ABSTRACT
Objective: During the perinatal period, women are at an increased risk for the onset/exacerbation of obsessive-compulsive disorder (OCD) and may experience perinatal-specific obsessions and/or compulsions. Past research has provided preliminary findings regarding the prevalence of OCD in the perinatal period but has often reported limited metrics and ignored perinatal specific symptoms. This research aimed to assess the prevalence and incidence of maternal OCD between the third trimester in pregnancy and 6 months postpartum.
Methods: An unselected sample of 763 English-speaking pregnant women and new mothers participated in a longitudinal, province-wide study between their third trimester in pregnancy and 9 months postpartum. They completed 3 online questionnaires and interviews (data collected between February 9, 2014, and February 14, 2017) and were administered a diagnostic interview to determine OCD status based on DSM-5 diagnostic criteria.
Results: A weighted prenatal period prevalence of 7.8% and a postpartum period prevalence of 16.9% were found. The average, prenatal, point prevalence estimate was 2.9%, and the average, postpartum, point prevalence estimate was 7.0%. Point prevalence gradually increased over the course of pregnancy and the early postpartum, attaining a peak of close to 9% at approximately 8 weeks postpartum, with a gradual decline thereafter. The cumulative incidence of new OCD diagnoses was estimated at 9% by 6 months postpartum.
Conclusions: Our study suggests that when women are encouraged to report their perinatal-specific symptoms, and current diagnostic criteria are applied, estimates for perinatal OCD may be higher than previously believed.
J Clin Psychiatry 2021;82(2):20m13398
To cite: Fairbrother N, Collardeau F, Albert AYK, et al. High prevalence and incidence of obsessive-compulsive disorder among women across pregnancy and the postpartum. J Clin Psychiatry. 2021;82(2):20m13398.
To share: https://doi.org/10.4088/JCP.20m13398
© Copyright 2021 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry/Island Medical Program, University of British Columbia, Victoria, Canada
bDepartment of Psychology, University of Victoria, Victoria, Canada
cWomen’s Health Research Institute, BC Women’s Hospital & Health Centre, Vancouver, Canada
dDepartment of Health Service and Population Research, King’s College London, London, United Kingdom
eDepartment of Family Practice, University of British Columbia, Vancouver, Canada
fDepartment of Psychology, University of British Columbia, Vancouver, Canada
gSchool of Population and Public Health, University of British Columbia, Vancouver, Canada
*Corresponding author: Nichole Fairbrother, PhD, Room 002, Pearkes Bldg, Queen Alexandra Centre for Children’s Health, 2400 Arbutus Rd, Victoria, BC V8N 1V7, Canada ([email protected]).
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
CME Background
Articles are selected for credit designation based on an assessment of the educational needs of CME participants, with the purpose of providing readers with a curriculum of CME articles on a variety of topics throughout each volume. Activities are planned using a process that links identified needs with desired results.
To obtain credit, read the article, correctly answer the questions in the Posttest, and complete the Evaluation. This activity is free.
CME Objective
After studying this article, you should be able to:
- Provide effective screening and assessment for perinatal obsessive-compulsive disorder
Accreditation Statement
The CME Institute of Physicians Postgraduate Press, Inc., is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians.
Credit Designation
The CME Institute of Physicians Postgraduate Press, Inc., designates this journal-based CME activity for a maximum of 1 AMA PRA Category 1 Credit™. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Note: The American Nurses Credentialing Center (ANCC) and the American Academy of Physician Assistants (AAPA) accept certificates of participation for educational activities certified for AMA PRA Category 1 Credit™ from organizations accredited by the ACCME.
Release, Expiration, and Review Dates
This educational activity was published in March 2021 and is eligible for AMA PRA Category 1 Credit™ through April 30, 2023. The latest review of this material was March 2021.
Financial Disclosure
All individuals in a position to influence the content of this activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past year, Marlene P. Freeman, MD, Editor in Chief, has received research funding from JayMac and Sage; has been a member of the advisory boards for Otsuka, Alkermes, and Sunovion; and has been a member of the Independent Data Safety and Monitoring Committee for Janssen. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure appears at the end of the article.
