Objective: Age-appropriate criteria for posttraumatic stress disorder (PTSD) in young children have been established. The present study investigated the long-term course of such PTSD and its predictors in young children.
Methods: Young children (aged 2-10 years) and parents/caregivers who had attended emergency departments after motor vehicle collisions (MVCs) between May 2004 and November 2005 were assessed at 2 to 4 weeks and 6 months post-MVC; 71 families were re-interviewed 3 years post-MVC. Participants were assessed according to standard DSM-IV criteria for PTSD and a well-validated alternative algorithm for diagnosing PTSD in young children (PTSD-AA). Demographic, trauma-related, and parental mental health variables and intellectual ability were also assessed at baseline.
Results: Using an “optimal-report” procedure (a positive diagnosis according to parent or child for older children, or just parent for younger children), 7.0% met criteria for DSM-IV PTSD and 16.9% for PTSD-AA at 3 years. Using parent report alone, these rates were 1.4% and 2.8%, respectively. Parent-child agreement for PTSD and PTSD-AA was no better than chance (Cohen κ = -0.03 and -0.04, respectively). Baseline parent posttraumatic stress relating to the child’s trauma, and not trauma severity, was correlated with optimal-report child PTSD-AA at each assessment (r values = 0.29-0.31) and accounted for unique variance in logistic regression models of this outcome at each assessment.
Conclusions: PTSD-AA in young children can persist for years but is underrecognized by parents despite its being shaped to a large extent by parents’ own acute traumatic stress in response to the child’s trauma.
Posttraumatic Stress Disorder in
Young Children 3 Years Posttrauma:
Prevalence and Longitudinal Predictors
ABSTRACT
Objective: Age-appropriate criteria for posttraumatic stress disorder (PTSD) in young children have been established. The present study investigated the long-term course of such PTSD and its predictors in young children.
Methods: Young children (aged 2–10 years) and parents/caregivers who had attended emergency departments after motor vehicle collisions (MVCs) between May 2004 and November 2005 were assessed at 2 to 4 weeks and 6 months post-MVC; 71 families were re-interviewed 3 years post-MVC. Participants were assessed according to standard DSM-IV criteria for PTSD and a well-validated alternative algorithm for diagnosing PTSD in young children (PTSD-AA). Demographic, trauma-related, and parental mental health variables and intellectual ability were also assessed at baseline.
Results: Using an “optimal-report” procedure (a positive diagnosis according to parent or child for older children, or just parent for younger children), 7.0% met criteria for DSM-IV PTSD and 16.9% for PTSD-AA at 3 years. Using parent report alone, these rates were 1.4% and 2.8%, respectively. Parent-child agreement for PTSD and PTSD-AA was no better than chance (Cohen κ = –0.03 and –0.04, respectively). Baseline parent posttraumatic stress relating to the child’s trauma, and not trauma severity, was correlated with optimal-report child PTSD-AA at each assessment (r values = 0.29–0.31) and accounted for unique variance in logistic regression models of this outcome at each assessment.
Conclusions: PTSD-AA in young children can persist for years but is underrecognized by parents despite its being shaped to a large extent by parents’ own acute traumatic stress in response to the child’s trauma.
J Clin Psychiatry
dx.doi.org/10.4088/JCP.15m10002
© Copyright 2016 Physicians Postgraduate Press, Inc.
aDepartment of Clinical Psychology, University of East Anglia, Norwich, United Kingdom
bInstitute of Psychiatry, Psychology and Neuroscience, King’s College, London, United Kingdom
cEmergency Department, King’s College Hospital, London, United Kingdom
dMedical Research Council Cognition & Brain Sciences Unit and Cambridgeshire and Peterborough NHS Foundation Trust, Cambridge, United Kingdom
*Corresponding author: Richard Meiser-Stedman, PhD, Department of Clinical Psychology, University of
East Anglia, Norwich, NR4 7TJ, United Kingdom
([email protected]).
Posttraumatic stress disorder (PTSD) is a common debilitating disorder in youth.1 Until recently, the reactions of preschool and young children to trauma have received little attention.2 The past decade has witnessed far greater coverage of the reactions of young children to traumatic stressors,3 a step change facilitated by the proposal of age-appropriate criteria for diagnosing PTSD. These criteria make allowances for the developmental limitations when assessing symptoms in this age group and the need to rely on parental/caregiver reporting.4 Amending the number of avoidance symptoms required (from 3 to 1) and dropping the requirement that a peritraumatic affective response be observed yield a far greater proportion who meet the threshold for “caseness” in young children.5,6 Multiple studies have attested to the construct and predictive validity7,8 of this age-appropriate alternative algorithm for diagnosing PTSD in young children (hereafter PTSD-AA), and minor amendments to the original PTSD-AA criteria led to the introduction of a preschool PTSD diagnosis within the DSM-5.9 Neither PTSD-AA nor the DSM-5 preschool PTSD diagnosis requires a peritraumatic affective response, but both require 1 re-experiencing symptom, 1 avoidance symptom, and 2 hyperarousal symptoms, where clinically significant distress or impairment in relationships is present.
