A Review of Potential Adverse Effects of Long-Term Opioid Therapy: A Practitioner’s Guide

ABSTRACT
Objective: Review, synthesize, and summarize recent evidence on adverse effects of long-term opioid treatment for noncancer pain and present an organ system-based guide for primary care physicians in initiating and monitoring patients receiving chronic opioid therapy.
Data Sources: A search for studies published in peer-reviewed journals from 2005 to 2011 was conducted using MEDLINE, Agency for Healthcare Research and Quality Clinical Guidelines and Evidence Reports, and the Cochrane Database of Systematic Reviews. Related citations and expert recommendations were included.
Data Extraction: Studies were selected if the search terms opioid and the organ system of interest were in the article’s title, abstract, or text. Systems considered were gastrointestinal, respiratory, cardiovascular, central nervous, musculoskeletal, endocrine, and immune. Of 1,974 initially reviewed articles, 74 were selected for evidence regarding effects of chronic opioid use on that organ system. Of these articles, 43 were included on the basis of direct relevance to opioid prescriptions in the primary care setting.
Data Synthesis: A qualitative review was performed because the number of articles pertaining to specific adverse effects of opioids was typically small, and the diversity of adverse effects across systems precluded a quantitative analysis.
Results: Through a variety of mechanisms, opioids cause adverse events in several organ systems. Evidence shows that chronic opioid therapy is associated with constipation, sleep-disordered breathing, fractures, hypothalamic-pituitary-adrenal dysregulation, and overdose. However, significant gaps remain regarding the spectrum of potentially opioid-related adverse effects. Opioid-related adverse effects can cause significant declines in health-related quality of life and increased health care costs.
Conclusions: The diverse adverse effects potentially caused by chronic opioid therapy support recommendations for judicious and selective opioid prescribing for chronic noncancer pain by primary care physicians. Additional research clarifying the risks and management of potential adverse effects of chronic opioid therapy is needed to guide clinical practice.
Prim Care Companion CNS Disord
2012;14(3):doi:10.4088/PCC.11m01326
© Copyright 2012 Physicians Postgraduate Press, Inc.
Submitted: December 1, 2011; accepted February 9, 2012.
Published online: June 14, 2012.
Corresponding author: AnGee Baldini, MD, The George Washington University School of Medicine and Health Sciences, 2601 Virginia Ave NW, Rm 112, Washington, DC 20052 ([email protected]).
A recent national call for action to reduce prescription opioid abuse and overdose announced by the White House Office of National Drug Control Policy, the Drug Enforcement Agency, and the US Food and Drug Administration recommended improved physician education concerning opioid prescribing.1,2 This call for action was prompted by the large number of deaths due to opioid overdose reported by the Centers for Disease Control and Prevention.3 As chronic pain has a reported prevalence of up to 40% in developed countries, with 10% to 25% of the population experiencing clinically significant dysfunction related to chronic pain, use of opioids for treating chronic noncancer pain has become more common following recommendations of several pain societies.4 The prevalence of long-term opioid use has increased markedly since the 1980s, with an estimated 6 to 8 million Americans taking opioids for long-term management of chronic noncancer pain based on the reported prevalence of use of chronic opioid therapy.5,6 Despite widespread use, there remains a dearth of concise information on adverse effects of opioids in a form suitable for primary care physicians.7 This review considers scientific studies published in the last 6 years that provide information relevant to potential adverse opioid effects. This information is presented in an organ system-based approach to facilitate use in clinical practice by primary care physicians. The aim is to enhance the physician’s ability to discuss potential adverse effects of opioids with patients considering long-term treatment with these medications for chronic noncancer pain, as well as to increase vigilance of physicians and patients in identifying potential adverse effects that may be due to opioid medication use.
METHOD
A search for evidence-based studies published in peer-reviewed journals from 2005 to 2011 was conducted using MEDLINE, Agency for Healthcare Research and Quality Clinical Guidelines and Evidence Reports, and the Cochrane Database of Systematic Reviews. A qualitative review was performed because the number of articles pertaining to specific adverse effects of opioids was typically small, and the diversity of adverse effects across systems precluded a quantitative analysis. Systems considered were gastrointestinal, respiratory, cardiovascular, central nervous, musculoskeletal, endocrine, and immune. Within each system, we initially considered articles that met the criteria of including the terms opioid and the particular organ system in the title, abstract, or body of the article. Among 1,974 initially identified articles, 74 of those incorporating direct evidence of chronic opioid use on systems of interest were identified. Of these articles, 43 were selected on the basis of relevance to prescribing in primary care practice. Additional articles identified by expert recommendation and relevant bibliographies augmented this review.
