Background: Electroconvulsive therapy (ECT) is an important therapy for treatment-resistant depression and is especially effective for elderly individuals with depression. This is the first US nationally representative description of ECT in the elderly.
Methods: Using 2014-2015 Medicare claims data, we compared elderly individuals with major depressive disorder (using ICD-9 and ICD-10 codes) who received ECT with those who did not on demographic and clinical measures. We characterized treatment patterns by setting and the proportion of individuals receiving index and continuation/maintenance courses, subtherapeutic courses of ECT, and post-ECT follow-up care.
Results: Of all Medicare beneficiaries aged 65 years and older diagnosed with depression in 2014-2015, 7,817 (0.41%) received 1 or more ECT sessions. Compared to the general population of elderly Medicare beneficiaries with depression, recipients of ECT were slightly younger and more likely to be male, non-Hispanic, and white and live in a zip code with a higher median income. Among those who received any ECT, 33.7% received < 5 total treatments. Of those who received an index ECT treatment, 33.7% received a continuation/maintenance course of ECT, while 60.9% received some form of post-ECT follow-up treatment (additional ECT or new psychotropic medication). Receipt of psychotherapy was the strongest predictor of those who received ≥ 5 ECT treatments (adjusted odds ratio = 1.43; 95% CI, 1.22 to 1.67).
Conclusions: Despite substantial evidence of efficacy, ECT use remains rare among elderly patients with depression. Findings suggest a potential need for efforts to increase the proportion of patients receiving adequate courses of ECT and evidence-based post-ECT follow-up care.
This CME activity is expired. For more CME activities, visit CMEInstitute.com.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders

CME Background
Articles are selected for credit designation based on an assessment of the educational needs of CME participants, with the purpose of providing readers with a curriculum of CME articles on a variety of topics throughout each volume. Activities are planned using a process that links identified needs with desired results.
To obtain credit, read the article, correctly answer the questions in the Posttest, and complete the Evaluation. A $10 processing fee will apply.
CME Objective
After studying this article, you should be able to:
- Consider a therapeutic course of electroconvulsive therapy for older patients with treatment-resistant depression
Accreditation Statement
The CME Institute of Physicians Postgraduate Press, Inc., is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians.
Credit Designation
The CME Institute of Physicians Postgraduate Press, Inc., designates this journal-based CME activity for a maximum of 1 AMA PRA Category 1 Credit™. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Note: The American Nurses Credentialing Center (ANCC) and the American Academy of Physician Assistants (AAPA) accept certificates of participation for educational activities certified for AMA PRA Category 1 Credit™ from organizations accredited by ACCME.
Release, Expiration, and Review Dates
This educational activity was published in July 2020 and is eligible for AMA PRA Category 1 Credit™ through August 31, 2020. The latest review of this material was June 2020.
Financial Disclosure
All individuals in a position to influence the content of this activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past year, Marlene P. Freeman, MD, Editor in Chief, has received research funding from JayMac and Sage; has been a member of the advisory boards for Otsuka, Alkermes, and Sunovion; has been a member of the Independent Data Safety and Monitoring Committee for Janssen; has been a member of the Steering Committee for Educational Activities for Medscape; and, as a Massachusetts General Hospital (MGH) employee, works with the MGH National Pregnancy Registry, which is sponsored by Teva, Alkermes, Otsuka, Actavis, and Sunovion, and works with the MGH Clinical Trials Network and Institute, which receives research funding from multiple pharmaceutical companies and the National Institute of Mental Health. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure appears at the end of the article.
ABSTRACT
Background: Electroconvulsive therapy (ECT) is an important therapy for treatment-resistant depression and is especially effective for elderly individuals with depression. This is the first US nationally representative description of ECT in the elderly.
Methods: Using 2014-2015 Medicare claims data, we compared elderly individuals with major depressive disorder (using ICD-9 and ICD-10 codes) who received ECT with those who did not on demographic and clinical measures. We characterized treatment patterns by setting and the proportion of individuals receiving index and continuation/maintenance courses, subtherapeutic courses of ECT, and post-ECT follow-up care.
Results: Of all Medicare beneficiaries aged 65 years and older diagnosed with depression in 2014-2015, 7,817 (0.41%) received 1 or more ECT sessions. Compared to the general population of elderly Medicare beneficiaries with depression, recipients of ECT were slightly younger and more likely to be male, non-Hispanic, and white and live in a zip code with a higher median income. Among those who received any ECT, 33.7% received < 5 total treatments. Of those who received an index ECT treatment, 33.7% received a continuation/maintenance course of ECT, while 60.9% received some form of post-ECT follow-up treatment (additional ECT or new psychotropic medication). Receipt of psychotherapy was the strongest predictor of those who received ≥ 5 ECT treatments (adjusted odds ratio = 1.43; 95% CI, 1.22 to 1.67).
Conclusions: Despite substantial evidence of efficacy, ECT use remains rare among elderly patients with depression. Findings suggest a potential need for efforts to increase the proportion of patients receiving adequate courses of ECT and evidence-based post-ECT follow-up care.
J Clin Psychiatry 2020;81(4):19m13186
To cite: Rhee TG, Olfson M, Sint K, et al. Characterization of the quality of electroconvulsive therapy among older Medicare beneficiaries. J Clin Psychiatry. 2020;81(4):19m13186.
To share: https://doi.org/10.4088/JCP.19m13186
© Copyright 2020 Physicians Postgraduate Press, Inc.
aDepartment of Community Medicine and Health Care, School of Medicine, University of Connecticut, Farmington, Connecticut
bYale Depression Research Program, Department of Psychiatry, Yale School of Medicine, New Haven, Connecticut
cDepartment of Psychiatry, College of Physicians and Surgeons, Columbia University, New York, New York
dCenter for Outcomes Research and Evaluation, Yale-New Haven Hospital, New Haven, Connecticut
*Corresponding author: Samuel T. Wilkinson, MD, Yale Depression Research Program, Yale School of Medicine, 100 York St, STE 2J, New Haven, CT 06511 ([email protected]).
