ABSTRACT
Mental health clinicians often hear seriously ill patients ask the unanswerable: Why did this happen? What is the meaning of my suffering? In the inpatient setting, general medical ward, or oncology unit, patients are confronted with their mortality in new, urgent ways. Palliative medicine, or the specialized, comprehensive care of patients facing a life-limiting illness, occupies a unique and liminal space. Although often practiced by clinicians with non–mental health training backgrounds, there exists ample psychological content to be explored in the palliative care encounter. In this article, we present the case of a husband and international businessperson who experienced terminal complications from an advanced stage lung cancer. His illness was not responsive to multiple cancer-directed treatments, and he developed respiratory failure requiring high levels of supplemental oxygen support, from which he was unable to wean. Palliative care consultation was sought with the multiple objectives of ameliorating his severe death anxiety and persistent dyspnea as well as assisting in the clarification of his end-of-life wishes. Our goal with this case presentation and related discussion is to introduce the psychological aspects of palliative medicine to psychiatrists and psychotherapists.
J Clin Psychiatry 2022;83(2):22ct14391
To cite: Rosenberg LB, Fishel AK, Harley R, et al. Psychological dimensions of palliative care consultation: approaches to seriously ill patients at the end of life. J Clin Psychiatry. 2022;83(2):22ct14391.
To share: https://doi.org/10.4088/JCP.22ct14391
© Copyright 2022 Physicians Postgraduate Press, Inc.
aDivision of Palliative Care and Geriatric Medicine, Massachusetts General Hospital, Harvard Medical School, Boston, Massachusetts
bFamily and Couples Therapy Program, Massachusetts General Hospital, and Department of Psychiatry, Harvard Medical School, Boston, Massachusetts
cDialectical Behavior Therapy Program, Massachusetts General Hospital, and Department of Psychiatry, Harvard Medical School, Boston, Massachusetts
dAvery D. Weisman Psychiatry Consultation Service and Thomas P. Hackett Center for Scholarship in Psychosomatic Medicine, Massachusetts General Hospital, and Department of Psychiatry in the field of Psychosomatic Medicine/Consultation, Harvard Medical School, Boston, Massachusetts
eFeinberg School of Medicine, Northwestern University, Chicago, Illinois, and the Mongan Institute, Massachusetts General Hospital, Boston, Massachusetts
fCenter for Anxiety and Traumatic Stress Disorders, Massachusetts General Hospital, Harvard Medical School, Boston, Massachusetts
*Corresponding author: Leah B. Rosenberg, MD, 600 Austen, 55 Fruit St, Boston, MA 02114 ([email protected]).
Presented here is a series that highlights the discussion of a complex case by several expert clinicians, faculty members of Massachusetts General Hospital/Harvard Medical School, from distinct fields of study. Cross Talk demonstrates that clinical challenges can often be improved upon by leveraging more, rather than fewer, clinical perspectives.
Palliative medicine, or specialized medical care for people living with life-altering or life-limiting serious illness, has developed significantly over the last 20 years.1 Growing out of the hospice movement, which revolutionized pain and symptom management care for people in the end-of-life period, palliative care has come into its own as a mature specialty with expanding fellowship training programs, board certification, and deepening areas of research and innovation.2 Palliative care is delivered when and where patients need it, including inpatient consultative services, outpatient clinics, and community-based programs.3 Palliative care clinicians and researchers have spearheaded the development of serious illness communication, which has accordingly influenced general medical encounters that focus on goals of care and difficult prognostic information.4 This approach to communication has roots in the psychotherapeutic model but is largely practiced by clinicians trained in internal medicine, family medicine, or advanced practice nursing with little or no explicit training in talk therapy. As the American population ages, palliative care will become an increasingly crucial element of high-quality care.