RESULTS
Gastrointestinal System Effects
Constipation is a prevalent adverse effect of chronic opiate therapy that is widely recognized by physicians and patients alike as an unwanted consequence of opioid use.8 The pathophysiology of this process results from stimulation of κ and μ opioid receptors in the gastrointestinal tract. Multiple studies report that 40%-45% of patients on opiate therapy experience constipation, while 25% experience nausea.9 Constipation due to opioid use frequently remains refractory to treatment with stool softeners and laxatives.10 Constipation can be so severe that some patients reduce their medication dosage or discontinue opiate use altogether. In its most severe instances, opiate use has been shown to increase the risk of bowel obstruction, which can result in hospitalization or death.11 In addition to causing constipation and nausea, opiate use can cause vomiting, abdominal cramping, and bloating. The overall risk of gastrointestinal bleeding is similar to nonsteroidal anti-inflammatory (NSAID) agents.12

- Increasing numbers of deaths are due to opioid overdose among patients prescribed long-term opioid therapy to manage chronic pain.
- Opioid therapy can adversely affect respiratory, gastrointestinal, musculoskeletal, cardiovascular, immune, endocrine, and central nervous systems.
- The higher the daily dose of prescribed opioid, the higher the risk of overdose and other significant problems such as fractures, addiction, intestinal blockages, and sedation.
- Physicians and patients are encouraged to weigh the full spectrum of medical risks against a realistic assessment of observed benefits for pain.
The consequences of constipation and other gastrointestinal effects merit special attention. Constipation is associated with significant economic and quality of life burdens. Surveys have recently found that as many as one-third of chronically constipated patients report substantial psychological distress and an increased prevalence of depression relative to control patients.13 Patients with gastrointestinal complaints related to opioid use have been shown to have significantly higher emergency room visits and hospital admissions, longer hospital stays, and more primary care visits.14 The associated impairment in quality of life should be carefully weighed against opioid efficacy for chronic pain.15
Respiratory System Effects
An association between sleep-disordered breathing and chronic opiate use has been found in recent studies. Chronic opiate use has been shown to be associated with multiple features of sleep-disordered breathing, including central sleep apnea, ataxic breathing, hypoxemia, and carbon dioxide retention.16,17 Among patients on around-the-clock opioid therapy for at least 6 months, the prevalence of sleep-disordered breathing (ranging from mild to severe central and/or obstructive apnea) has been found to be as high as 75%.18 In contrast, in general population samples, sleep-disordered breathing is observed in 3%-20% of persons.19,20 In a small study, central sleep apnea was found in 30% of patients on chronic methadone therapy.21 Up to 10% of patients on chronic opiate therapy experience some degree of hypoxemia (oxyhemoglobin saturation of less than 90%).22 The adverse respiratory effects of opioids appear to occur in a dose-dependent fashion. Ataxic breathing has been observed in up to 92% of individuals taking a morphine-equivalent dose of 200 mg, 61% of individuals taking under 200 mg, and just 5% of individuals not taking opioids.17 While risk of mortality from opiate overdose has been well established, morbidity from chronic sleep-disordered breathing needs further research, as available studies are of relatively small and unrepresentative samples.19-24
Respiratory System Depression
A potentially life-threatening side effect of opioid therapy is respiratory depression, bradycardia, and hypotension, which occurs in opioid overdose. Although the mechanisms are not well understood, a physiologic tolerance to analgesia does not necessarily parallel a tolerance to the respiratory effects of opioids. Patients prescribed larger opioid doses were found to experience substantially increased overdose risk.25 There are differing estimates of this risk, but recent literature has demonstrated an 8.9-fold increase among patients prescribed > 100 mg/day (relative to patients on opioid regimens of less than 20 mg) and a 3.7-fold increase among patients prescribed > 50 mg/day.20,25 Among persons on higher opioid doses, the risk of opioid overdose was estimated to be 1.8% per year of opioid use. Additionally, 12% of identified overdoses were fatal, suggesting an annual fatal overdose risk of about 2 per 1,000 per year among patients on higher-dose opioid regimens. These estimates are consistent with Centers for Disease Control and Prevention mortality surveillance data on deaths from drug overdose, which now roughly equal motor vehicle accidents as a leading cause of death among 35-54 year olds.3
Cardiovascular System Effects
Recently, a large cohort study among Medicare patients with arthritis found that when opioid therapy was compared with NSAIDs and selective cyclooxygenase-2 (COX-2) inhibitors, opioid therapy was associated with a 77% increased risk of cardiovascular events (eg, myocardial infarction, heart failure). In the first 30 days, the risk of cardiovascular events was similar across different opioid medications. However, after 180 days of therapy, codeine was associated with a 62% increase in these adverse events as compared to hydrocodone.11,12 Another large cohort study based on health insurance claims also showed increased risks of myocardial infarction and cardiovascular revascularization among patients on chronic opioid therapy relative to the general population.26 These findings of adverse cardiovascular effects to opioids may be explained by potential biases in observational research and need to be replicated, but it cannot be assumed that opioids have lower cardiotoxicity than COX-2 inhibitors in the absence of adequate empirical research to support such a conclusion.
