Objective: We assessed the clinical utility of the Alabama Brief Cognitive Screener (ABCs), an alternative to the Mini-Mental State Examination (MMSE), for cognitive screening in a new electronic medical record. Other available nonproprietary instruments were determined to be more tuned to milder deficits than the MMSE.
Methods: The ABCs was administered as part of routine clinical assessment in the University of Alabama at Birmingham memory disorders clinics from April 30, 2012, to April 30, 2015. Outpatients (N = 1,589) with clinician diagnoses (ICD-9-CM) of memory loss, mild cognitive impairment, neurodegenerative cognitive impairment, Alzheimer’s dementia, or dementia not otherwise specified were included in the analysis. Memory disorder clinicians used multiple sources of information for assignment of diagnoses, including interviews with patients and caregivers, the ABCs, figure copy, semantic fluencies, phonemic fluencies, ratings of daily function, imaging, laboratory tests, and medical records.
Results: Scoring distribution by diagnosis was mild cognitive impairment (n = 310): mean (SD) = 25.47 (3.37), median = 26; Alzheimer’s dementia (n = 208): mean (SD) = 16.42 (6.33), median = 17; cerebral degeneration (n = 371): mean (SD) = 20.61 (5.90), median = 21; memory loss (n = 583): mean (SD) = 24.90 (5.09), median = 27; and dementia (n = 117): mean (SD) = 15.18 (6.34), median = 15. Mean ABCs scores differed by diagnosis (Wilcoxon signed-ranks Z = 483.5, P < .001). This finding was consistent with a meta-analysis of MMSE performance between groups.
Conclusions: ABCs scores vary appropriately by diagnosis and resemble MMSE scoring distributions. The ABCs provides a nonproprietary alternative to the MMSE to assess the severity of cognitive deficits.
Alabama Brief Cognitive Screener:
Utility of a New Cognitive Screening Instrument
in a Memory Disorders Clinic
ABSTRACT
Objective: We assessed the clinical utility of the Alabama Brief Cognitive Screener (ABCs), an alternative to the Mini-Mental State Examination (MMSE), for cognitive screening in a new electronic medical record. Other available nonproprietary instruments were determined to be more tuned to milder deficits than the MMSE.
Methods: The ABCs was administered as part of routine clinical assessment in the University of Alabama at Birmingham memory disorders clinics from April 30, 2012, to April 30, 2015. Outpatients (N = 1,589) with clinician diagnoses (ICD-9-CM) of memory loss, mild cognitive impairment, neurodegenerative cognitive impairment, Alzheimer’s dementia, or dementia not otherwise specified were included in the analysis. Memory disorder clinicians used multiple sources of information for assignment of diagnoses, including interviews with patients and caregivers, the ABCs, figure copy, semantic fluencies, phonemic fluencies, ratings of daily function, imaging, laboratory tests, and medical records.
Results: Scoring distribution by diagnosis was mild cognitive impairment (n = 310): mean (SD) = 25.47 (3.37), median = 26; Alzheimer’s dementia (n = 208): mean (SD) = 16.42 (6.33), median = 17; cerebral degeneration (n = 371): mean (SD) = 20.61 (5.90), median = 21; memory loss (n = 583): mean (SD) = 24.90 (5.09), median = 27; and dementia (n = 117): mean (SD) = 15.18 (6.34), median = 15. Mean ABCs scores differed by diagnosis (Wilcoxon signed-ranks Z = 483.5, P < .001). This finding was consistent with a meta-analysis of MMSE performance between groups.
Conclusions: ABCs scores vary appropriately by diagnosis and resemble MMSE scoring distributions. The ABCs provides a nonproprietary alternative to the MMSE to assess the severity of cognitive deficits.
Prim Care Companion CNS Disord 2019;21(2):18m02336
To cite: Natelson Love MC, Pilonieta G, Geldmacher DS. Alabama Brief Cognitive Screener: utility of a new cognitive screening instrument in a memory disorders clinic. Prim Care Companion CNS Disord. 2019;21(2):18m02336.
