Articles are selected for credit designation based on an assessment of the educational needs of CME participants, with the purpose of providing readers with a curriculum of CME articles on a variety of topics throughout each volume. Activities are planned using a process that links identified needs with desired results.
To obtain credit, read the article, correctly answer the questions in the Posttest, and complete the Evaluation. A $10 processing fee will apply.
After studying this article, you should be able to:
The CME Institute of Physicians Postgraduate Press, Inc., is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians.
The CME Institute of Physicians Postgraduate Press, Inc., designates this journal-based CME activity for a maximum of 1 AMA PRA Category 1 Creditâ„¢. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Note: The American Academy of Physician Assistants (AAPA) accepts certificates of participation for educational activities certified for AMA PRA Category 1 Creditâ„¢ from organizations accredited by ACCME or a recognized state medical society. Physician assistants may receive a maximum of 1 hour of Category I credit for completing this program.
This educational activity was published in May 2019 and is eligible for AMA PRA Category 1 Creditâ„¢ through June 30, 2021. The latest review of this material was April 2019.
All individuals in a position to influence the content of this activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past year, Marlene P. Freeman, MD, Editor in Chief, has received research funding from JayMac and Sage; has been a member of the advisory boards for Otsuka, Alkermes, and Sunovion; has been a member of the Independent Data Safety and Monitoring Committee for Janssen; and, as a Massachusetts General Hospital (MGH) employee, works with the MGH National Pregnancy Registry, which is sponsored by Teva, Alkermes, Otsuka, Actavis, and Sunovion, and works with the MGH Clinical Trials Network and Institute, which receives research funding from multiple pharmaceutical companies and the National Institute of Mental Health. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure appears at the end of the article.
Objective: This study examines the effects of sex and pubertal status on the association between attention-deficit/hyperactivity disorder (ADHD) and depression symptoms in preadolescence through late adolescence.
Methods: Participants were 472 youth from the Multimodal Treatment Study of Children With ADHD. The study sample included 308 youth with DSM-IV ADHD, recruited from 1993 through 1996, and 164 comparison youth who were recruited approximately 2 years later. Self-reported depression symptoms from the Children’s Depression Inventory and pubertal status from the Tanner Self-Report Scale were collected, along with combined parent-teacher reports of ADHD. Regression analyses examined the impact of ADHD, sex, pubertal status, and their interactions on total depression symptoms and related subscales (ie, negative mood, interpersonal problems, ineffectiveness, anhedonia, and negative self-esteem) in preadolescence. Next, path models examined associations between ADHD, sex, and pubertal status on depression symptoms into middle and late adolescence.
Results: In preadolescence, significant ADHD ×— sex ×— puberty interactions emerged for total depression symptoms and anhedonia (P < .05). Higher levels of ADHD severity were associated with higher levels of depression in early maturing girls and later maturing boys. Effects appear to be driven by anhedonia. Longitudinal effects emerged showing that total depression symptoms and anhedonia in preadolescence predicted levels of each respective outcome into late adolescence.
Conclusions: Sex and pubertal status meaningfully impact the association between ADHD and depression symptoms in youth and should be considered in future work and treatment.

CME Background
Articles are selected for credit designation based on an assessment of the educational needs of CME participants, with the purpose of providing readers with a curriculum of CME articles on a variety of topics throughout each volume. Activities are planned using a process that links identified needs with desired results.
To obtain credit, read the article, correctly answer the questions in the Posttest, and complete the Evaluation. A $10 processing fee will apply.
CME Objective
After studying this article, you should be able to:
- Consider the impact of sex and pubertal status on the association between ADHD and depression symptoms in young patients
Accreditation Statement
The CME Institute of Physicians Postgraduate Press, Inc., is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians.
Credit Designation
The CME Institute of Physicians Postgraduate Press, Inc., designates this journal-based CME activity for a maximum of 1 AMA PRA Category 1 Creditâ„¢. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Note: The American Academy of Physician Assistants (AAPA) accepts certificates of participation for educational activities certified for AMA PRA Category 1 Creditâ„¢ from organizations accredited by ACCME or a recognized state medical society. Physician assistants may receive a maximum of 1 hour of Category I credit for completing this program.
Release, Expiration, and Review Dates
This educational activity was published in May 2019 and is eligible for AMA PRA Category 1 Creditâ„¢ through June 30, 2021. The latest review of this material was April 2019.
Financial Disclosure
All individuals in a position to influence the content of this activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past year, Marlene P. Freeman, MD, Editor in Chief, has received research funding from JayMac and Sage; has been a member of the advisory boards for Otsuka, Alkermes, and Sunovion; has been a member of the Independent Data Safety and Monitoring Committee for Janssen; and, as a Massachusetts General Hospital (MGH) employee, works with the MGH National Pregnancy Registry, which is sponsored by Teva, Alkermes, Otsuka, Actavis, and Sunovion, and works with the MGH Clinical Trials Network and Institute, which receives research funding from multiple pharmaceutical companies and the National Institute of Mental Health. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure appears at the end of the article.
ABSTRACT
Objective: This study examines the effects of sex and pubertal status on the association between attention-deficit/hyperactivity disorder (ADHD) and depression symptoms in preadolescence through late adolescence.
Methods: Participants were 472 youth from the Multimodal Treatment Study of Children With ADHD. The study sample included 308 youth with DSM-IV ADHD, recruited from 1993 through 1996, and 164 comparison youth who were recruited approximately 2 years later. Self-reported depression symptoms from the Children’s Depression Inventory and pubertal status from the Tanner Self-Report Scale were collected, along with combined parent-teacher reports of ADHD. Regression analyses examined the impact of ADHD, sex, pubertal status, and their interactions on total depression symptoms and related subscales (ie, negative mood, interpersonal problems, ineffectiveness, anhedonia, and negative self-esteem) in preadolescence. Next, path models examined associations between ADHD, sex, and pubertal status on depression symptoms into middle and late adolescence.
Results: In preadolescence, significant ADHD ×— sex ×— puberty interactions emerged for total depression symptoms and anhedonia (P < .05). Higher levels of ADHD severity were associated with higher levels of depression in early maturing girls and later maturing boys. Effects appear to be driven by anhedonia. Longitudinal effects emerged showing that total depression symptoms and anhedonia in preadolescence predicted levels of each respective outcome into late adolescence.
Conclusions: Sex and pubertal status meaningfully impact the association between ADHD and depression symptoms in youth and should be considered in future work and treatment.
J Clin Psychiatry 2019;80(3):18m12548
To cite: Babinski DE, Waschbusch DA, Waxmonsky JG. Sex and pubertal status moderate the association between ADHD and depression symptoms: an examination from preadolescence through late adolescence. J Clin Psychiatry. 2019;80(3):18m12548.
To share: https://doi.org/10.4088/JCP.18m12548
© Copyright 2019 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Penn State College of Medicine, Hershey, Pennsylvania
*Corresponding author: Dara E. Babinski, PhD, Department of Psychiatry, 22 Northeast Dr, Hershey, PA 17033 ([email protected]).
