Olfactory Reference Syndrome as a Subtype of Body Dysmorphic Disorder
To the Editor: Olfactory reference syndrome (ORS) is a putative psychiatric condition whose main symptom is a belief that one emits an offensive body odor that is often noted by other people.1 Although early authors suggested that mental disorders such as schizophrenia, affective disorders, somatoform disorders, and temporal lobe epilepsy should be excluded before a diagnosis of ORS is made,2 other researchers have concluded that this condition may occur as a consequence of different neuropsychiatric conditions.3,4
Even though some authors1 have suggested that all of their ORS patients were hallucinating, the core of the illness is regarded as delusional in DSM-IV-TR, particularly because several patients describe the odor graphically, with secondary illusional or hallucinatory misinterpretations.4 To further complicate the issue, Pryse-Phillips’ 1 ORS patients reported frequent use of deodorant or excessive washing (82%) and unnecessary changing of clothes (68%). Therefore, it is sometimes unclear whether an individual complaining of an “imagined odor” has a hallucinatory or delusional disorder or, in fact, an obsessive-compulsive spectrum disorder.4-6
In this report, our goal was to contribute to the literature by providing a “snapshot” of a number of cases of ORS under treatment in several Brazilian university centers, all systematically evaluated with an assessment package specifically designed to capture the diverse psychopathology and personal history of ORS patients.
Method. Researchers at 7 university psychiatric services that comprise the Brazilian Research Consortium on Obsessive-Compulsive Spectrum Disorders7 were asked to identify and evaluate patients with ORS under treatment in their clinics with an assessment package that included (1) the Olfactory Reference Inventory-Revised, a semistructured interview designed to capture diverse aspects of the psychopathologic and personal history of ORS patients (available from the authors on request); (2) the Yale-Brown Obsessive Compulsive Scale Modified for Olfactory Reference Syndrome (YBOCS-ORS), a 12-item semistructured clinician-rated instrument designed to rate severity of ORS (available from the authors on request); and (3) the Structured Clinical Interview for DSM-IV Axis I Disorders.8 Declaration of Helsinki guidelines were followed, and the research was conducted from December 2004 to December 2006.
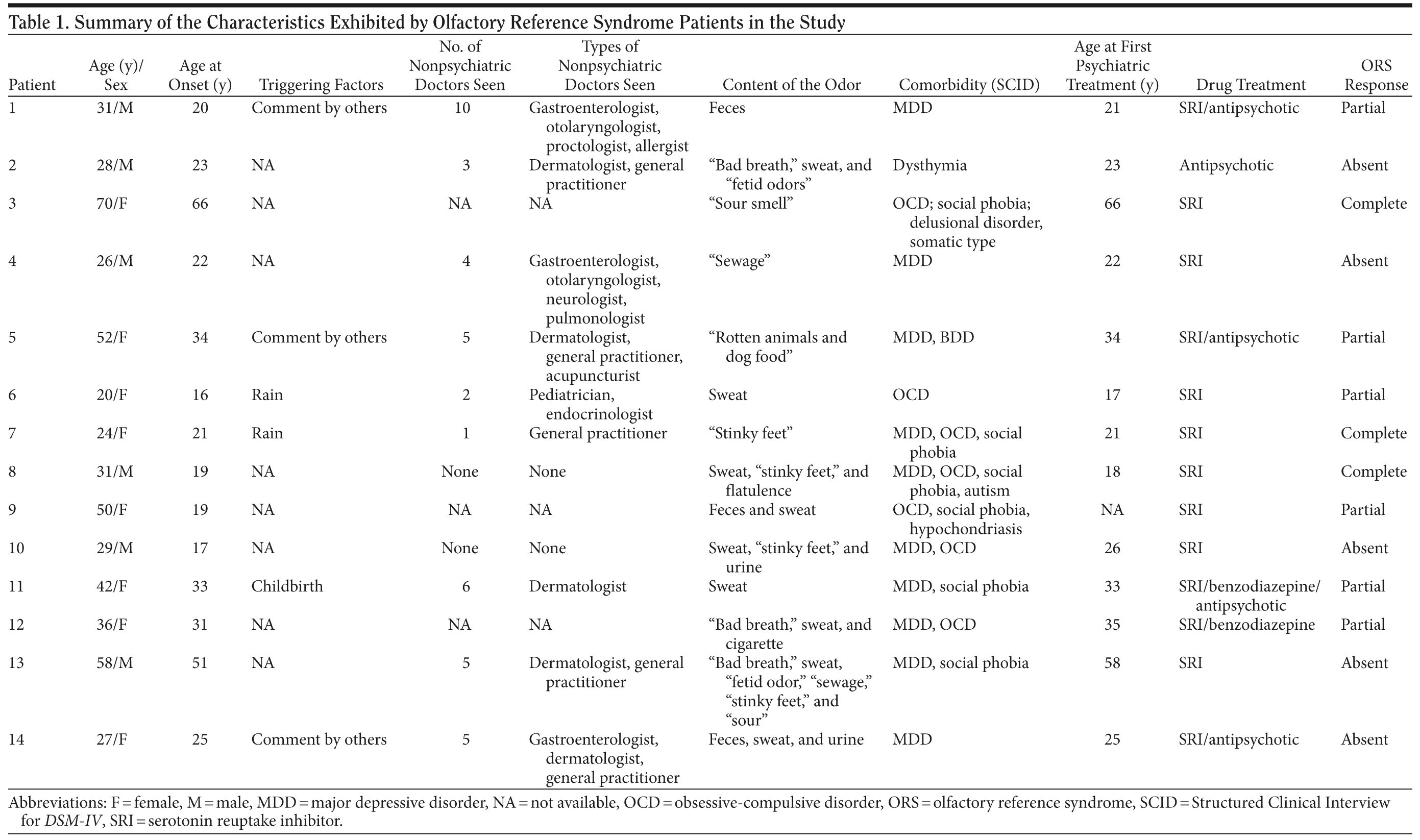
Results. We identified 14 patients with ORS (Table 1). Patients with ORS believe they have a physical problem and often seek evaluation and treatment with nonpsychiatric physicians.4,9-12 In our sample, patients with ORS reported having been seen by a mean ± SD of 4.5 ± 2.8 different nonpsychiatric medical doctors. Indeed, individuals with ORS sought psychiatric treatment a mean of 13.6 ± 10.4 years after the onset of subthreshold symptoms. This finding indicates that it is important to educate physicians on the main features of ORS to facilitate early recognition and avoid unwarranted delays in the treatment of this disorder.