See letter by di Giacomo et al and reply by Fairbrother and Collardeau
Obsessive-compulsive disorder (OCD) is an anxiety-related condition of particular importance for perinatal women due to strong evidence of an increased risk of onset and exacerbation during reproduction.1 OCD is characterized by obsessions (recurrent, unwanted, and distressing thoughts, images, or impulses) or compulsions (repetitive mental or behavioral acts) and is associated with high levels of distress and impairment.2,3 Among perinatal women, the content of obsessions often involves infant-related harm.1,4 Compulsions are less common and often involve checking and reassurance seeking.4 Perinatal OCD has negative implications for fetal, newborn, and infant health and, in the postpartum period, interferes with parenting, relationship functioning, and daily living.5–9
Although harming obsessions are common among women who suffer from postpartum OCD, and are not associated with a risk of behaving violently, many primary care providers are unaware of this and may struggle to differentiate perinatal OCD from psychosis. Consequently, there is an assumption that all infant-related harming ideation represents a risk to infant safety.10,11 Harming obsessions are often not queried during perinatal OCD assessments, and, worse, anecdotal reports of child removals are not unheard of.12 Consequently, perinatal women experiencing OCD characterized by harming obsessions are fearful of child removal and are consequently less likely to seek care.12 Improving our understanding of the prevalence and course of perinatal OCD will improve targeting of resources for prevention, screening, and treatment.
A recent meta-analysis provides the most up to date and valid estimates of perinatal OCD prevalence (2.3% in pregnancy, 1.7% postpartum, and 2.2% overall) and includes all available studies in which high quality methodology was employed.13 Of the 16 included studies, 15 employed DSM-IV diagnostic criteria, and none used DSM-5. Only 1 of the included studies examined the course of OCD across multiple time-points.14 None reported perinatal OCD incidence, cumulative incidence, or week-by-week point prevalence estimates. Further, only 1 of the reported studies provided OCD period prevalence estimates for the whole of pregnancy and the postpartum.15 However, that evaluation did not include perinatal-specific questions and was not based on DSM-5 diagnostic criteria.
Beyond the very limited reporting of prevalence/incidence metrics in previous research, and the need for a perinatal OCD prevalence/incidence study based on DSM-5 diagnostic criteria, there is also a very strong need to include perinatal-specific obsessive-compulsive (OC) symptoms in OCD diagnostic assessments. While some women who experience OCD during the perinatal period report exclusively non–perinatal-related obsessions and compulsions, as noted above, perinatal OCD is often characterized by infant-related obsessional content (thoughts, images, and impulses). Frequently, this ideation involves some form of harm to the infant (eg, contamination that may harm the infant, harm as a result of parental distraction or neglect, unwanted images or thoughts of behaving sexually with the infant, or unwanted thoughts of harming the infant on purpose). While standard OC assessment asks about unwanted, intrusive thoughts involving germs, dirt, ordering and arranging, violence, harm, and sexuality, perinatal women appear not to interpret these questions to include any intrusions related to their infant. In our experience studying perinatal OCD, when only traditional, non–perinatal-specific questions are asked during OCD assessment (in particular, questions about obsessional content), perinatal women (including those who are experiencing high levels of infant-related intrusive ideation) frequently fail to report their infant-related obsessions because they fail to recognize that this is what is being asked about. Consequently, OCD assessments that fail to include questions about perinatal-specific symptoms (in particular questions about infant-related obsessional content and the impact of OC symptoms on one’s parenting as well as other aspects of functioning) may underestimate maternal perinatal OCD prevalence. Only 1 of the perinatal OCD prevalence/incidence studies included in the most recent meta-analysis queried perinatal-specific obsessions and compulsions, and none asked as specifically and thoroughly about obsessions of infant-related harm as was done in the current study.16
The current study provides the most detailed assessment of perinatal OCD epidemiology to date. Specifically, we address the above gaps in the literature by employing DSM-5 diagnostic criteria, incorporating a detailed assessment of obsessions of infant-related harm and corresponding compulsions into diagnostic assessments and reporting on the (a) point prevalence of OCD from the third trimester of pregnancy to 25 weeks postpartum, (b) period prevalence of OCD in pregnancy and the postpartum, and (c) incidence of OCD in the postpartum period in a representative sample of English-speaking Canadian women.
METHODS
The current report of findings is part of a larger study. A detailed complete study protocol is available in BMC Psychiatry.17,18
Ethics
Ethics approval for this province-wide study was granted by all relevant research ethics boards. Participants provided written informed consent at the initial prenatal assessment. Due to the sensitive nature of the research questions, consent was repeated at the first postpartum assessment. Upon completion of participation, the study debriefing form was sent to participants.
Participants
Seven hundred sixty-three English-speaking women living in the Province of British Columbia, Canada (BC) participated in this longitudinal study. Of these, a subset of 580 completed 1 or more diagnostic interviews, and their data form the basis of this report of findings. Data were collected from February 9, 2014, until February 14, 2017.
Procedures
We employed a range of recruitment strategies, including hospital-based recruitment, community-based recruitment, and rurally focused approaches, to maximize sample representativeness. Direct recruitment methods were used in 8 hospitals across BC, and indirect recruitment methods were used in an additional hospital, as well as private clinics, trade shows, community events, and prenatal centers across the province. Women could express interest about the study in person, via phone, or via e-mail. They could elect to complete all the questionnaires online (most participants) or to have paper questionnaires sent to their home.