Affective symptoms such as anxiety and depression are quite common in palliative care populations, affecting between 24%–48%, with a lower percentage meeting the criteria for a formal anxiety disorder diagnosis.5 As such, patients may not meet with mental health clinicians but rather have their psychological symptoms addressed during a palliative care encounter. Death anxiety, theorized in the 1960s by psychiatrists Ernest Becker and Irvin Yalom, encompasses the lifelong paradox of having to balance daily concerns and joys with the rising awareness of mortality.6,7 In serious illness, particularly during the crisis of inpatient hospitalization, patients can become increasingly affected by death anxiety and even experience death panic, in which communication and function are impaired.8
Palliative care clinicians routinely explore and clarify a psychological concept called prognostic awareness, or “a patient’s capacity to understand his or her prognosis and the likely illness trajectory.”3(p894) In the clinical practice of palliative care, inpatient consultation is often requested for the management of physical symptoms such as pain, dyspnea, nausea, constipation, anxiety, or delirium with the additional intention for the clinician to address the patient’s prognostic awareness during the encounter. A recent systematic review of the concept found that essential components include an accurate estimation of possible recovery or incurable nature, awareness of mortality, and understanding of the goals of treatment.9 When patient prognostic awareness is rated by researchers as “more accurate,” patients are more likely to have reduced aggressiveness of care at the end of life and possibly increased depressive symptoms.10–12 Other scholars have situated prognostic awareness within the construct of general health literacy, although there is likely an emotional and existential component to this aspect of self-knowledge that sets it apart.13,14
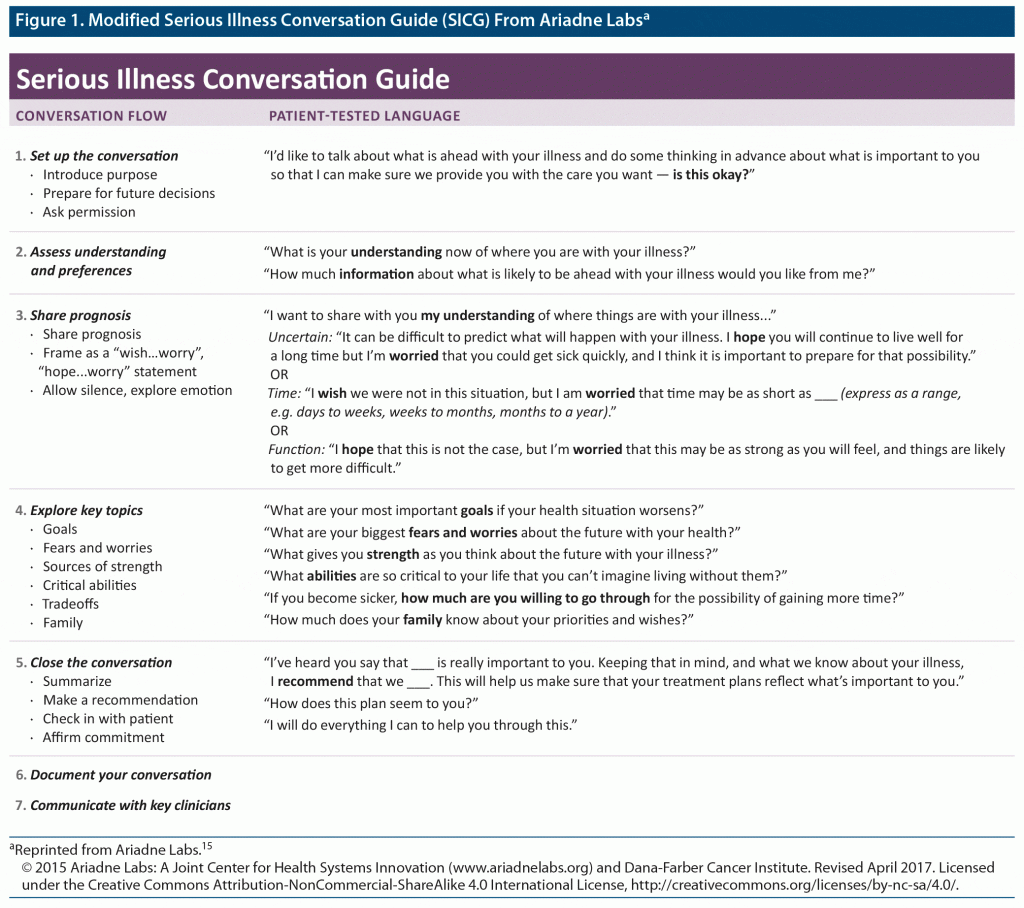
Non-palliative care specialists can also assess prognostic awareness with the use of systematic tools such as a Serious Illness Communication Guide (SICG) (Figure 1).15 Ariadne Labs, based in Boston, Massachusetts, and affiliated with the Dana-Farber Cancer Institute, developed and disseminated a SICG that may be adapted for a wide variety of clinical roles and situations. This type of communication shares facets with many of the core skills of psychotherapy: active listening, complex reflections, assessment of informational preferences, and exploration of deeply felt goals and values.16,17 This standardized framework may be useful for clinical psychiatrists who care for seriously ill patients with coexisting mental health problems, although literature on this specific population is currently lacking.
In the following, we hope to illuminate the psychologically oriented approach of consultative palliative care for a patient approaching the end of life with severe anxiety and unclear goals of care.
Case History and Treatment Course
Dr Rosenberg: Stephen was a 60-year-old, white, married, LGBTQ-identified, employed man with hypertension and an 18-month history of non–small cell lung cancer, metastatic to bone, liver, and brain. He had minimally used tobacco products approximately 30 years ago. He was referred to inpatient palliative care while hospitalized in an oncology unit at the Massachusetts General Hospital for anxiety, dyspnea, and clarification of the goals of care.
