Objective: To help clinicians recognize that hypertension, hypertensive urgency, and hypertensive emergency can arise in patients detoxifying from alcohol. Diagnostic and treatment implications are reviewed to help clinicians manage blood pressure in these situations.
Data Sources: PubMed was searched with no restrictions on publication date or study type in June 2019 using the terms (alcohol withdrawal) AND hypertension.
Study Selection: Of 531 studies retrieved, all were reviewed, and articles older than 20 years were excluded. Of the remaining 158 articles, all were reviewed by full-text reading, and 17 were selected based on relevance. Seven UpToDate articles and 2 older papers were also included for relevance.
Data Extraction: Various other searches were also performed; however, no relevant hits resulted when the following terms were entered: (hypertensive urgency/emergency) AND alcohol withdrawal OR detoxification; (hypertensive urgency/emergency) AND (alcohol withdrawal OR detoxification) AND treatment-resistant hypertension.
Results: Hypertension is typically self-limited in alcohol withdrawal syndrome; however, treatment is important to prevent hypertensive urgency or emergency. There is a paucity of data on how best to manage hypertension in patients withdrawing from alcohol, with treatment often individualized. Patients with underlying treatment-resistant hypertension may have more difficult-to-control blood pressure, especially in the first 24 hours of withdrawal.
Conclusions: Multiple medications may be used to treat hypertension in the setting of alcohol withdrawal, with selection based on side effect profile and the patient’s other comorbidities. In patients for whom there is concern for hypertensive urgency versus emergency, full medical evaluation is indicated to identify any potential end-organ damage.

CME Background
Articles are selected for credit designation based on an assessment of the educational needs of CME participants, with the purpose of providing readers with a curriculum of CME articles on a variety of topics throughout each volume. Activities are planned using a process that links identified needs with desired results.
To obtain credit, read the article, correctly answer the questions in the Posttest, and complete the Evaluation. A $10 processing fee will apply.
CME Objective
After studying this article, you should be able to:
‘ ¢Manage hypertension in patients withdrawing from alcohol to prevent hypertensive urgency and emergency
Accreditation Statement
The CME Institute of Physicians Postgraduate Press, Inc., is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians.
Credit Designation
The CME Institute of Physicians Postgraduate Press, Inc., designates this journal-based CME activity for a maximum of 1.0 AMA PRA Category 1 Creditâ„¢. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Note: The American Academy of Physician Assistants (AAPA) accepts certificates of participation for educational activities certified for AMA PRA Category 1 Creditâ„¢ from organizations accredited by ACCME or a recognized state medical society. Physician assistants may receive a maximum of 1.0 hour of Category I credit for completing this program.
Release, Expiration, and Review Dates
This educational activity was published in December 2019 and is eligible for AMA PRA Category 1 Creditâ„¢ through December 31, 2021. The latest review of this material was December 2019.
Financial Disclosure
All individuals in a position to influence the content of this activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past year, Larry Culpepper, MD, MPH, Editor in Chief, has been a consultant for Alkermes, Harmony Biosciences, Merck, Shire, Supernus, and Sunovion. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure appears at the end of the article.
This CME activity is expired. For more CME activities, visit cme.psychiatrist.com.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
ABSTRACT
Objective: To help clinicians recognize that hypertension, hypertensive urgency, and hypertensive emergency can arise in patients detoxifying from alcohol. Diagnostic and treatment implications are reviewed to help clinicians manage blood pressure in these situations.
Data Sources: PubMed was searched with no restrictions on publication date or study type in June 2019 using the terms (alcohol withdrawal) AND hypertension.
Study Selection: Of 531 studies retrieved, all were reviewed, and articles older than 20 years were excluded. Of the remaining 158 articles, all were reviewed by full-text reading, and 17 were selected based on relevance. Seven UpToDate articles and 2 older papers were also included for relevance.
Data Extraction: Various other searches were also performed; however, no relevant hits resulted when the following terms were entered: (hypertensive urgency/emergency) AND alcohol withdrawal OR detoxification; (hypertensive urgency/emergency) AND (alcohol withdrawal OR detoxification) AND treatment-resistant hypertension.
