See free commentary by Singh
Objective: To evaluate the presence of affective signs and symptoms as precursors of bipolar disorder in prospective studies, including assessment of their prevalence, duration, and predictive value.
Data Sources: We followed PRISMA guidelines to search PubMed, CINAHL, PsycINFO, EMBASE, SCOPUS, and ISI Web of Science databases to May 31, 2013, using the terms bipolar disorder AND (antecedent* OR predict* OR prodrom* OR prospect*) AND (diagnosis OR development). Hand searching of identified reports led to additional relevant references.
Study Selection: We included only English-language articles containing (1) prospective, longitudinal studies with at least 2 structured clinical assessments (intake and follow-up); (2) no previous DSM-III or DSM-IV diagnoses of bipolar I or bipolar II; and (3) diagnostic outcome of bipolar I or bipolar II. Studies of subjects at familial risk of bipolar disorder were excluded, as these have been reviewed elsewhere.
Data Extraction: We tabulated details of study design, outcomes, precursors, and predictive value. Only studies reporting a positive predictive association were included.
Results: In 26 published reports meeting selection criteria, methods varied widely in terms of design, duration of follow-up, ages, and populations investigated. Despite such heterogeneity in methods, findings were notably consistent. Precursors of bipolar disorder include mood lability, subsyndromal and major depression, subsyndromal hypomanic symptoms with or without major depression, cyclothymia and bipolar not otherwise specified, major depression with psychotic features, and other psychotic disorders. Bipolar disorder was also predicted by juvenile onset of major depression as well as frequency and loading of hypomanic or depressive symptoms.
Conclusions: Despite the limitations of published reports, prospectively identified precursors of bipolar disorder typically arose years prior to syndromal onset, often with significant early morbidity and disability. Prospectively identified precursors of bipolar disorder are generally consistent with findings in retrospective and family-risk studies. Combining precursors and other risk factors may increase predictive value, support earlier diagnosis, improve treatment, and limit disability in bipolar disorder.
This CME activity is expired. For more CME activities, visit CMEInstitute.com.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
ABSTRACT
Objective: To evaluate the presence of affective signs and symptoms as precursors of bipolar disorder in prospective studies, including assessment of their prevalence, duration, and predictive value.
Data Sources: We followed PRISMA guidelines to search PubMed, CINAHL, PsycINFO, EMBASE, SCOPUS, and ISI Web of Science databases to May 31, 2013, using the terms bipolar disorder AND (antecedent* OR predict* OR prodrom* OR prospect*) AND (diagnosis OR development). Hand searching of identified reports led to additional relevant references.
Study Selection: We included only English-language articles containing (1) prospective, longitudinal studies with at least 2 structured clinical assessments (intake and follow-up); (2) no previous DSM-III or DSM-IV diagnoses of bipolar I or bipolar II; and (3) diagnostic outcome of bipolar I or bipolar II. Studies of subjects at familial risk of bipolar disorder were excluded, as these have been reviewed elsewhere.
Data Extraction: We tabulated details of study design, outcomes, precursors, and predictive value. Only studies reporting a positive predictive association were included.
Results: In 26 published reports meeting selection criteria, methods varied widely in terms of design, duration of follow-up, ages, and populations investigated. Despite such heterogeneity in methods, findings were notably consistent. Precursors of bipolar disorder include mood lability, subsyndromal and major depression, subsyndromal hypomanic symptoms with or without major depression, cyclothymia and bipolar not otherwise specified, major depression with psychotic features, and other psychotic disorders. Bipolar disorder was also predicted by juvenile onset of major depression as well as frequency and loading of hypomanic or depressive symptoms.
Conclusions: Despite the limitations of published reports, prospectively identified precursors of bipolar disorder typically arose years prior to syndromal onset, often with significant early morbidity and disability. Prospectively identified precursors of bipolar disorder are generally consistent with findings in retrospective and family-risk studies. Combining precursors and other risk factors may increase predictive value, support earlier diagnosis, improve treatment, and limit disability in bipolar disorder.
J Clin Psychiatry 2015;76(5):614-624
© Copyright 2015 Physicians Postgraduate Press, Inc.
Submitted: November 22, 2013; accepted July 14, 2014 (doi:10.4088/JCP.13r08900).
‘ Deceased.
Corresponding author: Gianni L. Faedda, MD, 245 East 50th St, Ste 2A, New York, NY 10022 ([email protected]).
Bipolar disorder is a major psychiatric illness, with lifetime prevalence of approximately 1.0% for bipolar I, 1.1% for bipolar II, and 2.4% for bipolar not otherwise specified (NOS).1 Bipolar disorder is strongly associated with family psychiatric history and early onset age (peaking at ages 15-25 years) and is often comorbid with substance abuse, anxiety, behavioral, and personality disorders, with high rates of suicide as well as excess mortality from medical disorders.2 Diagnosis and treatment of bipolar disorder are typically delayed for 5-15 years from estimated onset, especially in adult cases involving young onset, particularly cases with initial depression.3
The transition from normality to illness occurs gradually in most psychiatric syndromes4 with the more or less subtle or gradual appearance of symptoms of varying degrees of severity, duration, co-occurrence, and associated disability. Although episodes of hypomania or mania can onset suddenly with little preceding psychopathology, many retrospective and family risk studies have detected attenuated symptoms before the syndromal onset of bipolar disorder,3,5-10 including mood-shifts, emotional lability, irritability, depressive and hypomanic symptoms, sleep disturbances, distractibility, hyperactivity, impulsivity, anxiety, and aggression; such symptoms have been identified 1.8-7.3 years before a first major mood episode and sometimes more than a decade earlier, especially in childhood or adolescence.1,3-7,10-15
Little is known about the prevalence of acute versus gradual onset of mania, hypomania, mixed states, and depression. Most studies of bipolar I and first-episode mania recruited inpatients and reported a sudden onset, more males, and a younger age at onset of mania compared to depression.9,16 Studies of bipolar II and first-episode depression that recruited inpatients and outpatients described a sudden onset of depression, usually in females, with a younger age at onset of depression.17,18
The relative frequency of prodromal manifestations is also unknown, and few studies report the onset type (ie, acute vs gradual), and the proportion of bipolar I and bipolar II cases is not always specified.3,5,8-10 Nevertheless, bipolar I or bipolar II usually onsets with depression, younger age at onset, more recurrences, and a more disabling course of illness.3,6,10,12,19 The early psychopathology of bipolar disorder may also alter normative developmental processes and further complicates the task of clarifying the development of the disorder in children, adolescents, and young adults.
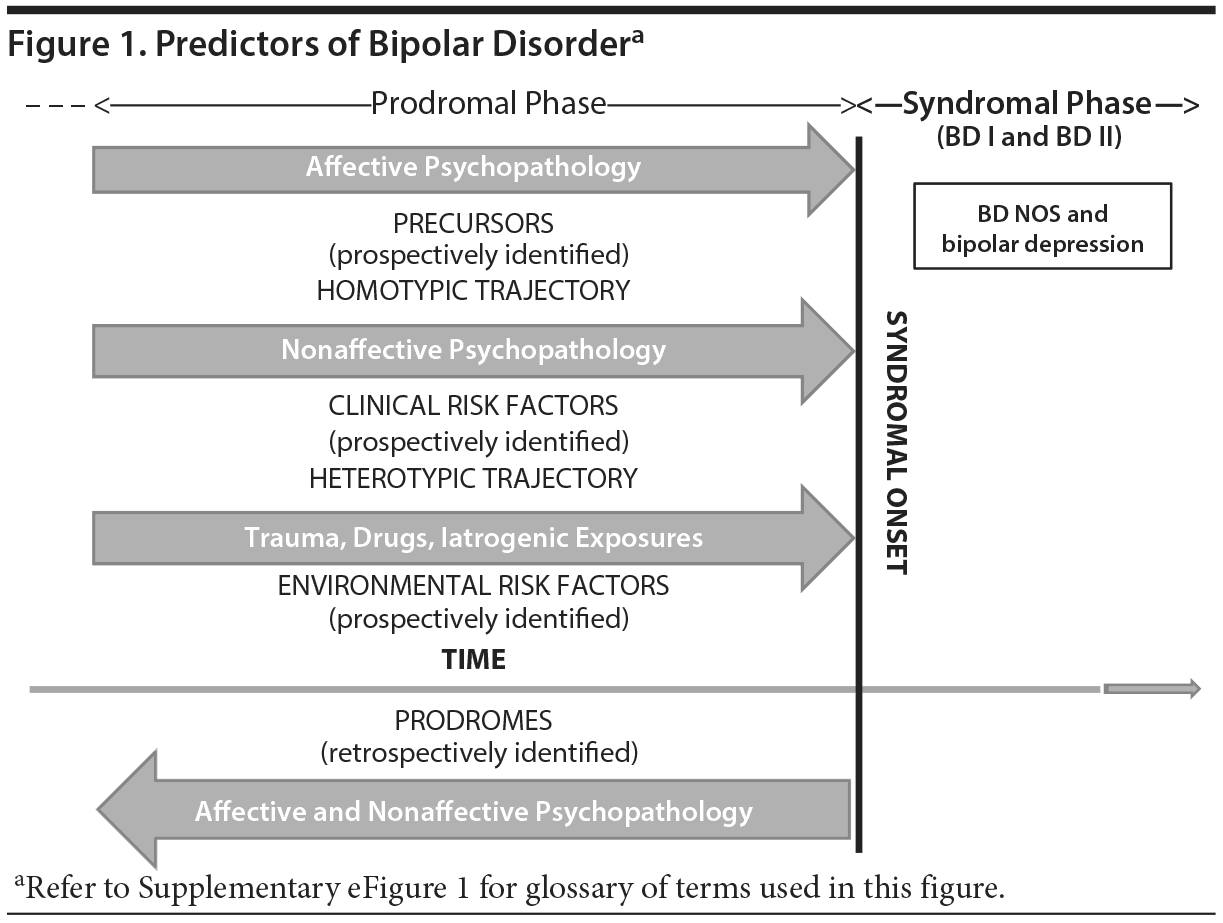
The lack of accepted terms to define and study the onset of bipolar disorder has prompted the International Society for Bipolar Disorder to convene a task force to improve timely diagnosis and early intervention. Among those clinical symptoms or syndromes that precede the syndromal onset of bipolar disorder, we define precursors, clinical risk factors, and environmental risk factors (exposures) as prospectively identified variables that increase the risk of later bipolar disorder (Figure 1; also Supplementary eFigure 1 [available at Psychiatrist.com]), as suggested by Eaton4; precursors and clinical and environmental risk factors are collectively referred to as clinical predictors. Risk factors can be environmental (prenatal and perinatal exposures, traumatic events, substances of abuse, effects of medicines) or personal (ie, clinical risk factors) and will be reviewed separately.
