Prim Care Companion CNS Disord 2023;25(2):22br03441
To cite: Mahlstedt JH, Avery JD, Mroczkowski MM. An approach to address the need for adolescent opioid stabilization and treatment. Prim Care Companion CNS Disord. 2023;25(2):22br03441.
To share: https://doi.org/10.4088/PCC.22br03441
© 2023 Physicians Postgraduate Press, Inc.
aNewYork-Presbyterian Westchester Behavioral Health Center, White Plains, New York
bDepartment of Psychiatry, Weill Cornell Medicine, New York, New York
cDepartment of Psychiatry, Columbia University Irving Medical Center, New York, New York
*Corresponding author: John H. Mahlstedt, MD, Office C203, 21 Bloomingdale Rd, White Plains, NY 10605 ([email protected]).
Despite national efforts to identify and treat substance use disorders, drug overdose deaths remain stubbornly high in the United States. In 2019, there were 70,630 overdose deaths across the United States, and roughly 70% involved opioids.1 During the coronavirus disease 2019 pandemic, the rates of overdose have increased, including those in adolescents.2 Adolescent overdose deaths in the United States have increased in the past decade; there were 518 overdose deaths in 2010 compared to 954 in 2020, and deaths increased further to 1,146 in 2021.3 Despite recent improvements in identifying and treating substance use disorders, opioid use and addiction still start at young ages. Furthermore, nationwide surveys have reported at least 5%–6% of high school students have tried prescription opioids non-medically before graduating.4
The American Academy of Pediatrics Committee on Substance Use and Prevention advocates for increasing access to medication-assisted treatment (MAT) for opioid use disorder in young people and for pediatricians to prescribe these medications when indicated.5 Yet, studies6 show the majority of youth with opioid use disorder do not receive MAT, and those who do are often delayed by at least 6 months from their diagnosis. In the fall of 2020, we set out to create a hospital enterprise–wide protocol to identify and treat opioid use disorder in youth, with the shared goals of providing evidenced-based care in a standardized manner across the 13-hospital enterprise and decreasing delays to treatment.
Protocol Development and Implementation
First, we created an evidenced-based opioid stabilization protocol for adolescent patients visiting the emergency department or on the medical floors. We outlined the rationale and process for using medications for opioid use disorder, including buprenorphine, clonidine, methadone, naltrexone, and other adjuvant medications.
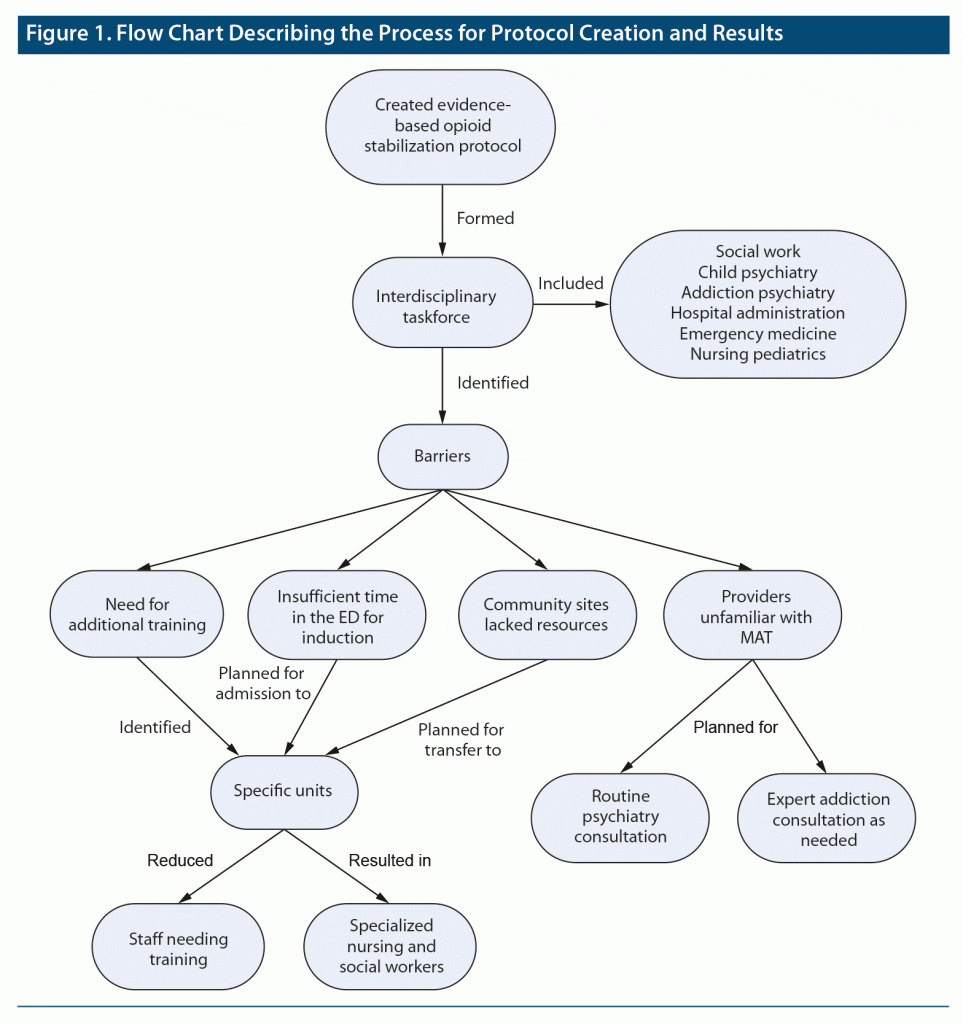
We then formed an interdisciplinary enterprise-wide taskforce, including child and adolescent psychiatry, addiction psychiatry, emergency medicine, pediatrics, pharmacy, hospital administration, nursing leadership, and others. In 7 meetings, we finalized the protocol, as well as identified and addressed many barriers in providing this care. The barriers included concerns about increased clinical demands, using unfamiliar medications, and a lack of resources at community sites.