Results: Hypertension is typically self-limited in alcohol withdrawal syndrome; however, treatment is important to prevent hypertensive urgency or emergency. There is a paucity of data on how best to manage hypertension in patients withdrawing from alcohol, with treatment often individualized. Patients with underlying treatment-resistant hypertension may have more difficult-to-control blood pressure, especially in the first 24 hours of withdrawal.
Conclusions: Multiple medications may be used to treat hypertension in the setting of alcohol withdrawal, with selection based on side effect profile and the patient’s other comorbidities. In patients for whom there is concern for hypertensive urgency versus emergency, full medical evaluation is indicated to identify any potential end-organ damage.
Prim Care Companion CNS Disord 2019;21(6):19r02513
To cite: Bojdani E, Chen A, Zhang T, et al. Hypertensive urgency and emergency in alcohol withdrawal: a literature review. Prim Care Companion CNS Disord. 2019;21(6):19r02513.
To share: https://doi.org/10.4088/PCC.19r02513
© Copyright 2019 Physicians Postgraduate Press, Inc.
aHarvard South Shore Psychiatry Residency Training Program, Brockton, Massachusetts
bVA Boston Healthcare System, Brockton, Massachusetts
cDepartment of Psychiatry, Harvard Medical School, Boston, Massachusetts
dBoston University School of Medicine, Boston, Massachusetts
eDepartment of Internal Medicine, University of Maryland Upper Chesapeake Medical Center, Bel Air, Maryland
*Corresponding author: Ermal Bojdani, MD, Harvard South Shore Psychiatry Residency Training Program, 940 Belmont St, Brockton, MA 02301 ([email protected]).
Alcohol withdrawal is a clinical diagnosis and as defined by DSM-51 criteria must include (1) cessation or reduction in heavy and prolonged alcohol use, (2) at least 2 of 8 listed physical or psychiatric symptoms such as nausea/vomiting and anxiety, (3) functional impairment, and (4) signs and symptoms not attributable to any other condition. Symptoms typically begin 6-24 hours after a patient’s last drink and follow a general course. Minor withdrawal, including headache, tremors, and anxiety, occurs 6-36 hours after the last drink. Some patients also experience seizures, hallucinations, and delirium tremens, which is generally termed complicated withdrawal. Seizures, which occur 6-48 hours after the last drink, are present in 10%-30% of patients.2 Alcoholic hallucinosis, which is typically visual but may also include auditory and tactile hallucinations, occurs 12-48 hours after the last drink. Delirium tremens, which is distinguished from alcoholic hallucinosis by unstable vital signs and fluctuating attention and cognition, occurs 72-96 hours after a patient’s last drink and is present in 1%-4% of hospitalized patients experiencing alcohol withdrawal.2
While it is unclear why some people experience greater withdrawal symptoms than others, there is evidence for genetic predisposition.3 A key vital sign often affected in alcohol withdrawal is blood pressure. An elevation in blood pressure can also worsen to the level of hypertensive urgency or emergency. Hypertensive urgency is defined as a blood pressure in the “severe” range (≥ 180/≥ 120 mm Hg) in a patient who is relatively or completely asymptomatic and has no signs or symptoms of acute end-organ damage.4 Hypertensive emergency is present when there is significantly elevated blood pressure with signs or symptoms of acute, ongoing target organ damage.5 Although hypertension arises frequently in patients detoxifying from alcohol, guidance for optimal management is needed given lack of protocols. Here, we review diagnostic and treatment implications to help clinicians manage blood pressure in patients detoxifying from alcohol.
