Major Depressive Disorder, Mental Health Care, and the Use of Guidelines in the Middle East
A large gap exists between the number of people needing treatment and the number of people receiving treatment for depression in the Middle East. Barriers to mental health care in the region have included the lack of education for primary health care providers about mental illnesses, the scarcity of trained mental health care specialists, the lack of resources in developing countries, and the stigmatization of mental illness in Middle Eastern cultures. Guidelines for the treatment of depression have not been developed in most countries of the region. Guidelines have been published for both general practitioners and for psychiatrists in Turkey, and they are similar to guidelines published in the West. These guidelines are assessed using the AGREE instrument. Although guidelines recommend antidepressants as a first-line treatment for depression, many physicians in Middle Eastern countries prescribe benzodiazepines. One reason for this treatment gap may be that patients with depression often seek treatment from primary care providers and report somatic symptoms. Primary care providers may not be as knowledgeable about the diagnosis of depression or its treatment as psychiatrists and may not have access to certain classes of medications. More education for both physicians and patients in the Middle East is needed to decrease the stigma associated with depression.
(J Clin Psychiatry 2010;71[suppl E1]:e07)
From the Department of Psychiatry, ÅžiÅŸli Etfal Teaching and Research Hospital, Istanbul, Turkey.
This article is derived from the roundtable discussion "International Consensus Group on Depression," which was held on September 1, 2009, in Tokyo, Japan, and supported by an educational grant from GlaxoSmithKline.
Dr Karamustafalıoğlu has received grant/research support from Pfizer and Sanovel; has received honoraria from Lundbeck, Wyeth, Bristol-Myers Squibb, Abdi İbrahim, Egis, and Eczacıbaşı-Zentiva; and is a member of the speakers/advisory boards for Johnson & Johnson, GlaxoSmithKline, Eli Lilly, and Pfizer.
Corresponding author: OÄŸuz KaramustafalıoÄŸlu, MD, Tevfik SaÄŸlam Cad., YalçindaÄŸ, Apt. No. 13/2 DikilitaÅŸ/Bakırköy, Istanbul, Turkey ([email protected]).
doi:10.4088/JCP.9058se1c07gry
© Copyright 2010 Physicians Postgraduate Press, Inc.
The Middle East encompasses a heterogeneous array of countries with distinct cultures, customs, ethnicities, and languages. However, although great strides have been made in recent decades, one commonality among these nations has been the lack of available mental health care services.1 Barriers to mental health care in the region have included the lack of education for primary health care providers about mental illnesses, the scarcity of trained mental health care specialists, the lack of resources in developing countries, and the stigmatization of mental illness in Middle Eastern cultures.2,3
Some studies4-8 have shown a high prevalence of mental disorders in the Middle East, partly due to the strong impact that exposure to war events has on its population.1,4,7,8 The changes occurring in traditional cultures due to urbanization, such as the move away from extended families toward nuclear families, are another contributing factor.9 The growing problem of substance abuse in the region and the major natural disasters that have occurred in the last decade, including earthquakes and floods, have added to the number of psychosocial and environmental stressors that can increase the rates of mental disorders.1 However, some Middle Eastern countries have been slow to respond to the growing need to improve the quality and availability of mental health care services. Improving mental health care in the region is a multidimensional process, complicated by differing cultures, customs, and cost pressures within each country, but mental health providers can be instrumental in developing local treatment guidelines and in promoting the adoption of an evidence-based culture of practice for treating patients with mental disorders.
For Clinical Use
- In the Middle East, patients who present with somatic complaints rather than mood complaints should be screened for symptoms of depression.
- Until more regional guidelines are developed, physicians in the Middle East should follow international guidelines when treating patients for depression.
- Physicians in the Middle East, especially primary care physicians, should receive more training regarding the appropriate use of antidepressants and benzodiazepines.
- Patients in the Middle East need more education about depression and other mental illnesses to reduce the negative feelings associated with these disorders.