Up to 50% of individuals with attention-deficit/hyperactivity disorder (ADHD) also have a depression diagnosis in their lifetime,1,2 an incidence rate more than twice that of the general population.3 ADHD and depression are each associated with a range of impairments, including academic underachievement, interpersonal dysfunction, and substance use initiation and problems. However, the co-occurrence of ADHD and depression is associated with even greater adversity than either ADHD or depression alone, including more suicide attempts, inpatient hospitalizations, and substance abuse.1,4 Despite the high risk for depression, not all youth with ADHD develop mood difficulties.5,6 Identifying which children are at highest risk for developing depression is critical.
Studies linking ADHD and depression have predominantly included boys,2 as clinic-referred samples are disproportionately composed of more boys than girls.7 Yet, emerging work suggests that girls with ADHD may be at greater risk for depression than boys.1,8,9 For example, one large prospective longitudinal study of girls with (n = 140) and without (n = 122) ADHD demonstrated that 65% of girls with ADHD versus 21% of girls without ADHD developed depression in adolescence/young adulthood, and girls with ADHD experienced earlier onset (ie, 9.7 vs 12.6 years old), more recurrent depression, and more suicide attempts and psychiatric hospitalizations compared to girls without ADHD.1 Another sample of girls with (n = 140) and without (n = 88) ADHD also evidenced heightened risk for depression in adolescence10 and young adulthood,9 as well as significantly higher rates of self-harm and suicide attempts by young adulthood (average age, 19.6 years).9 Self-harm and suicide attempts emerged most clearly among girls manifesting the hyperactive/impulsive versus inattentive ADHD subtype, although effects of ADHD subtype on depression severity or diagnosis were not apparent.9 However, whether or not the risk for depression is specific to girls versus boys with ADHD has received very little study. As one exception, Chronis-Tuscano and colleagues8 examined 125 children with ADHD along with 123 demographically matched children without ADHD. Although the sample included only 18 girls with ADHD, girls with ADHD demonstrated the highest risk for depression and suicide attempts by age 18 compared to other groups, and this sex difference emerged in early adolescence.
Beginning in adolescence, depression emerges prominently for girls, regardless of ADHD, with twice as many girls meeting diagnostic criteria for depression compared to boys.11 Given the salience of early adolescent developmental changes associated with the onset of puberty, researchers have focused on the role of pubertal development to explain the dramatic sex-specific rise in depression symptoms and have highlighted early pubertal maturation as a risk factor for depression in girls.12-15 For example, weight gain, breast development, and menarche meaningfully impact how girls interact with their environment, particularly with peers, and how girls view themselves. Work in this area has most often examined girls; however, prior to the onset of puberty, boys manifest higher levels of depression compared to girls, and more advanced pubertal development has sometimes been associated with decreases in depression for boys.16,17 Contrasting effects of early puberty in boys have also emerged, with some data showing increases in depression13 and other data indicating no effect on depression. 14
Although the effects of early puberty on depression may be more pronounced for girls than boys, it is not clear that early puberty in and of itself is associated with depression. Instead, support has emerged for an accentuation model,18,19 whereby early pubertal status is associated with depression in girls when other risk factors are present, including ineffective coping and childhood conduct problems.12,19 While we are not aware of work that has specifically examined the effects of childhood ADHD and early pubertal status on depression in girls, ADHD and conduct problems are highly comorbid,1 suggesting that ADHD may also be associated with high risk for depression among early maturing girls. Importantly, the emergence of depression in adolescence increases the risk for ongoing difficulties with depression across the life course,1,20 and there is some evidence that early pubertal development has long-lasting effects on the risk for depression,21 especially among early maturing girls with behavioral difficulties.12 Research is needed to clarify the role of pubertal development in the association between ADHD and depression from preadolescence through late adolescence.
Depression is a heterogeneous disorder, and examining dimensions of depression may further clarify the relation between ADHD, early puberty, and sex on depression symptoms to identify important targets for prevention and intervention. Depressed mood and anhedonia (ie, low positive affect and lack of pleasure in activities) are the core features of depression, and girls more frequently manifest depressed mood while boys more frequently manifest anhedonia.22 However, both girls and boys with ADHD are at particular risk for manifesting anhedonia,23 and pubertal development has been shown to impact the neural circuitry associated with anhedonia and reward responsiveness in both boys and girls.24 To our knowledge, the impact of ADHD, sex, and pubertal status on other facets of depression, including feelings of ineffectiveness, negative self-esteem, and interpersonal problems, has not been examined. However, self-esteem difficulties and interpersonal concerns emerge more prominently for girls compared to boys in adolescence,25 and early pubertal development may increase risk for these problems in girls with ADHD. Furthermore, these increased difficulties for girls with ADHD may lead to greater feelings of ineffectiveness.
The goal of this study was to examine sex and pubertal status as moderators of associations between ADHD and depression symptoms in girls and boys from preadolescence through late adolescence. ADHD was considered dimensionally, using a total symptom severity score derived from maternal and teacher ratings. Additionally, total depression symptoms were considered, as were dimensions of depression, including negative mood, interpersonal problems, ineffectiveness, anhedonia, and negative self-esteem. It was hypothesized that higher levels of ADHD (ie, greater total ADHD symptom severity) would be associated with greater depressive symptoms in preadolescence and that girls, particularly early maturing girls, would demonstrate the most elevated depression scores. The effects of sex and pubertal development on the longitudinal association between ADHD symptom severity and depressive symptomatology were hypothesized to extend into adolescence and late adolescence. However, specific hypotheses about which subscales would be most relevant for youth with high levels of ADHD were not made, due to the limited extant research in this area, although we expected that anhedonia may emerge as particularly relevant for youth with high levels of ADHD. Specific hypotheses were not made regarding boys, ADHD, early pubertal status, and depression symptoms given mixed findings.13,14,16
METHODS
Data from the Multimodal Treatment Study of Children with ADHD (MTA) were analyzed. The MTA is a large multisite trial of 3 treatments—pharmacologic, behavioral, and their combination—as well as a community control, delivered over 14 months to children with DSM-IV ADHD, combined type.26 Youth with ADHD were recruited from 1993 through 1996. At the onset of treatment, the MTA included 579 children ages 7.0-9.9 years (mean age = 8.2 years), in first through fourth grades. Previous research provides more in-depth description of the sample, which was 80% male and 61% white.26
Upon completion of the treatment study, children with ADHD and their parents were invited to participate in a follow-up study to assess the long-term outcomes of children with ADHD. Approximately 2 years after the initial recruitment of children with ADHD, a comparison group of 289 was also recruited. Children in this group, referred to as the local normative comparison group (LNCG), were recruited to reflect the local populations from which the MTA sample was drawn. LNCG children were selected from the same schools and grades and in the same proportion of girls and boys as MTA children and were not excluded for the presence of ADHD. The LNCG had the same entry criteria as the MTA children except for ADHD diagnosis and age; they were matched to the age of children with ADHD who had participated in the MTA treatment trial 24 months after initiating the MTA study.
