Major Depressive Disorder Treatment Guidelines in America and Europe
The various major American and European guidelines for the treatment of depression provide similar basic principles of treatment, which include individualizing the treatment plan, preparing the patient for potential long-term treatment, providing measurement-based care, and treating to remission. While the guidelines are all evidence-based, certain factors can influence differences in specific recommendations, such as the consensus group’s composition, underlying mandates, and cultural attitudes. The similarities and differences among 6 sets of guidelines from Europe and the Americas published in the past decade are reviewed here (American Psychiatric Association, British Association for Psychopharmacology, Canadian Network for Mood and Anxiety Treatments, National Institute for Health and Clinical Excellence, Texas Medication Algorithm Project, and World Federation of Societies of Biological Psychiatry). In the guidelines, mild depression has the most variance in treatment recommendations; some, but not all, guidelines suggest that it may resolve with exercise or watchful waiting, but psychotherapy or antidepressants could be used if initial efforts fail. Moderate and severe major depression carry broadly similar recommendations among the guidelines. First-line treatment recommendations for moderate major depressive disorder include antidepressant monotherapy, psychotherapy, and the combination of both. Severe depression may require the combination of an antidepressant and an antipsychotic, electroconvulsive therapy, or the combination of an antidepressant and psychotherapy. Benzodiazepines play a very limited role in the treatment of depression; if the patient has catatonic depression, acutely suicidal depression, or depression with symptoms of anxiety, agitation, or insomnia, benzodiazepines are recommended by some guidelines for short-term treatment only.
(J Clin Psychiatry 2010;71[suppl E1]:e04)
From the Department of Psychiatry and Behavioral Sciences, Duke University School of Medicine, Durham, North Carolina.
This article is derived from the roundtable discussion “International Consensus Group on Depression,” which was held on September 1, 2009, in Tokyo, Japan, and supported by an educational grant from GlaxoSmithKline.
Dr Davidson is an advisor for AstraZeneca, Transcept, and ZARS; has received honoraria as a speaker from DCH Regional Medical Center (Alabama), GlaxoSmithKline, the American Psychiatric Association (APA), AstraZeneca, the Japanese Society of Anxiety Disorders Research, the Tokyo Academy of Cognitive Therapy, Sharp HealthCare, USC School of Medicine, and the University of New Mexico; and has received royalties/license fees from MultiHealth Systems, Inc, Guilford Publications, APA, the Connor-Davidson Resilience Scale, and the Social Phobia Inventory.
Corresponding author: Jonathan R. T. Davidson, MD, 3068 Baywood Dr, Seabrook Island, SC 29455 ([email protected]).
doi:10.4088/JCP.9058se1c.04gry
© Copyright 2010 Physicians Postgraduate Press, Inc.
The various major Western guidelines for the treatment of depression largely agree on the main principles of treatment. While the guidelines are all evidence-based, factors that can influence specific recommendations include the composition of the consensus group, any underlying mandate, and cultural attitudes. The similarities and differences among 6 sets of guidelines from Europe and the Americas are reviewed.
For Clinical Use
- Major American and European guidelines agree on basic principles for the treatment of depression and generally make similar recommendations for achieving remission
- The main first-line approaches, especially for moderate and severe depression, are antidepressants and/or evidence-based psychotherapy; benzodiazepines have a very limited role in managing depressed patients
- Treatment strategies should ultimately be determined on an individual basis
Major American and European Guidelines
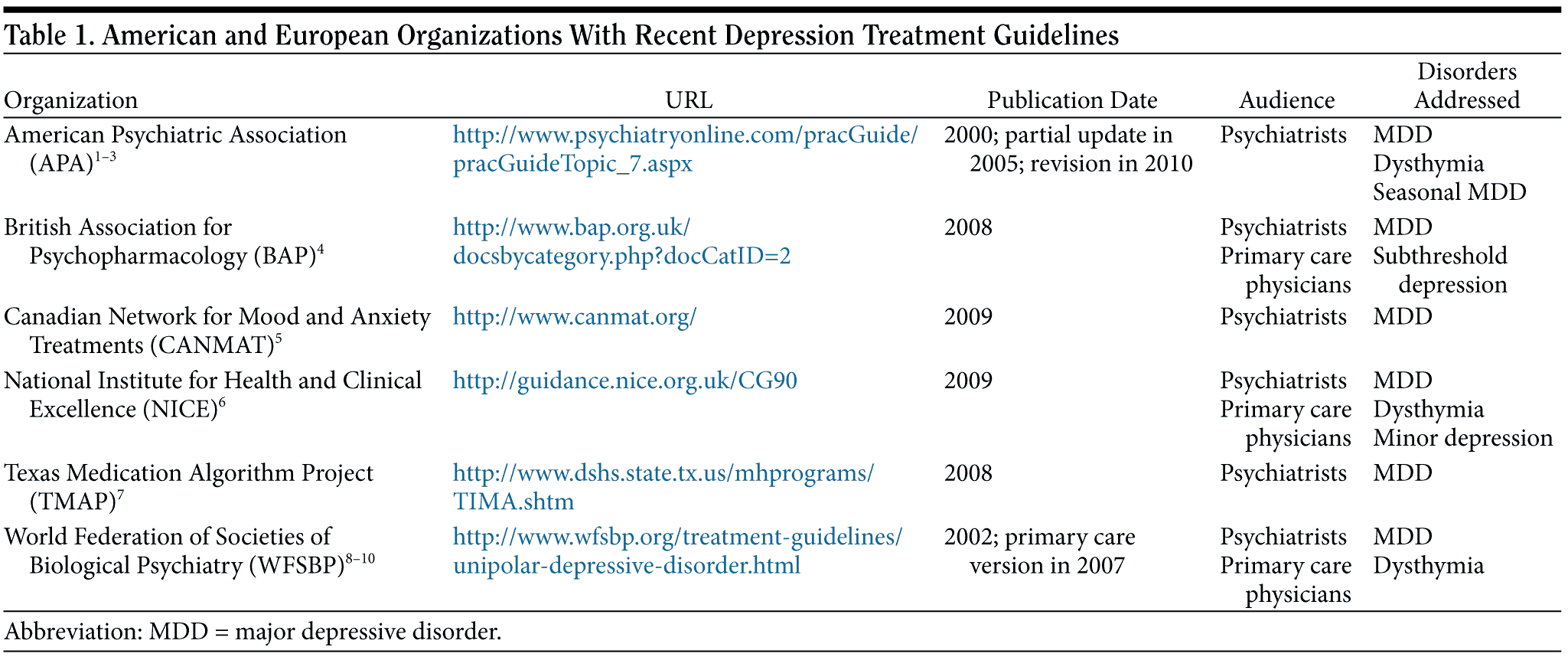
Depression treatment guidelines have been published in the past decade by the American Psychiatric Association (APA),1-3 British Association for Psychopharmacology (BAP),4 Canadian Network for Mood and Anxiety Treatments (CANMAT),5 National Institute for Health and Clinical Excellence (NICE),6 Texas Medication Algorithm Project (TMAP),7 and World Federation of Societies of Biological Psychiatry (WFSBP).8-10 The complete guidelines and any modifications can be accessed at each organization’s website (Table 1). All of the guidelines address a psychiatric audience, but the NICE, BAP, and WFSBP guidelines speak to physicians in primary care settings as well. The CANMAT and TMAP guidelines address only major depressive disorder (MDD), while the APA, BAP, NICE, and WFSBP guidelines also cover subthreshold or minor depression and dysthymia.