Women completed online questionnaires and a telephone interview in late pregnancy (mean = 36.89 weeks, SD = 1.96) and twice postpartum (mean = 9.09 weeks, SD = 1.94; and mean = 21.27 weeks, SD = 3.83). Participants were followed from late pregnancy to a maximum of 38 weeks postpartum. The earliest that a participant completed the initial, prenatal interview was 32 weeks gestation. The latest completion dates for the second postpartum interview were at 38 weeks postpartum. Participants who missed the late pregnancy or the early postpartum questionnaires completed a short demographics questionnaire and were eligible to complete later assessments. Of the 580 participants, 270 provided data for all 3 interviews; 182 provided data for 2 of the 3 interviews, and 122 provided data for 1 interview only. Diagnostic data were collected retrospectively for a number of participants who missed the interview in pregnancy (n = 101) and in the early postpartum (n = 49).
Diagnostic interviews. The Structured Clinical Interview for DSM-5 (SCID-5)19 is a structured diagnostic interview for DSM-5 that was used to assess OCD. Similar to previous versions, the SCID-5 is psychometrically sound.20 All interviewers were trained to a strict criterion by the principal investigator (see Collardeau et al18 for details). Symptom severity was rated on a 0 (none) to 8 (very severe/disabling) scale, using the following descriptors: absent (0), subclinical (3 to 3.5), full diagnostic criteria (4 to 8), and partial (0.5 to 2.5) and full (0) remission. At each interview, participants were asked about current OC symptoms (ie, past 2 weeks). With the exception of the first postpartum interview, participants were also asked to identify the 2-week period (prenatal and postpartum) when their OC symptoms were at their most intense. Diagnostic status and severity ratings were provided for current and most intense time periods. In addition to standard diagnostic questions about obsessions and compulsions, participants were also asked in detail (postpartum only) about infant-related harm thoughts and associated behaviors. Resulting obsessions and compulsions of infant-related harm were then included in the overall evaluation of OCD diagnostic status and severity.
Reliability checks for interviews. Following data collection, reliability checks were completed by a senior interviewer and 2 experts in OCD. Of the interviews with an audio file (81.7% of the total), 25% of those with significant OCD symptomatology (subclinical, clinical, partial remission) were reviewed, whereas 5% with no diagnosis of OCD were reviewed. Interviews were proportionally and randomly sampled from each interviewer and at each time point. The interrater reliability among the 3 raters, based on the intraclass correlation coefficient using a 2-way random effect model for consistency, ranged from 0.75 to 0.98 across the different time points, indicating good to excellent reliability. The lowest interrater reliability occurred for ratings of participants’ most intense period of OCD symptoms since birth at the last interview (all other reliability ratings were above 0.85). The most intense period was slightly more difficult to evaluate due to occasional vagueness and inconsistencies in some participants’ recollections. Participants’ reports on symptoms occurring in the past 2 weeks before the interviews, as well as reports on the most intense period of symptoms during the pregnancy, yielded higher agreement between raters.
Validity check for interviews. To further ensure diagnostic validity, 2 senior members of our team subsequently relistened to 100% of the interviews for which a diagnosis of OCD was given (ie, severity ≥ 4), and an audio file was available. Any discrepancies between the diagnosis or severity rating provided by the original interviewer and that obtained during the relistening were resolved via consultation with our OCD experts. In 5 cases, diagnostic severity was reduced from above threshold for full criteria (ie, severity ≥ 4) to below (ie, subclinical or in partial remission). In 1 case, relistening resulted in an increase in the diagnostic severity rating provided.
Statistical Analyses
All analyses were carried out in R v3.5.3.21
Weighting. To maximize representativeness, we used data weighting based on summary statistics provided to us by Perinatal Services BC22 over the time period of the study. We used a raking procedure23 implemented in the “anesrake” package24 to weight the respondents based on location of delivery (hospital name or home), parity, maternal age, and mode of delivery (vaginal vs cesarean). All subsequent analyses employed these weights to reduce bias associated with frequency discrepancies from the population.
Point prevalence. Due to the potential of a curvilinear relationship between prevalence and time relative to delivery, point prevalence of OCD diagnoses over time from late pregnancy through the postpartum period was estimated using generalized additive mixed modeling (GAMM) with the participant ID as a random effect and survey weights included as implemented in the “mgcv” package.25 GAMMs allow for flexible line fitting and do not impose a specific shape on the curve (eg, linear or polynomial), while still allowing for estimation of the dependent variable, and accounting for auto-correlation. Finally, mixed-effects models use all available data and are not restricted to analysis of those with all 3 interviews. Average point prevalence for the prenatal and postpartum periods was estimated using predictions from the GAMM model in addition to point estimates at 6 weeks prepartum, 10 weeks postpartum, and 20 weeks postpartum.
