Objective: To estimate the risks for psychopathology and functional impairments in adulthood among a longitudinal sample of youth with and without attention-deficit/hyperactivity disorder (ADHD) diagnosed in childhood.
Method: This was a case-controlled, 16-year (15-19 years) prospective follow-up study of ADHD. 140 boys with and 120 without DSM-III-R ADHD were recruited from pediatric and psychiatric settings. The main outcome measures were structured diagnostic interviews and measures of psychosocial, educational, and neuropsychological functioning. Data were collected from 1988 to 2006.
Results: At the 16-year follow-up, subjects with ADHD continued to significantly differ from controls in lifetime rates of antisocial, mood, anxiety, and addictive disorders, but with the exception of a higher interval prevalence of anxiety disorders (20% vs 8%; z = 2.32, P = .02) and smoking dependence (27% vs 11%; z = 2.30, P = .02), the incidence of individual disorders in the 6-year interval between the current and prior follow-up did not differ significantly from controls. At follow-up, the ADHD subjects compared with controls were significantly (P < .05) more impaired in psychosocial, educational, and neuropsychological functioning, differences that could not be accounted for by other active psychopathology.
Conclusions: These long-term prospective findings provide further evidence for the high morbidity associated with ADHD across the life cycle, stressing the importance of early recognition of this disorder for prevention and early intervention strategies. These findings also indicate that, in adulthood, ADHD confers significant risks for impairment that cannot be accounted for by other psychopathology.
J Clin Psychiatry 2012;73(7):941-950
© Copyright 2012 Physicians Postgraduate Press, Inc.
Submitted: November 10, 2011; accepted January 25, 2012(doi:10.4088/JCP.11m07529).
Corresponding author: Joseph Biederman, MD, Massachusetts General Hospital, 55 Fruit St, Yawkey 6A, Boston, MA 02114 ([email protected]).
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
ABSTRACT
Objective: To estimate the risks for psychopathology and functional impairments in adulthood among a longitudinal sample of youth with and without attention-deficit/hyperactivity disorder (ADHD) diagnosed in childhood.
Method: This was a case-controlled, 16-year (15-19 years) prospective follow-up study of ADHD. 140 boys with and 120 without DSM-III-R ADHD were recruited from pediatric and psychiatric settings. The main outcome measures were structured diagnostic interviews and measures of psychosocial, educational, and neuropsychological functioning. Data were collected from 1988 to 2006.
Results: At the 16-year follow-up, subjects with ADHD continued to significantly differ from controls in lifetime rates of antisocial, mood, anxiety, and addictive disorders, but with the exception of a higher interval prevalence of anxiety disorders (20% vs 8%; z = 2.32, P = .02) and smoking dependence (27% vs 11%; z = 2.30, P = .02), the incidence of individual disorders in the 6-year interval between the current and prior follow-up did not differ significantly from controls. At follow-up, the ADHD subjects compared with controls were significantly (P < .05) more impaired in psychosocial, educational, and neuropsychological functioning, differences that could not be accounted for by other active psychopathology.
Conclusions: These long-term prospective findings provide further evidence for the high morbidity associated with ADHD across the life cycle, stressing the importance of early recognition of this disorder for prevention and early intervention strategies. These findings also indicate that, in adulthood, ADHD confers significant risks for impairment that cannot be accounted for by other psychopathology.
J Clin Psychiatry 2012;73(7):941-950
© Copyright 2012 Physicians Postgraduate Press, Inc.
Submitted: November 10, 2011; accepted January 25, 2012 (doi:10.4088/JCP.11m07529).
Corresponding author: Joseph Biederman, MD, Massachusetts General Hospital, 55 Fruit St, Yawkey 6A, Boston, MA 02114 ([email protected]).
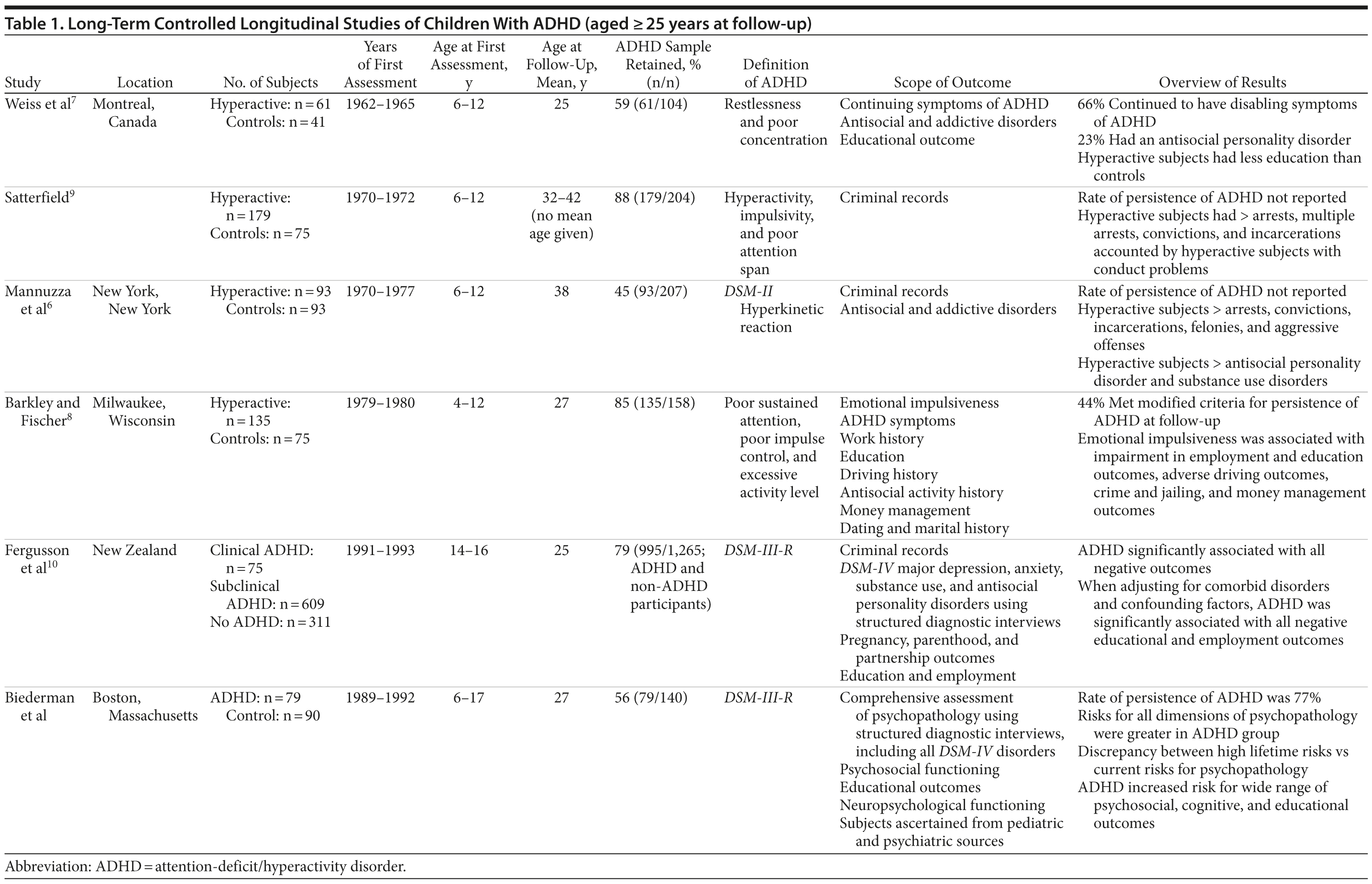
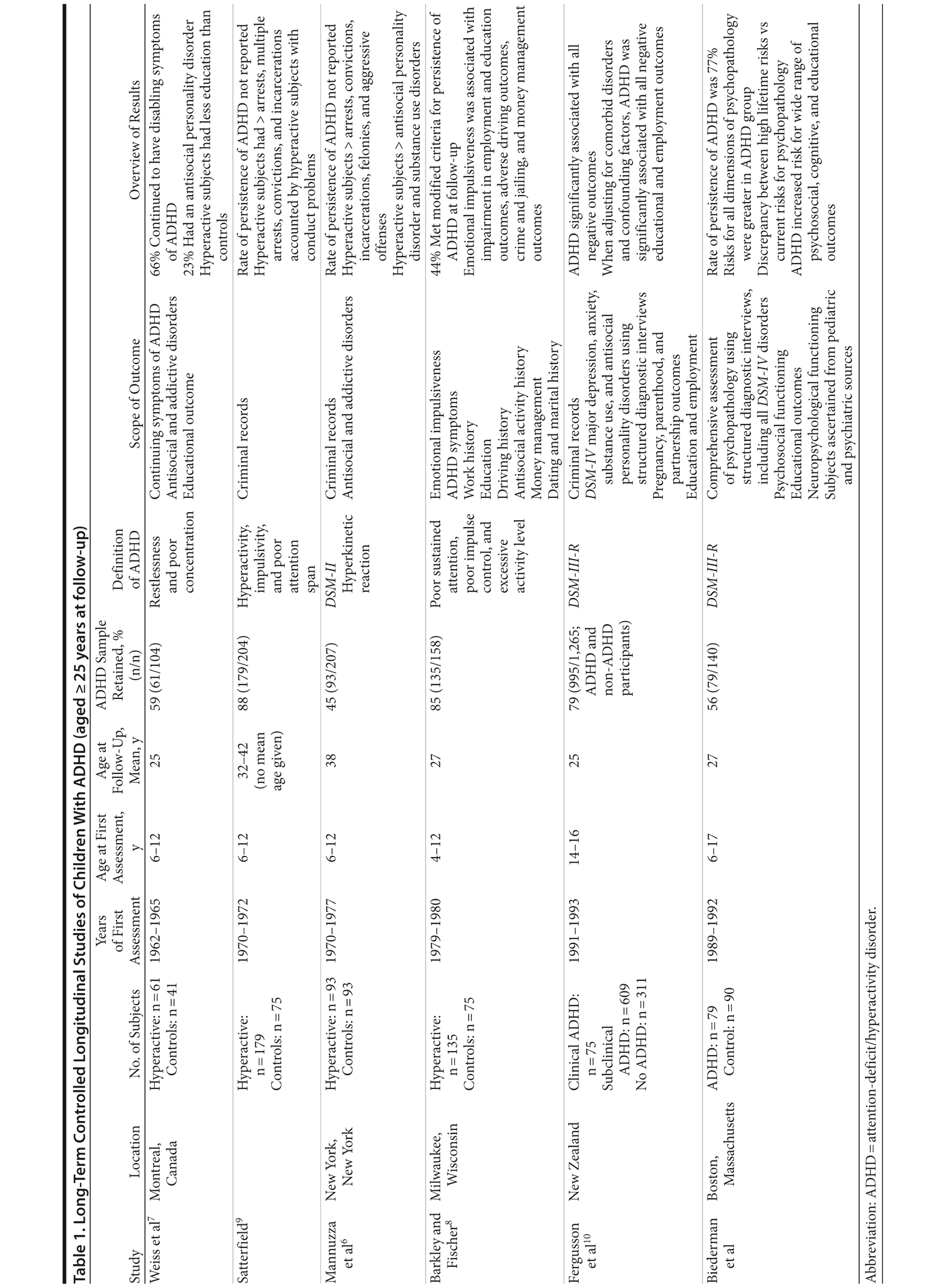
Among follow-up studies of children with attention-deficit/hyperactivity disorder (ADHD),1-5 very few have assessed adult outcomes (Table 1). Moreover, the overwhelming majority of long-term follow-up studies of adults who had ADHD as children (eg, mean age > 25 years) ascertained samples of children with “hyperactivity” and had a limited focus on antisocial and addictive disorders in adulthood (Table 1).6-9 Fergusson et al10 conducted the only adult outcome of adolescents diagnosed with DSM-III ADHD criteria (Table 1). However, because most prior long-term follow-up studies were not long enough, more work is needed to better connect the prospective pediatric literature with that of retrospective adult ADHD.