To share: https://doi.org/10.4088/PCC.18m02336
© Copyright 2019 Physicians Postgraduate Press, Inc.
aDepartment of Neurology, University of Alabama at Birmingham, Birmingham, Alabama
bDepartment of Neurology, Birmingham Veterans Affairs Medical Center, Birmingham, Alabama
*Corresponding author: Giovanna Pilonieta, DDS, MPH, Department of Neurology, University of Alabama at Birmingham, Ste 640, Sparks Center, 1720 7th Ave South, Birmingham, AL 35294-0017 ([email protected]).
Assessment of cognition is an established element of both primary care and specialty medical practice. Guidelines call for structured assessment of cognition among older adults with standardized instruments1 and for annual assessment of cognition for people with dementia using reliable, validated tests.2 Quantitative tests of cognition are also recommended for initial assessment of suspected dementia in primary care settings.3
The Mini-Mental State Examination (MMSE)4 has become the most widely used of these tests.5 Originally developed as a means to rapidly measure cognitive function among psychiatric patients, its ease of use and face validity led to widespread adoption. The MMSE’s authors have acknowledged that it was developed as a standardized administration of well-known cognitive assessment elements and that the instrument has shortcomings.6 However, the MMSE’s clinical utility is unquestionable, and an extensive body of literature has defined its performance across a wide variety of health states, diseases, cultures, and languages.
Alternative instruments such as the Saint Louis University Mental Status (SLUMS) examination7 and the Montreal Cognitive Assessment (MoCA)8 have been developed. They have proved to be useful, valid tests.8–10 On the whole, they are somewhat more difficult than the MMSE, resulting in different scores and diagnostic categories in equivalent samples.11 The greater difficulty has made these tools useful to detect conditions characterized by less severe cognitive deficits such as mild cognitive impairment, which had not been defined when the MMSE was published.10,12
Although widely used in both clinical and research settings for over 2 decades, and freely available through the internet, the MMSE’s copyright changed hands in 2000. The new rights holder became aggressive in protecting their copyright and actively suppressed presumptive violations.13 With impending implementation of a new electronic medical records system at our institution, a need existed for a psychometrically valid and neuropsychologically sound alternative to the MMSE that would (1) perform similarly in primary care and neurologic populations, (2) not violate the MMSE copyright, and (3) be readily adaptable for implementation in the electronic medical record.
METHODS
We examined the structure of available brief cognitive instruments assessed in the Dementia Working Group’s development of quality standards for dementia care2 ranging from very brief tests like the Mini-Cog14 and Six-Item Screener15 to standard screeners like the MMSE, MoCA, and SLUMS, as well as extended batteries like the Modified Mini-Mental State (3MS)16 and the Florida Mental Status Exam.17 The Severe MMSE,18 Blessed Orientation-Memory-Concentration Test,19 and Short Portable Mental Status Questionnaire20 were also reviewed.
Common themes identified across most or all of these tests were verbal recall immediately and after brief delay (usually of 3–5 words), orientation to time and place, calculation, naming, repetition, and figure drawing or copying. Since one goal of the new instrument was to mimic MMSE scoring distributions, we attempted to select items of similar difficulty while addressing some of the potentially problematic MMSE items such as the difficulty associated with the alternative items of serial 7 subtractions and spelling world backward, the challenges of knowing the county for people traveling long distances for evaluation, and the idiomatic, agrammatic phrase “no ifs, ands, or buts,” which is unfamiliar to many patients.
In addition to the themes observed in existing screening examinations, we intended for the new instrument to meet documentation requirements of the 1997 Documentation Guidelines for Evaluation and Management Services from the US Centers for Medicare and Medicaid Services (Table 1).21 Additionally, since cognitive testing can be construed as a procedure, we chose to include 2 personal identifiers (name and year of birth) as scored items, which is consistent with the Joint Commission on Accreditation of Healthcare Organizations National Patient Safety Goals.22 These items also previously appeared in the severe impairment MMSE adaptation developed at our institution.18

A draft 30-item instrument was developed by one of the authors (D.S.G.) and reviewed for face validity and consensus by the faculty of the University of Alabama at Birmingham (UAB) Divisions of Memory Disorders and Behavioral Neurology and Neuropsychology. Minor revisions and suggestions were incorporated. The instrument was named the Alabama Brief Cognitive screener (ABCs). An immediate clinical need for a nonproprietary instrument to be incorporated in the electronic medical record led to implementation with plans to assess validity and reliability based on its performance in the clinical setting. This process closely parallels the initial implementation of the MMSE.4,6 The implemented version of the ABCs is depicted in Figure 1.
