Background: Substance use is a common comorbidity with psychotic illnesses. Although several theories exist to explain this link, individual reasons for use may differ. The aim of this study was to evaluate patient perceptions of the reasons for and consequences of their substance use in patients with psychosis and compare them with those of an age-, sex-, and tobacco use-matched control sample without psychosis.
Method: Consecutively admitted patients were divided into 2 groups, those who had substance dependence without psychosis (n = 32), admitted in our addiction unit, and those who had psychotic illness with substance dependence, admitted in our inpatient psychosis unit and referred to as the dual-diagnosis group (n = 62). Patients were administered the Schedules for Clinical Assessment in Neuropsychiatry for ICD-10 Diagnostic Criteria for Research to confirm schizophrenia, bipolar affective disorder, and substance dependence diagnoses and were asked open-ended questions to evaluate the perceived reasons for and consequences of their substance use. The study was conducted from July to September 2006.
Results: There were significant differences between the 2 groups in reasons for maintenance and relapse of both cannabis use and alcohol use, the 2 most common substances. While the substance dependence without psychosis group attributed both maintenance and relapse to external factors such as nature of work, social milieu, or peer pressure, the dual-diagnosis group attributed them to internal factors such as enhancement of positive mood and alleviation of withdrawal effects.
Conclusions: Individuals with psychosis have greater vulnerability to internal factors, which may maintain substance use. Targeting perceived internal factors may play a useful role in management and possibly identification and prevention of psychosis in vulnerable individuals in the future.
Prim Care Companion J Clin Psychiatry 2010;12(5):e1-e7
Submitted: November 15, 2009; accepted January 28, 2010.
Published online: September 2, 2010 (doi:10.4088/PCC.09m00926gry).
Corresponding author: Sahoo Saddichha, MD, National Institute of Mental Health and Neurosciences (NIMHANS), Bangalore, India ([email protected]).
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
CME Background
Articles are selected for credit designation based on an assessment of the educational needs of CME participants, with the purpose of providing readers with a curriculum of CME articles on a variety of topics throughout each volume. Activities are planned using a process that links identified needs with desired results.
To obtain credit, read the material and go to PSYCHIATRIST.COM to complete the Posttest and Evaluation online.
CME Objective
After studying this article, you should be able to:
- When treating individuals with psychosis and substance abuse, inquire about reasons for using substances, and target components of treatment toward resolving those reasons
Accreditation Statement
The CME Institute of Physicians Postgraduate Press, Inc., is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians.
Credit Designation
The CME Institute of Physicians Postgraduate Press, Inc., designates this educational activity for a maximum of 1.5 AMA PRA Category 1 Creditsâ„¢. Physicians should only claim credit commensurate with the extent of their participation in the activity.
Date of Original Release/Review
This educational activity is eligible for AMA PRA Category 1 Credit through September 30, 2013. The latest review of this material was July 2010.
Financial Disclosure
All individuals in a position to influence the content of this activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past 3 years, Larry Culpepper, MD, MPH, Editor in Chief, has been a consultant and a member of the advisory boards for AstraZeneca, Cephalon, Forest, Pfizer, Wyeth, Eli Lilly, Takeda, Merck, Neurocrine, sanofi, Bristol-Myers Squibb, and Otsuka and has been a member of the speakers panels for Forest, Wyeth, and Pfizer. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure appears at the end of the article.
Abstract
Background: Substance use is a common comorbidity with psychotic illnesses. Although several theories exist to explain this link, individual reasons for use may differ. The aim of this study was to evaluate patient perceptions of the reasons for and consequences of their substance use in patients with psychosis and compare them with those of an age-, sex-, and tobacco use-matched control sample without psychosis.
Method: Consecutively admitted patients were divided into 2 groups, those who had substance dependence without psychosis (n = 32), admitted in our addiction unit, and those who had psychotic illness with substance dependence, admitted in our inpatient psychosis unit and referred to as the dual-diagnosis group (n = 62). Patients were administered the Schedules for Clinical Assessment in Neuropsychiatry for ICD-10 Diagnostic Criteria for Research to confirm schizophrenia, bipolar affective disorder, and substance dependence diagnoses and were asked open-ended questions to evaluate the perceived reasons for and consequences of their substance use. The study was conducted from July to September 2006.
Results: There were significant differences between the 2 groups in reasons for maintenance and relapse of both cannabis use and alcohol use, the 2 most common substances. While the substance dependence without psychosis group attributed both maintenance and relapse to external factors such as nature of work, social milieu, or peer pressure, the dual-diagnosis group attributed them to internal factors such as enhancement of positive mood and alleviation of withdrawal effects.
Conclusions: Individuals with psychosis have greater vulnerability to internal factors, which may maintain substance use. Targeting perceived internal factors may play a useful role in management and possibly identification and prevention of psychosis in vulnerable individuals in the future.
Prim Care Companion J Clin Psychiatry 2010;12(5):e1-e7
© Copyright 2010 Physicians Postgraduate Press, Inc.
Submitted: November 15, 2009; accepted January 28, 2010.
Published online: September 2, 2010 (doi:10.4088/PCC.09m00926gry).
Corresponding author: Sahoo Saddichha, MD, National Institute of Mental Health and Neurosciences (NIMHANS), Bangalore, India ([email protected]).