Initially diagnosed after developing progressive malaise and intermittent small-volume hemoptysis, Stephen had undergone multiple rounds of standard chemotherapies and was at the point of considering investigational trials. He had tolerated treatment well, with few missed or dose-reduced cycles of chemotherapy, and yet the cancer had progressed. On a new trial drug, he was scheduled for re-staging full body CAT scans in 3 weeks to evaluate response. These scans, 3 weeks away, were a beacon for his hope and mental focus. He expressed to multiple clinicians that he just “needed to get there.” He had never visited the outpatient palliative care clinic and had not been prescribed opioid medication for pain despite multiple osseous sites of metastasis. He had no family history of lung cancer.
Stephen had no history of mental health diagnoses including generalized anxiety or major depression. He had taken alprazolam for flights from time to time. He had never been admitted to a mental health setting but had seen a psychotherapist several years ago during his coming out process. Given the palliative care frame, less is known about this encounter with formal psychotherapy. Aside from his cancer diagnosis, he told me that his life had been “coming along pretty well now.” He had been legally married to Carlos for 5 years and together with him much longer, lived in a comfortable home in a Boston suburb, and felt he had a close relationship with his parents, who were both living though dealing with multiple health problems of their own. Given the COVID-19 pandemic, he had not seen them in person for many months.
Admitted from the oncology clinic 1 week prior, Stephen had originally presented for worsening shortness of breath. On examination, he was found to have a peripheral oxygen saturation of 85% on room air and was currently using 6 L of supplemental oxygen through nasal cannula and occasionally a non-rebreather face mask for recovery after movement from the bed to chair or short walks. He was cachectic with visible temporal wasting and mild pitting edema to the midshins, bilaterally. His lung examination was significant for dullness to percussion at bilateral bases and the use of accessory neck and abdominal muscles to breathe. On the mental status examination, he was anxious in appearance, alert, dressed in a hospital gown, and perseverative in thought process, although he was quite dyspneic during the encounter. Neurologic examination was limited, but no gross motor or sensory deficits were observed. Laboratory data were largely unremarkable, with normal complete blood count findings and basic metabolic panel with a serum albumin of 3.0, indicating that he was malnourished. The impact of the widespread cancer had taken a toll on his appetite for food.
Stephen had reluctantly agreed to consultation from palliative care. He had met earlier in the hospitalization with another inpatient palliative care attending physician and began to explore what he would want if things continued to deteriorate. In her notes, I read that he expressed “not wanting to be a vegetable” and wanting his husband and parents “to be in consensus” about end-of-life decisions. He understood at that time, 10 days prior to our meeting, that he “did not expect to live for another 50 years” and was seeking “stability” if cure was not possible. He said to my colleague, “I just want to get through this, on to the next thing. I was shocked when palliative care was consulted—isn’t that just for people who are dying?” They agreed together to focus on his symptom management. Stephen was recommended lorazepam 1 mg IV every 4 hours as needed and began taking it 2 or 3 times a day. I became involved about 5 days after the initial palliative care consultation as he began to experience worsening dyspnea and anxiety.
Prior to his hospital admission, he met with his oncologist, who was clearly concerned about his declining functional condition. He was short of breath with short walks and self-care activities. His oncologist asked if he had considered advance care planning or executed a will. His response to her was, “I’m only 60, I’m not ready for those things yet.” He was singularly focused on undergoing further immunotherapy for the cancer. In the hospital, he showed similar reluctance to engage on these issues. From time to time, Carlos would intercept team clinicians in the hallway outside Stephen’s room, expressing concern about his breathing. During my interactions with the couple together, I never witnessed Carlos express his fears in Stephen’s presence. Palliative care clinicians are often followed into the corridor by worried family members who are reluctant to give voice to their concerns in front of the patient. This, too, is a challenge of our frame. In palliative care, we consider the patient and their trusted loved ones to be our unit of care and concern. I continually felt the tension of Carlos’ silence in the room juxtaposed with his anxious questions outside in the hallway.
The oncology floor team also hovered in the hallway when I entered the unit. There was a pervasive concern among them that Stephen was getting sicker from a respiratory perspective and “didn’t get it.” Such statements from referring clinicians often allude to a patient’s inaccurate or limited prognostic awareness.18 Stephen avoided discussions of his likely lifespan and trajectory, often turning the conversation to logistic topics or becoming “shut down” and resistant to exploration.
First visit. I began the interview as I usually did, with questions about his physical symptoms: pain, shortness of breath, nausea, insomnia, and the like. He was experiencing back pain on and off from metastatic spread, but the most intrusive symptom was the persistent breathlessness. Tumor was blocking a main branch of his respiratory tree; perhaps there was infection or fluid, but perhaps not. Having asked about his body, I transitioned to his mind. The following is an excerpt from the first encounter.
Clinician: I imagine you didn’t expect to be admitted into the hospital when you went to the oncology clinical appointment. How has the last week been for you?
Patient: It’s been hard. It’s a long day in this room.
Clinician: Are you feeling nervous or anxious?