These guidelines are all based on levels of published evidence, which give greatest weight to placebo-controlled double-blind trials, but certain factors besides evidence can influence guideline recommendations. One factor is the composition of the committee that develops the guideline, including the mix of professional specialty, such as health economists, consumer representatives, and others. Another factor is whether the group has an underlying mandate such as to ration access to treatment or choice of treatment, whether it was commissioned by a governmental authority, eg, NICE, or a professional organization, eg, BAP. Sometimes cultural attitudes also differ, such as where to set the threshold for recommending medication; experts in some geographic areas or cultures, for example, may be more inclined to prescribe medication for depression than for anxiety because the latter is perceived as less severe. The choice of medication may be influenced by stigma within a culture, eg, where benzodiazepines are (inappropriately) recommended for depression because they are seen as less stigmatizing drugs than antidepressants. However, despite variations in some specific recommendations, the American and European guidelines provide similar messages on the basic principles of treatment for depression.
Basic Principles of Depression Treatment
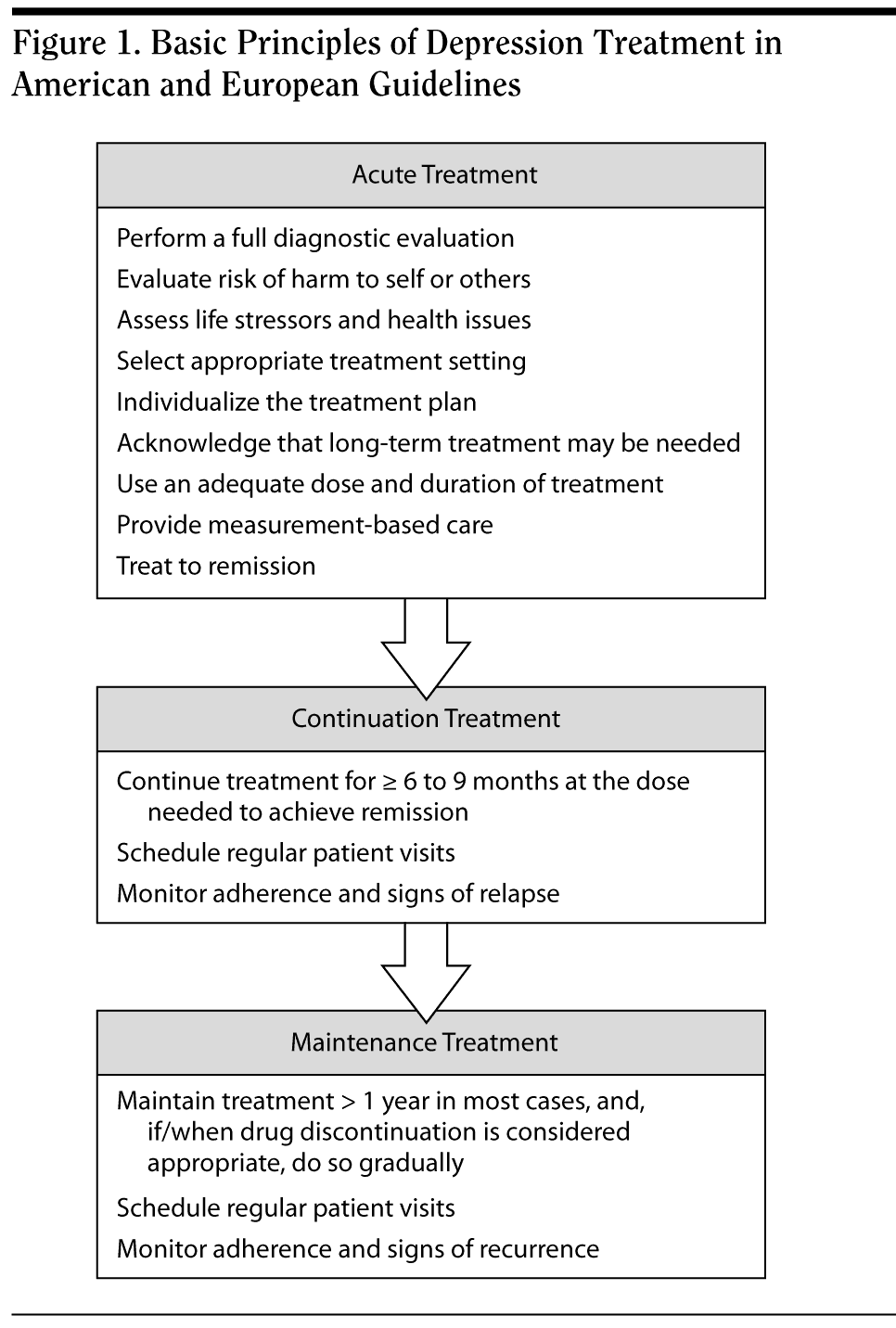
Guidelines address much more than just specific questions about which form of pharmacotherapy or psychotherapy should be used or what dose should be used. The recommendations exist within the context of basic depression treatment principles (Figure 1). These principles include giving the patient a full diagnostic evaluation, explaining the fact that depression may be better regarded as a chronic or a relapsing recurrent illness, and individualizing the treatment plan to the patient’s needs. Each drug trial should have an adequate dose and duration, ie, 8 to 12 weeks with at least 4 weeks at an adequate dose. Treatment should continue until the patient not only responds but reaches remission. All of the guidelines agree on the need for continuation of the antidepressant for at least 6 to 9 months at the dose needed to reach recovery. Although the American and European guidelines on depression management provide similar general treatment recommendations, some variations exist in the criteria for the severity of depression and in certain treatment strategies.
