Objective: The nonmedical use of stimulants (misuse) in the college setting remains of utmost public health and clinical concern. The objective of this study was to evaluate comprehensively the characteristics of college students who misused stimulants, attending to rates of attention-deficit/hyperactivity disorder (ADHD), other psychopathology, and substance use disorders.
Methods: The data presented are from a cross-sectional study of college students who misused prescription stimulant medications (not including cocaine or methamphetamine) and controls (college students without stimulant misuse). Between May 2010 and May 2013, college students were assessed blindly for psychopathology and substance use disorder by way of Structured Clinical Interview for DSM-IV-TR Axis I Disorders, Research Version, Patient Edition (SCID-I/P) and completion of self-report questionnaires.
Results: The analysis included 198 controls (mean ± SD age = 20.7 ± 2.6 years) and 100 stimulant misusers (20.7 ± 1.7 years). Misusers, when compared to controls, were more likely to endorse alcohol, drug, alcohol + drug, and any substance use disorder (all P values < .01). When a subset of stimulant misusers (n = 58) was examined, 67% had a full or subthreshold prescription stimulant use disorder. Misusers also had higher rates of conduct disorder (10% vs 3%; P = .02) and ADHD (including subthreshold cases; 27% vs 16%; P = .02) in addition to lower Global Assessment of Functioning score (P < .01). Higher rates of misuse of immediate-release—relative to extended-release—stimulants were reported.
Conclusions: Our data suggest that, compared to controls, college students who misuse stimulant medications are more likely to have ADHD, conduct disorder, stimulant and other substance use disorder, and overall dysfunction.’ ‹

Nonmedical Stimulant Use in College Students:
Association With Attention-Deficit/Hyperactivity Disorder and Other Disorders
ABSTRACT
Objective: The nonmedical use of stimulants (misuse) in the college setting remains of utmost public health and clinical concern. The objective of this study was to evaluate comprehensively the characteristics of college students who misused stimulants, attending to rates of attention-deficit/hyperactivity disorder (ADHD), other psychopathology, and substance use disorders.
Methods: The data presented are from a cross-sectional study of college students who misused prescription stimulant medications (not including cocaine or methamphetamine) and controls (college students without stimulant misuse). Between May 2010 and May 2013, college students were assessed blindly for psychopathology and substance use disorder by way of Structured Clinical Interview for DSM-IV-TR Axis I Disorders, Research Version, Patient Edition (SCID-I/P) and completion of self-report questionnaires.
Results: The analysis included 198 controls (mean ± SD age = 20.7 ± 2.6 years) and 100 stimulant misusers (20.7 ± 1.7 years). Misusers, when compared to controls, were more likely to endorse alcohol, drug, alcohol + drug, and any substance use disorder (all P values < .01). When a subset of stimulant misusers (n = 58) was examined, 67% had a full or subthreshold prescription stimulant use disorder. Misusers also had higher rates of conduct disorder (10% vs 3%; P = .02) and ADHD (including subthreshold cases; 27% vs 16%; P = .02) in addition to lower Global Assessment of Functioning score (P < .01). Higher rates of misuse of immediate-release—relative to extended-release—stimulants were reported.
Conclusions: Our data suggest that, compared to controls, college students who misuse stimulant medications are more likely to have ADHD, conduct disorder, stimulant and other substance use disorder, and overall dysfunction.
J Clin Psychiatry 2016;77(7):940-947
dx.doi.org/10.4088/JCP.14m09559
© Copyright 2016 Physicians Postgraduate Press, Inc.
aPediatric Psychopharmacology Program, Division of Child Psychiatry, Massachusetts General Hospital, Boston
bDepartment of Psychiatry, Massachusetts General Hospital, and Harvard Medical School, Boston
*Corresponding author: Timothy E. Wilens, MD, Child Psychiatry Service, Massachusetts General Hospital, 55 Fruit St, YAW 6A, Boston, MA 02114 ([email protected]).
Attention-deficit/hyperactivity disorder (ADHD) is estimated to affect up to 8% of college students in the United States.1 Stimulant medications are among the first-line agents for the treatment of ADHD in adolescents and young adults.2-4 Although stimulants are highly efficacious and have a well-documented safety profile,2 the nonmedical use of stimulant medications (eg, the use of stimulants without a prescription),5 particularly among college students, appears to be gaining weight as an important part of the drug-use problem.
Several college-based studies6-12 have documented the prevalence of nonmedical use of stimulants. For example, Teter et al9 surveyed a random sample of 4,580 college students and found that the lifetime and past-year prevalence rates for illicit use of prescription stimulants were 8.3% and 5.9%, respectively. The College Alcohol Study reported by McCabe et al6 found that at some US colleges, 1 in every 4 students had misused stimulants in the past year. More recent data suggest that, over a 4-year period, almost two-thirds of college students were offered prescription stimulants for nonmedical use, and 31% had used stimulants for nonmedical purposes.11 Together, these studies show that rates of nonmedical use of prescription stimulants are a growing public health concern.
Studies have begun to shed light on the characteristics and context of stimulant misuse. Characteristics associated with stimulant misuse include white race and fraternity or sorority affiliation.6-9,13 High rates of substance use disorders have also been reported in association with stimulant misuse.12-14 Studies are inconsistent on findings between sexes including both rates and context of misuse.7,8,15-17
Despite the clear evidence of stimulant misuse in college students, a dearth of information remains as to the reasons and context for use. For instance, to our knowledge, there is a scarcity of studies that have specifically evaluated ADHD and other psychopathological diagnoses using structured psychiatric interviews in college students misusing stimulants. To this end, we sought to examine the gaps in the literature by studying a heterogeneous sample of college students attending to ADHD, psychiatric, and substance use disorders; types of stimulants misused; and context of misuse. On basis of the literature,12,13 we hypothesized that stimulant misusers, compared to college students with no misuse of stimulants (controls), would have higher rates of ADHD symptoms or a full diagnosis of ADHD. We also hypothesized that rates of substance use disorders would be higher in stimulant misusers than in controls. Second, we speculated that stimulant misusers would have higher rates of other psychopathology than controls and that there would be a preponderance of misuse of immediate-release relative to extended-release stimulants.