Patient: Well, a little, wouldn’t you be? Last night I felt that I had to have a bowel movement, so I asked the nurse to help me into the bathroom. Afterward, when I was back in bed, I was so out of breath. I could never get back to where I was at the beginning of the night. I was good when the night began. What a dumb thing to do, right? I overdid it. That’s my problem.
Clinician: It sounds like a difficult night, even frightening.
Patient: It’s just a matter of figuring things out.
[Pause]
Clinician: What do you make of all of this? Where do you feel you are in the course of this illness?
Patient: What kind of question is that? Why can’t you be more positive?
Clinician: What would it mean to be more positive now?
[He grimaced, turned his gaze away from me, and began asking Carlos about a planned medical procedure later that day. I had been dismissed from his attention.]
Clinician: We’ve talked about a lot, Stephen. I see you’re tired. Let’s try the medications that we have started for your shortness of breath and check in tomorrow.
Stephen shifted back and forth in the chair, eyes gazing over my shoulder toward the ceiling tiles. Uncharacteristically, I was standing in his room. Now, during the COVID-19 pandemic, I never sat, although being seated knee-to-knee with patients had long been a key point of my practice. I felt uncomfortable out in the world, as if the air were potentially poisonous. In a similar way, Stephen gasped around an obstructing tumor within him, gripping his airways as he tried to speak, laugh, and, above all, convince his husband that everything was still okay. Apart, together, and globally, Stephen and I were stalked by something unseeable, pernicious, and barely discussable.
Multiple clinicians felt as if they were not “getting through” to Stephen. He had a way of constructing a logical sequence to the worsening symptoms, turning them into a problem to be solved through reason. My empathic gestures and techniques felt as though they were falling flat. There are times when the assessment of a patient’s prognostic awareness feels like a game of tennis in which the patient keeps lobbing responses back over the net. On this first visit, I wanted to develop a sense of Stephen’s prognostic awareness, or illness understanding. I asked questions to better ascertain how sick he felt he was and even if he was afraid or aware of dying. Generally, palliative care clinicians open such a portion of the interview with a question focused on the patient’s hopes and worries for their overall illness and for the hospitalization. We often use open-ended questions, complex reflections, and brief summarizations during the encounter to explore a patient’s conception of the illness.
Second visit (48 hours later). Paged early by his nurse, I arrived to find Stephen “tripod-ing,” or leaning forward on his arms to catch his breath. His eyes briefly regarded me as I entered, surgical mask and face shield in place, as I was now accustomed to doing with every patient. Stephen required oxygen delivered through high-flow nasal cannula to maintain a livable level and could barely move even so. Through my mask, I had to speak even louder to be heard over the constant hum and whoosh of the supplemental high flow oxygen. This device was the most breathing support one could receive short of an intubation. He smiled tightly as I entered, his hands encircling bed pillows from home on either side. The clinical conversation during the second meeting was as follows:
Clinician: How are you?
Patient: Doing fine. Feeling better than before.
Clinician: I see.
Patient: Last night was tough. Really tough. I don’t think I got a bit of sleep at all. But this morning, things are better. I took my meds, even walked around the room. I just have to hang on until the chemo starts working. I have scans in 3 weeks.
Clinician: Stephen, I’m worried. You need a plan B. What if you become worse while you’re waiting?
Patient: What do you mean, “a plan B”? Living is the only plan.
Clinician: If you get sicker than you are now and choose to go to the intensive care unit, I am worried that you will have your last moments with doctors and nurses instead of Carlos and your parents. I want to make sure our planning fits your wishes.
Patient: This is just a temporary reset. I just need more time. I don’t want any of this. And you. Can you leave? My anxiety is through the roof. You aren’t helping.
I said goodbye and left the room. I walked to the desk, where the medical team asked, “How did it go? Does he ‘get it’ yet?” He had been placed on the “watch list” for patients who are likely to crash and require transfer to an ICU. No one thought he would recover from such a decline.
Later that day, I received an email from Stephen’s oncology attending physician, copied to the trainees of the primary team as well as my palliative care fellow, which read as follows:
[Stephen] brought up to us again this afternoon that he would prefer not to see Leah anymore. We discussed it as a team this afternoon, and we want to provide the most patient centered care possible, especially at the end of his life. Therefore, we feel that it is most appropriate to transition him to another palliative care attending.
I wrote back quickly and made accommodations to transfer his care to a colleague. I felt ashamed of my “dismissal” from the case. Where had the breakdown occurred? The following day, Stephen lost consciousness with increasing requirements for oxygen. His family chose to refocus his care on comfort-oriented measures, and he died in the early evening with his husband at bedside.
Reflecting on the case, I see both Stephen and I as existing in the “in-between spaces.” He was between life and death, insight and denial, and death anxiety and acceptance. As palliative care clinicians, we occupy the liminal space between medicine and mental health. We see ourselves as “transdisciplinary” in approach, able to flex into the domains of social work and spiritual care when a situation requires it. This flexibility also makes us vulnerable. Patients like Stephen can wonder who exactly we are and what message we bring. Why can’t we “be more positive?” If we can be “fired” from the clinical team, does that mean that discussions around prognostic awareness can also be disavowed?