MENTAL HEALTH CARE IN THE MIDDLE EAST
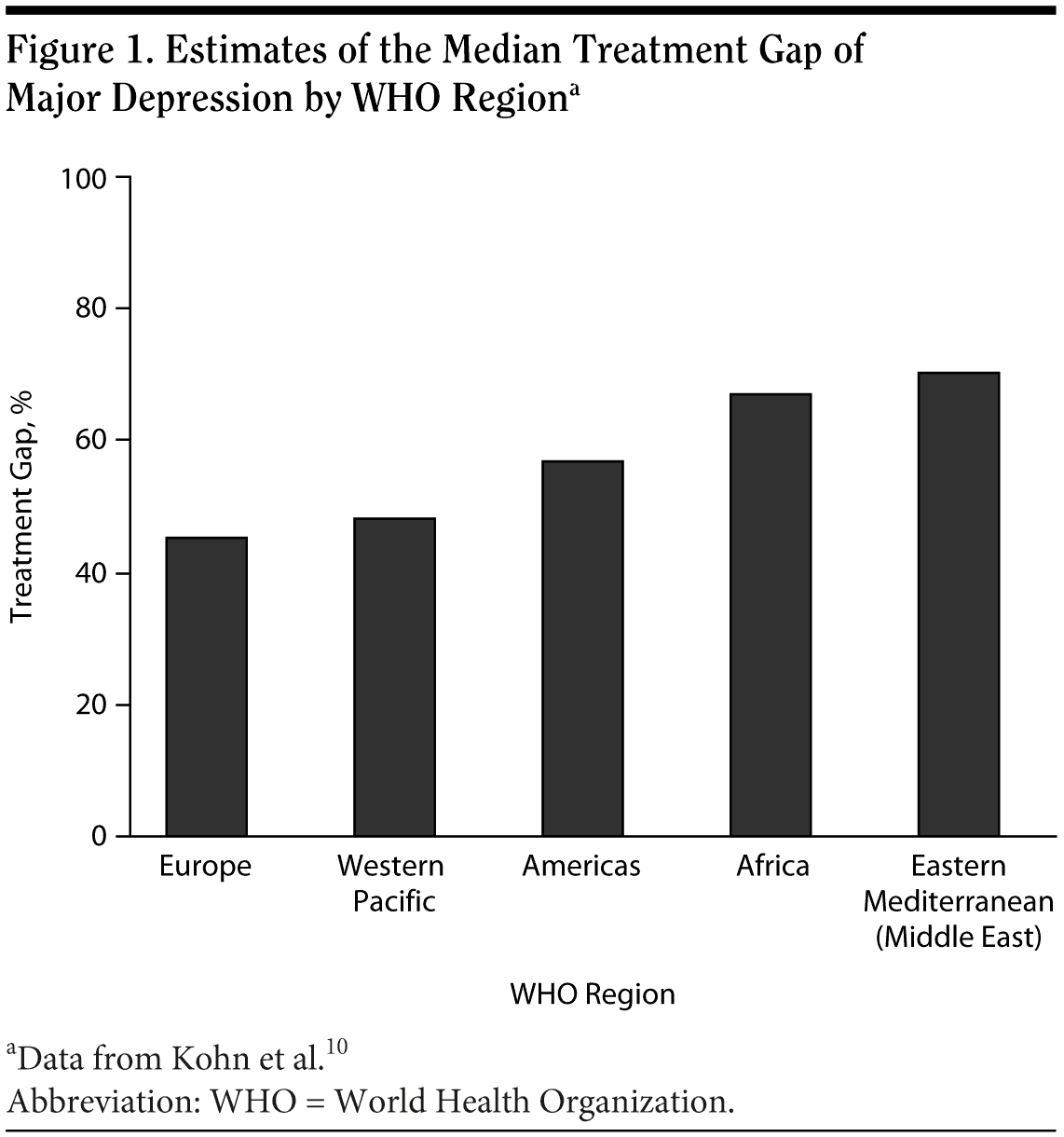
The treatment gap that exists for mental disorders has been well documented, both around the world and specifically in the Middle East (Figure 1).10 For instance, a Lebanese study8 found that one-fourth of the population met the criteria for at least 1 lifetime psychiatric disorder, but less than half of those with mood disorders had ever been treated for that diagnosis. For those who did receive treatment, the median delay from onset of the mood disorder to treatment was 6 years. Treatment rates for other diagnoses, such as anxiety or substance abuse, were even lower. As Lebanon has one of the highest ratios of physicians to the general population in the Middle East, these low treatment levels are more likely due to factors such as the stigma attached to mental illness, the lack of awareness of mental disorders among both patients and health care providers, and the lack of specialized mental health care providers, than to the shortage of physicians that is seen in some Middle Eastern countries.