Criteria for Severity of Depression
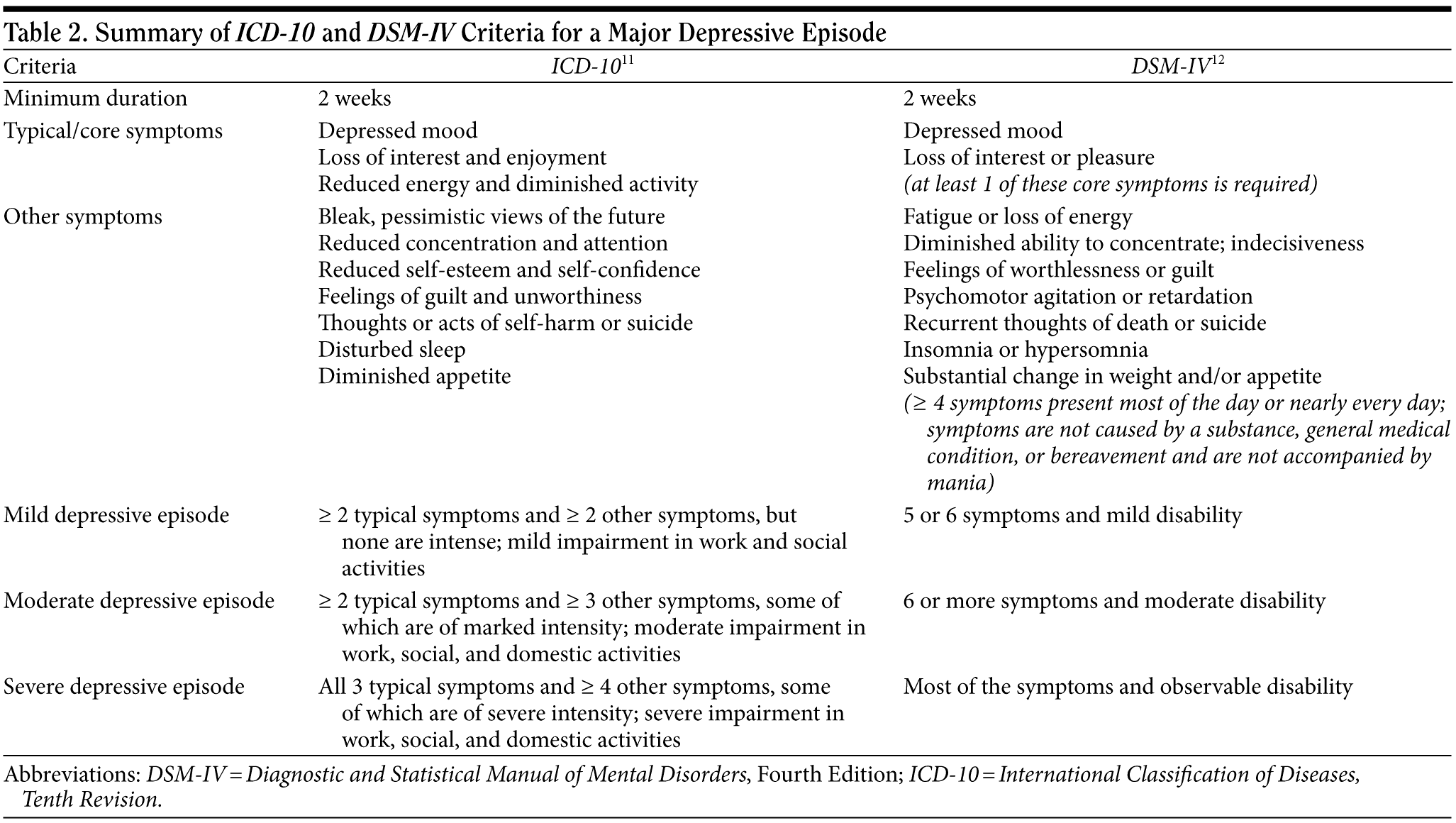
The major Western guidelines categorize treatment decisions based on the severity of the patient’s depression. To define depression severity, they use the criteria from the International Classification of Diseases, Tenth Revision (ICD-10)11 or the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV)12 (Table 2). According to the ICD-10, severity is based on the number of depressive symptoms that are present. Three or fewer symptoms does not constitute MDD, 4 symptoms equates to mild depression, 5 to 6 symptoms equates to moderate depression, and 7 to 10 symptoms denotes severe depression. The fourth category also includes a subtype of severe depression with psychotic symptoms.
In the APA, NICE, and CANMAT guidelines, the measurement of severity is based on the definition of MDD in the DSM-IV. According to DSM-IV criteria, subthreshold depression is defined as having fewer than 5 symptoms (equivalent to the ICD-10 definition of mild depression). In threshold cases of MDD, mild depression meets the minimum criteria, moderate depression means that the patient has more than the minimum number of symptoms plus moderate impairment, and severe depression comprises most of the depressive symptoms plus marked impairment.
The BAP and WFSBP guidelines refer to both the ICD-10 and DSM-IV criteria for depression. The TMAP recommendations for treating MDD do not distinguish between levels of severity, but measuring severity is encouraged, and patients with greater severity would enter the algorithm at later stages. For patients with psychotic symptoms, TMAP provides a separate algorithm.
First-Line Treatment Recommendations
The guidelines basically agree on first-line treatments for moderate and severe major depression, but greater variance exists in first-line treatment recommendations for mild major depression. Not all of the guidelines address subthreshold depression or dysthymia, but those that do have similar recommendations.