Substance use is an increasingly burgeoning problem that affects the course and outcome of psychotic illnesses.1-3 A substantial portion (15%-60%) of patients with psychosis have been found to use psychoactive drugs.4-6 The Epidemiologic Catchment Area study, the largest study in this area, revealed a lifetime prevalence of 47% for substance misuse in patients with schizophrenia, of which 33.7% met criteria for an alcohol disorder and 27.5% for another drug misuse disorder, and also revealed a 56% prevalence of substance use disorder in bipolar illness.7 However, little is known about the clinical epidemiology of and reasons for use in psychiatric patients. Such information may be clinically useful and help in the formulation of multimodal treatment plans for such dual-diagnosis patients.2
Although several hypotheses have been put forward to explain the relationship between psychosis and substance use,8,9 3 theories are most widely accepted. The first hypothesizes that substance abuse may increase the risk of schizophrenia, at least in vulnerable individuals10,11; the self-medication hypothesis suggests that patients use drugs to alleviate the symptoms of psychosis or the debilitating side effects caused by antipsychotic medications, such as extrapyramidal12; and, finally, others believe that the association could be merely coincidental, with reasons comparable to those of the general population.13
Our study attempted to evaluate these hypotheses by exploring the reasons for substance use in patients with psychosis and comparing them with the reasons for substance use in a group without psychosis. We used retrospectively gathered data to conduct a multidimensional comparison of perceived reasons for substance use between patients with psychosis and those without. We believed that comparisons between these 2 groups could help in identifying differences, if any, that may explain the high comorbidity of substance use disorder in patients with psychosis and therefore help in formulating specific treatment strategies. The aims of this study were to (1) determine substances of dependence in dual-diagnosis patients, (2) compare psychotic and nonpsychotic patients on clinical and sociodemographic variables, and (3) obtain data from patients on the perceived reasons for and consequences of their own substance use.
METHOD
Participants
The study was conducted from July to September 2006. Following ethical approval of the study protocol by the Institutional Review Board of the Central Institute of Psychiatry, Ranchi, India, consecutively admitted patients who had a dual-clinical diagnosis of schizophrenia or bipolar illness with substance dependence were enrolled in the study. After admission, potential subjects identified by clinic staff were screened before entry into the study. The subjects were required to meet the following criteria: probable clinical diagnosis of schizophrenia/bipolar affective disorder and substance dependence; absence of mental retardation, other comorbidity, organic brain disease or brain injury, and acute psychotic symptoms; and likely ability to tolerate an extended interview.
Clinical Points
- Substance use maintenance in psychosis may be due to attempts to cope with negative moods, to feel energetic or feel good, and to reduce withdrawal or to get high.
- Reasons for substance dependence differ between patients with and without psychosis, with those who have psychosis perhaps having greater internal vulnerabilities.
- Testing the beliefs provided by patients for using substances or providing individuals with alternative ways to achieve these effects can be an important component of treatment.
Patients were excluded if they did not give written informed consent or had a Mini-Mental State Examination14 score of less than 24. The total sample consisted of 100 dual-diagnosis subjects, of whom 91 agreed to participate in the extended interview. A control sample who had diagnoses of substance dependence only and was matched for age, sex, and tobacco use (with the Fagerström Test for Nicotine Dependence15) (n = 49; 1 dropped out) was chosen from consecutive admissions at the Centre for Addiction Psychiatry. The numbers differ for the groups because the inpatient unit for psychosis is larger (beds = 300) than the addiction unit (beds = 40). All subjects interviewed were also male because the Deaddiction Center in the institute caters mainly to male patients, with very rare female admissions; hence, female subjects were not included.
Procedures
Potential subjects were taken from consecutive admissions among those who agreed to be interviewed and were currently in remission (Brief Psychiatric Rating Scale-16 item [BPRS]16 score of less than 16). They were then introduced to the interviewer (S.S.), who was blind to the diagnosis and status of patients. The primary investigator then explained the nature of the research project and sought the potential subjects’ written informed consent. Patients who were well enough to participate in the study (BPRS score of less than 16) were administered the relevant sections of the Schedules for Clinical Assessment in Neuropsychiatry17 for ICD-10 Diagnostic Criteria for Research18 by the trained rater (S.S.) to confirm earlier diagnoses of schizophrenia/bipolar affective disorder and substance dependence. The structured interview used in the study also collected relevant clinical and demographic data. Because structured questionnaires may limit responses of participants, subjects were asked open-ended questions about their “reasons for initiation, maintenance, and relapse” for each category of substance they had used in order to obtain perceived reasons and consequences of substance use. Patients were asked, “What is the single most important reason you think that made you start/continue/restart the substance?” and variations thereof. All participants were asked similar questions. Because the study was retrospective, questions were framed individually to trigger patients’ recall using questions anchored to personal and impersonal or important social events and defining the technical terms.19
The answers given were noted verbatim and subsequently grouped (during data analysis) into 2 main categories: external loci factors and internal loci factors. External loci factors were defined as those in which the perceived cause was “nonself,” and internal factors, as those in which the cause was “within self.” More details of the division have been explained in another paper.20
Subjects were then asked about the “consequences of substance use” for each category of substance they had used, and these were subsequently grouped into 3 main categories: medical consequences, psychological consequences, and socio-occupational consequences.
Each interview took between 30 and 90 minutes to complete (mean time: 47 minutes). When subjects found the interview process too tiring and requested to terminate the interview before its completion, the interview was suspended but completed within 48 hours. At the end of the interview, urine toxicology was performed if clinically required. A history of substance use in first-degree relatives based on family history data obtained from the patients was also collected.