With the establishment of a reliable and valid diagnostic algorithm in younger children, it has been possible to turn to researching the prevalence, course, etiology, and treatment of PTSD in this age group. Previously, we examined the reactions of 2- to 10-year-old children exposed to MVCs and explored the course of DSM-IV–defined PTSD and PTSD-AA from the acute posttrauma phase (ie, the first 4 weeks) to a 6-month follow-up assessment.7 Although the subsequent preschool PTSD criteria within DSM-5 specify an age range up to 6 years, at the time of this initial study, it was important to examine the boundary conditions of the original PTSD-AA diagnosis up to the age of 10 years.4 The present study presents data from a 3-year follow-up of this cohort, allowing consideration of several pertinent questions relating to younger children’s responses to trauma.
First, the longer-term course of posttraumatic stress reactions in early childhood needs to be established. Adults report significant psychopathology related to traumatic experiences in early childhood10; however, many of these studies are based on retrospective accounts of multiple and repeated trauma exposure (eg, abuse) in childhood typically accompanied by other adversities (eg, neglect, parental mental illness). Long-term follow-up studies of single traumas have addressed older children and adolescents and have found that PTSD may persist for years in a substantial minority.11
Second, it is important to consider the validity of parental reports of their child’s dysfunction. Reliance on parent reporting introduces tremendous scope for bias in terms of under- and overreporting of symptomatology.
Third, early diagnostic markers for predicting a long-term, suboptimal response to traumatic stressors can be identified. Unique to this study is the ability to consider acute stress disorder (ASD), an early diagnostic marker found to have utility in adults and older youth.12,13
Finally, it is essential to identify early demographic, trauma severity, and familial predictors of PTSD/PTSD-AA. These data would inform the early clinical management of PTSD and theoretical models of dysfunction in this age group.3 A recent review2 suggested that there have been inconsistent results observed for the relationship between demographic variables (ie, age, sex) and PTSD in preschool and young children but more substantive evidence for trauma severity and parent mental health as risk factors for PTSD. Apart from a study14 that tracked preschoolers’ PTSD symptoms in response to a missile attack, most research has been cross-sectional and has commonly addressed children exposed to interpersonal or domestic violence.2
This study therefore addressed the following research questions:
1. What is the prevalence of PTSD/PTSD-AA in children 3 years after an MVC, and to what extent is this affected by age at the time of the trauma?
2. To what extent do children and their parents or caregivers (hereafter just “parents”) agree in their assessment of the child’s PTSD/PTSD-AA?
3. How well does ASD function as a predictor of PTSD/PTSD-AA at this 3-year follow-up?
4. Which (if any) demographic, trauma severity, parental mental health, and intellectual variables predict PTSD/PTSD-AA at each time point?
METHODS
Participants
Participants were from a previously reported prospective study7 of young children aged 2–10 years at the time of study entry who attended an emergency department in South London between May 2004 and November 2005 following an MVC. Exclusion criteria were the presence of moderate-to-severe intellectual disabilities or moderate-to-severe traumatic brain injury. Of 114 child-parent dyads recruited for the initial 2- to 4-week posttrauma assessment (T1), 109 (95.6%) completed a 6-month follow-up assessment (T2). At T2, permission was sought to recontact families for a potential 3-year posttrauma assessment (T3); all families gave consent to being recontacted.
Of the families who completed T1 and T2 assessments (n = 109), 33 (30.3%) could not be contacted again and 5 (4.6%) were no longer willing to participate. One parent did not complete the interviews at the T1 and T2 assessments, although their child did complete these interviews; only the child’s data were included in the analyses presented here. Parents of 71 children (62.2% of T1 sample, 65.1% of T2 sample) consented to the T3 interview. Interviews were conducted with the child’s mother (n = 64), father (n = 2), grandmother (n = 2), uncle (n = 2), or aunt (n = 1). In 53 cases, the children themselves (if 7 years or older) completed a structured interview for PTSD. The 18 children who did not complete the T3 interview assessment themselves were still under 7 years of age (n = 12), not allowed by their parents to do the interview (n = 3), unwilling to participate (n = 2), or withdrew during the interview (n = 1).
The final T3 sample (age at MVC, mean = 6.5 years, SD = 2.8; age at T3, mean = 10.3 years, SD = 2.9), were assessed on average 3.8 years (SD = 0.4) post-MVC. Thirty-four (47.9%) were female, and 42 (59.2%) belonged to a minority ethnic group. Twenty-seven (38.0%) were pedestrians, 36 (50.7%) car passengers, 4 (5.6%) cyclists (who collided with a motor vehicle), and 4 (5.6%) bus passengers. Twenty participants (28.2%) had no injuries, 46 (64.8%) had only soft tissue injuries, and 5 (7.0%) had sustained a fracture. Four participants (5.6%) had lost consciousness, and 11 (15.5%) were admitted to the hospital. There were no significant differences between participants at T3 and those who participated only at the T1 and T2 assessments with respect to age, sex, ethnicity, MVC type, triage category, degree of injury, loss of consciousness, or hospital admission (all P values > .18). Furthermore, there were no differences in T2 parent- or child-reported PTSD symptom counts between those families that completed the T3 assessment and those that did not (t106 = 0.36, P = .7 and t42 = 0.87, P = .4, respectively).
Measures
Demographic and trauma-related variables. These data were gathered from the hospital emergency department records or parent interviews at T1. The presence of pre-MVC emotional or behavioral disorders was established in an interview with parents (endorsed by parents as present or absent).