Subthreshold Depression and Dysthymia
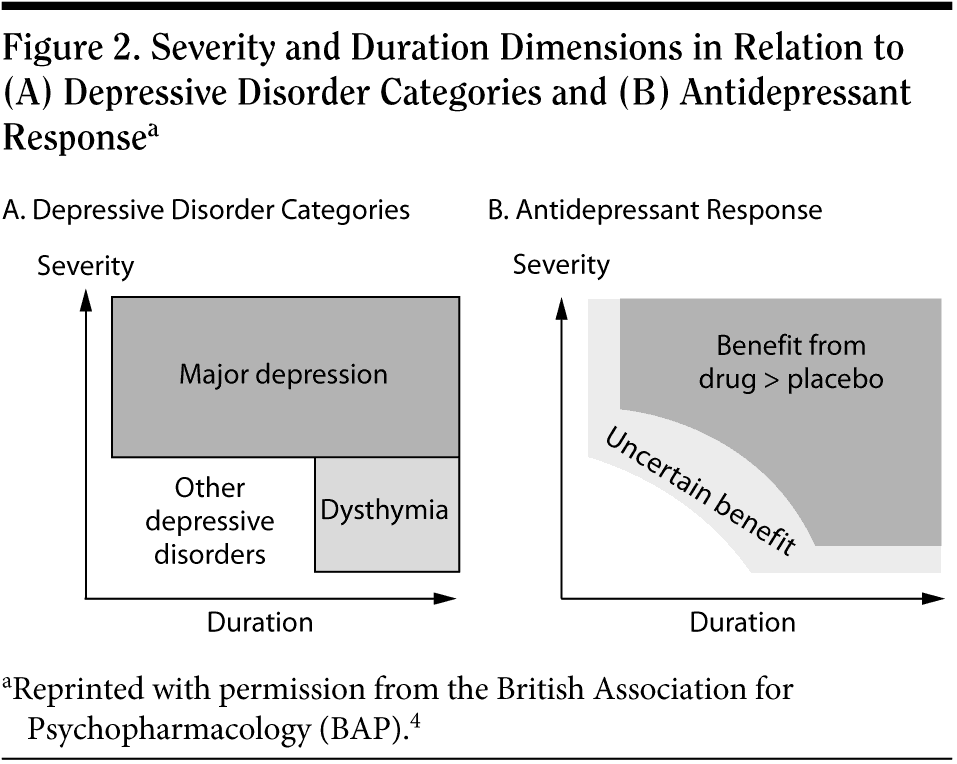
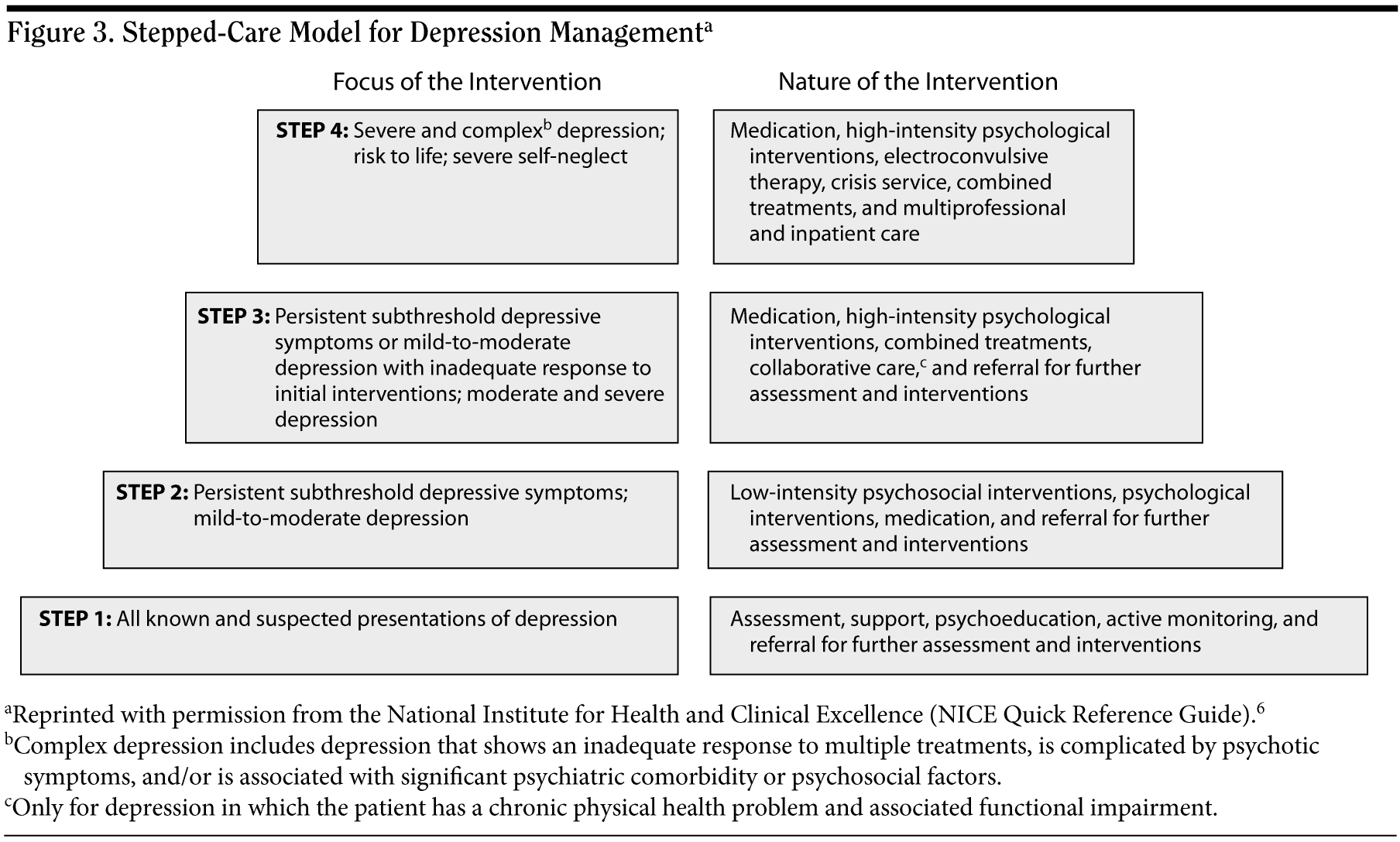
The benefit of medication in subthreshold depression is uncertain. It is believed that, the greater the severity and duration of symptoms, the more clear the benefit of antidepressants, as illustrated in the BAP guidelines (Figure 2). For subthreshold depression that has lasted at least 2 years, the BAP guidelines recommend antidepressants. If the duration of subthreshold depression is less than 2 years, antidepressants are not recommended as first-line treatment but can be considered if (1) the duration is at least 2 to 3 months and/or (2) the patient has a history of recurrent moderate to severe major depression. Otherwise, minimum treatment should involve regular follow-up and symptom monitoring. The NICE guidelines offer similar recommendations and provide a stepped-care model of depression treatment based on the level of severity (Figure 3).
