Objective: To characterize treatment trajectories in children newly diagnosed with attention-deficit/hyperactivity disorder (ADHD).
Methods: We utilized billing records of children aged 3 to 18 years in 28 US states’ Medicaid programs between 1999 and 2006. Children entered the cohort at the first ADHD diagnosis (ICD-9-CM: 314.00) preceded by ≥ 6 months with no psychotropic medication use and no psychiatric diagnoses. We followed children for 5 years to assess use of (1) psychotropic polypharmacy (the use of ≥ 3 psychotropic medication classes), (2) antipsychotics, and (3) anticonvulsants. We used mixed-effects logistic regression to model the probability of each utilization outcome as a function of age at ADHD diagnosis and follow-up year, adjusted for sociodemographic factors.
Results: Our cohort included 16,626 children of whom 79.2% received stimulants, 33.2% antidepressants, and 23.1% α-agonists, and 25.3% received psychotropic polypharmacy treatment at least once in a subsequent year. Antipsychotics (7.1%-14.7%), anticonvulsants (4.0%-7.9%), and psychotropic polypharmacy (8.5%-13.4%) use increased from year 1 to 5, but this increase was confined to children between ages 3 and 9 at ADHD diagnosis. Children diagnosed at age 3 had the most substantial increase in each outcome (OR = 1.80 [95% CI, 1.36-2.38]; 1.85 [1.38-2.47]; 2.14 [1.45-3.16]), respectively. Also, 39.1% of 9,680 children-years with psychotropic polypharmacy therapy had no psychiatric diagnoses other than ADHD.
Conclusions: Psychotropic polypharmacy, antipsychotic, and anticonvulsant use increased with each year of follow-up. This effect was strongly mediated by the age of ADHD diagnosis with substantial increases in preschoolers but no corresponding effect in older children. It was only partially explained by physician diagnoses of concomitant mental disorders.

Differential Risk of Increasing Psychotropic Polypharmacy Use in Children Diagnosed With ADHD as Preschoolers

ABSTRACT
Objective: To characterize treatment trajectories in children newly diagnosed with attention-deficit/hyperactivity disorder (ADHD).
Methods: We utilized billing records of children aged 3 to 18 years in 28 US states’ Medicaid programs between 1999 and 2006. Children entered the cohort at the first ADHD diagnosis (ICD-9-CM: 314.00) preceded by ≥ 6 months with no psychotropic medication use and no psychiatric diagnoses. We followed children for 5 years to assess use of (1) psychotropic polypharmacy (the use of ≥ 3 psychotropic medication classes), (2) antipsychotics, and (3) anticonvulsants. We used mixed-effects logistic regression to model the probability of each utilization outcome as a function of age at ADHD diagnosis and follow-up year, adjusted for sociodemographic factors.
Results: Our cohort included 16,626 children of whom 79.2% received stimulants, 33.2% antidepressants, and 23.1% α-agonists, and 25.3% received psychotropic polypharmacy treatment at least once in a subsequent year. Antipsychotics (7.1%-14.7%), anticonvulsants (4.0%-7.9%), and psychotropic polypharmacy (8.5%-13.4%) use increased from year 1 to 5, but this increase was confined to children between ages 3 and 9 at ADHD diagnosis. Children diagnosed at age 3 had the most substantial increase in each outcome (OR = 1.80 [95% CI, 1.36-2.38]; 1.85 [1.38-2.47]; 2.14 [1.45-3.16]), respectively. Also, 39.1% of 9,680 children-years with psychotropic polypharmacy therapy had no psychiatric diagnoses other than ADHD.
Conclusions: Psychotropic polypharmacy, antipsychotic, and anticonvulsant use increased with each year of follow-up. This effect was strongly mediated by the age of ADHD diagnosis with substantial increases in preschoolers but no corresponding effect in older children. It was only partially explained by physician diagnoses of concomitant mental disorders.
J Clin Psychiatry 2017;78(7):e774-e781
https://doi.org/10.4088/JCP.16m10884
© Copyright 2017 Physicians Postgraduate Press, Inc.
aDepartment of Pharmaceutical Outcomes and Policy, College of Pharmacy, University of Florida, Gainesville
bCenter for Health Services Research on Pharmacotherapy, Chronic Disease Management, and Outcomes, Institute for Health, Health Care Policy and Aging Research, Department of Pharmacy Practice and Administration, Ernest Mario School of Pharmacy, Rutgers, The State University of New Jersey
cDepartment of Psychiatry, The Zucker Hillside Hospital, North Shore-Long Island Jewish Health System, Glen Oaks, New York
dNew York State Psychiatric Institute, Columbia University Medical Center, New York
*Corresponding author: Almut G. Winterstein, PhD, Department of Pharmaceutical Outcomes and Policy, University of Florida, College of Pharmacy, PO Box 100496, Gainesville, FL 32610-0496 ([email protected]).
Many reports in North America and Europe in the past decade describe increases in use of psychotropic medications among children, in particular those involving attention-deficit/hyperactivity disorder (ADHD) medications and atypical antipsychotics1-9
This growth appears not only related to an increased prevalence of mental disorder diagnoses but also because of increasing use of psychotropic polypharmacy.10,11 For example, 1996-2007 National Ambulatory Medical Care Survey data7 of child and adolescent visits to office-based physicians in which a mental disorder was diagnosed showed an increase of multiclass psychotropic treatment from 22% (1996-1999) to 32% (2004-2007), with notable increases of coprescription patterns for ADHD medications and antipsychotic medications. An analysis of Texas Medicaid recipients reported that 25% of recipients receiving ADHD treatment used more than 1 medication, most commonly concomitant antidepressants (15%) or antipsychotics (12%).12
ADHD is a particular focus of psychotropic polypharmacy because of its high prevalence and early age at onset. Yet little is known about the efficacy or safety of concomitant treatment regimens for ADHD.11,13,14 To establish targets for comparative safety and effectiveness research in this area, a greater understanding is needed of common psychotropic regimens and their correlates in community practice.
We aimed to determine the prevalence of psychotropic treatment in a cohort of children newly diagnosed with ADHD who had not been recently treated with psychotropic medications. We followed the children over 5 years to characterize trajectories in treatment patterns over time and to evaluate whether their age at the time of ADHD diagnosis influenced these treatment trajectories.