METHODS
Subjects
We recruited 100 subjects who were not receiving prescription stimulants therapeutically (ie, in relation to a diagnosis of ADHD) but endorsed stimulant misuse (misusers) and 200 subjects who were not being treated with stimulant medication, had never misused prescription stimulants, and for whom a prior diagnosis of ADHD was not exclusionary (controls). Subjects from both groups were college students in the Boston metropolitan area recruited by way of Internet advertisements (eg, craigslist.com, myspace.com). These advertisements asked for college students in the Boston area to participate in a study examining the causal factors, context, and characteristics of misuse of stimulants in college students, focusing on ADHD and other neuropsychological disorders. We recruited both men and women between the ages of 18 and 28 years who were currently enrolled in a local undergraduate program. All subjects completed an informed consent to participate in the study. We obtained a federal release of confidentiality, and the institutional review board approved all aspects of the study.
We excluded subjects with any major sensorimotor handicaps that would impede the testing process, such as paralysis, deafness, blindness, profound disorders of language such as autism, inadequate command of the English language, or an estimated full-scale IQ less than 80. Subjects provided written informed consent to participate in the study. In order to have a more representative sample of both sexes (40% of college students in the Boston area were male), we overrecruited males.

- Misuse of stimulants may not be an isolated occurrence and may be associated with a separate substance use disorder that necessitates identification, referral, and treatment.
- Some misusers may be self-medicating. These individuals should be screened for attention-deficit/hyperactivity disorder (ADHD), substance use disorder, psychiatric disorders, and overall dysfunction.
- Compared to immediate-release stimulants, the extended-release stimulants appear to be less misused and should be prescribed for college students with ADHD and those with a history of substance use disorder plus ADHD to reduce the potential for misuse and diversion.
A 2-stage recruitment procedure selected subjects. First, subjects answered a self-report Internet screen, which we designed using the online survey creation program Illume from DatStat. This is a platform for electronic data capture that streamlines data collection and management and ensures data integrity. Second, following recruitment, subjects were asked to complete a brief Internet screening survey on “college lifestyle.” Embedded in the lifestyle survey was the 6-item World Health Organization screen for ADHD,18 questions of stimulant misuse, and a question about whether or not the potential subject had a diagnosis (by a doctor) and was currently being treated for ADHD with a stimulant. Potential subjects were able to respond by phone or email for further information before taking the survey. These screens were used to determine whether subjects were eligible for the stimulant misuse group or the control group. Eligible individuals were contacted to complete a direct interview and self-report questionnaires at Massachusetts General Hospital.
For the purpose of this research, stimulant misuse included those stimulants with US Food and Drug Administration indications for ADHD, namely amphetamine (dextroamphetamine, lisdexamfetamine, immediate- and extended-release mixed amphetamine salts, and immediate- and extended-release methylphenidate) but did not include modafinil, armodafinil, methamphetamine, or other sympathomimetic amines (eg, cocaine, 3, 4-methylenedioxymethamphetamine [MDMA]).
Assessments
All diagnostic assessments were made using DSM-IV-based structured interviews19 by raters with bachelor’s or master’s degrees in psychology, with extensive training and supervision from the senior investigator. Raters and reviewers were blind to the ascertainment status of probands. Psychiatric assessments for subjects relied on the Structured Clinical Interview for DSM-IV-TR Axis I Disorders, Research Version, Patient Edition (SCID-I/P).20 For every diagnosis, information was gathered regarding the ages at onset and offset of full syndromic criteria and treatment history. Global Assessment of Functioning (GAF)19 was rated lifetime and current for each study subject. Students were assessed between May 2010 and May 2013.
Self-report and clinician-rated measures were collected using DatStat Illume. Subjects and/or research staff entered survey responses into electronic assessment forms, and the responses were then transmitted securely via encrypted connection and stored in a secure database.
All cases were presented to a committee composed of board-certified child psychiatrists and/or licensed psychologists. Diagnoses presented for review were considered positive only if the diagnosis was considered clinically meaningful due to the nature of the symptoms, the associated impairment, and the coherence of the clinical picture. All cases of suspected drug or alcohol abuse or dependence were further reviewed by a child and adult psychiatrist with additional addiction credentials (moderate and/or severe substance use disorder results are reported). Potential subjects who identified substance use disorder issues that were severe enough to require immediate attention were given referrals to local treatment centers.
To assess the reliability of our diagnostic procedures, we previously computed κ coefficients of agreement by having 3 experienced, board-certified child and adult psychiatrists diagnose subjects from audiotaped interviews made by the assessment staff. Based on 500 assessments from interviews of children and adults, the median κ coefficient was 0.98. κ Coefficients for individual diagnoses included major depression (1.0), mania (0.95), ADHD (0.88), conduct disorder (1.0), oppositional defiant disorder (0.90), antisocial personality disorder (0.80), and substance use disorder (1.0).
ADHD. We assessed ADHD using the SCID supplemented by childhood modules of ADHD from the Kiddie-Schedule for Affective Disorders and Schizophrenia for School-Age Children (K-SADS)21 and included full and subthreshold cases in our results. We included subthreshold cases due to the dimensional nature of ADHD and evidence of functional impairment across domains associated with subthreshold symptoms.22 We used the Adult ADHD Clinical Diagnostic Scale (ACDS)23 to additionally assess ADHD symptoms.