The lack of psychiatrists and other mental health care specialists in the region and the stigma associated with mental illness mean that most patients will seek treatment from a primary care provider, and many will complain of somatic symptoms such as headache, backache, and abdominal pain rather than mood or anxiety symptoms. In fact, almost half of the primary care patients in the United Arab Emirates who were found to have a psychiatric disorder described their symptoms as somatic instead of psychological.11 Another study3 in the United Arab Emirates demonstrated the need for additional education and training regarding psychiatric illnesses among general practitioners. Primary care physicians were surveyed on their knowledge about anxiety, depression, and drug interactions, and a majority of the survey questions were answered incorrectly by at least 50% of the physicians. A study12 in Saudi Arabia also found that primary care physicians fared poorly when diagnosing somatization disorder and depression. This study recommended additional psychiatric training for primary care providers and patient education regarding the need to report psychological symptoms to family physicians.
In Jordan, Nasir and Al-Qutob2 used a series of focus groups of primary care providers (both physicians and nonphysicians) to examine barriers to the diagnosis and treatment of depression. Cultural resistance to the diagnosis (ie, Arab culture emphasizes the community over the individual, making individual treatment more difficult), the perceived stigma of depression, the lack of appropriate treatments in the primary care setting, and the lack of education regarding depression among primary care providers all contributed to a low level of recognition and treatment of depression. Awareness of specific diagnostic criteria was low, and the need for ongoing care was rarely recognized.
TREATMENT GUIDELINES IN THE MIDDLE EAST
The need for comprehensive guidelines for the identification, diagnosis, and treatment of depression in the Middle East is evident. However, a thorough online keyword search, an investigation of the Web sites of psychiatry and psychology associations for each country, and discussions with opinion leaders in the region revealed that most countries have not yet developed these guidelines. Only 2 depression treatment guidelines, both from Turkey, were identified, 1 published for primary care physicians in 2003 by the Ministry of Health Mental Health Department13 and another published in 2008 for psychiatrists by the Mood Disorders Study Group of the Psychiatric Association of Turkey.14
Guideline Recommendations
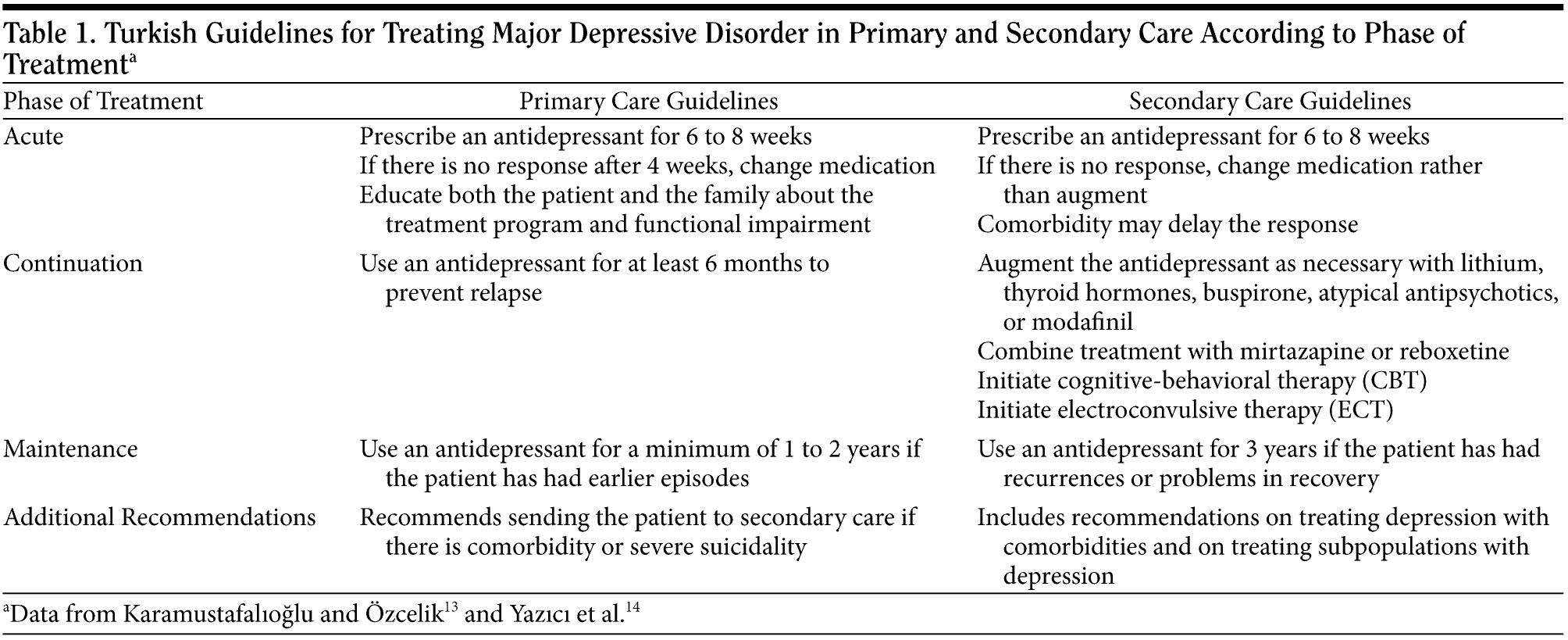
Both guidelines give recommendations for treating depression during the acute, continuation, and maintenance phases of treatment (Table 1). The guidelines both call for antidepressant treatment for 6 to 8 weeks for acute care. The primary care guidelines advise waiting a minimum of 4 weeks after treatment initiation before changing medication due to lack of response, and note the importance of educating both the patient and the patient’s family about the treatment program and about the functional impairment that depression causes. The guidelines for psychiatrists recommend changing medications (rather than augmenting the original medication) if the patient has no response, and also note that comorbidity may delay the patient’s response to treatment.
