Psychoeducational Interventions for Family Members of People With Schizophrenia: A Mixed-Method Systematic Review
ABSTRACT
Objective: This systematic review investigates the effectiveness
of psychoeducation in improving the well-being of family members of people with schizophrenia and identifies the common ingredients, implementation considerations, and participants’ feedback.
Data Sources: Published articles in either English or Chinese which reported psychoeducational intervention studies that targeted family members of people with schizophrenia as participants, were searched with the keywords schizophrenia and/or psychosis and psychoeducation/psychoeducational interventions in 8 databases (MEDLINE, PsycINFO, CINAHL, EMBASE, Web of Science, Applied Social Sciences Index and Abstracts [ASSIA], Cochrane Reviews Library, and CENTRAL), from the
time of inception of the various databases to March 2012.
Study Selection: Fifty-eight articles reporting 44 research studies met
all the inclusion criteria and the quality assessment requirement and
were included in the review.
Data Extraction: Data from trials, quantitative studies, and qualitative research were extracted to address 3 parallel syntheses, following the Evidence for Policy and Practice Information Coordination Centre
mixed-method systematic approach.
Results: Psychoeducation was found to be consistently effective in improving family members’ knowledge and coping. However, it was less successful in changing family members’ psychological morbidities, burden, or expressed emotion. Common ingredients across interventions included coverage of common coping strategies and problem-solving strategies to enhance communication or coping. Particularly valued by family carers were a group format to share experiences with other carers, skillful facilitation by professionals, and knowledge and skill development.
Conclusions: This review indicates that psychoeducation should be routinely provided to family members as early as possible following contact with health services. Suggestions are made for optimal psychoeducational intervention design and its successful implementation, and for further research to establish the enhanced effect of booster sessions, between-session practice, and online delivery.
J Clin Psychiatry 2013;74(12):e1145–e1162
© Copyright 2013 Physicians Postgraduate Press, Inc.
Submitted: December 1, 2012; accepted August 6, 2013 (doi:10.4088/JCP.12r08308).
Corresponding author: Jacqueline Sin, MSc, RMN, James Clerk Maxwell Bldg, King’s College London, 57 Waterloo Rd, London SE1 8WA England ([email protected]).
Psychoeducation, that is, information given on a condition and its management,1 is recommended as both an evidence-based and cost-effective treatment for all service users diagnosed with schizophrenia or a related disorder.1,2 A Cochrane review1 of psychoeducation for people with schizophrenia found that it is effective in reducing relapse and readmission and encouraging medication compliance. Families’ involvement in the intervention, with or without service users, is identified as a key factor2; but the effect of psychoeducation on the well-being of the families of people with schizophrenia remains unclear.
Psychoeducational interventions have education as their cardinal feature and prime aim. It is hypothesized that the effectiveness of psychoeducation hinges on the impact of knowledge on stress appraisal and coping and subsequently perceived subjective burden and self-efficacy among family carers,3 an idea that builds upon the theory of stress and coping proposed by Lazarus4,5 in the 1960s. In a family setting of informal caring, improvement in coping and management by family members is believed to be influential in shaping service users’ prognosis and relapse rates; hence, many psychoeducational intervention studies target family members as participants.6–11 Research has also identified increased vulnerability to both physical and mental ill health among family carers,12 in part due to the burden and distress associated with their status as caregivers.13 Effective interventions for family carers are needed.
Family members are often the target participants of psychoeducational interventions.14,15 Some studies have evaluated the impact of the intervention on family members directly by using validated tools, but existing systematic reviews on psychoeducation and family intervention have focused on service users’ outcomes,1,2,16 thus missing the opportunity to identify the effectiveness of psychoeducational interventions for families directly. This systematic review aims to address this knowledge gap by evaluating the effectiveness of psychoeducational interventions in improving the well-being of families of individuals diagnosed with schizophrenia. The review also identifies the common essential ingredients of effective interventions, facilitating factors and barriers to implementation, and the families’ experiences and views of such interventions for their perceived acceptability. The review informs the development of future psychoeducational interventions targeting families directly, which may enhance the benefits of such interventions for service users.
METHOD
This review adopts the mixed-method approach advocated by the Evidence for Policy and Practice Information Coordination Centre,17 which covers a wide remit of relevant literature investigating psychoeducational interventions that target family members of individuals diagnosed with schizophrenia or a related psychotic disorder. Four parallel syntheses using studies with different methods were devised to address specific review objectives and to investigate specific outcomes of interest, as summarized below and in Table 1.
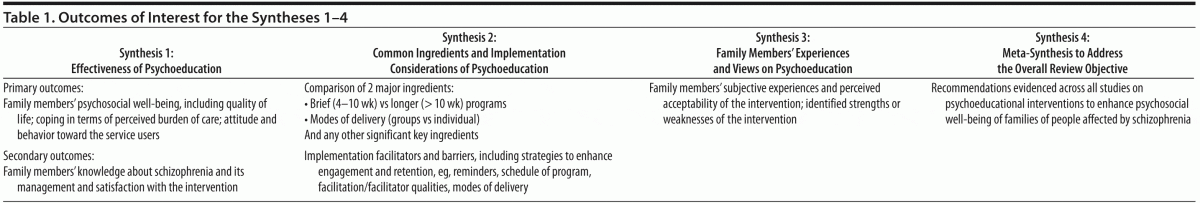
- To investigate the effectiveness of psychoeducational interventions for family members, using experimental and quasi-experimental intervention studies.
- To explore the essential ingredients, enablers, and barriers to implementation of psychoeducational interventions, using intervention studies with quantitative methods, with subgroup analysis focusing on 2 common design variants: brief (4–10 weeks) versus long interventions (more than 10 weeks in duration of programs) and modes of delivery of the intervention.
- To describe the perspectives of family members targeted by the interventions, using qualitative and survey studies.
- To identify the optimal design ingredients and implementation considerations of psychoeducational interventions for family carers by combining the former 3 syntheses using a “meta-synthesis matrix.”
Data Sources, Study Selection, and Data Extraction
The search sought to identify published articles written in either English or Chinese languages that reported research studies in which psychoeducational interventions were received by families/relatives/family members (including parents, siblings, relatives, family caregivers/carers, partners, spouses) who are involved in supporting and caring for a family member with schizophrenia. We used key search terms from the Cochrane Schizophrenia Group and Central Register of Controlled Trials and various synonyms of the keywords schizophrenia and/or psychosis and psychoeducation/psychoeducational interventions, which were used in combination with free text to maximize the sensitivity of the search. Relevant studies were identified through electronic searches of the following databases: MEDLINE, PsycINFO, CINAHL, EMBASE, Cochrane Reviews Library and Cochrane Central Register of Controlled Trials (CENTRAL), and Web of Science and Applied Social Sciences Index and Abstracts (ASSIA). The databases were searched from the time of their inception to March 2012. In addition, the reference lists of all included studies and of relevant existing systematic reviews1,2 were checked for possible studies. Authors of published articles were contacted to retrieve relevant information about their study that was either not reported or unclear from the published article.
Initial screening was undertaken by 1 researcher (J.S.) and then checked by the other (I.J.N.). One researcher (J.S.) extracted the data from the selected studies. The other author (I.J.N.) verified the extracted data and made corrections when necessary. Each study was critically appraised independently by the 2 authors against the Critical Appraisal Skills Program tools for appraising evidence.18 Disagreements were resolved through discussion. Six studies were found to have methodological flaws that rendered the study results unreliable and so were excluded from the review. These studies and other excluded studies are detailed in the Supplementary eTable 1 (available at PSYCHIATRIST.COM) and the overview of studies section.