Daily functioning/interaction with peers. We used the self-reported, 16-item Quality of Life Enjoyment and Satisfaction Questionnaire (Q-LES-Q)24 to evaluate the degree of enjoyment and satisfaction experienced in 8 areas of daily functioning. Socioeconomic status of each subject was determined by applying the Hollingshead-Redlich codes25,26 to the subject’s family of origin.
Drug use. We evaluated the misuse of prescribed medications through the assessment of substance use, misuse, abuse, and dependence by structured interview, by self-report on the Drug Use Screening Inventory (DUSI),27 and by query for the appropriate use of prescribed medications on the MGH ADHD Medication Misuse and Diversion Assessment, 14,28 a self-report tool that encompasses misuse or abuse of medication, euphoria on medication, and concurrent use of drugs or alcohol.29 During study enrollment, we updated to a more comprehensive version of the SCID20 that included specific questions regarding the severity of prescription stimulant misuse. As a result, only stimulant misusers who were interviewed after the updated version was implemented received a diagnosis of full, subthreshold, or no prescription stimulant use disorder. A subthreshold diagnosis on the SCID was made if the subjects had more than half, but less than all, of the required symptoms for a full substance use disorder or as a result of clinician judgment upon blinded review of the structured interview.
Statistical Analysis
A priori to any analysis, we aggregated the anxiety disorders into 1 outcome named multiple anxiety disorders. To be placed in this category, subjects must have met the criteria for diagnosis of at least 2 of the following disorders: social phobia, separation anxiety, specific phobia, panic, agoraphobia, antisocial personality, posttraumatic stress, and obsessive-compulsive. We used the Student t test for continuous outcomes, the Wilcoxon rank sum tests for socioeconomic status, and Pearson χ2 for binary outcomes. Fisher exact test was used in the event of small numbers. We used Cox proportional hazards models and survival curves to examine the differences between substance use among controls and misusers. For the rating scales, we used logistic regression for the DUSI and the ACDS and ordered logistic regression for the Q-LES-Q. To determine whether sex affected the relationship between misusers and the endorsement of psychiatric disorders and substance use disorder, we included the interaction term misuse status by sex in all models. If the interaction was not significant, we removed it from the analyses and collapsed the results; if it was significant, we reported the results by sex. All statistical analyses were conducted using Stata 12.0. All tests were 2-tailed, with an α level set at .05 unless noted otherwise. Data are presented as mean ± SD unless otherwise specified.
RESULTS
Clinical Characteristics of the Sample
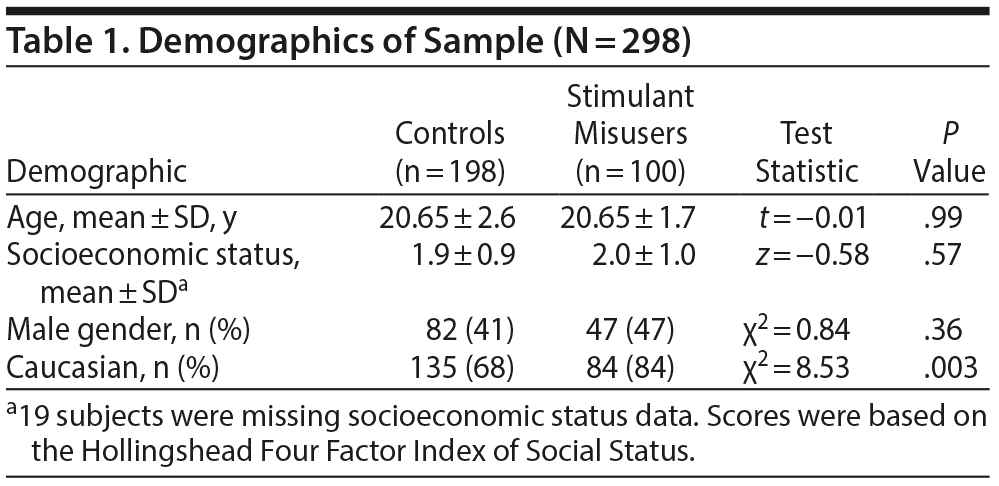
Two controls were dropped a priori because of inconsistent data after it was determined through the assessment questionnaires that they had potentially misused stimulants; therefore, our final sample included 100 misusers and 198 controls (N = 298). There were no significant differences between misusers and controls in age, socioeconomic status, or gender (Table 1). We did find, however, that misusers were more likely to be white than controls (P = .003). As a result, we adjusted for race across all analyses.