In the continuation phase, the primary care guidelines recommend continuing the antidepressant treatment for at least 6 months to prevent relapse. The psychiatric guidelines recommend augmentation and combination therapies during the continuation phase if the patient has a partial response to the first medication. In addition, cognitive-behavioral therapy, electroconvulsive therapy, and other stimulation methods may be initiated.
For maintenance care, a minimum of 1 to 2 years of antidepressant treatment is recommended by the primary care guidelines for patients with earlier episodes of depression, while the psychiatric guidelines recommend 3 years of antidepressant treatment for patients with recurrences. The primary care guidelines recommend referrals to secondary care for patients with comorbidity or severe suicidality, while the secondary care guidelines have additional recommendations for treating depression with comorbidities (including anxiety disorders or medical comorbidities such as diabetes) and treating depression in specific subpopulations (including postpartum women and geriatric and adolescent patients).
Guideline Appraisals
Interest in treatment guidelines as a tool for assisting clinicians has grown in recent years, as governmental agencies and health care and professional organizations attempt to improve and standardize patient care. However, certain pitfalls must be avoided when developing these guidelines, including recommendations that lack evidence-based support, guidelines based on personal preference or value judgments, treatment inflexibility that does not account for individual patient circumstances, and recommendations based on priorities other than optimal patient care (eg, cost control).15
In an effort to improve the quality of practice guidelines, an international group of researchers, known as the Appraisal of Guidelines, REsearch and Evaluation (AGREE) Collaboration, developed an appraisal instrument to assess the process and reporting of the development of individual guidelines.16 Although the AGREE instrument does not validate the recommendations contained within a guideline, it does provide a set of criteria that can be used both to appraise existing guidelines and as a framework for developing high-quality guidelines (Table 2). The criteria comprise 6 domains: scope and purpose, stakeholder involvement, rigor of development, clarity and presentation, applicability, and editorial independence. Each of the quality items in the domains is judged on a Likert scale (1 = strongly disagree, 2 = disagree, 3 = agree, and 4 = strongly agree). The overall judgment of whether a set of guidelines should be used has 4 options, ie, strongly recommend, recommend (with provisos or alterations), would not recommend, and unsure.