Data Analysis Strategy
The analysis began with an overview of study characteristics followed by tabulation of extracted data. Meta-analysis of the trials would be considered for synthesis 1, if the studies were sufficiently homogeneous. Otherwise, if considerable heterogeneity between the different studies was identified, the data were to be synthesized using a narrative approach instead. A narrative approach was to be used for syntheses 2 and 3, considering the mixed-method evidence to be reviewed in each. Thematic synthesis was then conducted for each synthesis.17 Finally, meta-synthesis of the design and key ingredients of the intervention underpinning the relationship between the effectiveness of the intervention, any identified implementation-enhancing factors and barriers, and families’ subjective experiences of the intervention was conducted across all quantitative and qualitative data.17
Definition of Key Terms
For the purpose of this systematic review, psychoeducational interventions were conceptualized as interventions with a prime aim to instill information or knowledge on the illness condition and its management.1,2 These psychoeducational interventions included any group or individual program involving interaction between information provider and participants, using different delivery modes, like face-to-face or online support. It is also common that these interventions have multiple components that may consist of, for instance, cognitive and/or behavioral training elements and peer support and/or discussion, with a primary aim of enhancing problem-solving and/or coping with caring-related or illness management issues.1 To qualify as a psychoeducational intervention, the education element had to be significant within the design and be prominent in terms of time duration within the overall content/duration of the multimodal intervention (at least 50% of the total duration) and be professionally led or cofacilitated by a professional. Considering that psychoeducational interventions commonly aim to change complex behaviors and attitudes (eg, coping, psychosocial well-being, self-efficacy), interventions that had a duration shorter than 4 weeks were excluded.2 Brief interventions that focused purely on didactic education or health-information giving using textual or video materials solely were classified as bibliotherapy and were excluded.
RESULTS
Overview of Studies
The search process and total number of articles included and excluded in the review are summarized in Figure 1. In total, 56 articles reporting the results of 41 studies were excluded for the following reasons: poor methodological quality (6 studies), failure to fully meet the inclusion criteria (ie, not meeting definition for intervention, service user, or family member) (31 studies), or reporting no usable data on family members’ outcomes (4 studies). Excluded studies are summarized in Supplementary eTable 1.
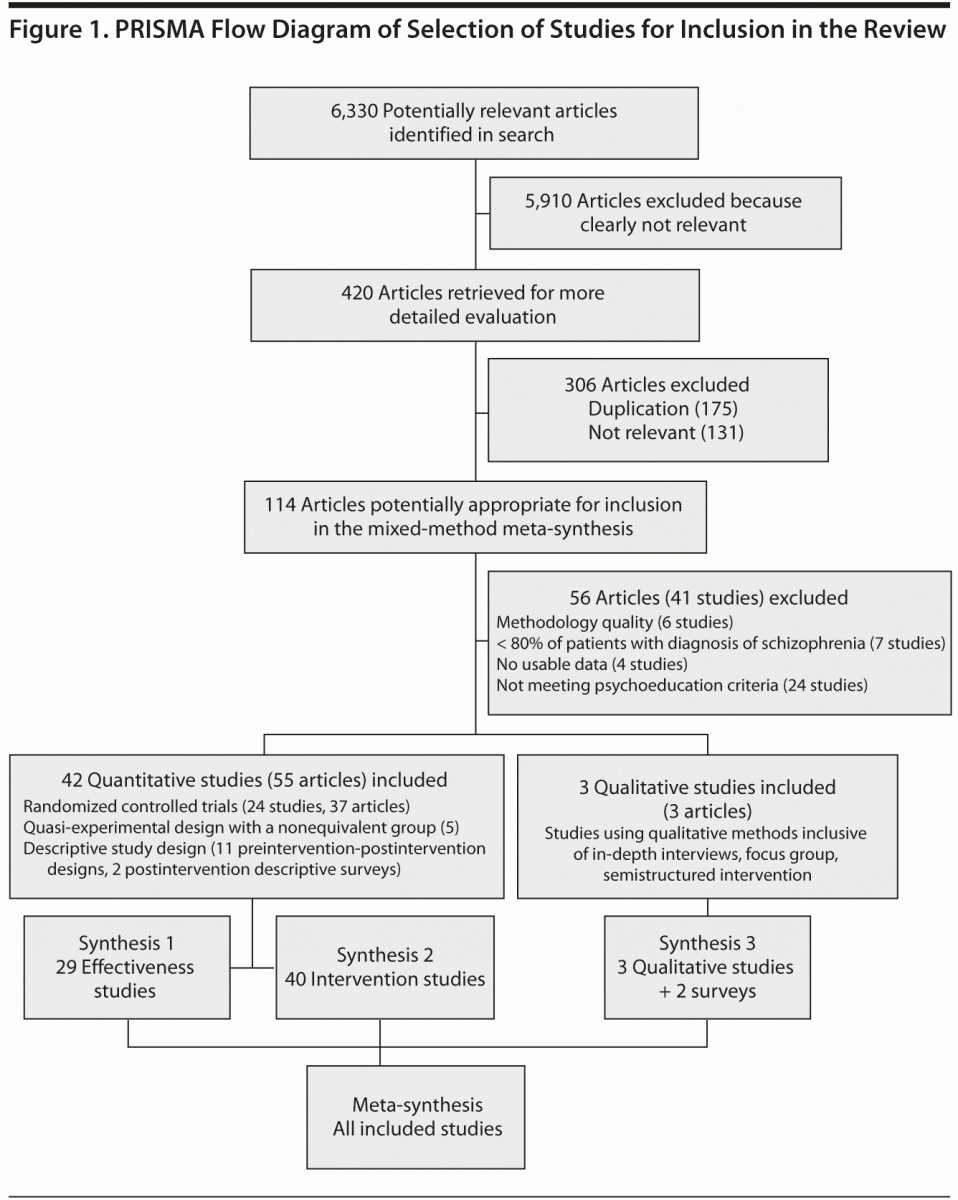
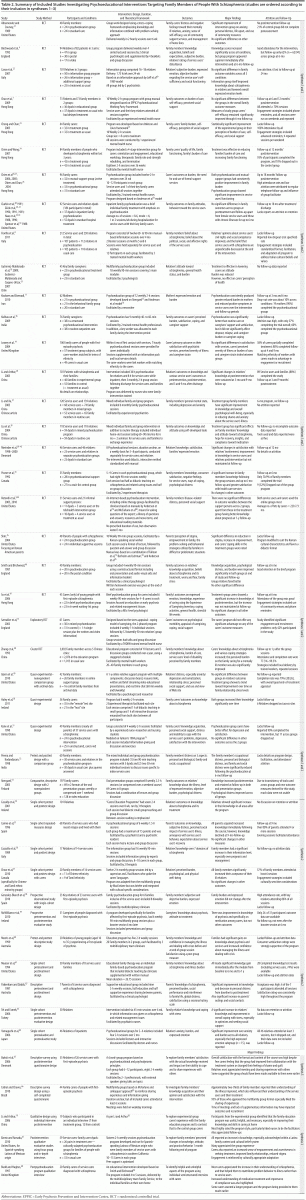
Fifty-eight articles (56 published in English and 2 in Chinese) reporting findings from 44 studies met all the inclusion criteria and the quality assessment requirement18 and were included in the review. These studies originated from North America (10 studies), China (9 studies), United Kingdom (5 studies), Europe (11 studies), Middle East (2 studies), South America (2 studies), Pan-Asia (3 studies), and Australia (2 studies). One study by Li and Arthur19,20 reported findings from both a randomized controlled trial evaluating the effectiveness of psychoeducation on family members, as well as their views on the intervention. Table 2 summarizes the design features of the 44 included studies. Further critique of the quality of the studies is included within each synthesis.
