhood abuse and neglect: specificity of effects on adolescent and young adult depression and suicidality. J Am Acad Child Adolesc Psychiatry. 1999;38(12):1490-1496. PubMed doi:10.1097/00004583-199912000-00009
6. Quitkin FM, Rabkin JG, Stewart JW, et al. Sleep of atypical depressives. J Affect Disord. 1985;8(1):61-67. PubMed doi:10.1016/0165-0327(85)90073-4
7. Bruder GE, Quitkin FM, Stewart JW, et al. Cerebral laterality and depression: differences in perceptual asymmetry among diagnostic subtypes. J Abnorm Psychol. 1989;98(2):177-186. PubMed doi:10.1037/0021-843X.98.2.177
8. Stewart JW, Quitkin FM, McGrath PJ, et al. Defining the boundaries of atypical depression: evidence from the HPA axis supports course of illness distinctions. J Affect Disord. 2005;86(2-3):161-167. PubMed doi:10.1016/j.jad.2005.01.009
9. Liebowitz MR, Quitkin FM, Stewart JW, et al. Phenelzine v imipramine in atypical depression: a preliminary report. Arch Gen Psychiatry. 1984;41(7):669-677. PubMed doi:10.1001/archpsyc.1984.01790180039005
10. Quitkin FM, McGrath PJ, Stewart JW, et al. Atypical depression, panic attacks, and response to imipramine and phenelzine: a replication. Arch Gen Psychiatry. 1990;47(10):935-941. PubMed doi:10.1001/archpsyc.1990.01810220051006
11. Cristancho MA, O’ Reardon JP, Thase ME. Atypical depression in the 21st century: diagnostic and treatment issues. Psychiatric Times. 2011;28:42-46.
12. Stewart JW, McGrath PJ, Rabkin JG, et al. Atypical depression: a valid clinical entity? Psychiatr Clin North Am. 1993;16(3):479-495. PubMed
13. Harkness KL, Monroe SM. Childhood adversity and the endogenous versus nonendogenous distinction in women with major depression. Am J Psychiatry. 2002;159(3):387-393. PubMed doi:10.1176/appi.ajp.159.3.387
14. Frank E, Anderson B, Reynolds CF 3rd, et al. Life events and the research diagnostic criteria endogenous subtype: a confirmation of the distinction using the Bedford College methods. Arch Gen Psychiatry. 1994;51(7):519-524. PubMed doi:10.1001/archpsyc.1994.03950070011005
15. Parker G, Gladstone G, Wilhelm K, et al. Dysfunctional parenting: over-representation in non-melancholic depression and capacity of such specificity to refine sub-typing depression measures. Psychiatry Res. 1997;73(1-2):57-71. PubMed doi:10.1016/S0165-1781(97)00113-3
16. Matza LS, Revicki DA, Davidson JR, et al. Depression with atypical features in the National Comorbidity Survey: classification, description, and consequences. Arch Gen Psychiatry. 2003;60(8):817-826. PubMed doi:10.1001/archpsyc.60.8.817
17. Levitan RD, Parikh SV, Lesage AD, et al. Major depression in individuals with a history of childhood physical or sexual abuse: relationship to neurovegetative features, mania, and gender. Am J Psychiatry. 1998;155(12):1746-1752. PubMed
18. Young EA, Abelson JL, Curtis GC, et al. Childhood adversity and vulnerability to mood and anxiety disorders. Depress Anxiety. 1997;5(2):66-72. PubMed doi:10.1002/(SICI)1520-6394(1997)5:2<66::AID-DA2>3.0.CO;2-3
19. Brown GW, Craig TKJ, Harris TO, et al. Development of a retrospective interview measure of parental maltreatment using the Childhood Experience of Care and Abuse (CECA) instrument—a life-course study of adult chronic depression-1. J Affect Disord. 2007;103(1-3):205-215. PubMed doi:10.1016/j.jad.2007.05.022
20. Wiersma JE, Hovens JG, van Oppen P, et al. The importance of childhood trauma and childhood life events for chronicity of depression in adults. J Clin Psychiatry. 2009;70(7):983-989. PubMed doi:10.4088/JCP.08m04521