Children with ADHD, puberty, and depression symptom ratings at the preadolescent (ie, 36 month follow-up) wave were included in this study. Pubertal data were available on a portion of the sample.27 Thus, the current study included 250 boys and 58 girls previously treated for ADHD and 131 boys and 33 girls in the LNCG. Data collected at the 36 (preadolescence, mean age = 11.39 years, SD = 0.86), 72 (adolescence, mean age = 14.48 years, SD = 0.94), and 96 (late adolescence, mean age = 16.12 years, SD = 0.72) month waves were used. No differences in baseline characteristics have been found between MTA children retained and not retained at the 36 month follow-up wave.28 Follow-up data from this cohort of youth were available for 426 (90.3%) at 72 months and 350 (74.2%) at 96 months.
Measures
ADHD and oppositional defiant disorder symptoms. The Swanson, Nolan, and Pelham scale (SNAP) assessed DSM-IV ADHD and oppositional defiant disorder (ODD) symptoms26 at 36 months and includes 18 ADHD items and 8 ODD items, rated on a 4-point scale: 0 (not at all), 1 (just a little), 2 (quite a bit), or 3 (very much). The ADHD and ODD total symptom scores were averaged from maternal and teacher reports. The SNAP has been used widely and has demonstrated adequate psychometric properties.29
Pubertal status. The Tanner Self-Report Scale assessed pubertal development at 36 months. Children rated 5 items about their sexual maturation, including their overall sexual maturation and rate of pubertal development in the past 6 weeks. Children were also presented with pictures reflecting pubertal stages. Girls were asked to select which picture reflected their current breast and pubic hair development, and boys selected pictures reflecting development of genital and pubic hair development. Items were scored from 1 to 5 and averaged, with higher mean scores indicating more mature development.30 Stage 2 represents puberty onset, whereas stage 3 represents more advanced and overt signs of puberty. Previous work within the MTA sample has shown large child self-report-clinician Tanner rating correlations.27
Depression symptoms. The Children’s Depression Inventory (CDI)31 includes 27 items asking children to select one of 3 statements that best describes their current thoughts or behaviors. Items are scored from 0 to 2, with higher scores indicating greater depression severity. The CDI is a widely used measure of child depression symptoms and has demonstrated adequate psychometric properties.32,33 Total scores above 13 are consistent with clinical levels of depression.33 The CDI also includes 5 subscales, including negative mood, interpersonal problems, ineffectiveness, anhedonia, and negative self-esteem.
Medication treatment history. The Services for Children and Adolescents-Parent Interview34 assessed history of medication treatment of children with ADHD. Following Swanson and colleagues,35 a minimum medication regimen of at least 10 mg/d of stimulant medication for at least 50% of the days since the previous assessment was defined (ie, yes or no) at each of the waves. Participants were categorized into 3 long-term patterns of medication treatment: consistent (ie, meeting the minimum medication regimen requirement at each interval), inconsistent (ie, meeting the minimum medication regimen in some but not all intervals), and negligible (ie, not meeting the minimum medication regimen in any of the intervals).
Data Analytic Plan
Bivariate associations between preadolescent ADHD severity, sex, and pubertal status with all depression variables were quantified. In these analyses, only variables collected in preadolescence (ie, 36 months) were examined. Next, also using only preadolescent variables, ADHD symptom severity, sex, and pubertal status and their interactions were regressed onto each depression scale using centered independent variables. Significant 3-way and 2-way interactions were followed up using simple slopes tests and slopes difference tests using values of the variables 1 standard deviation above and below their mean value. Thus, the high ADHD score used was 29.56 (calculated by the mean plus 1 standard deviation: 17.52 + 12.04) while the low ADHD score was 5.48 (calculated by the mean minus 1 standard deviation: 17.52 – 12.04). The early puberty score was 3.50 (calculated by the sample pubertal development mean plus 1 standard deviation: 2.86 + 0.64), while the late puberty score was 2.22 (calculated by the sample puberty mean minus 1 standard deviation: 2.86 – 0.64). Dummy coding (ie, 0 = male, 1 = female) was used for the categorical youth sex variable. Given the high comorbidity between ADHD and ODD,1,36 and robust associations between childhood ODD and depression,37 analyses controlled for ODD severity. Medication treatment history (up to the 36 month wave) was also included as a covariate. Study site, verbal IQ, and race were considered as covariates, but none of these variables impacted results, and they were omitted from final analyses.
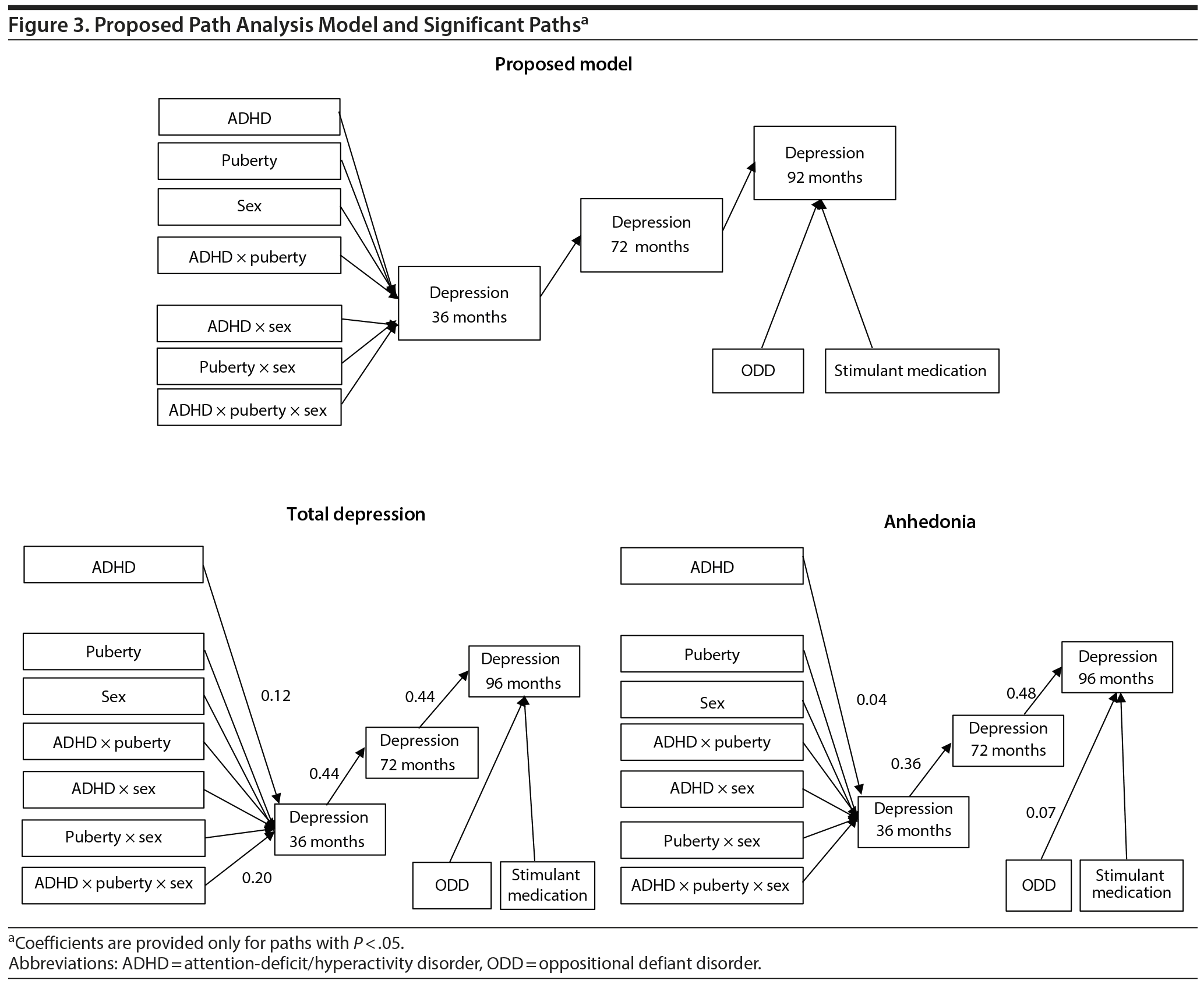
Significant 3-way interactions identified in preadolescence were examined longitudinally using data collected at 72 and 96 months. Path analysis, computed using SPSS AMOS 24 (IBM; Armonk, NY), tested models in which ADHD severity, sex, pubertal status, and their interactions were entered as independent variables to predict depression symptoms over time (see Figure 3 for the proposed model). Direct paths from independent variables to depression at 36 months, with subsequent paths to depression at 72 and 96 months, were examined. ODD severity in preadolescence and stimulant medication history (up to 96 months) were included as covariates. Full information maximum likelihood estimation accommodated missing data.