This review focuses on precursors of bipolar disorder, their characteristics and timing based on available prospective studies in which outcomes are bipolar I or bipolar II. Our emphasis on prospective studies reflects methodological concern to limit the effects of inaccurate or incomplete information (recall bias) and selection bias (diagnosed cases) associated with retrospective analyses.
Research addressed the following questions: (1) Is there evidence of a prodromal phase of bipolar disorder in prospective studies? (2) Are there specific premorbid affective signs and symptoms (precursors) that predict bipolar disorder? (3) What are the nature, timing, and duration of precursors? (4) How sensitive and specific are they in predicting later diagnosable bipolar disorder? and (5) Does the prodromal phase differ by bipolar subtype?

- Precursors of bipolar disorder include mood lability, subsyndromal hypomanic symptoms, subsyndromal depression, cyclothymia and bipolar not otherwise specified (NOS), and major depression, especially with hypomanic or psychotic symptoms.
- Monotonically increasing rates of progression to bipolar disorder were found in cohorts and community samples with isolated hypomanic symptoms, cyclothymic disorder, and bipolar NOS.
- Young age at onset of depression, hypomanic symptoms, cyclothymic temperament, psychotic features, suicidal ideation, and family history of bipolar disorder were associated with unfavorable clinical outcomes.
- The loading and persistence of hypomanic symptoms and positive family history increased the rates of bipolar disorder.
DATA SOURCES
We carried out a computerized search of PubMed, CINAHL, PsycINFO, EMBASE, SCOPUS, and ISI Web of Science databases from inception up to May 31, 2013, using the following search algorithm: (bipolar disorder AND [antecedent* OR predict* OR prodrom* OR prospect*] AND [diagnosis OR development]). Hand searching of references in identified reports led to additional relevant reports.
STUDY SELECTION AND DATA EXTRACTION
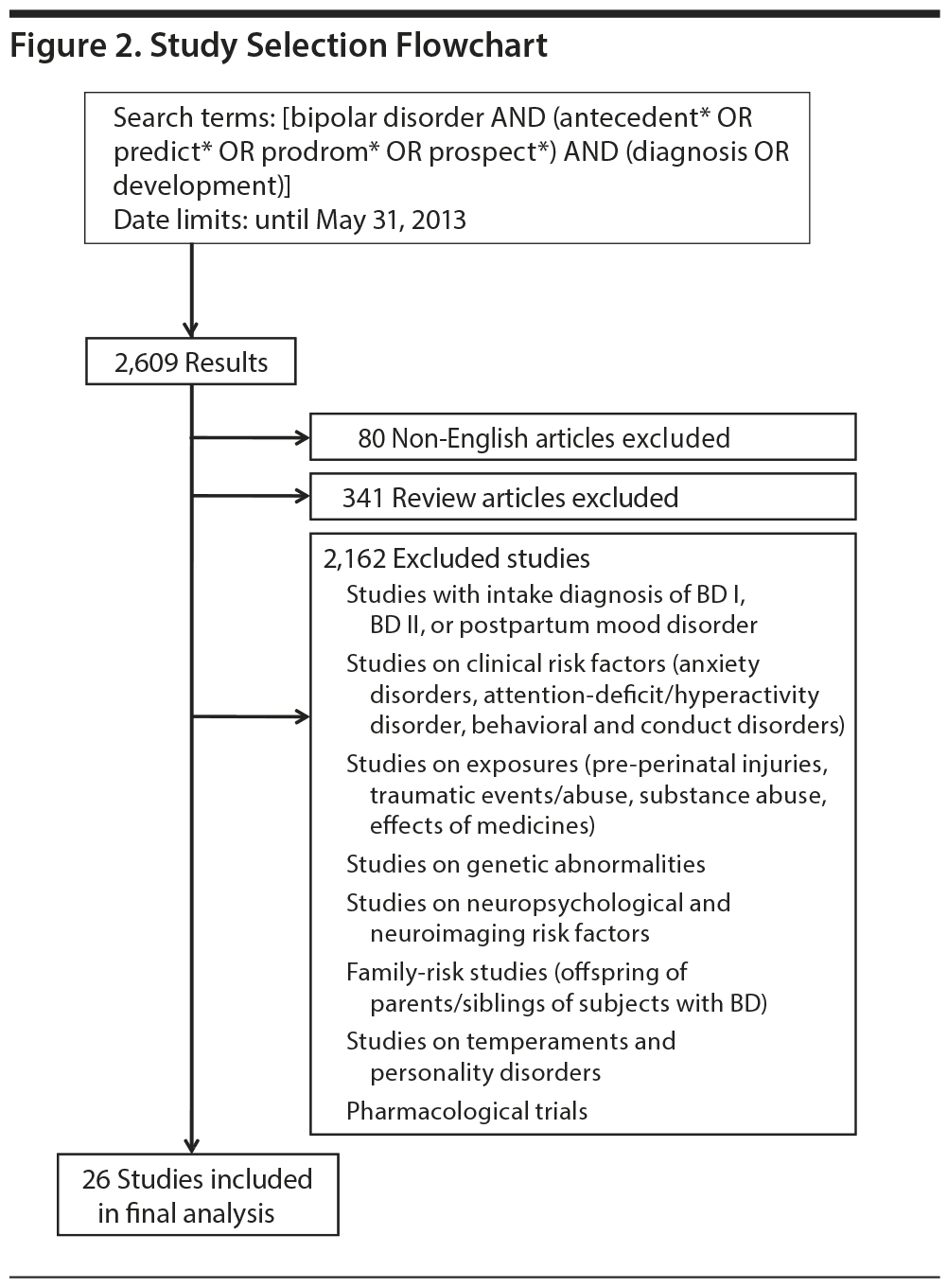
Articles selected were published in the English language and met the following inclusion criteria: (1) prospective, longitudinal studies with at least 2 structured clinical assessments (intake and follow-up); (2) diagnoses at intake that included DSM-III or DSM-IV major depressive episode (MDE) and major depressive disorder (MDD), dysthymia, cyclothymia, or bipolar NOS as well as subjects with subsyndromal affective disorders or symptoms; (3) diagnostic outcome at follow-up of bipolar I or bipolar II. Exclusion criteria are detailed in Figure 2.
We identified a total of 26 reports meeting inclusion criteria. We followed PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses: http://www.prisma-statement.org) guidelines, and for each article selected, we extracted the following information: number of subjects, initial diagnosis, age at intake, study design and assessment tool, duration of follow-up, percentage of subjects diagnosed as bipolar I or bipolar II during follow-up, and clinical features predicting later bipolar diagnosis and their statistical power (odds ratio [OR] or adjusted odds ratio, hazard ratio, likelihood ratio, or Bayesian sensitivity, specificity, and positive or negative predictive value). Only studies reporting a positive predictive value were included in this review.