Psychopathology
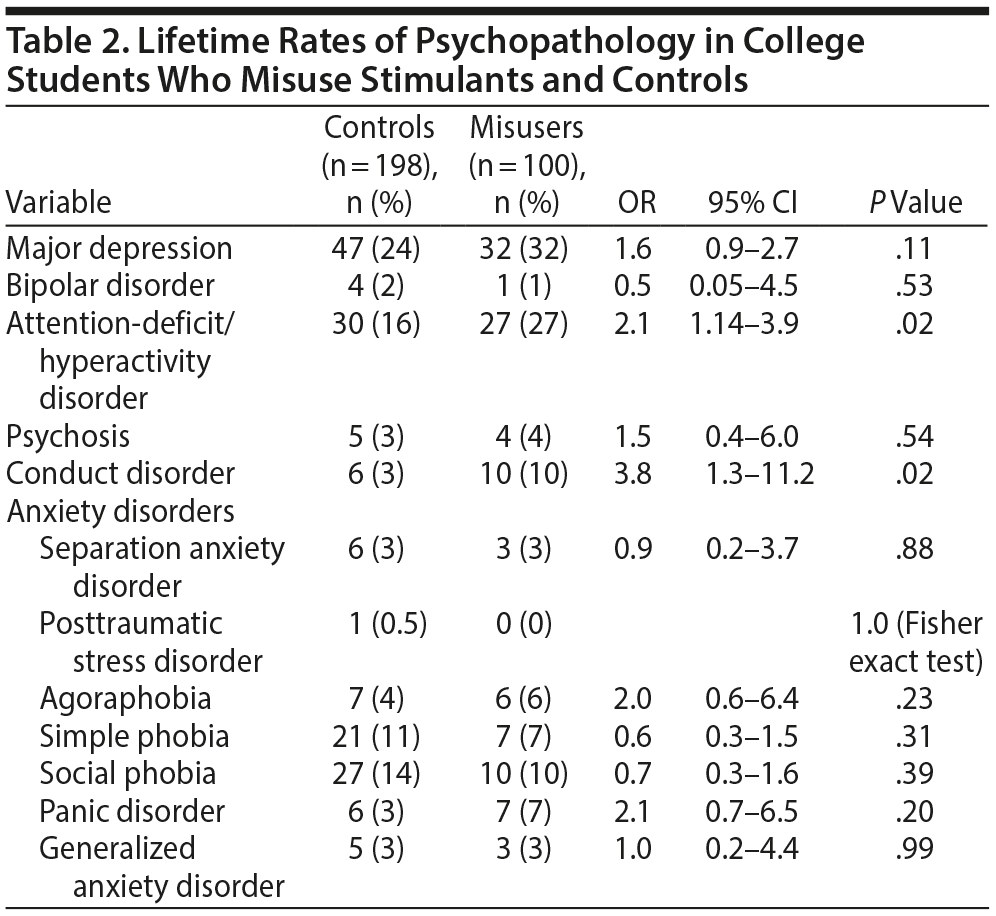
As seen in Table 2, misusers compared to controls were more likely to endorse ADHD (n=27 [27%] vs n=30 [16%]; P = .02) and conduct disorder (n=10 [10%] vs n=6 [3%]; P = .02) when adjusting for race and sex. Also, for lifetime GAF, we found that misusers were more likely to have impairment than controls (56.7 ± 7.6 vs 62.1 ± 8.7; β = −5.3; 95% CI, −7.4 to −3.3; P < .01), when adjusting for race and sex.
The status-by-sex interaction term was found to be significant for misuse status and multiple anxiety disorders (P = .03); male misusers were more likely to endorse multiple anxiety disorders than male controls (OR = 16.8; 95% CI, 1.7 to 170.4; P = .02). There was no significant difference between female misusers and controls in the endorsement of multiple anxiety disorders (OR = 0.60, 95% CI, 0.19 to 1.96; P = .40). There were no significant differences between misusers and controls in the endorsement of any other disorder.
We examined specific ratings on the ACDS. After adjusting for race and sex, misusers were more likely than controls to report moderate to severe difficulty sustaining attention (P = .007), being easily distracted (P = .02), and not listening (P = .04) during childhood. Similarly, misusers were more likely to report moderate to severe difficulty following instructions (P = .02) and dislike for tasks that require attention during adulthood (P = .01). Misusers were more likely to report an onset of ADHD prior to age 7 years (P = .04), the presence of significant and sufficient current ADHD symptoms (P = .02), and the symptoms as primarily due to ADHD and not another mental health disorder (P = .02).
Substance Use Disorder
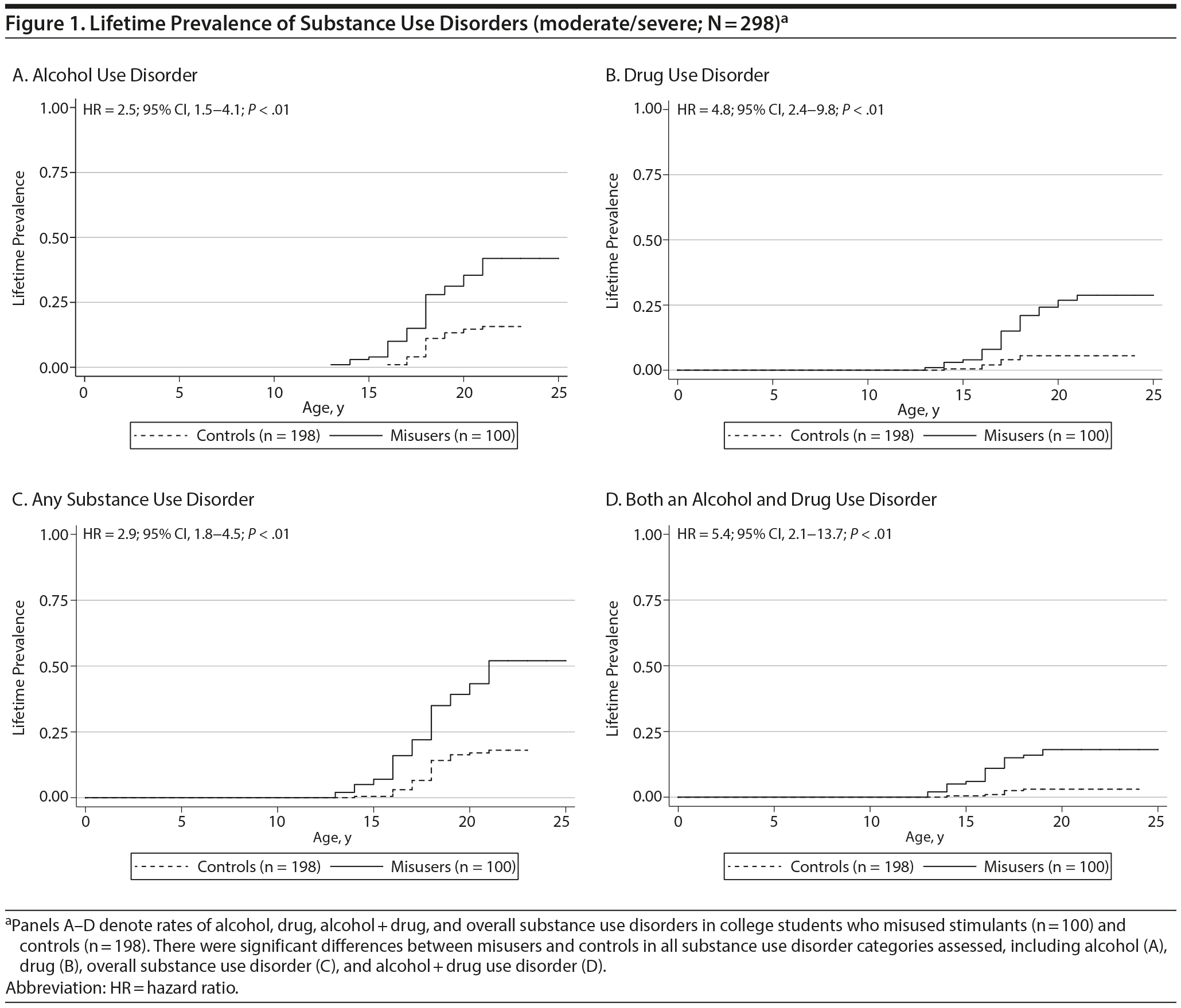
We found that stimulant misusers were more likely than controls to report having an alcohol, drug, alcohol + drug, or overall substance use disorder (all P values < .01, Figure 1A-D). Stimulant misusers were 2.9 times more likely to manifest a substance use disorder compared to controls (P < .01). Additionally, stimulant misusers were 5.4 times more likely than controls to report having a combined alcohol plus drug use disorder (P < .01). We further examined a subset of our misuse group; among those who were administered the updated version of the structured psychiatric interview20 (n = 58), which queried for prescription stimulant misuse specifically, we found that, overall, 67% (n = 39) met criteria for threshold or subthreshold stimulant use disorder, with 9% (n = 5) meeting a full (stimulant other than cocaine or methamphetamine) stimulant use disorder and 58% (n = 34) a subthreshold diagnosis of a stimulant use disorder (ie, abuse or dependence of prescription stimulants).
Stimulant Preparation Misused
On the basis of the self-report MGH ADHD Medication Misuse and Diversion Assessment, stimulant misusers reported that they bought or traded the ADHD medication from any of the following individuals (not mutually exclusive): friend (n = 84; 84%), family member (n = 8; 8%), acquaintance (n = 27; 27%), stranger (n = 1; 1%), or someone not listed (n = 1, 1%). Stimulant misusers were more likely to use, purchase, and/or trade immediate-release (76%) compared to extended-release (58%) ADHD medication (not mutually exclusive). Among those who had met criteria for a full or subthreshold diagnosis of a stimulant misuse disorder (n = 39), we found 51% (n = 20) were using mixed amphetamine salts-immediate release, 31% (n = 12) could not recall the specific stimulant, 10% (n = 4) reported immediate-release methylphenidate, and 8% (n = 3) used immediate-release dextroamphetamine. No subject with a stimulant use disorder endorsed misusing/abusing an extended-release stimulant.