Child posttraumatic stress disorder. The study outcome measures were structured interviews of child PTSD/PTSD-AA completed by parents and children 7 years or older. In addition to reporting parent- and child-report data, “combined-report” diagnoses (ie, from both parent and child responses, where both were available) and “optimal-report” diagnoses (based on the maximal information available, ie, parent-only responses for children under age 7 or combined report for children 7 years or older) are presented. This is consistent with practice parameter recommendations that data from multiple informants be routinely obtained and their utility maximized.15 While the use of the optimal-report diagnosis increases the available sample size, the use of different assessment strategies in each age group may be viewed as methodologically problematic. To be transparent, the data for combined-report PTSD (ie, for children 7 years or older) are therefore also reported.
The PTSD Semi-Structured Interview and Observational Record for Infants and Young Children (IORYC)4,6 was used to assess parent-report PTSD/PTSD-AA at each assessment point. The IORYC can yield a DSM-IV PTSD as well as PTSD-AA diagnosis. The IORYC possesses good interrater reliability4,5 and construct validity.7
At T1 and T2, child-report PTSD/PTSD-AA were assessed (for those 7 years or older) using the Clinician Administered PTSD Scale–Child and Adolescent Version (CAPS-CA).16 The CAPS-CA is a child-report structured interview for assessing PTSD that possesses good psychometric properties.17 For children 7 years or older at T3, child-report PTSD/PTSD-AA were assessed using the PTSD Schedule of the Anxiety Disorder Interview Schedule for DSM-IV, Child and Parent Schedule (ADIS-C/P).18 The ADIS-C/P can be used to derive a PTSD-AA diagnosis (as PTSD-AA criteria are a subset of DSM-IV criteria). The ADIS-C/P was selected for use at T3 given its suitability for telephone administration.
Continuous measures of PTSD severity were derived by counting endorsed symptoms; these data are reported in supplementary analyses (see Supplementary eTables 1–6 at PSYCHIATRIST.COM).
Parental mental health. Parental posttraumatic stress symptomatology at T1 relating to the child’s MVC was indexed using the Posttraumatic Diagnostic Scale.19 Parental depressive symptomatology at T1 was assessed using the Depression subscale of the Hospital Anxiety and Depression Scale.20
Child intellectual performance. To investigate whether posttraumatic stress was related to intellectual functioning, the British Picture Vocabulary Scale, second edition, a standardized test of receptive vocabulary,21 was administered at T1.
Procedure
The T3 assessment was approved by Bexley and Greenwich Research Ethics Committee (08/H0809/18). To facilitate participation in the T3 assessment, telephone interviewing was used.
RESULTS
Prevalence of PTSD at 3-Year Follow-Up (T3)
The prevalence of PTSD-AA and PTSD diagnoses at T3, differentiated by age group at MVC and informant, is displayed in Table 1. Parent-report diagnoses were reported in only 1 or 2 cases. Child- and combined-report or optimal-report diagnoses were much more frequently endorsed (ranging from 7.0%–20.8%).
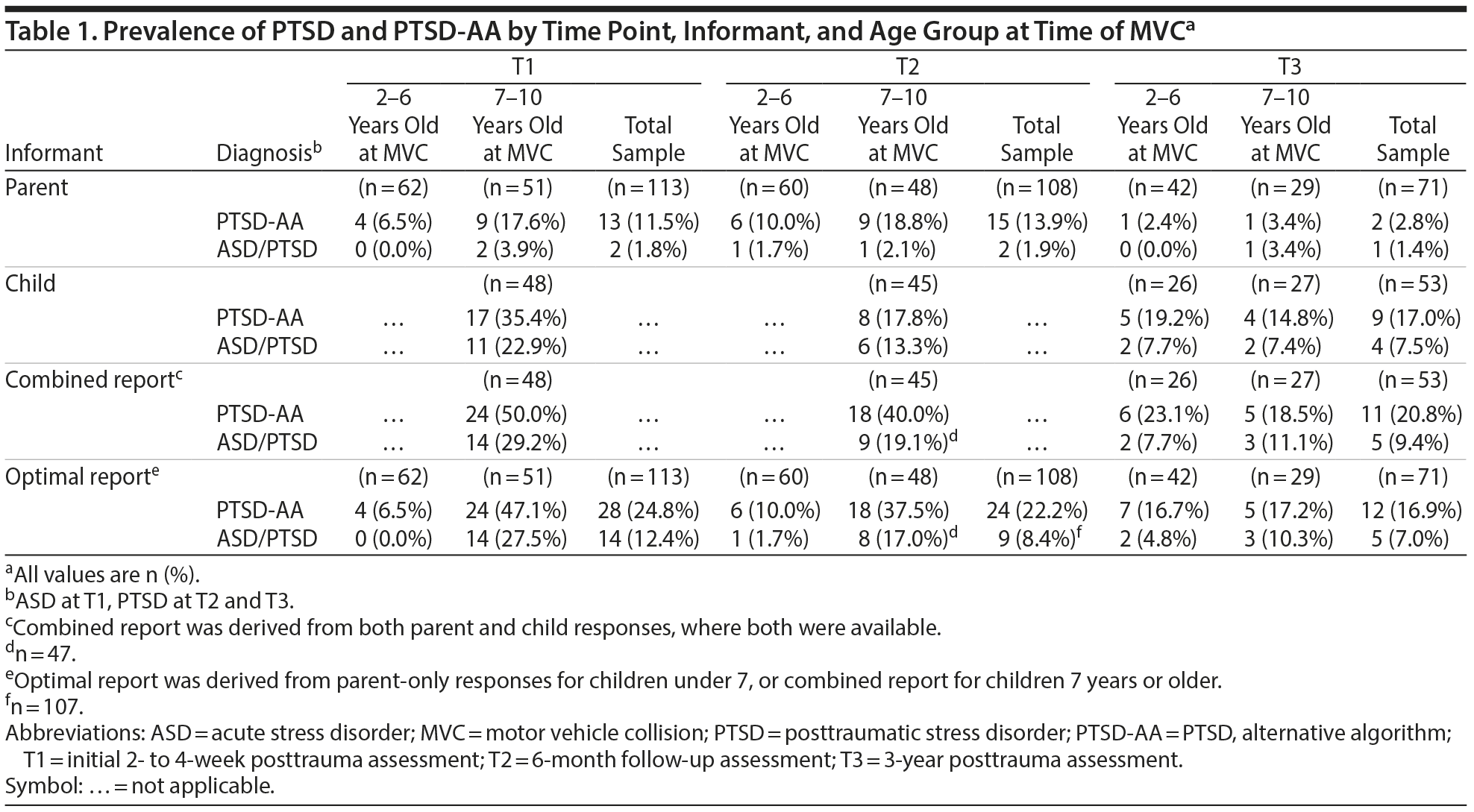