Central Nervous System Effects
Opioid neurotoxicity is a significant issue, especially among the elderly. Dizziness and sedation are also central nervous system effects that can lead to unintended consequences among those receiving long-term opioid therapy, such as falls, fractures, and respiratory depression.27 Hyperalgesia associated with excessive sensitivity to pain has been reported in patients on chronic opioid therapy.28 In addition, patients on chronic opioid therapy have been shown to have relatively higher levels of comorbid clinical depression of up to 38%.29 Interestingly, it has been shown that patients on chronic opioid therapy with comorbid mental illness have a significantly higher amount of emergency room visits.30 Concomitant use of other central nervous system depressants such as benzodiazepines, barbiturates, and alcohol aggravate respiratory depression and can progress to apnea.27
Musculoskeletal System Effects
One significant adverse effect of opioid therapy is its association with an increased risk of fractures. While the primary mechanism of this increased risk is poorly understood, the prevailing theory is that opiate use leads to an increased risk of falls through its central nervous system effects such as dizziness and reduced alertness.31 Recent meta-analyses have reported a relative risk of fractures of around 1.4 for elderly patients on opiate therapy. However, some estimates have placed the hazard ratio for increased fracture risk at close to 4.9 when comparing patients taking opioids to age-matched controls taking NSAIDs.32 While the relative risk is modest, since the base rates of serious fractures are high among older adults, the absolute increase in risk is notable. In populations over age 65 years, opiate therapy conferred a risk of up to 1.6 for fractures.32,33 Recent studies have found that doses of propoxyphene and morphine over 50 mg doubled the risk of fractures in the elderly, with an annual fracture rate of 9.95%.34,35 In addition, higher dosages of opioids correspond to a higher fracture risk among patients.36 One study found that short-acting opioids confer a significantly greater risk of fracture than long-acting opioids within the first 2 weeks of use.37
Nearly all of these studies noted the need for further research into increased risk of fractures. While the number of hip fractures has steadily decreased over time, overall mortality has remained at a notably high level of 21.9% after 1 year.38 Furthermore, those who do survive such an event often do not regain their health-related quality of life. They often have precipitous declines in mental and physical health, may require institutional care, and also have decreased quality-adjusted life-years.39,40 With regard to other analgesic therapies, opiates showed a statistically significant increase in fractures when compared to alternative medications such as NSAIDS and celecoxibs.10
Endocrine System Effects
Chronic opioid therapy has been found to have a strong impact on the male and female endocrine system. The mechanism of these effects is believed to occur through opiate interaction with the hypothalamic-pituitary-adrenal axis in humans. Opiates have been shown to affect the release of every hormone from the anterior pituitary including growth hormone, prolactin, thyroid-stimulating hormone, adrenocorticotropic hormone, and lutein-stimulating hormone.41 Individuals on chronic opioid therapy have been shown to have a hyperfunctioning hypothalamic-pituitary-adrenal axis accompanied by decreased functioning of the hypothalamic-pituitary-gonadal axis. Of all of the endocrinopathies observed, some of the most profound pertain to the decrease of gonadotropin-releasing hormone.42 This decrease in gonadotropin-releasing hormone can manifest clinically in males as hypogonadism, also known as opiate-induced androgen deficiency, sexual dysfunction, infertility, fatigue, and decreased levels of testosterone.43 The decrease in testosterone is of special concern because preliminary studies have suggested increased risk of metabolic syndrome and insulin resistance.41