RESULTS
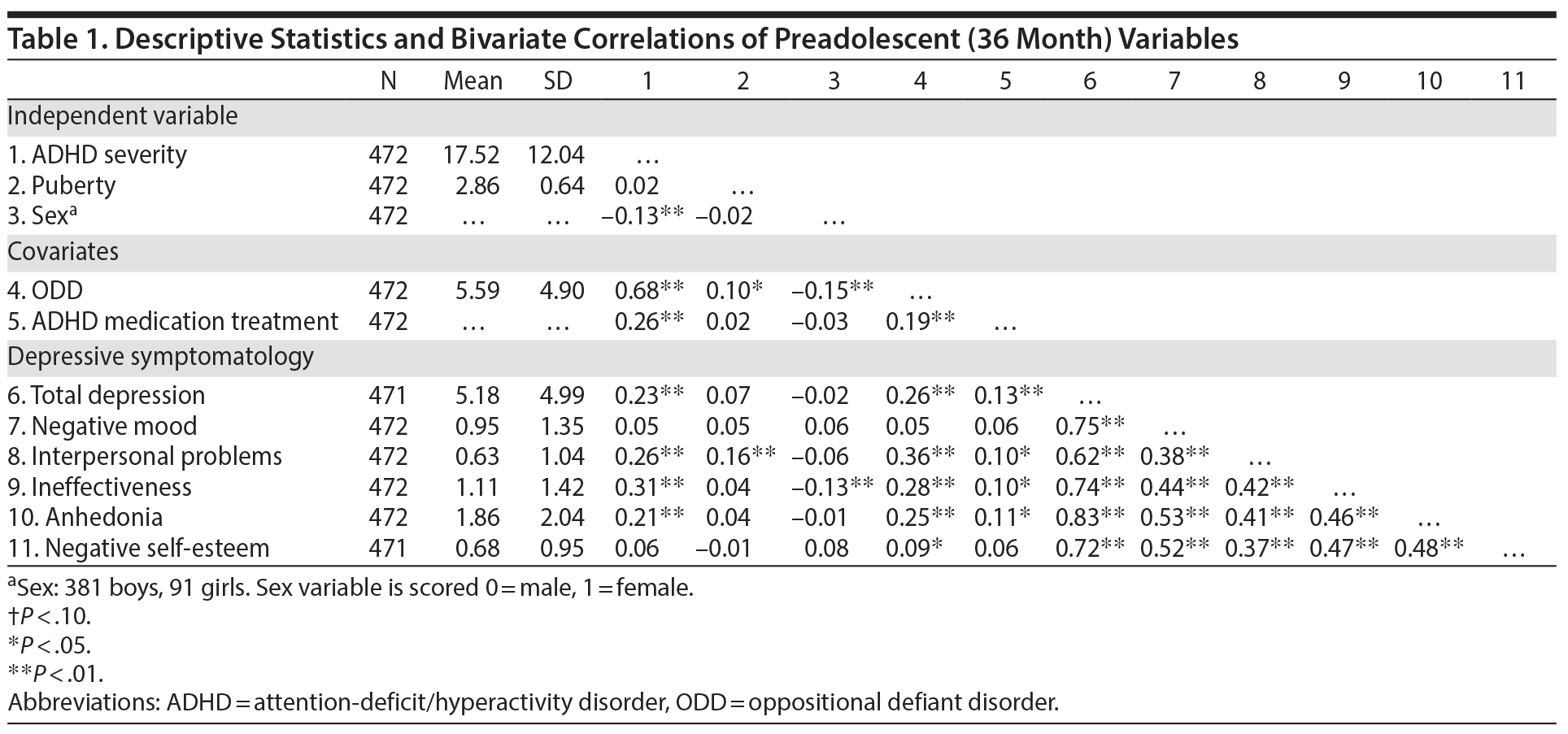
Descriptive statistics and bivariate correlations among preadolescent (ie, 36 months) variables appear in Table 1. A significant correlation emerged between ADHD severity and total depression, interpersonal problems, ineffectiveness, and anhedonia. Pubertal maturation was associated with greater interpersonal problems, and male sex was associated with higher ratings of ineffectiveness.
