Objective: Polypharmacy is common and especially challenging in the context of borderline personality disorder in light of impulsivity and self-harm associated with the disorder, risk of adverse drug-drug interactions, and financial burden. Reduction in polypharmacy could be conceptualized as a high priority in the treatment of borderline personality disorder. This case aims to demonstrate that potential.
Method: This case report presents outcomes data for an individual with borderline personality disorder during the course of an extended psychiatric hospitalization. Symptomatic change is based on the Patient Health Questionnaire Somatic, Anxiety, and Depression Symptoms scales and World Health Organization 5-Item Well-Being Index. Change in polypharmacy is presented both in terms of absolute number and complexity of the medication regimen. Clinical outcomes data are provided at 2, 12, and 24 weeks postdischarge.
Results: During a 56-day hospitalization, the patient demonstrated clinical improvement across clinical domains—all occurred within the context of reduced number (43%) and complexity (40%) of her medication regimen. Symptomatic improvement was sustained up to 6 months postdischarge.
Conclusions: Despite good intentions, polypharmacy can be associated with iatrogenic harm and contribute to functional impairment, especially in the context of borderline personality disorder, in which symptomatic fluctuations are part of the illness itself. A reduction in the patient’s high-risk polypharmacy during treatment represents a noteworthy treatment outcome in and of itself. Additional measures of medication risk and liability have the potential to become markers of clinical effectiveness.

Reducing Adverse Polypharmacy in Patients With Borderline Personality Disorder:
An Empirical Case Study
ABSTRACT
Objective: Polypharmacy is common and especially challenging in the context of borderline personality disorder in light of impulsivity and self-harm associated with the disorder, risk of adverse drug-drug interactions, and financial burden. Reduction in polypharmacy could be conceptualized as a high priority in the treatment of borderline personality disorder. This case aims to demonstrate that potential.
Method: This case report presents outcomes data for an individual with borderline personality disorder during the course of an extended psychiatric hospitalization. Symptomatic change is based on the Patient Health Questionnaire Somatic, Anxiety, and Depression Symptoms scales and World Health Organization 5-Item Well-Being Index. Change in polypharmacy is presented both in terms of absolute number and complexity of the medication regimen. Clinical outcomes data are provided at 2, 12, and 24 weeks postdischarge.
Results: During a 56-day hospitalization, the patient demonstrated clinical improvement across clinical domains—all occurred within the context of reduced number (43%) and complexity (40%) of her medication regimen. Symptomatic improvement was sustained up to 6 months postdischarge.
Conclusions: Despite good intentions, polypharmacy can be associated with iatrogenic harm and contribute to functional impairment, especially in the context of borderline personality disorder, in which symptomatic fluctuations are part of the illness itself. A reduction in the patient’s high-risk polypharmacy during treatment represents a noteworthy treatment outcome in and of itself. Additional measures of medication risk and liability have the potential to become markers of clinical effectiveness.
Prim Care Companion CNS Disord 2015;17(4):doi:10.4088/PCC.14m01760
© Copyright 2015 Physicians Postgraduate Press, Inc.
Submitted: December 8, 2014; accepted March 10, 2015.
Published online: July 30, 2015.
Corresponding author: Alok Madan, PhD, MPH, The Menninger Clinic, 12301 S Main St, Houston, TX 77035 ([email protected]).