METHODS
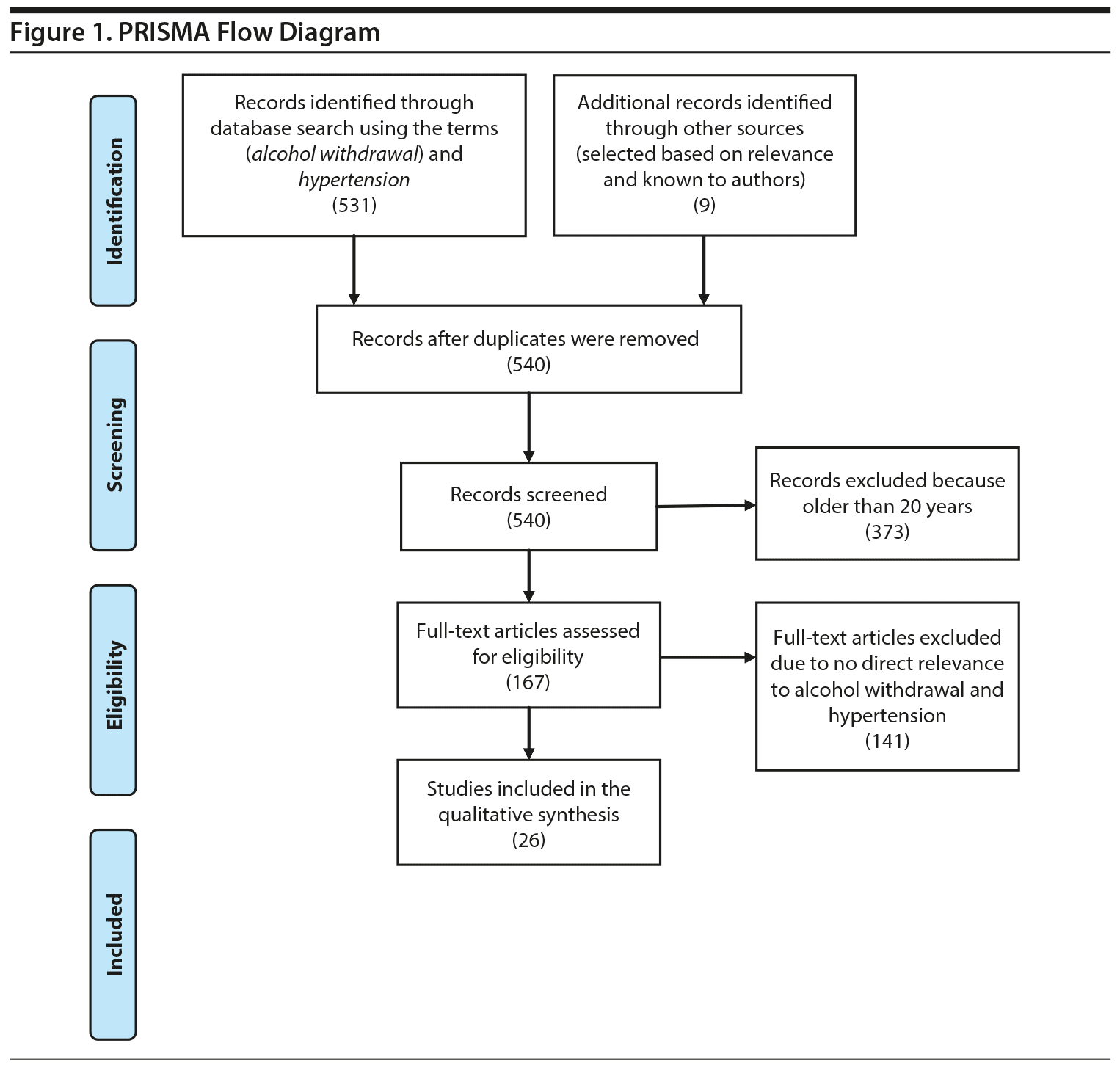
PubMed was searched with no restrictions on publication date or study type in June 2019 using the terms (alcohol withdrawal) AND hypertension. Of 531 studies retrieved, all were reviewed, and articles older than 20 years were excluded. Of the remaining 158 articles, all were reviewed by full-text reading, and some were excluded due to no relevance to alcohol withdrawal and hypertension. Nine additional records were identified through other sources (ie, selected based on relevance and known to the authors). Twenty-six articles2-27were included in the final review: 17 articles3,6-9,12,14–16,20–27 identified in the PubMed search, 7 UpToDate articles,2,4,5,13,17-19 and 2 older articles10,11(Figure 1). Various other searches were performed; however, no relevant hits resulted when the following terms were entered: (hypertensive urgency/emergency) AND alcohol withdrawal OR detoxification; (hypertensive urgency/emergency) AND (alcohol withdrawal OR detoxification) AND treatment-resistant hypertension.