In the case of child- and combined-report diagnoses (Table 1), these rates were reduced relative to T1 and T2. The proportion of cases at T3 meeting criteria for PTSD-AA or PTSD based on an optimal-report procedure also show improvement relative to earlier assessments (not previously reported; PTSD-AA prevalence was 28/113 [24.8%] at T1 and 24/108 [22.2%] at T2; ASD prevalence was 14/113 [12.4%] cases at T1 and PTSD prevalence was 9/107 [8.4%] cases at T2). PTSD-AA, regardless of informant, was observed at a rate more than twice as great as that observed for standard PTSD criteria, as found previously.7
To investigate whether being a preschool-aged child at the MVC influenced the risk of developing PTSD/PTSD-AA at T3, age-related comparisons were made. No age-group–related differences were observed, ie, children not old enough to self-report PTSD symptoms at T1/T2 (ie, 2–6 years old) were as likely to meet criteria for PTSD/PTSD-AA (regardless of informant) at T3 as those children who had provided self-report at T1/T2 (ie, 7–10 years old; Fisher exact test, P values > .3); moreover, there were no differences in mean child-reported symptoms at T3 between children aged 2–6 years and children aged 7–10 years at T1 (t51 = 0.17, NS).
Since PTSD-AA can be diagnosed on the basis of fewer symptoms than PTSD, the increased prevalence of PTSD-AA may not be related to its developmental appropriateness but to its reduced symptom requirement. We therefore examined the mean number of symptoms for positive cases of each diagnosis at T3. There were no significant differences in symptom counts (although PTSD symptom counts were numerically higher) for diagnoses based on child report, combined parent-child report, or optimal report (all t values < 1.92, NS); parent-report comparison was not possible as only 1 child met criteria for parent-report PTSD. Moreover, with respect to child-report impairment severity, there were no differences between child-report PTSD and PTSD-AA cases (t = 0.3, P > .6), or between optimal- or combined-report PTSD and PTSD-AA (optimal and combined report, t = 0.3, P > .6).
Parent-Child Agreement at T3
Parent-child agreement (Cohen κ) for the 53 children where data from both informants were available for PTSD was –0.03 and for PTSD-AA was –0.04—no better than chance. These figures did not differ even when restricting the calculations to older children who had been able to provide self-report at earlier assessments (–0.06 and –0.05, respectively; n = 27).
The Utility of Baseline (T1) PTSD Diagnoses
in Predicting PTSD at 3-Year Follow-Up (T3)
The sensitivity, specificity, positive predictive value (proportion diagnosed at T1 who retained the diagnosis at T3), and negative predictive value (proportion with no diagnosis at T1 who remained diagnosis-free at T3) for each diagnosis and informant are reported in Table 2. The strong relationship between parent-reported T1 ASD and T3 PTSD is most likely a statistical artifact caused by the low numbers of positive cases for parent report. The ability of T1 diagnoses to predict PTSD or PTSD-AA at 3 years (T3) was weak. For diagnoses that involved child report (child-alone, combined report, or optimal report), prediction statistics for T3 PTSD-AA were generally superior to those for T3 PTSD, notably when considering sensitivity and positive predictive values. The addition of parent report within combined-report diagnosis did not improve predictive ability above that of child report alone; indeed, specificity statistics for T3 PTSD-AA appeared to be weakened. Parent-report diagnoses (T1 ASD or PTSD-AA) were very insensitive predictors of corresponding child-report diagnoses at T3.