Synthesis 1: Effectiveness of Psychoeducational Intervention
for Family Members
This synthesis of intervention studies included 24 randomized controlled trials and a further 5 trials with quasi-experimental designs (Table 2, references 6–11,14,15, 20–53). The 29 trials originated from China (9 trials; 2 published in Chinese,37,38 7 in English), United States (6 trials), Canada (1 trial), Europe (5 trials), United Kingdom (4 trials), India (2 trials), Chile (1 trial), and Iran (1 trial). Altogether these trials included a total of 6,164 participants: 823 service users, and 5,341 family members of people diagnosed with schizophrenia or related psychotic disorders. The sample sizes in the included studies vary substantially; the smallest study had 40 family carers,46 while the largest study, conducted across 5 cities in China, included 3,092 relatives.48 Across the 29 trials, the mean sample size was 212, while the median sample size was 84.
Only 8 trials (28%) recruited both service users and their key family carers as service user–carer pair participants (dyad).7,8,20,28,37–39,44 Commonly in those studies conducted in Oriental-Asia countries that targeted dyad participants, the service users and their family carers attended the sessions/intervention together.7,20,28,37,38 Other studies arranged separate or parallel sessions/programs for the service users and their families, respectively.8,39,44
Most of the trials (21 of the total of 29, [72%]) recruited family members only as participants, although some of the studies also collected service users’ outcomes, most frequently their general mental state and number of relapses.27,43,47,49 Most of these trials recruited 1 close relative or family member who had key care-giving responsibilities or most contacts with the service users in the study.6,14,15,46 Of the 16 studies that specified the relationships of the participants to the concerned service users, 1 study,11 conducted in Iran, was dedicated to mothers. Two further studies focused on parents as participants: parents in
Ireland50 and American-Korean parents.45 The remaining 13 studies usually had
mothers or parents as the majority of participants, ranging from 60% to 85% of the total participants. Spouses, if included, especially in studies conducted in Oriental-Asian countries such as China and India, were among the second most common participants, ranging from 4% to 32% of the total participants.7,48 Children and siblings of service users were the other 2 most frequently involved family members, although each rarely comprised more than 5% of the total participants on average in most trials.
The earliest research into psychoeducational intervention for families of people diagnosed with schizophrenia dates back to 1987 by Smith and Birchwood46 in the United Kingdom and Abramowitz and Coursey21 in the United States. These early studies explored various formats and modes of delivery and informed the design of these interventions, either on their own or in combination with other therapeutic components within a broader multimodal intervention, such as family intervention.69–71 In the following decade, clinical implementation and research into psychoeducational interventions spread widely to the East.38,48 Indeed, since the late 1990s, studies conducted in China and other non-English speaking countries have started to dominate the published literature. Many of these later studies tend to be bigger in scale and aim to establish psychoeducation as a cost-effective intervention for family carers, building on the findings of earlier studies that developed and established the feasibility of psychoeducation as a discrete intervention.8,48 A high proportion of these later trials also had an additional aim in adapting and modifying the well-established psychoeducation approaches from the United Kingdom or the United States into many non-Caucasian ethnic groups (eg, Korean,45,72 Chinese,20,37 South American Latino,35,66 and Indian36,52).
Despite the long tradition and the few seminal theoretical frameworks underpinning the psychoeducational interventions, as discussed at the outset of this review, only 6 of the 29 trials mentioned the theoretical framework they used in designing the psychoeducational interventions and, hence, the rationale for selection of the primary (and secondary) outcome(s).7,15,22,23,27,51 Among those studies that identified their theoretical base, Carra and colleagues’ study22 cited Leff and colleagues’ (1989) model,69 and Kane and colleagues’ study51 used an intervention that was developed on Falloon’s model of family psychoeducation.73 The few trials conducted in Hong Kong all cited a well-established theoretical model in supporting the development and design of their interventions, including Early Psychosis Prevention and Intervention Centre (EPPIC) Psychoeducational Working Party Framework,74 Atkinson and Coia’s framework,75 and Anderson and colleagues’ model.76 Szmukler and colleagues’ study15 was clear in addressing the family carers’ coping through psychoeducation using Lazarus’ stress appraisal and coping theory.4
The trials included tested the effectiveness of the psychoeducational intervention on family members of people affected by long-term schizophrenia or related disorders, with only 3 studies focused on families of individuals with first-episode psychosis.14,24,47 Altogether, the studies cover a range of care settings, including inpatient,32 community,7,15,26 and cross inpatient-community rehabilitation.20,48
Most of the trials used “standard care” or “treatment as usual” as the comparison to evaluate the effectiveness of psychoeducational interventions (19 of 29 trials, 66%). A few studies compared psychoeducational groups with other modes of delivery using a less intensive format: for example, postal booklet or video (Internet-link).6,46,50,53 Only a handful of studies compared psychoeducation with another active intervention head to head, like a mutual support group that was carer led25–27 or a behavioral family group.36
The outcomes reported across the studies vary a great deal. Most frequently reported primary and/or secondary outcomes are family members’ knowledge (acquisition) of schizophrenia and management of common symptoms. Other frequently reported outcomes are coping, attitude toward the illness or to the service users, perceived burden, expressed emotion, perceived social support, distress and psychological morbidity, and general well-being. Overall, there is substantial heterogeneity across the studies, including variations in the populations, the design and delivery of the interventions, and a wide range of outcome measures being reported. Furthermore, the scales used to measure the variety of outcomes over a range of time points (from 1 day to 2 years following intervention) differ substantially, rendering most results across studies incomparable. For instance, family carers’ well-being has been measured using a number of scales that report either a number of positive direct measures (such as quality of life, mental well-being) or an array of quasi measures of well-being like psychological morbidity (either in a general sense as distress or in specific definitions, as depression or anxiety, fear, and worry). Many of the scales were outcomes of modification or adaptation of validated scales made by the research teams to suit local ethnic needs,36,38 and there are also many examples of invalidated scales generated ad hoc by researchers. This limitation rendered a lot of reported data unusable and findings difficult to generalize outside of the research area. A couple of the trials that tested the efficacy or feasibility of online/Web-based psychoeducational intervention for family carers (and service users as well)9,44,49 focused on usability, retention, and attrition in addition to the outcomes of distress or self-efficacy.
As quantitative data could not be statistically combined for a meta-analysis, extracted outcome data were synthesized into a narrative summary herewith. In terms of effectiveness, most studies that targeted knowledge (acquisition) as a primary or secondary outcome reported significant improvement at end of treatment6,20,23,37–44,47,48 and also at follow-up.6,9,20,23,37,38,43,44 Moreover, perceived self-efficacy or confidence related to coping with the caring situation and problem-solving23,25–27 and satisfaction with the intervention23,39,43 were often found to be positively correlated to increased knowledge. Some studies reported that they successfully enhanced the family members’ perceived social support, especially when the interventions were delivered in a group format,23,24 although increased use of services due to increased knowledge of available resources was also reported.9,15,44,49 However, psychoeducation would seem to have less impact on other outcomes, especially on family carers’ perceived burden, service use, psychological well-being or distress, with a few studies reporting no difference between intervention and comparison groups.7,14,15
Synthesis 2: Common Ingredients and
Implementation Considerations of Effective Psychoeducational Interventions
In addition to the 29 experimental and quasi-experimental trials discussed in synthesis 1, eleven additional quantitative studies using single cohort/within-subject preintervention and postintervention design (5 from Europe, 2 from Australia, 1 from United States, 1 from Canada, 1 from Turkey, and 1 from Japan) were included in a second synthesis (see Table 2, references 54–64) to establish the common ingredients of psychoeducational interventions and implementation considerations. In comparison to the 29 trials, the quality of the 11 quantitative studies included in this second synthesis was weaker overall. The sample size ranged from 7 parents62 to 101 relatives54 (mean = 38, median = 31). All nonexperimental studies, apart from 1 by Canive et al,55 included no follow-up after the completion of the psychoeducational interventions.