Drug Use Screening Inventory
We had fully completed DUSI reports on 233 subjects. When adjustment was made for race and sex, misusers compared to controls endorsed significantly higher rates of initiating use of their preferred drug to “get high” (73% vs 39%; OR = 4.1; 95% CI, 2.3 to 7.4; P < .01) or to “sleep better” (19% vs 6%; OR = 4.2; 95% CI, 1.7 to 10.3; P = .002). Misusers also reported continued use of their preferred drug to “get high” (73% vs 41%; OR = 3.9; 95% CI, 2.1 to 7.0; P < .01) or to “sleep better” (23% vs 12%; OR = 2.4; 95% CI, 1.1 to 5.0; P = .02). When adjustment was made for race and sex on the Q-LES-Q, misusers were more likely than controls to report a lower “overall sense of well-being” (β = −0.5; 95% CI, −0.9 to −0.004; P = .048).
DISCUSSION
The results of this study partially support our hypotheses that stimulant misusers, compared to controls, are at higher risk for ADHD and/or multiple drug and alcohol use disorders. In this study, stimulant misusers were also more likely to have a poorer quality of life relative to controls. These data add to the existing literature highlighting the elevated risk for ADHD and multiple substance use disorders in those with stimulant misuse. Accordingly, college students who misuse stimulants should be carefully screened for ADHD and substance use disorder.
Our use of structured psychiatric interviews to quantify the prevalence of ADHD and stimulant abuse among misusers represents a different means of data collection compared to more standard survey studies. However, our results are remarkably consistent with survey studies that intimate high rates of ADHD and likely self-medication in samples of stimulant misusers. For instance, the almost 2-fold higher risk for ADHD among stimulant misusers is consistent with Upadhyaha et al,30 who showed increased risk for ADHD symptoms in college-aged stimulant misusers. Similarly, Rabiner et al31 found that students who did not endorse frequent substance use, but endorsed severe attention problems, were 5-times more likely to have an onset of nonmedical use of stimulants between freshman and sophomore year of college compared to those that did not endorse attention problems. Some misusers may be driven to use stimulants in an effort to achieve better grades, increase productivity, and self-treat their threshold or subthreshold ADHD, which are motivations not typically associated with the abuse of alcohol or other drugs. Given that stimulants are used to treat ADHD and executive functioning deficits, and that “self-medication” of executive dysfunctioning has been purported in stimulant misusers,32,33 further analyses examining clinical and objective evidence of neuropsychological and executive functioning deficits in this population are necessary.