For dysthymia, the APA guidance notes that antidepressants, but not psychotherapy, have been found to have efficacy, but the combination had the greatest efficacy. The WFSBP guidelines recommend that antidepressant treatment for dysthymia should be continued at least 2 to 3 years.
Mild Depression
Slightly more divergence of opinion exists for the preferred management of mild depression than for moderate and severe forms, perhaps because fewer data exist for mild depression. Many aspects of mild depression are not as well understood as are the more severe forms of the illness.
For mild depression, the WFSBP guidelines advise watchful waiting, psychoeducation, psychosocial interventions, psychotherapy, or an antidepressant, depending on the details of the case. The APA guidelines advise psychotherapy or antidepressant monotherapy, depending on patient preference, but combination treatment if the patient has a history of partial response to a single mode of treatment. The CANMAT guidelines state that cognitive therapy, cognitive-behavioral therapy (CBT), and interpersonal therapy (IPT) have efficacy equivalent to that of antidepressants for first-line treatment of mild or moderate depression.
The NICE guidelines advise physicians to first try to manage depression from subthreshold to moderate severity via guided self-help based on CBT, computerized CBT, and group exercise, with the patient being allowed to select the most preferred mode of treatment, as well as sleep hygiene education. In the stepped-care model (see Figure 3), antidepressants are not recommended for mild depression until simpler treatments have failed because of the poor risk-benefit ratio. If low-intensity treatments have been ineffective, an antidepressant or CBT can be used. Antidepressants can be tried initially for a mild depressive episode if the patient has a history of more severe episodes.
The BAP guidelines for mild depression recommend CBT, behavior therapy with activity scheduling, IPT, or antidepressant drugs if the patient has a history of chronic mild depression or previous moderate-to-severe depression; they recommend not using St John’s wort as first-line therapy but considering it for patients who cannot tolerate antidepressants and for whom other first-line treatments are not feasible. All of the guidelines that discuss St John’s wort agree that the available formulations vary in potency and that data on long-term use of the treatment are needed.
Moderate Depression
For first-line treatment of moderate depression, the APA guidelines recommend antidepressants alone; psychotherapy may be considered depending on patient needs or preference. Antidepressants and psychotherapy may be used together for patients with significant psychosocial problems or Axis II disorders.
The first treatment stage of the TMAP MDD algorithm gives the options of a selective serotonin reuptake inhibitor (SSRI), a serotonin-norepinephrine reuptake inhibitor (SNRI), bupropion, mirtazapine, or evidence-based psychotherapy. At this stage, nefazodone, tricyclic antidepressants (TCAs), and monoamine oxidase inhibitors (MAOIs) are not recommended due to safety concerns.
The NICE guidelines recommend that patients with mild or moderate depression who have not responded fully to low-intensity treatment should receive an antidepressant or individual CBT or IPT (see Figure 3). Moderate depression may require a combination of both an antidepressant and either CBT or IPT. The NICE guidelines are favorably inclined toward SSRIs, especially the generic ones that provide better cost-effectiveness. They caution that drug interactions are more likely with fluoxetine, fluvoxamine, and paroxetine than other SSRIs and that paroxetine is associated with more difficult withdrawal than other SSRIs.
The WFSBP guidelines recommend antidepressants and/or psychotherapy along with psychosocial interventions, and the BAP guidelines recommend antidepressants, CBT, IPT, or behavior therapy with activity scheduling as first-line treatments for moderate depression. The CANMAT guidelines are similar to the others, advising the use of SSRIs, the SNRI venlafaxine, cognitive therapy, or IPT.
All of these guidelines agree that an antidepressant drug is a legitimate first-line choice for the treatment of moderate depression, and all except the NICE guidelines recommend evidence-based psychotherapy as another first-line treatment option. The NICE group recognizes that antidepressants are more cost-effective as a first-line treatment for acute, moderate depression.
Severe Depression
For severe depression, all of the guidelines agree that first-line treatment options include electroconvulsive therapy (ECT), the combination of an antidepressant and psychotherapy, or the combination of an antidepressant agent with an antipsychotic agent if the depression has psychotic features. In general, a course of ECT would be between 6 and 10 treatments, and the maximum would be 20 sessions. Guidelines other than WFSBP do not specify what kind of ECT should be used, but the WFSBP recommendation is for bilateral ECT. The WFSBP notes that unilateral ECT may have less potential for temporary memory loss than bilateral ECT, but, to equal the efficacy of bilateral ECT, unilateral placement of the electrodes requires a dose of electricity 6 times the seizure threshold. However, the effects of ECT are not long-lasting.
The WFSBP guidelines also promote the first-line use of TCAs and SNRIs for severe depression. The CANMAT guidelines state that psychotherapy alone may have less efficacy than does medication for severe depression; they recommend the combination of IPT with an antidepressant. The NICE guidelines recommend the combination of individual CBT with an antidepressant for first-line treatment of severe depression.
Response Measurement and Intervention
The guidelines recommend the use of measurement-based care to track treatment outcomes and determine when to intervene; for more information on measurement-based care, please see the article “How to Monitor Response in Major Depressive Disorder” in this supplement by Alan J. Gelenberg, MD.13 Some guidelines refer to specific measures to define response and remission. For example, the TMAP guidelines track treatment progress by using patient scores on the 16-item Quick Inventory of Depressive Symptomatology (QIDS-16).14 Remission corresponds to a score of 0 to 5, partial response to a score of 6 to 8, and nonresponse to 9 or more; the maximum score on the QIDS-16 is 27. The algorithm authors encourage clinicians to use the QIDS or other scales to measure symptom severity and assess side effects and global functioning at each visit. The TMAP guidelines describe critical decision points at which treatment interventions should be considered.