We excluded family-risk studies (offspring of parents/siblings of subjects diagnosed with bipolar disorder), as they have been reviewed elsewhere.20 Also, while many affected patients have a positive family history for bipolar disorder, this is not true for all patients with bipolar disorder, because of misdiagnosis, undiagnosed illness, recurrent depression not meeting criteria for bipolar disorder, or the lack of family history. This suggests that there may be sporadic or nonfamilial forms of illness. Furthermore, most family risk studies focus on offspring of adults or siblings of subjects with bipolar I,2 although there are exceptions.14,15
RESULTS
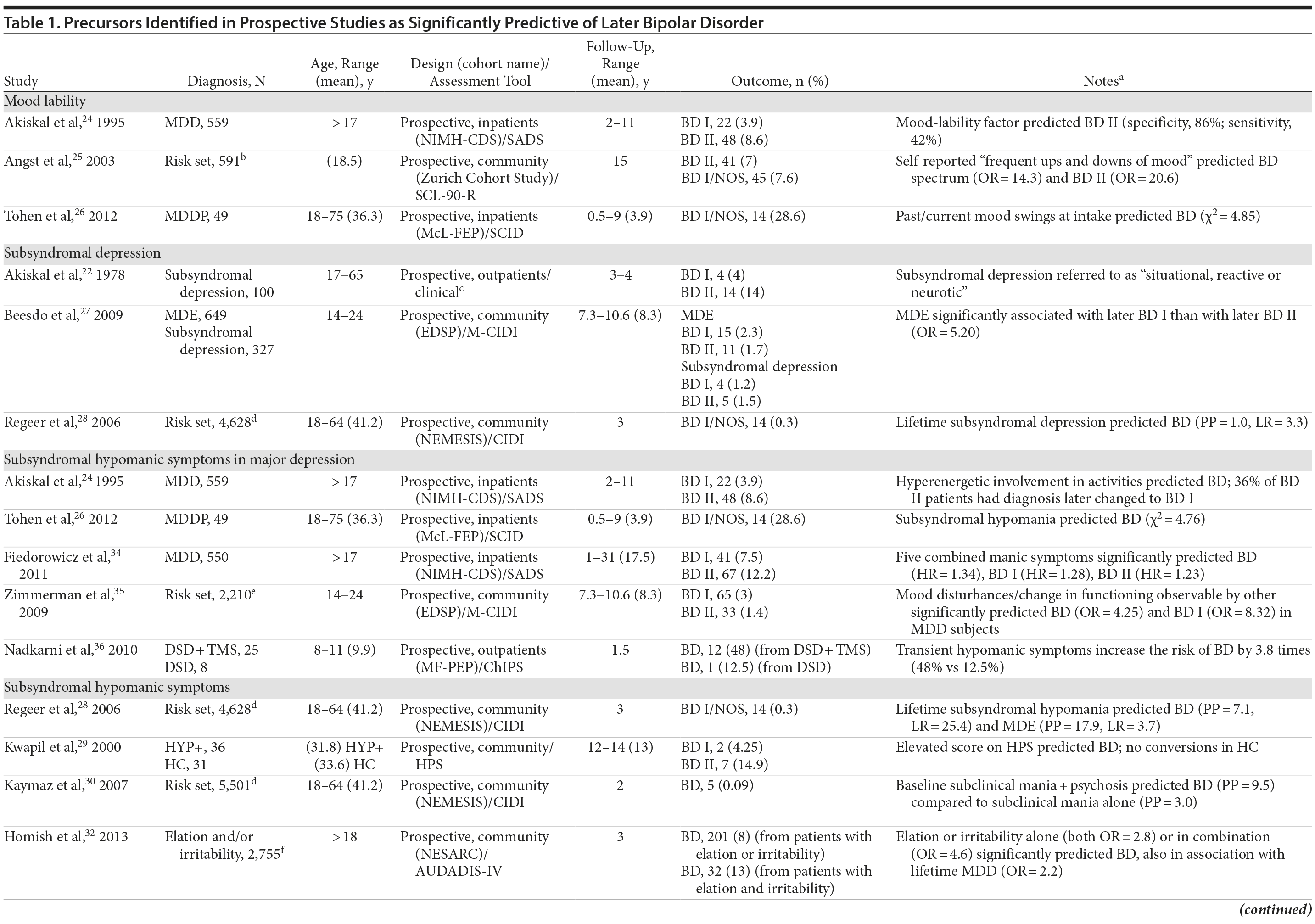
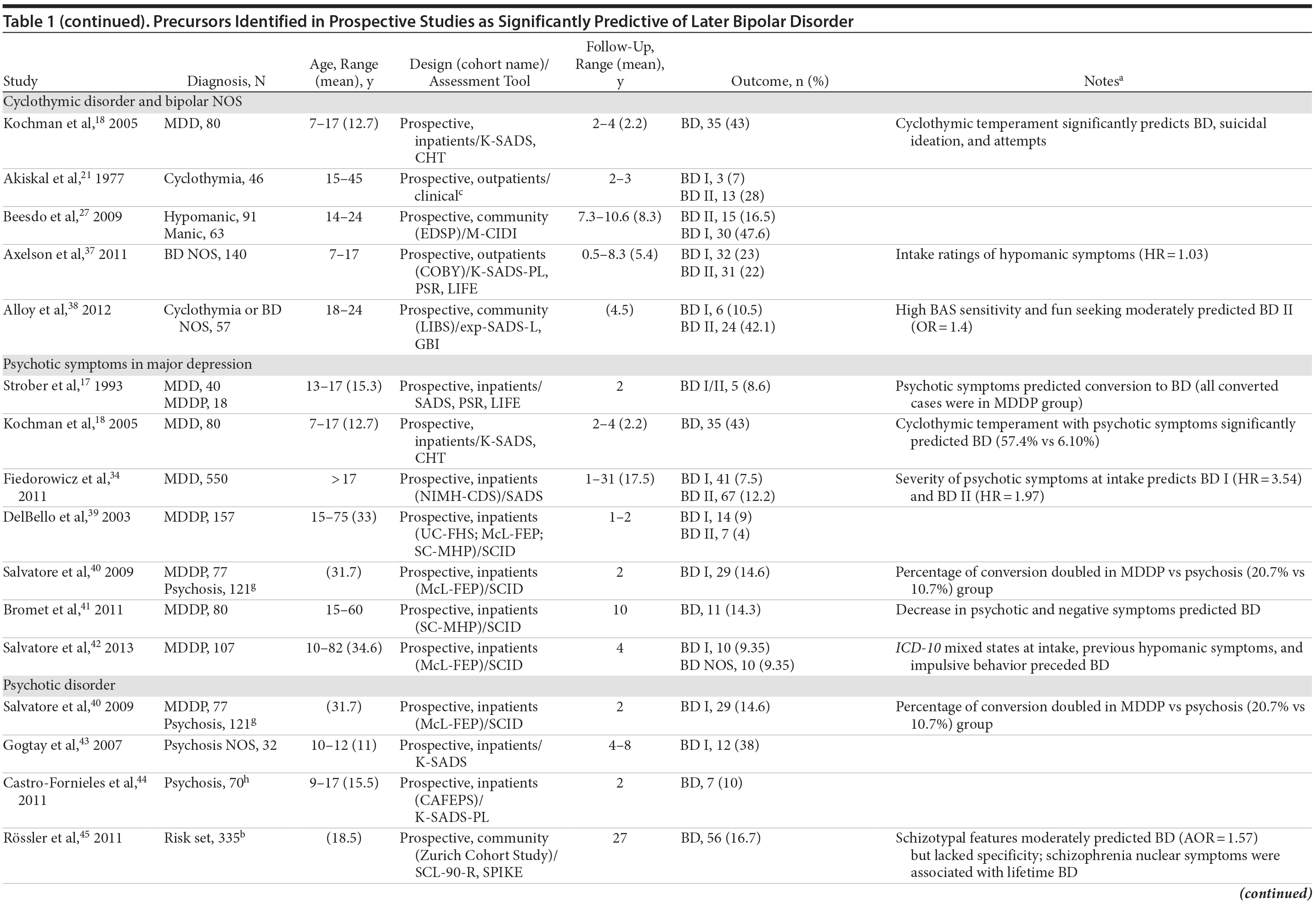
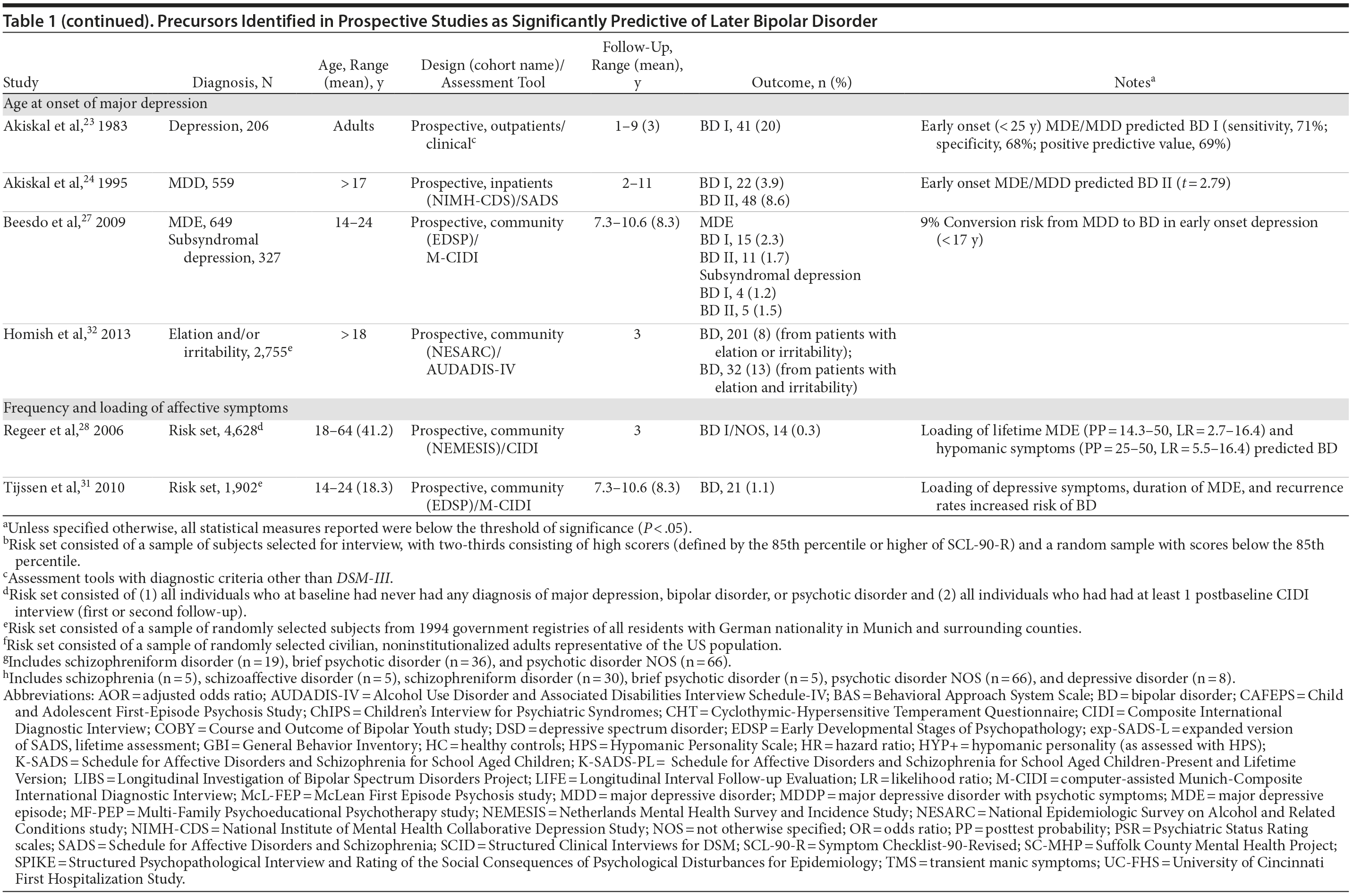
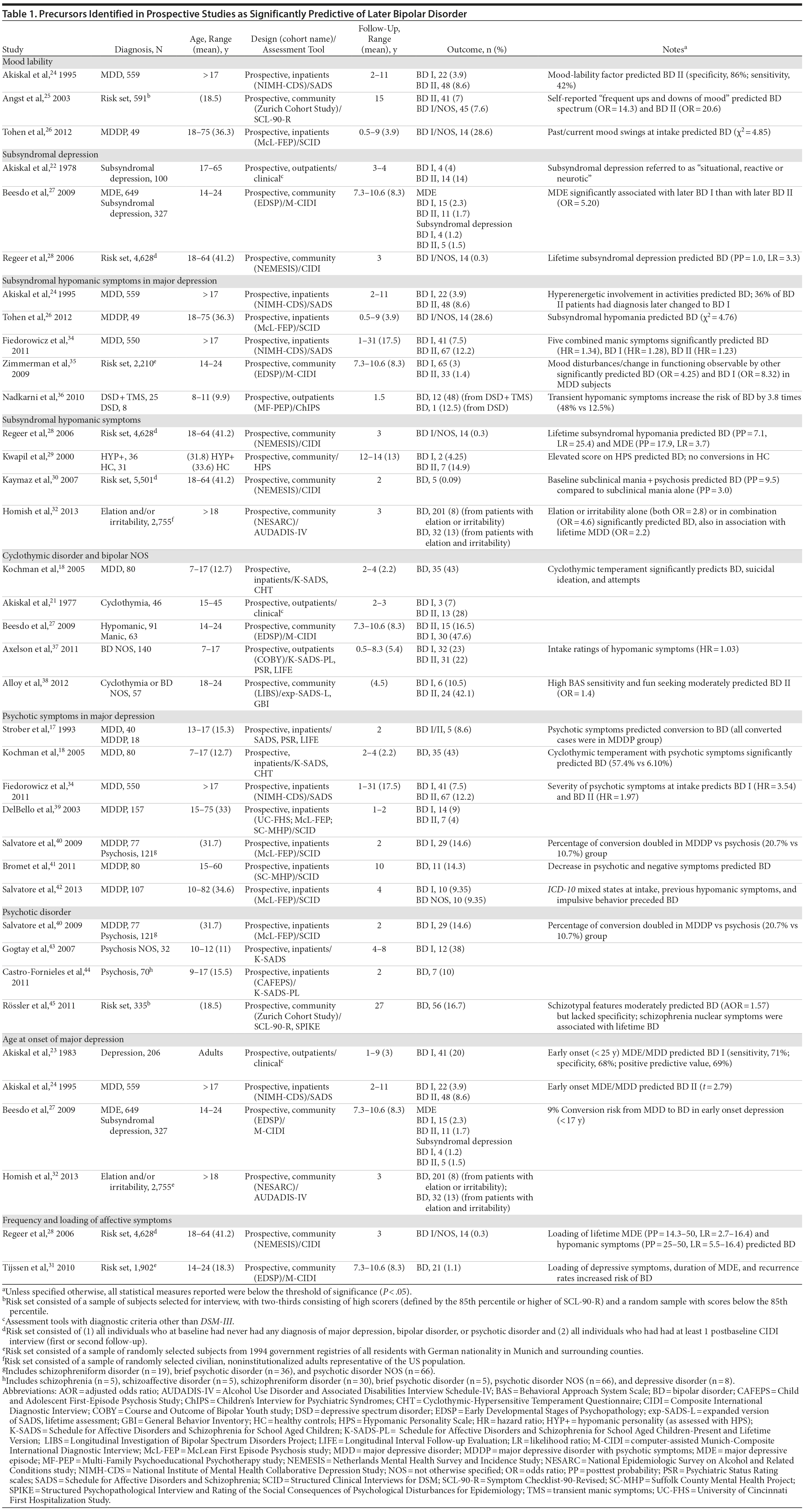
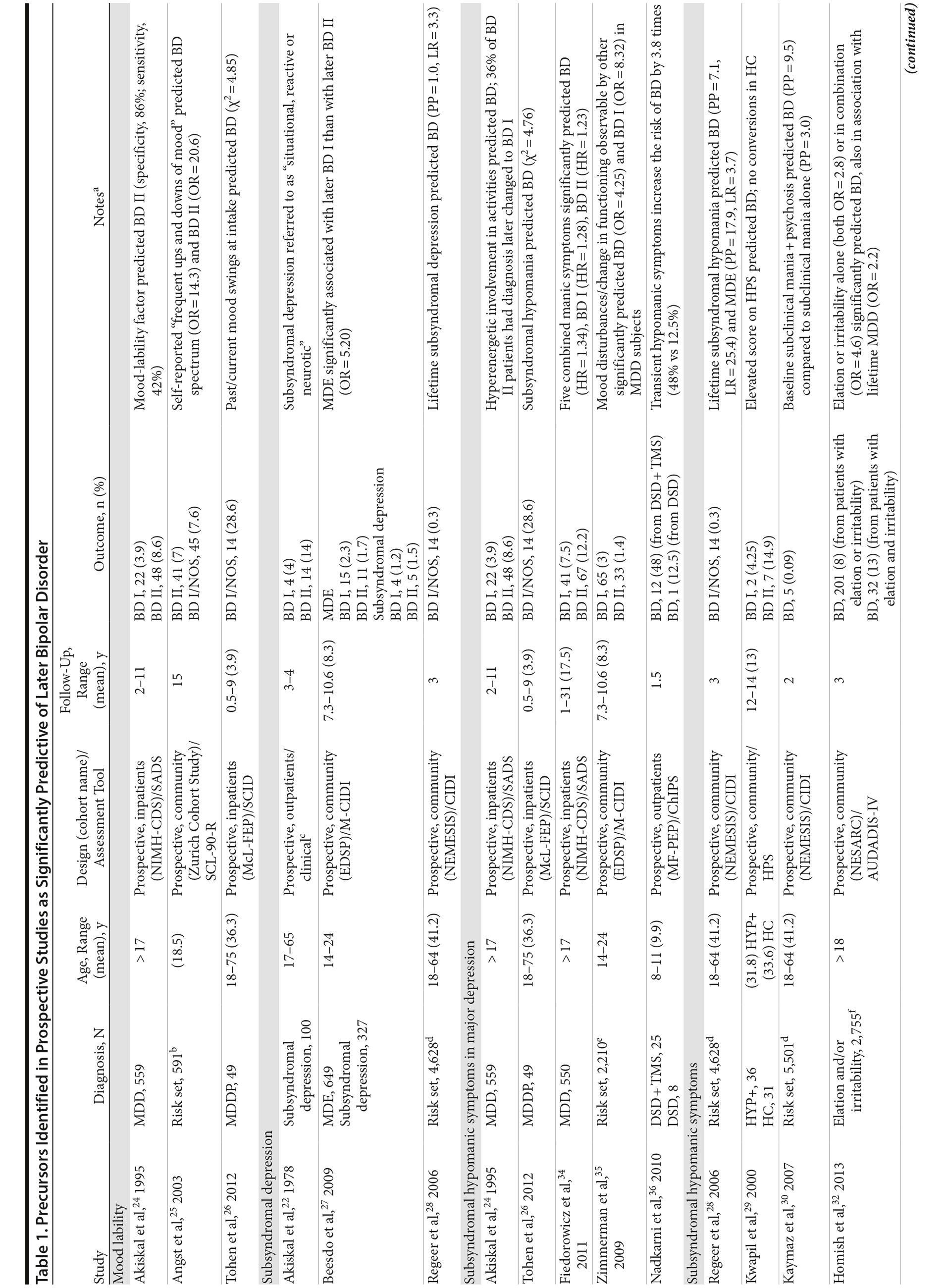
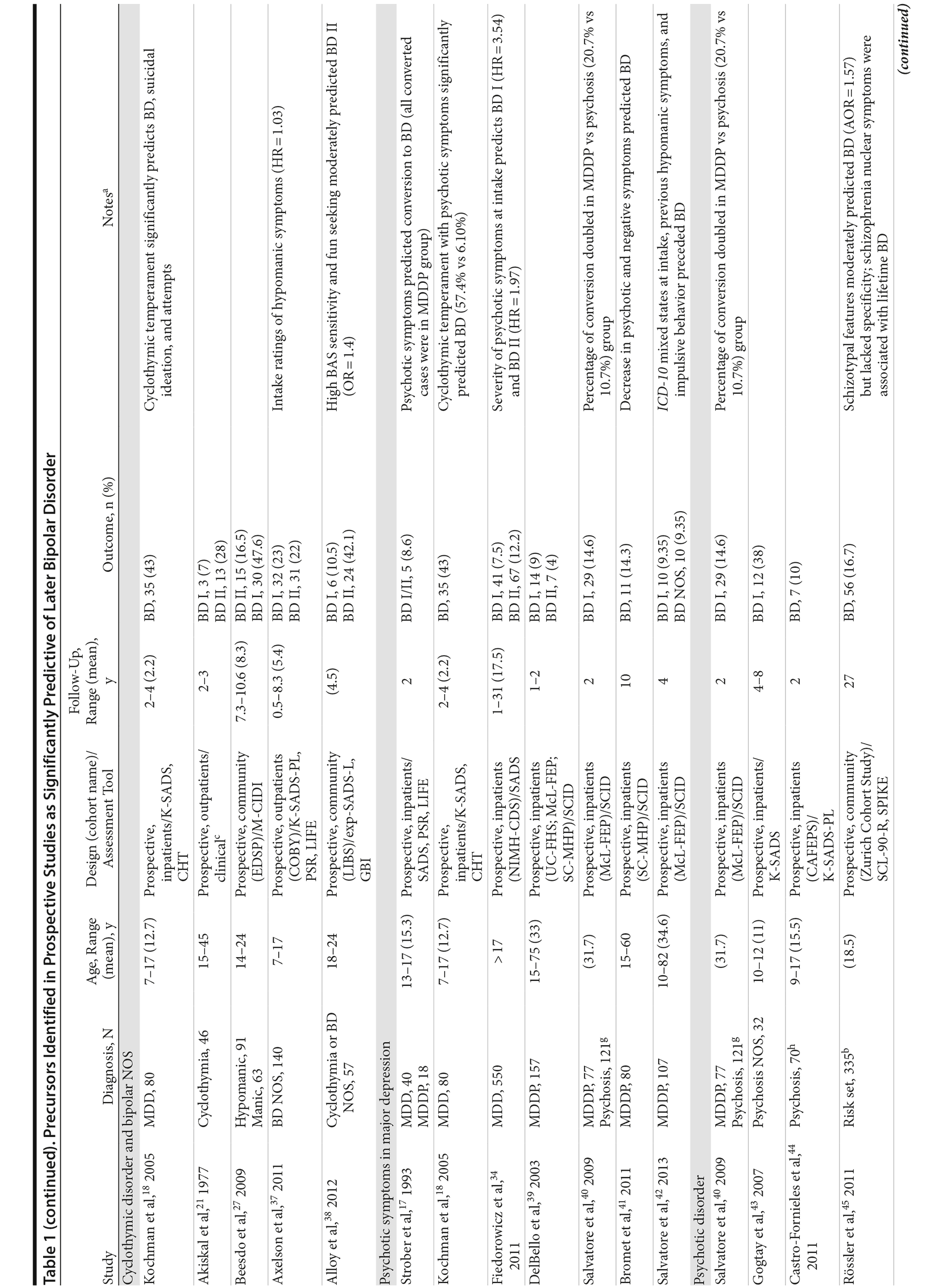
Figure 2 shows a flowchart of the number of articles identified and their disposition; Table 1 summarizes the findings obtained.

Summary of Methods Used in the Studies
Sample characteristics. Six studies included child and/or adolescent subjects, 12 studies included adult subjects, and 8 studies included subjects spanning from childhood to adulthood. All studies included subjects of both sexes. The group sample sizes for the studies varied widely, with groups as small as 32 to as large as 5,501.
Diagnosis. Six studies included subjects with intake diagnosis of MDD or depression, 6 studies included samples with MDD with psychotic features, 3 studies included psychotic (non-MDD) patients, 3 studies included subjects diagnosed with cyclothymic disorder or bipolar NOS, 5 studies had subjects with subsyndromal depressive or hypomanic symptoms, and 6 community studies included subjects at risk (see Table 1). Diagnoses were obtained with structured interviews using DSM-III, DSM-III–R, or DSM-IV criteria in all studies selected except for Akiskal et al.21-23 The assessment tools also included self-reports of hypomanic or temperamental features in patients with major and minor depression (see Table 1), but their validity, reliability, or predictive value was not always reported and could not be operationalized. We refer the reader to the original reports for details about the psychometric properties of instruments used.
Design. All studies included were longitudinal and prospective: 11 studies included inpatients, 5 studies followed outpatients, and 10 studies included a community sample. The duration of follow-up varied markedly, ranging from 6 months to 31 years.
Summary of Results
Mood lability. We found that mood lability predicted bipolar II (but not bipolar I) in adult inpatients with MDD,24 whereas it predicted bipolar II and bipolar spectrum disorders (MDD and subsyndromal hypomania) in young adults in a community risk set.25 Past or current mood lability at intake predicted a change of diagnosis to bipolar I or bipolar NOS in adults hospitalized for MDD with psychotic features.26