Major depressive disorder (MDD) is a persistent and disabling condition, is the most common major mental illness worldwide, and is associated with significant morbidity and mortality.1 The burden of MDD is especially high among the geriatric population, where standard pharmacotherapies are associated with greater side effect burden2 and unremitted depression is strongly associated with disability and loss of independence.3 Older adults are also at highest risk for suicide4 and are among the fastest growing demographic in the US population.5
Electroconvulsive therapy (ECT) is the most effective treatment for MDD,6-10 with remission rates of 80%-90% when used as first line treatment. Moreover, ECT results in remission rates of 50%-70% in treatment-resistant depression (TRD)11 compared to remission rates of 13%-14% in TRD using conventional antidepressants.12 ECT has been shown to be especially effective in older adults.11,13 A recent cost-effectiveness analysis concluded that ECT is cost-effective after inadequate response to 2 antidepressants,14 and ECT can reduce risk of 30-day hospital readmissions among hospitalized patients with depression.13
Despite evidence that ECT is an effective treatment for patients with severe mood disorders, little is known about the use and quality of ECT in community practice. Early research suggested that among inpatients with recurrent MDD, ECT recipients were more likely to be older, white, and affluent compared to inpatients that did not receive ECT. More recently, ECT was used by 0.25% of a large cohort of privately insured US adults with MDD.15 However, no nationally representative descriptions of ECT use have been provided of the geriatric population. To address this knowledge gap, we used the 2014-2015 Medicare claims database to examine ECT use among older Medicare beneficiaries with depression.

- Electroconvulsive therapy (ECT) is an important treatment for geriatric depression, yet the quality and epidemiology of ECT among the geriatric population are not well established.
- Nationally representative data from Medicare show that a very small portion of those with depression (0.41%) received ECT.
- About a third of patients who started ECT received fewer than 5 treatments, suggesting that a substantial portion of patients receive a subtherapeutic course.
METHODS
Data Source
Data for this study were from the Medicare claims database from 2014 and 2015, the most recently available data at the time the project was initiated. These data are based on Medicare claims files, including the Medicare Master Beneficiary Summary File, inpatient and outpatient claims files, carrier files, and Part D Event Drug files.
Sample
We obtained data from all older Medicare beneficiaries (≥ 65 years old) who received at least 1 ECT procedure in 2014 or 2015, as identified by CPT code 90870 or 90871, ICD-9 code 94.27, or ICD-10 codes GZB0ZZZ-GZB4ZZZ. We also obtained data from a 25% random sample of all geriatric Medicare beneficiaries who had a code for major depressive disorder in 2014 or 2015, as identified by ICD-9 codes 296.2x and 296.3x as well as ICD-10 diagnosis codes of F32.x and F33.x.
Psychiatric, Medical, and Service Use Measures
We assessed sociodemographic characteristics, comorbid medical and psychiatric diagnoses, service use, and psychotropic medication prescriptions during 2014-2015. Sociodemographic characteristics were age, gender, and race/ethnicity. We also included median income of each patient’s residential zip code area, which was acquired from the American Community Survey from 2010, the most recently available data. Medical comorbidity was measured by Elixhauser score,16 excluding mental disorder diagnoses. We examined behavioral comorbidities separately from the modified Elixhauser score.
Service use was assessed by the proportion of patients with any inpatient mental health treatment during 2014-2015 and by the number of psychiatric and substance use visits (excluding ECT visits), emergency department visits, and medical and surgical outpatient visits. The proportions receiving psychotropic medication prescriptions filled in 2014-2015 were also calculated from individual claims. Psychotropic medications were classified into the following groups: antidepressants, antipsychotics, lithium, other mood stabilizers, stimulants, and anxiolytics/sedatives/hypnotics. We also classified patients by geographic residence into 4 Census regions: Northeast, Midwest, South, or West.
Analysis
We used descriptive statistics to characterize the total number of older Medicare beneficiaries who received ECT, the proportion of older Medicare beneficiaries with depression who received ECT, the relative breakdown of inpatient versus outpatient ECT utilization, the continuity of the transition from inpatient to outpatient ECT, and the course of ECT treatments for geriatric patients.
Among patients who received ECT, we calculated the proportion who received < 5 ECT treatments in an acute series and considered this treatment pattern to be a subtherapeutic dose. This definition is based on clinical experience, ECT guidelines,10 and evidence from a recent clinical trial in geriatric patients that over 80% of patients who remit to ECT require 5 or more treatments.17 We quantified the proportion of ECT treated patients who received subtherapeutic ECT doses and compared the characteristics of patients receiving therapeutic and subtherapeutic ECT doses. For these analyses, we compared clinical measures in the 6 months prior to treatment. These cohorts were also used to characterize index and continuation/maintenance courses of ECT (see below).
Characterization of Index and Continuation/Maintenance Courses of ECT
We characterized whether ECT was provided as part of different courses of therapy. Our definition of an index course of ECT was receiving 5 or more ECT sessions within a 30-day period. This definition was based on previously published claims data18 and recent data from the Prolonging Remission in Depressed Elderly (PRIDE) study.17 Any subsequent ECT session was part of the index series if it occurred < 7 days following the most recent ECT session. Given the difficulty of distinguishing between continuation and maintenance ECT series using claims data and the fact that continuation and maintenance ECT series both seek to prevent relapse and recurrence, we grouped later ECT sessions into a category of combined continuation/maintenance ECT courses. A continuation/maintenance course was composed of ECT sessions meeting the following criteria: (1) there were at least 3 ECT sessions; (2) the ECT sessions occurred 7 to 42 days following the last treatment of an identified index course or the most recent continuation/ maintenance ECT session; and (3) the ECT session was not part of the most recent or any subsequent index series of ECT. An ECT series had to follow an index series of ECT to be defined as a continuation/maintenance series.