The decreased pulsatile release of gonadotropin-releasing hormone and subsequent decrease in luteinizing and follicle-stimulating hormones may have dramatic clinical consequences in women as well. Decreased circulating levels of estrogen, low follicle-stimulating hormone, and increased prolactin can lead to osteoporosis, oligomenorrhea, and galactorrhea.41 These preliminary findings suggest the need for caution when prescribing to patients with existing conditions such as osteopenia. It has been noted that these side effects are reversible with cessation of treatment or lower dosing.44
Immune System Effects
Several types of opioids, most notably morphine and fentanyl, have intrinsic immunosuppressive effects. Clinical sequelae of these effects are difficult to assess, as specific mechanisms of action need further research. It is believed that these opioids directly affect the μ-opioid receptor on all immune cells. They may also modulate the immune function indirectly through glucocorticoids released by the hypothalamic-pituitary-adrenal axis and norepinephrine released by the sympathetic nervous system.45 Recent literature has shown an increase in pneumonia in elderly patients on chronic opioid therapy.46
Addiction and Misuse
Prescription drug abuse is the fastest rising drug addiction problem in the United States.1 Opioid misuse in the United States and Canada can be quite common, involving about one-quarter of prescribed patients. Opioid dependence and misuse includes a range of drug-taking behaviors such as increasing dose without prescription, obtaining additional opioids from other doctors, purposeful sedation, use for purposes other than pain relief, and hoarding pain medications.47,48 Clinicians should be vigilant of early requests for refills, misplacing prescriptions, and increases in medical dosages, as all of these behaviors can be indicative of abuse.49 Current literature remains inconclusive on the overall risk of opioid addiction; however, opioid misuse has been found to be relatively common in a thorough study of general practice patients.50 With this finding in mind, it has been found that long-term opioid treatment is associated with an 87% increase in all-cause mortality.51 From a psychiatric standpoint, opioid abusers exhibited a higher prevalence of depression, anxiety disorders, and bipolar disorder than nonabusers and also were more than 10 times as likely to use inpatient mental health services.52,53
DISCUSSION
With diverse adverse effects from chronic opiate therapy of concern to physicians and patients, a systems-based approach can help facilitate appropriate prescriptions and pain management. Opioid efficacy in treating pain must be balanced against the quality of life burden from constipation and other gastrointestinal side effects. Due to the effects of opioids on the respiratory system, caution must be exercised when prescribing opioids to patients exhibiting signs and symptoms of sleep-disordered breathing or those at risk for developing this problem. From a cardiovascular standpoint, opioid use has been associated with adverse events; however, these results need additional controlled research. From a neurologic and musculoskeletal standpoint, the elderly seem an especially vulnerable population to the side effects of opioids, with both depressed mentation and increased risk of hip fractures. Physicians must maintain vigilance when prescribing to this patient population, especially if these patients have medical conditions that predispose them to fractures such as osteoporosis. Physician awareness of the endocrine and immunosuppressive effects of opioids, along with the potential for overdose, can aid in patient education. Since opioids have a high potential for abuse, patients must be periodically screened for opioid misuse and drug-taking behaviors. Across diverse organ systems, opioids may exert side effects in a dose-dependent fashion.