This issue is particularly relevant in the context of associated psychiatric disorders. Studies of adult ADHD clearly document that ADHD is associated with high levels of functional impairment.11-15 However, because adult ADHD is also associated with high rates of other psychiatric disorders,16-18 questions remain as to whether the morbidity and dysfunction associated with ADHD are due to ADHD itself or its associated psychiatric disorders.
The retrospective and cross-sectional findings in the literature on adult ADHD document a large discrepancy between the high lifetime and the low current rates of others psychiatric disorders,19 along with high levels of current impairment in multiple domains. This pattern of findings suggests that the functional impairments of ADHD adults are not due to associated disorders but to ADHD itself. However, the discrepancy between lifetime and current disorders observable in prospective samples has not been adequately investigated. Prior longitudinal studies have also not disentangled the contributions of ADHD and other active psychopathology to functional impairments in adulthood. Clarifying these issues will lead to an improved understanding of the adult outcome of ADHD youth, which has important implications in forecasting prognosis, as clinicians need to know when the clinical picture of a pediatric disorder indicates a compromised course over time.
The main purpose of this long-term, 16-year follow-up study was to estimate the burden of psychopathology and dysfunction associated with ADHD into adulthood and to investigate whether the morbidity of ADHD is due to ADHD or its associated psychiatric disorders. We tested the hypothesis that participants who had ADHD in childhood would manifest greater impairment and dysfunction in adulthood when compared with non-ADHD controls of the same age and sex. We further hypothesized that patterns of impairments in adults who had ADHD as children would be independent of other psychiatric disorders. To the best of our knowledge, this is one of the most comprehensive and longest follow-up studies of children with ADHD reaching adult years.
- Results from this long-term follow-up study from childhood into adult life emphasize the long-term disability associated with attention-deficit/hyperactivity disorder (ADHD) in adult life, encouraging efforts at early identification and treatment of children with ADHD to help mitigate such adverse outcomes.
- This study’s findings also emphasize the high level of persistence of neuropsychological deficits despite decline in core symptoms of ADHD.
METHOD
Subjects
Detailed study methodology was previously reported.19 Briefly, subjects were derived from a longitudinal case-control family study of white boys 6-17 years old with (n = 140) and without (n = 120) DSM-III-R ADHD ascertained from pediatric and psychiatric clinics. Excluded were adopted subjects or subjects with psychosis, autism, inadequate command of the English language, or a full-scale IQ < 80. The present study reports on a mean follow-up of 16 years (range, 15-19), in which 79 boys with ADHD and 90 controls from the original sample completed a full follow-up assessment (21-36 years, mean ± SD = 27.4 ± 3.7). All subjects provided written informed consent. The institutional review board approved this study. Data were collected from 1988 to 2006.
Follow-Up Assessment Procedures
We used the Structured Clinical Interview for DSM-IV (SCID)20 supplemented with modules from the DSM-IV-modified K-Kiddie Schedule for Affective Disorders and Schizophrenia-Epidemiologic Version (K-SADS-E)21 to assess childhood diagnoses. We interviewed all subjects and their mothers about their offspring. Subjects were asked about symptoms that were present in the past 5 years since the last follow-up, which we termed interval diagnosis. Of the 169 subjects with a full diagnostic interview, the proportion that provided direct only, mother only, and both types of reports were 58%, 6%, and 36%, respectively (16%, 6%, and 78%, respectively, for the ADHD module). We combined data from direct and indirect interviews by considering a diagnostic criterion positive if it was endorsed in either interview.
Interviewers were blind to baseline ascertainment group, ascertainment site and prior assessments. They had undergraduate degrees in psychology and were extensively trained. κ Coefficients of agreement between interviewers and board-certified child and adult psychiatrists and experienced licensed clinical psychologists were previously reported19 (median κ for individual disorders = 0.98). A committee of board-certified child and adult psychiatrists and child psychologists blindly reviewed all assessments and resolved diagnostic uncertainties. κ Coefficients between individual clinicians and the review committee were previously reported19 (median κ of individual disorders = 0.87).
Two measures of persistent ADHD were defined as meeting full or subthreshold criteria for DSM-IV ADHD during the interval between the 10-year and 16-year assessments. A subthreshold ADHD case was defined as endorsing more than half but less than full diagnostic criteria (ie, at least 4 ADHD symptoms).