The use of multiple medications to treat a single patient—polypharmacy—is common, especially among psychiatric patients1 and patients with borderline personality disorder in particular,2 and has seen a marked increase in recent decades.3 The prescription of multiple psychoactive agents in the name of clinical effectiveness comes at the expense of pharmaceutical parsimony and patient safety. The common practice of prescribing multiple antipsychotic medications is a prime example—especially among individuals with borderline personality disorder and comorbid schizoaffective disorder, bipolar disorder, and/or posttraumatic stress disorder. There is a growing literature highlighting the significant adverse consequences associated with combining multiple antipsychotics.4 This research base is the rationale for 1 of the recently introduced Hospital-Based Inpatient Psychiatric Services core measures, by which The Joint Commission and the Centers for Medicaid and Medicare Services rate the quality of inpatient psychiatric hospitals and reimburse services in the United States.5 Specifically, inpatient psychiatric facilities will be asked to make publicly available data related to the proportion of discharged patients who were prescribed multiple antipsychotic medications with and without appropriate justification.5
Psychiatric polypharmacy is especially challenging in the context of borderline personality disorder in light of impulsivity and self-harm associated with the disorder, risk of adverse drug-drug interactions, and financial burden. There is international consensus that psychopharmacologic agents should be used as adjunctive treatment for specific symptoms and/or as treatment for comorbid psychiatric conditions6-9; 1 of a number of psychotherapies should be the front-line treatment.10 Despite these guidelines, psychiatric polypharmacy in this population is common11 and is a significant safety concern. Further, polypharmacy in general is associated with increased risk of adverse drug-drug interactions, adverse drug-gene interactions, and significant financial burden to the individual and society.12
With this case report, we highlight the use of polypharmacy in the context of a complex clinical presentation and the reduction in absolute number and complexity of a medication regimen after an extended hospitalization with sustained symptomatic benefit 6 months following discharge.
CLINICAL PRESENTATION
Ms A is a middle-aged entrepreneur who presented for an extended psychiatric hospitalization with long-standing psychiatric and polypharmacy histories. Her psychiatric difficulties began at age 4, when her pediatrician prescribed amphetamines due to hyperactivity. She described feeling suicidal since age 12, and at age 19, she attempted suicide, for which she was acutely hospitalized. At admission, Ms A reported experiencing chronic suicidal ideation with nonsuicidal self-injury (≥ 20 incidents over her lifetime). She also detailed a history of impulsive and potentially dangerous behaviors, including sexual intercourse in public places, excessive spending (lifetime), and several risky business decisions that resulted in significant financial loss (within the year preceding this hospitalization). Her history was marked by affective instability and mood reactivity (hypomanic symptoms and dysphoria lasting for a few hours), chronic feelings of emptiness, desperate attempts to avoid abandonment, and difficulty controlling anger (physical altercations with her husband when he tried to leave her). Of note, Ms A detailed a history of disordered eating beginning during her husband’s protracted illness, including binges and associated weight gain. She reported last bingeing in the month preceding the index hospitalization.

- Despite good intentions, polypharmacy is common and especially challenging in the context of borderline personality disorder in light of impulsivity and self-harm associated with the disorder, risk of adverse drug-drug interactions, and financial burden.
- A reduction in patients’ high-risk polypharmacy during treatment represents a noteworthy treatment outcome in and of itself and might be conceptualized as a marker of clinical effectiveness.
Interpersonally, Ms A was born the youngest of 3 children and raised in an affluent community. Her father died when she was a young child; her mother remarried 3 times. For the most part, she was raised by a nanny, with whom she remained close. Shortly after college, Ms A married. Her husband unexpectedly died when she was in her early 30s. She has had only 1 significant relationship since that time. She has no children and limited interpersonal relations outside of her immediate family and nanny. During her 30s, Ms A was vocationally successful, working in the banking and real estate industries, but experienced a significant decline in functioning in the year preceding her hospitalization. She reportedly had been engaged in mental health treatment since her mid-20s, with 4 different therapists and 3 psychiatrists. She recently began seeing a new therapist after her therapist of 6 years terminated treatment due to her level of suicidality. Ms A presented for inpatient treatment in the context of worsening depression, persistent suicidal ideation, functional decline, and significant financial distress.
As part of standard of care, Ms A completed a comprehensive, empirically based assessment at admission, every 2 weeks during her hospitalization, at discharge, and at scheduled intervals following her hospitalization (2, 12, and 24 weeks). At admission, she completed the Structured Interview for DSM-IV-TR Axis I Disorders13 (SCID-I) and the Structured Interview for DSM-IV Axis II Personality Disorders14 (SCID-II). She received SCID-I-confirmed diagnoses of bipolar disorder not otherwise specified and eating disorder not otherwise specified, as well as a SCID-II-confirmed diagnosis of borderline personality disorder (meeting 6 criteria). Using research-based and objective measures to obtain psychiatric diagnoses allowed for confidence in the accuracy of appropriately diagnosing underlying psychopathology, especially in the context of comorbid bipolar disorder and borderline personality disorder, for which the differential diagnosis can be difficult.