Statistical Analyses
The data were statistically analyzed by means of t test for descriptive variables and the χ2 test for categorical variables. The results were compared between the groups (substance dependence vs dual-diagnosis) for use of alcohol and cannabis, which emerged as the 2 most common substances used.
RESULTS
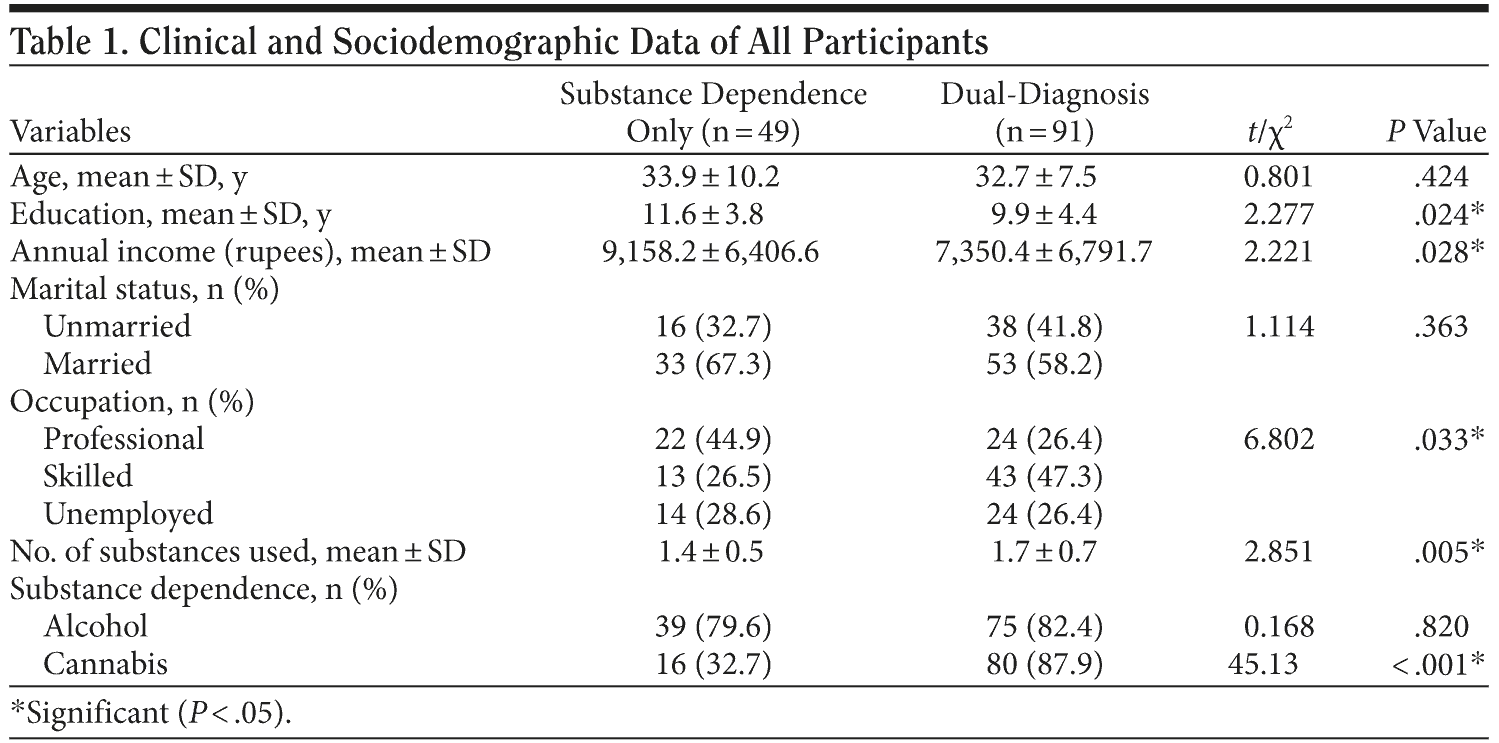
Table 1 presents the clinical and sociodemographic data of all participants. There were no differences between the substance dependence and dual-diagnosis groups in either age or marital status. There was a significant difference noted in education and income, with substance dependence patients having higher education and income levels than dual-diagnosis subjects. Dual-diagnosis patients also used a significantly higher number of substances (1.7) than the substance dependence group (1.4). Although no significant difference was noted in alcohol dependence between the groups, a significant difference was noted in cannabis dependence, with 88% of subjects in the dual-diagnosis group having cannabis dependence compared to just 33% in the substance dependence group.