To measure overall functioning, we used the DSM-IV Global Assessment of Functioning (GAF).22 Socioeconomic status was measured using the 5-point Hollingshead scale23 (higher score = lower socioeconomic status) composed of educational level (scored 1-7, higher score = higher level) and occupational level (scored 1-9, higher score = higher level). Socioeconomic status was defined by the educational and occupational levels of the person(s) financially responsible for the household that the subject was currently living in. At follow-up, socioeconomic status was the personal socioeconomic status of the subject if the subject was financially independent. Information was also collected on treatment history, family functioning with the Moos Family Environment Scale,24 and the Behavior Rating Inventory of Executive Function-Adult Version (BRIEF-A).25
Subjects were administered 2 subtests from the Wechsler Abbreviated Scale of Intelligence (WASI) to estimate IQ,26 all subtests from the Working Memory Index (digit span, letter number, arithmetic), and the Processing Speed Index (digit symbol/coding, symbol search) from the Wechsler Adult Intelligence Scale III (WAIS-III)27 (individual scores as well as index scores were included in analysis). To assess executive functions, we used 3 subtests from the Delis Kaplan Executive Function System (O-KEFS)28: the tower subtest, color-word interference subtest, and trail making test. The Test of Word Reading Efficiency (TOWRE)29 and the Wide Range Achievement Test-III (WRAT-III)30 measured academic achievement.
Statistical Analysis
Analyses of demographic factors relied on Pearson χ2 tests, t tests, and Wilcoxon rank sum tests for binary, continuous, and ordinal variables, respectively. We examined psychopathology throughout the lifespan (lifetime diagnoses) and psychopathology since the 10-year follow-up (interval diagnoses). A lifetime history of a disorder was defined as a positive response at any assessment (baseline, 1-year, 4-year, 10-year, or 16-year follow-up) versus a negative response at all assessments. We used logistic regression to compare ADHD and control subjects on lifetime and interval diagnoses. Functional outcomes and neuropsychological test scores at the 16-year follow-up were analyzed by using logistic or linear regression, depending on the distribution of the outcome variable, and controlled for any demographic confounders. All tests were 2-tailed, with α set at .05.
RESULTS
Attrition and Demographic Characteristics
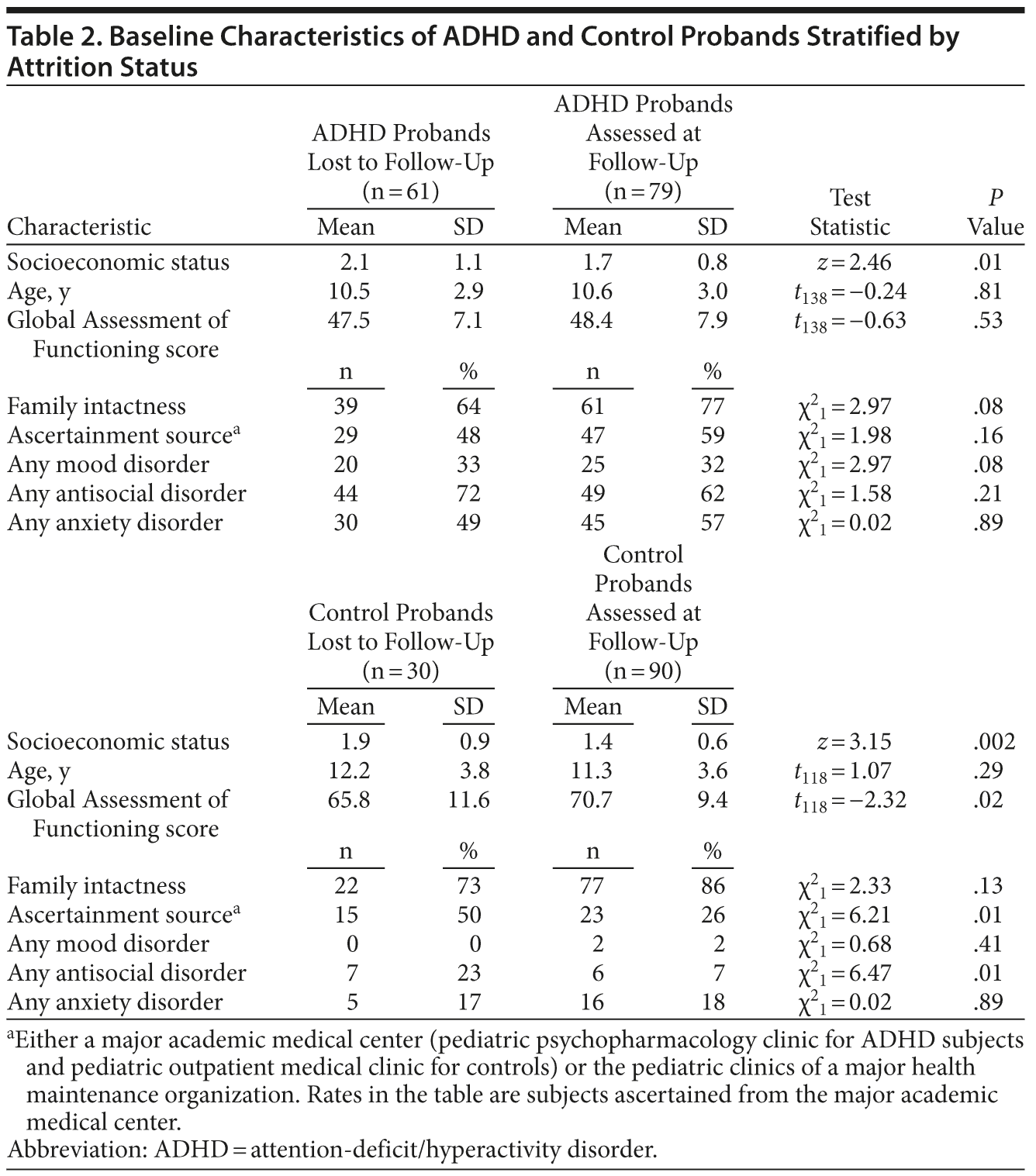
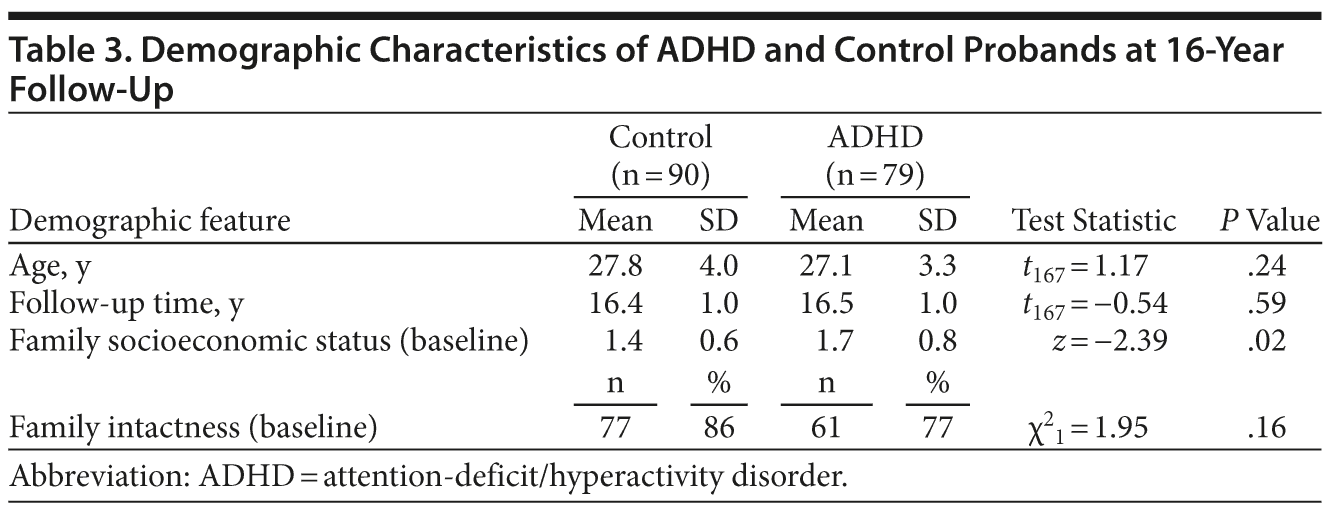
Of the 140 boys with ADHD and 120 controls recruited at baseline, 79 (56%) and 90 (75%), respectively, were reassessed at the 16-year follow-up. The control group had a significantly higher rate of successful reassessment (χ21 = 9.80, P = .002). Subjects successfully followed up had a higher baseline socioeconomic status than those lost to follow-up, and controls at follow-up had higher baseline GAF scores and a lower rate of baseline antisocial disorders than those lost to follow-up (Table 2). Men who had ADHD as boys had lower baseline family of origin socioeconomic status than controls (Table 3). Therefore, baseline socioeconomic status was controlled for in all statistical tests.