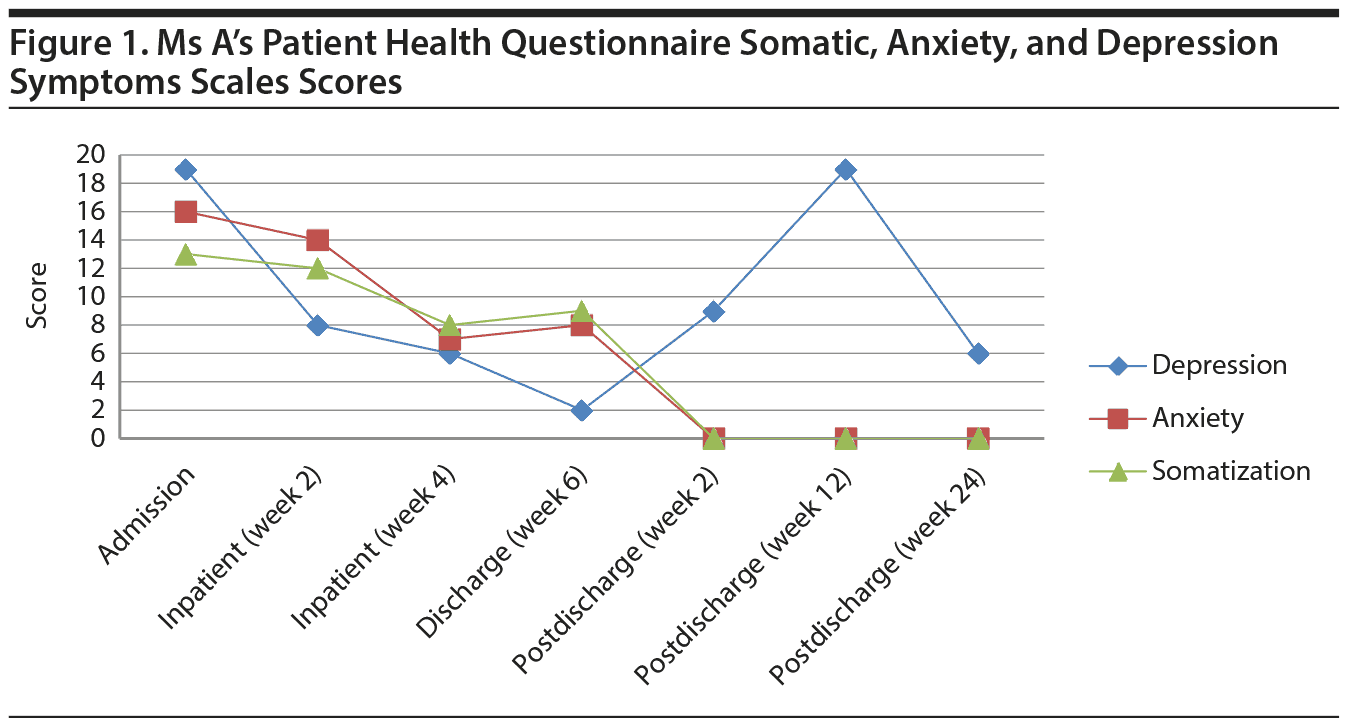
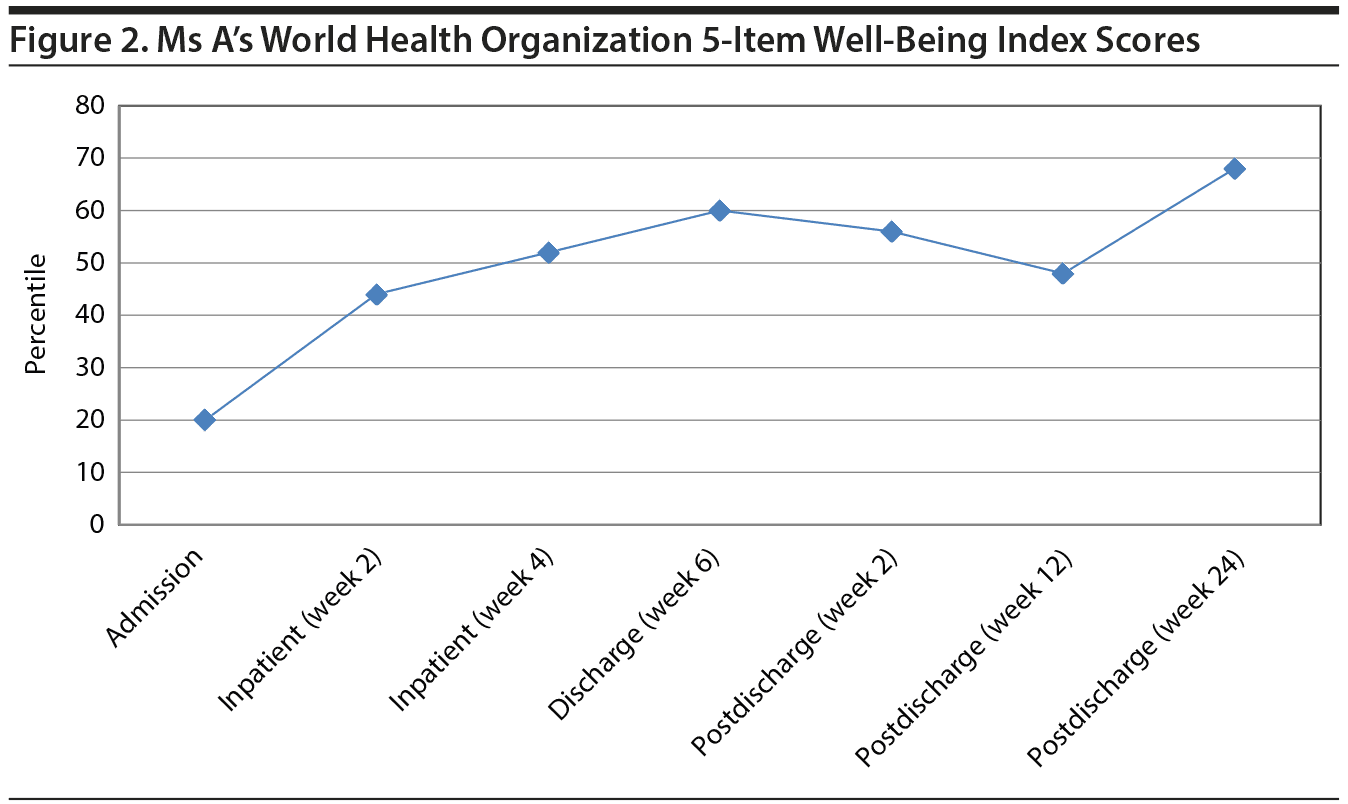
In line with recommended measures for use in borderline personality disorder outcomes research,15 Ms A also completed measures of symptomatic functioning and general well-being, including the Patient Health Questionnaire (PHQ) Somatic, Anxiety and Depressive Symptoms scales16 (PHQ-15, 7-item Generalized Anxiety Disorder scale [GAD-7], and PHQ-9, respectively). She presented with moderately severe depression (PHQ-9 score = 19, severe range ≥ 20), severe anxiety (GAD-7 score = 16, severe range ≥ 15), and medium levels of somatization (PHQ-15 score = 13, high somatization ≥ 15) (Figure 1). Medically, Ms A evidenced significant somnolence, poor diabetic control, and self-described questionable medication compliance and poor eating habits; she reported a life-long history of irritable bowel syndrome. Laboratory tests revealed elevated blood glucose, liver function tests, thyroid-stimulating hormone, and prolactin levels. Overall, she presented with poor general well-being, as assessed using the World Health Organization 5-Item Well-Being Index17 (WHO-5 score = 20th percentile, Figure 2).