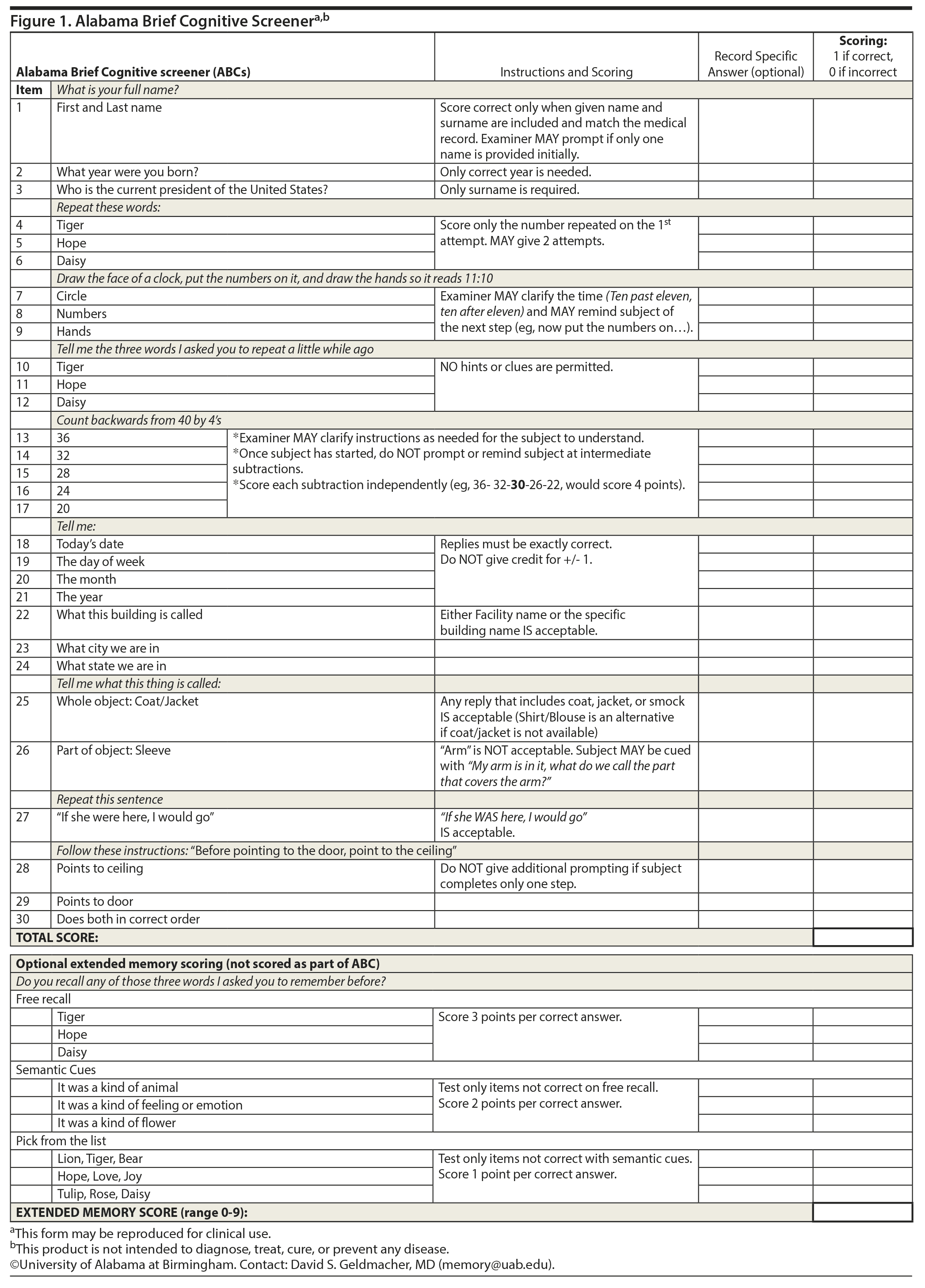
The ABCs was administered as part of the routine clinical assessment in the UAB memory disorders clinics from April 30, 2012, to April 30, 2015. The UAB memory disorders clinics serve as the sole neurology-based referral center for dementia and related disorders in the state of Alabama and portions of the surrounding states, representing a service area encompassing over 5 million individuals. The majority of ABCs testing was conducted by a licensed practical nurse trained on administration of the instrument and with more than 5 years’ experience in the administration of brief cognitive tests. Administration of the ABCs takes approximately 5–7 minutes. Approval for post hoc chart review was obtained from the institutional review board. All study procedures were adherent to the Helsinki principles.