The APA, BAP, and NICE guidelines are vague about how to define response, although the BAP guidelines do advise using simple, standardized rating scales for assessing response. The NICE guidelines state that a routine outcome monitoring process should be used to ensure that patients who have not received benefit from initial treatments are promptly moved up to the next step of treatment in the stepped-care model.
The WFSBP and CANMAT guidelines define response using the percentage of change in symptoms from baseline per standardized rating scales. In the WFSBP guidelines, a ≤ 25% symptomatic improvement from baseline represents nonresponse, a 26% to 49% improvement from baseline indicates partial response, and a ≥ 50% decrease in symptoms denotes response. The CANMAT definitions propose closely similar criteria; nonresponse corresponds to a < 20% decrease in symptom score, minimal response to 20% to 50% improvement, partial response to a > 50% reduction, and full response to a normal symptom score.
Remission, according to the WFSBP guidelines, should mean, at a minimum, that the patient is asymptomatic and has experienced improved occupational and psychosocial functioning. The CANMAT guidelines concur that remission is recognized as an asymptomatic state, rather than simply improvement to the point of no longer meeting full threshold criteria for MDD.
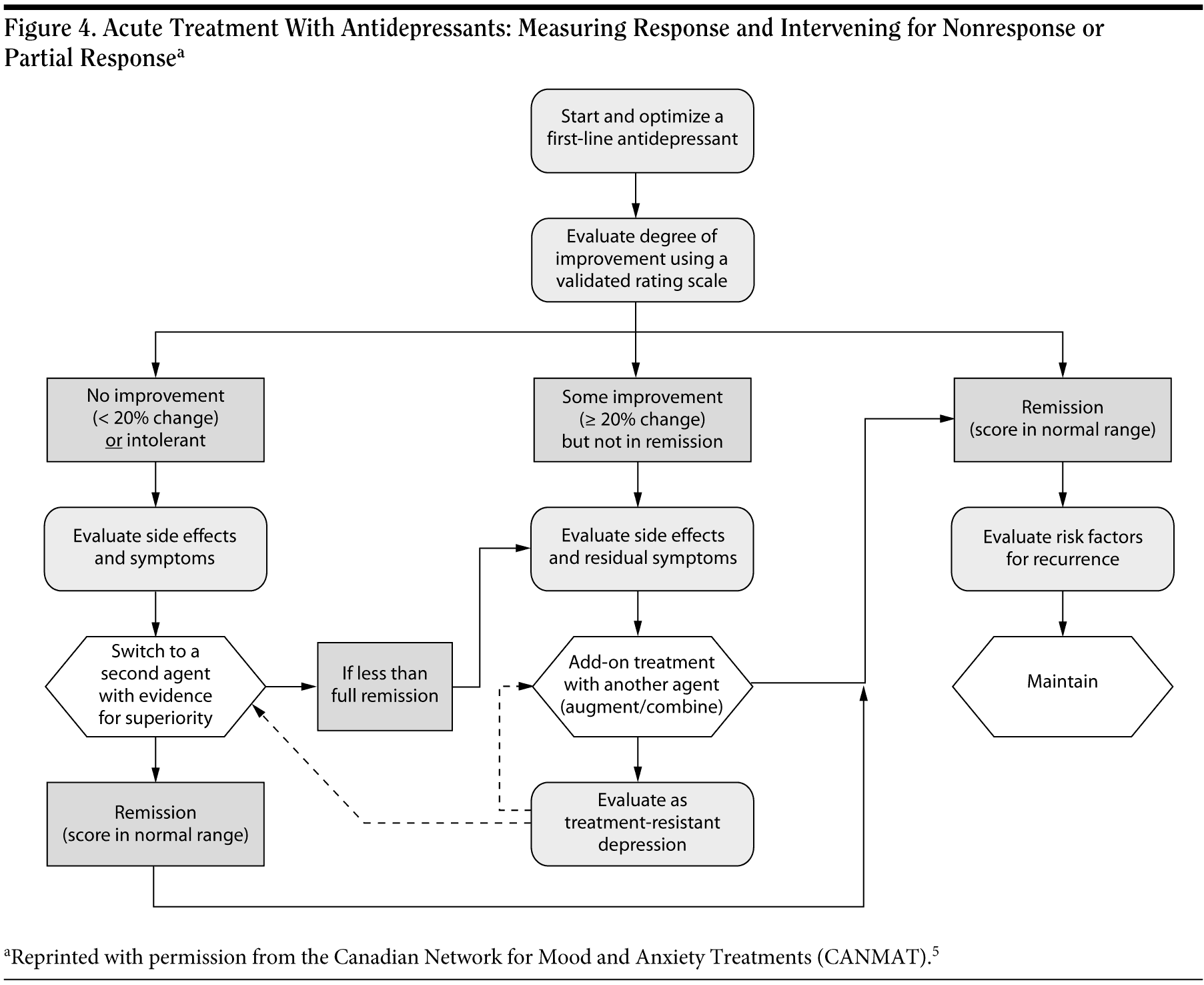
All of the guidelines agree that second-line options, after first trying a dose increase, include switching, combining, or augmenting the initial treatment (Figure 4). If the first-line treatment has not worked (ie, the result was nonresponse), most guidelines suggest switching to another antidepressant. If the first-line treatment has led to partial response, the first type of treatment can be augmented with another one.
The TMAP instructions for managing partial response specify augmenting the first-line drug with a drug that has a different mechanism of action. For example, if the patient is taking an SSRI, then the physician could add bupropion or mirtazapine. If the patient is taking bupropion, then the physician could add an SSRI or an SNRI. For nonresponders or patients who show poor tolerance of the first-line drug choice, then the physician could switch to an antidepressant drug of a different class. If the patient began with an SSRI, then he or she could switch to mirtazapine or bupropion, for example, or perhaps an SNRI.
Maintenance treatment is normally required after the acute and continuation phases to reduce the chance of a recurrence (see Figure 1). The TMAP manual states that about half of all patients with a history of 1 previous episode will have a recurrence, and about 90% of those who have had 3 episodes will have a recurrence without long-term antidepressant treatment.