The outcome of each interview (OCD diagnosis or not) was evaluated with respect to the timing at which the interview occurred. The timing was coded as a function of the infant’s birth. Specifically, the date of each interview was recoded as the number of weeks, prior to or following the infant’s birth, at which it was conducted. We then combined the times of the interviews into a single variable in weeks with time of delivery = 0. For this analysis only, we excluded 92 women who had completed only the 33-week interview as we were unable to accurately calculate the number of weeks pre-delivery without knowing their gestational age at delivery. This left 983 interviews from 488 women.
Using all of the data available, the latest visit occurred at 38 weeks postpartum, while the earliest occurred 12 weeks prior to delivery. Estimates of OCD prevalence from visits greater than 25 weeks postpartum were very uncertain with extremely wide confidence intervals. Therefore, we fit the model excluding the data from 71 visits that occurred after 25 weeks. The model using the full range of data is presented in Supplementary Figure 1.
Period prevalence. Period prevalence of OCD diagnoses was estimated for both the prenatal period (ie, the beginning of pregnancy until the time of the prenatal interview, n = 375) and the postpartum period (ie, from the time of delivery until the time of the second postpartum interview, n = 535). Confidence intervals using survey weights for period prevalence were calculated using the svyciprop function from the “survey” package26,27 for the pregnancy period. Given that women were followed for different lengths of time in the postpartum period, we estimated the period prevalence using a logistic regression with a complementary log-log link offset for person time of follow-up in weeks and survey weights. We also estimated period prevalence for smaller subsets of time (up to 8.8 weeks, and up to 13 weeks postpartum) for comparisons to previous studies by restricting to participants with follow-up within that time frame (n = 49 and n = 87). This mimics what would have happened had we stopped interviewing at those times. However, it does miss some cases where in retrospect women would have indicated OCD symptoms during those time frames but were interviewed at a later time postpartum. Therefore, these are likely underestimates of the true period prevalence.
Postpartum incidence. Postpartum (n = 535) OCD incidence was defined as (a) failing to meet full diagnostic criteria for OCD at any point in the prenatal period and (b) meeting full diagnostic criteria for OCD at some point in the postpartum period. Consequently, postpartum incidence estimates may include some women who reported subclinical OC symptoms prenatally or who had previously (eg, childhood) met full diagnostic criteria for OCD at some earlier time in their life. Cumulative incidence was estimated using Kaplan-Meier curves with survey weighting. Time to diagnosis was defined as the weeks postpartum of diagnosis or censored at the last follow-up date available. Incidence rate was calculated as the number of new diagnoses divided by the total person time of follow-up (defined as weeks postpartum of diagnosis, or censored at the last follow-up date available) using survey weights as implemented in the svyratio function. Incidence rate is reported as number of new cases per 1,000 women per week postpartum. Confidence intervals were calculated using the exact method.
RESULTS
Sample Characteristics and Representativeness
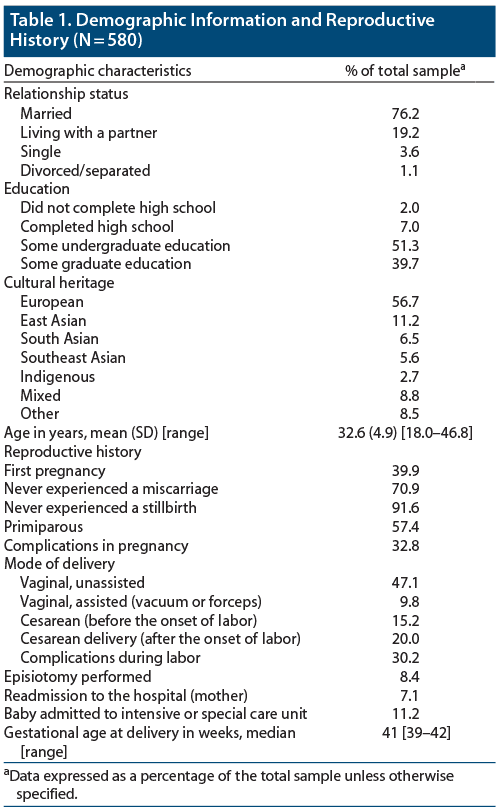
Participant demographic and reproductive history information is provided in Table 1. The current sample differed significantly from the study population with respect to parity (χ21 = 26.9 [N = 133,636], P < .0001), age (χ26 = 28.5 [N = 133,637], P < .0001), and mode of delivery (χ21 = 6.2 [N = 133,600], P = .01). Specifically, our sample contained a greater proportion of nulliparous women compared with Provincial data (55% vs 46%), our participants were slightly older than those in the population (63% vs 58% 30–40 years old), and slightly more women in our sample gave birth via cesarean section (35% vs 33%). No significant differences in birth locations were found. As noted in the data analytic section, data weighting has been used to account for those differences.