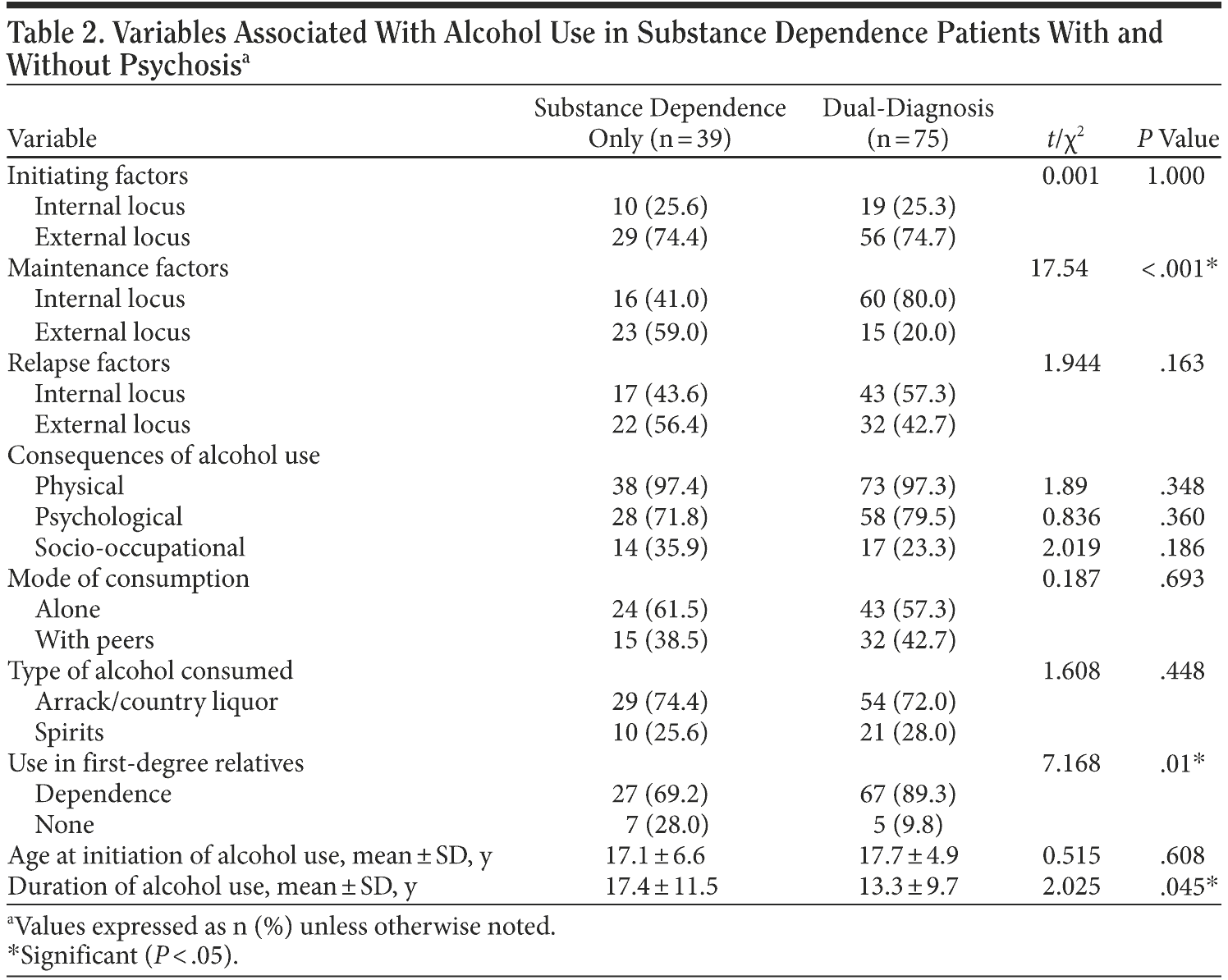
Table 2 presents the variables associated with alcohol use. No difference was seen in initiating factors for alcohol use between the 2 groups. There was, however, a significant difference noted in maintenance factors, with the majority in the substance dependence group (59%) attributing it to external factors (such as withdrawal features, social milieu, and peer pressure) and the majority in the dual-diagnosis group (80%) attributing it to internal factors (such as craving, enhancing positive mood, and alleviating negative mood). There were no significant differences noted in relapse factors between the groups.
When the consequences of alcohol use were analyzed, no differences were noted between the 2 groups in the physical, psychological, or socio-occupational domains. Alcohol dependence was noted in a significantly greater majority of first-degree relatives of dual-diagnosis subjects (89%) compared with substance dependence subjects (69%). Although ages at initiation of alcohol use did not differ, the duration of alcohol use differed significantly between the groups, with the substance dependence group having a longer duration (17 years) than the dual-diagnosis group (13 years).
