Alcohol and Prescription Drug Abuse and Borderline Personality Disorder Symptomatology Among Male and Female Perpetrators of Partner Violence
To the Editor: Relationships between alcohol misuse and violence are well known.1 As examples, alcohol misuse is associated with personal injuries,2 perpetration of dating violence,3 and partner violence4 (ie, there appears to be a general association between alcohol misuse and person-related violence to self/others). Similarly, substance misuse is associated with borderline personality disorder (BPD).5 Given these general relationships, we hypothesized that among individuals court ordered to treatment for perpetration of partner violence, BPD symptomatology would nonetheless predict for higher rates of alcohol and prescription drug misuse.
Method. Participants in this study were adult men and women residing in the midcentral United States who were court referred to treatment for the perpetration of partner violence. Of the 235 individuals approached, 193 agreed to participate (170 men, 23 women), for a response rate of 82.1%. All endorsed an age range between 18 and 65 years, with most indicating an age between 21 and 40 years (71.5%). Likewise, 83 were white (43.0%), 38 were black (19.7%), 28 were Native American (14.5%), 22 were Hispanic/Latino (11.4%), 21 were other (10.9%), and 1 was Asian (0.5%). Data were collected from June 2013 to October 2013.
Participants were solicited, provided informed consent, and completed surveys onsite at 1 of 24 different treatment groups conducted across 4 agencies. Each subject completed the Self-Harm Inventory (SHI),6 a 22-item, yes/no, self-report inventory that explores participants’ histories of self-harm behavior and assesses for BPD symptomatology. The SHI total score is the summation of "yes" responses.6 In comparison with the Diagnostic Interview for Borderlines,7 cutoff scores on the SHI of 5 (traditional cutoff) and 7 (more conservative cutoff) demonstrate an accuracy in BPD diagnosis of 84% and 88%, respectively.6 This project was approved by an institutional review board.
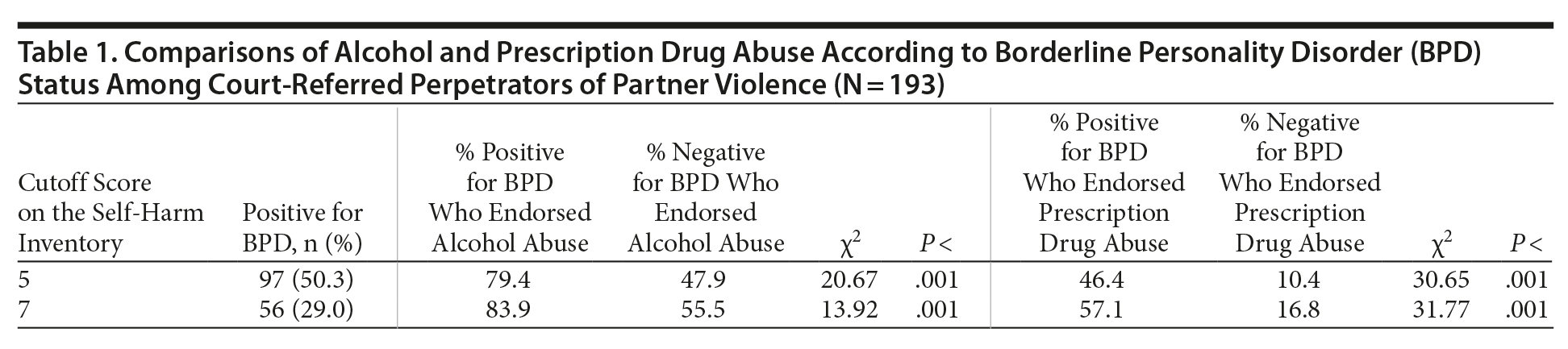
Results. Of 193 respondents, 123 endorsed the SHI item pertaining to having ever intentionally abused alcohol (63.7%), whereas 55 endorsed the SHI item pertaining to having ever abused prescription drugs (28.5%). These 2 items of interest were not included in the scoring of the SHI for determination of BPD symptomatology. Table 1 provides comparisons for self-reported alcohol and prescription drug abuse among participants, according to cutoff scores of 5 (traditional) and 7 (more conservative) for BPD symptomatology. The BPD subsample consistently evidenced greater rates of alcohol and prescription drug abuse regardless of cutoff score.
The potential limitations of this study include the use of a self-report measure for BPD (risk of false positives), a severe group of partner-violent individuals (ie, findings may not generalize to less severe individuals), and use of single-item measures for alcohol abuse and prescription drug abuse. However, to our knowledge, this is the first study to confirm these clinically distinguishing relationships—that individuals with BPD symptomatology demonstrate higher rates of abuse of alcohol and prescription drugs, even in a sample of individuals convicted for perpetration of partner violence. Findings indicate the need for thorough substance abuse assessment and treatment in perpetrators of partner violence with BPD symptomatology.
References
1. Proescholdt MG, Walter M, Wiesbeck GA. Alcohol and violence: a current review[in German]. Fortschr Neurol Psychiatr. 2012;80(8):441-449. PubMed
2. Zerhouni O, Bרgue L, Brousse G, et al. Alcohol and violence in the emergency room: a review and perspectives from psychological and social sciences. Int J Environ Res Public Health. 2013;10(10):4584-4606. PubMed doi:10.3390/ijerph10104584
3. Rothman EF, McNaughton Reyes L, Johnson RM, et al. Does the alcohol make them do it? dating violence perpetration and drinking among youth. Epidemiol Rev. 2012;34(1):103-119. PubMed doi:10.1093/epirev/mxr027
4. Cunradi CB. Neighborhoods, alcohol outlets and intimate partner violence: addressing research gaps in explanatory mechanisms. Int J Environ Res Public Health. 2010;7(3):799-813. PubMed doi:10.3390/ijerph7030799
5. Sansone RA, Sansone LA. Substance use disorders and borderline personality: common bedfellows. Innov Clin Neurosci. 2011;8(9):10-13. PubMed
6. Sansone RA, Wiederman MW, Sansone LA. The Self-Harm Inventory (SHI): development of a scale for identifying self-destructive behaviors and borderline personality disorder. J Clin Psychol. 1998;54(7):973-983. PubMed doi:10.1002/(SICI)1097-4679(199811)54:7<973::AID-JCLP11>3.0.CO;2-H
7. Kolb JE, Gunderson JG. Diagnosing borderline patients with a semistructured interview. Arch Gen Psychiatry. 1980;37(1):37-41. PubMed doi:10.1001/archpsyc.1980.01780140039004
Author affiliations: Departments of Psychiatry and Internal Medicine, Wright State University School of Medicine, Dayton, and Department of Psychiatry Education, Kettering Medical Center, Kettering, Ohio (Dr Sansone); The Violence Prevention Program, University of Central Oklahoma, Edmond, Oklahoma (Mr Elliott); and Department of Psychology, Columbia College, Columbia, South Carolina (Dr Wiederman).
Potential conflicts of interest: None reported.
Funding/support: None reported.
Published online: November 27, 2014.
Prim Care Companion CNS Disord 2014;16(6):doi:10.4088/PCC.14l01678
© Copyright 2014 Physicians Postgraduate Press, Inc.