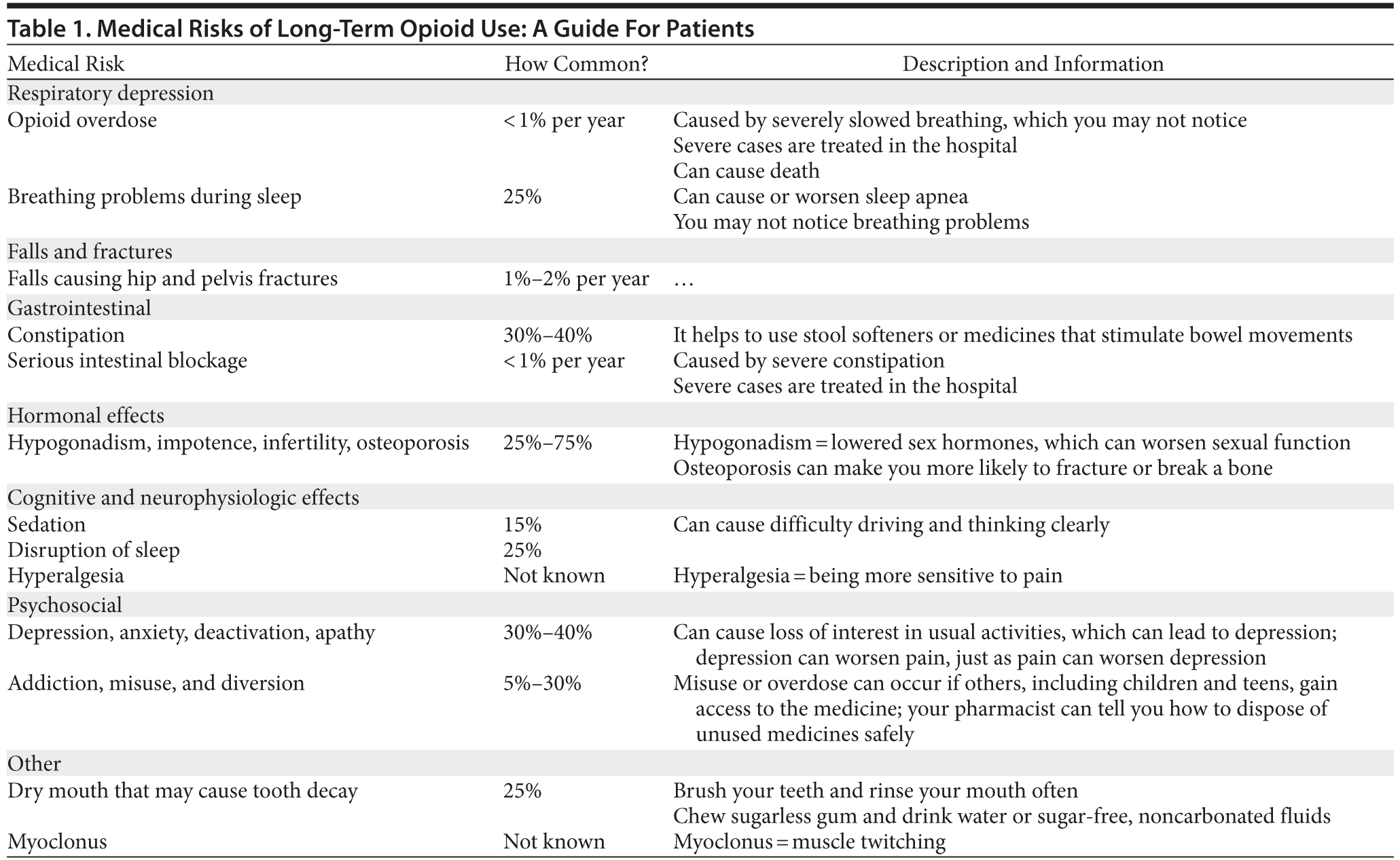
Physicians are responsible for discussing potential risks of chronic opioid therapy with patients considering this treatment option. This discussion is necessary to increase patient awareness of potential adverse effects should they occur and also to help patients weigh risks relative to potential benefits. Table 1 provides a summary of potential adverse effects, written in plain language and readily understood by most patients, to facilitate discussion of risks with patients.
Despite increased use of opioids for long-term management of chronic pain, there remain large gaps in understanding of the basic physiology, efficacy, and side effects of opioid medications, particularly when used over long periods of time.54 Limitations of this literature review are inextricably linked to the weaknesses in the available evidence. There is a need for additional research on adverse effects of opioids across all systems and for studies that evaluate aggregate risks of chronic opioid therapy relative to observed benefits. Future research should take into account not just adverse effects related to chronic opioid therapy, but also differences in risk by differences in regimen (eg, by dose, sustained-release versus short-acting opioids) and by the methods of prescribing and monitoring. Research must also investigate the long-term efficacy of chronic opioid therapy, titrating opioid dosages appropriately, developing care plans for patients at varying levels of drug abuse, and adequacy of monitoring.49 A systems-based understanding and characterization of adverse effects may help improve patient care outcomes in managing chronic pain.
In conclusion, chronic opioid treatment for noncancer pain is associated with diverse adverse effects across many organ systems. These effects range from common adverse events such as constipation and sleep disturbance, to less frequent but potentially lethal outcomes such as respiratory depression. The combination of central nervous system effects such as sedation and dizziness and musculoskeletal sequelae such as osteoporosis may increase risks of serious fractures. Opiate-induced androgen deficiency (hypogonadism) and associated problems of sexual dysfunction and infertility may result from opioid effects on the endocrine system. Recent studies also suggest negative cardiovascular effects such as increased risk of myocardial infarction or heart failure, as well as increased pneumonia risk among the elderly, possibly associated with immunosuppression.11,12,46
Prescription drug misuse and abuse is the fastest-rising drug addiction problem in the United States. The mean daily dose of prescribed opioids is strongly associated with risk of opioid overdose. Patients receiving 200 mg or more of morphine (or equivalent) per day showed a nearly 3-fold increase in opioid-related mortality.51 Opioid therapy may have important effects on the gastrointestinal, respiratory, musculoskeletal, and endocrine systems. The resulting adverse effects of opioid use are often realized in a dose-dependent fashion that can lead to significant decrements in quality of life and potential for overdose and death. For these reasons, it is essential that the full spectrum of risks of chronic opioid therapy be weighed against a realistic assessment of observed benefits for pain and function among all patients considering or receiving opioids for management of chronic noncancer pain.