We found that nearly half of stimulant misusers manifest a substance use disorder. Most commonly reported were alcohol, marijuana, and then “prescription” stimulants. Moreover, a disproportionate rate of combined drug plus alcohol use disorders were found in stimulant misusers compared to controls. The high rates of substance use disorder are consistent with other studies.5,12,13,34,35 For instance, in a series of well-conducted longitudinal analyses, Arria et al35 also showed that the onset of substance use disorder appears to precede stimulant misuse. The speculation can be made that substance use disorder resulted in academic decline, which prompted ancillary stimulant misuse to improve academic performance in already failing college students.
It may be that stimulant misusers with substance use disorder have a more pernicious use disorder; for instance, our data predominately show that stimulant misusers endorsed the use of alcohol and drugs for euphoria. In contrast, subjects in other samples of similarly aged individuals predominately endorsed continued drug and alcohol use for attenuation of mood, sleep, or other reasons, but not for euphoria as in the current study.14 These DUSI-derived self-report data, coupled with the finding of a substantially higher risk for combined drug plus alcohol use disorders in stimulant misusers, suggest that stimulant misusers may manifest not only a higher risk but a more severe form of substance use disorder relative to controls.
In previous studies of college students who use stimulants nonmedically, the rates of substance use disorders remain largely uncharted. In the current study, our data show that, among misusers who answered interview questions about prescription stimulants specifically (n = 58), a majority (67%) endorsed either a full or a subthreshold stimulant use disorder—indicating that the nonmedical use of stimulants is not necessarily a single episode and may be associated with a separate substance use disorder that necessitates identification, referral, and treatment. In fact, stimulant use disorders may require an entirely unique classification, as the behaviors and causalities may be entirely unrelated to other substance use disorders. Regardless, given the high rates of substance use disorder in our groups, college students who misuse stimulants should be systematically screened for alcohol, stimulant, and other substance use disorders.
There has been speculation about the differential abuse liabilities of immediate- and extended-release stimulants.36 In our entire group of misusers, over three-quarters reported misusing the immediate-release preparations. Moreover, among those with a stimulant use disorder, the vast majority reported misusing the immediate-release stimulant preparations, while approximately one-quarter were unaware of the specific preparation, and no individual specifically endorsed using extended-release preparations. Our current data add to the stimulant human abuse liability literature37,38 highlighting that immediate-release stimulants appear to be misused at higher rates than extended-release preparations in groups of college students. Besides the various differences in pharmacokinetics, the significantly lower cost of immediate-release stimulants39 may also play a role in increasing the ease and likelihood of procurement for misuse. Accordingly, our study further supports the notion of utilizing extended- and not immediate-release stimulants in high-risk groups such as college-aged individuals.36
The current study has a number of methodological limitations. Our students were derived from the metropolitan Boston area and may not generalize to other regions. While the overall sample size was modest (N = 298), the cell sizes in specific groups were relatively small, thus limiting our power. We utilized structured interviews for substance use disorder instead of biological testing, which may have underestimated the actual prevalence. Since we relied on self-report for some of our measures, our subjects may not have completed their questionnaires fully and/or may have underreported their pathology. While we attempted to utilize descriptions, pictures, and brand and generic names of the various stimulants, our data were limited to our subjects’ recollection of the preparations they had misused. Our data are cross-sectional, and as such, are associative in nature.
Despite these methodological shortcomings, the aggregate of high rates of ADHD, substance use disorder including stimulant use disorders, and a lower quality of life indicate that college students who misuse prescription stimulants are clearly struggling. Our data suggest a preponderance of misuse of immediate- relative to extended-release stimulants. Added to previous calls for college health professionals to screen for stimulant misuse,8,12,40 the current data, in conjunction with recent literature, emphasize the need to further screen those with nonmedical use of stimulants for ADHD, stimulant and other substance use disorder, and overall dysfunction.
Submitted: September 30, 2015; accepted October 12, 2015.
Drug names: armodafinil (Nuvigil), dextroamphetamine (Dexedrine and others), lisdexamfetamine (Vyvanse), methamphetamine (Desoxyn and others), methylphenidate (Ritalin, Aptensio XR, and others), mixed amphetamine salts (Adderall XR others), modafinil (Provigil and others).
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Financial disclosure: Dr Wilens receives or has received grant support from National Institutes of Health (NIH) and National Institute on Drug Abuse (NIDA) and Pfizer; is or has been a consultant for Euthymics/Neurovance, NIH, NIDA, Ironshore, Sunovion, Theravance, and Tris Pharma; has authored Straight Talk About Psychiatric Medications for Kids (Guilford Press); has coedited ADHD in Children and Adults (Cambridge Press), and Massachusetts General Hospital Comprehensive Clinical Psychiatry (Sage); is co-owner of a copyrighted diagnostic questionnaire (Before School Functioning Questionnaire); has a licensing agreement with Ironshore (BSFQ Questionnaire); is Chief, Division of Child and Adolescent Psychiatry and (Co) Director of the Center for Addiction Medicine at Massachusetts General Hospital; and serves as a consultant to the US National Football League (ERM Associates), US Minor/Major League Baseball, Bay Cove Human Services (Clinical Services), and Phoenix House. Dr Yule received grant support from the American Academy of Child and Adolescent Psychiatry Pilot Research Award for Junior Faculty supported by Lilly USA. Dr Anselmo and Mss Zulauf and Martelon and Messrs Morrison, Simon, and Carrellas have no conflict of interest relevant to this article to disclose.