Subsyndromal depression. An 18% rate of later diagnoses of bipolar disorder, especially bipolar II, was reported among adult outpatients with mild depressive episodes (defined as situational, reactive, or neurotic)22; lower rates were reported in community studies of young adults (1.5% bipolar II, 1.2% bipolar I)27 and adults (0.3% for bipolar disorder).28
Subsyndromal hypomanic symptoms. Elevated scores on the Hypomanic Personality Scale significantly predicted later bipolar disorder, especially bipolar II,29 in a cohort of college students compared to healthy controls. Also, lifetime subsyndromal hypomanic symptoms predicted bipolar I, bipolar NOS, and a major depressive episode in a Dutch community sample of adults,28 and the combination of subclinical mania with subclinical psychosis at baseline predicted 3 times more new diagnoses of bipolar disorder as compared to those with subclinical mania only.30 In the Early Developmental Stages of Psychopathology (EDSP) community study, the majority of youths experiencing an episode of hypomania or mania experienced isolated hypomanic and/or depressive symptoms; number and persistence of symptoms increased monotonically during prospective follow-up before criteria for bipolar disorder were met.31 In a community study, symptoms of elation or irritability, and especially their combination, predicted later hypomania or mania independent of major depression in 3 years of follow-up.32
Major depression. We recently reviewed studies (both prospective and retrospective) on rates of conversion from MDD to bipolar I or bipolar II, differentiating cases of spontaneous conversion from those emerging with antidepressant use.33 The rate of spontaneous hypomania or mania was 3.3% (0.36% per year) and similar in prospective and retrospective studies but much lower than the 8.2% (4.1% per year) risk of mania or hypomania associated with antidepressant treatment; moreover, changes of diagnosis to bipolar disorder were 4.5 times higher among juveniles than adults.33
Subsyndromal hypomanic symptoms in major depression. In adults with current MDD,24 the presence of the hypomanic symptom hyperenergetic involvement in activities predicted diagnostic switch to bipolar disorder, with more cases involving later hypomanic than manic episodes; however, more than one-third of those diagnosed with bipolar II later developed mania, suggesting a progression of intensity of mood elevation. In the same cohort, but with longer follow-up,34 the sum of ratings of 5 hypomanic symptoms moderately but significantly predicted bipolar disorder, with a similar relationship to later mania or hypomania; in bivariate analyses, decreased need for sleep, unusually high energy, and increased goal-directed activity significantly predicted both hypomania and mania, whereas grandiosity predicted only mania. The presence of at least 3 hypomanic symptoms was fairly specific in predicting bipolar disorder.34