The duration of the psychoeducational interventions reported by the 40 quantitative studies ranged from 4 weeks (ie, the minimal duration as inclusion criteria)6,46,51,52 to 12 months.48,49,57 Commonly, interventions lasted between 8 and 36 weeks for 6 to 12 weekly or biweekly sessions.7,15,22,24 Some used a special schedule so that early sessions were delivered more frequently than latter sessions, which were spaced out with longer gaps between sessions.20,38 Programs by McWilliams et al59 and Fiorillo et al8 used booster sessions following a gap from the completion of the main education program.
In terms of formats of delivery, there were 4 main categories: individual, in that a therapist would see a relative or a whole family unit for the intervention14,61; groups, in which relatives would attend sessions together6,7,48; mixed, in that the programs usually would start with a few individual sessions before all relatives were brought together in a support/discussion group15,20; and other, that is, any format or mode that did not fit any of the other 3 categories, such as innovative online delivery that, despite no face-to-face contacts between participants and facilitators, provided both information and peer support through an online discussion forum or virtual groups.9,44,49 Table 3 summarizes all interventions in terms of their duration (brief [4–10 weeks] vs long [> 10 weeks] programs) and specifies the total contact hours and the delivery format of each program.
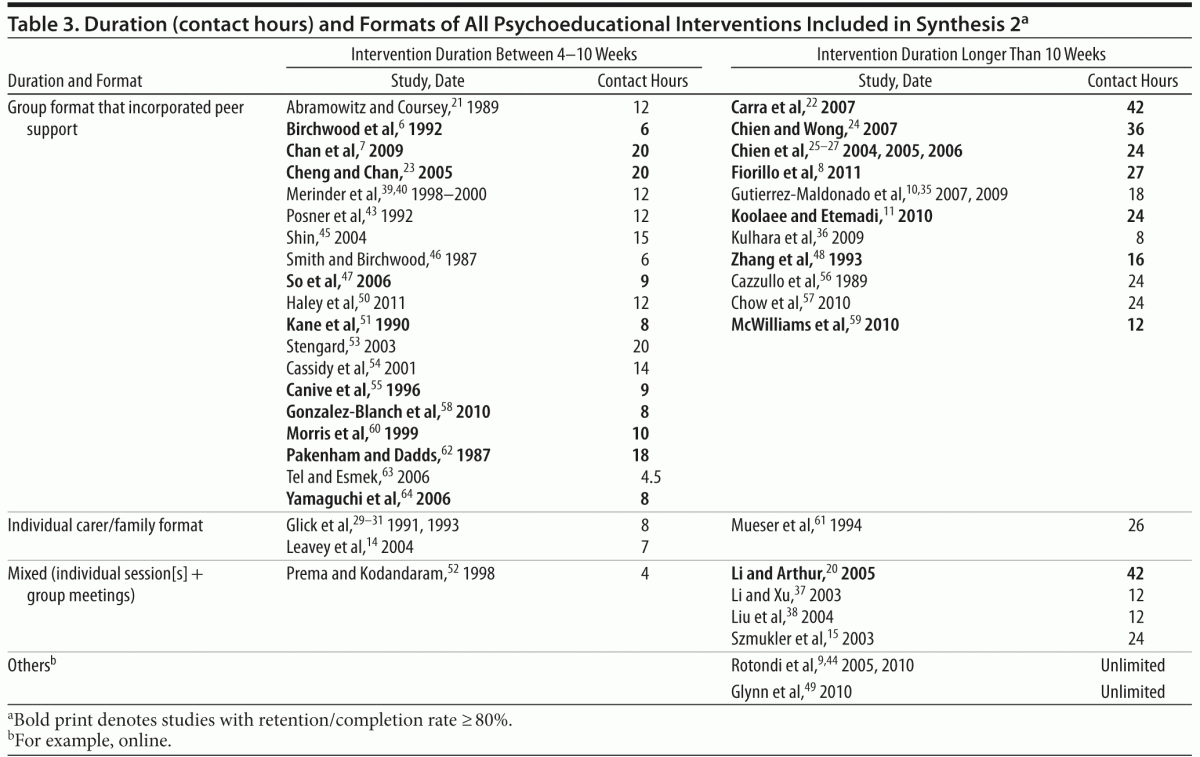
Across all 40 quantitative studies, 15 studies (38%) gave
no data on retention, completion, or attrition explicitly. Of the remainder that reported completion and attrition, 18 studies (45%) reported good completion (≥ 80%) or low attrition (< 20%) and are highlighted in Table 3. Seven studies (17%) reported substantial recruitment, retention, and engagement problems; for instance, Leavey et al14 reported that only 58% of participants partially completed the treatment, and Szmukler et al15 reported a recruitment rate of 42% from all potentially suitable family carers across South London regions.
Subgroup analysis comparing brief (≤ 10 weeks) versus long (> 10 weeks) interventions was inconclusive, although many more studies reported brief rather than long interventions, so limiting the evidence upon which an evaluation could be made. Furthermore, duration of programs may not accurately reflect their intensity in terms of total hours of contact, which also depends on a combination of program design factors, such as the frequency and length of sessions and group size. For instance, while all brief programs were delivered within 10 weeks, most covered 6–12 hours of contact time,6,39,40,46,47,63,64 a minority delivered up to 30 hours of contact.21,23,53,56,57,61 Most longer programs delivered a higher number of contact hours, ranging 24–36 hours.11,24–27, However, some longer programs delivered less frequent sessions and ended up with a small number of contact hours, ranging from 8 to 12 hours.36–38,59 Overall, the contact time of the interventions that have the successful recruitment and retention rate is estimated at 16–18 hours over 8–24 weeks. The studies that have evaluated group programs incorporating a peer support element report them to be popular with families, and recruitment, retention, and completion rates appear to be comparable to those of individual psychoeducation programs (see Table 3).
An array of engagement strategies were used by the studies, with varying degrees of success. These are summarized below:
- Running sessions outside of office hours, including weekends to facilitate attendance by working relatives.7,23,27,47
- Repeating sessions 2 or more times to enhance flexibility for relatives to choose sessions convenient for themselves.7,23,24
- Modifying programs to meet local cultural ethnic preferences: eg, a more didactic format for Korean American parents45; including a Sunday lunch
and meeting in Chinatown for Chinese relatives
in Canada.57 - Reminders in advance of sessions via phone.23,24,47
- Engagement reinforcement between program facilitator(s) and participants by arranging preprogram meetings.15,47
- Matching the ethnicity of the facilitator(s) to the participants.14,45,57
- Conducting sessions in a local neighborhood to enhance convenience of attendance.48,50,57
- Facilitation by experienced mental health workers; for instance, a number of studies specified using experienced mental health nurses with at least 10 years’ postqualifying experience and specific training in running educational groups7,15,20,23,24 and many others were run by experienced clinical psychologists/ researchers.6,46,60
- Provision of computers and online access to the relatives to facilitate their use of the online
support resource.9,44
All psychoeducational interventions reported by the studies shared the cardinal feature of education about schizophrenia and related caring issues. Most programs included coverage of some common coping strategies to help family members communicate with the service users and/or problem-
solve common caring issues more effectively. Among those strategies, problem-solving skills, communication skills, and information on local resources most commonly formed the program content.7,15,24,45,60 The overall program content tended to be delivered in a modular design, with the program spread out over its duration.