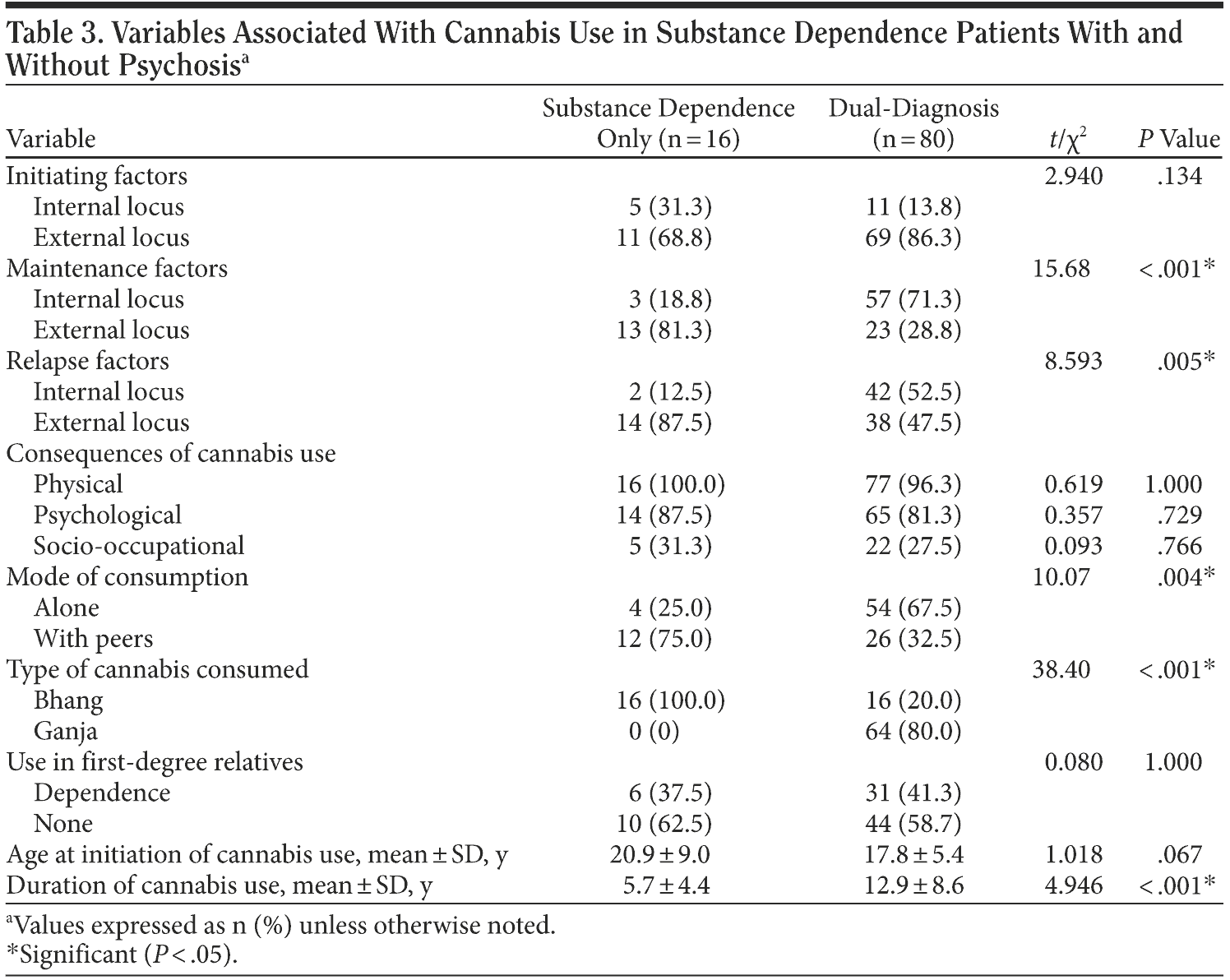
Table 3 presents the variables associated with cannabis use. Significant differences were found in both maintenance and relapse factors between the groups. While the majority in the substance dependence group (81%) attributed external factors (such as nature of work, seeing others take cannabis, and peer pressure) as reasons for maintenance, the majority in the dual-diagnosis group (71%) attributed it to internal factors (such as craving, low self-esteem, and relieving negative feelings). Similarly, a majority of substance dependence subjects (87.5%) gave external factors as reasons for relapse, while a majority of dual-diagnosis subjects (52.5%) gave internal factors as reasons.
No significant differences were noted in the analysis of consequences of cannabis use in any of the 3 domains. Dual-diagnosis subjects (67.5%) were observed to use cannabis more often alone than with peers and to use it mainly in the form of ganja (80%). Although there was no difference in ages at initiation of cannabis use, the dual-diagnosis group had a significantly greater duration of cannabis use (12.9 years) when compared to the substance dependence group (5.7 years).
DISCUSSION
Several studies have examined the clinical correlates and reasons for substance use in patients suffering from psychosis.21,22 Many of these studies have focused on substance use in either schizophrenia21 or affective psychoses.22 The clinical and sociodemographic profile of participants in our sample is similar to those reported in these previous outpatient and community studies,21-25 with cannabis used most frequently, followed by alcohol, and patients with psychosis using more substances than those without. Although substantial, most of the previous studies were limited by the absence of a well-matched control group without psychosis. Our study attempts to bridge this gap by comparing substance dependence in patients with and without psychosis.
Most of our patients were in their 30s and had been educated up to high school, a finding similar to other studies.21,22 Subjects with substance dependence only, however, had higher mean incomes than the dual-diagnosis subjects. Although the prevalence of unemployment was similar in both groups, we believe, as we noted in our study, that patients with psychosis are often employed in underpaid or noncompetitive/nonprofessional jobs resulting in lower mean incomes.26 Even if patients with psychosis are well employed, we believe that they are severely disabled by their illness and have more off days than days of gainful employment.27
Our study also found no significant difference in marital status between the 2 groups. This is surprising, because most Western studies have reported a differing marital status for patients with psychosis,28-30 namely one of remaining single through either nonmarriage or separation. We believe that the cultural and traditional system in India, which ensures marriage for every individual as part of his/her duty and promotes the belief that a stable marriage may help cure mental illness, could account for such findings. Our findings have been corroborated by other studies from India, which have also noted high rates of marriage (up to 70%) in this population.31-34 The relationship is complex, and the question of whether marital status is best seen as a cause or an effect of psychosis is still not well understood.