Patients from 5 academic neurologists and 2 nurse practitioners with specialty practices in cognitive and behavioral neurology were included. Patients with clinician diagnoses of memory loss (ICD-9-CM 780.93), mild cognitive impairment (331.83), neurodegenerative cognitive impairment (331.9), Alzheimer’s dementia (331.0), or dementia not otherwise specified (NOS, 294.8) were included in the analysis.
Operationally, memory disorder clinicians used multiple sources of information for assignment of diagnoses, including interviews with patients and caregivers, the ABCs, figure copy, word list generation (semantic and phonemic fluencies), ratings of daily function, imaging, laboratory tests, and medical records. All of these factors were used for diagnostic assignments when available at the time of the visit. Clinical criteria for mild cognitive impairment23 and Alzheimer’s disease24 were employed. “Memory loss” was typically used as a diagnosis when a patient had memory symptoms or impairments insufficient to meet criteria for mild cognitive impairment or dementia. “Neurodegenerative cognitive impairment” was generally used at initial visits when patients had evidence for meaningful cognitive impairment, but criteria for a specific disorder were not met (eg, prior records, laboratory tests or imaging were pending at the time of the visit). “Dementia NOS” was used when dementia was clearly present, but the clinician could not classify the patient to any more specific category often because of severity or unavailable history regarding the onset and early symptoms or multiple contributing causes.
Statistical analysis was performed by using t and χ2 tests to compare the associations between diagnosis, age, and sex. Independent sample t test and Wilcoxon-Kruskal-Wallis rank sum were used to analyze performance for the ABCs across the diagnoses. These statistical analyses were performed using SAS (version 9.3) software (SAS Institute, Cary, North Carolina).