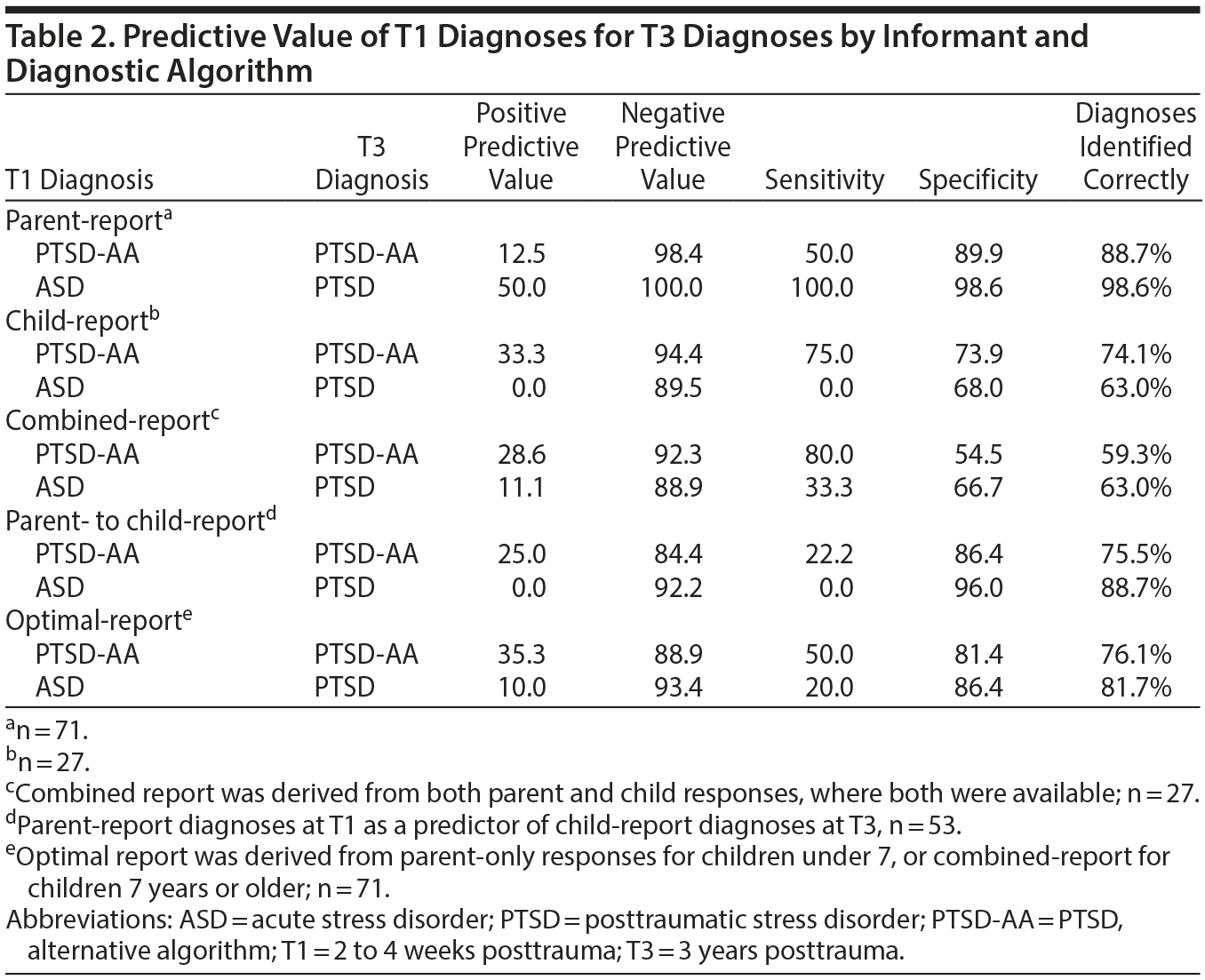
Of 11 cases who met criteria for combined-report PTSD-AA diagnosis at T3, only 4 had PTSD-AA at T1 based on parent report; likewise, for the 12 cases meeting criteria for PTSD-AA at T3 based on optimal report, only 4 had PTSD-AA at T1 based on parent report.
Correlates and Predictors of
Optimal-Report PTSD-AA at Each Assessment
As the optimal-report PTSD-AA diagnosis is most closely aligned with best diagnostic practice of utilizing multiple informants,15 this diagnosis was the dependent variable for correlational analyses (see Table 3) and regression modeling addressing possible risk factors for posttraumatic stress symptomatology (PTSS). Logistic regression was used to explore which variables accounted for unique variance in optimal-report PTSD-AA. Only significant zero-order correlates were included in these models; a forward conditional method of entry was used. For optimal-report PTSD-AA at T1, age, sex, persistent injury, and concurrent parental PTSS scores accounted for unique variance (χ24 = 41.25, P < .0001; Nagelkerke R2 = 0.53). Ethnicity, parental presence during the collision, and parental depression at T1 were not retained in the model. For optimal-report diagnoses at the 6-month assessment (T2), T1 persistent injury and T1 parental PTSS were retained in the model (χ22 = 21.91, P < .0001; Nagelkerke R2 = 0.41), but not age, ethnicity, intellectual performance, triage, fracture, admission, or post-MVC separation greater than 1 hour. For optimal-report diagnoses at the 3-year assessment (T3), T1 parental PTSS was retained in the model (χ21 = 6.30, P < .012; Nagelkerke R2 = 0.16), but not post-MVC separation greater than 1 hour or parental depression. Parental PTSS at baseline was therefore the only variable to account for unique variance at each assessment point.