ADHD and Preadolescent Depression Symptoms: Moderation by Sex and Pubertal Status
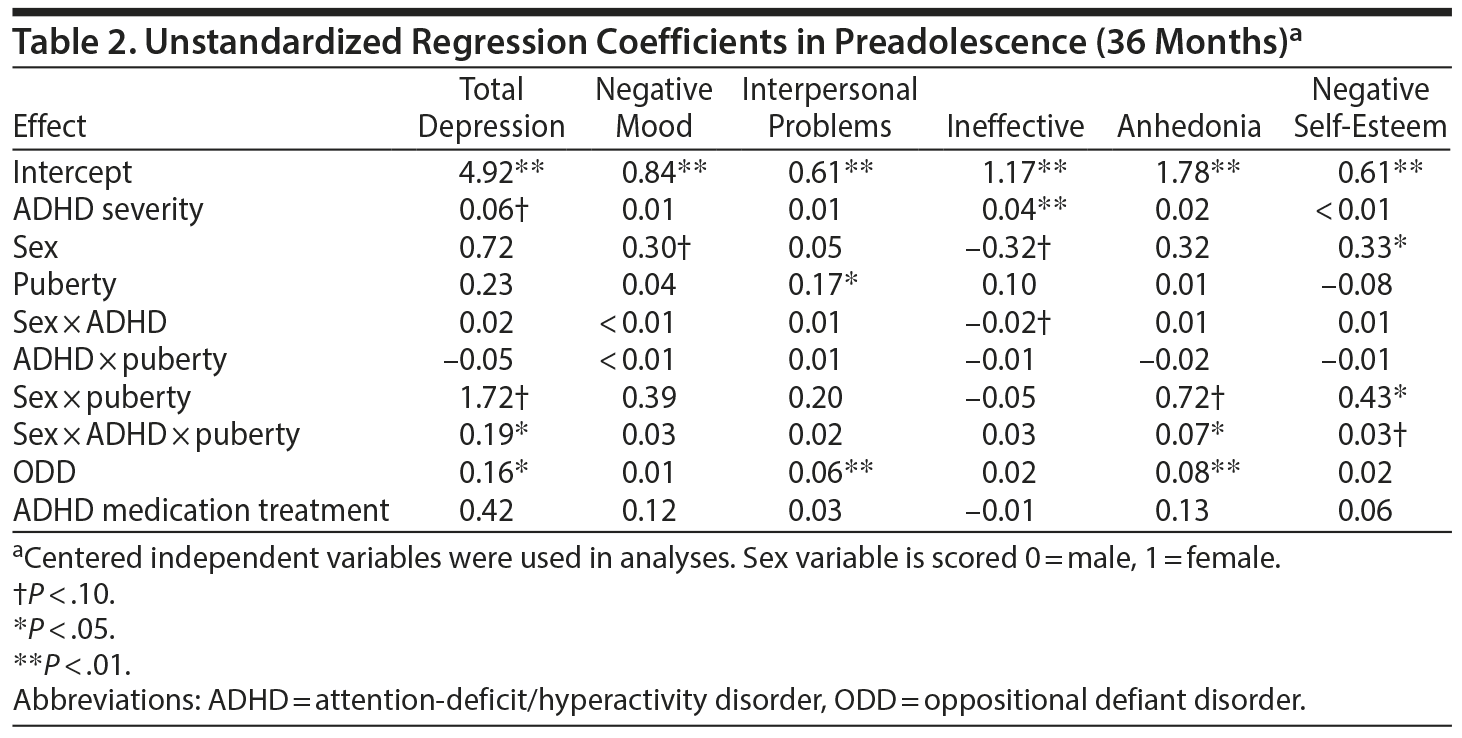
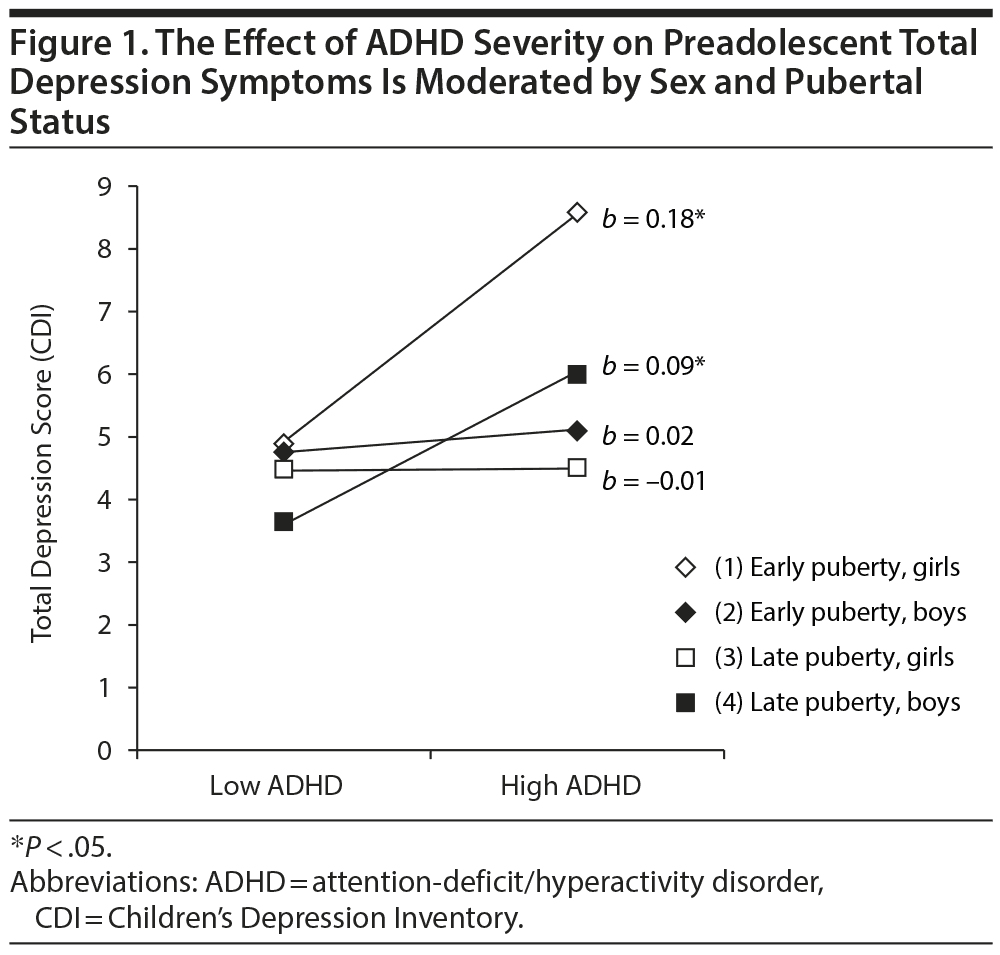
Total depression symptoms. Regressions examining associations between ADHD and depression variables are described in Table 2. An ADHD ×— sex ×— puberty interaction emerged for total depression (Figure 1). Greater ADHD severity was associated with greater depression for early maturing girls and later maturing boys. For later maturing girls and early maturing boys, ADHD and depression symptoms were not associated.
Negative mood. ADHD severity, sex, and pubertal status were not significantly associated with negative mood.
Interpersonal problems. Greater pubertal maturation was associated with greater interpersonal problems. No effects of ADHD severity or sex emerged.
Ineffectiveness. Higher levels of ADHD were related to greater ineffectiveness. No effects of pubertal status or sex emerged.