Of men who had ADHD as boys, 99% had received some form of treatment for ADHD during their lives (3% [n = 2] counseling alone, 8% [n = 6] medication alone, and 89% [n = 70] both counseling and medication). At the 16-year follow-up assessment, 23% of ADHD boys were receiving some form of treatment for the disorder in the past month (6% [n = 5] medication alone and 16% [n = 13] both counseling and medication). The rate of full or subthreshold DSM-IV ADHD between 10- to 16-year assessments was 77% (61/79), and that of current (past month) was 61% (47/77, two missing).
Risk for Psychiatric Disorders
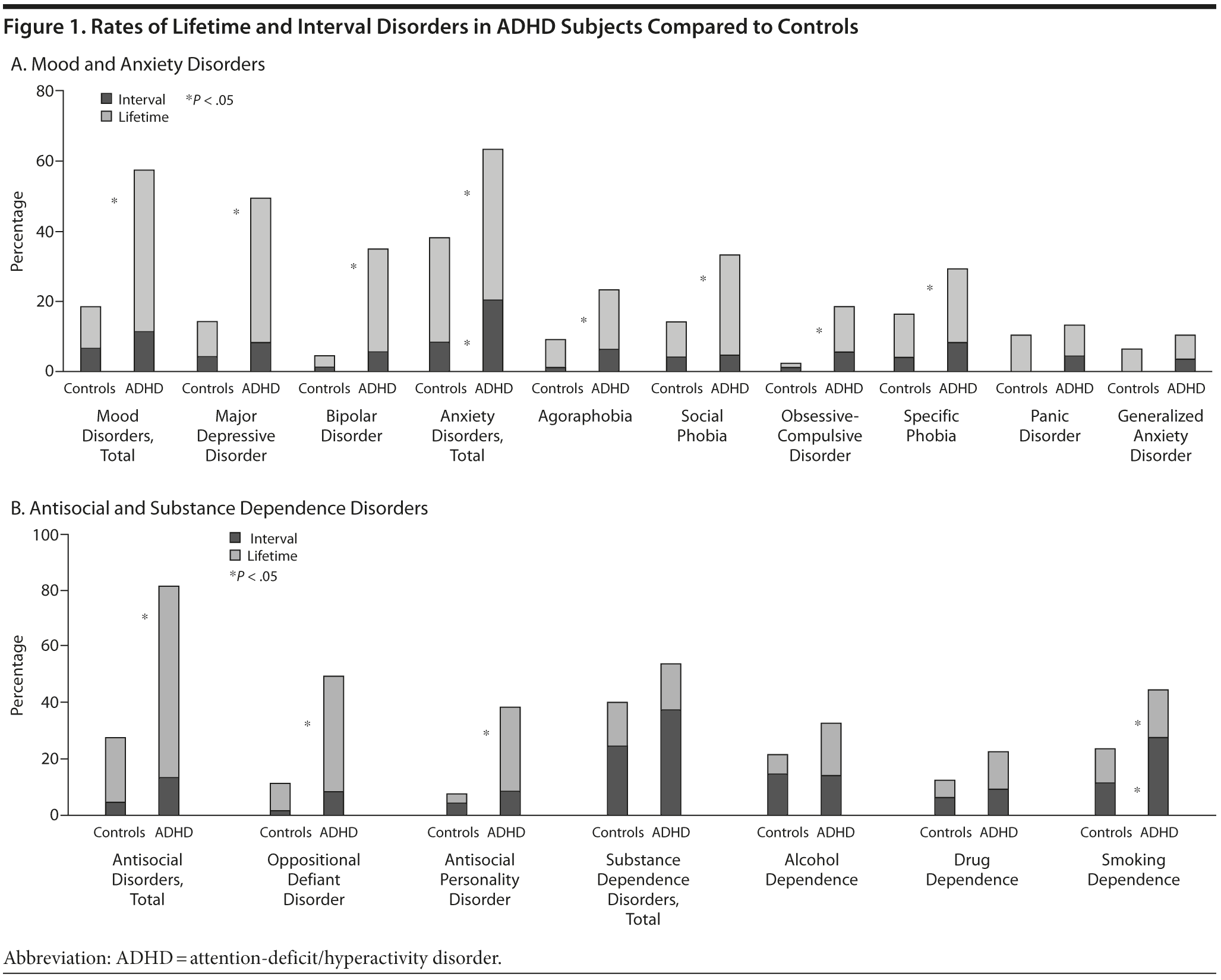
At the 16-year follow-up, subjects with ADHD continued to significantly differ from controls in lifetime rates of antisocial, mood, and anxiety disorders (with the exception of panic and generalized anxiety disorders) and smoking dependence (Figure 1). In contrast, with the exception of higher interval prevalence of anxiety disorders (20% vs 8%, z = 2.32, P = .02) and smoking dependence (27% vs 11%, z = 2.30, P = .02), the incidence of individual interval disorders were markedly lower and were not statistically significant from those of controls. Within the ADHD group, persistent ADHD was not significantly associated with anxiety disorders and smoking dependence (z = 0.43, P = .67, and z = 0.48, P = .64, respectively) or any other disorder in the interval period (all P values > .05).
Functional, Educational, Occupational, and Cognitive Outcomes
Compared to controls, men who had ADHD as boys had significantly more impaired current (last month) global functioning (mean ± SD GAF scores = 62.5 ± 8.2 vs 66.6 ± 6.2, t154 = 3.22, P = .002) and significantly more current family conflict (Moos Family Environment Scale scores = 44.4 ± 11.9 vs 39.4 ± 7.6, t90 = 2.24, P = .03).