RESULTS
Trajectory and Pathophysiology of Hypertension During Alcohol Withdrawal
One potentially serious manifestation of alcohol withdrawal is hypertension. Those admitted for detoxification often have a blood pressure above 140/90 mm Hg, although it typically normalizes within a few days; this has been demonstrated even in patients with an underlying diagnosis of hypertension. For example, in 1 study6 comparing hypertensive heavy alcohol consumers undergoing withdrawal to those not undergoing withdrawal, blood pressures in the former group were significantly decreased by the third day of withdrawal. Another study7 found significant cardiovascular changes including systolic blood pressure, diastolic blood pressure, heart rate, and total peripheral resistance in the first 3 days of alcohol withdrawal. However, by days 10 and 30 after withdrawal, the parameters had improved and were nearly identical, suggesting the changes were transient and correlated to the alcohol withdrawal period.7 Thus, it appears that hypertension in alcohol withdrawal should improve after the acute withdrawal period. If patients continue to have elevated blood pressure after withdrawal is complete, they may require more comprehensive medical workup and follow-up.7
Various mechanisms contribute to alcohol-induced hypertension, including upregulation of the sympathetic nervous system and aberrations in various factors (superoxide anion, hydrogen peroxide, nitrate/nitrite).6-11 Alcohol consumption can lead to selective vasoconstriction (largely contributed by calcium ions), halting nitric oxide’s effect on the endothelium. On a more chronic trajectory, one can see depletion of magnesium, ATPase downregulation, and disruption in calcium homeostasis.8 Rat models indicate effects on the renal corpuscles and glomeruli6, in addition to implicating angiotensin I and II as mediators of hypertension in the withdrawal phase. Alcohol consumption and withdrawal may worsen baseline resistant hypertension and can lead to a hypertensive urgency or emergency.12
Treatment of Alcohol Withdrawal to Prevent Hypertensive Urgency
Management of alcohol withdrawal includes treatment with benzodiazepines or other drugs (Table 1), correction of metabolic abnormalities, and determination of level of care (ie, psychiatric facility vs medical floor vs intensive care unit [ICU]). The Clinical Institute Withdrawal Assessment for Alcohol-Revised (CIWA-Ar)28 is commonly used for patients who can tolerate medications by mouth and provides a dosing scale for benzodiazepines based on symptoms. In those with severe liver disease, use of lorazepam or oxazepam is preferred over diazepam or chlordiazepoxide due to decreased hepatotoxic metabolites. For patients in severe withdrawal who require tracheal intubation and mechanical ventilation, other scales may be used including the Richmond Agitation-Sedation Scale29 to target appropriate level of sedation. For such patients, ICU level of care is often required. In those with refractory delirium tremens, phenobarbital or propofol is often considered as additional or alternate treatment.13 To help predict complicated withdrawal symptoms, the Prediction of Alcohol Withdrawal Severity Scale30 can be used. This 10-question scale was studied in medically ill, hospitalized patients to identify those at risk for complicated withdrawal and is currently the best predictor for clinically significant withdrawal.14
Risk Factors for Hypertensive Urgency During Alcohol Withdrawal
Patients abusing alcohol or detoxifying from alcohol can experience blood pressure and other vital sign derangements on a spectrum, and they tend to present to an outpatient doctor’s office or the emergency department to initiate care. Mild withdrawal symptoms may be managed on an outpatient basis; however, for those with more severe symptoms, treatment in an inpatient setting is preferred.15 Tachycardia (heartbeat > 100-120 bpm) and hypertension with systolic blood pressure > 145 mm Hg may represent potential risk factors or predictors of a more complicated course.16