To avoid truncation in this portion of the analysis, we used a restricted cohort, excluding individuals whose first documented ECT was before July 1, 2014, or after October 31, 2015. To characterize the quality of post-ECT care, we calculated the proportion of patients who received post-ECT follow-up treatment among those who received an index course of treatment. We defined post-ECT follow-up treatment as receiving either a continuation or maintenance ECT course or starting a new psychotropic medication with antidepressant properties (antidepressant, mood stabilizer, or antipsychotic) sometime after start of index course up until within 30 days of the last ECT session in an index course.
Analysis was conducted in Stata 15.1 MP/6-Core (College Station, Texas). We only analyzed data for individuals who had continuous Medicare coverage during 2014-2015. This study was approved by the Institutional Review Board at Yale University.
RESULTS
In 2014-2015, a total of 7,817 Medicare beneficiaries aged 65 years or older with continuous coverage had 1 or more claim for ECT (Table 1). After adjusting for the sampling of our dataset, we estimate that there were 1.89 million older Medicare beneficiaries with a diagnosis of MDD during this time period. Among older Medicare beneficiaries with a diagnosis of depression in 2014-2015 and continuous Medicare coverage, 0.41% received ECT during this time period. We calculated an average annual rate using the number of patients who received ECT in a given year by the total number of patients with MDD in a given year. This yielded an annual rate of 0.30% of older Medicare beneficiaries with depression who received ECT.
Demographic Characteristics
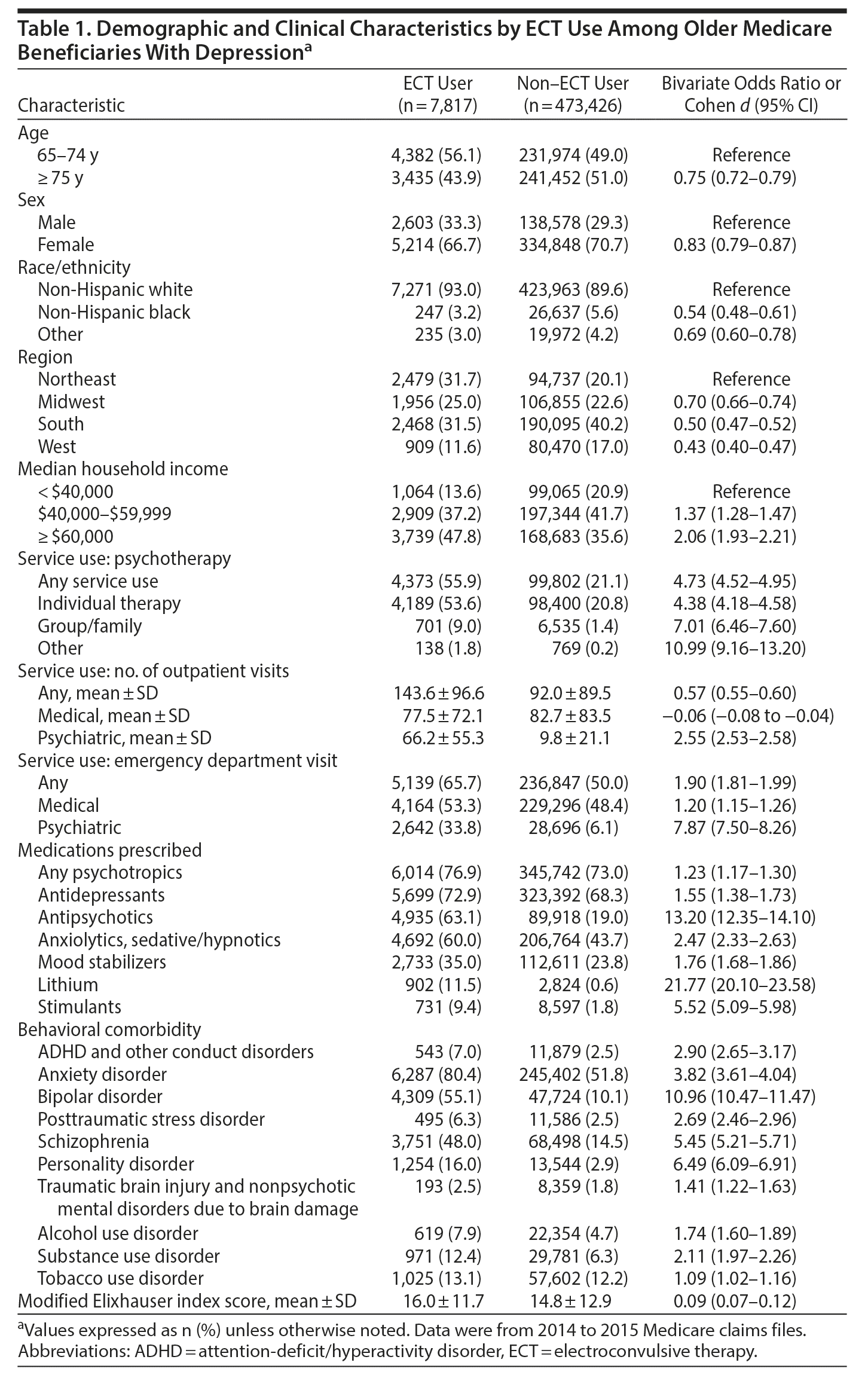
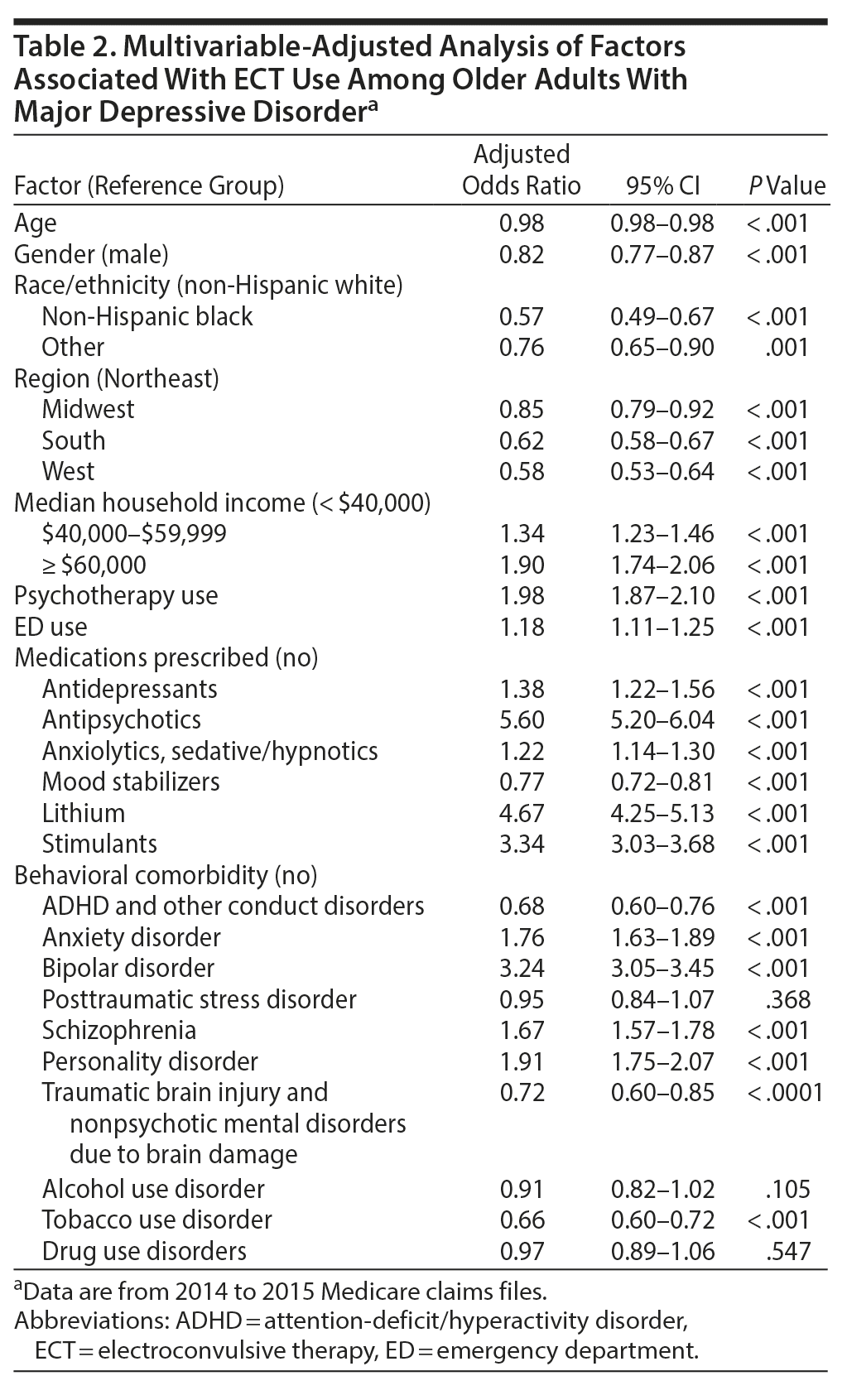
Compared to older Medicare beneficiaries with depression who did not receive ECT, those who received ECT were younger and more likely to be male and non-Hispanic white and live in zip code regions with higher median incomes (Table 1). Those who received ECT were also less likely to live in the South, West, and Midwest Census regions (reference: Northeast). These differences persisted after controlling for multiple covariates using a multivariable-adjusted analysis (Table 2).