The peer support element was commonly emphasized in those programs using a group format. However, none of the studies explicitly discussed the theoretical model used to guide the peer support or group discussion element, if used. If group discussion was included, most programs described it being used to reinforce mutual learning and support among family carers.15,21 Most programs had the peer support/group discussion element scheduled into the later part of the sessions, and discussion focused on the education topics covered in the early part of the sessions6,7,24,59,62 across the program. A few programs completed all the didactic education in the early part of the program before focusing on peer-support group in the latter half of the program.15,20
Between-session practice of skills learned from the sessions was rarely emphasized across programs. Only 2 studies provided a rationale to reinforce between-session learning and practice through reading, quiz, and homework tasks.6,46
Synthesis 3: Family Members’ Experiences and Perceived Acceptability of Psychoeducation
Altogether, 5 studies19,65–68 explored family members’ experiences of receiving psychoeducation and perceived acceptability of the intervention. One study originated from each of the 5 countries: China,19 Brazil,66 United States,67 United Kingdom,68 and Denmark.65 Three used qualitative methods like semistructured interviews and focus groups with participants following the intervention,19,67,68 and 2 used a postintervention questionnaire survey.65,66 Table 2 summarizes these 5 studies.
In general, the family members’ satisfaction reported across the 5 studies in this synthesis was high. Common components of the programs that were repeatedly highlighted and attributed to the high satisfaction included group format that reinforced listening to and sharing of experiences66,67; skillful facilitation by mental health professionals, especially their engaging attitudes toward family carers19,65,67; and psychoeducation being useful and helpful in filling a gap in the knowledge and skills needed by family carers.19,66,68
Although a couple of the programs targeted family members of individuals affected by first-episode psychosis and thus would have recruited the families in an early stage of their involvement with the health care services,65,66 families wanted the provision to be made even earlier. This demand for early psychoeducational intervention for families was echoed in other studies.68 On the contrary, the timing of the sessions and the lack of alternative or additional provision of audio-visual aids or supplementary information to face-to-face didactic presentation were highlighted as detrimental to family members’ satisfaction.66 Sessions run in evenings and weekends were in demand by working relatives.66
When discussing satisfaction and acceptability of such interventions, family members tended to list their perceived benefits as increased knowledge, changed attitude and belief toward the service users and hence modified behavior (eg, lessen criticism toward bizarre behavior or speech by service users), and improved sense of social support and empowerment.19,65,68
Meta-Synthesis: Implications From Literature for the Design of Psychoeducational Interventions
In the overall meta-synthesis, a matrix is developed in which the findings from the parallel syntheses were juxtaposed17 to make recommendations regarding designing and conducting psychoeducational interventions with family members of individuals affected by schizophrenia (Table 4).

Based on this meta-synthesis, the following recommendations are made regarding key ingredients in designing psychoeducational interventions and best practice considerations in delivering such interventions for family members:
- Effective psychoeducational interventions all shared some common features in terms of content: in particular, information on psychosis and its management and coping strategies for family
carers to manage the caring. - Group programs that reinforce participant sharing of experiences, knowledge, and caregiving skills were more successful in engaging and retaining participants than programs that did not.
- Considerations for successful implementation are as important as the program design. Flexible scheduling and skillful facilitation are crucial in engaging with family members and accommodating their other commitments.
- Family members expect and appreciate psychoeducation to increase their knowledge about the illness and its management and, thus, enhance their coping and confidence/self-efficacy in dealing with caring demands.
- Many family members particularly appreciate sharing their experiences with other family carers, finding that it reduced their sense of isolation and enhanced mutual support.
- Families wanted psychoeducation to be provided to them as early as possible, once their family member becomes known to mental health services.
DISCUSSION
The current review of 44 studies across the world over the last 3 decades reflects the wealth of information about and increasing interest in psychoeducational interventions. The relative high number of trials included suggests that psychoeducational interventions are widely researched and popular in clinical practice across different continents.
The major output of this review is recommendations on the design of effective psychoeducational intervention for family members of people affected by schizophrenia, grounded in the evidence from existing quantitative and qualitative studies (see Meta-Synthesis section and Table 4). The findings of the review indicate that psychoeducation should be routinely provided to family members as early as possible following contact with health services. This recommendation echoes the existing and prior reviews in which psychoeducation was recommended to be routinely provided to service users with schizophrenia themselves due to its effectiveness in reducing relapses and promoting compliance with medication.1,2
This review identified specific and direct benefits of psychoeducational interventions for family members. These benefits include increased knowledge, which commonly correlates to better self-perceived coping and/or self-efficacy, and increased sense of social support.6,20,22–24,48 However, a number of direct and positive measures of psychological well-being of family members are reported with an array of quasi measures, including psychological morbidity, negative impact from caring, and more entrenched and in-depth constructs like beliefs and attitude toward the service users and/or illness.7,14,15 The sheer number of different scales used across studies to report these various outcomes presents a challenge to interpretation of results and renders the option of meta-analysis of findings across studies as inappropriate.77
Furthermore, caution is required when interpreting and generalizing the findings of studies reported here, as their participants were largely composed of mothers who had
an adult child affected by long-term schizophrenia. Most of
these mothers would have been in their key caring role for a long time and in their late adulthood (aged 60+ years). It seems possible that a high proportion of these family carers would have developed well-established beliefs about how much psychoeducation might or, more likely, might not change their caring situation, which might, in turn, influence their assessment of change in outcomes like burden, expressed emotion, and psychological morbidity.
Some studies argue that psychoeducational interventions should be used as an initial part of a more complex intervention, like family intervention.69,71 Psychoeducation, given it is well received by families, could then serve to build a baseline knowledge and repertoire of coping strategies in the families as well as help engage them with health care service/professionals in preparation for more intensive intervention. Some researchers6,7,46,70 also suggest that more intensive and complex interventions conducted over a longer period are required to complement psychoeducation and to produce an impact on intricate outcomes like beliefs and behavior toward schizophrenia or the service users with schizophrenia.
Future Research and Clinical Implications
Some common components of successful psychoeducational interventions appear to be well established. However, this review found a number of characteristics to vary across successful programs. The intervention duration and schedules of successful psychoeducational programs vary, with programs ranging from 6 to 42 hours across 4 to 52 weeks. The role and effectiveness of booster sessions, which were sometimes used in programs, are underexplored in previous studies. This review thus falls short of recommending an optimal intervention duration, although the contact time of the successful interventions is estimated at 16–18 hours over 8–24 weeks.
The collective understanding of the role and function of out-of-session practice and that of the group element, within the overall intervention design, remains limited. Only 2 trials investigated the differential effectiveness of out-of-session practice through quiz, exercises, and/or homework tasks,6,46 and neither produced conclusive findings. The lack of attention to this feature is contrary to the ethos of ongoing practice and adoption of skills and knowledge learned in everyday life being core to all psychosocial interventions. Across all group program studies, little was articulated on the theoretical framework or facilitation considerations in terms of the peer support element. Group discussion, sharing personal experiences in caring, and mutual learning were the 3 most commonly noted activities in groups. Otherwise, there was no consensus over the group size6,15,20,48,53 nor group mix considering participants’ gender, length of caring, and any other demographic factors. Nonetheless, given that the group discussion element seems crucial in the effectiveness and engagement of the interventions with the participants, facilitators may wish to pay particular attention to these aspects.