When evaluated using the AGREE instrument, both of the depression treatment guidelines from Turkey can be recommended with provisos or modifications. In the domain of scope and purpose, the overall objectives, clinical questions covered, and the patients to whom the guidelines were meant to apply are all described at an acceptable level. Both guidelines are also acceptable in the stakeholder involvement domain, except in the area of soliciting patients’ views and preferences.
The rigor of development of these guidelines was not high. The primary care guidelines did not clearly describe the criteria for selecting evidence or the methods used in formulating the recommendations, and neither set of guidelines had external reviews by experts prior to publication or provided a procedure for updating the guidelines.
Regarding clarity and presentation, both guidelines are acceptable in that the recommendations are specific and unambiguous, different options are clearly presented, and key recommendations are easily identified. However, neither set of the guidelines is supported with tools for application.
The guidelines are both poor in the domain of applicability, which refers to addressing potential barriers to applying the recommendations, considering the potential cost implications, and presenting the key review criteria for monitoring and auditing purposes. In the last domain, editorial independence, both guidelines had excellent independence of the editors from the funding body, but neither recorded conflicts of interest among the guideline development members.
PRESCRIBING PATTERNS FOR DEPRESSION MEDICATIONS IN THE MIDDLE EAST
The guidelines published in Turkey recommend the use of antidepressants as first-line treatment for depression, as do guidelines published in other areas of the world. In addition, most guidelines recommend against the use of benzodiazepines for treating depression, except in a few special cases, because of the risks involved with this class of drugs. However, benzodiazepines are frequently used in Middle Eastern countries to treat depression. One reason may be due to patients with depression in the region seeking treatment from primary care providers. Primary care providers in Jordan reported that they most frequently used benzodiazepines and anticonvulsants to treat patients with depression, partly because those classes of drugs were available to primary care centers whereas antidepressants were not.2 Patients in Jordan must be referred to a psychiatrist for antidepressant treatment, and many patients find treatment by a psychiatrist unacceptable because of the shame they attach to a psychiatric diagnosis.
My associates and I examined benzodiazepine use in Turkey and found that psychiatry and nonpsychiatry residents and, to some extent, specialists, especially in rural areas, lacked knowledge about the pharmacodynamics and pharmacokinetics of these medications.17 Half or fewer physicians knew about the potential for abuse of benzodiazepines, the need to avoid their use in patients with substance use disorders, or the possibility of certain side effects. Rural physicians prescribed benzodiazepines more frequently than urban physicians for depression (P = .009).