When the factors for initiation of alcohol and cannabis use were analyzed, no differences were observed. This is not surprising, because initiation is often dictated by external factors like easy availability, peer pressure, or emulation of role models, reasons that our subjects attributed and that have also been observed in other studies.35,36 However, once initiated, alcohol and cannabis use have differing reasons for maintenance, as described by our subjects. Maintenance of alcohol dependence in substance dependence patients was dictated by external factors such as nature of work, social milieu, or peer pressure, a finding similar to our earlier study20 and other addiction studies.35 This is in comparison to the internal factors dictating alcohol dependence in patients with psychosis, such as withdrawal, low self-esteem, and elevating negative moods, a finding corroborated by several studies.37,38 Similar findings can be observed for cannabis dependence, with substance dependence patients attributing it to external factors and dual-diagnosis patients attributing it to internal factors.39 Therefore, regardless of the substance type, results indicate 3 main motives for substance use maintenance in patients with psychosis: (1) to cope with negative moods, “decrease depression,” or “relax”21; (2) to feel energetic, improve low self-esteem, or “feel good”13,21; and (3) to reduce withdrawal, “get high,” or achieve intoxication.21
Relapse factors in alcohol dependence did not differ significantly between the 2 groups. However, significant differences were noted for cannabis dependence. Most substance dependence patients again attributed it to external factors such as seeing others take it, taking it after eating/drinking, and taking it with other substances,13,40-43 while the dual-diagnosis patients attributed it to internal factors such as need for concentration, enhancement of positive mood, and alleviation of withdrawal effects. These findings suggest that the course and pattern of dependence differs between patients with and without psychosis, with the former group being especially vulnerable to the neuromodulating effects of cannabis and alcohol.42-44 This is especially concerning because psychic dependence is stronger and develops faster for “elevating” drugs like cannabis than for “depressing” drugs like alcohol,45 and in individuals vulnerable to psychosis, cannabis use may precipitate psychosis,46 lending credence to the common vulnerability model.10,11
We also observed that dual-diagnosis patients tended to use cannabis more often alone and used ganja more than bhang (bhang is a preparation from the leaves and flowers [buds] of the female cannabis plant that is consumed in the Indian subcontinent as a beverage, while ganja is the Indian name for marijuana, usually consumed by smoking in specially designed pipes). We believe that the factors of internal loci for maintenance and relapse, as detailed above, may be responsible for the solitary drug-taking behavior. Further, the higher concentrations of Δ9 tetrahydrocannabinol in ganja than in bhang may play an etiologic role in causing psychosis in vulnerable individuals. A stronger family history of alcohol dependence than cannabis dependence was also noted, pointing to the role of genetic mechanisms for alcohol dependence.47 We also observed that although cannabis use was initiated at similar ages, the durations differed between the groups. Since the clinical histories of the subjects with cannabis dependence pointed to earlier admissions, we believe that patients with substance dependence came to clinical attention earlier than patients who developed psychosis. This suggests that the prodrome of psychosis may often be confused with that of cannabis intoxication, leading to delayed referrals. An early psychosis program that specifically identifies vulnerable individuals and refers them for treatment would go a long way toward reducing the incidence of psychosis.
In analyzing the perceived consequences of substance use, we observed that medical, psychological, and socio-occupational consequences of both alcohol and cannabis use were perceived equally by both groups. This is in contrast to other studies from India that have noted socio-occupational consequences to be the most important factor in substance disorder patients.35,48,49
The finding that patients with psychosis differed significantly from patients with only substance dependence in their reasons for substance use, especially cannabis, suggests that perhaps patients with psychosis have greater vulnerabilities to internal factors than those with only substance dependence50 and varying expectations that substance use will improve their mood or increase self-esteem. Using substances to cope with factors of internal loci such as to deal with unpleasant affect or to enhance positive mood is linked with increased use and substance use problems such as increased risk for dependence. The reasons given by these individuals are obviously important perceived benefits and beliefs that maintain their alcohol and cannabis use. Therefore, Spencer and colleagues have suggested that “testing these beliefs or providing individuals with alternative ways to achieve these effects is an important component of treatment.”51(p243) This provides validation for cognitive-behavioral treatments that address motives for substance use.
There are a few limitations to our study. The relatively small sample size and inclusion of only men may limit the generalizability of our findings. We believe that our open-ended questions may have attracted some bias in answering the questions. There is also the question of recall bias; however, we believe this was minimized by framing questions to trigger recall using questions anchored to personal and impersonal or important social events.
CONCLUSION
To conclude, patients with psychosis differed significantly from patients without psychosis in their substance dependence patterns. Internal factors dictated maintenance and relapse in patients with psychosis. Targeting of these perceived factors may play a useful role in management and possibly identification and prevention of psychosis in vulnerable individuals in the future. Mental health services should identify patients with psychosis who use alcohol, cannabis, and other drugs and discuss with them the impact of such use on their disorder. Multimodal treatment plans will play an important role in the management of such individuals.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration−approved labeling has been presented in this article.
Author affiliations: Department of Psychiatry, National Institute of Mental Health and Neurosciences (NIMHANS), Bangalore, India (Dr Saddichha); Departments of Psychiatry (Dr Prakash) and Addiction Psychiatry (Dr Khess), Central Institute of Psychiatry, Ranchi, India; and Crisis Resolution and Home Treatment, University Hospital of North Tees, Cleveland, United Kingdom (Dr Sinha).
Financial disclosure: Drs Saddichha, Prakash, Sinha, and Khess have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: None reported.
Previous presentation: Part of the findings in this article were presented under the Rafaelsen Young Investigator Award at the CINP International Thematic Meeting on Major Psychoses and Substance Abuse; April 25-27, 2009; Edinburgh, United Kingdom.