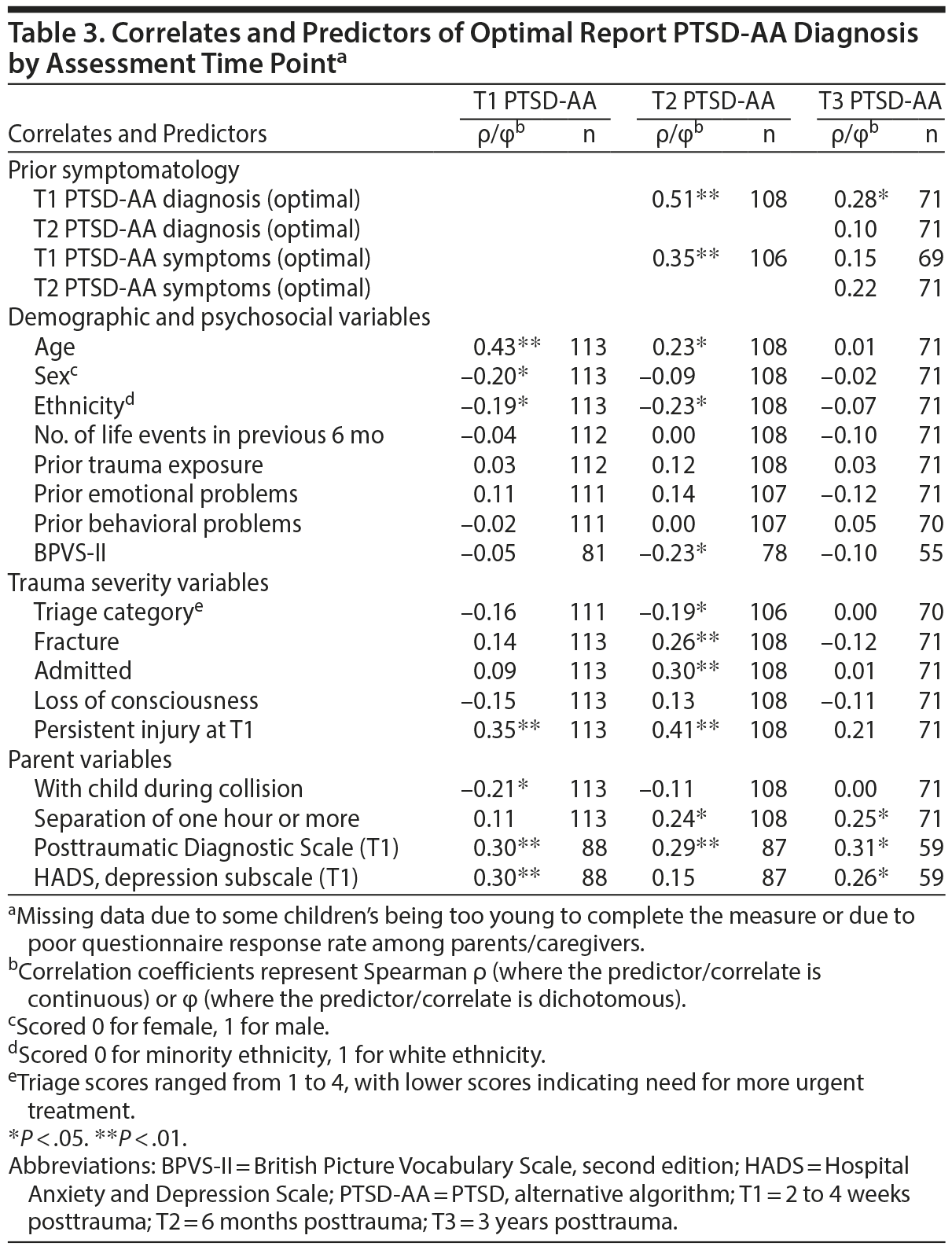
When initial optimal-report diagnosis at T1 was also entered in the first step of the model for T2, only persistent injury was retained in the model, with optimal-report diagnosis at T1 also accounting for unique variance (χ23 = 26.11, P < .0001; Nagelkerke R2 = 0.47). When initial optimal-report diagnosis at T1 was also entered in the first step of the model for T3, only T1 parental PTSS was retained in the model, with T1 optimal-report diagnosis not accounting for significant unique variance (χ23 = 12.29, P < .007; Nagelkerke R2 = 0.30).
To allow closer investigation of predictive data, parent-report, child-report, and optimal-report correlational data for symptom counts and the corresponding regression models are presented in supplementary data (Supplementary eTables 1–6); these are broadly consistent with findings presented here.
DISCUSSION
This study addressed the assessment, prevalence, course, and risk factors for DSM-IV PTSD and PTSD-AA in young children exposed to an MVC 3 years earlier. With respect to our first question (ie, the prevalence of PTSD at 3 years post-MVC), child- and combined-report data suggested that a significant minority continues to present with clinically significant PTSS, even at this long-term follow-up assessment. Reliance on parent report alone, however, yielded very few cases, regardless of diagnostic algorithm. The use of PTSD-AA at T3 doubled the prevalence of disorder (whether based on child report, combined report, or optimal report) relative to PTSD at T3, consistent with data from T1 and T2 assessments.7 The discrepancy between parent and child report was further borne out when addressing our second question (ie, the extent that children and their parents agree in their assessment), where parent-child agreement at T3 was no better than chance at the level of diagnosis.