The presence of subsyndromal hypomania at baseline in a cohort of community at-risk adolescents and young adults with lifetime MDD significantly increased the likelihood of a later diagnosis of bipolar and bipolar I (compared to those without); in particular, “mood disturbances or change in functioning observable by others” (DSM-IV manic episode, criterion D) was a strong predictor of change of diagnosis from MDD to bipolar disorder and especially to bipolar I.35 Similarly, the presence of current subsyndromal hypomanic symptoms significantly predicted bipolar I and bipolar NOS in psychotic MDD adults.26 Additionally, among children with depressive spectrum disorders (MDD and/or dysthymia), the presence of transient manic symptoms was associated with almost 4 times increase in bipolar spectrum disorders (bipolar I, bipolar II, or bipolar NOS) after 18 months of follow-up.36
Cyclothymic disorder and bipolar NOS. Among adolescent and adult outpatients diagnosed with cyclothymic disorder, 35% developed bipolar disorder within 3 years,21 while in children and adolescents hospitalized with MDD, high scores on the Cyclothymic-Hypersensitive Temperament Rating Scale significantly predicted diagnoses of bipolar disorder.18
Among youths with hypomania but without a lifetime history of major depression, 16.5% developed an MDE and were rediagnosed as bipolar II, while the rest continued to experience hypomania alone.27 Higher rates of conversion from bipolar NOS to bipolar disorder were also reported in the Course and Outcome of Bipolar Youth study37: over 5 years, 23% were rediagnosed with bipolar I (following hypomania in 61% of cases) and 22% with bipolar II; elevated intake ratings of hypomanic symptoms predicted conversion. Of 119 subjects without a lifetime history of hypomania at intake, later bipolar disorder occurred in 44% (24% bipolar I, 20% bipolar II), particularly in those with a family history of mania or hypomania.37
A similar pattern of results in adults with bipolar NOS or cyclothymic disorder were reported by Alloy,38 who found that more than half developed bipolar disorder over 4.5 years, especially bipolar II; higher levels of interpersonal sensitivity and fun seeking predicted conversion.38
Psychotic symptoms in major depression. Psychotic features predicted conversion to bipolar disorder in a cohort of adolescents hospitalized for MDD (compared to those without psychotic features),17 a finding replicated by Kochman18: depressed youths with psychotic features and cyclothymic temperament were 9.40 times more likely to be diagnosed with bipolar disorder compared to those without.