This CME activity is expired. For more CME activities, visit cme.psychiatrist.com.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
REFERENCES
1. Blanchard JJ, Brown SA, Horan WP, et al. Substance use disorders in schizophrenia: review, integration, and a proposed model. Clin Psychol Rev. 2000;20(2):207-234. PubMed doi:10.1016/S0272-7358(99)00033-1
2. Kavanagh DJ, McGrath J, Saunders JB, et al. Substance misuse in patients with schizophrenia: epidemiology and management. Drugs. 2002;62(5):743-755. PubMed doi:10.2165/00003495-200262050-00003
3. Bartels SJ, Drake RE, Wallach MA. Long-term course of substance use disorders among patients with severe mental illness. Psychiatr Serv. 1995;46(3):248-251. PubMed
4. Condren RM, O’ Connor J, Browne R. Prevalence and patterns of substance misuse in schizophrenia: a catchment area case-control study. Psychiatr Bull. 2001;25(1):17-20. doi:10.1192/pb.25.1.17
5. Hambrecht M, Häfner H. Cannabis, vulnerability, and the onset of schizophrenia: an epidemiological perspective. Aust N Z J Psychiatry. 2000;34(3):468-475. PubMed
6. Menezes PR, Johnson S, Thornicroft G, et al. Drug and alcohol problems among individuals with severe mental illness in south London. Br J Psychiatry. 1996;168(5):612-619. PubMed doi:10.1192/bjp.168.5.612
7. Regier DA, Farmer ME, Rae DS, et al. Comorbidity of mental disorders with alcohol and other drug abuse: results from the Epidemiologic Catchment Area (ECA) Study. JAMA. 1990;264(19):2511-2518. PubMed doi:10.1001/jama.264.19.2511
8. Thornicroft G. Cannabis and psychosis: is there epidemiological evidence for an association? Br J Psychiatry. 1990;157(1):25-33. PubMed doi:10.1192/bjp.157.1.25
9. Silver H, Abboud E. Drug abuse in schizophrenia: comparison of patients who began drug abuse before their first admission with those who began abusing drugs after their first admission. Schizophr Res. 1994;13(1):57-63. PubMed doi:10.1016/0920-9964(94)90060-4
10. Mueser KT, Yarnold PR, Bellack AS. Diagnostic and demographic correlates of substance abuse in schizophrenia and major affective disorder. Acta Psychiatr Scand. 1992;85(1):48-55. PubMed doi:10.1111/j.1600-0447.1992.tb01441.x
11. Mueser KT, Yarnold PR, Levinson DF, et al. Prevalence of substance abuse in schizophrenia: demographic and clinical correlates. Schizophr Bull. 1990;16(1):31-56. PubMed
12. Khantzian EJ. The self-medication hypothesis of addictive disorders: focus on heroin and cocaine dependence. Am J Psychiatry. 1985;142(11):1259-1264. PubMed
13. Fowler IL, Carr VJ, Carter NT, et al. Patterns of current and lifetime substance use in schizophrenia. Schizophr Bull. 1998;24(3):443-455. PubMed
14. Folstein MF, Folstein SE, McHugh PR. “Mini-mental state”: a practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975;12(3):189-198. PubMed doi:10.1016/0022-3956(75)90026-6
15. Heatherton TF, Kozlowski LT, Frecker RC, et al. The Fagerström Test for Nicotine Dependence: a revision of the Fagerström Tolerance Questionnaire. Br J Addict. 1991;86(9):1119-1127. PubMed doi:10.1111/j.1360-0443.1991.tb01879.x
16. Overall JE, Gorham DR. The Brief Psychiatric Rating Scale. Psychol Rep. 1962;10(3):799-812. doi:10.2466/PR0.10.3.799-812
17. van Gulick-Bailer M, Maurer K, Hafner H, eds. Schedules for Clinical Assessment in Neuropsychiatry: SCAN, PSE 10 Interview. Bern, Switzerland: Hans Huber; 1995.
18. World Health Organization (WHO). ICD-10 Classification of Mental and Behavioural Disorders. Diagnostic Criteria for Research (DCR). Geneva, Switzerland: World Health Organization; 1993.
19. Carlat DJ. Asking questions III: tricks for improving patient recall. In: The Psychiatric Interview: A Practical Guide. 2nd ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2005:27-29.
20. Saddichha S, Sinha BNP, Khess CRJ. The role of gateway drugs and psychosocial factors in substance dependence in Eastern India. Int J Psychiatry Med. 2007;37(3):257-266. PubMed doi:10.2190/PM.37.3.b
21. Dixon L, Haas G, Weiden PJ, et al. Drug abuse in schizophrenic patients: clinical correlates and reasons for use. Am J Psychiatry. 1991;148(2):224-230. PubMed
22. Strakowski SM, DelBello MP, Fleck DE, et al. Effects of co-occurring alcohol abuse on the course of bipolar disorder following a first hospitalization for mania. Arch Gen Psychiatry. 2005;62(8):851-858. PubMed doi:10.1001/archpsyc.62.8.851
23. Sevy S, Robinson DG, Holloway S, et al. Correlates of substance misuse in patients with first-episode schizophrenia and schizoaffective disorder. Acta Psychiatr Scand. 2001;104(5):367-374. PubMed doi:10.1034/j.1600-0447.2001.00452.x
24. Kessler RC, Crum RM, Warner LA, et al. Lifetime co-occurrence of DSM-III-R alcohol abuse and dependence with other psychiatric disorders in the National Comorbidity Survey. Arch Gen Psychiatry. 1997;54(4):313-321. PubMed
25. Kumar PNS, Raju SS. Impact of substance abuse comorbidity on psychopathology and pattern of remission in mania. Indian J Psychiatry. 1998;40(4):357-363.