RESULTS
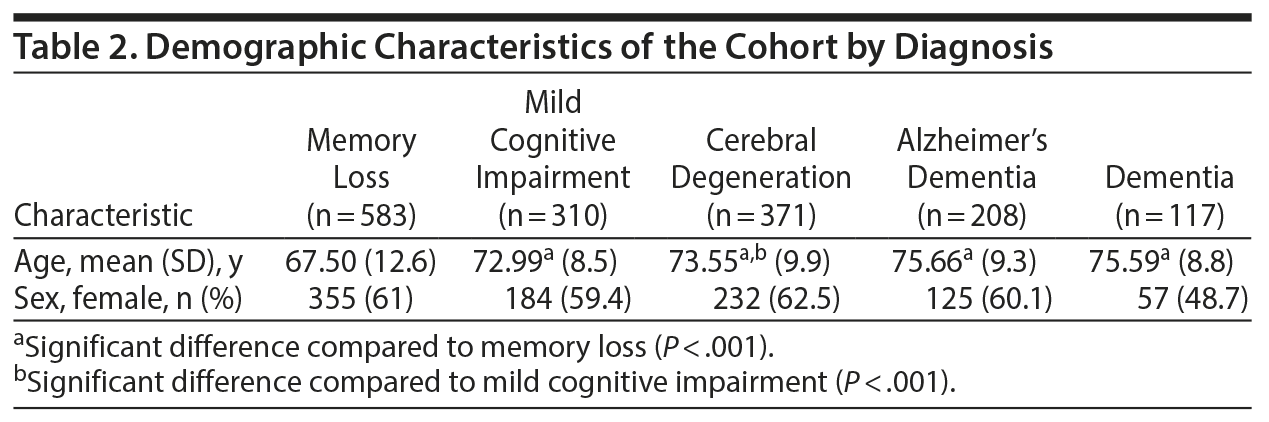
Data were available from 1,589 individuals (953 [60%] women, 636 [40%] men; mean age of 71.65 years) (Table 2). Age varied by diagnostic category (analysis of variance F=37.89, P < .001), with memory loss patients having a mean age of 67.5 years, while the other 4 groups’ mean age ranged from 73.0 (mild cognitive impairment) to 75.7 (Alzheimer’s dementia). Mean ABCs scores differed by diagnosis (Wilcoxon signed-ranks Z = 483.5, P < .001). This result was consistent with performance of the MMSE in a meta-analysis of MMSE in Alzheimer’s disease by Han and colleagues.25
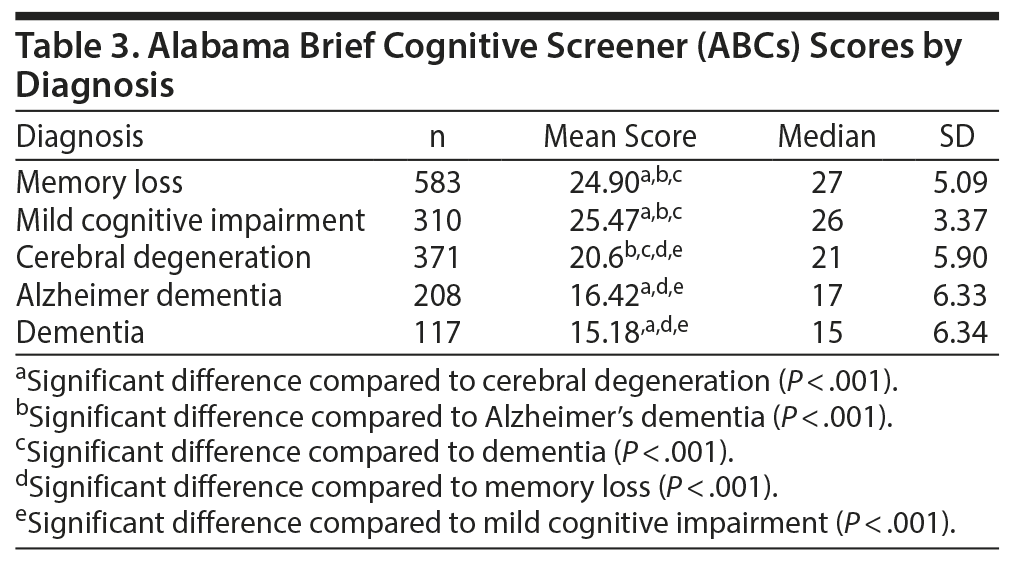
Scoring distributions by diagnosis are reported in Table 3. As intended from the construction of the instrument, patients with the diagnoses of mild cognitive impairment had higher mean scores than those with Alzheimer’s-type and unspecified dementia. (P < .001). Additionally, those with unspecified memory loss achieved higher scores than the dementia groups (P < .001). Patients with dementia had the lowest ABCs score (15.18 ± 6.3).
DISCUSSION
ABCs scores vary appropriately by diagnosis. This finding is similar to the performance of the MMSE shown by Benson and colleagues26 between individuals with normal cognition, mild cognitive impairment, and Alzheimer’s dementia. A meta-analysis25 of MMSE in Alzheimer’s disease reported a mean score among 3,260 subjects of 16.08 out of 30. Our sample of 208 subjects had a mean ABCs score of 16.42. The mean MMSE score in mild cognitive impairment among 1,376 subjects was 26.78,25 while our sample of 310 subjects had a mean ABCs score of 25.47. This result suggests that the ABCs and MMSE scores have similar distributions in these clinical populations.