21. Levitan RD, Rector NA, Sheldon T, et al. Childhood adversities associated with major depression and/or anxiety disorders in a community sample of Ontario: issues of co-morbidity and specificity. Depress Anxiety. 2003;17(1):34-42. PubMed doi:10.1002/da.10077
22. Stewart JW, McGrath PJ, Quitkin FM, et al. DSM-IV depression with atypical features: is it valid? Neuropsychopharmacology. 2009;34(13):2625-2632. PubMed doi:10.1038/npp.2009.99
23. Novick JS, Stewart JW, Wisniewski SR, et al;; STAR*D investigators. Clinical and demographic features of atypical depression in outpatients with major depressive disorder: preliminary findings from STAR*D. J Clin Psychiatry. 2005;66(8):1002-1011. PubMed doi:10.4088/JCP.v66n0807
24. Posternak MA, Zimmerman M. Partial validation of the atypical features subtype of major depressive disorder. Arch Gen Psychiatry. 2002;59(1):70-76. PubMed doi:10.1001/archpsyc.59.1.70
25. Carpenter LL, Tyrka AR, Ross NS, et al. Effect of childhood emotional abuse and age on cortisol responsivity in adulthood. Biol Psychiatry. 2009;66(1):69-75. PubMed doi:10.1016/j.biopsych.2009.02.030
26. Fries E, Hesse J, Hellhammer J, et al. A new view on hypocortisolism. Psychoneuroendocrinology. 2005;30(10):1010-1016. PubMed doi:10.1016/j.psyneuen.2005.04.006
27. Yehuda R. Biology of posttraumatic stress disorder. J Clin Psychiatry. 2001;62(suppl 17):41-46. PubMed
28. Stein MB, Yehuda R, Koverola C, et al. Enhanced dexamethasone suppression of plasma cortisol in adult women traumatized by childhood sexual abuse. Biol Psychiatry. 1997;42(8):680-686. PubMed doi:10.1016/S0006-3223(96)00489-1
29. Newport DJ, Heim C, Bonsall R, et al. Pituitary-adrenal responses to standard and low-dose dexamethasone suppression tests in adult survivors of child abuse. Biol Psychiatry. 2004;55(1):10-20. doi:10.1016/S0006-3223(03)00692-9 PubMed
30. Karlović D, Serretti A, Vrkić N, et al. Serum concentrations of CRP, IL-6, TNF-α and cortisol in major depressive disorder with melancholic or atypical features. Psychiatry Res. 2012;198(1):74-80. PubMed doi:10.1016/j.psychres.2011.12.007
31. Anisman H, Ravindran AV, Griffiths J, et al. Endocrine and cytokine correlates of major depression and dysthymia with typical or atypical features. Mol Psychiatry. 1999;4(2):182-188. PubMed doi:10.1038/sj.mp.4000436
32. Levitan RD, Vaccarino FJ, Brown GM, et al. Low-dose dexamethasone challenge in women with atypical major depression: pilot study. J Psychiatry Neurosci. 2002;27(1):47-51. PubMed
33. Wong ML, Kling MA, Munson PJ, et al. Pronounced and sustained central hypernoradrenergic function in major depression with melancholic features: relation to hypercortisolism and corticotropin-releasing hormone. Proc Natl Acad Sci U S A. 2000;97(1):325-330. PubMed doi:10.1073/pnas.97.1.325
34. Gold PW, Chrousos GP. Organization of the stress system and its dysregulation in melancholic and atypical depression: high vs low CRH/NE states. Mol Psychiatry. 2002;7(3):254-275. PubMed doi:10.1038/sj.mp.4001032
35. Breslau N, Davis GC, Peterson EL, et al. A second look at comorbidity in victims of trauma: the posttraumatic stress disorder-major depression connection. Biol Psychiatry. 2000;48(9):902-909. PubMed doi:10.1016/S0006-3223(00)00933-1
36. First MB, Spitzer RL, Gibbon M, et al. Structured Clinical Interview for DSM-IV-TR Axis I Disorders-Patient Edition (with psychotic screen). New York, NY: Biometrics Research Department, New York State Psychiatric Institute; 2002.