Susan Sontag speaks of the “two countries” of serious illness and health in her seminal work, Illness as Metaphor.19 Underneath the protective equipment and in the space between, there were two worlds, two ecosystems, two climates in the room with Stephen: that which was under our masks and face shields and that which transcended the equipment. I wasn’t sure what was getting through. The COVID-19 pandemic has changed many things for “process-oriented” specialties such as psychiatry and palliative care. Within my masked environment, I could sense my own grimace and encouraging smiles, experience the warmth of an outbreath, and feel my lips tighten over my teeth in worry. The physical equipment became the concrete manifestation of a reality about palliative care that I had always known on some level. There is a yawning distance in the space between patient and clinician. They are not just sick, but dying, and I am well, or appear so. I have a 3-month-old daughter, constantly in my thoughts as I walk the halls of a hospital during a respiratory pandemic. They have their own battered lungs to consider as they watch perhaps hundreds of hospital workers come and go, empty the trash, bring the meal, insert the IV, give the “bad news.” During the COVID-19 pandemic, we are all in the liminal space between—what is being passed between us? Will it hurt us? Will it kill us? What will it do to the ones we love most? Together and apart, Stephen and his clinicians experienced his quest for more life amid an inevitable, and deeply challenging, confrontation with mortality.
Family/Couples Therapy Perspective
Dr Anne K. Fishel
When patients can discuss their goals for their end-of-life care, they suffer less, hold on longer to being engaged with loved ones, and die more peacefully. The bereaved are also somewhat less likely to suffer from a major depression.20 But not everyone faces death head on, and surely there are many good ways to exit this world. As Atul Gawande wrote in Being Mortal, “[People] want to end their stories on their own terms.”21(p249) Stephen’s terms seemed not to be aligned with Dr Rosenberg’s well-intentioned palliative practices.
Perhaps some additional interventions might have helped:
- Pandemic masking, along with the thrumming of machines, made connection very difficult. If Stephen had been offered some agency when he was feeling so powerless, he might have engaged more; the clinician could have said, eg, “I wonder if anything could make this conversation less effortful—do you want to try writing notes back and forth? Or I could meet with you on Zoom from another room so that I can take my mask off?” “Give me a hand signal if you don’t find a question helpful.”
- As a couples therapist, I construe both members of the couple as my patient. Instead of talking with Carlos in the hall, he could have been brought to Stephen’s bedside. “This illness is happening to both of you. It’s very common for the emotional labor to be divvied up between a couple—hope and despair, seeking more information versus taking in as little as possible, surrendering versus never giving up. How are you two managing?”
- Questions focusing on the present could be asked of the couple. “What do you do that brings Stephen comfort? What helps, and what doesn’t?”
- If allowed, questions about the future could also be posed. “Some couples who are dealing with serious illness find certain conversations really helpful. Would you like to hear about that?”
Then, I might offer research on end-of-life conversations,22 maybe referring to them as “conversations when the future is uncertain.” These conversations include offering expressions of love, reminiscing and sharing stories, giving or receiving forgiveness, expressing gratitude, and talking about concerns about what lies ahead. Could Carlos have initiated any of these?
I think Stephen answered Dr Rosenberg’s questions about being more positive when he turned away silently toward Carlos. Relying on Carlos for comfort was what it meant to be more positive. And having Carlos by his side was the way he ended his life on his own terms.
Dialectical Behavior Therapy Perspective
Dr Rebecca Harley
For cases that fit, dialectical behavior therapy (DBT) offers a toolbox of behavioral strategies that clinicians can reach into and use. Underpinning that toolbox is a set of ideas that I find clinically useful even in cases where the behavioral tools are not necessary—concepts like the dialectical tension between opposing forces and radical acceptance. These concepts existed well before DBT, but DBT does a nice job of making them accessible to both clinicians and patients.
From a DBT perspective, the dialectical tension between acceptance and change is part of every clinical interaction. By “acceptance,” we mean acknowledging reality. Not approving of it or agreeing with it, just acknowledging the reality of something as it is. By “change,” we mean working toward something being different than it is. Ideally, we need both acceptance and change, but it is possible to get stuck “pulling on just one side of the rope.” Sometimes in intolerably painful situations, it is the change side of the rope that people get stuck exclusively pulling. Stephen could not acknowledge that he was dying and could only strive for change. In his conversations with Dr Rosenberg, he was pulling as hard as he possibly could on the change side of the rope. Dr Rosenberg was compelled to pull hard on the acceptance side of the rope in kind, to see if she could help him acknowledge the reality of his impending death. Paradoxically, and in parallel, that puts her in the position of also pulling hard for change.