METHODS
Study Population
We used a study population that had been assembled for the evaluation of central nervous stimulant risk on severe cardiac events and that has been described elsewhere.15 In brief, the cohort was established from the 28 US states with the largest child and adolescent population eligible for Medicaid fee-for-service benefits between 1999 and 2006, representing 24 million children and adolescents. Medicaid billing records summarized in the Medicaid Extract Files (MAX) by the Centers for Medicare and Medicaid Services (CMS) provided inpatient and outpatient claims with mental health diagnoses and pharmacy claims with details on dispensed prescriptions.
In the following analyses, children had to be at least 3 years and not more than 14 years of age at the date of the first observed diagnosis of ADHD (ICD-9-CM: 314.0x) preceded by at least 6 months of continuous Medicaid enrollment (index date). We further required availability of a 5-year follow-up period with subsequent ADHD diagnoses no later than 12 months of each previous diagnosis and without occurrence of a hospitalization of more than 30 days, occurrence of the 19th birthday, death, or pregnancy. In an attempt to focus the analysis on new treatment episodes of ADHD, we further restricted the cohort to no other psychiatric diagnoses (ICD-9-CM: 290-319) or psychotropic medication use during the pre-index 6-month period.
Psychotropic Medication Exposure
Psychotropic medication use was defined from pharmacy claims with a start date at the day of dispensing. On the basis of its National Drug Code (NDC), we classified each psychotropic medication into 1 of 7 classes according to the American Hospital Formulary System (AHFS),16 including (1) stimulants (including atomoxetine), (2) α-agonists, (3) antidepressants, (4) antipsychotics, (5) anticonvulsants, (6) anxiolytics/hypnotics/sedatives, and (7) lithium.

- In the past decade, there has been a significant increase in use of psychotropic monotherapy and polypharmacy among children and early adolescents with ADHD. Yet the relationship between age at onset and subsequent magnitude of psychotropic use has not been characterized.
- Preschoolers with ADHD had increased odds of receiving antipsychotics, anticonvulsants, and polypharmacy regimens during early adolescence when compared with children with later onset of ADHD.
- Preschool onset of ADHD may signal increased clinical complexity, misapplication of formal ADHD diagnostic criteria, or other psychiatric conditions. More research is needed to understand the underlying concomitant mental disorders and develop evidence-based algorithms to align treatments with each patient’s clinical needs.
Study Outcomes
We divided each patient’s follow-up period into five 1-year periods, and then classified each of these years with regard to the use of the 7 defined psychotropic medication classes, determined by presence of at least 1 pharmacy claim from the respective class. We used this classification to define 3 binary outcome variables: (1) psychotropic polypharmacy (the use of at least 3 medication classes at any time during a follow-up year), (2) use of antipsychotic medication at any time during a follow-up year, and (3) use of anticonvulsant medication at any time during a follow-up year.
Concomitant Psychiatric Disorders
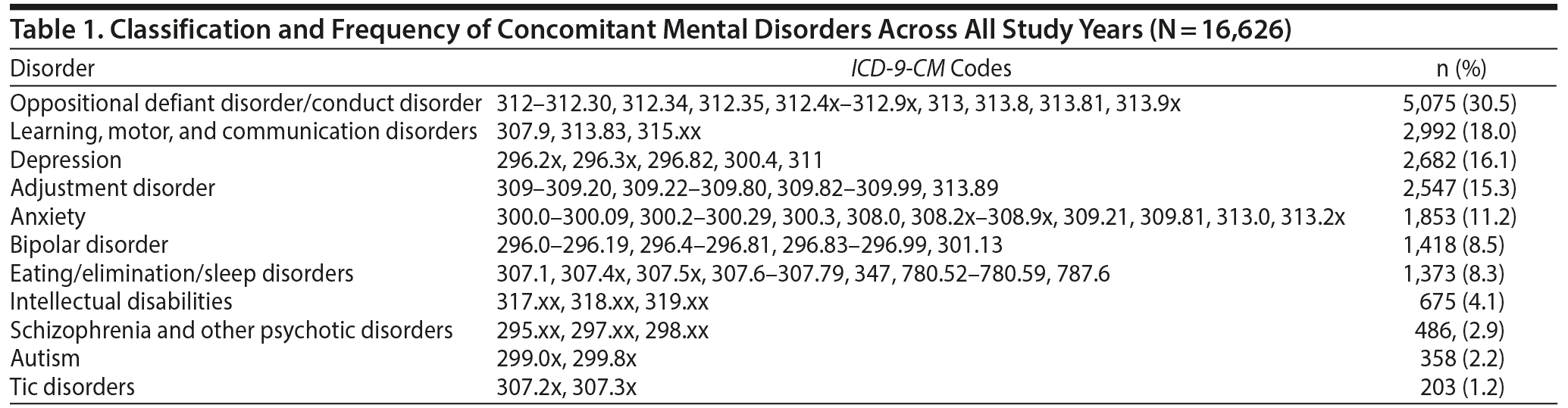
To characterize the association between the number of concomitant psychiatric disorders and the use of psychotropic polypharmacy at any time during a follow-up year, we considered 11 different classes of psychiatric disorders (Table 1). We then estimated the frequency of ADHD-concomitant disorders across all study years.
Data Analysis
We used mixed-effects logistic regression17 to model the probability of each of the 3 binary outcome variables as a function of age at the time of ADHD diagnosis and year postdiagnosis. We added the following covariates to our model to adjust for confounding: sex, race, calendar year of the beginning of a follow-up year, Medicaid eligibility indicators for foster-care status, disability status (Supplemental Security Income—SSI), and poverty status (Temporary Assistance for Needy Families) during each follow-up year. We also included low or high ADHD prevalence (categorized by median across all 50 states and the District of Columbia) in the state of Medicaid eligibility for each follow-up year as reported by the Centers for Disease Control and Prevention (CDC).3 Study states in the lower 2 quartiles of ADHD prevalence were Georgia, Iowa, Idaho, Illinois, Minnesota, Nebraska, New Hampshire, New York, and Texas.
We used restricted cubic splines (RCS)18 to represent the effect of age at ADHD diagnosis, and allowed the RCS age-trend shape to vary independently across follow-up year through the use of interaction terms, ie, each follow-up year was represented with a separate trend curve. We viewed the 5 binary responses from a patient follow-up period as a 5-element response vector with possible correlation among the elements and used a first-order autoregressive (AR1) covariance structure to model patient as a random effect in order to account for this correlation.17 We fit our models using PROC GLIMMIX in SAS Version 9.2 (SAS Institute, Cary, North Carolina) and used the fitted models to estimate odds ratios with 95% confidence intervals and predicted probabilities of medication use by age at ADHD diagnosis and follow-up year. The study was approved by the University of Florida Institutional Review and Privacy Boards and the Centers for Medicare and Medicaid Services Privacy Board.