Point Prevalence
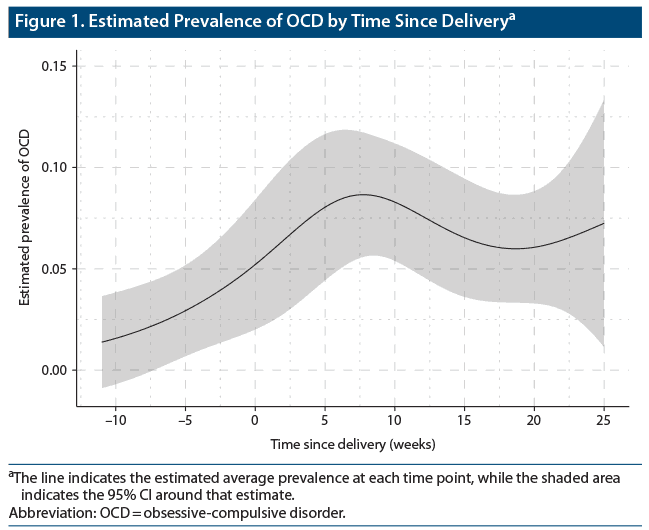
The estimated point prevalence of OCD diagnosis from the model was 2.6% (95% CI 0.4–4.8) at 6 weeks prior to delivery, 8.3% (95% CI 5.4–11.2) at 10 weeks postpartum, and 6.1% (95% CI 3.3–8.8) at 20 weeks postpartum. Looking at the estimates for the interviews prior to 25 weeks postpartum, the regression suggests that there was a steady rise in OCD diagnoses through late pregnancy that peaked at approximately 8 weeks postpartum with an estimated point prevalence of 8.7% (95% CI 5.6–11.7). Thereafter, the probability of OCD diagnoses declined and leveled out (Figure 1). The average point prevalence during the prenatal period was estimated as 2.9% (95% CI 2.7– 3.2), and the average point prevalence during the postpartum period was 7.0% (95% CI 6.9–7.2).
Period Prevalence
For the period prevalence estimates, we had prenatal data from 375 participants and postpartum data from 535 participants. Weighted period prevalence during pregnancy was estimated as 7.8% (95% CI 5.1–12.0). At the beginning of the postpartum period, 93 of 535 women had a diagnosis of OCD. The period prevalence in the entire postpartum period (up to the final postpartum interview at 38 weeks) was estimated using a logistic regression with complementary log-log link and controlling for variable follow-up time as 16.9% (95% CI 14.0–20.2). When we restricted the follow-up time to 8.8 weeks, the period prevalence was 6.9% (95% CI 2.2–20.9), and up to 13 weeks it was 7.8% (95% CI 3.6–16.6).
Incidence of New OCD Diagnoses
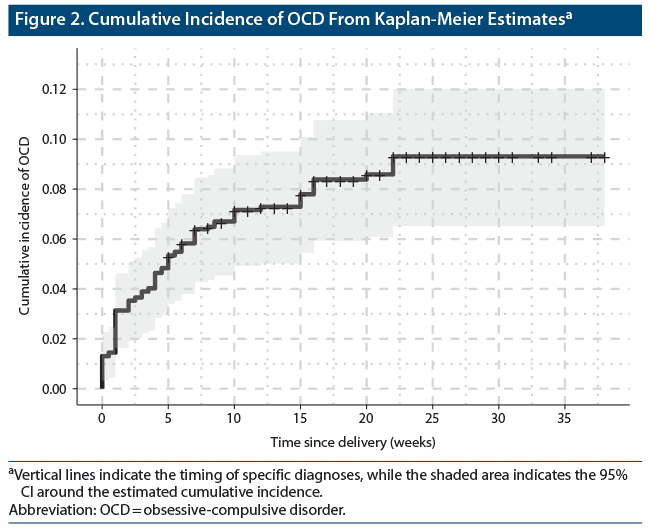
The incidence of new OCD diagnoses was estimated at 4.7 (95% CI 3.2–6.1) new cases per 1,000 women per week postpartum. There were 49 new cases of OCD diagnosed during the postpartum period, with a total person time of follow-up (in weeks) of 9,612. The average person time of follow-up was 18.0 weeks (SD = 7.1 weeks). The cumulative incidence of new cases of OCD was 5% (95% CI 3–6), 6% (4–8), 7% (5–10), and 8% (6–11) for 4, 8, 12, and 16 weeks postpartum, respectively (Figure 2). The total number of observed new diagnoses (n = 49) was reached by 22 weeks postpartum, with the highest rate of new diagnoses occurring within the first 10 weeks postpartum. By 6 months postpartum, the cumulative incidence rose to 9% (95% CI 6–12).