The term radical acceptance means, from deep within ourselves, turning toward allowing reality to be how it already is—because it already is, whether we like it or not—rather than refusing it in all the ways we try consciously and unconsciously to refuse.
Knowing that it would have been difficult to do, with both an expectant medical team and the likelihood of Stephen’s imminent death waiting just outside the door, I wonder how it would have felt to “let go of the rope” and turn toward radical acceptance of the whole moment Stephen was in—that he was dying and that he could not talk about it. Sometimes letting go of trying to change the clinical moment lets us be more present inside of it. If there was no particular outcome to be achieved other than to be together and offer whatever comfort could be found, I wonder if there might have been relief in that for Stephen and for Dr Rosenberg.
Consultation-Liaison Psychiatry Perspective
Dr Theodore A. Stern
My mission, as a consultation psychiatrist, is to be practical and pithy. Although Stephen was fighting to survive, his health care providers broached the potential for a dire outcome. However, interviews targeted his psychiatric symptoms and disorders (eg, generalized anxiety disorder, death anxiety) and their pharmacologic management. Rather than pathologize him and his interactions, it might have helped to unearth his strengths.
Anxiety at the end of life does not always result from a fear of death; being dyspneic, being afraid that he would not survive until he could begin immunotherapy,23 and having doubts about Carlos’ coping capacity could have also generated distress. Not every conversation needs to focus on dying; there might also have been room for “casual conversations” and talk about what Stephen did for fun.
As with near-misses, we can perform a root-cause analysis to identify what went awry (eg, being fired from a patient’s care) and why. Being fired may be the symptom and not the problem. Were there mismatched expectations, empathic failures (due to use of personal protective equipment [PPE]), or poorly timed interactions? Was Dr Rosenberg “set up to fail” (since palliative care was called because death was near), or were COVID-19 and the required PPE interfering with their rapport? Our consultations are not all about us; however—much like a driver attending to what is happening inside and outside a car—paying attention to our thoughts, feelings, and associations during the clinical encounter, a process called autognosis (self-knowledge, or “knowing your car”), facilitates clinical care (“safe driving”) and guides communication.24
Denial is not always maladaptive (eg, walking too briskly to show that his lungs are working well) and pathological. As a businessman, Stephen might have calculated that the cost of discussing dying wasn’t worth the price. And, although he believed that he did not need to write a will or an advance directive, the best time to prepare such documents is long before one becomes ill.
Although working with people at the end of life is often challenging, crises bring opportunities; we can provide information, comfort, support, and guidance. Physicians’ qualities that are valued by patients at the end of life include competence, concern, comfort, communication, cheerfulness, consistency, and truth-telling.25 Palliative care and consultation psychiatry are art forms and science; they can be honed by practice, patience, and humility while considering biological, psychological, social, and existential components.
Psychodynamic/Palliative Care Perspective
Dr Linda Emanuel
Stephen reacted characteristically for someone who is not adjusted to the harsh reality of death and whose defenses are failing to manage fear. People better able to contemplate death may have more of the following features. They may feel that death is familiar and normal; have loved ones who have died; have an integrated and meaningful way of thinking about death in the grand scheme of things; have “holding” relationship(s) in which profoundly difficult feelings can be processed; have physical distress minimized; have avoided trauma and mental health conditions that limit relatedness; and know how to let go (grieve) and “take in” others (internalize) and be among loved ones who also know how to do so.26–28 Very few patients possess all of these, but it helps clinicians to note any that their patient does have, because these features offer ways to help manage overwhelming fear, that great impediment to non-traumatic dying.
When feelings are unmanageable, people can engage in projective identification, with one “putting onto” another the unwanted feeling (“Death is frightening; you are the death doctor; I don’t like you”) to the point that the other may “own it” and feel bad or a failure.29 Feelings travel contagiously, in this case from Stephen to Dr Rosenberg. They also morph (“I am frightened” becomes “You are bad,” and then possibly in Dr Rosenberg, “I am no good”). In such situations, patients may do best with nonverbal (we might say pre-verbal) presence, with the clinician silently acknowledging the totality of the patient.30,31
When palliative medicine is consulted, the unit of care includes not only the patient’s family but also the referring team, in part because transference of feeling from the patient to the team also occurs.32 Stephen’s palpable fear unnerved the primary team, who then asked Dr Rosenberg to hold the difficult emotions. When Stephen’s dystonic reaction made his medical team feel that their efforts had failed, their email, which publicly rendered Dr Rosenberg as the one who failed, may have served to ensure that she held as much of the difficult feeling as possible. Conceivably, Dr Rosenberg could have offered early affirmation to the referring team that some patients will not explicitly “get it.” Respecting the patient’s defenses by leaving them to continue, which occurred in the end by allowing the family and team to more explicitly face reality for Stephen, is sometimes the best available option and might have led to less acting out.