Clinical Comorbidities
Compared to older Medicare beneficiaries with depression who did not receive ECT, those who received ECT were significantly more likely to have psychiatric comorbidities, most notably bipolar disorder, personality disorders, and schizophrenia. They were also more likely to have anxiety disorders, posttraumatic stress disorder, and substance and alcohol use disorders. In addition, they had slightly higher medical comorbidity burden, as evidenced by a higher modified Elixhauser index score (Table 1).
Service Utilization
Compared to Medicare beneficiaries with depression who did not receive ECT, those who received ECT were significantly more likely to receive psychotherapy (ORs > 4 for all), have emergency department visits for psychiatric problems (OR = 7.87), and have more outpatient visits for psychiatric problems (not including ECT visits, Cohen d = 2.55).
Characterization of ECT Quality
Inpatient versus outpatient use. Most individuals (2,938; 71.2%) who received ECT began in the inpatient setting, with approximately half (50.7%) receiving only inpatient ECT. Approximately one-third (33.7%) received ECT in both inpatient and outpatient settings and 18.8% received only outpatient ECT (Table 3).
Characterization of index and maintenance/continuation courses and post-ECT follow-up. Of those who received ECT, 60.4% received 1 or more index course, with a mean number of 8.46 sessions per index course. Of those who received an index course, 33.7% had a continuation/maintenance course following any index course, with a mean of 4.19 sessions per continuation/maintenance course. Of those with an index ECT course, 60.9% had some form of post-ECT follow-up mental treatment, either a continuation/maintenance ECT course or a new medication with antidepressant properties (antidepressant, mood stabilizer, or antipsychotic medication).