With respect to our third question (ie, the ability of T1 diagnoses to predict T3 diagnoses), T1 PTSD-AA was more powerful at predicting the same diagnosis at T3 than T1 ASD at predicting PTSD at T3. Nevertheless, there seemed to be considerable natural recovery for PTSD-AA, as well as instances where children had PTSD at T3 (according to either diagnostic algorithm) but were not recognized as such during the T1 assessment. Parent report was either a weak predictor of diagnosis at T3 follow-up or did not add to child report alone.
In addressing our fourth question (ie, risk factors for PTSD), parents’ own PTSS at study entry (T1) accounted for unique variance in optimal-report PTSD-AA at each assessment. Persistent injury at T1 accounted for unique variance in models of PTSD-AA at T1 and T2 (consistent with other studies2 showing a link between trauma severity and PTSD) but not at T3, while female sex and age were only risk factors (ie, accounted for unique variance) for PTSD-AA at T1. Intelligence was mostly not significantly related to PTSD.
These findings emphasize the importance of considering young children’s long-term responses to traumatic stressors. As with earlier findings6,14 young children may develop clinically significant PTSS that persists for years and that in many instances may not be recognized by their parents. The number of participants reporting PTSD-AA 3 years later that had not been recognized by parents at an earlier assessment suggests that, even with the accommodations made for diagnosing PTSD in this age group, the reliance on parent report may be inadequate for identifying PTSD in some young children. Preschoolers were as likely as elementary-school–aged children to meet criteria for PTSD at T3. These findings also emphasize the importance of using a developmentally appropriate tool for diagnosing PTSD in children (eg, DSM-5 preschool child PTSD); the use of the PTSD-AA diagnosis more than doubled the number of cases identified by the DSM-IV PTSD diagnosis alone.
The present study adds to earlier work in this area by relating chronic reactions to acute responses, in terms of both children’s own acute reactions and their parent’s reactions. With respect to the early identification of children at risk of a chronic reaction to a traumatic stressor, diagnostic tools (particularly child-report PTSD-AA) have some predictive ability. However, the utility of such constructs should not be overstated; there is considerable natural recovery over time, as well as some cases who met diagnostic threshold at a 3-year follow-up (T3) but who did not do so at previous assessments.
The current study strengthens the case for considering parental mental health in the aftermath of trauma, with parental acute PTSS at study entry consistently predicting their child’s PTSS, even 3 years posttrauma; strikingly, this was despite parents being very unlikely to acknowledge clinically significant PTSS in their child at this assessment. The direction of this effect is unclear. Parents’ own initial T1 PTSS could have been worsened by their children’s T1 symptoms, children’s responses across time points could have been shaped by their parents’ initial reactions (eg, modeling avoidance), or a bidirectional effect may have resulted in a mutual amplification of symptomatology.22
The importance of familial factors in driving PTSD in this group was further underscored by the significant relationship between separation from parent during the trauma and PTSD in the first weeks following the trauma. The role of families in the development of chronic responses to traumatic stressors in young children still warrants further research, but these data speak to the need to consider trauma-exposed parent-child dyads from the outset, rather than young children in isolation. Providing support for parents in the aftermath of trauma (eg, with psychoeducation about their own, as well as their child’s, posttraumatic stress) is therefore indicated. With respect to other risk factors, the relationship between trauma severity indices and PTSD-AA was mainly limited to the 6-month follow-up, but is supportive of a dose-response relationship for trauma exposure and PTSD risk in young children.
The study has several limitations. In particular, it suffers from a relatively small sample size. Given the number of analyses undertaken (even if many were only exploratory), the chance that a type I error could occur was increased. Moreover, the power of the regression models was modest; larger samples may have revealed more predictor variables.
In conclusion, this study suggests that a significant minority of young children exposed to single-event trauma may develop PTSD/PTSD-AA that persists for years. While parents’ own PTSS in the acute phase may contribute to persistent PTSD in young children, the present study also suggests that parents may fail to observe persistent PTSD in their children when the trauma occurs in early childhood.
Submitted: March 30, 2015; accepted March 3, 2016.
Online first: November 8, 2016.
Potential conflicts of interest: Drs Meiser-Stedman, Smith, Yule, Glucksman, and Dalgleish have no interests to disclose.
Funding/support: The initial phase of data collection was funded through a Peggy Pollak Research Fellowship in Developmental Psychiatry awarded to Dr Meiser-Stedman by the Psychiatry Research Trust and a grant from the Steel Charitable Trust. T3 data collection was supported by a United Kingdom National Health Service–funded training scheme placement in clinical psychology. Dr Meiser-Stedman was supported while writing this manuscript by a United Kingdom Medical Research Council Clinician Scientist Fellowship (G0802821) held at the Medical Research Council Cognition & Brain Sciences Unit in Cambridge.
Role of the sponsor: The study funders and sponsors had no role in the design, conduct, or decision to publish this study.
Supplementary material: Available at PSYCHIATRIST.COM.