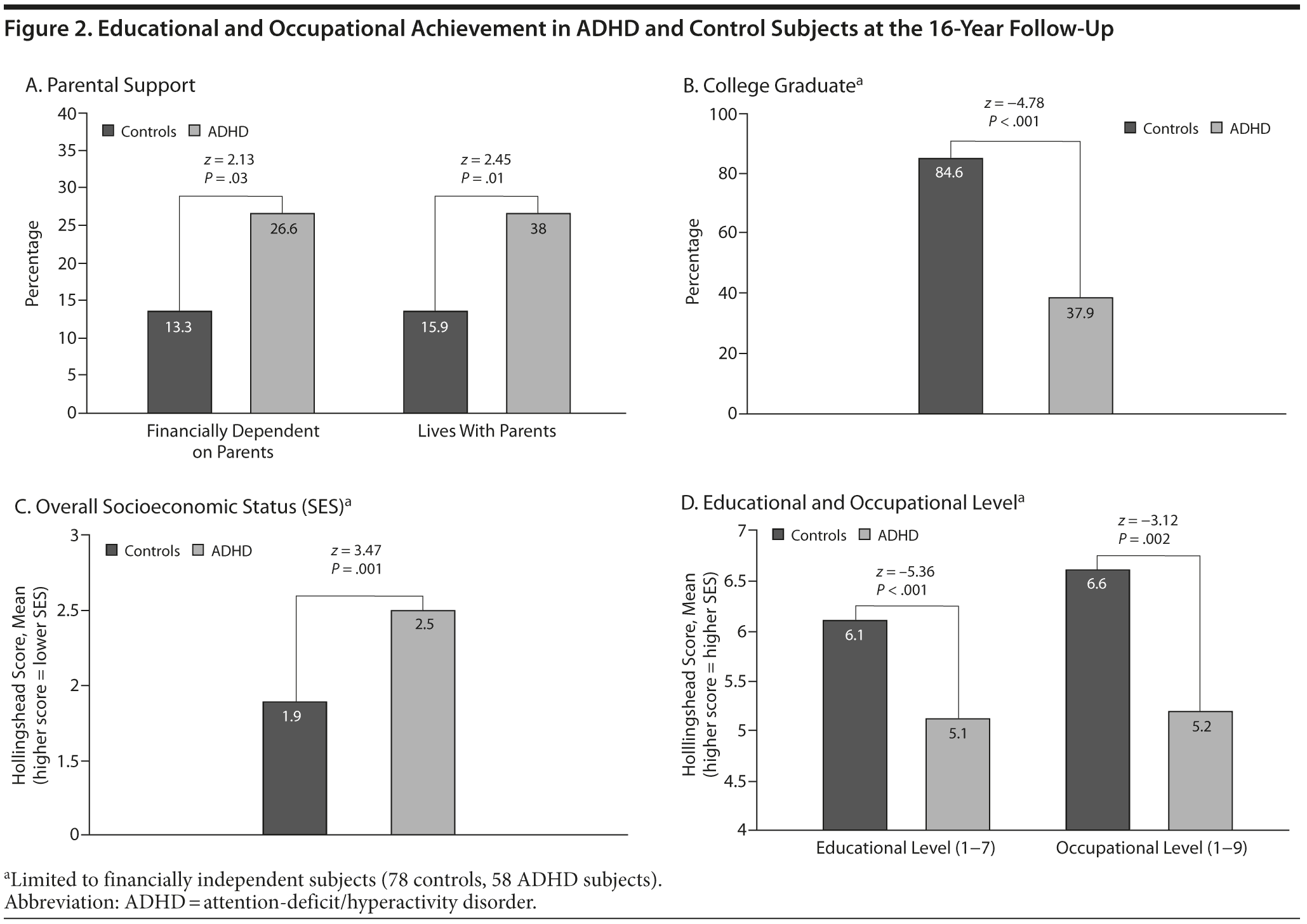
Men who had ADHD as boys were significantly more likely to be financially dependent on their parents versus controls (Figure 2A). Within the group of financially independent boys (78 controls, 58 ADHD subjects), the controls, when grown up, had a higher rate of college graduation versus men who had ADHD as boys (Figure 2B). Within this group of financially independent subjects, boys with ADHD also had significantly lower personal socioeconomic status (vs their family of origin socioeconomic status) (Figure 2C and 2D). With the exceptions of being financially independent (P = .08) and living with parents (P = .06), all educational and occupational outcomes remained significant after controlling for the total number of psychiatric disorders other than ADHD in the interval period (all P values < .01). Within the ADHD group, none of the educational and occupational achievement outcomes were significantly associated with persistent ADHD (all P values > .20).
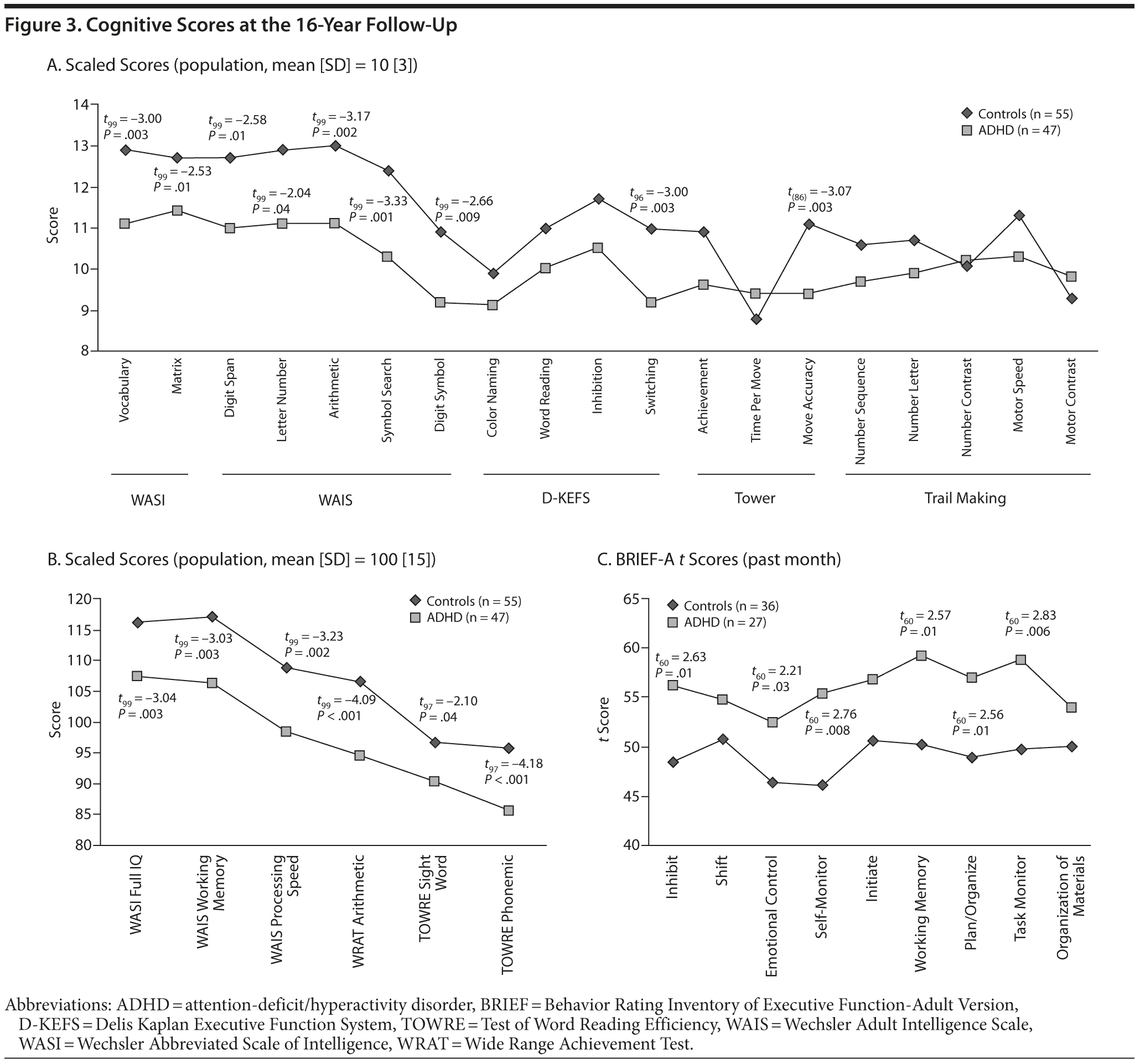
Men who had ADHD as boys were also significantly more impaired than controls on all measures of the WASI and WAIS, D-KEFS switching, TOWRE move accuracy, WRAT arithmetic, and TOWRE sight word and phonemic scores (Figure 3A and 3B). The boys with ADHD also had a significantly higher rate of arithmetic learning disability (WRAT score ≤ 85) versus controls (32% vs 13%, z = 2.03, P = .04) and significantly more impaired scores on most scales of the BRIEF-A (Figure 3C). When controlling for psychiatric disorders other than ADHD, all neuropsychological findings remained statistically significant except for WAIS letter number (P = .053) and rate of arithmetic learning disability (P = .06). However, only self-monitoring from the BRIEF-A remained statistically significant after controlling for interval disorders (P = .03). Within the ADHD group, persistent ADHD was not significantly associated with any psychometric testing measures (all P values > .05). On the other hand, compared to subjects with remittent ADHD, persistent ADHD was significantly associated with more impaired mean ± SD scores on the inhibit (58.6 ± 9.3 vs 48.9 ± 11.0), shift (57.8 ± 10.5 vs 46.1 ± 9.3), emotional control (55.2 ± 9.8 vs 44.4 ± 6.6), initiate (59.9 ± 12.1 vs 47.911.3), working memory (62.1 ± 12.6 vs 49.3 ± 11.4), and planning/organizing (60.4 ± 10.4 vs 46.9 ± 10.6) scales of the BRIEF-A (all P values < .05).