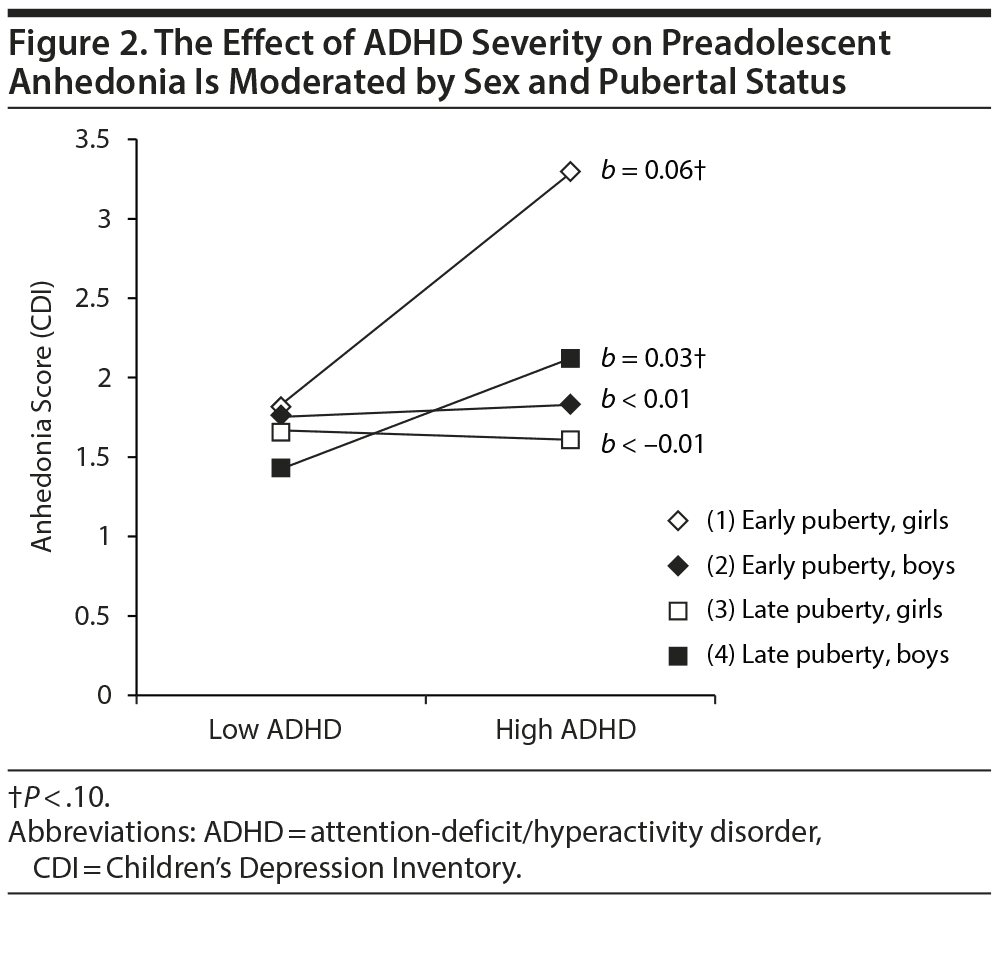
Anhedonia. An ADHD ×— sex ×— puberty interaction emerged (Figure 2). Greater ADHD severity was marginally significantly associated with greater anhedonia for later maturing boys. Among early maturing girls, ADHD severity was marginally associated with greater anhedonia. ADHD and anhedonia were not significantly associated for early maturing boys or later maturing girls.
Negative self-esteem. A sex ×— puberty interaction emerged. Negative self-esteem increased (b = 0.14, P < .001) for early versus later maturing girls, whereas negative self-esteem decreased for early versus later maturing boys (b = -0.28, P = .022). There was no effect of ADHD severity.
ADHD and Depression Symptoms Into Late Adolescence
Based on the 3-way interactions that emerged related to total depression and anhedonia, path models were examined in these two domains (Figure 3). For total depression, the model demonstrated good fit (χ219 = 45.07, P < .01; root mean square error of approximation [RMSEA] = 0.05 [0.03-0.07]; comparative fit index [CFI] = 0.98). Depression symptoms at 36 months predicted 72 month depression symptoms, which subsequently predicted 96 month depression symptoms. The anhedonia path model also exhibited good fit (χ219 = 42.60, P < .01; RMSEA = 0.05 [0.03-0.07]; CFI = 0.98). A significant path emerged from the 3-way interaction between ADHD, sex, and puberty to 36 month anhedonia, which subsequently predicted 72 month anhedonia, which in turn predicted 96 month anhedonia.
DISCUSSION
In preadolescence, sex and pubertal status moderated the relation between ADHD and total depression symptoms and anhedonia. For early maturing girls, ADHD was associated with greater depression and marginally associated with greater anhedonia, even when controlling for ODD severity and stimulant medication use. For later maturing boys, greater ADHD was significantly associated with greater total depression symptoms and marginally associated with anhedonia. The effects of sex and pubertal status on depression symptoms and anhedonia in preadolescence were predictive of depression and anhedonia scores into adolescence and late adolescence.
These findings extend work showing higher rates of depression in girls with versus without ADHD in adolescence and young adulthood,1,8,9 to identify early puberty as an important consideration. Anhedonia appeared to be the most relevant subscale for early maturing girls with ADHD, which contrasts some work showing that depressed mood and negative affect are particularly relevant for girls.22 While girls with ADHD were the main focus of the study, effects in boys also emerged. Among later maturing boys, greater ADHD was associated with greater depression, and anhedonia scores apparently were driving this effect. Anhedonia is a strong predictor of major depressive disorder38 and overall impairment, including suicidality,39 and affective neuroscience work suggests that pubertal-related changes in reward responsivity underlie the manifestation of anhedonia.38 Yet more work is needed to clarify the differential effects of pubertal status on depression in girls versus boys with ADHD.
Preadolescent depression and anhedonia significantly predicted respective scores into adolescence, and adolescent scores subsequently significantly predicted late adolescent scores, pointing to the long-term effects of pubertal development on mood.12 Early pubertal status has been associated with a broad range of additional long-term negative outcomes in girls beyond depression, including conduct problems, earlier onset of alcohol use, sexual initiation, and early pregnancy,40 and depression has been identified as a contributing factor in these outcomes.41 Thus, additional attention to understanding the effects of pubertal status on depression in girls and boys with ADHD has far reaching implications.
Although ADHD and depression symptoms were significantly associated, the level of self-reported depression, even among early maturing girls with ADHD, was below the clinical cutoff.33 This was unexpected, because previous reports show significant depression in youth in preadolescence,20 particularly girls with ADHD.36 However, much of this work has measured depression using clinical interviews with parents and children, which may provide more information than child self-report alone. Despite the generally low CDI scores documented in preadolescence in the MTA, similar preadolescent CDI scores have been documented in the largest study of girls with ADHD,36 and prospective longitudinal studies from that sample show pronounced risk for depression, suicidality, and self-harm as girls age into adolescence and young adulthood.9 Thus, subclinical depression scores may still be meaningful, as subthreshold depressive symptoms are associated with long-term risk for depression20 and suicidal behavior42 and a number of treatment studies point to the value of intervention targeting subthreshold depression as a way to mitigate risk for major depressive disorder.43
Additional limitations are important to mention. First, puberty assessments beyond self-report were not included. Second, the MTA included only children diagnosed with the combined subtype of ADHD, limiting generalizability to other ADHD presentations. Third, most children in the MTA received evidence-based treatment for ADHD, either stimulant medication and/or behavior modification over an extended period of time, and it may be that treatments for ADHD are protective against depression.44 Relatedly, there is some evidence that ADHD may be associated with earlier maturation, although stimulant medication may delay growth. Findings regarding growth in the MTA have been mixed.27,45 We controlled for medication history as we believed this question was beyond the scope of our work.