It has been suggested that a single imaginary odor usually predominates as the focus of major concern in patients with ORS.13 In fact, while the most frequent complaint of our ORS sample involved an unpleasant odor of sweat (71.4%; n = 10) emanating from the patient’s armpits (57.1%; n = 8), the majority of the patients reported a significant concern over 2 or more independent unpleasant body odors, a phenomenon that mirrors that found with regard to physical defects in body dysmorphic disorder (BDD).14 Also, some of our patients with ORS reported olfactory experiences that changed in content (28.6%; n = 4) and/or in origin (14.3%; n = 2) over time.
Perhaps because of our selection methods, researchers categorized the olfactory experience as an obsession or overvalued idea in most cases (64.3%; n = 9). Only 21.4% of our sample was characterized as delusional, thus suggesting that it may be inappropriate to classify ORS as a delusional disorder. Further, all patients displayed compulsive rituals, especially excessive washing (64.3%; n = 9); use of exaggerated amounts of deodorant, soap, cologne, or powder (64.3%; n = 9); frequent clothes changing or laundering (57.1%; n = 8); and persistent reassurance seeking (57.1%; n = 8). The mean YBOCS-ORS total score (possible range, 0-40) was 27.7 ± 6.1 (severe). Accordingly, obsessive-compulsive symptoms were often present in the cases previously reported in the literature.1,11,15-19
Major depressive disorder (MDD) and obsessive-compulsive disorder (OCD) were the most common comorbid psychiatric conditions, described in 71.4% (n = 10) and 50.0% (n = 7) of our patients, respectively. The remarkably high prevalence of MDD is consistent with previous reports of patients with ORS.4,20 It must be noted that MDD and OCD were found to be the most common comorbid psychiatric disorders among patients with BDD from different cultures,14,21 thus suggesting that ORS may be a variant of BDD. Unfortunately, because we did not collect data on the age at onset of every psychiatric disorder presented by our patients, we were unable to determine whether the disorders were primary or secondary conditions.
Almost all patients reported a fear of causing disgust (92.9%; n = 13), a phenomenon that has been described as a central feature of the so-called “contrite reaction,” ie, a deeply ashamed, embarrassed, self-abasing, and sensitive reaction to the patient’s own odor.1 Indeed, as Phillips et al13 suggested, the syndrome is sometimes defined in terms that emphasize the fear of offending others—for example, “an anxious fear or conviction that one emits bad odors that offend other persons.”22 The resulting anxiety leads to dysfunctional avoidant behaviors in the social realm, including sitting far from others or moving as little as possible to avoid spreading the supposed odor.11,19,22 In our sample, avoidance behaviors were rated at least as severe in 57.1% of the cases, a phenomenon also known to occur in BDD.