Summary: Integrative/Generalist Perspective
Dr Jonah N. Cohen
Cross Talk asks clinical questions that are important for a specific case but also have relevance for clinical care more broadly. For instance, how has PPE in COVID-19 influenced clinical work? What are the predictors of a more adaptive response to one’s death? How could Dr Rosenberg have forged a connection with Stephen, and what strategies or frameworks might a clinician use in a similar circumstance? We owe Dr Rosenberg and Stephen a debt of gratitude for allowing us a window into the profound nature of their work and for the opportunity to explore these questions.
First, Drs Rosenberg, Fishel, and Stern all discuss the potential negative impact of PPE on establishing a therapeutic connection. Stephen did not have the chance to take in Dr Rosenberg’s nonverbals, an essential element of communication particularly in the context of intense affects. Dr Fishel discusses how directly acknowledging this to Stephen may have been helpful and lists some creative workarounds (eg, written notes, Zoom, hand signals).
Second, Drs Rosenberg, Fishel, and Emanuel give us insight into (1) the importance of discussing end-of-life processes and the idea of prognostic awareness and (2) predictors of which patients will be able to approach the reality of their death with greater ease. Those who have already experienced death of a loved one, have a strong sense of relatedness, and have a framework for thinking about death typically have an easier time facing the reality of their death. Although we do not know how these characteristics apply to Stephen specifically, it is important for practitioners to be aware of these factors in their own work.
Finally, the panelists provide some suggestions about how one might approach a clinical situation in which the patient and clinician have different beliefs about what might be helpful and, as Dr Rosenberg describes, how one might build a bridge to span the yawning distance between patient and clinician. Dr Emanuel discusses projective identification, an important process by which the clinician may come to know the strong emotions that a patient has but might be unable to consciously bare. Drs Fishel, Harley, and Stern all discuss how a paradoxical intervention may have been helpful. For instance, Dr Stern discusses how initiating casual conversations and thereby taking the intense focus off death may have been helpful. Dr Fishel discusses effectively talking to Stephen through Carlos, one way of diffusing intense emotion. Dr Harley provides us with a useful theoretical framework of acceptance and change to organize these suggestions. Perhaps if Dr Rosenberg had radically accepted Stephen’s refusal to talk about the end of his life, this would have implicitly allowed Stephen to feel understood and to know that Dr Rosenberg grasped the gravity of his unbearable fear. Overall, Stephen’s case highlights several issues pertinent for treating patients at the end of life, particularly during COVID-19.
Published online: February 22, 2022.
Potential conflicts of interest: Dr Stern has received royalties from Elsevier for editing psychiatry textbooks. Dr Cohen is a board member of the Endowment for the Advancement of Psychotherapy at Massachusetts General Hospital. All other authors report no disclosures/conflicts of interest.
Funding/support: Cross Talk is financially supported by the Endowment for the Advancement of Psychotherapy at Massachusetts General Hospital.
Role of the sponsor: The funding agency had no role in the preparation, review, or approval of the manuscript or the decision to submit the manuscript for publication.
Statement of de-identification: The patient featured in this case has been de-identified, as next-of-kin were unavailable. The names of the patient and his spouse have been changed to protect confidentiality.
Clinical Points
- Intense transference is possible in clinical relationships that are not overtly psychodynamic in orientation, and it can create or endanger the therapeutic value of the care.
- The constructs of death anxiety and death panic from existential psychotherapy are active throughout the lifespan, but particularly so in times of serious illness.
- Infection control measures such as masking and social distancing have led to empathic disconnection in clinical work with seriously ill patients.
- Team-based interdisciplinary care can optimally support clinicians in difficult end-of-life cases.
References (32)

- Bernacki RE, Block SD; American College of Physicians High Value Care Task Force. Communication about serious illness care goals: a review and synthesis of best practices. JAMA Intern Med. 2014;174(12):1994–2003. PubMed CrossRef
- Kamal AH, Maguire JM, Meier DE. Evolving the palliative care workforce to provide responsive, serious illness care. Ann Intern Med. 2015;163(8):637–638. PubMed CrossRef
- Jackson VA, Jacobsen J, Greer JA, et al. The cultivation of prognostic awareness through the provision of early palliative care in the ambulatory setting: a communication guide. J Palliat Med. 2013;16(8):894–900. PubMed CrossRef
- Bernacki R, Hutchings M, Vick J, et al. Development of the Serious Illness Care Program: a randomised controlled trial of a palliative care communication intervention. BMJ Open. 2015;5(10):e009032. PubMed CrossRef
- Atkin N, Vickerstaff V, Candy B. “Worried to death”: the assessment and management of anxiety in patients with advanced life-limiting disease, a national survey of palliative medicine physicians. BMC Palliat Care. 2017;16(1):69. PubMed CrossRef
- Becker E. The Denial of Death. 1st pbk ed. Free Press; 1975.