There are limitations to this study. As a chart review study, no autopsy confirmation of diagnoses was available in this sample. The information used to establish diagnosis most likely varied between clinicians and differed from one patient to another on the basis of availability of family members, medical records, prior imaging, and other variables typically observed in clinical practice. Importantly, ABCs scores themselves were a factor in diagnostic assignment, inserting potential bias into the assigned diagnoses. However, these variables reflect the reality of clinical practice, in which cognitive test scores are an important part of diagnostic assignments. Importantly, the diagnoses in these groups were determined by academic medical center expert providers in cognitive neurology and included other factors such as reported daily function, mood assessments, and cognitive testing outside the ABCs in the determination of diagnosis. The consistency of performance between the ABCs and Han and colleagues’ meta-analysis25 of the MMSE in similar settings indicates that the design goals of the ABCs were met. Future studies should include direct comparison to the MMSE as well as other validated cognitive tests to increase validity. Data are also currently being collected to identify how age and educational attainment influence results, as these variables are typically used in interpreting MMSE scores.
The ABCs shows promise as an easily administered, nonproprietary alternative to the MMSE for use as a screening instrument to both identify and assess severity of cognitive deficits in medical practice. Although the ABCs is copyrighted, it is intended to remain free and available for use in clinical and noncommercial research use. Further characterization of the instrument is underway, including its effectiveness in measuring progression of deficits in patients with neurodegenerative disease and its relationship to instrumental activities of daily living. Primary care physicians play a critical role in the detection, diagnosis, and treatment of people with Alzheimer’s disease and other disorders with cognitive symptoms.27 Data from the ABCs indicate it might prove a worthwhile tool for expansion of dementia assessment in primary care settings.
Submitted: June 1, 2018; accepted November 28, 2019.
Published online: March 14, 2019.
Potential conflicts of interest: None.
Funding/support: None.
Previous presentation: Poster presented at the 2014 International Neuropsychological Society annual meeting; February 12–15, 2014; Seattle, Washington ▪ American Academy of Neurology annual meeting; April 26–May 3, 2014; Philadelphia, Pennsylvania ▪ Alzheimer’s Association International Conference; July 18–23, 2015; Washington, DC ▪ American Neurological Association annual meeting; October 16–18, 2016; Baltimore, Maryland.
REFERENCES
1. Cordell CB, Borson S, Boustani M, et al; Medicare Detection of Cognitive Impairment Workgroup. Alzheimer’s Association recommendations for operationalizing the detection of cognitive impairment during the Medicare annual wellness visit in a primary care setting. Alzheimers Dement. 2013;9(2):141–150. PubMed CrossRef
2. Odenheimer G, Borson S, Sanders AE, et al. Quality improvement in neurology: dementia management quality measures. Neurology. 2013;81(17):1545–1549. PubMed CrossRef
3. Simmons BB, Hartmann B, Dejoseph D. Evaluation of suspected dementia. Am Fam Physician. 2011;84(8):895–902. PubMed
4. Folstein MF, Folstein SE, McHugh PR. “Mini-mental state”: a practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975;12(3):189–198. PubMed CrossRef
5. Tombaugh TN, McIntyre NJ. The Mini-Mental State Examination: a comprehensive review. J Am Geriatr Soc. 1992;40(9):922–935. PubMed CrossRef