RESULTS
Our cohort included 16,626 children and youth with a mean age at ADHD diagnosis (study index date) of 8.0 ± 2.53 years (Table 2). Most of the children were white males with 12.8% in foster care and 23.0% receiving Temporary Assistance for Needy Families, indicating poverty.
Psychotropic Medication Utilization Over 5-Year Follow-Up
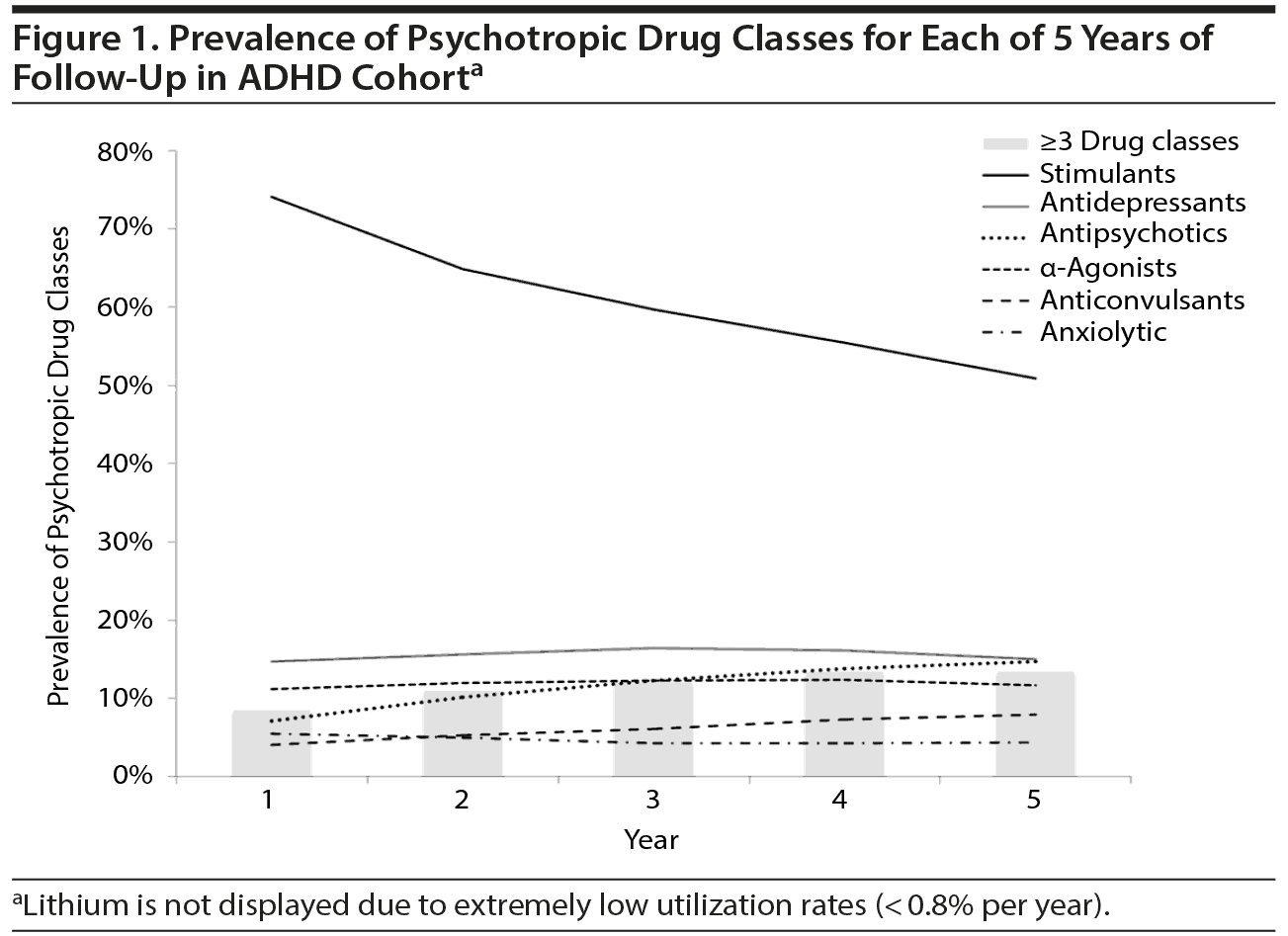
At some point during the 5-year follow-up, most children received stimulants (79.2%), followed by antidepressants (33.2%), α-agonists (23.1%), and antipsychotics (22.8%). One quarter of children (25.3%) had at least 1 follow-up year during which they filled prescriptions for 3 or more different psychotropic medication classes. While the proportion of children with no psychotropic use increased with each year of follow-up from 20.7% to 43.4%, we also noted an increase in the use of 3 or more classes from 8.5% of children in year 1 to 13.4% in the fifth year of follow-up (Figure 1).
Decreases in overall psychotropic medication utilization were mainly driven by decreases in stimulant use, while increases occurred in the use of antipsychotics and anticonvulsants (Figure 1). Specifically, antipsychotic use increased from 7.1% during the first year of ADHD diagnosis to 14.7% at year 5, compared to 4.0% versus 7.9% for anticonvulsants.
Determinants of Antipsychotic, Anticonvulsant, and Psychotropic Polypharmacy Treatment
Male sex, white race, and presence in foster care significantly increased the probabilities of antipsychotic, anticonvulsant, and psychotropic polypharmacy treatment in any study year (eAppendix 1). Interestingly, residence in a high-prevalence ADHD state, matching CDC data, decreased the chance of antipsychotic use (OR = 0.81; 95% CI, 0.75-0.88) but did not affect anticonvulsant use or overall psychotropic polypharmacy treatment.