Drug names: fentanyl (Duragesic and others), methadone (Methadose and others).
Author affiliations: The George Washington University School of Medicine and Health Sciences, Washington, DC (Dr Baldini); and Group Health Research Institute, Seattle, Washington (Drs Von Korff and Lin).
Potential conflicts of interest: Dr Von Korff receives support from grants to the Group Health Research Institute from Johnson & Johnson for developing a risk score for chronic pain prognosis and a study of acetaminophen use. Dr Lin has received grant/research support from National Institute of Mental Health and Group Health Foundation and serves on the speakers or advisory boards of Physicians Postgraduate Press, Inc. Dr Baldini reports no financial or other affiliations relevant to the subject of this article.
Funding/support: This work was supported by grants from the Group Health Foundation, the National Institute on Drug Abuse (R01 DA022557), and the National Institute on Aging (R01 AG034181).
REFERENCES
1. Office of National Drug Control Policy. 2011 Prescription Drug Abuse Prevention Plan. Epidemic: Responding to America’s Prescription Drug Abuse Crisis, 2011. http://www.whitehouse.gov/ondcp/prescription-drug-abuse. Accessed March 27, 2012.
2. Okie S. A flood of opioids, a rising tide of deaths. N Engl J Med. 2010;363(21):1981-1985. PubMed doi:10.1056/NEJMp1011512
3. Paulozzi L, Jones CM, Mack KA, et al. Vital Signs: Overdoses of Prescription Opioid Pain Relievers—United States 1999-2008. Centers for Disease Control and Prevention. MMWR Morb Mortal Wkly Rep. 2011;60(43):1487-1492. PubMed
4. American Pain Society. Clinical Guidelines for the Use of Chronic Opioid Therapy in Chronic Noncancer Pain, Evidence Review, 2009. http://www.ampainsoc.org/library/cp_guidelines.htm. Accessed March 27, 2012.
5. Trescott CE, Beck RM, Seelig MD, et al. Group Health’s initiative to avert opioid misuse and overdose among patients with chronic noncancer pain. Health Aff (Millwood). 2011;30(8):1420-1424. PubMed doi:10.1377/hlthaff.2011.0759
6. Leverence RR, Williams RL, Potter M, et al; PRIME Net Clinicians. Chronic non-cancer pain: a siren for primary care: a report from the PRImary care MultiEthnic Network (PRIME Net). J Am Board Fam Med. 2011;24(5):551-561. PubMed doi:10.3122/jabfm.2011.05.110030
7. Manchikanti L, Vallejo R, Manchikanti KN, et al. Effectiveness of long-term opioid therapy for chronic non-cancer pain. Pain Physician. 2011;14(2):E133-E156. PubMed
8. Bell TJ, Panchal SJ, Miaskowski C, et al. The prevalence, severity, and impact of opioid-induced bowel dysfunction: results of a US and European Patient Survey (PROBE 1). Pain Med. 2009;10(1):35-42. PubMed doi:10.1111/j.1526-4637.2008.00495.x
9. Panchal SJ, Mueller-Schwefe P, Wurzelman JI. Opioid induced bowel dysfunction: prevalence, pathophysiology, and burden. Int J Clin Pract. 2007; 61:(7):1181-1187. PubMed
10. Swegle JM, Logemann C. Management of common opioid-induced adverse effects. Am Fam Physician. 2006;74(8):1347-1354. PubMed
11. Solomon DH, Rassen JA, Glynn RJ, et al. The comparative safety of opioids for nonmalignant pain in older adults. Arch Intern Med. 2010;170(22):1979-1986. PubMed doi:10.1001/archinternmed.2010.450
12. Solomon DH, Rassen JA, Glynn RJ, et al. The comparative safety of analgesics in older adults with arthritis. Arch Intern Med. 2010;170(22):1968-1976. PubMed doi:10.1001/archinternmed.2010.391
13. Dennison C, Prasad M, Lloyd A, et al. The health-related quality of life and economic burden of constipation. Pharmacoeconomics. 2005;23(5):461-476. PubMed doi:10.2165/00019053-200523050-00006
14. Kwong WJ, Diels J, Kavanagh S. Costs of gastrointestinal events after outpatient opioid treatment for non-cancer pain. Ann Pharmacother. 2010;44(4): 630-640.