Perinatal Onset of OCD
One hundred women in this study, at some point in the perinatal period, reported symptoms consistent with a diagnosis of OCD. For 60 of these women, clinical levels of OCD began during this pregnancy or postpartum. The remainder reported an onset of symptoms or diagnosis that occurred prior to this most recent pregnancy.
DISCUSSION
In this study of perinatal OCD prevalence and incidence, we provide detailed prevalence estimates and, for the first time, true postpartum incidence and cumulative incidence.
Prenatal and postpartum average prevalence estimates were 2.9% and 7.0%, respectively. Point prevalence gradually increased during pregnancy and the early postpartum, attaining a peak of 8.7% at approximately 8 weeks postpartum, with a gradual decline thereafter. Although our average prenatal point prevalence estimate of 2.9% (95% CI 2.7–3.2) is similar to the point prevalence estimate reported in the most recent meta-analysis (ie, 2.3% [1.1–3.9]), and the confidence intervals overlap, our confidence interval is narrower and based on a smaller time window.13 Our average postpartum point prevalence estimate of 7.0% (95% CI 6.9–7.2) is significantly higher than the 1.7% (0.2–4.3) reported in the most recent meta-analysis, including higher than the 12-week period prevalence estimate (3.6%; 95% CI 1.5–5.7) we reported in our own earlier work.15 The gradual decline in point prevalence across the postpartum suggests that OCD may not be a persistent mental health condition for all of the new mothers who initially meet criteria for this disorder.
We report a prenatal period prevalence of 7.8% (95% CI 5.1–12.0) and a postpartum period prevalence of 16.9% (95% CI 14.0–20.2). To our knowledge, there are no other published studies of prenatal period prevalence. To facilitate comparisons with previous studies of postpartum period prevalence, we also calculated the period prevalence up to 8.8 weeks postpartum (6.9%; 95% CI 2.2–20.9) and up to 13.0 weeks postpartum (7.8%; 95% CI 3.6–16.6). The 2 studies to report on 8.8-week postpartum period prevalence obtained much lower estimates of 1.0% and 2.5%.16,28 In the one study of postpartum period prevalence to 13.0 weeks postpartum (conducted by our team), we also obtained a period prevalence estimate lower than the 7.8% obtained in the current study (ie, 3.4%).15
In the current study, the cumulative incidence of new cases of OCD postpartum was 5% at 1 month postpartum, 6% at 2 months postpartum, and then gradually increased by 1% a month to 9% at 5 months postpartum. Overall, our data suggest that, among perinatal women, the probability of developing OCD in the first 6 months postpartum is approximately 9%.
Both the point and period prevalence estimates in the current study were consistently higher in the postpartum period compared with in pregnancy. Further, each of our estimates are significantly higher than those reported in previous research.13 Because of these differences, we spent a significant amount of time verifying the accuracy of our diagnoses (see details in the Methods section) and considering the reasons for this. In our opinion, our much higher prevalence estimates can be attributed to both a more comprehensive evaluation of perinatal-specific OC symptoms than has previously been undertaken and differences between DSM-IV and DSM-5 diagnostic criteria.29,30
With 1 exception, we are the only group to have included perinatal-specific questions during the diagnostic interview.16 In comparison with the only other study to do this, we included a much more thorough perinatal-related OC assessment process. Specifically, questions about recurrent thoughts and repetitive behaviors were asked twice: once separately from postpartum harm thoughts and once only for postpartum harm thoughts. From there, all other interview questions were asked about non-perinatal and perinatal-specific ideation and behavior combined. In our opinion, this allowed women a greater opportunity to reflect on their infant-related harm thoughts and the OC symptoms related to them. Consequently, symptoms related to perinatal-specific obsessions and compulsions were more likely to be reported and included in the overall assessment of OCD.
Ours is the first study of perinatal OCD prevalence and incidence to employ DSM-5 diagnostic criteria. DSM-5 diagnostic criteria for OCD are significantly less stringent than DSM-IV diagnostic criteria.29,30 Specifically, the DSM-IV criteria for obsessions required that unwanted intrusive ideation (a) cause marked anxiety or distress, (b) be inappropriate in content, and (c) exclude excessive, real life worries. Further, obsessions and compulsions needed to be recognized as excessive or unreasonable. These criteria have been dropped in the DSM-5.