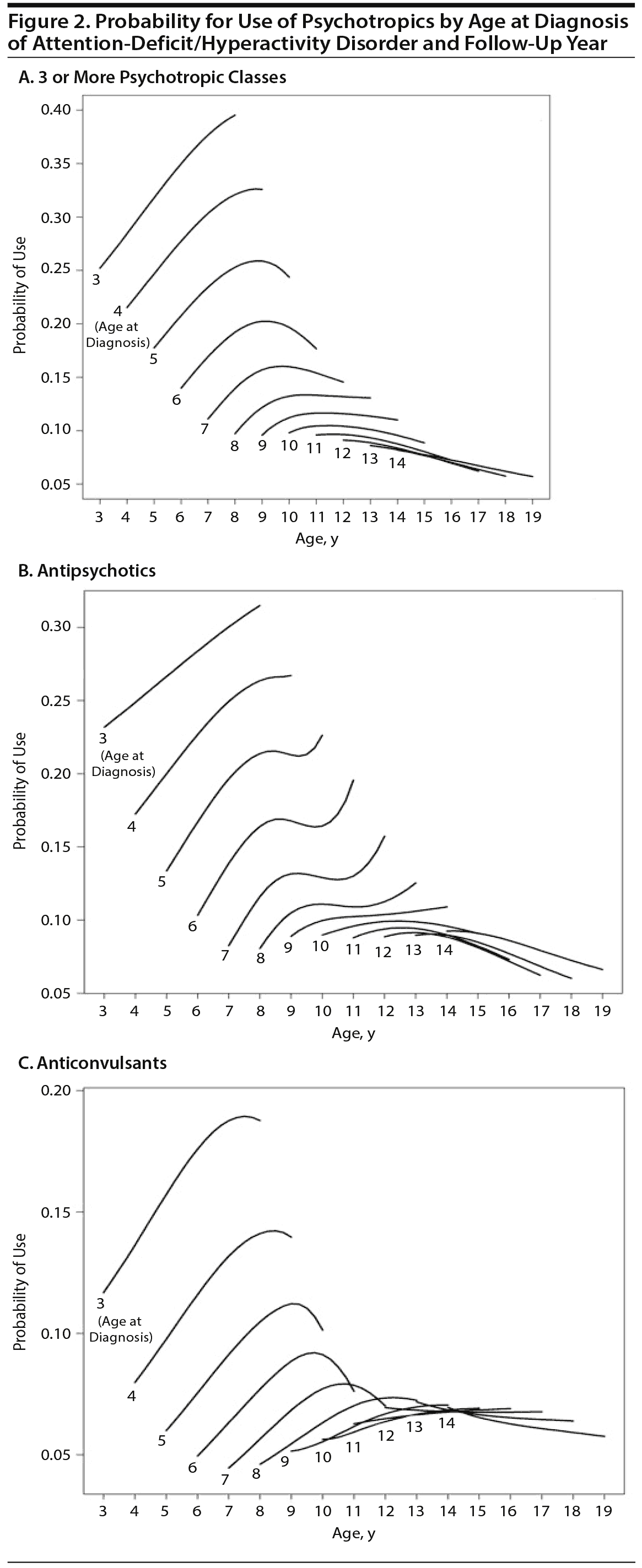
The general trend for increasing probabilities of psychotropic polypharmacy, anticonvulsant, or antipsychotic use over the course of follow-up did not hold if interactions between diagnosis age and follow-up year were examined. For children diagnosed between ages 3 and 9, each year of follow-up increased their probability for psychotropic polypharmacy therapy, antipsychotic, and anticonvulsant use, with the most pronounced effect in children diagnosed at age 3 (Figure 2). For example, this age group showed an 85% (OR = 1.85; 95% CI, 1.38-2.47) increase in the probability for antipsychotic use at year 5 of follow-up. Respective odds ratios for anticonvulsant use and psychotropic polypharmacy therapy were 2.14 (95% CI, 1.45-3.16) and 1.80 (95% CI, 1.36-2.38). In contrast, children diagnosed after age 9 showed no significant growth in any of the 3 utilization outcomes over time.
Figure 2 illustrates the interactions between age at diagnosis and the 3 utilization outcomes. Probabilities are standardized to white males who live in a state with high ADHD prevalence and are not in foster care, not in poverty, and not disabled. For children at young age at ADHD diagnosis, the probability for use of psychotropic polypharmacy increased with each year of follow-up, whereas this trend appeared to be reversed for children at older age at cohort entry. Of note, younger age at ADHD diagnosis was a pronounced determinant of psychotropic polypharmacy, regardless of the biological age at follow-up. For example, at age 10, probabilities were distinctly higher for a child diagnosed at age 8 or age 5 than for a 10-year-old child just diagnosed with ADHD. Children diagnosed at age 9 or later had comparably low probabilities for psychotropic polypharmacy therapy no matter what follow-up year was considered.
Trends for the use of antipsychotics and anticonvulsants were quite similar. Again, younger age at ADHD diagnosis was highly associated with use of antipsychotics or anticonvulsants and showed continuous increases in later follow-up years. In contrast, use of antipsychotics or anticonvulsants in children with ADHD diagnosis in later years of childhood was generally lower and showed flat or decreasing probabilities over the 5-year follow-up period.
Psychotropic Polypharmacy Therapy and Diagnosis of Other Mental Health Disorders
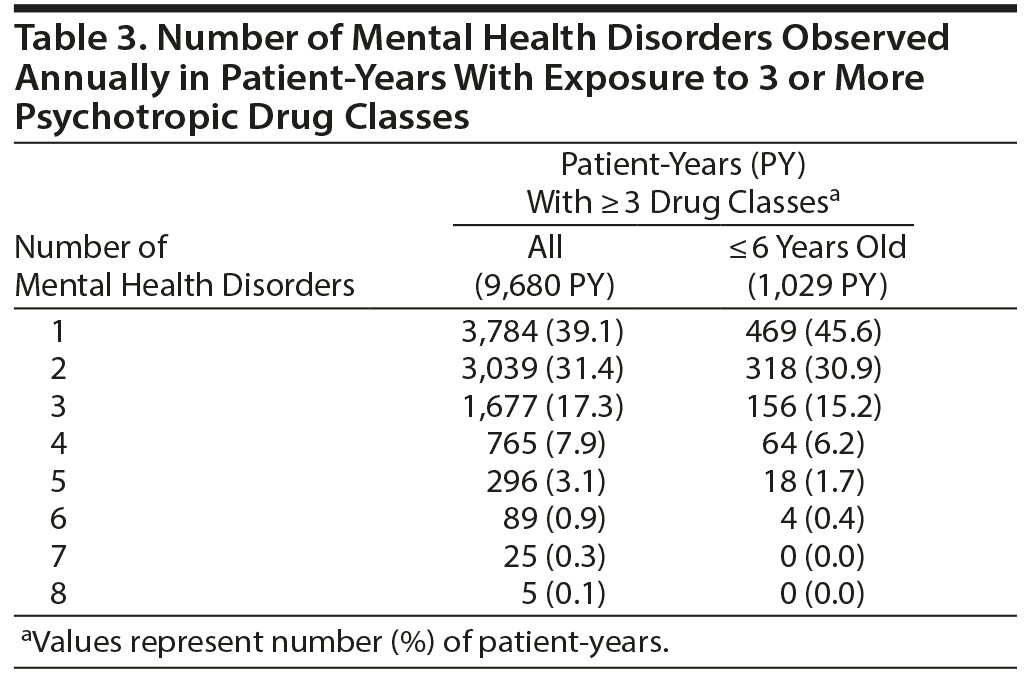
The most common concomitant mental health disorders in this pediatric ADHD population were oppositional defiant and conduct disorder (30.5%); learning, motor, and communication disorders (18.0%); and depression (16.1%, Table 1). Patient-years with psychotropic polypharmacy therapy had a mean of 1.92 (95% CI, 1.90-1.94) mental health diagnoses (including ADHD) compared to 1.35 (95% CI, 1.34-1.36) in children prescribed fewer than 3 medication classes (P < .0001), suggesting that psychotropic polypharmacy was introduced due to manifestation of concomitant mental health disorders. However, 39.1% of 9,680 children-years with psychotropic polypharmacy had only a diagnosis of ADHD with no other mental health diagnoses (Table 3). Likewise, examination of psychotropic polypharmacy therapy restricted to children age 6 or younger revealed 45.6% with only an ADHD diagnosis.