26. Marwaha S, Johnson S. Schizophrenia and employment—a review. Soc Psychiatry Psychiatr Epidemiol. 2004;39(5):337-349. PubMed doi:10.1007/s00127-004-0762-4
27. Jablensky A, McGrath J, Herrman H, et al. National Survey of Mental Health and Wellbeing. Report 4. People Living with Psychotic Illness: An Australian Study. Canberra, Australia: Mental Health Branch. Commonwealth Department of Health and Aged Care; 1999.
28. Nanko S, Moridaira J. Reproductive rates in schizophrenic outpatients. Acta Psychiatr Scand. 1993;87(6):400-404. PubMed doi:10.1111/j.1600-0447.1993.tb03395.x
29. Lane A, Byrne M, Mulvany F, et al. Reproductive behaviour in schizophrenia relative to other mental disorders: evidence for increased fertility in men despite decreased marital rate. Acta Psychiatr Scand. 1995;91(4):222-228. PubMed doi:10.1111/j.1600-0447.1995.tb09772.x
30. Weissman MM, Bland RC, Canino GJ, et al. Cross-national epidemiology of major depression and bipolar disorder. JAMA. 1996;276(4):293-299. PubMed doi:10.1001/jama.276.4.293
31. Batra L, Gautam S. Psychiatric morbidity and personality profile in divorce seeking couples. Indian J Psychiatry. 1995;37:179-185.
32. Thara R, Srinivasan TN. Marriage and gender in schizophrenia. Indian J Psychiatry. 1997;39:64-69.
33. Ponnudurai R, Jayakar J, Sathiya Sekaran B. Assessment of mortality and marital status of schizophrenic patients over a period of 13 years. Indian J Psychiatry. 2006;48(2):84-87. doi:10.4103/0019-5545.31595
34. Thara R, Srinivasan TN. Outcome of marriage in schizophrenia. Soc Psychiatry Psychiatr Epidemiol. 1997;32(7):416-420. PubMed
35. Meena KP, Vohra AK, Rajput R. Prevalence and pattern of alcohol and substance abuse in urban areas of Rohtak City. Indian J Psychiatry. 2002;44(4):219-220.
36. Margoob MA, Majid A, Hussain A, et al. Changing sociodemographic and clinical profile of substance use disorder patients in Kashmir valley. JK Pract. 2004;11(1):14-16.
37. Pristach CA, Smith CM. Self-reported effects of alcohol use on symptoms of schizophrenia. Psychiatr Serv. 1996;47(4):421-423. PubMed
38. Mental Health Foundation. Cheers? Understanding the Relationship Between Alcohol and Mental Health. London, England: Mental Health Foundation; 2006.
39. Schofield D, Tennant C, Nash L, et al. Reasons for cannabis use in psychosis. Aust N Z J Psychiatry. 2006;40(6-7):570-574. PubMed
40. Test MA, Wallisch LS, Allness DJ, et al. Substance use in young adults with schizophrenic disorders. Schizophr Bull. 1989;15(3):465-476. PubMed
41. Chandrasekaran R, Sivaprakash B, Chitraleka V. Five years of alcohol de-addiction services in a tertiary care general hospital. Indian J Psychiatry. 2001;43(1):58-60.
42. Iversen L. Cannabis and the brain. Brain. 2003;126(pt 6):1252-1270. PubMed doi:10.1093/brain/awg143
43. Herkenham M. Cannabinoid receptor localization in brain: relationship to motor and reward systems. Ann N Y Acad Sci. 1992;654(1):19-32. PubMed doi:10.1111/j.1749-6632.1992.tb25953.x
44. Tupala E, Tiihonen J. Dopamine and alcoholism: neurobiological basis of ethanol abuse. Prog Neuropsychopharmacol Biol Psychiatry. 2004;28(8):1221-1247. PubMed doi:10.1016/j.pnpbp.2004.06.022
45. Park K. Mental health. In: Park’s Textbook of Preventive and Social Medicine. 18th ed. Jabalpur, India: Banarsidas Bhanot Publishers; 2005:632-637.
46. Zammit S, Lewis G. Exploring the relationship between cannabis use and psychosis. Addiction. 2004;99(10):1353-1355. PubMed doi:10.1111/j.1360-0443.2004.00843.x
47. Oroszi G, Goldman D. Alcoholism: genes and mechanisms. Pharmacogenomics. 2004;5(8):1037-1048. PubMed doi:10.1517/14622416.5.8.1037
48. Mattoo SK, Basu D. Clinical course of alcohol dependence. Indian J Psychiatry. 1997;39(4):294-299.
49. Chavan BS, Arun P, Bhargava R, et al. Prevalence of alcohol and drug dependence in rural and slum population of Chandigarh: a community survey. Indian J Psychiatry. 2007;49(1):44-48. doi:10.4103/0019-5545.31517
50. Goswami S, Singh G, Mattoo SK, et al. Courses of substance use and schizophrenia in the dual-diagnosis patients: is there a relationship? Indian J Med Sci. 2003;57(8):338-346. PubMed
51. Spencer C, Castle D, Michie PT. Motivations that maintain substance use among individuals with psychotic disorders. Schizophr Bull. 2002;28(2):233-247. PubMed
Enjoy this premium PDF as part of your membership benefits!