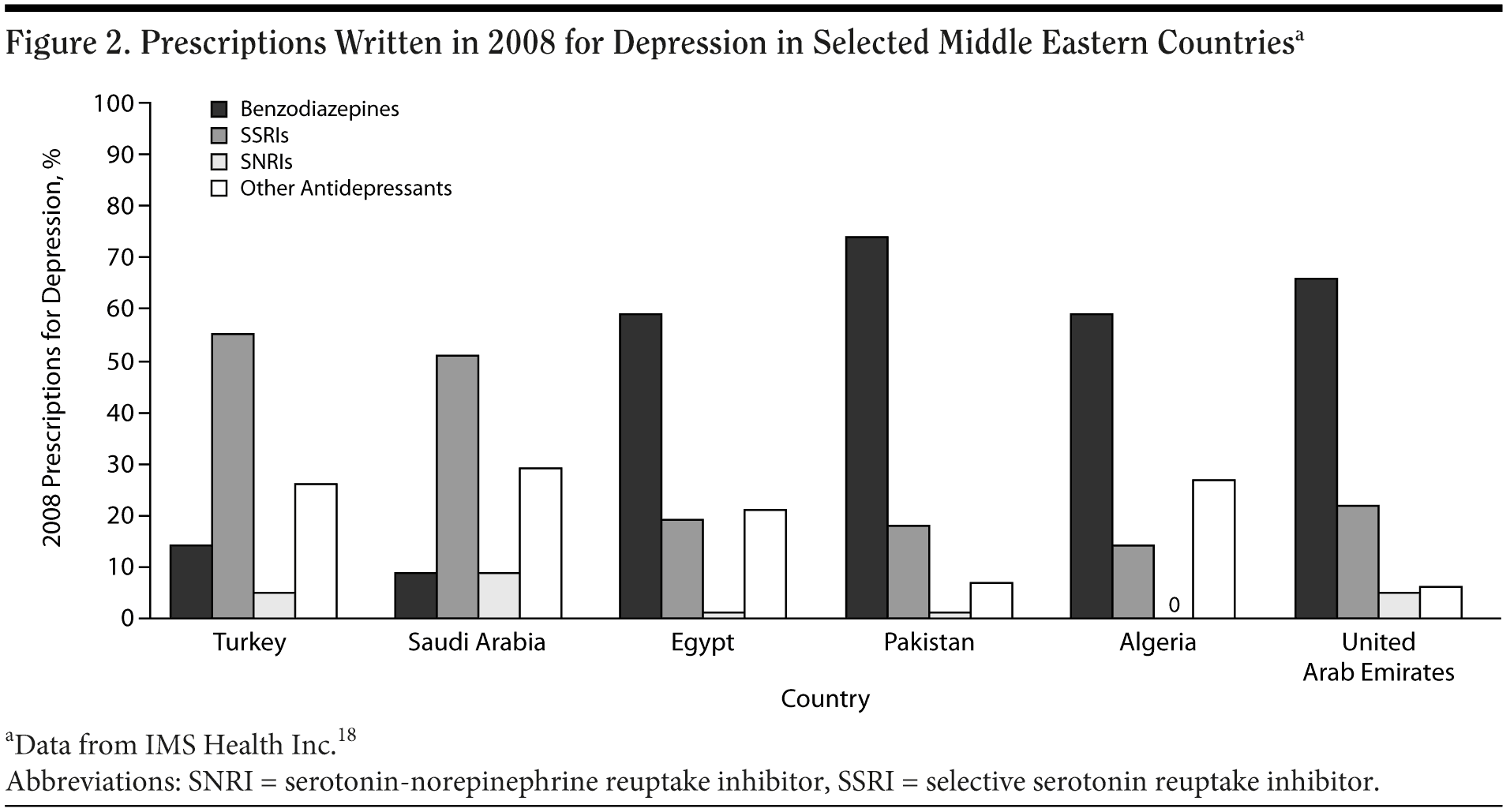
Benzodiazepine use for the treatment of depression in the Middle East does vary by country (Figure 2).18 For example, of all prescriptions written in 2008 for depression in Egypt, Pakistan, Algeria, and the United Arab Emirates, more than 50% were for benzodiazepines, whereas in Turkey and Saudi Arabia, less than 15% of those prescriptions were for benzodiazepines. In Turkey and Saudi Arabia, more than 50% of depression prescriptions were for selective serotonin reuptake inhibitors (SSRIs), while in Egypt, Pakistan, Algeria, and the United Arab Emirates, less than 25% of prescriptions for depression were for SSRIs. In all of these countries, serotonin-norepinephrine reuptake inhibitors (SNRIs) were less than 10% of the prescriptions for depression. Several reasons may account for differing prescribing patterns for antidepressants. For instance, the wealthier countries, such as Saudi Arabia and the United Arab Emirates, have a higher prescription rate for SNRIs than less-wealthy countries. The laws governing the prescribing of medications may also affect these rates. In Turkey, general practitioners cannot prescribe SNRIs directly, but must first refer patients to a psychiatrist. If the psychiatrist authorizes it, the general practitioner can then prescribe an SNRI for the patient; otherwise, these physicians can only prescribe tricyclic antidepressants (TCAs) or SSRIs.