DISCUSSION
Our study has several important findings. First, utilization of psychotropic polypharmacy therapy in general, and antipsychotics and anticonvulsants in particular, increased during the study period (1999-2006). Focusing on newly diagnosed children with ADHD and no other mental health diagnoses or psychotropic medication use in the previous 6 months, we found that a quarter of children had at least 1 follow-up year in which prescriptions for psychotropic polypharmacy were filled. Second, in preschoolers and elementary-school children, each year of follow-up increased the probability for psychotropic polypharmacy, antipsychotic, and anticonvulsant use, while the opposite was true for older children. Third, even if adjusted for current age, calendar year, and year of follow-up, a child’s age at ADHD diagnosis was a strong predictor of psychotropic polypharmacy, antipsychotic, and anticonvulsant use. Specifically, a child at age 10 had a much higher probability to use psychotropic polypharmacy, antipsychotics, and anticonvulsants if the original diagnosis of ADHD had been made at age 6 compared to a child whose first ADHD diagnosis occurred at age 9. Finally, while presence of additional mental health diagnoses explained psychotropic polypharmacy therapy to a certain extent, more than a third of children-years with psychotropic polypharmacy therapy had only a diagnosis of ADHD. This observation was true across all age groups and slightly more pronounced in younger children.
Our findings confirm previous reports on increases in psychotropic polypharmacy therapy, but reported prevalence rates vary due to differences in underlying definitions.7,19,20 We used a liberal definition that required presence of 3 or more psychotropic medication classes within a given follow-up year, which cannot establish concomitant use. We further did not consider polypharmacy within a psychotropic medication class, which would have increased observed rates. Instead, we focused on describing children’s mental health treatment pattern in terms of exposure to varying psychotropic classes in order to identify populations at greatest need for further study. Based on these findings, the safety and effectiveness of combinations of stimulants, antipsychotics, and anticonvulsants deserve special attention. Without additional clinical detail, which is unavailable in administrative datasets, it is impossible to determine reasons for the relatively common coprescription of anticonvulsants, anxiolytics, antipsychotics, and antidepressants in these Medicaid patients despite the paucity of evidence-based support for these regimens.21 Yet, some plausible explanations include a failure to achieve remission with stimulant monotherapy,22 possible underdosing of stimulants,23 difficulty accessing psychosocial treatments,24 and complex comorbid clinical presentations, including clinically relevant problems with impulsivity, agitation, and aggression.
Other reports have described an association between younger age and use of stimulants,25,26 but little information is available on antipsychotic and anticonvulsant use in children with ADHD. Examining cohorts without requirement for specific mental health disorders, some studies have reported opposite age effects for use of antipsychotics5,27 and psychotropic polypharmacy,28 possibly due to different psychiatric profiles in general mental health populations compared to our cohort of children with ADHD.
We are unaware of any study that has investigated temporal changes in psychotropic treatment patterns of children who had new episodes of ADHD and no other preceding mental disorder diagnosis. That the complexity of pharmacologic treatment increased significantly over time raises questions about the underlying indications and disease progression. These questions are particularly important for the third of our study years where psychotropic polypharmacy occurred in children with only a diagnosis of ADHD. One explanation for such a multifaceted treatment regimen could be stimulant-resistant aggressive symptoms, which might be treated with risperidone and other antipsychotic medications.29 Consistent with this observation, previous reports have pointed out that children and adolescents with ADHD appear to account for a substantial proportion of antipsychotic use.30,31 Alternatively, it is possible that clinicians avoid giving additional diagnoses that may be perceived as being stigmatizing, such as oppositional defiant disorder or conduct disorder.
The most important finding in this context is the pronounced effect of the ADHD diagnosis age on psychotropic use pattern. It may not be surprising that children whose parents seek mental health services for them at an early age may have more severe or complex symptoms, resulting in psychotropic polypharmacy treatment approaches.32 However, because younger children showed no difference in the frequency of concomitant mental health disorders from their older counterparts, questions about the age-related differences in choice of treatment regimen remain.
There is limited evidence supporting the effectiveness and safety of ADHD medication in preschoolers. The 70-week, 6-site National Institute of Mental Health (NIMH) Preschool ADHD Treatment Study (PATS)33 reported that preschoolers may benefit from low doses of methylphenidate, but closer monitoring was required because of somewhat greater side effects. It is worth mentioning that participant children were included in the PATS study only if they failed to benefit from behavioral therapy. Such an approach follows current guideline protocols by using psychotherapy as first-line treatment.34 By contrast, medications are often prioritized over psychotherapy in clinical practice, especially primary care settings. For example, Finnerty and colleagues35 recently reported that most Medicaid-insured youth have not received a psychosocial service visit in the 3 months preceding their antipsychotic medication treatment initiation. Also, CDC data from public and private services found that approximately three-quarters of children aged 2-5 years with an ADHD diagnosis received medication, and only about half or fewer received any psychological services.36 The apparent disconnect between evidence-based medicine and current clinical practice37 is partly contingent on lack of proper training in evidence-based psychotherapies, insufficient financial incentives to provide it, barriers regarding coordination of care across specialties, and availability of such services.