15. Hjalte F, Berggren AC, Bergendahl H, et al. The direct and indirect costs of opioid-induced constipation. J Pain Symptom Manage. 2010;40(5):696-703. PubMed doi:10.1016/j.jpainsymman.2010.02.019
16. Yue HJ, Guilleminault C. Opioid medication and sleep-disordered breathing. Med Clin North Am. 2010;94(3):435-446. PubMed doi:10.1016/j.mcna.2010.02.007
17. Walker JM, Farney RJ, Rhondeau SM, et al. Chronic opioid use is a risk factor for the development of central sleep apnea and ataxic breathing. J Clin Sleep Med. 2007;3(5):455-461. PubMed
18. Webster LR, Choi Y, Desai H, et al. Sleep-disordered breathing and chronic opioid therapy. Pain Med. 2008;9(4):425-432. PubMed doi:10.1111/j.1526-4637.2007.00343.x
19. Jennum P, Riha RL. Epidemiology of sleep apnoea/hypopnoea syndrome and sleep-disordered breathing. Eur Respir J. 2009;33(4):907-914. PubMed doi:10.1183/09031936.00180108
20. Punjabi NM. The epidemiology of adult obstructive sleep apnea. Proc Am Thorac Soc. 2008;5(2):136-143. PubMed doi:10.1513/pats.200709-155MG
21. Wang D, Teichtahl H, Drummer O, et al. Central sleep apnea in stable methadone maintenance treatment patients. Chest. 2005;128(3):1348-1356. PubMed doi:10.1378/chest.128.3.1348
22. Mogri M, Desai H, Webster L, et al. Hypoxemia in patients on chronic opiate therapy with and without sleep apnea. Sleep Breath. 2009;13(1):49-57. PubMed doi:10.1007/s11325-008-0208-4
23. Paulozzi LJ, Ryan GW. Opioid analgesics and rates of fatal drug poisoning in the United States. Am J Prev Med. 2006;31(6):506-511. PubMed doi:10.1016/j.amepre.2006.08.017
24. Bohnert AS, Valenstein M, Bair MJ, et al. Association between opioid prescribing patterns and opioid overdose-related deaths. JAMA. 2011;305(13):1315-1321. PubMed doi:10.1001/jama.2011.370
25. Dunn KM, Saunders KW, Rutter CM, et al. Opioid prescriptions for chronic pain and overdose: a cohort study. Ann Intern Med. 2010;152(2):85-92. PubMed
26. Carman WJ, Su S, Cook SF, et al. Coronary heart disease outcomes among chronic opioid and cyclooxygenase-2 users compared with a general population cohort. Pharmacoepidemiol Drug Saf. 2011;20(7):754-762. PubMed doi:10.1002/pds.2131
27. Chou R, Fanciullo GJ, Fine PG, et al; American Pain Society-American Academy of Pain Medicine Opioids Guidelines Panel. Clinical guidelines for the use of chronic opioid therapy in chronic noncancer pain. J Pain. 2009;10(2):113-130, e22. PubMed doi:10.1016/j.jpain.2008.10.008
28. Silverman SM. Opioid induced hyperalgesia: clinical implications for the pain practitioner. Pain Physician. 2009;12(3):679-684. PubMed
29. Sullivan MD, Von Korff M, Banta-Green C, et al. Problems and concerns of patients receiving chronic opioid therapy for chronic non-cancer pain. Pain. 2010;149(2):345-353. PubMed doi:10.1016/j.pain.2010.02.037
30. Braden JB, Russo J, Fan MY, et al. Emergency department visits among recipients of chronic opioid therapy. Arch Intern Med. 2010;170(16):1425-1432. PubMed doi:10.1001/archinternmed.2010.273
31. Vestergaard P, Rejnmark L, Mosekilde L. Fracture risk associated with the use of morphine and opiates. J Intern Med. 2006;260(1):76-87. PubMed doi:10.1111/j.1365-2796.2006.01667.x
32. Miller M, Sturmer T, Azrael D, et al. Opioid analgesics and the risk of fractures in older adults with arthritis. J Am GeriatrSociety. 2011;59(3)430-438
33. Takkouche B, Montes-Mart×nez A, Gill SS, et al. Psychotropic medications and the risk of fracture: a meta-analysis. Drug Saf. 2007;30(2):171-184. PubMed doi:10.2165/00002018-200730020-00006
34. Shorr RI, Griffin MR, Daugherty JR, et al. Opioid analgesics and the risk of hip fracture in the elderly: codeine and propoxyphene. J Gerontol. 1992;47(4):M111-M115. PubMed
35. Ensrud KE, Blackwell T, Mangione CM, et al; Study of Osteoporotic Fractures Research Group. Central nervous system active medications and risk for fractures in older women. Arch Intern Med. 2003;163(8):949-957. PubMed doi:10.1001/archinte.163.8.949