Of relevance to the current study, most unwanted intrusive thoughts (thoughts, images, and impulses) of accidental, infant-related harm would not have qualified as “inappropriate” under DSM-IV. Further, for unwanted intrusive thoughts of both accidental and intentional infant-related harm, obsessional content overlapped significantly with mothers’ current concerns about their infant’s safety. With respect to compulsions, many women in the study failed to perceive their infant-related compulsive behavior as excessive. These changes from the DSM-IV to the DSM-5 likely increase the prevalence of OCD overall, including for perinatal women, as documented in the current study.
Limitations and Future Directions
Study limitations are as follows. Although recruitment mostly occurred during pregnancy, a subset of participants joined the study after childbirth. These women may have been attracted to the study because of their experience of postpartum unwanted, intrusive thoughts. Further, history of OCD prior to participation was collected only for participants who experienced subclinical or clinical OCD symptoms. Thus, we are unfortunately unable to report on the incidence of postpartum OCD separately for participants with and without a previous history of OCD. Given that data were collected in only 1 Canadian province, generalizability of findings to other cultures is limited. Future research should address these limitations and assess our hypothesis that changes in the diagnostic criteria for OCD may have impacted prevalence estimates.
Clinical Implications
Findings from this research reaffirm that perinatal OCD is a prevalent condition, especially in the postpartum period. Point prevalence estimates also suggest that perinatal OCD may naturally resolve over time for some postpartum women. While the higher prevalence and incidence reported in this study may be in part explained by the change in diagnostic criteria from DSM-IV to DSM-5, perinatal women, in particular new mothers, may also fail to recognize their perinatal-specific postpartum OC symptoms in standard OCD assessment interviews. Consequently, diagnostic interviewing for perinatal OCD should be tailored to the specific needs and experiences of perinatal women.
Submitted: April 11, 2020; accepted December 9, 2020.
Published online: March 23, 2021.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents or device therapies that is outside US Food and Drug Administration–approved labeling has been presented in this activity.
Financial disclosure: Drs Fairbrother, Albert, Challacombe, Thordarson, Woody, and Janssen and Ms Collardeau have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: This work was funded by an Operating Grant from the Canadian Institutes of Health Research (CIHR), Ottawa, Canada.
Role of the sponsor: The funding agency (CIHR) reviewed the proposed research in full, prior to funding approval. The funding agency had no further role in the conduct of the study.
Previous presentation: Data from this study on the prevalence and incidence of perinatal OCD were presented at the Canadian Psychological Association’s 2020 Annual National Convention; Montréal, Canada; May 28–30, 2020 (in-person convention cancelled due to COVID-19; may be delivered in online format).
Acknowledgments: The authors thank the study interviewers: Melanie Bennett, BA, University of Victoria; Erinn Doncaster, BSW, University of Victoria; Madeline Nealis, MPH, University of Colorado Boulder; and Sheila Paoli, MA. Each have no conflicts of interest to declare.
Supplementary material: Available at Psychiatrist.com.
Clinical Points
- To date, no studies of perinatal-occurring OCD have (a) been based on DSM-5 criteria; (b) carefully distinguished point prevalence, period prevalence, and incidence; or (c) included much-needed questions about perinatal-specific obsessive-compulsive symptoms.
- Perinatal OCD appears to be significantly more common than previously believed, and clinicians should inquire about perinatal-specific obsessive-compulsive symptoms, in particular obsessions of infant-related harm.
Editor’s Note: We encourage authors to submit papers for consideration as a part of our Focus on Women’s Mental Health section. Please contact Marlene P. Freeman, MD, at [email protected].
References (30)

- Russell EJ, Fawcett JM, Mazmanian D. Risk of obsessive-compulsive disorder in pregnant and postpartum women: a meta-analysis. J Clin Psychiatry. 2013;74(4):377–385. PubMed CrossRef NLM
- Coluccia A, Fagiolini A, Ferretti F, et al. Adult obsessive-compulsive disorder and quality of life outcomes: a systematic review and meta-analysis. Asian J Psychiatr. 2016;22:41–52. PubMed CrossRef NLM
- Stasik SM, Naragon-Gainey K, Chmielewski M, et al. Core OCD symptoms: exploration of specificity and relations with psychopathology. J Anxiety Disord. 2012;26(8):859–870. PubMed CrossRef NLM
- Fairbrother N. Obsessions and compulsions during pregnancy and the postpartum period. In: Wenzel A, ed. The Oxford Handbook of Perinatal Psychology. New York, NY: Oxford University Press; 2016:167–181.
- Brander G, Rydell M, Kuja-Halkola R, et al. Association of perinatal risk factors with obsessive-compulsive disorder: a population-based birth cohort, sibling control study. JAMA Psychiatry. 2016;73(11):1135–1144. PubMed CrossRef NLM
- Coplan RJ, O’Neil K, Arbeau KA. Maternal anxiety during and after pregnancy and infant temperament at three months of age. J Prenat Perinat Psychol Health. 2005;19(3):199–215.