In addition, several factors outside clinical settings may also help explain the current imbalance between medication and psychotherapy use. First, in the last couple of decades, medical education has prioritized training in pharmacotherapy over behavioral and psychosocial techniques.38 Second, increasing pressure from parents to reduce to a minimum social and cognitive impairments in their children may also be fueling the rise in ADHD medication use.39 Third, the pharmaceutical industry has invested heavily in direct-to-consumer marketing, with a 3-fold increase in their spending for psychotropic medication promotion between 1996 and 2005.40 This advertising overload may have contributed to altering the perception of the benefit/safety ratio (highlighting the effectiveness and reducing safety concerns) by clinicians and patients. Fourth, health insurance coverage varies from state to state and health plan to health plan, discouraging in some cases the use of behavioral therapy as a cost containment scheme.41 Lastly, the mental health specialist shortage throughout the United States remains a significant barrier.42 In light of limited clinical trial evidence concerning psychotropic polypharmacy regimens and antipsychotic or anticonvulsant use for ADHD alone, future comparative effectiveness and safety research might focus on preschool-aged and school-aged children, especially considering their vulnerability for adverse effects. That treatment patterns differ so dramatically in children without recent mental health history who enter mental health care at younger versus older age clearly deserves further investigation.
Several limitations of this study deserve mentioning. Our study used a large cohort of children eligible for Medicaid services in 28 states, and findings cannot be generalized to publicly insured children and adolescents. Because children receive comprehensive medication benefits under Medicaid, we are confident in the validity of the information on dispensed medications. We restricted our population to children who had not received psychotropic medications or any mental health diagnosis during a 6-month look-back period before the index ADHD diagnosis. While this approach does not assure that children were truly newly diagnosed with ADHD and naׯve to psychotropics, it does reflect a new episode of mental health treatment and psychotropic medication therapy. As now documented in the revised DSM-5 criteria, ADHD can manifest after age 7, which provides some assurance that our definition of diagnosis age may reflect the actual age of ADHD manifestation.43 Even though we controlled for various patient characteristics to ensure comparable age cohorts, there may be other unmeasured differences between the groups. We purposely did not adjust for any additional mental health disorders diagnosed during follow-up, because these disorders would be expected to correlate with treatment pattern.44 It is important to note that all cohorts consisted of newly diagnosed ADHD patients with no other mental health history or psychotropic treatment within 6 months prior to cohort entry. Thus, the observed age-related differences in treatment pattern may be explained by differences in diagnoses that followed the initial ADHD diagnosis but not the disorder spectrum that was documented at the time of study entry (ie, the first ADHD diagnosis). In addition, some of the clinical diagnostic patterns, such as the relatively high proportion of patients diagnosed with bipolar disorder, may reflect misapplications of formal diagnostic criteria.45 It should be noted that billing data in outpatient settings limit the number of ICD-9 codes reported. As a consequence, we may be underestimating both the number of eligible children with a compatible ADHD diagnosis and the number of their comorbidities, but such measurement error should affect age group to a similar extent. Concerns also exist regarding the validity of clinical pediatric diagnoses in administrative health data.46 Finally, the data are a decade old and may not be indicative of current medication trends for preschoolers with ADHD.
It is important to note that we did not require overlapping time periods for dispensed medication classes to consider them polypharmacy regimens in a given observation year. Thus, therapy may have been concomitant or, alternatively, it may have been sequential. In both instances, it appears as though for a substantial proportion of younger children, use of traditional and FDA-approved ADHD medications did not suffice or that other mental health comorbidities complicated the clinical course. This finding in younger children is in stark contrast to that in children who were diagnosed with ADHD later in childhood or adolescence where no increase in psychotropic polypharmacy (using the same definition), antipsychotic, or anticonvulsant use was observed. Important in this context is the increasing shift of ADHD treatment to primary care, which may result in different diagnostic and treatment practices than those observed by psychiatric specialists. We also need to differentiate more accurately whether the impressive rise of ADHD diagnosis is driven by increased awareness and appreciation of the disorder, by interactions between concomitant mental disorders, or by the increase of inaccurate diagnosis. The separation of these 3 factors would help sharpen treatment selection and may reduce unneeded polypharmacy. While billing data from physician office visits may not have captured all diagnoses and thus may not provide a comprehensive picture of type and severity of symptoms, it is unlikely that such imprecision would have been different across age groups. The diagnostic criteria for ADHD in this study have shown good predictive validity in terms of functional impairment over time.47 Also, rates of psychiatric comorbidity appear to be similar to those in older children.48
Future research should aim at a better understanding of the underlying concomitant disorders to help define clinical targets for intervention, especially in children who present for the treatment of ADHD at earlier ages. Earlier engagement of consultation with child and adolescent psychiatrists, especially for younger patients with more complex clinical presentations, may help to improve quality of care. At the same time, more research is needed on stepped-based models of care to inform the development of evidence-based algorithms to help guide management so that treatment modalities align with each patient’s clinical needs. Such research should further clarify the role that diagnosis age plays on illness expression, illness course, and psychotropic treatment regimen. Finally, further investigation of more recent data would be warranted to explore the effect of recent changes in diagnostic criteria and treatment guidelines on prescribing practices.
CONCLUSION
In this cohort of newly diagnosed children with ADHD without recent psychotropic medications, the probability of psychotropic polypharmacy, antipsychotic, and anticonvulsant use increased with each year of follow-up. However, this effect was strongly mediated by age at ADHD diagnosis with profound increases in all 3 outcomes in preschoolers and no such effect in children diagnosed with ADHD after elementary school. Thus, earlier diagnosis of ADHD was associated with increasingly complex therapy involving multiple non-ADHD medications. This effect was explained only in part by the presence of physician office claims with diagnoses of concomitant mental disorders.
Submitted: April 20, 2016; accepted October 6, 2016.
Published online: July 5, 2017.
Potential conflicts of interest: Dr Correll has been a consultant and/or advisor to or has received honoraria from Alkermes, Forum, Gerson Lehrman Group, IntraCellular Therapies, Janssen/J&J, Lundbeck, MedAvante, Medscape, Otsuka, Pfizer, ProPhase, Sunovion, Supernus, Takeda, and Teva; has provided expert testimony for Bristol-Myers Squibb, Janssen, and Otsuka; has served on a Data Safety Monitoring Board for Lundbeck and Pfizer; and has received grant support from Takeda. The remaining authors have no conflicts of interest to declare.
Funding/support: Funding for this study was partly received through the grant R01-HS0185606 from the Agency of Healthcare Research and Quality (AHRQ).
Role of the sponsor: The funding sources had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication.
Disclaimer: The views expressed herein are those of the authors and do not necessarily represent the views of the AHRQ, a division of the US Department of Health & Human Services.