6. Folstein M. The birth of the MMS. Current Contents; 1990:18.
7. Tariq SH, Tumosa N, Chibnall JT, et al. Comparison of the Saint Louis University Mental Status examination and the Mini-Mental State Examination for detecting dementia and mild neurocognitive disorder: a pilot study. Am J Geriatr Psychiatry. 2006;14(11):900–910. PubMed CrossRef
8. Nasreddine ZS, Phillips NA, Bédirian V, et al. The Montreal Cognitive Assessment, MoCA: a brief screening tool for mild cognitive impairment. J Am Geriatr Soc. 2005;53(4):695–699. PubMed CrossRef
9. Cummings-Vaughn LA, Chavakula NN, Malmstrom TK, et al. Veterans Affairs Saint Louis University Mental Status examination compared with the Montreal Cognitive Assessment and the Short Test of Mental Status. J Am Geriatr Soc. 2014;62(7):1341–1346. PubMed CrossRef
10. Smith T, Gildeh N, Holmes C. The Montreal Cognitive Assessment: validity and utility in a memory clinic setting. Can J Psychiatry. 2007;52(5):329–332. PubMed CrossRef
11. Howland M, Tatsuoka C, Smyth KA, et al. Detecting change over time: a comparison of the SLUMS examination and the MMSE in older adults at risk for cognitive decline. CNS Neurosci Ther. 2016;22(5):413–419. PubMed CrossRef
12. Trzepacz PT, Hochstetler H, Wang S, et al; Alzheimer’s Disease Neuroimaging Initiative. Relationship between the Montreal Cognitive Assessment and Mini-Mental State Examination for assessment of mild cognitive impairment in older adults. BMC Geriatr. 2015;15(1):107. PubMed CrossRef
13. Newman JC, Feldman R. Copyright and open access at the bedside. N Engl J Med. 2011;365(26):2447–2449. PubMed CrossRef
14. Borson S, Scanlan J, Brush M, et al. The Mini-Cog: a cognitive ‘vital signs’ measure for dementia screening in multi-lingual elderly. Int J Geriatr Psychiatry. 2000;15(11):1021–1027. PubMed CrossRef
15. Callahan CM, Unverzagt FW, Hui SL, et al. Six-item screener to identify cognitive impairment among potential subjects for clinical research. Med Care. 2002;40(9):771–781. PubMed CrossRef
16. Teng EL, Chui HC. The Modified Mini-Mental State (3MS) Examination. J Clin Psychiatry. 1987;48(8):314–318. PubMed
17. Doty L, Bowers D, Heilman KM. Florida Mental Status Exam for progressive dementia screening [abstract] Gerontologist. 1990;30:20A [special issue].
18. Harrell LE, Marson D, Chatterjee A, et al. The Severe Mini-Mental State Examination: a new neuropsychologic instrument for the bedside assessment of severely impaired patients with Alzheimer disease. Alzheimer Dis Assoc Disord. 2000;14(3):168–175. PubMed CrossRef
19. Katzman R, Brown T, Fuld P, et al. Validation of a short Orientation-Memory-Concentration Test of cognitive impairment. Am J Psychiatry. 1983;140(6):734–739. PubMed CrossRef
20. Pfeiffer E. A Short Portable Mental Status Questionnaire for the assessment of organic brain deficit in elderly patients. J Am Geriatr Soc. 1975;23(10):433–441. PubMed CrossRef
21. Centers for Medicare & Medicaid Services. 1997 Documentation Guidelines for Evaluation and Management Services. https://www.cms.gov/outreach-and-education/medicare-learning-network-mln/mlnedwebguide/downloads/97docguidelines.pdf. Accessed June 21, 2016.
22. JCAHO approves National Patient Safety Goals for 2003. Jt Comm Perspect. 2002;22(9):1–3. PubMed
23. Winblad B, Palmer K, Kivipelto M, et al. Mild cognitive impairment–beyond controversies, towards a consensus: report of the International Working Group on Mild Cognitive Impairment. J Intern Med. 2004;256(3):240–246. PubMed CrossRef
24. American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fourth Edition, Text Revision. Washington, DC: American Psychiatric Association; 2000.
25. Han L, Cole M, Bellavance F, et al. Tracking cognitive decline in Alzheimer’s disease using the Mini-Mental State Examination: a meta-analysis. Int Psychogeriatr. 2000;12(2):231–247. PubMed CrossRef
26. Benson AD, Slavin MJ, Tran TT, et al. Screening for early Alzheimer’s disease: is there still a role for the Mini-Mental State Examination? Prim Care Companion J Clin Psychiatry. 2005;7(2):62–69. PubMed CrossRef
27. Geldmacher DS, Kerwin DR. Practical diagnosis and management of dementia due to Alzheimer’s disease in the primary care setting: an evidence-based approach. Prim Care Companion CNS Disord. 2013;15(4):PCC.12r01474. PubMed. 10.4088/PCC.12r01474
Enjoy this premium PDF as part of your membership benefits!