As far back as the late 1980s, psychoeducational programs, especially when delivered in a group format, were proposed as a cost-effective intervention for service users and their families.6,46,69 Nonetheless, research since then appears to have focused on spreading the interventions worldwide, and the feasibility of psychoeducational interventions for families across different settings and cultural ethnic context has been supported by recent studies. Little progress has been made in understanding the best design of the intervention, how the interventions impact or do not impact particular family outcomes, and how these impacts correlate to service users’ outcomes like decreased relapse and better compliance. This dearth of information suggests that future studies should be more congruent and focused in their selection of primary outcome(s) of psychoeducational interventions by using well-validated outcome measurement scales77 that are sensitive to the intervention and reflect its core tenants and theoretical underpinnings, as well as family members’ expectations. In psychiatry, there has been a call for an increased effort to develop and apply agreed standardized sets of outcomes in clinical trials that are of value to all those interested in the results of evaluative studies, similar to the established initiatives such as the Core Outcome Measures for Effectiveness Trials (COMET).77
The majority of the studies included in this review used a face-to-face delivery format, mostly through groups. However, in the last decade, innovative design and delivery formats using online medium have arisen, as evidenced in 2 studies9,44,49 in the United States and 1 study78 in the United Kingdom, supplemented with low-intensity phone and/or e-mail support from mental health workers. While these appeared novel in the mental health field, psychoeducational interventions using online delivery and design have gathered more momentum and evidence in other long-term ill-health conditions (eg, dementia, diabetes, stroke care) worldwide.79,80 Given ever-increasing demands on integrating evolving technologies to enhance accessibility and flexibility of evidence-based interventions,80,81 further development to optimize online design and delivery of psychoeducational interventions for people with schizophrenia and their families would appear to be a worthwhile endeavor.
Limitations of the Review
This review focuses on the outcomes of psychoeducation for family members, rather than service users. But outcomes for family members are invariably reported as secondary outcomes, with those for service users being the primary outcomes, even though in most studies family members alone were the recipients of psychoeducational interventions. The secondary status of family members’ outcomes is a limitation of this review. While family members’ participation in psychoeducation is widely regarded as pivotal, the research targeting family members and reporting outcomes for them is limited, possibly because research that gives primacy to service user outcomes is more attractive to research funders. While the published literature was comprehensively searched for this review, there is also a possibility of publication bias in that studies with negative outcomes for service users (but possibly not for family members) are in the “file drawer.”17,77 Due to limitation of resources of the review team, only English and Chinese articles were considered for inclusion.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration–approved labeling has been presented in this article.
Author affiliations: Florence Nightingale School of Nursing and Midwifery (Dr Norman and Ms Sin), and Institute of Psychiatry (Ms Sin), King’s College London, England.
Financial disclosure: Dr Norman and Ms Sin have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: This review was developed as part of the E Sibling Research Project. Ms Sin is funded by a National Institute for Health Research (NIHR) Doctoral Research Fellowship (NIHR-DRF-2011-129) (United Kingdom).
Disclaimer: This article presents independent research funded by the NIHR. The views expressed are those of the authors and not necessarily those of the NHS, the NIHR, or the Department of Health.
Acknowledgments: The authors thank Karen Poole, MSc, Information Science, Information Specialist—Biomedical and Health Research, King’s College London, for her professional advice and assistance in the systematic search process. Ms Poole has no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Supplementary material: See accompanying pages.
REFERENCES
1. Xia J, Merinder LB, Belgamwar MR. Psychoeducation for schizophrenia. Cochrane Database Syst Rev. 2011;(6):CD002831. PubMed
2. National Institute for Clinical Excellence (NICE). Schizophrenia—The NICE Guideline on Core Interventions in the Treatment and Management of Schizophrenia in Adults in Primary and Secondary Care (Updated Edition). London, UK: The British Psychological Society & The Royal College of Psychiatrists; 2010.
3. Szmukler GI, Herrman H, Colusa S, et al. A controlled trial of a counselling intervention for caregivers of relatives with schizophrenia. Soc Psychiatry Psychiatr Epidemiol. 1996;31:137–148. doi:10.1007/BF00785760
4. Lazarus P, Folkman S. Stress, Appraisal and Coping. New York, NY: Springer Publishing; 1984.
5. Lazarus RS. Psychological Stress and the Coping Process. New York, NY: McGraw-Hill; 1966.
6. Birchwood M, Smith J, Cochrane R. Specific and non-specific effects of educational intervention for families living with schizophrenia: a comparison of three methods. Br J Psychiatry. 1992;160(6):806–814. doi:10.1192/bjp.160.6.806 PubMed
7. Chan SW, Yip B, Tso S, et al. Evaluation of a psychoeducation program for Chinese clients with schizophrenia and their family caregivers. Patient Educ Couns. 2009;75(1):67–76. doi:10.1016/j.pec.2008.08.028 PubMed
8. Fiorillo A, Bassi M, de Girolamo G, et al. The impact of a psychoeducational intervention on family members’ views about schizophrenia: results from the OASIS Italian multi-centre study. Int J Soc Psychiatry. 2011;57(6):596–603. doi:10.1177/0020764010376607 PubMed
9. Rotondi AJ, Haas GL, Anderson CM, et al. A clinical trial to test the feasibility of a telehealth psychoeducational intervention for persons with schizophrenia and their families: intervention and 3-month findings. Rehabil Psychol. 2005;50(4):325–336. doi:10.1037/0090-5550.50.4.325
10. Gutiérrez-Maldonado J, Caqueo-Urízar A, Ferrer-García M. Effects of a psychoeducational intervention program on the attitudes and health perceptions of relatives of patients with schizophrenia. Soc Psychiatry Psychiatr Epidemiol. 2009;44(5):343–348. doi:10.1007/s00127-008-0451-9 PubMed
11. Koolaee AK, Etemadi A. The outcome of family interventions for the mothers of schizophrenia patients in Iran. Int J Soc Psychiatry. 2010;56(6):
634–646. doi:10.1177/0020764009344144 PubMed
12. Department of Health (DOH). Recognised, Valued and Supported: Next Steps for the Carers Strategy. London, UK: HMSO; 2010.
13. Kuipers E, Raune D. The early development of EE and burden in the families of first onset psychosis. In: Birchwood M, Fowler D, eds. Early Intervention in Psychosis: A Guide to Concepts, Evidence and Interventions. Chichester, UK: John Wiley and Sons; 2000:128–140.
14. Leavey G, Gulamhussein S, Papadopoulos C, et al. A randomized controlled trial of a brief intervention for families of patients with a first episode of psychosis. Psychol Med. 2004;34(3):423–431. doi:10.1017/S0033291703001594 PubMed
15. Szmukler G, Kuipers E, Joyce J, et al. An exploratory randomised controlled trial of a support programme for carers of patients with a psychosis. Soc Psychiatry Psychiatr Epidemiol. 2003;38(8):411–418. doi:10.1007/s00127-003-0652-1 PubMed
16. Pharoah F, Mari J, Rathbone J, et al. Family intervention for schizophrenia. Cochrane Database Syst Rev. 2010;(12):CD000088. PubMed
17. Evidence for Policy and Practice Information Co-ordiantion Centre (EPPI-Centre). EPPI-Centre Methods for Conducting Systematic Reviews. London: Institute of Education, University of London; 2010.
18. Critical Appraisal Skills Programme (CASP). CASP critical appraisal checklist. http://www.casp-uk.net/find-appraise-act/appraising-the-evidence/. Accessed July 1, 2013.