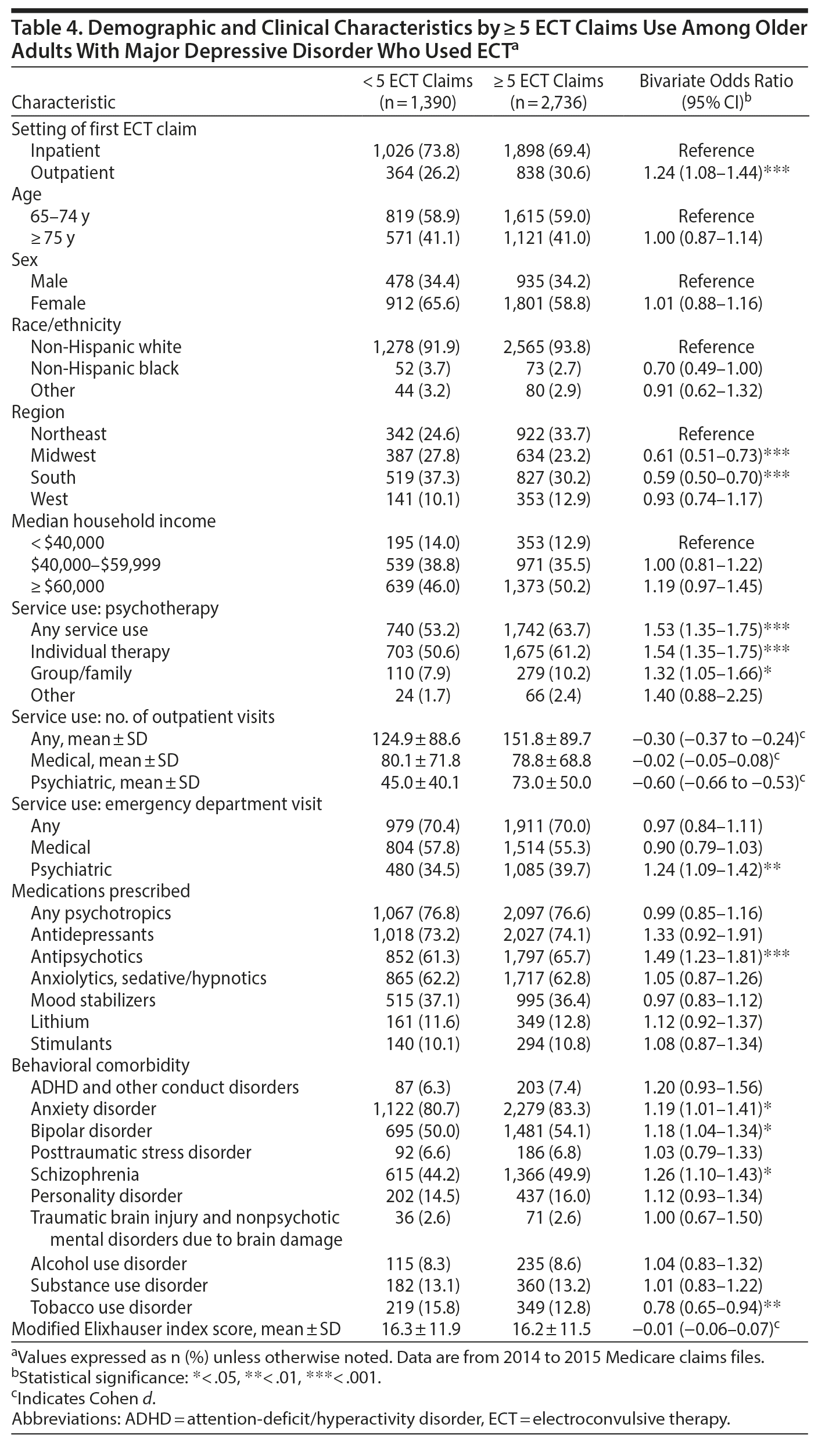
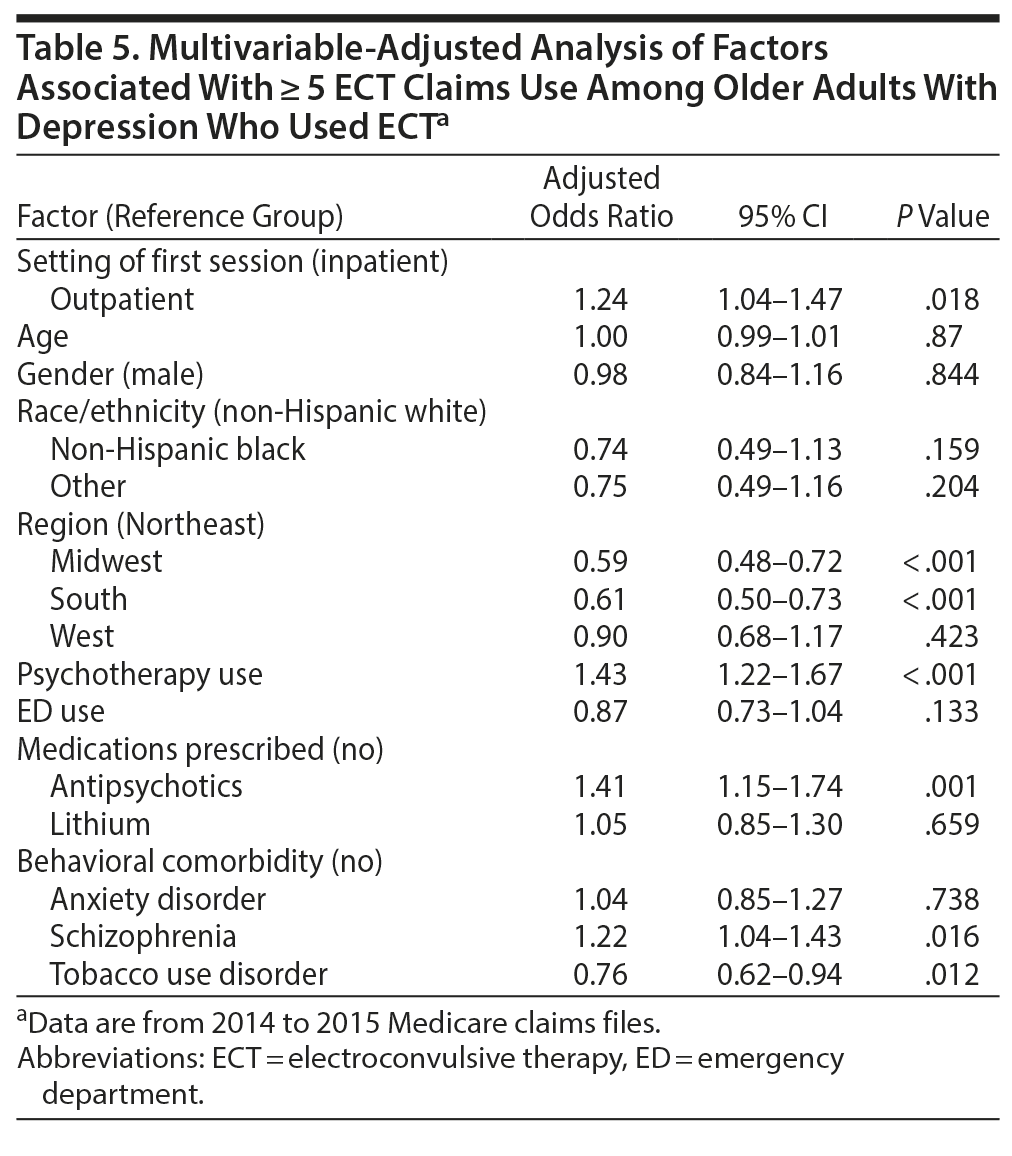
Subtherapeutic ECT treatment. There were 1,390 older Medicare beneficiaries with continuous coverage who received < 5 ECT treatments, representing 33.7% of the individuals who received any ECT during this time. Compared to the individuals who received therapeutic courses of ECT, those who received subtherapeutic courses of ECT were more likely to be non-Hispanic black, less likely to have received psychotherapy, less likely to have received antidepressant medication, and more likely to have received ECT only in an inpatient setting (Table 4). This pattern of subtherapeutic ECT use was more common in the South and Midwest than in the Northeast. After controlling for other covariates, the strongest predictor of whether patients received ≥ 5 ECT treatments was engagement in psychotherapy (adjusted OR = 1.43; 95% CI, 1.22 to 1.67; Table 5).
DISCUSSION
Among elderly Medicare beneficiaries with depression, an estimated 0.41% received 1 or more ECT sessions during the study period. Recipients of ECT were younger, more likely to be male, more likely to be white, and more likely to live in a more affluent area compared to the general population of Medicare beneficiaries with depression. Among those who received ECT, approximately one-third (33.7%) received 4 or fewer ECT sessions, likely representing a subtherapeutic course, suggesting a need for focusing on increasing the number of ECT treatments in the management of older adults with MDD. There were few patient-level demographic or clinical factors that predicted who received subtherapeutic doses of ECT.
As compared to non-ECT patients, our finding that ECT patients were more likely to be non-Hispanic white and living in zip code regions with higher median incomes is in line with findings of inpatient ECT treatment patterns from over 20 years ago.19 The finding that ECT is less likely to be used in the West has also been found in prior reports.15,19 This regional variation could be partly explained by variations in legal statutes governing ECT. For example, California has among the most stringent laws in this respect and requires 3 physicians to document that the patient has capacity to consent to the procedure.20