Previous presentation: Presented at the 28th International Conference on Pharmacoepidemiology & Therapeutic Risk Management; August 23-26, 2012; Barcelona, Spain.
Additional information: The original data set for the Medicaid Extract Files (MAX) is available from the Centers for Medicare and Medicaid Services (CMS).
Supplementary material: See accompanying pages.
REFERENCES
1. Hsia Y, Maclennan K. Rise in psychotropic drug prescribing in children and adolescents during 1992-2001: a population-based study in the UK. Eur J Epidemiol. 2009;24(4):211-216. PubMed doi:10.1007/s10654-009-9321-3
2. Zwaanswijk M, van Dijk CE, Verheij RA. Child and adolescent mental health care in Dutch general practice: time trend analyses. BMC Fam Pract. 2011;12:133. PubMed doi:10.1186/1471-2296-12-133
3. Increasing Prevalence of Parent-Reported Attention-Deficit/Hyperactivity Disorder Among Children—United States, 2003 and 2007. CDC website. https://www.cdc.gov/mmwr/preview/mmwrhtml/mm5944a3.htm. Accessed July 20, 2016.
4. Chai G, Governale L, McMahon AW, et al. Trends of outpatient prescription drug utilization in US children, 2002-2010. Pediatrics. 2012;130(1):23-31. PubMed doi:10.1542/peds.2011-2879
5. Cooper WO, Arbogast PG, Ding H, et al. Trends in prescribing of antipsychotic medications for US children. Ambul Pediatr. 2006;6(2):79-83. PubMed doi:10.1016/j.ambp.2005.11.002
6. Olfson M, Crystal S, Huang C, et al. Trends in antipsychotic drug use by very young, privately insured children. J Am Acad Child Adolesc Psychiatry. 2010;49(1):13-23. PubMed
7. Comer JS, Olfson M, Mojtabai R. National trends in child and adolescent psychotropic polypharmacy in office-based practice, 1996-2007. J Am Acad Child Adolesc Psychiatry. 2010;49(10):1001-1010. PubMed doi:10.1016/j.jaac.2010.07.007
8. Olfson M, Blanco C, Liu SM, et al. National trends in the office-based treatment of children, adolescents, and adults with antipsychotics. Arch Gen Psychiatry. 2012;69(12):1247-1256. PubMed doi:10.1001/archgenpsychiatry.2012.647
9. Olfson M, Blanco C, Wang S, et al. National trends in the mental health care of children, adolescents, and adults by office-based physicians. JAMA Psychiatry. 2014;71(1):81-90. PubMed doi:10.1001/jamapsychiatry.2013.3074
10. Mojtabai R, Olfson M. National trends in psychotropic medication polypharmacy in office-based psychiatry. Arch Gen Psychiatry. 2010;67(1):26-36. PubMed doi:10.1001/archgenpsychiatry.2009.175
11. Bhatara V, Feil M, Hoagwood K, et al. National trends in concomitant psychotropic medication with stimulants in pediatric visits: practice versus knowledge. J Atten Disord. 2004;7(4):217-226. PubMed doi:10.1177/108705470400700404
12. Barner JC, Khoza S, Oladapo A. ADHD medication use, adherence, persistence and cost among Texas Medicaid children. Curr Med Res Opin. 2011;27(suppl 2):13-22. PubMed doi:10.1185/03007995.2011.603303
13. Bussing R, Winterstein AG. Polypharmacy in attention deficit hyperactivity disorder treatment: current status, challenges and next steps. Curr Psychiatry Rep. 2012;14(5):447-449. PubMed doi:10.1007/s11920-012-0295-6
14. Toteja N, Gallego JA, Saito E, et al. Prevalence and correlates of antipsychotic polypharmacy in children and adolescents receiving antipsychotic treatment. Int J Neuropsychopharmacol. 2014;17(7):1095-1105. PubMed doi:10.1017/S1461145712001320
15. Winterstein AG. Cardiovascular safety of stimulants in children: findings from recent population-based cohort studies. Curr Psychiatry Rep. 2013;15(8):379. PubMed doi:10.1007/s11920-013-0379-y
16. AHFS Drug Information 2016 Edition. AHFS Clinical Drug Information website. http://www.ahfsdruginformation.com/ahfs-drug-information/. Accessed July 20, 2016.
17. Littell RC, Milliken GA, Stroup WW, et al. SAS for Mixed Models, Second Edition. SAS website. https://www.sas.com/store/prodBK_59882_en.html. Accessed July 20, 2016.
18. Harrell FE. Regression Modeling Strategies: With Applications to Linear Models, Logistic Regression, and Survival Analysis. New York, NY: Springer New York; 2001. doi:10.1007/978-1-4757-3462-1
19. Chen H, Patel A, Sherer J, et al. The definition and prevalence of pediatric psychotropic polypharmacy. Psychiatr Serv. 2011;62(12):1450-1455. PubMed doi:10.1176/appi.ps.000642011
20. Zito JM, Safer DJ, Sai D, et al. Psychotropic medication patterns among youth in foster care. Pediatrics. 2008;121(1):e157-e163. PubMed doi:10.1542/peds.2007-0212
21. Olfson M. Combination psychotropic regimens in community practice. J Am Acad Child Adolesc Psychiatry. 2014;53(9):942-944. PubMed doi:10.1016/j.jaac.2014.05.018
22. The MTA Cooperative Group. Multimodal Treatment Study of Children with ADHD. A 14-month randomized clinical trial of treatment strategies for attention-deficit/hyperactivity disorder. Arch Gen Psychiatry. 1999;56(12):1073-1086. PubMed doi:10.1001/archpsyc.56.12.1073
23. Blader JC, Pliszka SR, Jensen PS, et al. Stimulant-responsive and stimulant-refractory aggressive behavior among children with ADHD. Pediatrics. 2010;126(4):e796-e806. PubMed doi:10.1542/peds.2010-0086
24. Zima BT, Bussing R, Tang L, et al. Quality of care for childhood attention-deficit/hyperactivity disorder in a managed care Medicaid program. J Am Acad Child Adolesc Psychiatry. 2010;49(12):1225-1237, 1237.e1-1237.e11. PubMed
25. Visser SN, Lesesne CA, Perou R. National estimates and factors associated with medication treatment for childhood attention-deficit/hyperactivity disorder. Pediatrics. 2007;119(suppl 1):S99-S106. PubMed doi:10.1542/peds.2006-2089O