CONCLUSION
A gap exists between the standard of care and actual clinical practice in both diagnosing and treating depression in the Middle East. Most countries in the region lack written guidelines for the treatment of depression, either from government institutions or from psychiatric or professional associations. Guidelines from Turkey have been published for both general practitioners and for psychiatrists, and they are similar to guidelines published in the West. (For information on European and American guidelines, see the article "Major Depressive Disorder Treatment Guidelines in America and Europe" by Jonathan R. T. Davidson, MD.19) However, although most international guidelines and those from Turkey recommend antidepressants for treating depression, many physicians in Middle Eastern countries prescribe benzodiazepines. One reason may be that patients often seek treatment from primary care providers for depression, in part due to the lack of specialized psychiatric providers in the Middle East, but also because of the stigma attached to mental illness in many Middle Eastern cultures. Primary care providers may not be as knowledgeable about antidepressants as psychiatrists, and, in fact, may not have access to certain classes of medications. To improve the treatment of depression in the Middle East, more treatment guidelines tailored to the region need to be developed, physicians need more education on identifying and treating psychiatric disorders, and patient education is needed to reduce the stigma associated with depression and other mental disorders in the region.
DISCUSSION
Dr Terao: I see in Turkey and Saudi Arabia a very flowing algorithm, where fewer benzodiazepines and more SSRIs are prescribed. Why are there such differences in prescribing patterns in other countries?
Dr Karamustafalıoğlu: Well, it may partly be a matter of education and getting the data out. In Turkey, we have a lot of educational programs, so it is easier to follow the European style of treatment. For Saudi Arabia, it is my understanding that many doctors accepted to practice there were licensed in either England or the United States.
Professor Nutt: But it may also be cost factors, and perhaps how the medications are paid for. I am not sure to what extent the government or the people themselves pay for these medications. For instance, in some countries, the tricyclics might be much cheaper than the SSRIs.
Dr Papakostas: Another thing to keep in mind is the number of patents in some countries. A lack of patent protection for certain medications may render one type of agent cheaper than others in some countries.
Dr Karamustafalıoğlu: Yes, that is true. There is no patent protection in Turkey for some medications, like the SSRI fluoxetine, which is therefore inexpensive. But the newer antidepressants, like the SNRI duloxetine, do have patent protection.
Dr Papakostas: And, in some countries, even the newer antidepressants may not have patent protection, which may be another factor that might explain the differences in prescribing practices.
Dr Davidson: But, in some countries, physicians are actually prescribing benzodiazepines for depression instead of antidepressants. In Pakistan, about 70% of depression prescriptions are for a benzodiazepine, and about 30% are for antidepressants. Education is needed about using antidepressants for depression regardless of how inexpensive some benzodiazepines may be compared with antidepressants.
Dr Papakostas: Sometimes patients will self-medicate with benzodiazepines, perhaps because a friend told them the medication is good for depression.
Dr Karamustafalıoğlu: These data reflect only prescription rates. I am not sure of the regulations in all of the countries, but in most you cannot get benzodiazepines without a prescription. Since 1981, Turkey has had a special prescription for tranquilizers, so that these prescriptions can be tracked electronically. If a doctor is prescribing a higher number of these medications than other doctors, the physician will receive a warning letter from the government about the situation. If it continues, an inspector comes in to try and see why it is happening.
Professor Nutt: So, there is an effort to restrict benzodiazepine use. Thank you very much for these interesting data.
Disclosure of off-label usage: The author has determined that, to the best of his knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration−approved labeling has been presented in this article.
REFERENCES
1. World Health Organization, Regional Office for the Eastern Mediterranean. Mental health in the Eastern Mediterranean Region: reaching the unreached. Cairo: World Health Organization, Regional Office for the Eastern Mediterranean; 2006.