DISCUSSION
This 16-year follow-up found that, compared with age- and sex-matched controls, by a mean age of 27 years, men who had ADHD as boys had statistically indistinguishable rates of antisocial, mood, and alcohol and drug addictions in the 6-year interval since their prior assessment. Despite these low rates of interval psychiatric disorders, men who had ADHD as boys were at significantly higher risk than controls for a wide range of adverse psychosocial, educational, occupational, and cognitive outcomes, even after controlling for psychiatric disorders, indicating that these impairments were due to ADHD itself and not to other psychiatric disorders. The consistency in findings between these prospective results with those derived from retrospective studies of adults with ADHD18,31 strongly supports the syndromic continuity between pediatric and adult ADHD.
The discrepancies between high lifetime rates and modest current rates of psychiatric disorders in this longitudinal sample are highly consistent with results from cross-sectional and retrospective studies of adults with ADHD.18 In both study designs, ADHD adults have high lifetime rates of mood, anxiety, and antisocial disorders but much more modest interval or current diagnoses of the same disorders when compared with those in non-ADHD controls. Although the reasons for these discrepancies are not entirely clear, they suggest that psychiatric disorders emerge early on in development in childhood and adolescence19 and subsequently remit. The subjects reassessed at follow-up had a lower percentage of antisocial disorders at baseline compared to subjects lost to follow-up, which may have contributed to low rates of psychiatric disorders at follow-up. It is also possible that ADHD individuals with anxiety disorders are higher functioning and more likely to participate in a follow-up study. Since in this prospective study the majority of ADHD subjects had been treated with stimulants, and we previously documented that stimulant treatment mitigates the development of other psychiatric disorders at the 10-year follow-up of this sample,32 it is also possible that the marked decline in psychiatric disorders from childhood to adulthood may have been due to the benefits of treatment. Weiss and colleagues7 found that 23% of “relatively untreated” hyperactive children had antisocial personality disorder at the 15-year follow-up. In comparison, only 8% of our ADHD subjects were diagnosed with antisocial personality disorder at the 16-year follow-up, and all but 1 of our subjects had received treatment for ADHD at some point in their lives. Further analysis should be conducted to test the hypothesis that treatment for ADHD lowers the risk for developing additional disorders.
Two exceptions to the lack of differences in interval disorders between men who had ADHD as boys and controls were the significantly higher interval prevalence of anxiety disorders and smoking dependence in the ADHD group. The higher rates of anxiety disorders in this long-term longitudinal sample indicate that anxiety disorders may be more persistent than other disorders in adults who had ADHD as children. Similar findings of an increased risk for anxiety disorders in individuals with ADHD have been reported in the pediatric and adult literature.18,33-37 Considering that ADHD and anxiety disorders require different treatment approaches, this knowledge should help guide therapeutic approaches aimed at individuals with ADHD and anxiety disorders.
The overrepresentation of nicotine dependence identified in this long-term longitudinal sample of men who had ADHD as boys is consistent with a large body of literature showing that a disproportionately large number of individuals with ADHD smoke, with an earlier initiation, a greater risk of progression to regular smoking, and a greater difficulty quitting smoking, as compared to non-ADHD counterparts.38-41 Glass and Flory42 summarized several possible mechanisms for the relationship between ADHD and smoking. One hypothesis is that ADHD patients self-medicate with nicotine. Another is that there are overlapping social, cognitive, and biological risk factors for ADHD and smoking. Considering that the onset of ADHD is, on average, 10 years prior to the onset of smoking, children with ADHD are a very important at-risk population for preventive and early intervention efforts aimed at mitigating this risk.
Despite the low rates of psychiatric disorders, men who had ADHD as boys were significantly more impaired than controls in all measures of the WASI and WAIS, D-KEFS switching, TOWRE move accuracy, WRAT arithmetic, and TOWRE sight word and phonemic scores. Men who had ADHD as boys also had a significantly higher rate of arithmetic learning disability (WRAT score ≤ 85) than controls. The majority of these findings remained significant even after controlling for other psychiatric disorders, indicating that these cognitive deficits are due to ADHD itself.
The persistence of psychometrically assessed neuropsychological deficits from childhood into adult life is consistent with previous retrospective and cross-sectional studies of adults with ADHD documenting similar cognitive deficits in studies of adults with ADHD.43 Considering the high level of persistence of neuropsychological deficits into adult years44 and the high level of morbidity associated with them,45,46 serious consideration should be given to include persistence of neuropsychological deficits in the conceptualization of persistence of ADHD based solely on symptoms of the disorder. Saylor et al47 suggest that including the assessment of adaptive and executive function in clinical trials may contribute to understanding and treating ADHD. Men who had ADHD as boys also had significantly more impaired scores on most scales of the BRIEF-A subscales assessing behavioral concomitants of executive function deficits. Although most of these differences lost significance after controlling for other psychiatric disorders, if these disorders have a legitimate relationship with ADHD, covarying for them may remove variance that is due to ADHD and therefore should not be considered confounding factors.8,48
In this long-term longitudinal follow-up study, men who had ADHD as boys were significantly more likely to be financially dependent on their parents, less likely to graduate from college, and had a lower social class than controls. With few exceptions, these outcomes remained significant after controlling for other psychiatric disorders in the interval period. These findings are consistent with other studies of ADHD adults49 and adults who had ADHD as children,16,50 which also found that adults who had ADHD as children were less likely than controls to be financially independent, had a lower personal socioeconomic status, were less likely to graduate from college, and had a lower occupational level. These functional deficits are likely to be aggravated by the higher levels of neuropsychological impairment, which we observed both on psychometric tests and on behavioral measures of executive dysfunction.
The risks for anxiety disorders and smoking dependence were independent of the persistence of ADHD in our sample, suggesting that these disorders are part of the developmental progression of psychopathology in children with ADHD and are not solely concurrent comorbidities. Likewise, neuropsychological, educational, and occupational deficits were all impaired in adulthood regardless of the course of ADHD. Only self-reported executive function deficits were associated with persistent ADHD.
The strengths of this report include the well-characterized sample, the long-term follow-up period reaching adult years, and the use of contemporaneous assessment methods, diagnostic criteria, and statistical approaches. This study is especially important since very few prior studies have followed ADHD children into adulthood who had been diagnosed with modern diagnostic criteria (ie, DSM-III or later) (Table 1). Since our sample was ascertained from both pediatric and psychiatric sources, this feature enhances the generalizability of our findings.
However, some methodological limitations were operant as well. Because our sample was white and referred, our results may not generalize to other ethnic groups or community samples. Although subjects who were not assessed at the 16-year follow-up had a lower socioeconomic status than subjects who were, every Hollingshead socioeconomic status category assessed at baseline (ie, levels 1 through 4) was also represented in the sample that was reascertained, minimizing the effect of any bias. Another limitation was that controls at follow-up had higher baseline GAF scores and a lower rate of baseline antisocial disorders than those lost to follow-up. Yet, despite this limitation, our controls showed lifetime rates of disorders consistent with what one would expect from population studies. Although there were no other meaningful differences at baseline between subjects who were not assessed at the 16-year follow-up and subjects who were, we cannot rule out the possibility that attrition bias may have affected our findings. Although our low retention rate in the ADHD group is a limitation, Table 1 shows that it was within the range of other longitudinal studies of ADHD. In a longitudinal clinical trial of asthma medication, Bender and colleagues51 found that pediatric dropouts were significantly more likely than completers to have lower IQ and problem-solving test scores, as well as more behavioral problems. This helps explain the higher dropout rate in our ADHD group, because lower neuropsychological test scores and more behavioral problems are correlates of ADHD. Although our sample was originally ascertained according to DSM-III-R criteria, considering the very high overlap between DSM-III-R and DSM-IV criteria (93%),52 any effect should be minimal. The generalizability of this study is limited to children referred for ADHD and treated naturalistically for the disorder. Longitudinal studies in the community or with untreated subjects with ADHD may help to understand the natural history of this disorder.