37. Davidson JR, Miller RD, Turnbull CD, et al. Atypical depression. Arch Gen Psychiatry. 1982;39(5):527-534. PubMed doi:10.1001/archpsyc.1982.04290050015005
38. Breslau N, Chilcoat HD, Kessler RC, et al. Previous exposure to trauma and PTSD effects of subsequent trauma: results from the Detroit Area Survey of Trauma. Am J Psychiatry. 1999;156(6):902-907. PubMed
39. Niedenthal PM, Setterlund MB. Emotion congruence in perception. Pers Soc Psychol Bull. 1994;20(4):401-411. doi:10.1177/0146167294204007
40. Hansen CH, Shantz CA. Emotion-specific priming: CONGRUENCE effects on affect and recognition across negative emotions. Pers Soc Psychol Bull. 1995;21(6):548-557. doi:10.1177/0146167295216001
41. Bower GH. Mood and memory. Am Psychol. 1981;36(2):129-148. PubMed doi:10.1037/0003-066X.36.2.129
42. Watkins PC, Vache K, Verney SP, et al. Unconscious mood-congruent memory bias in depression. J Abnorm Psychol. 1996;105(1):34-41. PubMed doi:10.1037/0021-843X.105.1.34
43. Kensinger EA. Remembering the details: effects of emotion. Emot Rev. 2009;1(2):99-113. PubMed doi:10.1177/1754073908100432
44. Ritchey M, Dolcos F, Cabeza R. Role of amygdala connectivity in the persistence of emotional memories over time: an event-related FMRI investigation. Cereb Cortex. 2008;18(11):2494-2504. PubMed doi:10.1093/cercor/bhm262
45. Levitan RD, Atkinson L, Pedersen R, et al. A novel examination of atypical major depressive disorder based on attachment theory. J Clin Psychiatry. 2009;70(6):879-887. PubMed doi:10.4088/JCP.07m03306
46. Chrousos GP. Stressors, stress, and neuroendocrine integration of the adaptive response: the 1997 Hans Selye Memorial Lecture. Ann N Y Acad Sci. 1998;851(1):311-335. PubMed doi:10.1111/j.1749-6632.1998.tb09006.x
47. Simon NM, Smoller JW, McNamara KL, et al. Telomere shortening and mood disorders: preliminary support for a chronic stress model of accelerated aging. Biol Psychiatry. 2006;60(5):432-435. PubMed doi:10.1016/j.biopsych.2006.02.004
48. Caspi A, Sugden K, Moffitt TE, et al. Influence of life stress on depression: moderation by a polymorphism in the 5-HTT gene. Science. 2003;301(5631):386-389. PubMed doi:10.1126/science.1083968
49. Kaufman J, Yang B-Z, Douglas-Palumberi H, et al. Social supports and serotonin transporter gene moderate depression in maltreated children. Proc Natl Acad Sci U S A. 2004;101(49):17316-17321. PubMed doi:10.1073/pnas.0404376101
50. Shyn SI, Hamilton SP. The genetics of major depression: moving beyond the monoamine hypothesis. Psychiatr Clin North Am. 2010;33(1):125-140. PubMed doi:10.1016/j.psc.2009.10.004
51. Taylor BW, MacIntyre J, Forgeron P. Trauma recurrence in the pediatric emergency population. J Trauma. 1999;46(3):479-482. PubMed doi:10.1097/00005373-199903000-00024
52. Rothschild R, Quitkin HM, Quitkin FM, et al. A double-blind placebo-controlled comparison of phenelzine and imipramine in the treatment of bulimia in atypical depressives. Int J Eat Disord. 1994;15(1):1-9. PubMed doi:10.1002/1098-108X(199401)15:1<1::AID-EAT2260150102>3.0.CO;2-E
53. Sullivan PF, Bulik CM, Carter FA, et al. The significance of a history of childhood sexual abuse in bulimia nervosa. Br J Psychiatry. 1995;167(5):679-682. PubMed doi:10.1192/bjp.167.5.679
54. Benazzi F. Atypical depression with hypomanic symptoms. J Affect Disord. 2001;65(2):179-183. PubMed doi:10.1016/S0165-0327(00)00266-4
55. Neria Y, Bromet EJ, Carlson GA, et al. Assaultive trauma and illness course in psychotic bipolar disorder: findings from the Suffolk county mental health project. Acta Psychiatr Scand. 2005;111(5):380-383. PubMed doi:10.1111/j.1600-0447.2005.00530.x
56. Carr SN, Francis AJP. Do early maladaptive schemas mediate the relationship between childhood experiences and avoidant personality disorder features? a preliminary investigation in a non-clinical sample. Cognit Ther Res. 2010;34(4):343-358. doi:10.1007/s10608-009-9250-1
57. Herman JL, Perry JC, van der Kolk BA. Childhood trauma in borderline personality disorder. Am J Psychiatry. 1989;146(4):490-495. PubMed
58. Alpert JE, Uebelacker LA, McLean NE, et al. Social phobia, avoidant personality disorder and atypical depression: co-occurrence and clinical implications. Psychol Med. 1997;27(3):627-633. PubMed doi:10.1017/S0033291797004765
59. Perugi G, Toni C, Travierso MC, et al. The role of cyclothymia in atypical depression: toward a data-based reconceptualization of the borderline-bipolar II connection. J Affect Disord. 2003;73(1-2):87-98. PubMed doi:10.1016/S0165-0327(02)00329-4
60. Horwath E, Johnson J, Weissman MM, et al. The validity of major depression with atypical features based on a community study. J Affect Disord. 1992;26(2):117-125. PubMed doi:10.1016/0165-0327(92)90043-6
61. Pribor EF, Yutzy SH, Dean JT, et al. Briquet’s syndrome, dissociation, and abuse. Am J Psychiatry. 1993;150(10):1507-1511. PubMed
62. Sack M, Lahmann C, Jaeger B, et al. Trauma prevalence and somatoform symptoms: are there specific somatoform symptoms related to traumatic experiences? J Nerv Ment Dis. 2007;195(11):928-933. PubMed doi:10.1097/NMD.0b013e3181594846
This PDF is free for all visitors!