Funding/support: This work was supported by an NIH K24 DA016264 grant to Dr Wilens.
Role of the sponsor: The funding sources had no role in the design and conduct of the study; collection, management, analysis, or interpretation of the data; or preparation, review, or approval of the manuscript.
Previous presentation: This study was accepted or presented at the American Society of Addiction Medicine 45th Annual Meeting; April 10-13, 2014; Orlando, Florida ▪ the American Academy of Child and Adolescent Psychiatry 61st Annual Meeting; October 20-25, 2014; San Diego, California ▪ and the American Academy of Addiction Psychiatry 25th Annual Meeting and Symposium; December 4-7, 2014; Aventura, Florida.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
REFERENCES
1. Weyandt LL, DuPaul G. ADHD in college students. J Atten Disord. 2006;10(1):9-19. PubMed doi:10.1177/1087054705286061
2. Greenhill LL, Pliszka S, Dulcan MK, et al; American Academy of Child and Adolescent Psychiatry. Practice parameter for the use of stimulant medications in the treatment of children, adolescents, and adults. J Am Acad Child Adolesc Psychiatry. 2002;41(suppl):26S-49S. PubMed doi:10.1097/00004583-200202001-00003
3. Wilens TE, Spencer TJ. Understanding attention-deficit/hyperactivity disorder from childhood to adulthood. Postgrad Med. 2010;122(5):97-109. PubMed doi:10.3810/pgm.2010.09.2206
4. Stevens JR, Wilens TE, Stern TA. Using stimulants for attention-deficit/hyperactivity disorder: clinical approaches and challenges. Prim Care Companion CNS Disord. 2013;15(2):doi:10.4088/PCC.12f01472. PubMed doi:10.4088/pcc.12f01472
5. McCabe SE, West BT. Medical and nonmedical use of prescription stimulants: results from a national multicohort study. J Am Acad Child Adolesc Psychiatry. 2013;52(12):1272-1280. PubMed doi:10.1016/j.jaac.2013.09.005
6. McCabe SE, Knight JR, Teter CJ, et al. Non-medical use of prescription stimulants among US college students: prevalence and correlates from a national survey. Addiction. 2005;100(1):96-106. PubMed doi:10.1111/j.1360-0443.2005.00944.x
7. McCabe SE, Teter CJ, Boyd CJ. Medical use, illicit use, and diversion of abusable prescription drugs. J Am Coll Health. 2006;54(5):269-278. PubMed doi:10.3200/JACH.54.5.269-278
8. Teter CJ, McCabe SE, Cranford JA, et al. Prevalence and motives for illicit use of prescription stimulants in an undergraduate student sample. J Am Coll Health. 2005;53(6):253-262. PubMed doi:10.3200/JACH.53.6.253-262
9. Teter CJ, McCabe SE, LaGrange K, et al. Illicit use of specific prescription stimulants among college students: prevalence, motives, and routes of administration. Pharmacotherapy. 2006;26(10):1501-1510. PubMed doi:10.1592/phco.26.10.1501
10. Teter CJ, Falone AE, Cranford JA, et al. Nonmedical use of prescription stimulants and depressed mood among college students: frequency and routes of administration. J Subst Abuse Treat. 2010;38(3):292-298. PubMed doi:10.1016/j.jsat.2010.01.005
11. Garnier-Dykstra LM, Caldeira KM, Vincent KB, et al. Nonmedical use of prescription stimulants during college: four-year trends in exposure opportunity, use, motives, and sources. J Am Coll Health. 2012;60(3):226-234. PubMed doi:10.1080/07448481.2011.589876
12. Arria AM, Caldeira K, O’ Grady KE, et al. Nonmedical use of prescription stimulants among college students: associations with attention-deficit-hyperactivity disorder and polydrug use. Pharmacotherapy. 2008;28(2):156-169. PubMed doi:10.1592/phco.28.2.156
13. Wilens TE, Adler LA, Adams J, et al. Misuse and diversion of stimulants prescribed for ADHD: a systematic review of the literature. J Am Acad Child Adolesc Psychiatry. 2008;47(1):21-31. PubMed doi:10.1097/chi.0b013e31815a56f1
14. Wilens TE, Gignac M, Swezey A, et al. Characteristics of adolescents and young adults with ADHD who divert or misuse their prescribed medications. J Am Acad Child Adolesc Psychiatry. 2006;45(4):408-414. PubMed doi:10.1097/01.chi.0000199027.68828.b3
15. Poulin C. Medical and nonmedical stimulant use among adolescents: from sanctioned to unsanctioned use. CMAJ. 2001;165(8):1039-1044. PubMed
16. Wu LT, Schlenger WE. Psychostimulant dependence in a community sample. Subst Use Misuse. 2003;38(2):221-248. PubMed doi:10.1081/JA-120017246
17. Hall KM, Irwin MM, Bowman KA, et al. Illicit use of prescribed stimulant medication among college students. J Am Coll Health. 2005;53(4):167-174. PubMed doi:10.3200/JACH.53.4.167-174
18. Kessler RC, Adler L, Ames M, et al. The World Health Organization Adult ADHD Self-Report Scale (ASRS): a short screening scale for use in the general population. Psychol Med. 2005;35(2):245-256. PubMed doi:10.1017/S0033291704002892
19. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. Fourth Edition. Washington, DC: American Psychiatric Association Association; 1994.