Limited Role of Benzodiazepines
The guidelines acknowledge only a limited value of benzodiazepines as short-term adjunctive therapy and only in certain cases. For example, in catatonic depression, which is rare, the use of intravenous benzodiazepines or barbiturates may be helpful along with a concurrent antidepressant, according to the APA.
The APA, BAP, NICE, and TMAP guidelines also allow that benzodiazepines can be used for a short time with an antidepressant if the patient has symptoms of anxiety or insomnia; however, the APA notes that withdrawal from the medication may be difficult for some patients, and no data support sustained benefit. Even if patients have MDD and anxiety symptoms, the APA does not recommend benzodiazepines as the primary or continuing treatment. The CANMAT guidelines state that lorazepam and other benzodiazepines are not recommended as monotherapy for anxious depression because of possible dependency, but they could be used for short-term adjunctive therapy.
The WFSBP guidelines acknowledge the quick onset of action of benzodiazepines in treating agitation, anxiety, and insomnia and suggest that, under some circumstances, benzodiazepines may also be used in suicidal depression. However, a risk-benefit analysis must be carefully conducted. Benzodiazepines are not recommended for patients with substance use disorders and are not recommended for a period of use longer than 4 weeks. The NICE guidelines state that benzodiazepines do not have a specific antidepressant effect.
Special Considerations
Special Populations
All of the guidelines discuss special populations—eg, pediatric or geriatric populations and pregnant patients—to a greater or lesser extent. For example, the CANMAT guidelines note that pharmacodynamic and pharmacokinetic properties of drugs are affected by a very young age or a very old age, influencing not only side effects but also response. Doses should be adjusted appropriately in these populations. The BAP guidelines point out an increased risk of self-harm with antidepressant treatment in young patients. The WFSBP guidance states that children and adolescents appear to be more likely than adults to respond to placebo. The NICE guidance recommends more research on dosing of antidepressants in geriatric patients due to altered absorption and metabolism of drugs in later life. The CANMAT guidelines recognize that women have a higher lifetime risk for MDD than men and may present with more atypical symptoms, anxious symptoms, or somatic symptoms. Women also require special treatment considerations if they are or plan to become pregnant or are breast-feeding. The APA notes that cultural factors may cause depression to be expressed or described differently by different patients.
Comorbidities
The guidelines all address different types of comorbidity, ie, medical illness, Axis II disorders, and other Axis I disorders. According to the BAP guidelines, comorbid medical illness (especially common in older patients) may signal not only a less satisfactory response to antidepressants but also a higher risk of relapse of MDD. Depressive disorders often complicate neurologic, cardiovascular, and endocrine disorders as well as cancer, according to the CANMAT manual. When medical illness is comorbid with MDD, the choice of an antidepressant is likely to be influenced by the potential for drug-drug interactions with the patient’s current treatment(s) for the medical illness.
The APA and NICE guidelines note that patients with personality disorders are particularly vulnerable to episodes of MDD. Substance use disorders are also often comorbid with MDD, so the APA recommends that clinicians thoroughly query patients about substance use. If suspicion of substance abuse is aroused, questioning the patient’s family or friends may be necessary for confirmation. Benzodiazepines and MAOIs should be avoided in this population. Both the substance abuse and the MDD must be treated, but the substance abuse may have to be managed first, recommends the WFSBP. In patients with MDD and a comorbid anxiety disorder, both MDD and anxiety symptoms have been shown to be remedied with antidepressant treatment, according to the APA guidelines. The CANMAT guidelines state that eating disorders, schizophrenia, attention-deficit/hyperactivity disorder, and dementias are also often comorbid with depressive episodes or MDD.
Subtypes
Subtypes of depression are also covered by the guidelines, including psychotic, melancholic, atypical, chronic, and seasonal MDD. There are a number of separate guidelines for managing bipolar disorder (Table 3), including bipolar depression.
As noted above, the TMAP manual provides a separate algorithm for psychotic depression. The CANMAT guidelines point out that, although melancholic depression is usually severe, not all severe depression is melancholic in type. Atypical depression features include increased sleep and weight, a feeling of great fatigue, sensitivity to emotional rejection, phobic symptoms, and marked mood reactivity; according to the APA, MAOIs are especially effective treatment for atypical depression. The NICE guidelines state that atypical features are commonly associated with seasonal MDD or seasonal affective disorder. Chronic depression may preferentially respond to the combination of pharmacotherapy and psychotherapy, according to the CANMAT guidance, and ECT can be considered.
Conclusion
Evidence-based treatment guidelines are necessary to aid clinicians in treating depression to remission, and the American and European guidelines reviewed here generally make similar recommendations. The main first-line approaches, especially for moderate and severe depression, are antidepressants, such as SSRIs, and/or evidence-based psychotherapy. Benzodiazepines have a very limited role in managing depressed patients. Ultimately, treatment is determined on an individual basis, since the choice of drug or therapy requires not simply matching the patients’ symptoms to a point in the guidelines but considering a larger context that includes the patient’s psychosocial issues, comorbidities, and history.
DISCUSSION
Professor Nutt: Knowing that the depression treatment guidelines have a general consensus on many topics is reassuring. Of course, guidelines that promote exercise, for example, may have members of the panel who are runners; recommendations may understandably reflect the individual experiences of the group in addition to relying on evidence.
Dr Sakamoto: Most of the guidelines were divided according to severity of depression. I am unsure whether the severity of depression can be decided only according to number of depressive symptoms. For example, a patient may have only 2 or 3 depressive symptoms, but those symptoms are very severe.
Dr Davidson: The guidelines6 do distinguish between counting the symptoms and judging the severity or the significance of the symptoms. So, if you have a patient with only 3 symptoms, but those symptoms are very disturbing and troublesome, you would need to treat the patient as having a more severe problem. You could not just manage that problem with strategies such as active monitoring or telling him or her to run 3 times a week.
Besides the symptom count, clinicians must consider not only how bothersome the symptoms are but also the patient’s history. If a patient experienced terrible depression 5 years previously and recently has lost her job or made a suicide attempt, then her 3 symptoms of so-called “mild” depression take on more serious clinical significance. The symptom count is just a platform from which to begin. Of 10 people who have mild depression, the episode will subside for probably 8 or 9 of them if you do nothing or prescribe mild exercise, guided imagery, or guided self-help, but a couple of patients would likely need more treatment than that.