The suffering resulting from ORS has been reported to lead to suicidal ideation,4,11 suicidal behavior,10,17,23,24 and even completed suicide.25 Lifetime suicidal ideation was reported by 64.3% (n = 9) of our ORS patients, and past suicidal behavior was endorsed by 21.4% (n = 3). These rates of suicidal ideation and behavior were closer to those reported by North American (78% and 28%, respectively)26 and British outpatients with BDD (24% with a history of suicidal behavior)27 and higher than those exhibited by Pryse-Phillips’ ORS patients, who described either suicidal ideation or suicidal behavior in 43% of cases.1 Although we were unable to establish whether these symptoms could be specifically ascribed to ORS, we suggest that the latter condition could at the very minimum foster the morbidity among our patients.
Since ORS often goes undiagnosed in different clinical settings, there is a need for better recognition of this disorder. This would enable clinicians to provide appropriate clinical monitoring and treatment of these high-risk patients.13
Although available data on treatment are still limited, published case series support the use of a serotonin reuptake inhibitor (SRI), as a beneficial effect was reported in 10 of 15 (67%) cases.13 Accordingly, all of our patients with ORS were treated naturalistically with an SRI, either alone or in association with an antipsychotic (35.7%; n = 5). Furthermore, we found that 6 of 7 ORS patients with OCD were rated as at least partial responders, while 4 of 7 patients without OCD were rated as nonresponders, thus suggesting that identifying the pattern of comorbidity of ORS patients may have considerable impact on treatment decisions, with good response to an SRI seen in patients with ORS plus OCD.
Our study has some significant limitations. First, we enrolled only a small convenience number of patients, who were assessed by different examiners with a limited number of instruments. Yet, one should take into consideration that this is a remarkably rare disorder that could only be investigated due to the existence of a national research consortium whose researchers exhibited quite satisfactory interrater reliability.7 Second, the high prevalence of OCD-like features in our sample of patients with ORS could be ascribed to an ascertainment bias; that is, since these volunteers were recruited in university clinics specialized in OCD, it would be expected to find several cases with obsessive-compulsive symptoms. Nevertheless, it should be emphasized that comorbid OCD was much less common than comorbid MDD, as it was found in only half of the sample. Although we could not rule out the occurrence of ascertainment bias, the latter observation suggests that this phenomenon may not be as significant as initially thought.
To unveil the proper nosologic position of ORS, further clinical, follow-up, family, and psychobiological studies should carefully investigate the role of ORS, either as a subtype of another OCD spectrum disorder (eg, BDD) or as a specifier of OCD.
References
1. Pryse-Phillips W. An olfactory reference syndrome. Acta Psychiatr Scand. 1971;47(4):484-509. PubMed doi:10.1111/j.1600-0447.1971.tb03705.x
2. Toone BK. Psychomotor seizures, arterio-venous malformation and the olfactory reference syndrome. A case report. Acta Psychiatr Scand. 1978;58(1):61-66. PubMed doi:10.1111/j.1600-0447.1978.tb06921.x
3. Luckhaus C, Jacob C, Zıelasek J, et al. Olfactory reference syndrome manifests in a variety of psychiatric disorders. Int J Psychiatry Clin Pract. 2003;7(1):41-44. doi:10.1080/13651500310001059
4. Malasi TH, el-Hilu SM, Mirza IA, et al. Olfactory delusional syndrome with various aetiologies. Br J Psychiatry. 1990;156(2):256-260. PubMed doi:10.1192/bjp.156.2.256
5. Fontenelle LF, Lopes AP, Borges MC, et al. Auditory, visual, tactile, olfactory, and bodily hallucinations in patients with obsessive-compulsive disorder. CNS Spectr. 2008;13(2):125-130. PubMed
6. Bizamcer AN, Dubin WR, Hayburn B. Olfactory reference syndrome. Psychosomatics. 2008;49(1):77-81. PubMed doi:10.1176/appi.psy.49.1.77
7. Miguel EC, Ferr×£o YA, Rosário MC, et al. The Brazilian Research Consortium on Obsessive-Compulsive Spectrum Disorders: recruitment, assessment instruments, methods for the development of multicenter collaborative studies and preliminary results. Rev Bras Psiquiatr. 2008;30(3):185-196. PubMed doi:10.1590/S1516-44462008000300003
8. Del-Ben CM, Vilela JAA, Crippa JAS. Confiabilidade da “Entrevista Cl×nica Estruturada para o DSM-IV – Vers×£o Cl×nica” traduzida para o português. Rev Bras Psiquiatr. 2001;23(3):156-159. doi:10.1590/S1516-44462001000300008
9. Osman AA. Monosymptomatic hypochondriacal psychosis in developing countries. Br J Psychiatry. 1991;159(3):428-431. PubMed doi:10.1192/bjp.159.3.428
10. Davidson M, Mukherjee S. Progression of olfactory reference syndrome to mania: a case report. Am J Psychiatry. 1982;139(12):1623-1624. PubMed
11. Bishop ER Jr. An olfactory reference syndrome—monosymptomatic hypochondriasis. J Clin Psychiatry. 1980;41(2):57-59. PubMed
12. Iwu CO, Akpata O. Delusional halitosis. Review of the literature and analysis of 32 cases. Br Dent J. 1990;168(7):294-296. PubMed
13. Phillips KA, Gunderson C, Gruber U, et al. Delusions of body malodour: the olfactory reference syndrome. In: Brewer W, Castle D, Pantelis C, eds. Olfaction and the Brain. Cambridge, UK: Cambridge University Press; 2006:334-353.