REFERENCES
1. Alisic E, Zalta AK, van Wesel F, et al. Rates of post-traumatic stress disorder in trauma-exposed children and adolescents: meta-analysis. Br J Psychiatry. 2014;204(5):335–340. PubMed doi:10.1192/bjp.bp.113.131227
2. De Young AC, Kenardy JA, Cobham VE. Trauma in early childhood: a neglected population. Clin Child Fam Psychol Rev. 2011;14(3):231–250. PubMed doi:10.1007/s10567-011-0094-3
3. Stoddard FJ Jr. Outcomes of traumatic exposure. Child Adolesc Psychiatr Clin N Am. 2014;23(2):243–256. PubMed doi:10.1016/j.chc.2014.01.004
4. Scheeringa MS, Wright MJ, Hunt JP, et al. Factors affecting the diagnosis and prediction of PTSD symptomatology in children and adolescents. Am J Psychiatry. 2006;163(4):644–651. PubMed doi:10.1176/ajp.2006.163.4.644
5. Scheeringa MS, Peebles CD, Cook CA, et al. Toward establishing procedural, criterion, and discriminant validity for PTSD in early childhood. J Am Acad Child Adolesc Psychiatry. 2001;40(1):52–60. PubMed doi:10.1097/00004583-200101000-00016
6. Scheeringa MS, Zeanah CH, Myers L, et al. Predictive validity in a prospective follow-up of PTSD in preschool children. J Am Acad Child Adolesc Psychiatry. 2005;44(9):899–906. PubMed doi:10.1097/01.chi.0000169013.81536.71
7. Meiser-Stedman R, Smith P, Glucksman E, et al. The posttraumatic stress disorder diagnosis in preschool- and elementary school-age children exposed to motor vehicle accidents. Am J Psychiatry. 2008;165(10):1326–1337. PubMed doi:10.1176/appi.ajp.2008.07081282
8. De Young AC, Hendrikz J, Kenardy JA, et al. Prospective evaluation of parent distress following pediatric burns and identification of risk factors for young child and parent posttraumatic stress disorder. J Child Adolesc Psychopharmacol. 2014;24(1):9–17. PubMed doi:10.1089/cap.2013.0066
9. American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
10. Edwards VJ, Holden GW, Felitti VJ, et al. Relationship between multiple forms of childhood maltreatment and adult mental health in community respondents: results from the adverse childhood experiences study. Am J Psychiatry. 2003;160(8):1453–1460. PubMed doi:10.1176/appi.ajp.160.8.1453
11. Yule W, Bolton D, Udwin O, et al. The long-term psychological effects of a disaster experienced in adolescence, I: the incidence and course of PTSD. J Child Psychol Psychiatry. 2000;41(4):503–511. PubMed doi:10.1111/1469-7610.00635
12. Kassam-Adams N, Winston FK. Predicting child PTSD: the relationship between acute stress disorder and PTSD in injured children. J Am Acad Child Adolesc Psychiatry. 2004;43(4):403–411. PubMed doi:10.1097/00004583-200404000-00006
13. Meiser-Stedman R, Yule W, Smith P, et al. Acute stress disorder and posttraumatic stress disorder in children and adolescents involved in assaults or motor vehicle accidents. Am J Psychiatry. 2005;162(7):1381–1383. PubMed doi:10.1176/appi.ajp.162.7.1381
14. Laor N, Wolmer L, Cohen DJ. Mothers’ functioning and children’s symptoms 5 years after a SCUD missile attack. Am J Psychiatry. 2001;158(7):1020–1026. PubMed doi:10.1176/appi.ajp.158.7.1020
15. Hudziak JJ, Achenbach TM, Althoff RR, et al. A dimensional approach to developmental psychopathology. Int J Methods Psychiatr Res. 2007;16(suppl 1):S16–S23. PubMed doi:10.1002/mpr.217
16. Nader K, Kriegler JA, Blake DD, et al. Clinician Administered PTSD Scale, Child and Adolescent Version. White River Junction, VT: National Center for PTSD; 1996.
17. Carrion VG, Weems CF, Ray R, et al. Toward an empirical definition of pediatric PTSD: the phenomenology of PTSD symptoms in youth. J Am Acad Child Adolesc Psychiatry. 2002;41(2):166–173. PubMed doi:10.1097/00004583-200202000-00010
18. Silverman WK, Albano AM. Anxiety Disorder Interview Schedule for DSM-IV: Child and Parent Interview Schedule. San Antonio, TX: The Psychological Corporation; 1996.
19. Foa EB, Cashman L, Jaycox L, et al. The validation of a self-report measure of posttraumatic stress disorder: the Posttraumatic Diagnostic Scale. Psychol Assess. 1997;9(4):445–451. doi:10.1037/1040-3590.9.4.445
20. Zigmond AS, Snaith RP. The Hospital Anxiety and Depression Scale. Acta Psychiatr Scand. 1983;67(6):361–370. PubMed doi:10.1111/j.1600-0447.1983.tb09716.x
21. Dunn LM, Dunn LM, Whetton C, et al. The British Picture Vocabulary Scale, Second Edition. Windsor, UK: NFER-Nelson; 1997.
22. Smith P, Perrin S, Yule W, et al. War exposure and maternal reactions in the psychological adjustment of children from Bosnia-Hercegovina. J Child Psychol Psychiatry. 2001;42(3):395–404. PubMed doi:10.1111/1469-7610.00732
This PDF is free for all visitors!