20. Spitzer MB, Gibbon Mariam RL, Williams J. Structured Clinical Interview for DSM-IV-TR Axis I Disorders, Research Version, Patient Edition. (SCID-I/P). New York, NY: Biometrics Research, New York State Psychiatric Institute; 2002.
21. Ambrosini PJ. Historical development and present status of the Schedule for Affective Disorders and Schizophrenia for School-Age Children (K-SADS). J Am Acad Child Adolesc Psychiatry. 2000;39(1):49-58. PubMed doi:10.1097/00004583-200001000-00016
22. Hong SB, Dwyer D, Kim JW, et al. Subthreshold attention-deficit/hyperactivity disorder is associated with functional impairments across domains: a comprehensive analysis in a large-scale community study. Eur Child Adolesc Psychiatry. 2014;23(8):627-636. PubMed doi:10.1007/s00787-013-0501-z
23. Kessler RC, Green JG, Adler LA, et al. Structure and diagnosis of adult attention-deficit/hyperactivity disorder: analysis of expanded symptom criteria from the Adult ADHD Clinical Diagnostic Scale. Arch Gen Psychiatry. 2010;67(11):1168-1178. PubMed doi:10.1001/archgenpsychiatry.2010.146
24. Endicott J, Nee J, Harrison W, et al. Quality of Life Enjoyment and Satisfaction Questionnaire: a new measure. Psychopharmacol Bull. 1993;29(2):321-326. PubMed
25. Hollingshead AB. Four Factor Index of Social Status. New Haven, CT: Yale University Press; 1975.
26. Hollingshead A, Redlich F. Social Class and Mental Illness. New York, NY: John Wiley and Sons; 1958. doi:10.1037/10645-000
27. Tarter RE, Kirisci L. The Drug Use Screening Inventory for adults: psychometric structure and discriminative sensitivity. Am J Drug Alcohol Abuse. 1997;23(2):207-219. PubMed doi:10.3109/00952999709040942
28. Johnston LD, O’ Malley PM, Bachman JG. Monitoring the Future National Survey Results on Drug Use, 1975-2002. Volume II: College Students and Adults Ages 19-40 (NIH Publication No. 03-5376). Bethesda, MD: National Institute on Drug Abuse; 2003. http://monitoringthefuture.org/pubs/monographs/vol2_2002.pdf
29. Winhusen TM, Lewis DF, Riggs PD, et al. Subjective effects, misuse, and adverse effects of osmotic-release methylphenidate treatment in adolescent substance abusers with attention-deficit/hyperactivity disorder. J Child Adolesc Psychopharmacol. 2011;21(5):455-463. PubMed doi:10.1089/cap.2011.0014
30. Upadhyaya HP, Kroutil LA, Deas D, et al. Stimulant formulation and motivation for nonmedical use of prescription attention-deficit/hyperactivity disorder medications in a college-aged population. Am J Addict. 2010;19(6):569-577. PubMed doi:10.1111/j.1521-0391.2010.00078.x
31. Rabiner DL, Anastopoulos AD, Costello EJ, et al. Predictors of nonmedical ADHD medication use by college students. J Atten Disord. 2010;13(6):640-648. PubMed doi:10.1177/1087054709334505
32. Boyd CJ, McCabe SE, Cranford JA, et al. Adolescents’ motivations to abuse prescription medications. Pediatrics. 2006;118(6):2472-2480. PubMed doi:10.1542/peds.2006-1644
33. Rabiner DL, Anastopoulos AD, Costello EJ, et al. Motives and perceived consequences of nonmedical ADHD medication use by college students: are students treating themselves for attention problems? J Atten Disord. 2009;13(3):259-270. PubMed doi:10.1177/1087054708320399
34. McCabe SE, West BT, Teter CJ, et al. Characteristics associated with the diversion of controlled medications among adolescents. Drug Alcohol Depend. 2011;118(2-3):452-458. PubMed doi:10.1016/j.drugalcdep.2011.05.004
35. Arria AM, Caldeira KM, O’ Grady KE, et al. Drug exposure opportunities and use patterns among college students: results of a longitudinal prospective cohort study. Subst Abus. 2008;29(4):19-38. PubMed doi:10.1080/08897070802418451
36. Wilens TE, Morrison NR. The intersection of attention-deficit/hyperactivity disorder and substance abuse. Curr Opin Psychiatry. 2011;24(4):280-285. PubMed doi:10.1097/YCO.0b013e328345c956
37. Spencer TJ, Abikoff HB, Connor DF, et al. Efficacy and safety of mixed amphetamine salts extended release (adderall XR) in the management of oppositional defiant disorder with or without comorbid attention-deficit/hyperactivity disorder in school-aged children and adolescents: a 4-week, multicenter, randomized, double-blind, parallel-group, placebo-controlled, forced-dose-escalation study. Clin Ther. 2006;28(3):402-418. PubMed doi:10.1016/j.clinthera.2006.03.006
38. Parasrampuria DA, Schoedel KA, Schuller R, et al. Do formulation differences alter abuse liability of methylphenidate? A placebo-controlled, randomized, double-blind, crossover study in recreational drug users. J Clin Psychopharmacol. 2007;27(5):459-467. PubMed doi:10.1097/jcp.0b013e3181515205
39. Barner JC, Khoza S, Oladapo A. ADHD medication use, adherence, persistence and cost among Texas Medicaid children. Curr Med Res Opin. 2011;27(suppl 2):13-22. PubMed doi:10.1185/03007995.2011.603303
40. Arria AM, DuPont RL. Nonmedical prescription stimulant use among college students: why we need to do something and what we need to do. J Addict Dis. 2010;29(4):417-426. PubMed doi:10.1080/10550887.2010.509273
This PDF is free for all visitors!