26. Winterstein AG, Gerhard T, Shuster J, et al. Utilization of pharmacologic treatment in youths with attention deficit/hyperactivity disorder in Medicaid database. Ann Pharmacother. 2008;42(1):24-31. PubMed doi:10.1345/aph.1K143
27. Gersing K, Burchett B, March J, et al. Predicting antipsychotic use in children. Psychopharmacol Bull. 2007;40(3):116-124. PubMed
28. Constantine RJ, Boaz T, Tandon R. Antipsychotic polypharmacy in the treatment of children and adolescents in the fee-for-service component of a large state Medicaid program. Clin Ther. 2010;32(5):949-959. PubMed doi:10.1016/j.clinthera.2010.04.021
29. Armenteros JL, Lewis JE, Davalos M. Risperidone augmentation for treatment-resistant aggression in attention-deficit/hyperactivity disorder: a placebo-controlled pilot study. J Am Acad Child Adolesc Psychiatry. 2007;46(5):558-565. PubMed doi:10.1097/chi.0b013e3180323354
30. Crystal S, Olfson M, Huang C, et al. Broadened use of atypical antipsychotics: safety, effectiveness, and policy challenges. Health Aff (Millwood). 2009;28(5):w770-w781. PubMed doi:10.1377/hlthaff.28.5.w770
31. Birnbaum ML, Saito E, Gerhard T, et al. Pharmacoepidemiology of antipsychotic use in youth with ADHD: trends and clinical implications. Curr Psychiatry Rep. 2013;15(8):382. PubMed doi:10.1007/s11920-013-0382-3
32. Willoughby MT, Curran PJ, Costello EJ, et al. Implications of early versus late onset of attention-deficit/hyperactivity disorder symptoms. J Am Acad Child Adolesc Psychiatry. 2000;39(12):1512-1519. PubMed doi:10.1097/00004583-200012000-00013
33. Riddle MA, Yershova K, Lazzaretto D, et al. The Preschool Attention-Deficit/Hyperactivity Disorder Treatment Study (PATS) 6-year follow-up. J Am Acad Child Adolesc Psychiatry. 2013;52(3):264-278.e2. PubMed doi:10.1016/j.jaac.2012.12.007
34. Florida Psychotherapeutic Medication Guidelines for Children and Adolescents. University of South Florida Medicaid Drug Therapy Management Program for Behavioral Health website. http://medicaidmentalhealth.org/_assets/file/Guidelines/2015%20Florida%20Best%20Practice%20Medication%20Child-Adolescent%20Guidelines_online2.pdf. 2015. Accessed October 13, 2016.
35. Finnerty M, Neese-Todd S, Pritam R, et al. Access to psychosocial services prior to starting antipsychotic treatment among Medicaid-insured youth. J Am Acad Child Adolesc Psychiatry. 2016;55(1):69-76.e3. PubMed doi:10.1016/j.jaac.2015.09.020
36. Attention-Deficit/Hyperactivity Disorder (ADHD) Data and Statistics. CDC website. http://www.cdc.gov/ncbddd/adhd/data.html. Accessed July 21, 2016.
37. Chung J, Tchaconas A, Meryash D, et al. Treatment of attention-deficit/hyperactivity disorder in preschool-age children: child and adolescent psychiatrists’ adherence to clinical practice guidelines. J Child Adolesc Psychopharmacol. 2016;26(4):335-343. PubMed doi:10.1089/cap.2015.0108
38. McHugh RK, Barlow DH. The dissemination and implementation of evidence-based psychological treatments. A review of current efforts. Am Psychol. 2010;65(2):73-84. PubMed doi:10.1037/a0018121
39. Fewer Prescriptions for ADHD, Less Drug Abuse? The New York Times website. http://www.nytimes.com/roomfordebate/2012/06/09/fewer-prescriptions-for-adhd-less-drug-abuse/parents-have-fueled-the-abuse-of-adhd-medications. Accessed July 21, 2016.
40. Donohue JM, Cevasco M, Rosenthal MB. A decade of direct-to-consumer advertising of prescription drugs. N Engl J Med. 2007;357(7):673-681. PubMed doi:10.1056/NEJMsa070502
41. Dembosky A. Frustrated You Can’ t Find A Therapist? They’ re Frustrated, Too. Kais Health News website. http://khn.org/news/frustrated-you-cant-find-a-therapist-theyre-frustrated-too/. July 2016. Accessed July 22, 2016.
42. Thomas CR, Holzer CE 3rd. The continuing shortage of child and adolescent psychiatrists. J Am Acad Child Adolesc Psychiatry. 2006;45(9):1023-1031. PubMed doi:10.1097/01.chi.0000225353.16831.5d
43. NIH Fact Sheets – Attention Deficit Hyperactivity Disorder (ADHD). NIH Research Portfolio Online Reporting Tools (RePORT) website. https://report.nih.gov/nihfactsheets/ViewFactSheet.aspx?csid=25. Accessed July 20, 2016.
44. Shyu YC, Yuan SS, Lee SY, et al. Attention-deficit/hyperactivity disorder, methylphenidate use and the risk of developing schizophrenia spectrum disorders: A nationwide population-based study in Taiwan. Schizophr Res. 2015;168(1-2):161-167. PubMed doi:10.1016/j.schres.2015.08.033
45. Galanter CA, Pagar DL, Oberg PP, et al. Symptoms leading to a bipolar diagnosis: a phone survey of child and adolescent psychiatrists. J Child Adolesc Psychopharmacol. 2009;19(6):641-647. PubMed doi:10.1089/cap.2008.0151
46. Shiff NJ, Jama S, Boden C, et al. Validation of administrative health data for the pediatric population: a scoping review. BMC Health Serv Res. 2014;14:236. PubMed doi:10.1186/1472-6963-14-236
47. Lahey BB, Pelham WE, Loney J, et al. Three-year predictive validity of DSM-IV attention deficit hyperactivity disorder in children diagnosed at 4-6 years of age. Am J Psychiatry. 2004;161(11):2014-2020. PubMed doi:10.1176/appi.ajp.161.11.2014
48. Egger HL, Kondo D, Angold A. The epidemiology and diagnostic issues in preschool attention-deficit/hyperactivity disorder: a review. Infants & Young Children. 2006;19(2):109-122. doi:10.1097/00001163-200604000-00004
Editor’s Note: We encourage authors to submit papers for consideration as a part of our Focus on Childhood and Adolescent Mental Health section. Please contact Karen D. Wagner, MD, PhD, at [email protected].
Enjoy this premium PDF as part of your membership benefits!