Resistant hypertension, lifestyle factors, and medication noncompliance can also increase risk for hypertensive urgency. Resistant hypertension is defined as blood pressure that remains above goal despite concurrent use of 3 antihypertensives of different classes (with 1 a diuretic, and all prescribed at maximally tolerated or recommended doses) or blood pressure that is controlled with ≥ 4 medications. Risk factors include older age, African-American ethnicity, and diabetes.17 High salt diet, physical inactivity, and severe alcohol abuse also contribute to hypertension. Additionally, noncompliance with part or all of an antihypertensive regimen could increase risk for hypertensive urgency.18
Diagnostic Assessment and Treatment Considerations for Hypertensive Urgency
As mentioned previously, hypertensive urgency is defined as a blood pressure in the severe range (≥ 180/≥ 120 mm Hg) in a patient who is relatively or completely asymptomatic and has no signs or symptoms of acute end-organ damage.4 The optimal management of such patients is unclear, even more so when factors such as alcohol withdrawal complicate the picture. In patients detoxifying from alcohol who experience new-onset hypertension or elevation in blood pressure above their baseline but not in the severe range, general practice is to treat the alcohol withdrawal, often with a benzodiazepine, which in turn tends to lower the blood pressure. When there is no significant response to the benzodiazepine or when hypertensive urgency is reached, antihypertensives are often considered as part of acute treatment. On the basis of the articles reviewed, to date, there is no consensus or official guidance on which antihypertensive to use in alcohol withdrawal or how to use it. With respect to hypertensive urgency regardless of cause, a general goal is to reduce the blood pressure over a period of hours to days, with a target blood pressure of < 160/< 100 mm Hg, with no lowering by more than 25%-30% over the first 3 hours.4 Data to provide guidance on how best to do this are lacking; the approach is often individualized based on the patient and the physician. To lower blood pressure over a period of hours, oral clonidine (0.1 mg to 0.2 mg) or oral captopril (6.2 5 mg or 12.5 mg if the patient is not volume overloaded) is used, with an expected reduction in blood pressure of 20-30 mm Hg. Longer-acting drugs like amlodipine are considered thereafter.4 If the patient’s history of medication nonadherence is clear, resumption of one’s routine medications may be sufficient, although this may not be enough. If the doses of existing antihypertensives have not been fully optimized, one may consider increasing the dose. Data are also lacking in terms of recommendations for which agent to use to lower blood pressure over several days; calcium channel blockers (but not sublingual nifedipine), angiotensin receptor blockers, or β-blockers are often used. To exclude acute end-organ damage and hypertensive emergency, laboratory testing is required.4
Initial Treatment Escalation
Blood pressure derangements in alcohol withdrawal can also present as a hypertensive emergency. Hypertensive emergency describes a significantly elevated blood pressure with signs or symptoms of acute, ongoing target organ damage. For most of these cases, mean arterial pressure should be reduced by approximately 15% in the first hour, and then gradually over the next 23 hours, to reach a final pressure that is reduced by 25% compared to baseline.5 As data are lacking regarding superiority of one agent over another, parenteral and oral antihypertensive choice is often dictated by type of hypertensive emergency, local hospital formulary, and physician preference.5 Additionally, there is a paucity of data in the literature regarding the management of alcohol-related hypertensive emergency, and we were unable to find any guidance during our search. Given concern that an excessive hypotensive response could lead to ischemic complications, in those who are asymptomatic, slower reductions in blood pressure may be achieved with one of the oral agents described previously, such as clonidine. Parenteral drugs include sodium nitroprusside (provides nitric oxide that induces vasodilation, is given intravenously starting at 0.25 mcg/kg per minute with effect seen within 1 minute or less, increases risk of nitroprusside-induced cyanide poisoning with prolonged treatment), nitroglycerin, calcium channel blockers (such as clevidipine in select patients), labetalol, or hydralazine.19 Given that each medication has its own side effect profile, caution should be used when choosing an agent in select patients.