Dr Kanba: Do you think that antidepressants should not be used for mild depression?
Dr Davidson: For mild depression, the evidence base is not as strong as it is for more severe depression. One of the problems with using antidepressants for really mild depression is that the side effects tend to impede the modest gains that the patient would realize, and then you have a risk-benefit issue. As the depression becomes more severe, the willingness of patients to tolerate side effects is greater, and the use of medication may be more justified because the gain is so much greater. But, what the guidelines say about managing mild depression with strategies like exercise does not seem like bad advice.
Dr Gelenberg: Most of the focus in treating mild depression has been on avoidance of adverse effects, which is why treatments that do not seem to have any adverse potential, like appropriate exercise or omega-3 fatty acids, seem to be relatively favored.
Dr Higuchi: When patients take medication according to the guidelines and they do not experience any effect, then what do you do?
Dr Davidson: You want to be sure that you made the diagnosis correctly. Have you missed something? The patient could be drinking, for example, and a substance use disorder can interfere with treatment.
Professor Nutt: I see doctors who go through the guideline options and then give up if the patient is still symptomatic. If you give up, then the patient gives up.
Dr Gelenberg: With the number of permutations of guideline options, getting the patient to remission could require a lot of time.
Dr Zhang: Sometimes if you stop treatment, the patient gets better.
Dr Davidson: Sometimes, for a while. It is critical to maintain the patient’s hope and your own belief that together you can get to remission, although it may take a long time. Never stop trying. Try various combinations of treatment. You may have to be truly creative and come up with something that does not appear in the guidelines.
Dr Terao: Which areas of the guidelines should general practitioners perform?
Dr Davidson: It seems to me that most general practitioners would want to be familiar with first-line and second-line treatments to be competent. Beyond that, they need to know what the other stages are and when to refer patients or work collaboratively with specialists. Some general practitioners may have a special interest in mental health and may be willing to follow the guidelines a bit farther.
Drug names: bupropion (Aplenzin, Wellbutrin, and others), fluoxetine (Prozac and others), fluvoxamine (Luvox and others), lorazepam (Ativan and others), mirtazapine (Remeron and others), paroxetine (Paxil and others), venlafaxine (Effexor and others).
Disclosure of off-label usage: The author has determined that, to the best of his knowledge, fluvoxamine and lorazepam are not approved by the US Food and Drug Administration for the treatment of depression.
References
1. American Psychiatric Association. Practice Guideline for the Treatment of Patients With Major Depressive Disorder, 2nd ed. Am J Psychiatry. 2000;157(suppl 4):1-45. PubMed
2. American Psychiatric Association. Guideline watch: practice guideline for the treatment of patients with major depressive disorder, 2nd ed. http://www.psychiatryonline.com/pracGuide/pracGuideTopic_7.aspx. 2005. Accessed September 15, 2009.
3. Gelenberg AJ. The search for knowledge: developing the American Psychiatric Association’s practice guideline for major depressive disorder. J Clin Psychiatry. 2008;69(10):1658-1659. doi:10.4088/JCP.v69n1016 PubMed
4. Anderson IM, Ferrier IN, Baldwin RC, et al. Evidence-based guidelines for treating depressive disorders with antidepressants: a revision of the 2000 British Association for Psychopharmacology guidelines. J Psychopharmacol. 2008;22(4):343-396. doi:10.1177/0269881107088441 PubMed
5. Kennedy SH, Lam RW, Parikh SV, et al, for the Canadian Network for Mood and Anxiety Treatments. Canadian Network for Mood and Anxiety Treatments (CANMAT) clinical guidelines for the management of major depressive disorder in adults. J Affect Disord. 2009;117(suppl 1):S1-S2. doi:10.1016/j.jad.2009.06.043 PubMed
6. National Institute for Health and Clinical Excellence. Depression: the Treatment and Management of Depression in Adults. www.nice.org.uk/CG90. Published October 28, 2009. Accessed November 9, 2009.
7. Suehs BT, Argo TR, Bendele SD, et al. Texas Medication Algorithm Project Procedural Manual: Major Depressive Disorder Algorithms. Austin, TX: Texas Department of State Health Services; 2008.
8. Bauer M, Whybrow PC, Angst J, et al, for the World Federation of Societies of Biological Psychiatry Task Force on Treatment Guidelines for Unipolar Depressive Disorders. World Federation of Societies of Biological Psychiatry (WFSBP) Guidelines for Biological Treatment of Unipolar Depressive Disorders, part 1: acute and continuation treatment of major depressive disorder. World J Biol Psychiatry. 2002;3(1):5-43. doi:10.3109/15622970209150599 PubMed
9. Bauer M, Whybrow PC, Angst J, et al, for the World Federation of Societies of Biological Psychiatry (WFSBF) Task Force on Treatment Guidelines for Unipolar Depressive Disorders. World Federation of Societies of Biological Psychiatry (WFSBP) Guidelines for Biological Treatment of Unipolar Depressive Disorders, Part 2: maintenance treatment of major depressive disorder and treatment of chronic depressive disorders and subthreshold depressions. World J Biol Psychiatry. 2002;3(2):69-86. doi:10.3109/15622970209150605 PubMed
10. Bauer M, Bschor T, Pfennig A, et al, for the World Federation of Societies of Biological Psychiatry (WFSBP) Task Force on Unipolar Depressive Disorders. World Federation of Societies of Biological Psychiatry (WFSBP) Guidelines for Biological Treatment of Unipolar Depressive Disorders in Primary Care. World J Biol Psychiatry. 2007;8(2):67-104. doi:10.1080/15622970701227829 PubMed
11. World Health Organization. International Classification of Diseases, Tenth Revision. Geneva, Switzerland: World Health Organization; 1992.
12. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition. Washington, DC: American Psychiatric Association; 1994.
13. Gelenberg AJ. How to monitor response in major depressive disorder. J Clin Psychiatry. 2010;71(suppl E1):e01.
14. Rush AJ, Trivedi MH, Ibrahim HM, et al. The 16-Item Quick Inventory of Depressive Symptomatology (QIDS), clinician rating (QIDS-C), and self-report (QIDS-SR): a psychometric evaluation in patients with chronic major depression. Biol Psychiatry. 2003;54(5):573-583. doi:10.1016/S0006-3223(02)01866-8 PubMed