- House SJ, Tripathi SP, Knight BT, et al. Obsessive-compulsive disorder in pregnancy and the postpartum period: course of illness and obstetrical outcome. Arch Women Ment Health. 2016;19(1):3–10. PubMed CrossRef NLM
- Uguz F, Yuksel G, Karsidag C, et al. Birth weight and gestational age in newborns exposed to maternal obsessive-compulsive disorder. Psychiatry Res. 2015;226(1):396–398. PubMed CrossRef NLM
- Challacombe FL, Salkovskis PM, Woolgar M, et al. Parenting and mother-infant interactions in the context of maternal postpartum obsessive-compulsive disorder: effects of obsessional symptoms and mood. Infant Behav Dev. 2016;44:11–20. PubMed CrossRef NLM
- Fairbrother N, Woody SR. New mothers’ thoughts of harm related to the newborn. Arch Women Ment Health. 2008;11(3):221–229. PubMed CrossRef NLM
- Brok EC, Lok P, Oosterbaan DB, et al. Infant-related intrusive thoughts of harm in the postpartum period: a critical review. J Clin Psychiatry. 2017;78(8):e913–e923. PubMed CrossRef NLM
- Challacombe FL, Wroe AL. A hidden problem: consequences of the misdiagnosis of perinatal obsessive-compulsive disorder. Br J Gen Pract. 2013;63(610):275–276. PubMed CrossRef NLM
- Fawcett EJ, Fairbrother N, Cox ML, et al. The prevalence of anxiety disorders during pregnancy and the postpartum period: a multivariate Bayesian meta-analysis. J Clin Psychiatry. 2019;80(4):18r12527. PubMed CrossRef NLM
- Martini J, Knappe S, Beesdo-Baum K, et al. Anxiety disorders before birth and self-perceived distress during pregnancy: associations with maternal depression and obstetric, neonatal and early childhood outcomes. Early Hum Dev. 2010;86(5):305–310. PubMed CrossRef NLM
- Fairbrother N, Janssen P, Antony MM, et al. Perinatal anxiety disorder prevalence and incidence. J Affect Disord. 2016;200:148–155. PubMed CrossRef NLM
- Martini J, Wittich J, Petzoldt J, et al. Maternal anxiety disorders prior to conception, psychopathology during pregnancy and early infants’ development: a prospective-longitudinal study. Arch Women Ment Health. 2013;16(6):549–560. PubMed CrossRef NLM
- Fairbrother N, Young AH, Janssen P, et al. Depression and anxiety during the perinatal period. BMC Psychiatry. 2015;15(1):206. PubMed CrossRef NLM
- Collardeau F, Corbyn B, Abramowitz J, et al. Maternal unwanted and intrusive thoughts of infant-related harm, obsessive-compulsive disorder and depression in the perinatal period: study protocol. BMC Psychiatry. 2019;19(1):94. PubMed CrossRef NLM
- American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
- Shankman SA, Funkhouser CJ, Klein DN, et al. Reliability and validity of severity dimensions of psychopathology assessed using the Structured Clinical Interview for DSM-5 (SCID). Int J Methods Psychiatr Res. 2018;27(1):e1590. PubMed CrossRef NLM
- R: A Language and Environment for Statistical Computing. Vienna, Austria: R Foundation for Statistical Computing; 2019.
- British Columbia Perinatal Data Registry. Perinatal Services BC. February 9, 2014, to February 14, 2017. http://www.perinatalservicesbc.ca/our-services/data-surveillance/perinatal-data-registry/data-requests
- DeBell M, Krosnick JA. Computing Weights for American National Election Study Survey Data. American National Election Studies; 2009. ANES Technical Report series, No. nes012427.
- Pasek J. Anesrake: ANES Raking Implementation. Version 0.80. R; 2018. https://rdrr.io/cran/anesrake/
- Wood SN. Generalized Additive Models: An Introduction With R. 2nd ed. Boca Raton, Florida: Chapman and Hall/CRC; 2017.
- Lumley T. Survey: Analysis of Complex Survey Samples. R package version 3.35-1. R; 2019.
- Lumley T. Analysis of complex survey samples. J Stat Softw. 2004;9(8):1–19. CrossRef
- Wenzel A, Haugen EN, Jackson LC, et al. Anxiety symptoms and disorders at eight weeks postpartum. J Anxiety Disord. 2005;19(3):295–311. PubMed CrossRef NLM
- American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fourth Edition. Washington, DC: American Psychiatric Association; 1994.
- Obsessive-compulsive and related disorders. In: American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
This PDF is free for all visitors!