Our finding that 0.41% of elderly Medicare beneficiaries with depression received ECT is in keeping with a prior report of commercially insured individuals. Using the MarketScan data, Wilkinson and colleagues15 reported that fewer than 1% of adult individuals with depression received ECT during the study period. The proportions of individuals who received ECT from among those in a Veterans Health Administration setting who are receiving specialty mental health care are similarly low in local (0.45%)21 and national (0.11%)18 databases. These reports confirm the view that ECT is underutilized in community practice. While defining an appropriate use of ECT is challenging, given that treatment-resistant depression comprises up to 35% of individuals with depression and that ECT is the most effective treatment for this condition, ECT use rates below 1% suggest that efforts may be warranted to educate the public and professionals about effectiveness of ECT. Reasons for underuse of ECT are likely multifaceted and involve stigma, legal restrictions in some locales, the risk of cognitive side effects, and the overall complexity of administering ECT.22 Compared to prior reports,23 our data suggest that ECT use has decreased substantially in the last 20 years. However, formal analyses using the same dataset and methodological approach across years are required to evaluate trends in ECT use.
A substantial proportion (33.7%) of patients who received ECT did not receive a therapeutic course of treatment (defined as at least 5 ECT treatments within a 30-day period). There are at least 3 potential reasons that patients might stop ECT after 4 or fewer ECT sessions: (1) patients may have refused additional treatment, most likely due to side effects; (2) providers may have recommended cessation of treatment due to side effects or other untoward clinical sequelae; or (3) logistical barriers including insurance reimbursement, transition to outpatient care, transportation barriers, or a lack of an available anesthesiologist may have prevented further ECT therapy. Medicare claims data do not permit examination of the reasons for the high rate of subtherapeutic ECT dosing. In large clinical trials of ECT, discontinuation rates have ranged from 4.7% to 28.3% during the acute phase,8,17,24,25 though some of these trials used a more conservative definition of discontinuation before an adequate course of ECT. Notably, our rate of 33.7% is comparable to discontinuation rates of antidepressants in outpatient settings.26,27 After adjustment for relevant covariates, the strongest predictor of receiving 5 or more ECT sessions in index course was engagement in psychotherapy. This suggests that patients who received psychotherapy may have been more engaged in care or it might suggest that additional clinical attention in the form of psychotherapy helps to reassure patients and encourage them to continue ECT treatment.