Several prospective studies reported further evidence of diagnostic instability of psychotic MDD and its conversion to bipolar disorder, both in adolescents and adults.34,39-42
Psychotic disorders. In children hospitalized and initially diagnosed with psychosis NOS, 38% met criteria for bipolar I within 8 years,43 while another group reported a lower rate of conversion but with a shorter follow-up duration.44 Finally, in a 27-year follow-up of a community group of at-risk subjects, schizotypal features moderately predicted later bipolar disorder but lacked specificity45; similarly, schizophrenia nuclear symptoms (assessed with the Symptom Checklist-90-Revised) were associated with a lifetime diagnosis of bipolar disorder but also with phobias.45
Age at onset of major depression. Akiskal et al23 found that early onset of depression (age < 25 years) predicted later bipolar disorder; several other prospective studies24,27,32 had similar findings.
Frequency and loading of affective symptoms. The risk of bipolar disorder increased with the number of lifetime depressive episodes and with the number of hypomanic symptoms.28 Longer episodes of depression, greater loading of depressive symptoms, and higher recurrence rates predicted increased risk of later diagnoses of bipolar disorder.31
DISCUSSION
We found evidence of a prodromal phase of bipolar disorder, characterized by several precursors. Precursors of bipolar disorder had significant time depth, anticipating syndromal onset by years. Manic and depressive symptoms appeared early and increased in number, duration, and secondary impairment, following a chronic rather than episodic course over several years. Hypomanic and depressive symptoms increased the risk of their own recurrence and of the occurrence of episodes of opposite polarity. Monotonically increasing rates of progression to bipolar disorder were found in cohorts and community samples with isolated hypomanic symptoms,27-30,32,34,36 cyclothymic disorder,18,21,38 and bipolar NOS as well as those prospectively diagnosed with bipolar II and bipolar I.27,37,38 In spite of the relative frequency of unipolar hypomanic presentations, there was little or no evidence of a progression to mania as a necessary outcome, with significant numbers of those diagnosed with cyclothymic disorder or bipolar NOS never progressing to mania or those meeting criteria for bipolar II never experiencing mania.18,27,37,38
Some precursors were selective for bipolar I or bipolar II, but data on phenomenological differences by subtype in the prodromal features observed are insufficient.
While acute onset of mania or depression is often reported in retrospective studies,3,5,12 the presence of chronic and gradually worsening symptoms was found in most cases.
We also found a good deal of consistency between the present findings and those identified with retrospective studies.
Affective lability or mood swings before the diagnosis of bipolar disorder have been described in retrospective analyses of both youths and adults,5,8,10,46-48 although these symptoms were observed in only a significant minority of adults: 30% of bipolar I,21 33% of bipolar II,49 and 17% of first-episode bipolar I patients with psychotic features.48 We found that mood lability and cyclothymic features preceding depressive episodes were associated mainly with bipolar II18,21,24,25 and predicted bipolar II in 2 juvenile cohorts,18,38 confirming the presence of a homotypic trajectory of illness’ development.
A depressive onset is common in all subtypes of bipolar and cyclothymic disorder both in retrospective3,5,6,8,12,50 and prospective studies17,18,24,27,34,36-38 as well as family risk studies.15,20 Minor depression with subsyndromal hypomania in children predicted bipolar I and bipolar II,27,36 while in bipolar I adults presenting with euphoria and grandiosity, cross-sectional ORs were elevated for both dysthymia (OR = 13.6) and MDD (OR = 18.4).51 Young age at onset of depression, hypomanic symptoms (such as brief mood-elevation, irritability, increased energy, restlessness, or agitation), cyclothymic temperament, psychotic features, suicidal ideation, and a family history of bipolar disorder were associated with change in diagnosis to later bipolar disorder,18,24,27,30,31,34,45 a finding confirmed in retrospective studies.5,19,52-54 When minor or major depression occurred in the absence of putative markers of bipolar disorder (ie, hypomanic features, young onset age, or family history), the risk of progression to bipolar disorder was not increased.27,36 While the diagnoses of bipolar disorder are highly stable and reliable,40 variable proportions of subjects initially diagnosed with major depression were later rediagnosed as bipolar. Such outcome has been described in a substantial proportion of patients, especially in youth and early adulthood5,6,8,10,14,15,27 and often in response to antidepressant treatment.55 It is therefore a priority to identify those forms that tend to recur or develop into hypomania or mania, as this knowledge might have important diagnostic and prognostic value.
High scores in ratings of hypomanic personality traits and hypomanic symptoms in young depressed patients as well as early onset hypomania have predicted bipolar disorder in only a minority of subjects over relatively short periods of follow-up.27,28,32,36-38 Youths diagnosed with bipolar NOS at intake have later met criteria for bipolar I or II in less than half of cases within 5 years of follow-up, suggesting a developmental continuum of manic severity.27,37 Nevertheless, some cases of cyclothymic disorder, bipolar NOS, and bipolar II remain stable and do not develop into mania.27,37,38,56 In the Course and Outcome of Bipolar Youth study,37 at 2, 4, and 5 years of follow-up, 25%, 38%, and 45% of bipolar-NOS patients met criteria for bipolar I or II, and 28% followed a progression from bipolar NOS to bipolar II before experiencing mania, whereas 24% did not have another mood episode within 5 years. These findings suggest that the predictive power and diagnostic specificity of hypomanic symptoms and attenuated syndromes (cyclothymic disorder and bipolar NOS) for mania may be limited or that these syndromes themselves might represent stable outcomes. It is also clear, however, that in some adolescents, persistence (rather than the sole presence) of hypomanic or manic symptoms increases the risk of a progression to diagnosable bipolar disorder.31
Recurrent unipolar hypomania was found in 42% of the youths with bipolar disorder in the EDSP study.27 It is possible that such frequent occurrence of hypomanic symptoms in youth might represent developmental variations or self-limiting delays in mood regulation. Similarly, in the Longitudinal Assessment of Manic Symptoms study, Findling et al57 reported that only 15% of youths with high scores on the Parent-General Behavior Inventory (scores > 12) developed bipolar disorder; most of those went through an attenuated bipolar syndrome with most hypomanic symptoms either remitting with development or failing to progress to a bipolar syndrome. Consistent with the EDSP findings,27,56 hypomanic or manic symptoms might increase the risk of bipolar disorder only if recurrent, persistent or both, and especially when associated with other precursors (depressive symptoms31,36) and risk factors.27,36,56 Therefore, while hypomanic or manic symptoms were sensitive, they were not necessarily specific; they helped identify the subjects whose symptoms loading or persistence increased the risk for bipolar disorder.
Early onset of bipolar disorder was associated with greater familial risk of mood disorders17,21,37,39 as well as with suicidal risk, psychotic features, mixed episodes, substance abuse, panic disorder, attention-deficit/hyperactivity disorder, early sexual or physical abuse, neuropsychological dysfunction, poor response to lithium treatment, or unfavorable clinical outcomes.3,20,24,34,35,54,57 The presence of additional risk factors like a family history of bipolar disorder36-38 or the co-occurrence (loading) and persistence of hypomanic symptoms was correlated with increased rates of transition to bipolar disorder.31
From a prevention-early identification perspective, the predictive value of precursors is lower than it is for risk factors, as the definition of the outcome includes such signs and symptoms. To increase predictive power and accurately identify populations with different types and levels of risk, it is often necessary to combine different, ideally independent risk markers. Populations with 1 or more of the known precursors (eg, hypomania, mood swings), risk factors (socioeconomic, family history of bipolar disorder, an anxiety disorder), and exposures (cannabis abuse, trauma) should then be monitored to assess the variable’s predictive value.17,18,32,35-38,54,57
In a prevention model, a different threshold besides the syndromal one can be useful. For instance, different thresholds could be used based on symptoms progression, associated disability, and developmental delays: a monitoring threshold, an intervention’s threshold, and a treatment threshold might be helpful in establishing monitoring and treatment guidelines.