Despite these limitations, this 16-year follow-up found that men who had ADHD as boys were at higher risk than controls for a wide range of adverse psychosocial, educational, occupational, and cognitive outcomes, even after controlling for other psychiatric disorders. These results indicate that the many impairments associated with ADHD in adult life are due to ADHD itself and not to associated psychiatric disorders. The consistency in findings between these prospective results with those derived from retrospective studies of adults with ADHD strongly supports the syndromic continuity between pediatric and adult ADHD.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Author affiliations: Clinical and Research Programs in Pediatric Psychopharmacology and Adult ADHD of the Psychiatry Department, Massachusetts General Hospital, Boston (Dr Biederman, Mr Petty, and Mss Woodworth, Lomedico, and Hyder); Psychiatry Department, Harvard Medical School, Cambridge, Massachusetts (Dr Biederman); and Departments of Psychiatry and of Neuroscience and Physiology, SUNY Upstate Medical University, Syracuse, New York (Dr Faraone).
Financial disclosure: Dr Biederman is currently receiving research support from Elminda, Janssen, McNeil, and Shire. In 2011, he gave a single unpaid talk for Juste Pharmaceutical Spain; received honoraria from the Massachusetts General Hospital (MGH) Psychiatry Academy for a tuition-funded continuing medical education (CME) course; received an honorarium for presenting at an international scientific conference on ADHD; received an honorarium from Cambridge University Press for a chapter publication; and received departmental royalties from a copyrighted rating scale used for ADHD diagnoses that were paid by Eli Lilly, Shire, and AstraZeneca to the Department of Psychiatry at MGH. In 2010, he received a speaker’s fee from a single talk given at Fundación Dr Manuel Camelo A.C. in Monterrey, Mexico; received honoraria, paid to the Department of Psychiatry at MGH, for providing single consultations for Shionogi Pharma and Cipher Pharmaceuticals; and received honoraria from the MGH Psychiatry Academy for a tuition-funded CME course. In previous years, he received research support, consultation fees, or speaker’s fees for/from Abbott, Alza, AstraZeneca, Boston University, Bristol-Myers Squibb, Celltech, Cephalon, Eli Lilly, Esai, Fundacion Areces (Spain), Forest, Glaxo, Gliatech, Hastings Center, Janssen, McNeil, Medice Pharmaceuticals (Germany), Merck, MMC Pediatric, the National Alliance for Research on Schizophrenia and Depression, the National Institute on Drug Abuse, New River, the National Institute of Child Health and Human Development, the National Institute of Mental Health, Novartis, Noven, Neurosearch, Organon, Otsuka, Pfizer, Pharmacia, Phase V Communications, Physicians Academy, Prechter Foundation, Quantia Communications, Reed Exhibitions, Shire, Spanish Child Psychiatry Association, Stanley Foundation, UCB Pharma, Veritas, and Wyeth. In 2011, Dr Faraone received consulting income and research support from Shire and Alcobra and research support from the National Institutes of Health. In previous years, he received consulting fees or was on advisory boards or participated in CME programs sponsored by Shire, McNeil, Janssen, Novartis, Pfizer, and Eli Lilly. He receives royalties from books published by Guilford Press (Straight Talk About Your Child’s Mental Health) and by Oxford University Press (Schizophrenia: The Facts). Mr Petty and Mss Woodworth, Lomedico, and Hyder have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: This work was supported, in part, by a grant from the Lilly Foundation and the Pediatric Psychopharmacology Council Fund of the Massachusetts General Hospital, Boston.
Role of sponsor: The funding sponsor had no role in the study design, study implementation, data collection, management, analysis, interpretation, or preparation/approval of the manuscript.
REFERENCES
1. Hechtman L, Weiss G, Perlman T. Young adult outcome of hyperactive children who received long-term stimulant treatment. J Am Acad Child Psychiatry. 1984;23(3):261-269. PubMed doi:10.1016/S0002-7138(09)60501-X
2. Loney J, Kramer J, Milich RS. The hyperactive child grows up: predictors of symptoms, delinquency and achievement at follow-up. In: Gadow KD, Loney J, eds. Psychosocial Aspects of Drug Treatment for Hyperactivity. Boulder, CO: Westview Press; 1981:381-416.
3. August GJ, Stewart MA, Holmes CS. A four-year follow-up of hyperactive boys with and without conduct disorder. Br J Psychiatry. 1983;143(2):192-198. PubMed doi:10.1192/bjp.143.2.192
4. Gittelman R, Mannuzza S, Shenker R, et al. Hyperactive boys almost grown up, 1: psychiatric status. Arch Gen Psychiatry. 1985;42(10):937-947. PubMed
5. Hart EL, Lahey BB, Loeber R, et al. Developmental change in attention-deficit hyperactivity disorder in boys: a four-year longitudinal study. J Abnorm Child Psychol. 1995;23(6):729-749. PubMed doi:10.1007/BF01447474
6. Mannuzza S, Klein RG, Moulton JL 3rd. Lifetime criminality among boys with attention deficit hyperactivity disorder: a prospective follow-up study into adulthood using official arrest records. Psychiatry Res. 2008;160(3):237-246. PubMed doi:10.1016/j.psychres.2007.11.003
7. Weiss G, Hechtman L, Milroy T, et al. Psychiatric status of hyperactives as adults: a controlled prospective 15-year follow-up of 63 hyperactive children. J Am Acad Child Psychiatry. 1985;24(2):211-220. PubMed doi:10.1016/S0002-7138(09)60450-7
8. Barkley RA, Fischer M. The unique contribution of emotional impulsiveness to impairment in major life activities in hyperactive children as adults. J Am Acad Child Adolesc Psychiatry. 2010;49(5):503-513. PubMed
9. Satterfield JH, Faller KJ, Crinella FM, et al. A 30-year prospective follow-up study of hyperactive boys with conduct problems: adult criminality. J Am Acad Child Adolesc Psychiatry. 2007;46(5):601-610. PubMed doi:10.1097/chi.0b013e318033ff59
10. Fergusson DM, Boden JM, Horwood LJ. Classification of behavior disorders in adolescence: scaling methods, predictive validity, and gender differences. J Abnorm Psychol. 2010;119(4):699-712. PubMed doi:10.1037/a0018610
11. Surman CB, Biederman J, Spencer T, et al. Deficient emotional self-regulation and adult attention deficit hyperactivity disorder: a family risk analysis. Am J Psychiatry. 2011;168(6):617-623. PubMed doi:10.1176/appi.ajp.2010.10081172
12. Weiss MD, Gibbins C, Goodman DW, et al. Moderators and mediators of symptoms and quality of life outcomes in an open-label study of adults treated for attention-deficit/hyperactivity disorder. J Clin Psychiatry. 2010;71(4):381-390. PubMed doi:10.4088/JCP.08m04709pur
13. Biederman J, Petty CR, Monuteaux MC, et al. Adult psychiatric outcomes of girls with attention deficit hyperactivity disorder: 11-year follow-up in a longitudinal case-control study. Am J Psychiatry. 2010;167(4):409-417. PubMed doi:10.1176/appi.ajp.2009.09050736
14. Mick E, Faraone SV, Spencer T, et al. Assessing the validity of the quality of life enjoyment and satisfaction questionnaire short form in adults with ADHD. J Atten Disord. 2008;11(4):504-509. PubMed doi:10.1177/1087054707308468
15. Biederman J, Petty CR, Fried R, et al. Educational and occupational underattainment in adults with attention-deficit/hyperactivity disorder: a controlled study. J Clin Psychiatry. 2008;69(8):1217-1222. PubMed doi:10.4088/JCP.v69n0803
16. Barkley RA, Murphy KR, Fischer M. ADHD in Adults: What the Science Says. New York, NY: Guilford Press; 2008.
17. Faraone SV, Wilens TE, Petty C, et al. Substance use among ADHD adults: implications of late onset and subthreshold diagnoses. Am J Addict. 2007;16(suppl 1):24-32, quiz 33-34. PubMed doi:10.1080/10550490601082767
18. Faraone SV, Biederman J, Spencer T, et al. Diagnosing adult attention deficit hyperactivity disorder: are late onset and subthreshold diagnoses valid? Am J Psychiatry. 2006;163(10):1720-1729, quiz 1859. PubMed doi:10.1176/appi.ajp.163.10.1720
19. Biederman J, Monuteaux MC, Mick E, et al. Young adult outcome of attention deficit hyperactivity disorder: a controlled 10-year follow-up study. Psychol Med. 2006;36(2):167-179. PubMed doi:10.1017/S0033291705006410
20. First M, Spitzer R, Gibbon M, et al. Structured Clinical Interview for DSM-IV Axis I Disorders. Washington, DC: American Psychiatric Press; 1997.