19. Li Z, Arthur DG. An education intervention for families of people with schizophrenia in China: development and evaluation. J Psychosoc Nurs Ment Health Serv. 2006;44(2):38–47. PubMed
20. Li Z, Arthur D. Family education for people with schizophrenia in Beijing, China: randomised controlled trial. Br J Psychiatry. 2005;187(4):339–345. doi:10.1192/bjp.187.4.339 PubMed
21. Abramowitz IA, Coursey RD. Impact of an educational support group on family participants who take care of their schizophrenic relatives. J Consult Clin Psychol. 1989;57(2):232–236. doi:10.1037/0022-006X.57.2.232 PubMed
22. Carrà G, Montomoli C, Clerici M, et al. Family interventions for schizophrenia in Italy: randomized controlled trial. Eur Arch Psychiatry
Clin Neurosci. 2007;257(1):23–30. doi:10.1007/s00406-006-0677-z PubMed
23. Cheng L-Y, Chan S. Psychoeducation program for Chinese family carers of members with schizophrenia. West J Nurs Res. 2005;27(5):583–599, comment 600–603. doi:10.1177/0193945905275938 PubMed
24. Chien WT, Wong K-F. A family psychoeducation group program for
Chinese people with schizophrenia in Hong Kong. Psychiatr Serv. 2007;
58(7):1003–1006. doi:10.1176/appi.ps.58.7.1003 PubMed
25. Chien WT, Chan S, Morrissey J, et al. Effectiveness of a mutual support group for families of patients with schizophrenia. J Adv Nurs. 2005;51(6):
595–608. doi:10.1111/j.1365-2648.2005.03545.x PubMed
26. Chien W-T, Chan SWC. One-year follow-up of a multiple-family-group intervention for Chinese families of patients with schizophrenia. Psychiatr Serv. 2004;55(11):1276–1284. doi:10.1176/appi.ps.55.11.1276 PubMed
27. Chien W-T, Chan SW, Thompson DR. Effects of a mutual support group
for families of Chinese people with schizophrenia: 18-month follow-up.
Br J Psychiatry. 2006;189(1):41–49. doi:10.1192/bjp.bp.105.008375 PubMed
28. Clarkin JF, Glick ID, Haas GL, et al, eds. The Effects of Inpatient Family Intervention on Treatment Outcome. Washington, DC: American Psychiatric Press, Inc; 1991.
29. Glick ID, Clarkin JF, Spencer JH Jr, et al. A controlled evaluation of inpatient family intervention, 1: preliminary results of the six-month follow-up. Arch Gen Psychiatry. 1985;42(9):882–886. doi:10.1001/archpsyc.1985.01790320054007 PubMed
30. Glick ID, Spencer JH Jr, Clarkin JF, et al. A randomized clinical trial of inpatient family intervention, 4: follow-up results for subjects with schizophrenia. Schizophr Res. 1990;3(3):187–200. doi:10.1016/0920-9964(90)90036-7 PubMed
31. Glick ID, Clarkin JF, Haas GL, et al. Clinical significance of inpatient family intervention: conclusions from a clinical trial. Hosp Community Psychiatry. 1993;44(9):869–873. PubMed
32. Haas GL, Glick ID, Clarkin JF, et al. Inpatient family intervention: a randomized clinical trial, 2: results at hospital discharge. Arch Gen Psychiatry. 1988;45(3):217–224. doi:10.1001/archpsyc.1988.01800270025003 PubMed
33. Haas GL, Glick ID, Clarkin JF, et al. Gender and schizophrenia outcome:
a clinical trial of an inpatient family intervention. Schizophr Bull. 1990;16(2):
277–292. doi:10.1093/schbul/16.2.277 PubMed
34. Spencer JH Jr, Glick ID, Haas GL, et al. A randomized clinical trial of inpatient family intervention, 3: effects at 6-month and 18-month follow-ups. Am J Psychiatry. 1988;145(9):1115–1121. PubMed
35. Gutiérrez-Maldonado J, Caqueo-Urízar A. Effectiveness of a psycho-educational intervention for reducing burden in Latin American families
of patients with schizophrenia. Qual Life Res. 2007;16(5):739–747. doi:10.1007/s11136-007-9173-9 PubMed
36. Kulhara P, Chakrabarti S, Avasthi A, et al. Psychoeducational intervention for caregivers of Indian patients with schizophrenia: a randomised-controlled trial. Acta Psychiatr Scand. 2009;119(6):472–483. doi:10.1111/j.1600-0447.2008.01304.x PubMed
37. Li FM, Xu JH. Comparative study on the effect of family intervention on schizophrenia patients in convalescence and their family member. Health Psychol. 2003;11(2):129–130.
38. Liu L, Gao CF, Yue SY, et al. Effect of family intervention on rehabilitation
of schizophrenic patients in community. J Nurs Sci. 2004;3(19):3–6.
39. Merinder LB, Viuff AG, Laugesen HD, et al. Patient and relative education
in community psychiatry: a randomized controlled trial regarding its effectiveness. Soc Psychiatry Psychiatr Epidemiol. 1999;34(6):287–294. doi:10.1007/s001270050146 PubMed
40. Merinder LB. Impact of Patient and Relative Education on Knowledge, Satisfaction With Services and Clinical Outcome in Schizophrenia. Aarhus, Denmark: Faculty of Health Sciences, Univeristy of Aarhus; 2000.
41. Merinder LB, Viuff AG, Laugesen H, et al. Effects of psychoeducative methods: a randomised controlled study. Nord J Psychiatry. 1998;41(supplement):144.
42. Merinder LB, Viuff AG, Laugesen HD, et al. Patient and relative education
in community psychiatry: a randomised trial regarding its usefulness. Paper presented at: Proceedings of the 9th Congress of the Association of European Psychiatrists; September 20–24, 1998; Copenhagen, Denmark.
43. Posner CM, Wilson KG, Kral MJ, et al. Family psychoeducational support groups in schizophrenia. Am J Orthopsychiatry. 1992;62(2):206–218. doi:10.1037/h0079337 PubMed
44. Rotondi AJ, Anderson CM, Haas GL, et al. Web-based psychoeducational intervention for persons with schizophrenia and their supporters: one-year outcomes. Psychiatr Serv. 2010;61(11):1099–1105. doi:10.1176/appi.ps.61.11.1099 PubMed
45. Shin S-K. Effects of culturally relevant psychoeducation for Korean American families of persons with chronic mental illness. Res Soc Work Pract. 2004;14(4):231–239. doi:10.1177/1049731503262130
46. Smith JV, Birchwood MJ. Specific and non-specific effects of educational intervention with families living with a schizophrenic relative. Br J Psychiatry. 1987;150(5):645–652. doi:10.1192/bjp.150.5.645 PubMed
47. So H, Chen E, Wong C, et al. Efficacy of brief intervention for carers of people with first-episode psychosis: a waiting list controlled study. Hong Kong J Psychiatry. 2006;16(3):92–100.
48. Zhang M, Yan H, Yao C, et al. Effectiveness of psychoeducation of relatives of schizophrenic patients: a prospective cohort study in five cities of China. Int J Ment Health. 1993;22(1):47–59.
49. Glynn SM, Randolph ET, Garrick T, et al. A proof of concept trial of an online psychoeducational program for relatives of both veterans and civilians living with schizophrenia. Psychiatr Rehabil J. 2010;33(4):278–287. doi:10.2975/33.4.2010.278.287 PubMed
50. Haley C, O’Callaghan E, Hill S, et al. Telepsychiatry and carer education for schizophrenia. Eur Psychiatry. 2011;26(5):302–304. doi:10.1016/j.eurpsy.2009.12.021 PubMed
51. Kane CF, DiMartino E, Jimenez M. A comparison of short-term psychoeducational and support groups for relatives coping with chronic schizophrenia. Arch Psychiatr Nurs. 1990;4(6):343–353. doi:10.1016/0883-9417(90)90024-F PubMed
52. Prema T, Kodandaram P. Impact of mental health education on “distress experience” by the family members of the chronic mentally ill. Indian J Clin Psychol. 1998;25(2):174–177.