Limitations of this review are substantial. Heterogeneity of studies and samples precluded pooling of data that might clarify the timing and duration of such precursors. Similarly, only few studies provided data on sensitivity, specificity, and predictive value of reported precursors. Notably, the prevalence, sequence, and timing of psychopathology predictive of bipolar disorder remain understudied, lacking sensitivity and specificity. The assessment tools, their validity, reliability, or predictive value could not be operationalized in a review of published reports. While these are objective and not methodological limitations, a cautious interpretation of the findings as to their generalizability is necessary. Specifically, it prevents the use of the data summarized in efforts to define stages of illness other than the obvious presyndromal and postsyndromal phases. Family risk studies were not reviewed here, as they have been reviewed elsewhere.14,15,20 Finally, this review focused on the putative presence of a progression of affective psychopathology and did not address clinical risk factors, exposures (Figure 1), or the interaction of precursors, clinical risk factors, exposures, and other risk factors like family history of bipolar disorder or recurrent depression.
Drug names: lithium (Lithobid and others).
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Author affiliations: Lucio Bini Mood Disorders Center and New York University Medical Center and Child Study Center, New York, New York (Dr Faedda); International Consortium for Bipolar Disorder Research, McLean Hospital, Belmont (Drs Faedda, Salvatore, Vázquez, Tondo, and Baldessarini); Department of Psychiatry, Harvard Medical School, Boston (Drs Serra, Salvatore, Sani, Tondo, and Baldessarini), Massachusetts; Section of Psychiatry, Department of Biomedical and Specialty Surgical Sciences, University of Ferrara (Dr Marangoni); Centro Lucio Bini (Drs Serra, Sani, Tondo, Girardi, and Koukopoulos’ ); NESMOS Department (Neuroscience, Mental Health and Sensory Organs), “La Sapienza” University School of Medicine and Psychology, and Lithium Clinic, Sant’ Andrea Hospital (Drs Serra, Sani, and Girardi); IRCCS Santa Lucia Foundation, Department of Clinical and Behavioral Neurology, Neuropsychiatry Laboratory, “La Sapienza” University School of Medicine (Dr Sani), Rome; Section of Psychiatry, Department of Neuroscience, University of Parma (Dr Salvatore); Centro Lucio Bini, Cagliari (Dr Tondo), Italy; and Department of Neuroscience, University of Palermo, Buenos Aires, Argentina (Dr Vázquez).
‘ Deceased.
Financial disclosure: Drs Faedda, Marangoni, Serra, Salvatore, Sani, Vázquez, Tondo, Girardi, Baldessarini, and Koukopoulos have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: This study was supported by an NIMH award RC1 MH089743 to Martin H. Teicher, PhD, MD (with Dr Faedda); National Institutes of Health grants MH-47370 and MH-73049; a grant from the Aretצus Association and Lucio Bini Private Donors Research Fund (Dr Tondo); a NARSAD Young Investigator Award to Dr Salvatore; and a grant from the Bruce J. Anderson Foundation and the McLean Private Donors Research Fund (to Dr Baldessarini).
Role of the sponsor: The funding sources had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; and preparation, review, or approval of the manuscript.
Previous presentations: Findings from this review were presented as a poster at the International Society for Bipolar Disorders Meeting in Miami (June 13-16, 2013) and were Drs Faedda, Baldessarini, and Salvatore’s contribution to the “ISBD’s Task Force on Prodromes of Bipolar Disorder,” co-chaired by Drs Christoph Correll and Faedda.
Supplementary material: Available at PSYCHIATRIST.COM
REFERENCES
1. Merikangas KR, Akiskal HS, Angst J, et al. Lifetime and 12-month prevalence of bipolar spectrum disorder in the National Comorbidity Survey replication. Arch Gen Psychiatry. 2007;64(5):543-552. PubMed doi:10.1001/archpsyc.64.5.543
2. Goodwin FK, Jamison KR, eds. Manic Depressive Illness: Bipolar Disorder and Recurrent Depression. 2nd ed. New York, NY: Oxford University Press; 2007.
3. Leverich GS, Post RM, Keck PE Jr, et al. The poor prognosis of childhood-onset bipolar disorder. J Pediatr. 2007;150(5):485-490. PubMed doi:10.1016/j.jpeds.2006.10.070
4. Eaton WW, Badawi M, Melton B. Prodromes and precursors: epidemiologic data for primary prevention of disorders with slow onset. Am J Psychiatry. 1995;152(7):967-972. PubMed
5. Lish JD, Dime-Meenan S, Whybrow PC, et al. The National Depressive and Manic-Depressive Association (DMDA) survey of bipolar members. J Affect Disord. 1994;31(4):281-294. PubMed doi:10.1016/0165-0327(94)90104-X
6. Faedda GL, Baldessarini RJ, Suppes T, et al. Pediatric-onset bipolar disorder: a neglected clinical and public health problem. Harv Rev Psychiatry. 1995;3(4):171-195. PubMed doi:10.3109/10673229509017185
7. Egeland JA, Hostetter AM, Pauls DL, et al. Prodromal symptoms before onset of manic-depressive disorder suggested by first hospital admission histories. J Am Acad Child Adolesc Psychiatry. 2000;39(10):1245-1252. PubMed doi:10.1097/00004583-200010000-00011
8. Faedda GL, Baldessarini RJ, Glovinsky IP, et al. Pediatric bipolar disorder: phenomenology and course of illness. Bipolar Disord. 2004;6(4):305-313. PubMed doi:10.1111/j.1399-5618.2004.00128.x
9. Berk M, Dodd S, Callaly P, et al. History of illness prior to a diagnosis of bipolar disorder or schizoaffective disorder. J Affect Disord. 2007;103(1-3):181-186. PubMed doi:10.1016/j.jad.2007.01.027
10. Skjelstad DV, Malt UF, Holte A. Symptoms and signs of the initial prodrome of bipolar disorder: a systematic review. J Affect Disord. 2010;126(1-2):1-13. PubMed doi:10.1016/j.jad.2009.10.003
11. Youngstrom EA, Birmaher B, Findling RL. Pediatric bipolar disorder: validity, phenomenology, and recommendations for diagnosis. Bipolar Disord. 2008;10(1,pt 2):194-214. PubMed doi:10.1111/j.1399-5618.2007.00563.x
12. Perlis RH, Dennehy EB, Miklowitz DJ, et al. Retrospective age at onset of bipolar disorder and outcome during two-year follow-up: results from the STEP-BD study. Bipolar Disord. 2009;11(4):391-400. PubMed doi:10.1111/j.1399-5618.2009.00686.x
13. Shankman SA, Lewinsohn PM, Klein DN, et al. Subthreshold conditions as precursors for full syndrome disorders: a 15-year longitudinal study of multiple diagnostic classes. J Child Psychol Psychiatry. 2009;50(12):1485-1494. PubMed doi:10.1111/j.1469-7610.2009.02117.x
14. Vandeleur C, Rothen S, Gholam-Rezaee M, et al. Mental disorders in offspring of parents with bipolar and major depressive disorders. Bipolar Disord. 2012;14(6):641-653. PubMed doi:10.1111/j.1399-5618.2012.01048.x
15. Mesman E, Nolen WA, Reichart CG, et al. The Dutch bipolar offspring study: 12-year follow-up. Am J Psychiatry. 2013;170(5):542-549. PubMed doi:10.1176/appi.ajp.2012.12030401
16. Tohen M, Strakowski SM, Zarate C Jr, et al. The McLean-Harvard first-episode project: 6-month symptomatic and functional outcome in affective and nonaffective psychosis. Biol Psychiatry. 2000;48(6):467-476. PubMed doi:10.1016/S0006-3223(00)00915-X
17. Strober M, Lampert C, Schmidt S, et al. The course of major depressive disorder in adolescents, 1: recovery and risk of manic switching in a follow-up of psychotic and nonpsychotic subtypes. J Am Acad Child Adolesc Psychiatry. 1993;32(1):34-42. PubMed doi:10.1097/00004583-199301000-00006
18. Kochman FJ, Hantouche EG, Ferrari P, et al. Cyclothymic temperament as a prospective predictor of bipolarity and suicidality in children and adolescents with major depressive disorder. J Affect Disord. 2005;85(1-2):181-189. PubMed doi:10.1016/j.jad.2003.09.009
19. Judd LL, Schettler PJ, Akiskal H, et al. Prevalence and clinical significance of subsyndromal manic symptoms, including irritability and psychomotor agitation, during bipolar major depressive episodes. J Affect Disord. 2012;138(3):440-448. PubMed doi:10.1016/j.jad.2011.12.046
20. Duffy A, Alda M, Hajek T, et al. Early stages in the development of bipolar disorder. J Affect Disord. 2010;121(1-2):127-135. PubMed doi:10.1016/j.jad.2009.05.022
21. Akiskal HS, Djenderedjian AM, Rosenthal RH, et al. Cyclothymic disorder: validating criteria for inclusion in the bipolar affective group. Am J Psychiatry. 1977;134(11):1227-1233. PubMed