21. Orvaschel H. Schedule for Affective Disorder and Schizophrenia for School-Age Children Epidemiologic Version. 5th ed. Ft Lauderdale, FL: Nova Southeastern University, Center for Psychological Studies; 1994.
22. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition. Washington, DC: American Psychiatric Association; 1994.
23. Hollingshead AB. Four Factor Index of Social Status. New Haven, CT: Yale Press; 1975.
24. Moos RH, Moos BS. Manual for the Family Environment Scale. Palo Alto, CA: Consulting Psychologists Press; 1974.
25. Roth R, Isquith P, Gioia G. Brief-A Behavior Rating Inventory of Executive Function-Adult Version, Publication Manual. Lutz, FL. Psychological Assessment Resources Inc; 2005.
26. Wechsler D. Wechsler Abbreviated Scale of Intelligence (WASI), 4th ed. San Antonio, TX: The Psychological Corporation; 1999.
27. Wechsler D. Wechsler Adult Intelligence Scale III. 3rd ed. San Antonio, TX: The Psychological Corporation; 1997 [manual].
28. Delis D, Kaplan E, Kraemer JH. Delis-Kaplan Executive Function System (D-KEFS). San Antonio, TX: The Psychological Corporation; 2001.
29. Torgesen JK, Wagner RK, Rashotte CA. Test of Word Reading Efficiency. Austin, TX: Pro-Ed Inc; 1999.
30. Jastak J, Jastak S. Wide Range Achievement Test. 3rd ed. Wilmington, DE: Jastak Associates; 1993.
31. Biederman J, Faraone SV, Spencer T, et al. Patterns of psychiatric comorbidity, cognition, and psychosocial functioning in adults with attention deficit hyperactivity disorder. Am J Psychiatry. 1993;150(12):1792-1798. PubMed
32. Biederman J, Monuteaux MC, Spencer T, et al. Do stimulants protect against psychiatric disorders in youth with ADHD? a 10-year follow-up study. Pediatrics. 2009;124(1):71-78. PubMed doi:10.1542/peds.2008-3347
33. March JS, Swanson JM, Arnold LE, et al. Anxiety as a predictor and outcome variable in the multimodal treatment study of children with ADHD (MTA). J Abnorm Child Psychol. 2000;28(6):527-541. PubMed doi:10.1023/A:1005179014321
34. Jensen PS, Hinshaw SP, Kraemer HC, et al. ADHD comorbidity findings from the MTA study: comparing comorbid subgroups. J Am Acad Child Adolesc Psychiatry. 2001;40(2):147-158. PubMed doi:10.1097/00004583-200102000-00009
35. Biederman J, Faraone SV, Mick E, et al. Clinical correlates of ADHD in females: findings from a large group of girls ascertained from pediatric and psychiatric referral sources. J Am Acad Child Adolesc Psychiatry. 1999;38(8):966-975. PubMed doi:10.1097/00004583-199908000-00012
36. Biederman J, Faraone S, Milberger S, et al. A prospective 4-year follow-up study of attention-deficit hyperactivity and related disorders. Arch Gen Psychiatry. 1996;53(5):437-446. PubMed doi:10.1001/archpsyc.1996.01830050073012
37. Biederman J, Faraone SV, Monuteaux MC, et al. Gender effects on attention-deficit/hyperactivity disorder in adults, revisited. Biol Psychiatry. 2004;55(7):692-700. PubMed doi:10.1016/j.biopsych.2003.12.003
38. Humfleet GL, Prochaska JJ, Mengis M, et al. Preliminary evidence of the association between the history of childhood attention-deficit/hyperactivity disorder and smoking treatment failure. Nicotine Tob Res. 2005;7(3):453-460. PubMed doi:10.1080/14622200500125310
39. McClernon FJ, Fuemmeler BF, Kollins SH, et al. Interactions between genotype and retrospective ADHD symptoms predict lifetime smoking risk in a sample of young adults. Nicotine Tob Res. 2008;10(1):117-127. PubMed doi:10.1080/14622200701704913
40. Pomerleau CS, Downey KK, Snedecor SM, et al. Smoking patterns and abstinence effects in smokers with no ADHD, childhood ADHD, and adult ADHD symptomatology. Addict Behav. 2003;28(6):1149-1157. PubMed doi:10.1016/S0306-4603(02)00223-X
41. Wilens TE, Vitulano M, Upadhyaya H, et al. Cigarette smoking associated with attention deficit hyperactivity disorder. J Pediatr. 2008;153(3):414-419. PubMed doi:10.1016/j.jpeds.2008.04.030
42. Glass K, Flory K. Why does ADHD confer risk for cigarette smoking? a review of psychosocial mechanisms. Clin Child Fam Psychol Rev. 2010;13(3):291-313. PubMed doi:10.1007/s10567-010-0070-3
43. Faraone SV, Biederman J, Doyle AE, et al. Neuropsychological studies of late onset and subthreshold diagnoses of adult attention-deficit/hyperactivity disorder. Biol Psychiatry. 2006;60(10):1081-1087. PubMed doi:10.1016/j.biopsych.2006.03.060
44. Biederman J, Petty CR, Fried R, et al. Stability of executive function deficits into young adult years: a prospective longitudinal follow-up study of grown up males with ADHD. Acta Psychiatr Scand. 2007;116(2):129-136. PubMed doi:10.1111/j.1600-0447.2007.01008.x
45. Antshel KM, Faraone SV, Maglione K, et al. Executive functioning in high-IQ adults with ADHD. Psychol Med. 2010;40(11):1909-1918. PubMed doi:10.1017/S0033291709992273
46. Biederman J, Petty C, Fried R, et al. Impact of psychometrically defined deficits of executive functioning in adults with attention deficit hyperactivity disorder. Am J Psychiatry. 2006;163(10):1730-1738. PubMed doi:10.1176/appi.ajp.163.10.1730
47. Saylor KE, Buermeyer CM, Spencer TJ, et al. Adaptive changes related to medication treatment of ADHD: listening to parents of children in clinical trials of a novel nonstimulant medication. J Clin Psychiatry. 2002;63(suppl 12):23-28. PubMed
48. Angold A, Costello EJ, Erkanli A. Comorbidity. J Child Psychol Psychiatry. 1999;40(1):57-87. PubMed doi:10.1111/1469-7610.00424
49. Biederman J, Faraone SV, Spencer TJ, et al. Functional impairments in adults with self-reports of diagnosed ADHD: a controlled study of 1001 adults in the community. J Clin Psychiatry. 2006;67(4):524-540. PubMed doi:10.4088/JCP.v67n0403
50. Halm׸y A, Fasmer OB, Gillberg C, et al. Occupational outcome in adult ADHD: impact of symptom profile, comorbid psychiatric problems, and treatment: a cross-sectional study of 414 clinically diagnosed adult ADHD patients. J Atten Disord. 2009;13(2):175-187. PubMed doi:10.1177/1087054708329777
51. Bender BG, Iklé DN, DuHamel T, et al. Retention of asthmatic patients in a longitudinal clinical trial. J Allergy Clin Immunol. 1997;99(2):197-203. PubMed doi:10.1016/S0091-6749(97)70096-4
52. Biederman J, Faraone SV, Weber W, et al. Correspondence between DSM-III-R and DSM-IV attention-deficit/hyperactivity disorder. J Am Acad Child Adolesc Psychiatry. 1997;36(12):1682-1687. PubMed doi:10.1097/00004583-199712000-00016