53. Stengård E. Educational intervention for the relatives of schizophrenia patients in Finland. Nord J Psychiatry. 2003;57(4):271–277. doi:10.1080/08039480310002093 PubMed
54. Cassidy E, Hill S, O’Callaghan E. Efficacy of a psychoeducational intervention in improving relatives’ knowledge about schizophrenia and reducing rehospitalisation. Eur Psychiatry. 2001;16(8):446–450. doi:10.1016/S0924-9338(01)00605-8 PubMed
55. Cañive JM, Sanz-Fuentenebro J, Vázquez C, et al. Family psychoeducational support groups in Spain: parents’ distress and burden at none-month follow-up. Ann Clin Psychiatry. 1996;8(2):71–79. doi:10.3109/10401239609148804 PubMed
56. Cazzullo CL, Bertrando P, Clerici C, et al. The efficacy of an information group intervention on relatives of schizophrenics. Int J Soc Psychiatry. 1989;35(4):313–323. doi:10.1177/002076408903500403 PubMed
57. Chow W, Law S, Andermann L, et al. Multi-family psycho-education group for assertive community treatment clients and families of culturally diverse background: a pilot study. Community Ment Health J. 2010;46(4):364–371. doi:10.1007/s10597-010-9305-5 PubMed
58. González-Blanch C, Martín-Muñoz V, Pardo-García G, et al. Effects of family psychoeducation on expressed emotion and burden of care in first-episode psychosis: a prospective observational study. Span J Psychol. 2010;13(1):
389–395. doi:10.1017/S1138741600003942 PubMed
59. McWilliams S, Egan P, Jackson D, et al. Caregiver psychoeducation for first-episode psychosis. Eur Psychiatry. 2010;25(1):33–38. doi:10.1016/j.eurpsy.2009.08.006 PubMed
60. Morris E, Harris C, Nolan L. First psychosis liaison unity family education programme. Psychiatrist. 1999;23(4):212–214. doi:10.1192/pb.23.4.212
61. Mueser KT, Gingerich SL, Rosenthal CK. Educational Family Therapy for schizophrenia: a new treatment model for clinical service and research. Schizophr Res. 1994;13(2):99–107. doi:10.1016/0920-9964(94)90090-6 PubMed
62. Pakenham KI, Dadds MR. Family care and schizophrenia: the effects of a supportive educational program on relatives’ personal and social adjustment. Aust N Z J Psychiatry. 1987;21(4):580–590. doi:10.3109/00048678709158927 PubMed
63. Tel H, Esmek M. The effect of education on the approach of relatives to schizophrenia patients and their coping with stress. Neurol Psychiatr Brl 2006;13(1):55–58.
64. Yamaguchi H, Takahashi A, Takano A, et al. Direct effects of short-term psychoeducational intervention for relatives of patients with schizophrenia
in Japan. Psychiatry Clin Neurosci. 2006;60(5):590–597. doi:10.1111/j.1440-1819.2006.01563.x PubMed
65. Buksti AS, Munkner R, Gade I, et al; From the Danish National Multicenter Schizophrenia Project. Important components of a short-term family group programme. Nord J Psychiatry. 2006;60(3):213–219. doi:10.1080/08039480600636379 PubMed
66. Cabral RRF, Chaves AC. Multi-family group intervention in a programme
for patients with first-episode psychosis: a Brazilian experience. Int J Soc Psychiatry. 2010;56(5):527–532. doi:10.1177/0020764009102754 PubMed
67. Barrio C, Yamada A-M. Culturally based intervention development: the case of Latino families dealing with schizophrenia. Res Soc Work Pract. 2010;
20(5):483–492. doi:10.1177/1049731510361613 PubMed
68. Budd RJ, Hughes ICT. What do the carers of people with schizophrenia find helpful and unhelpful about psycho-education? Clin Psychol Psychother. 1997;4(2):118–124. doi:10.1002/(SICI)1099-0879(199706)4:2<118::AID-CPP108>3.0.CO;2-K
69. Leff J, Kuipers L, Berkowitz R, et al. A controlled trial of social intervention in the families of schizophrenic service users. Br J Psychiatry. 1982;141:121–134. doi:10.1192/bjp.141.2.121 PubMed
70. Barrowclough C, Tarrier N, Watts S, et al. Assessing the functional value of relatives’ knowledge about schizophrenia: a preliminary report. Br J Psychiatry. 1987;151(1):1–8. doi:10.1192/bjp.151.1.1 PubMed
71. Tarrier N, Barrowclough C, Vaughn C, et al. The community management of schizophrenia: a controlled trial of a behavioural intervention with families to reduce relapse. Br J Psychiatry. 1988;153(4):532–542. doi:10.1192/bjp.153.4.532 PubMed
72. Kim C, Mueser KT. The effects of social skills training vs psychoeducation
on negative attitudes of mothers of persons with schizophrenia: a pilot study. Psychiatry Investig. 2011;8(2):107–112. doi:10.4306/pi.2011.8.2.107 PubMed
73. Falloon IRH, Boyd I, McGill C. Family Care of Schizophrenia: A Problem-Solving Approach for the Treatment of Mental Illness. New York, NY: Guilford; 1985.
74. Early Psychosis Prevention and Intervention Centre (EPPIC). Care Management in Early Psychosis: A Handbook. Melbourne, Australia: EPPIC; 2001.
75. Atkinson JM, Coia DA. Families Coping With Schizophrenia—A Practitioner’s Guide to Family Groups. New York, NY: John Wiley; 1995.
76. Anderson CM, Reiss DJ, Hogarty GE. Schizophrenia and the Family: A Practitioner’s Guide to Psychoeducation and Management. New York, NY: Guilford; 1986.
77. Miyar J, Adams CE. Content and quality of 10,000 controlled trials in schizophrenia over 60 years. Schizophr Bull. 2013;39(1):226–229. doi:10.1093/schbul/sbr140 PubMed
78. Lobban F, Glentworth D, Wainwright L, et al. Relatives Education And Coping Toolkit—REACT. Study protocol of a randomised controlled trial
to assess the feasibility and effectiveness of a supported self management package for relatives of people with recent onset psychosis. BMC Psychiatry. 2011;11(1):100. doi:10.1186/1471-244X-11-100 PubMed
79. Powell J, Chiu T, Eysenbach G. A systematic review of networked technologies supporting carers of people with dementia. J Telemed Telecare. 2008;14(3):154–156. doi:10.1258/jtt.2008.003018 PubMed
80. Cucciare MA, Weingardt KR, eds. Using Technologies to Support Evidence-Based Behavioural Health Practices—A Clinician’s Guide. New York, NY: Routledge; 2010.
81. Powell J, Martin S, Sutcliffe P, et al. Young People and Mental Health—The Role of Information and Communication Technology (Warwick Medical School Research Project funded by Comic Relief). Warwick, UK: Warwick Medical School; 2010.
82. McFarlane WR, Lukens E, Link B, et al. Multiple-family groups and psychoeducation in the treatment of schizophrenia. Arch Gen Psychiatry. 1995;52(8):679–687. doi:10.1001/archpsyc.1995.03950200069016 PubMed
83. Berheim K, Lehman A. Working With Families of the Mentally Ill. New York: Norton; 1985.