36. Saunders KW, Dunn KM, Merrill JO, et al. Relationship of opioid use and dosage levels to fractures in older chronic pain patients. J Gen Intern Med. 2010;25(4):310-315. PubMed doi:10.1007/s11606-009-1218-z
37. Kamal-Bahl SJ, Stuart BC, Beers MH. Propoxyphene use and risk for hip fractures in older adults. Am J Geriatr Pharmacother. 2006;4(3):219-226. PubMed doi:10.1016/j.amjopharm.2006.09.005
38. Brauer CA, Coca-Perraillon M, Cutler DM, et al. Incidence and mortality of hip fractures in the United States. JAMA. 2009;302(14):1573-1579. PubMed doi:10.1001/jama.2009.1462
39. Rohde G, Haugeberg G, Mengshoel AM, et al. Two-year changes in quality of life in elderly patients with low-energy hip fractures: a case-control study. BMC Musculoskelet Disord. 2010;11(1):226. PubMed doi:10.1186/1471-2474-11-226
40. Tosteson AN, Gabriel SE, Grove MR, et al. Impact of hip and vertebral fractures on quality-adjusted life years. Osteoporos Int. 2001;12(12):1042-1049. PubMed doi:10.1007/s001980170015
41. Vuong C, Van Uum SH, O’ Dell LE, et al. The effects of opioids and opioid analogs on animal and human endocrine systems. Endocr Rev. 2010;31(1):98-132. PubMed doi:10.1210/er.2009-0009
42. Katz N, Mazer NA. The impact of opioids on the endocrine system. Clin J Pain. 2009;25(2):170-175. PubMed doi:10.1097/AJP.0b013e3181850df6
43. Rajagopal A, Vassilopoulou-Sellin R, Palmer JL, et al. Symptomatic hypogonadism in male survivors of cancer with chronic exposure to opioids. Cancer. 2004;100(4):851-858. PubMed doi:10.1002/cncr.20028
44. Rhodin A, Stridsberg M, Gordh T. Opioid endocrinopathy: a clinical problem in patients with chronic pain and long-term oral opioid treatment. Clin J Pain. 2010;26(5):374-380. PubMed doi:10.1097/AJP.0b013e3181d1059d
45. Sacerdote P. Opioid-induced immunosuppression. Curr Opin Support Palliat Care. 2008;2(1):14-18. PubMed doi:10.1097/SPC.0b013e3282f5272e
46. Dublin S, Walker RL, Jackson ML, et al. Use of opioids or benzodiazepines and risk of pneumonia in older adults: a population-based case-control study. J Am Geriatr Soc. 2011;59(10):1899-1907. PubMed doi:10.1111/j.1532-5415.2011.03586.x
47. Fleming MF, Balousek SL, Klessig CL, et al. Substance use disorders in a primary care sample receiving daily opioid therapy. J Pain. 2007;8(7):573-582. PubMed doi:10.1016/j.jpain.2007.02.432
48. Boscarino JA, Rukstalis M, Hoffman SN, et al. Risk factors for drug dependence among out-patients on opioid therapy in a large US health-care system. Addiction. 2010;105(10):1776-1782. PubMed doi:10.1111/j.1360-0443.2010.03052.x
49. Jackman RP, Purvis JM, Mallett BS. Chronic nonmalignant pain in primary care. Am Fam Physician.2008;78(10):1155-1162. PubMed
50. Von Korff M, Kolodny A, Deyo RA, et al. Long-term opioid therapy reconsidered. Ann Intern Med. 2011;155(5):325-328. PubMed
51. Gomes T, Mamdani MM, Dhalla IA, et al. Opioid dose and drug-related mortality in patients with nonmalignant pain. Arch Intern Med. 2011;171(7):686-691. PubMed doi:10.1001/archinternmed.2011.117
52. Cicero TJ, Lynskey M, Todorov A, et al. Co-morbid pain and psychopathology in males and females admitted to treatment for opioid analgesic abuse. Pain. 2008;139(1):127-135. PubMed doi:10.1016/j.pain.2008.03.021
53. White AG, Birnbaum HG, Mareva MN, et al. Direct costs of opioid abuse in an insured population in the United States. J Manag Care Pharm. 2005;11(6):469-479. PubMed
54. Chou R, Ballantyne JC, Fanciullo GJ, et al. Research gaps on use of opioids for chronic noncancer pain: findings from a review of the evidence for an American Pain Society and American Academy of Pain Medicine clinical practice guideline. J Pain. 2009;10(2):147-159, e15. PubMed doi:10.1016/j.jpain.2008.10.007