Experimental Treatment
Additional medications that may be considered, but are not the standard of care, include ketamine, dexmedetomidine, and cytoflavin. In a retrospective analysis of 30 patients,20 ketamine was initiated 41.4 hours after a lorazepam infusion, and all patients achieved initial symptom control (tachycardia, hypertension, diaphoresis, agitation, tremor, hallucinations, seizures, and progression of delirium tremens) within 1 hour of ketamine infusion. Two patients experienced hypertension and tachycardia due to ketamine use. The data suggest the potential benefit of adjunctive use of ketamine in providing improved symptom control for patients refractory to benzodiazepines and in potentially reducing lorazepam requirements.20 There is also some evidence for dexmedetomidine, an α-2-agonist, for refractory delirium tremens and other symptoms.9
In a retrospective study21 of 20 ICU patients treated with dexmedetomidine for alcohol withdrawal, results showed concomitant administration of dexmedetomidine reduced the amount of total benzodiazepines needed and provided for a smoother detox, with a likely more benign effect on the respiratory system.22 Moreover, a review article23 consisting of 1 randomized controlled trial, 1 prospective observational study, and 6 retrospective reviews of efficacy and safety of dexmedetomidine in alcohol withdrawal concluded that it reduces hypertension and tachycardia in alcohol withdrawal syndrome and reduces benzodiazepine requirements. However, there was no evidence that dexmedetomidine improved clinical endpoints such as need for mechanical ventilation, ICU level of care, or length of hospital stay.23
Finally, in a study24 in which 30 alcohol withdrawal patients were given cytoflavin and 30 were given placebo, cytoflavin was shown to be safe and efficient in the treatment of alcohol detoxification, as evidenced by objective vital signs, reduced subjective somatic symptoms, and CIWA-Ar scores.
Post Withdrawal Management
Post withdrawal, a fraction of patients will continue to have elevated blood pressure that may or may not be related to alcohol use; these patients are encouraged to follow up with their outpatient primary care doctor. Adherence to a low-salt diet and abstinence from alcohol consumption may lead to improved blood pressure management as well as an overall better quality of life. A systematic review25 of 63 studies showed that interventions aimed at alcohol reduction were beneficial at reducing alcohol-related injuries, recovering ventricular heart function in alcoholic cardiomyopathy, lowering blood pressure, reducing weight, and slowing progression of liver fibrosis due to alcohol. Benefits of alcohol abstinence were also shown in a study of 42 male heavy drinkers who had 1 month of alcohol cessation. Abstinence produced a decrease in average systolic blood pressure of 7.2 mm Hg, in diastolic blood pressure of 6.6 mm Hg, and in heart rate of 7.9 bpm. Alcohol cessation has been shown to be an integral part of blood pressure control in patients with alcohol use disorder.26,27
Limitations

- Data are lacking and more research is needed on how best to manage hypertension in alcohol withdrawal syndrome.
- Benzodiazepines and the alpha2-adrenergic agonist clonidine are helpful for the management of hypertension in patients detoxifying from alcohol.
- Abstinence from alcohol can lead to improved blood pressure in patients with hypertension.
The study was retrospective in nature and includes guidance from more recent publications, given general exclusion of articles older than 20 years. Additionally, although all types of available studies are included in the review, there is unfortunately a paucity of data from randomized controlled clinical trials on this topic.
DISCUSSION
Abnormalities in vital signs, especially blood pressure, are commonly seen in patients detoxifying from alcohol. The degree of these derangements is often dependent on various factors, including genetics and extent of drinking (including time and severity). Guidance on how to best manage hypertension, hypertensive urgency, and hypertensive emergency in patients withdrawing from alcohol is lacking. Here, we provide a review of relevant articles to start the discussion about this important topic. Despite lack of specific guidance, what is clear is that every effort should be made to control blood pressure during the withdrawal period. Hypertension is typically self-limited in alcohol withdrawal syndrome. However, patients with underlying treatment-resistant hypertension may have more difficult-to-control blood pressure, especially in the first 24 hours of withdrawal. Benzodiazepines and the alpha2-adrenergic agonist clonidine are helpful for the management of hypertension in patients detoxifying from alcohol. Post withdrawal, patients with persistent hypertension are encouraged to follow up with a primary care provider and consider alcohol abstinence for improved blood pressure and an overall better quality of life.
Submitted: July 12, 2019; accepted September 24, 2019.