The heightened preadolescent depression and anhedonia among early maturing girls with ADHD and later maturing boys with ADHD highlights the importance of future work that examines the developmental trajectories of girls and boys with ADHD. Although more work is needed to replicate and extend these findings, this work suggests that it may be important for clinicians to consider sex and pubertal status in boys and girls with ADHD. Attention to sex and pubertal status may identify trajectories of risk for depression that may require heightened monitoring and treatment. Treatments addressing anhedonia in early maturing preadolescent girls with ADHD and later maturing boys with ADHD, such as behavioral activation, may hold particular promise for mitigating long-term depression risk for girls and boys with ADHD.46 Continued examination of the risk for depression among girls and boys with ADHD and factors that exacerbate or mitigate this risk is greatly needed.
Submitted: August 28, 2018; accepted November 30, 2018.
Published online: May 21, 2019.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Financial disclosure: In the past 3 years, Dr Waxmonsky has received research funding from National Institutes of Health, Supernus, and Pfizer and served on the advisory boards for Noven, Ironshore, NLS Pharma, and Purdue Pharma. Dr Babinski has received research support from Purdue Pharma. Dr Waschbusch has no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: Dr Babinski’s research was supported by the Eunice Kennedy Shriver National Institute of Child Health and Human Development of the National Institutes of Health under Building Interdisciplinary Research Careers in Women’s Health award number K12HD055882.
Disclaimer: This presentation reflects the views of the authors and may not reflect the opinions or views of the MTA 192 Study Investigators or the National Institutes of Health.
Additional information: Data used in the preparation of this article were obtained from the limited access datasets distributed from the National Institutes of Health-supported Multimodal Treatment Study of Children with Attention-Deficit/Hyperactivity Disorder (MTA). This is a multisite, clinical trial and long-term follow-up study of children with ADHD who were randomly assigned to one of 4 treatment modalities. The study was conducted by the MTA Cooperative Group and supported by the National Institute of Mental Health with funds also contributed by the National Institute of Drug Abuse, the Department of Justice, and the Department of Education. The MTA Study has been supported by the following grant numbers: U01MH50440, U01MH50447, U01MH50453, U01MH50454, U01MH50461, and U01MH50467 and the following contract numbers: N01MH19204, N01MH19207, N01MH19208, N01MH19209, N01MH19210, N01MH19211, N01MH19212, HHSN271920800003-C, HHSN271920800004-C, HHSN271920800005-C, HHSN271920800006-C, HHSN271920800007-C, HHSN271920800008-C, and HHSN271920800009-C. The ClinicalTrials.gov identifier is NCT00000388.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
REFERENCES
1. Biederman J, Ball SW, Monuteaux MC, et al. New insights into the comorbidity between ADHD and major depression in adolescent and young adult females. J Am Acad Child Adolesc Psychiatry. 2008;47(4):426-434. PubMed CrossRef
2. Meinzer MC, Pettit JW, Viswesvaran C. The co-occurrence of attention-deficit/hyperactivity disorder and unipolar depression in children and adolescents: a meta-analytic review. Clin Psychol Rev. 2014;34(8):595-607. PubMed CrossRef
3. Kessler RC, Berglund P, Demler O, et al; National Comorbidity Survey Replication. The epidemiology of major depressive disorder: results from the National Comorbidity Survey Replication (NCS-R). JAMA. 2003;289(23):3095-3105. PubMed CrossRef
4. Riggs PD, Mikulich SK, Whitmore EA, et al. Relationship of ADHD, depression, and non-tobacco substance use disorders to nicotine dependence in substance-dependent delinquents. Drug Alcohol Depend. 1999;54(3):195-205. PubMed CrossRef
5. Bagwell CL, Molina BSG, Kashdan TB, et al. Anxiety and mood disorders in adolescents with childhood attention-deficit/hyperactivity disorder. J Emot Behav Disord. 2006;14(3):178-187. CrossRef
6. Molina BSG, Hinshaw SP, Swanson JM, et al; MTA Cooperative Group. The MTA at 8 years: prospective follow-up of children treated for combined-type ADHD in a multisite study. J Am Acad Child Adolesc Psychiatry. 2009;48(5):484-500. PubMed CrossRef
7. Babinski DE, Waschbusch DA. The interpersonal difficulties of women with ADHD. ADHD Rep. 2016;24(7):1-8. CrossRef
8. Chronis-Tuscano A, Molina BSG, Pelham WE, et al. Very early predictors of adolescent depression and suicide attempts in children with attention-deficit/hyperactivity disorder. Arch Gen Psychiatry. 2010;67(10):1044-1051. PubMed CrossRef
9. Hinshaw SP, Owens EB, Zalecki C, et al. Prospective follow-up of girls with attention-deficit/hyperactivity disorder into early adulthood: continuing impairment includes elevated risk for suicide attempts and self-injury. J Consult Clin Psychol. 2012;80(6):1041-1051. PubMed CrossRef
10. Hinshaw SP, Owens EB, Sami N, et al. Prospective follow-up of girls with attention-deficit/hyperactivity disorder into adolescence: Evidence for continuing cross-domain impairment. J Consult Clin Psychol. 2006;74(3):489-499. PubMed CrossRef
11. Nolen-Hoeksema S, Girgus JS. The emergence of gender differences in depression during adolescence. 1994;115(3):424-443.