To our knowledge, this is the first attempt to document post-ECT follow-up care. Abrupt cessation of ECT following treatment can lead to rapid relapse and return of symptoms.28 Standards of care and ECT guidelines emphasize that for those who achieve meaningful clinical improvement following ECT, continuation and maintenance treatment should be offered as either medication or additional ECT.29 In the Medicare population, 60.9% of patients received either continuation/maintenance ECT (28.3%) or a new psychotropic medication (43.8%). Because claims data do not yield information on depression severity, we are unable to contextualize these findings. Recent results from the PRIDE study have shown improvements in longer-term outcomes with continuation ECT and pharmacotherapy compared to pharmacotherapy alone.30 In the Medicare ECT cohort, half of all patients received ECT only in an inpatient setting. This suggests that a large portion of ECT recipients do not receive or are not offered ECT on a continuation/maintenance basis, as continuation/maintenance ECT is challenging to provide on inpatient units. Barriers to providing ECT on an outpatient basis likely include billing structures, space requirements, need for family/friends to provide transportation, and other factors.22
Preliminary studies investigating barriers to ECT implementation have identified several possible modifiable barriers. For example, some providers have cited that a lack of adequate space can restrain the expansion of existing services.22 Despite the passage of the Mental Health Parity and Addiction Equity Act, psychiatric services are reimbursed at relatively low rates compared with services provided by other specialties. Hence, ECT providers have reported that, in a busy hospital setting, times allotted for ECT can diminish if other, more profitable services have higher patient volumes. Currently, the Center for Medicaid/Medicare Services will not reimburse for ECT services performed outside of a hospital setting (for instance, in an outpatient, ambulatory surgical center), despite the fact that ECT is reported to be among the safest procedures involving general anesthesia with respect to peri-procedural mortality.31,32 The creation of billing codes for ECT outside of hospital settings may allow for expansion of services, shifting the space constraint to a “buyer’s market” and allowing ECT practitioners to expand services when clinical demand is high. Other potential approaches to enhancing the implementation of ECT include modifying educational curriculum requirements (currently, requirements for ECT didactics among psychiatrists in training are limited), reforms of legal restrictions, and education for the public as well as for practicing psychiatrists who potentially refer patients for ECT (“gatekeepers”).
The analyses presented here have several limitations. First, claims data do not provide information concerning symptom severity. It is therefore not possible to determine the percentage of patients who received 4 or fewer ECT treatment sessions achieved meaningful clinical improvement. Second, due to our inability to gauge what proportion of patients achieved meaningful clinical improvement, it is difficult to contextualize the proper proportion of patients who should have been offered continuation/maintenance ECT. Third, our data did not contain beneficiaries of the Medicare Advantage program, which comprises approximately 30% of all Medicare beneficiaries in the years examined. Finally, while our findings suggest that ECT utilization rates have declined in the last 20 years, formal analyses are required to evaluate trends.
In sum, these national data confirm that ECT use, even among geriatric patients with depression for whom considerable evidence of efficacy exists, was rare. A large proportion of older individuals who were treated with ECT received subtherapeutic courses, and only 60% received some post-ECT follow-up care. Quality improvement efforts could be directed at improving the implementation of ECT and ensuring adequate treatment courses and follow-up care. Provider- and hospital-level variation in ECT course and follow-up should be explored to identify factors associated with high quality care. Improving these quality measures and ensuring equitable and appropriate access to ECT in community settings are challenging given the complexity of ECT administration and attitudinal barriers. Intervention efforts might focus on revising educational curriculum requirements for psychiatrists in training, reforming legal restrictions, and educating referring psychiatrists (“gatekeepers”) and the general public.
Submitted: November 27, 2019; accepted March 25, 2020.
Published online: July 7, 2020.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents or device therapies that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Financial disclosure: Dr Wilkinson has received contract funding from Janssen and Sage Therapeutics for the conduct of clinical trials administered through Yale University; anticipates receiving contract funding from LivaNova and Oui Therapeutics for conducting clinical trials; and has received consulting fees from Janssen, Oui Therapeutics, and Biohaven Pharmaceuticals. Drs Rhee, Sint, and Olfson have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: This work was supported by a young investigator grant from the American Foundation for Suicide Prevention (Dr Wilkinson) and from the National Institute of Mental Health (R21MH117438). Dr Wilkinson also acknowledges support from the Agency for Healthcare Research and Quality (K12HS023000), the Brain and Behavior Research Foundation (formerly NARSAD), and the Robert E. Leet and Clara Guthrie Patterson Trust Mentored Research Award.
Role of the sponsor: Other than providing financial support, the funding agencies had no role in the conduct or publication of this study.
Additional information: The Medicare and National Death Index data used in this project reside on secure servers at Yale University. They are subject to Data Use Agreement #52334 between Yale University and the Research Data Assistance Center and are thus not available to the public. Queries can be directed to Dr Wilkinson.
This CME activity is expired. For more CME activities, visit cme.psychiatrist.com.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
REFERENCES
1. Kessler RC, Berglund P, Demler O, et al; National Comorbidity Survey Replication. The epidemiology of major depressive disorder: results from the National Comorbidity Survey Replication (NCS-R). JAMA. 2003;289(23):3095-3105. PubMed CrossRef
2. Atkin PA, Veitch PC, Veitch EM, et al. The epidemiology of serious adverse drug reactions among the elderly. Drugs Aging. 1999;14(2):141-152. PubMed CrossRef
3. Callahan CM, Wolinsky FD, Stump TE, et al. Mortality, symptoms, and functional impairment in late-life depression. J Gen Intern Med. 1998;13(11):746-752. PubMed CrossRef
4. Conwell Y, Duberstein PR, Caine ED. Risk factors for suicide in later life. Biol Psychiatry. 2002;52(3):193-204. PubMed CrossRef
5. He W, Goodkind D, Kowal PR. An Aging World: 2015. Washington, DC: United States Census Bureau; 2016.
6. Freeman CP. The therapeutic efficacy of electroconvulsive therapy (ECT): a double blind controlled trial of ECT and simulated ECT. Scott Med J. 1978;23(1):71-75. PubMed CrossRef
7. Johnstone EC, Deakin JF, Lawler P, et al. The Northwick Park electroconvulsive therapy trial. Lancet. 1980;2(8208-8209):1317-1320. PubMed CrossRef
8. Sackeim HA, Prudic J, Devanand DP, et al. A prospective, randomized, double-blind comparison of bilateral and right unilateral electroconvulsive therapy at different stimulus intensities. Arch Gen Psychiatry. 2000;57(5):425-434. PubMed CrossRef
9. Prudic J, Olfson M, Marcus SC, et al. Effectiveness of electroconvulsive therapy in community settings. Biol Psychiatry. 2004;55(3):301-312. PubMed CrossRef
10.American Psychiatric Association Committee on Electroconvulsive Therapy. The Practice of Electroconvulsive Therapy: Recommendations for Treatment, Training, and Privileging: A Task Force Report of the American Psychiatric Association. 2nd ed. Washington, DC: American Psychiatric Association; 2001.