22. Akiskal HS, Bitar AH, Puzantian VR, et al. The nosological status of neurotic depression: a prospective three- to four-year follow-up examination in light of the primary-secondary and unipolar-bipolar dichotomies. Arch Gen Psychiatry. 1978;35(6):756-766. PubMed doi:10.1001/archpsyc.1978.01770300098011
23. Akiskal HS, Walker P, Puzantian VR, et al. Bipolar outcome in the course of depressive illness: phenomenologic, familial, and pharmacologic predictors. J Affect Disord. 1983;5(2):115-128. PubMed doi:10.1016/0165-0327(83)90004-6
24. Akiskal HS, Maser JD, Zeller PJ, et al. Switching from ‘ unipolar’ to bipolar II: an 11-year prospective study of clinical and temperamental predictors in 559 patients. Arch Gen Psychiatry. 1995;52(2):114-123. PubMed doi:10.1001/archpsyc.1995.03950140032004
25. Angst J, Gamma A, Endrass J. Risk factors for the bipolar and depression spectra. Acta Psychiatr Scand suppl. 2003;108(418):15-19. PubMed doi:10.1034/j.1600-0447.108.s418.4.x
26. Tohen M, Khalsa HM, Salvatore P, et al. Two-year outcomes in first-episode psychotic depression: the McLean-Harvard First-Episode Project. J Affect Disord. 2012;136(1-2):1-8. PubMed doi:10.1016/j.jad.2011.08.028
27. Beesdo K, Höfler M, Leibenluft E, et al. Mood episodes and mood disorders: patterns of incidence and conversion in the first three decades of life. Bipolar Disord. 2009;11(6):637-649. PubMed doi:10.1111/j.1399-5618.2009.00738.x
28. Regeer EJ, Krabbendam L, de Graaf R, et al. A prospective study of the transition rates of subthreshold (hypo)mania and depression in the general population. Psychol Med. 2006;36(5):619-627. PubMed doi:10.1017/S0033291705006823
29. Kwapil TR, Miller MB, Zinser MC, et al. A longitudinal study of high scorers on the hypomanic personality scale. J Abnorm Psychol. 2000;109(2):222-226. PubMed doi:10.1037/0021-843X.109.2.222
30. Kaymaz N, van Os J, de Graaf R, et al. The impact of subclinical psychosis on the transition from subclinicial mania to bipolar disorder. J Affect Disord. 2007;98(1-2):55-64. PubMed doi:10.1016/j.jad.2006.06.028
31. Tijssen MJ, van Os J, Wittchen HU, et al. Prediction of transition from common adolescent bipolar experiences to bipolar disorder: 10-year study. Br J Psychiatry. 2010;196(2):102-108. PubMed doi:10.1192/bjp.bp.109.065763
32. Homish GG, Marshall D, Dubovsky SL, et al. Predictors of later bipolar disorder in patients with subthreshold symptoms. J Affect Disord. 2013;144(1-2):129-133. PubMed doi:10.1016/j.jad.2012.06.020
33. Baldessarini RJ, Faedda GL, Offidani E, et al. Antidepressant-associated mood-switching and transition from unipolar major depression to bipolar disorder: a review. J Affect Disord. 2013;148(1):129-135. PubMed doi:10.1016/j.jad.2012.10.033
34. Fiedorowicz JG, Endicott J, Leon AC, et al. Subthreshold hypomanic symptoms in progression from unipolar major depression to bipolar disorder. Am J Psychiatry. 2011;168(1):40-48. PubMed doi:10.1176/appi.ajp.2010.10030328
35. Zimmermann P, Brückl T, Nocon A, et al. Heterogeneity of DSM-IV major depressive disorder as a consequence of subthreshold bipolarity. Arch Gen Psychiatry. 2009;66(12):1341-1352. PubMed doi:10.1001/archgenpsychiatry.2009.158
36. Nadkarni RB, Fristad MA. Clinical course of children with a depressive spectrum disorder and transient manic symptoms. Bipolar Disord. 2010;12(5):494-503. PubMed doi:10.1111/j.1399-5618.2010.00847.x
37. Axelson DA, Birmaher B, Strober MA, et al. Course of subthreshold bipolar disorder in youth: diagnostic progression from bipolar disorder not otherwise specified. J Am Acad Child Adolesc Psychiatry. 2011;50(10):1001-1016, e3. PubMed doi:10.1016/j.jaac.2011.07.005
38. Alloy LB, Urošević S, Abramson LY, et al. Progression along the bipolar spectrum: a longitudinal study of predictors of conversion from bipolar spectrum conditions to bipolar I and II disorders. J Abnorm Psychol. 2012;121(1):16-27. PubMed doi:10.1037/a0023973
39. DelBello MP, Carlson GA, Tohen M, et al. Rates and predictors of developing a manic or hypomanic episode 1 to 2 years following a first hospitalization for major depression with psychotic features. J Child Adolesc Psychopharmacol. 2003;13(2):173-185. PubMed doi:10.1089/104454603322163899
40. Salvatore P, Baldessarini RJ, Tohen M, et al. McLean-Harvard International First-Episode Project: two-year stability of DSM-IV diagnoses in 500 first-episode psychotic disorder patients. J Clin Psychiatry. 2009;70(4):458-466. PubMed doi:10.4088/JCP.08m04227
41. Bromet EJ, Kotov R, Fochtmann LJ, et al. Diagnostic shifts during the decade following first admission for psychosis. Am J Psychiatry. 2011;168(11):1186-1194. PubMed doi:10.1176/appi.ajp.2011.11010048
42. Salvatore P, Baldessarini RJ, Khalsa HM, et al. Predicting diagnostic change among patients diagnosed with first-episode DSM-IV-TR major depressive disorder with psychotic features. J Clin Psychiatry. 2013;74(7):723-731, quiz 731. PubMed doi:10.4088/JCP.12m08328
43. Gogtay N, Ordonez A, Herman DH, et al. Dynamic mapping of cortical development before and after the onset of pediatric bipolar illness. J Child Psychol Psychiatry. 2007;48(9):852-862. PubMed doi:10.1111/j.1469-7610.2007.01747.x
44. Castro-Fornieles J, Baeza I, de la Serna E, et al. Two-year diagnostic stability in early-onset first-episode psychosis. J Child Psychol Psychiatry. 2011;52(10):1089-1098. PubMed doi:10.1111/j.1469-7610.2011.02443.x
45. Rössler W, Hengartner MP, Ajdacic-Gross V, et al. Sub-clinical psychosis symptoms in young adults are risk factors for subsequent common mental disorders. Schizophr Res. 2011;131(1-3):18-23. PubMed doi:10.1016/j.schres.2011.06.019
46. Fergus EL, Miller RB, Luckenbaugh DA, et al. Is there progression from irritability/dyscontrol to major depressive and manic symptoms? a retrospective community survey of parents of bipolar children. J Affect Disord. 2003;77(1):71-78. PubMed doi:10.1016/S0165-0327(02)00176-3
47. Luckenbaugh DA, Findling RL, Leverich GS, et al. Earliest symptoms discriminating juvenile-onset bipolar illness from ADHD. Bipolar Disord. 2009;11(4):441-451. PubMed doi:10.1111/j.1399-5618.2009.00684.x
48. Salvatore PBR, Baldessarini RJ, Khalsa HM, Vázquez GH, et al. Antecedents of manic vs other first-psychotic episodes in 263 bipolar-I disorder patients. Acta Psychiatr Scand 2014;129(4):275-285. doi:10.1111/acps.12170 PubMed
49. Skjelstad DV, Holte A, Malt UF. Genuine clinical predictors of bipolar II disorder: an exploration of temporal and contextual characteristics. J Affect Disord. 2011;135(1-3):419-423. PubMed doi:10.1016/j.jad.2011.08.029
50. Vieta E, Suppes T. Bipolar II disorder: arguments for and against a distinct diagnostic entity. Bipolar Disord. 2008;10(1, pt 2):163-178. PubMed doi:10.1111/j.1399-5618.2007.00561.x
51. Kessler RC, Rubinow DR, Holmes C, et al. The epidemiology of DSM-III-R bipolar I disorder in a general population survey. Psychol Med. 1997;27(5):1079-1089. PubMed doi:10.1017/S0033291797005333
52. Luby JL, Mrakotsky C. Depressed preschoolers with bipolar family history: a group at high risk for later switching to mania? J Child Adolesc Psychopharmacol. 2003;13(2):187-197. PubMed doi:10.1089/104454603322163907
53. Schaffer A, Cairney J, Veldhuizen S, et al. A population-based analysis of distinguishers of bipolar disorder from major depressive disorder. J Affect Disord. 2010;125(1-3):103-110. PubMed doi:10.1016/j.jad.2010.02.118
54. Moreno C, Hasin DS, Arango C, et al. Depression in bipolar disorder versus major depressive disorder: results from the National Epidemiologic Survey on Alcohol and Related Conditions. Bipolar Disord. 2012;14(3):271-282. PubMed doi:10.1111/j.1399-5618.2012.01009.x
55. Martin A, Young C, Leckman JF, et al. Age effects on antidepressant-induced manic conversion. Arch Pediatr Adolesc Med. 2004;158(8):773-780. PubMed doi:10.1001/archpedi.158.8.773
56. Tijssen MJ, van Os J, Wittchen HU, et al. Evidence that bipolar disorder is the poor outcome fraction of a common developmental phenotype: an 8-year cohort study in young people. Psychol Med. 2010;40(2):289-299. PubMed doi:10.1017/S0033291709006138
57. Findling RL, Jo B, Frazier TW, et al. The 24-month course of manic symptoms in children. Bipolar Disord. 2013;15(6):669-679. PubMed doi:10.1111/bdi.12100