12. Copeland W, Shanahan L, Miller S, et al. Outcomes of early pubertal timing in young women: a prospective population-based study. Am J Psychiatry. 2010;167(10):1218-1225. PubMed CrossRef
13. Ge X, Conger RD, Elder GHJ Jr. Pubertal transition, stressful life events, and the emergence of gender differences in adolescent depressive symptoms. Dev Psychol. 2001;37(3):404-417. PubMed CrossRef
14. Kaltiala-Heino R, Kosunen E, Rimpelפ M. Pubertal timing, sexual behaviour and self-reported depression in middle adolescence. J Adolesc. 2003;26(5):531-545. PubMed CrossRef
15. Mendle J, Turkheimer E, Emery RE. Detrimental psychological outcomes associated with early pubertal timing in adolescent girls. Dev Rev. 2007;27(2):151-171. PubMed CrossRef
16. Angold A, Costello EJ, Worthman CM. Puberty and depression: the roles of age, pubertal status and pubertal timing. Psychol Med. 1998;28(1):51-61. PubMed CrossRef
17. Conley CS, Rudolph KD. The emerging sex difference in adolescent depression: interacting contributions of puberty and peer stress. Dev Psychopathol. 2009;21(2):593-620. PubMed CrossRef
18. Caspi A, Moffitt TE. Individual differences are accentuated during periods of social change: the sample case of girls at puberty. J Pers Soc Psychol. 1991;61(1):157-168. PubMed CrossRef
19. Hamilton JL, Hamlat EJ, Stange JP, et al. Pubertal timing and vulnerabilities to depression in early adolescence: differential pathways to depressive symptoms by sex. J Adolesc. 2014;37(2):165-174. PubMed CrossRef
20. Keenan K, Hipwell A, Feng X, et al. Subthreshold symptoms of depression in preadolescent girls are stable and predictive of depressive disorders. J Am Acad Child Adolesc Psychiatry. 2008;47(12):1433-1442. PubMed CrossRef
21. Graber JA, Seeley JR, Brooks-Gunn J, et al. Is pubertal timing associated with psychopathology in young adulthood? J Am Acad Child Adolesc Psychiatry. 2004;43(6):718-726. PubMed CrossRef
22. Bennik EC, Nederhof E, Ormel J, et al. Anhedonia and depressed mood in adolescence: course, stability, and reciprocal relation in the TRAILS study. Eur Child Adolesc Psychiatry. 2014;23(7):579-586. PubMed CrossRef
23. Meinzer MC, Pettit JW, Leventhal AM, et al. Explaining the covariance between attention-deficit hyperactivity disorder symptoms and depressive symptoms: the role of hedonic responsivity. J Clin Psychol. 2012;68(10):1111-1121. PubMed CrossRef
24. Forbes EE, Ryan ND, Phillips ML, et al. Healthy adolescents’ neural response to reward: associations with puberty, positive affect, and depressive symptoms. J Am Acad Child Adolesc Psychiatry. 2010;49(2):162-72.e1, 5. PubMed
25. Rose AJ, Rudolph KD. A review of sex differences in peer relationship processes: potential trade-offs for the emotional and behavioral development of girls and boys. Psychol Bull. 2006;132(1):98-131. PubMed CrossRef
26. The MTA Cooperative Group. Multimodal Treatment Study of Children with ADHD. A 14-month randomized clinical trial of treatment strategies for attention-deficit/hyperactivity disorder. Arch Gen Psychiatry. 1999;56(12):1073-1086. PubMed
27. Greenfield B, Hechtman L, Stehli A, et al. Sexual maturation among youth with ADHD and the impact of stimulant medication. Eur Child Adolesc Psychiatry. 2014;23(9):835-839. PubMed CrossRef
28. Jensen PS, Arnold LE, Swanson JM, et al. 3-year follow-up of the NIMH MTA study. J Am Acad Child Adolesc Psychiatry. 2007;46(8):989-1002. PubMed CrossRef
29. Gau SS, Lin CH, Hu FC, et al. Psychometric properties of the Chinese version of the Swanson, Nolan, and Pelham, Version IV Scale-Teacher Form. J Pediatr Psychol. 2009;34(8):850-861. PubMed CrossRef
30. Tanner JM. Growth and endocrinology of the adolescent. In: Gardner JL, ed. Endocrine and Diseases of Childhood. 2nd ed. Philadelphia, PA: WB Saunders; 1975:14-64.
31. Kovacs M. Children’s Depression Inventory Manual. North Tonawanda, NY: Multi-Health Systems; 1992.
32. Saylor CF, Finch AJ Jr, Spirito A, et al. The Children’s Depression Inventory: a systematic evaluation of psychometric properties. J Consult Clin Psychol. 1984;52(6):955-967. PubMed CrossRef
33. Timbremont B, Braet C, Dreessen L. Assessing depression in youth: relation between the Children’s Depression Inventory and a structured interview. J Clin Child Adolesc Psychol. 2004;33(1):149-157. PubMed CrossRef
34. Jensen PS, Eaton Hoagwood K, Roper M, et al. The Services for Children and Adolescents-Parent Interview: development and performance characteristics. J Am Acad Child Adolesc Psychiatry. 2004;43(11):1334-1344. PubMed CrossRef
35. Swanson JM, Arnold LE, Molina BSG, et al; MTA Cooperative Group. Young adult outcomes in the follow-up of the Multimodal Treatment Study of Attention-Deficit/Hyperactivity Disorder: symptom persistence, source discrepancy, and height suppression. J Child Psychol Psychiatry. 2017;58(6):663-678. PubMed CrossRef
36. Hinshaw SP. Preadolescent girls with attention-deficit/hyperactivity disorder, I: background characteristics, comorbidity, cognitive and social functioning, and parenting practices. J Consult Clin Psychol. 2002;70(5):1086-1098. PubMed CrossRef
37. Burke JD, Hipwell AE, Loeber R. Dimensions of oppositional defiant disorder as predictors of depression and conduct disorder in preadolescent girls. J Am Acad Child Adolesc Psychiatry. 2010;49(5):484-492. PubMed
38. Pizzagalli DA. Depression, stress, and anhedonia: toward a synthesis and integrated model. Annu Rev Clin Psychol. 2014;10(1):393-423. PubMed CrossRef
39. Gabbay V, Johnson AR, Alonso CM, et al. Anhedonia, but not irritability, is associated with illness severity outcomes in adolescent major depression. J Child Adolesc Psychopharmacol. 2015;25(3):194-200. PubMed CrossRef
40. Deardorff J, Gonzales NA, Christopher FS, et al. Early puberty and adolescent pregnancy: the influence of alcohol use. Pediatrics. 2005;116(6):1451-1456. PubMed CrossRef
41. Bardone AM, Moffitt TE, Caspi A, et al. Adult physical health outcomes of adolescent girls with conduct disorder, depression, and anxiety. J Am Acad Child Adolesc Psychiatry. 1998;37(6):594-601. PubMed CrossRef
42. Fergusson DM, Horwood LJ, Ridder EM, et al. Subthreshold depression in adolescence and mental health outcomes in adulthood. Arch Gen Psychiatry. 2005;62(1):66-72. PubMed CrossRef
43. Cuijpers P, Smit F, van Straten A. Psychological treatments of subthreshold depression: a meta-analytic review. Acta Psychiatr Scand. 2007;115(6):434-441. PubMed CrossRef
44. Daviss WB, Birmaher B, Diler RS, et al. Does pharmacotherapy for attention-deficit/hyperactivity disorder predict risk of later major depression? J Child Adolesc Psychopharmacol. 2008;18(3):257-264. PubMed CrossRef
45. Swanson JM, Elliott GR, Greenhill LL, et al. Effects of stimulant medication on growth rates across 3 years in the MTA follow-up. J Am Acad Child Adolesc Psychiatry. 2007;46(8):1015-1027. PubMed CrossRef
46. Meinzer MC, Hartley CM, Hoogesteyn K, et al. Development and open trial of a depression preventive intervention for adolescents with attention-deficit/hyperactivity disorder. Cognit Behav Pract. 2018;25(2):225-239. CrossRef
This PDF is free for all visitors!