2. Nasir LS, Al-Qutob R. Barriers to the diagnosis and treatment of depression in Jordan: a nationwide qualitative study. J Am Board Fam Pract. 2005;18(2):125-131. doi:10.3122/jabfm.18.2.125 PubMed
3. Saeed M, McCall L. General practitioners knowledge and attitude towards anxiety and depression in Abu Dhabi. http://www.mejfm.com/journal/Jan06/GP-Knowledge.htm. Published 2006. Accessed October 8, 2009.
4. Ghosh N, Mohit A, Murthy RS. Mental health promotion in post-conflict countries. J R Soc Promot Health. 2004;124(6):268-270. doi:10.1177/146642400412400614 PubMed
5. Al-Khathami AD, Ogbeide DO. Prevalence of mental illness among Saudi adult primary-care patients in Central Saudi Arabia. Saudi Med J. 2002;23(6):721-724. PubMed
6. Al-Otaibi B, Al-Weqayyan A, Taher H, et al. Depressive symptoms among Kuwaiti population attending primary healthcare setting: prevalence and influence of sociodemographic factors. Med Princ Pract. 2007;16(5):384-388. doi:10.1159/000104813 PubMed
7. Mukhamadiev DM. Aspects of depressive states in repatriated female refugees. Ah Nevrol Psikhiatr Im S S Korsakova. 2003;103(1):21-23.
8. Karam EG, Mneimneh ZN, Dimassi H, et al. Lifetime prevalence of mental disorders in Lebanon: first onset, treatment, and exposure to war. PLoS Med. 2008;5(4):e61. doi:10.1371/journal.pmed.0050061 PubMed
9. Taqui AM, Itrat A, Qidwai W, et al. Depression in the elderly: does family system play a role? a cross-sectional study. BMC Psychiatry. 2007;7(1):57. doi:10.1186/1471-244X-7-57 PubMed
10. Kohn R, Saxena S, Levav I, et al. The treatment gap in mental health care. Bull World Health Organ. 2004;82(11):858-866. PubMed
11. El-Rufaie OEF, Al-Sabosy MA, Bener A, et al. Somatized mental disorder among primary care Arab patients: I. prevalence and clinical and sociodemographic characteristics. J Psychosom Res. 1999;46(6):549-555. doi:10.1016/S0022-3999(98)00101-9 PubMed
12. Becker SM. Detection of somatization and depression in primary care in Saudi Arabia. Soc Psychiatry Psychiatr Epidemiol. 2004;39(12):962-966. doi:10.1007/s00127-004-0835-4 PubMed
13. Karamustafalioglu O, Ozcelik B, eds, for the Ministry of Mental Health Department. Mental health in primary care [in Turkish]. Istanbul, Turkey: Renk Press; 2003.
14. Yazici O, Oral ET, Vahip S, eds, for the Mood Disorders Study Group of the Psychiatric Association of Turkey. Depression treatment guideline [in Turkish]. Istanbul, Turkey: Tuna Press; 2008.
15. Woolf SH, Grol R, Hutchinson A, et al. Clinical guidelines: potential benefits, limitations, and harms of clinical guidelines. BMJ. 1999;318(7182):527-530. PubMed
16. AGREE Collaboration. Development and validation of an international appraisal instrument for assessing the quality of clinical practice guidelines: the AGREE project. Qual Saf Health Care. 2003;12(1):18-23. doi:10.1136/qhc.12.1.18 PubMed
17. Karamustafalioglu O, Yilmaz M, Ozcelik B, et al. Benzodiazepine prescription patterns of psychiatry and non-psychiatry residents and specialists. Klinik Psikofarmakoloji Bulteni. 2005;15(1):5-13.
18. Health IMS. IMS Health dataview. http://www.imshealth.com. Published 2009. Accessed November 25, 2009.
19. Davidson JRT. Major depressive disorder treatment guidelines in America and Europe. J Clin Psychiatry. 2010;71(suppl E1):e04. doi:10.4088/JCP.9058se1C.04gry.