11.Greenberg RM, Kellner CH. Electroconvulsive therapy: a selected review. Am J Geriatr Psychiatry. 2005;13(4):268-281. PubMed CrossRef
12.Zisook S, Ganadjian K, Moutier C, et al. Sequenced Treatment Alternatives to Relieve Depression (STAR*D): lessons learned. J Clin Psychiatry. 2008;69(7):1184-1185. PubMed CrossRef
13.Slade EP, Jahn DR, Regenold WT, et al. Association of electroconvulsive therapy with psychiatric readmissions in US hospitals. JAMA Psychiatry. 2017;74(8):798-804. PubMed CrossRef
14.Ross EL, Zivin K, Maixner DF. Cost-effectiveness of electroconvulsive therapy vs pharmacotherapy/psychotherapy for treatment-resistant depression in the United States. JAMA Psychiatry. 2018;75(7):713-722. PubMed CrossRef
15.Wilkinson ST, Agbese E, Leslie DL, et al. Identifying recipients of electroconvulsive therapy: data from privately insured Americans. Psychiatr Serv. 2018;69(5):542-548. PubMed CrossRef
16.van Walraven C, Austin PC, Jennings A, et al. A modification of the Elixhauser comorbidity measures into a point system for hospital death using administrative data. Med Care. 2009;47(6):626-633. PubMed CrossRef
17.Kellner CH, Husain MM, Knapp RG, et al; CORE/PRIDE Work Group. Right unilateral ultrabrief pulse ECT in geriatric depression: phase 1 of the PRIDE Study. Am J Psychiatry. 2016;173(11):1101-1109. PubMed CrossRef
18.Peltzman T, Gottlieb DJ, Shiner B, et al. Electroconvulsive therapy in Veterans Health Administration hospitals: prevalence, patterns of use, and patient characteristics [published online ahead of print January 6, 2020]. J ECT. PubMed CrossRef
19.Olfson M, Marcus S, Sackeim HA, et al. Use of ECT for the inpatient treatment of recurrent major depression. Am J Psychiatry. 1998;155(1):22-29. PubMed CrossRef
20.Harris V. Electroconvulsive therapy: administrative codes, legislation, and professional recommendations. J Am Acad Psychiatry Law. 2006;34(3):406-411. PubMed
21.Wilkinson ST, Rosenheck RA. Electroconvulsive therapy at a Veterans Health Administration Medical Center. J ECT. 2017;33(4):249-252. PubMed CrossRef
22.Kitay BM, Sanacora G, Rosenheck RA, et al. Examining factors leading to underutilization of electroconvulsive therapy in the United States. Paper presented at: 2019 International Society of ECT and Neurostimulation Annual Meeting; San Francisco, CA.
23.Case BG, Bertollo DN, Laska EM, et al. Declining use of electroconvulsive therapy in United States general hospitals. Biol Psychiatry. 2013;73(2):119-126. PubMed CrossRef
24.Husain MM, Rush AJ, Fink M, et al. Speed of response and remission in major depressive disorder with acute electroconvulsive therapy (ECT): a Consortium for Research in ECT (CORE) report. J Clin Psychiatry. 2004;65(4):485-491. PubMed CrossRef
25.Sackeim HA, Prudic J, Nobler MS, et al. Effects of pulse width and electrode placement on the efficacy and cognitive effects of electroconvulsive therapy. Brain Stimul. 2008;1(2):71-83. PubMed CrossRef
26.McGettigan P, Kelly A, Carvahlo M, et al. Anti-depressants in primary care: analysis of treatment discontinuations. Pharmacoepidemiol Drug Saf. 2000;9(6):521-528. PubMed CrossRef
27.van Geffen EC, van Hulten R, Bouvy ML, et al. Characteristics and reasons associated with nonacceptance of selective serotonin-reuptake inhibitor treatment. Ann Pharmacother. 2008;42(2):218-225. PubMed CrossRef
28.Sackeim HA, Haskett RF, Mulsant BH, et al. Continuation pharmacotherapy in the prevention of relapse following electroconvulsive therapy: a randomized controlled trial. JAMA. 2001;285(10):1299-1307. PubMed CrossRef
29.Gill SP, Kellner CH. Clinical practice recommendations for continuation and maintenance electroconvulsive therapy for depression: outcomes from a review of the evidence and a consensus workshop held in Australia in May 2017. J ECT. 2019;35(1):14-20. PubMed CrossRef
30.Kellner CH, Husain MM, Knapp RG, et al; CORE/PRIDE Work Group. A novel strategy for continuation ECT in geriatric depression: phase 2 of the PRIDE Study. Am J Psychiatry. 2016;173(11):1110-1118. PubMed CrossRef
31.T׸rring N, Sanghani SN, Petrides G, et al. The mortality rate of electroconvulsive therapy: a systematic review and pooled analysis. Acta Psychiatr Scand. 2017;135(5):388-397. PubMed CrossRef
32.Watts BV, Groft A, Bagian JP, et al. An examination of mortality and other adverse events related to electroconvulsive therapy using a national adverse event report system. J ECT. 2011;27(2):105-108. PubMed CrossRef
This PDF is free for all visitors!