Published online: December 12, 2019.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, cytoflavin, dexmedetomidine, and ketamine are not approved by the US Food and Drug Administration for the treatment of hypertension in alcohol withdrawal.
Financial disclosure: Drs Bojdani, Chen, Naqvi, and Tahera and Ms Zhang have no personal affiliations or financial relationships with any commercial interest to disclose relative to this article.
Funding/support: None.
REFERENCES
1.American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
2.Pace C. Alcohol withdrawal: epidemiology, clinical manifestations, course, assessment, and diagnosis. UpToDate website. https://www.uptodate.com/contents/alcohol-withdrawal-epidemiology-clinical-manifestations-course-assessment-and-diagnosis?search=ALCOhol%20withdrawal&source=search_result&selectedTitle=2~150&usage_type=default&display_rank=2. Accessed February 23, 2019.
3.Grzywacz A, Jasiewicz A, Małecka I, et al. Influence of DRD2 and ANKK1 polymorphisms on the manifestation of withdrawal syndrome symptoms in alcohol addiction. Pharmacol Rep. 2012;64(5):1126-1134. PubMed CrossRef
4.Varon J. Management of severe asymptomatic hypertension (hypertensive urgencies) in adults. UpToDate website. https://www.uptodate.com/contents/management-of-severe-asymptomatic-hypertension-hypertensive-urgencies-in-adults?search=hypertensive%20urgency&source=search_result&selectedTitle=1~42&usage_type=default&display_rank=1. Accessed February 23, 2019.
5.Elliott WJ, Varon J. Evaluation and treatment of hypertensive emergencies in adults. UpToDate website. https://www.uptodate.com/contents/evaluation-and-treatment-of-hypertensive-emergencies-in-adults?search=evaluation-and-treatment-of-hypertensive-emergencies-in&source=search_result&selectedTitle=1~150&usage_type=default&display_rank=1. Accessed February 23, 2019.
6.Soardo G, Donnini D, Varutti R, et al. Effects of alcohol withdrawal on blood pressure in hypertensive heavy drinkers. J Hypertens. 2006;24(8):1493-1498. PubMed CrossRef
7.Kähkönen S, Zvartau E, Lipsanen J, et al. Effects of alcohol withdrawal on cardiovascular system. Prog Neuropsychopharmacol Biol Psychiatry. 2011;35(2):550-553. PubMed CrossRef
8.Wakabayashi I, Hatake K. Effects of ethanol on the nervous and vascular systems: the mechanisms of alcohol-induced hypertension. Nihon Eiseigaku Zasshi. 2001;55(4):607-617. PubMed CrossRef
9.Gonzaga NA, do Vale GT, Parente JM, et al. Ethanol withdrawal increases blood pressure and vascular oxidative stress: a role for angiotensin type 1 receptors. J Am Soc Hypertens. 2018;12(7):561-573. PubMed CrossRef
10.Hawley RJ, Nemeroff CB, Bissette G, et al. Neurochemical correlates of sympathetic activation during severe alcohol withdrawal. Alcohol Clin Exp Res. 1994;18(6):1312-1316. PubMed CrossRef
11.Littleton J. New medical review series—4, alcohol intoxication and physical dependence: a molecular mystery tour. Br J Addict. 1989;84(3):267-276. PubMed CrossRef
12.Ceccanti M, Sasso GF, Nocente R, et al. Hypertension in early alcohol withdrawal in chronic alcoholics. Alcohol Alcohol. 2006;41(1):5-10. PubMed CrossRef
13.Hoffman RS, Weinhouse GL. Management of moderate and severe alcohol withdrawal syndromes. UpToDate website. https://www.uptodate.com/contents/management-of-moderate-and-severe-alcohol-withdrawalsyndromes?search=ALCOhol%20withdrawal&source=search_result&selectedTitle=1~150&usage_type=default&display_rank=1. Accessed February 23, 2019.