14. Fontenelle LF, Telles LL, Nazar BP, et al. A sociodemographic, phenomenological, and long-term follow-up study of patients with body dysmorphic disorder in Brazil. Int J Psychiatry Med. 2006;36(2):243-259. PubMed doi:10.2190/B6XM-HLHQ-7X6C-8GC0
15. Stein DJ, Le Roux L, Bouwer C, et al. Is olfactory reference syndrome an obsessive-compulsive spectrum disorder? two cases and a discussion. J Neuropsychiatry Clin Neurosci. 1998;10(1):96-99. PubMed
16. Singh GP. Is olfactory reference syndrome an OCD? Indian J Psychiatry. 2006;48:201-202.
17. Ross CA, Siddiqui AR, Matas M. DSM-III: problems in diagnosis of paranoia and obsessive-compulsive disorder. Can J Psychiatry. 1987;32(2):146-148. PubMed
18. Brotman AW, Jenike MA. Monosymptomatic hypochondriasis treated with tricyclic antidepressants. Am J Psychiatry. 1984;141(12):1608-1609. PubMed
19. Marks I, Mishan J. Dysmorphophobic avoidance with disturbed bodily perception. A pilot study of exposure therapy. Br J Psychiatry. 1988;152(5):674-678. PubMed doi:10.1192/bjp.152.5.674
20. Alvarez WC. Practical Leads to Puzzling Diagnoses. Philadelphia, PA: JB Lippincott; 1958.
21. Phillips KA, Menard W, Fay C, et al. Demographic characteristics, phenomenology, comorbidity, and family history in 200 individuals with body dysmorphic disorder. Psychosomatics. 2005;46(4):317-325. PubMed doi:10.1176/appi.psy.46.4.317
22. Bourgeois M, Paty J. [Autodysosmophobia and the psychopathology of smell (a propos of 7 cases)]. Bord Med. 1972;5(17):2269-2286. PubMed
23. Beary MD, Cobb JP. Solitary psychosis—three cases of monosymptomatic delusion of alimentary stench treated with behavioural psychotherapy. Br J Psychiatry. 1981;138(1):64-66. PubMed doi:10.1192/bjp.138.1.64
24. Johanson E. Mild paranoia. Acta Psychiatr Scand. 1964;40(suppl 180):180:171. PubMed
25. Videbech T. Chronic olfactory paranoid syndromes. A contribution to the psychopathology of the sense of smell. Acta Psychiatr Scand. 1966;42(2):183-213. PubMed doi:10.1111/j.1600-0447.1966.tb01924.x
26. Phillips KA, Coles ME, Menard W, et al. Suicidal ideation and suicide attempts in body dysmorphic disorder. J Clin Psychiatry. 2005;66(6): 717-725. PubMed
27. Veale D, Boocock A, Gournay K, et al. Body dysmorphic disorder. A survey of fifty cases. Br J Psychiatry. 1996;169(2):196-201. PubMed doi:10.1192/bjp.169.2.196
Author affiliations: Anxiety and Depression Research Program, Institute of Psychiatry, Universidade Federal do Rio de Janeiro (IPUB/UFRJ), Rio de Janeiro (Drs Prazeres, Fontenelle, and Mendlowicz); Department of Psychiatry and Mental Health, Institute of Community Health, Universidade Federal Fluminense (MSM/UFF), Niterói (Drs Fontenelle and Mendlowicz); Department of Psychiatry, University of São Paulo Medical School (FMUSP), São Paulo (Drs de Mathis, Ferr×£o, de Brito, Diniz, and Miguel); Department of Psychiatry and Medical Psychology, São Paulo Medical School, Universidade Federal de São Paulo (EPM-UNIFESP), São Paulo (Dr Gonzalez); University Hospital, Universidade Federal da Bahia (UFBA), Salvador (Dr Quarantini); Department of Psychiatry, Universidade Estadual de Londrina (UEL), Londrina (Dr Marrocos), Brazil. Potential conflicts of interest: None reported. Funding/ support: This work was supported by a grant from the National Council for Scientific and Technological Development (CNPq/Brazil) (process number: 420.122/2005-2 – Instituto do Milênio).
doi:10.4088/JCP.09l05040
© Copyright 2010 Physicians Postgraduate Press, Inc.