We solved these problems in small interdepartmental work groups. Since these medications are lifesaving, and stabilization often requires a few days, we worked with leadership in hospital administration, pediatrics, and nursing to admit adolescent patients requiring opioid use treatment to 2 identified inpatient pediatrics units located in the 2 children’s hospitals of our enterprise. Nurses on these 2 units all received training in opioid withdrawal management, including administering the Clinical Opiate Withdrawal Scale7 and MAT medications. Additionally, the social work teams on both units received training on referrals for ongoing treatment. Our guidelines included a routine child and adolescent psychiatry consultation for each patient on this treatment protocol, along with additional consultation with adult addiction psychiatry as needed. Given the relative infrequency of adolescent patients on these treatment protocols, these 2 consultant teams worked to support the primary team in the use of MAT. Figure 1 provides a flowchart of the process for protocol creation and results.
Future Directions/Limitations
We hope that on our local hospital level, trainees in all involved disciplines will feel more comfortable using these medications in their clinical practice. The barriers to widespread implementation of similar guidelines include limited education, buprenorphine waiver issues, and stigma in treatment. We advocate for all hospitals to adopt similar guidelines of identifying 1 or more units for inpatient stabilization and MAT initiation, championed by nurses and social workers specifically trained in this area and led by pediatrics in close consultation with child and adolescent psychiatry and addiction psychiatry.
Submitted: October 28, 2022; accepted December 20, 2022.
Published online: April 18, 2023.
Relevant financial relationships: None.
Funding/support: NewYork-Presbyterian Hospital, Columbia University, and Weill Cornell University supported this project by supplying materials and salary support for the contributors.
Role of the sponsor: NewYork-Presbyterian Hospital, Columbia University, and Weill Cornell University had no role in the design and conduct of the study; collection, management, analysis, and interpretation of data; or preparation, review, or approval of the manuscript.
Acknowledgments: This work would not have been possible without the time, coordination, and dedication of countless professionals at NewYork-Presbyterian Hospital. We greatly appreciate the efforts of those in so many departments, including pediatrics, emergency medicine, addiction psychiatry, child and adolescent psychiatry, social work, nursing, hospital leadership, and many others, without whom this work could not have been accomplished. We are specifically grateful to Steven Kaplan, MD (NewYork-Presbyterian Hospital) for his mentorship. Dr Kaplan has no conflicts of interest related to the subject of this report.
References (7)

- Drug overdose deaths - health, United States. Centers for Disease Control and Prevention. Accessed January 21, 2022. https://www.cdc.gov/nchs/hus/topics/drug-overdose-deaths.htm
- American Medical Association. Issue brief: nation’s drug-related overdose and death epidemic continues to worsen. Accessed January 21, 2022. https://www.ama-assn.org/system/files/issue-brief-increases-in-opioid-related-overdose.pdf
- Friedman J, Godvin M, Shover CL, et al. Trends in drug overdose deaths among US adolescents, January 2010 to June 2021. JAMA. 2022;327(14):1398–1400. PubMed CrossRef
- Johnston LD, Miech RA, O’Malley PM, et al. Monitoring the future National Survey results on drug use, 1975–2019: overview, key findings on adolescent drug use. ED.gov website. Accessed January 21, 2022. https://eric.ed.gov/?id=ED611736
- Committee on Substance Use and Prevention. Medication-assisted treatment of adolescents with opioid use disorders. Pediatrics. 2016;138(3):e20161893. PubMed CrossRef
- Hadland SE, Wharam JF, Schuster MA, et al. Trends in receipt of buprenorphine and naltrexone for opioid use disorder among adolescents and young adults, 2001–2014. JAMA Pediatr. 2017;171(8):747–755. PubMed CrossRef
- Wesson DR, Ling W. The Clinical Opiate Withdrawal Scale (COWS). J Psychoactive Drugs. 2003;35(2):253–259. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!