14.Tolonen J, Rossinen J, Alho H, et al. Dexmedetomidine in addition to benzodiazepine-based sedation in patients with alcohol withdrawal delirium. Eur J Emerg Med. 2013;20(6):425-427. PubMed CrossRef
15.Muncie HL Jr, Yasinian Y, Oge’ L. Outpatient management of alcohol withdrawal syndrome. Am Fam Physician. 2013;88(9):589-595. PubMed
16.Mainerova B, Prasko J, Latalova K, et al. Alcohol withdrawal delirium: diagnosis, course and treatment. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub. 2015;159(1):44-52. PubMed CrossRef
17.Calhoun DA, Townsend RR. Definition, risk factors, and evaluation of resistant hypertension. UpToDate website. https://www.uptodate.com/contents/definition-risk-factors-and-evaluation-of-resistant-hypertension?search=resistant%20hypertension&source=search_result&selectedTitle=1~146&usage_type=default&display_rank=1. Accessed February 23, 2019.
18.Calhoun DA, Townsend RR. Treatment of resistant hypertension. UpToDate website. https://www.uptodate.com/contents/treatment-of-resistant-hypertension?search=resistant%20hypertension&source=search_result&selectedTitle=2~146&usage_type=default&display_rank=2. Accessed February 23, 2019.
19.Elliott WJ, Varon J. Drugs used for the treatment of hypertensive emergencies. UpToDate website. https://www.uptodate.com/contents/drugs-used-for-the-treatment-of-hypertensive-emergencies?search=hypertensive%20emergency&source=search_result&selectedTitle=3~150&usage_type=default&display_rank=3. Accessed February 23, 2019.
20.Shah P, McDowell M, Ebisu R, et al. Adjunctive use of ketamine for benzodiazephine-resistant severe alcohol withdrawal: a retrospective evaluation. J Med Toxicol. 2018;14(3):229-236. PubMed CrossRef
21.Rayner SG, Weinert CR, Peng H, et al; Study Institution. Dexmedetomidine as adjunct treatment for severe alcohol withdrawal in the ICU. Ann Intensive Care. 2012;2(1):12. PubMed CrossRef
22.Maccioli GA. Dexmedetomidine to facilitate drug withdrawal. Anesthesiology. 2003;98(2):575-577. PubMed CrossRef
23.Linn DD, Loeser KC. Dexmedetomidine for alcohol withdrawal syndrome. Ann Pharmacother. 2015;49(12):1336-1342. PubMed CrossRef
24.Minko AI, LinskiÄ IV, Kuz’ minov VN, et al. Cytoflavin in the detoxification of alcohol-dependent patients. Zh Nevrol Psikhiatr Im S S Korsakova. 2013;113(6):35-40. PubMed
25.Charlet K, Heinz A. Harm reduction: a systematic review on effects of alcohol reduction on physical and mental symptoms. Addict Biol. 2017;22(5):1119-1159. PubMed CrossRef
26.Aguilera MT, de la Sierra A, Coca A, et al. Effect of alcohol abstinence on blood pressure: assessment by 24-hour ambulatory blood pressure monitoring. Hypertension. 1999;33(2):653-657. PubMed CrossRef
27.Leal S, Ricardo Jorge DO, Joana B, et al. Heavy alcohol consumption effects on blood pressure and on kidney structure persist-after long term withdrawal. Kidney Blood Press Res. 2017;42(4):664-675. PubMed CrossRef
28.Sullivan JT, Sykora K, Schneiderman J, et al. Assessment of alcohol withdrawal: the revised clinical institute withdrawal assessment for alcohol scale (CIWA-Ar). Br J Addict. 1989;84(11):1353-1357. PubMed CrossRef
29.Sessler CN, Gosnell MS, Grap MJ, et al. The Richmond Agitation-Sedation Scale: validity and reliability in adult intensive care unit patients. Am J Respir Crit Care Med. 2002;166(10):1338-1344. PubMed CrossRef
30.Maldonado JR, Sher Y, Das S, et al. Prospective Validation Study of the Prediction of Alcohol Withdrawal Severity Scale (PAWSS) in Medically Ill Inpatients: a new scale for the prediction of complicated alcohol withdrawal syndrome. Alcohol Alcohol. 2015;50(5):509-518. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!