- Yalom ID. Staring at the Sun: Overcoming the Terror of Death. Jossey-Bass; 2008.
- Willis E, Mah K, Shapiro GK, et al. Testing terror management theory in advanced cancer. Death Stud. 2021;27:1–10. PubMed CrossRef
- Kühne F, Hermann M, Preisler M, et al. Prognostic awareness in advanced disease: a review update and concept analysis. Front Psychol. 2021;12:629050. PubMed CrossRef
- Chen CH, Chen JS, Wen F-H, et al. An individualized, interactive intervention promotes terminally ill cancer patients’ prognostic awareness and reduces cardiopulmonary resuscitation received in the last month of life: secondary analysis of a randomized clinical trial. J Pain Symptom Manage. 2019;57(4):705–714.e7. PubMed CrossRef
- Tang ST, Chang WC, Chen JS, et al. Associations of prognostic awareness/acceptance with psychological distress, existential suffering, and quality of life in terminally ill cancer patients’ last year of life. Psychooncology. 2016;25(4):455–462. PubMed CrossRef
- Brenner K, Greer JA, Jackson V, et al. Development of a prognostic awareness impact scale for patients with advanced cancer. J Palliat Med. Published online October 11, 2021. PubMed CrossRef
- Janssens A, Derijcke S, Galdermans D, et al. Prognostic understanding and quality of life in patients with advanced lung cancer: a multicenter study. Clin Lung Cancer. 2019;20(3):e369–e375. PubMed CrossRef
- Gelfman LP, Sudore RL, Mather H, et al. Prognostic awareness and goals of care discussions among patients with advanced heart failure. Circ Heart Fail. 2020;13(9):e006502. PubMed
- Ariadne Labs. Serious Illness Conversation Guide. https://www.ariadnelabs.org/wp-content/uploads/2017/05/SI-CG-2017-04-21_FINAL.pdf. 2015. Revised April 2017. Accessed February 8, 2022.
- Fleming J. Teaching the basic skills of psychotherapy. Arch Gen Psychiatry. 1967;16(4):416–426. PubMed CrossRef
- Lundh LG, Falkenström F. Towards a person-oriented approach to psychotherapy research. J Pers Oriented Res. 2019;5(2):65–79. PubMed CrossRef
- Jacobsen J, Brenner K, Greer JA, et al. When a patient is reluctant to talk about it: a dual framework to focus on living well and tolerate the possibility of dying. J Palliat Med. 2018;21(3):322–327. PubMed CrossRef
- Sontag S. Illness as Metaphor. Farrar, Straus, and Giroux; 1978.
- Wright AA, Zhang B, Ray A, et al. Associations between end-of-life discussions, patient mental health, medical care near death, and caregiver bereavement adjustment. JAMA. 2008;300(14):1665–1673. PubMed CrossRef
- Gawande A. Being Mortal: Medicine and What Matters in the End. Metropolitan Books; 2014.
- Keeley MP, Generous MA. Final conversations: overview and practical implications for patients, families, and healthcare workers. Behav Sci (Basel). 2017;7(2):17–26. PubMed CrossRef
- Reynolds KL, Cohen JV, Zubiri L, et al, eds. Facing Immunotherapy: A Guide for Patients and their Families. Massachusetts General Hospital Psychiatry Academy; 2020.
- Stern TA, Prager LM, Cremens MC. Autognosis rounds for medical house staff. Psychosomatics. 1993;34(1):1–7. PubMed CrossRef
- Cassem NH, Brendel RW. End of life issues: Principles of care and ethics. In: Stern TA, Fricchione GL, Cassem NH, et al, eds. Massachusetts General Hospital Handbook of General Hospital Psychiatry. 5th ed. Mosby/Elsevier; 2004.
- Emanuel LL, Reddy N, Hauser J, et al. And yet it was a blessing: the case for existential maturity. J Palliat Med. 2017;20(4):318–327. PubMed CrossRef
- Emanuel L, Brody S. Psychodynamic therapy in the terminally ill. In: Chochinov HM, Breitbart W, eds. Handbook of Psychiatry in Palliative Medicine. 2nd ed. Oxford University Press. Forthcoming.
- Winnicott DW. Fear of breakdown. Int Rev Psychoanal. 1974;1:103–107.
- Klein M. Mourning and its relation to manic depressive states. In: Klein M, ed. The Writings of Melanie Klein. Vol. 1, Love Guilt and Reparation (1921–1945). The Free Press; 1940:344–369.
- Bion WR. Learning From Experience. Karnac; 1984.
- Bergstein A. Attacks on linking or a drive to communicate? tolerating the paradox. Psychoanal Q. 2015;84(4):921–942. PubMed CrossRef
- Brenner KO, Jacobsen JC, Emanuel LL. Referral relationship: illuminating the ways palliative care creates a holding environment for referring clinicians. J Palliat Med. Published online January 11, 2022. CrossRef
This PDF is free for all visitors!