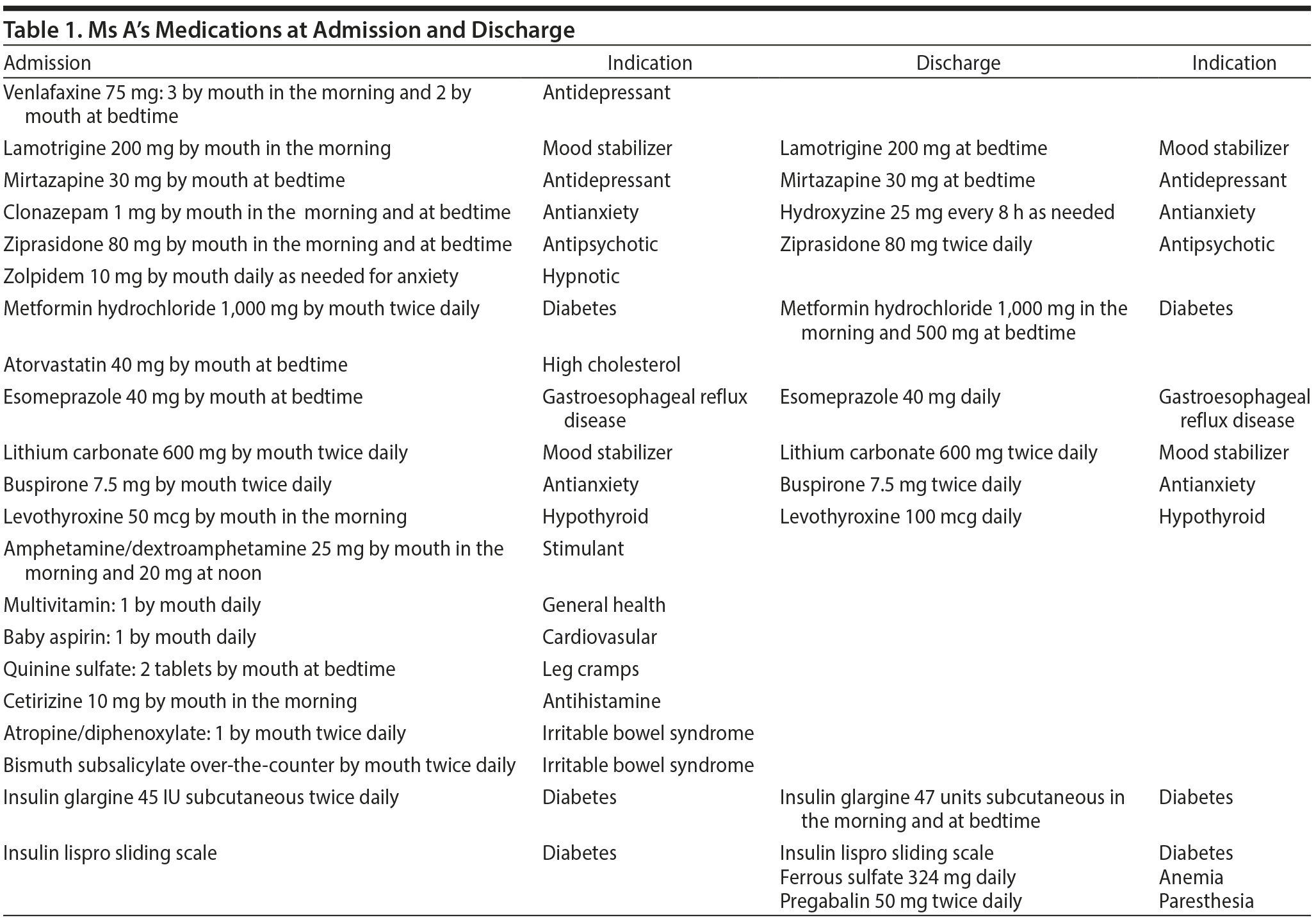
Ms A’s admission medications included lithium, venlafaxine, lamotrigine, mirtazapine, clonazepam, ziprasidone, zolpidem, buspirone, d-/l-amphetamine, metformin, insulin, atorvastatin calcium, levothyroxine, esomeprazole magnesium, and diphenoxylate/atropine. Though she struggled to recall details of her pharmacologic history, Ms A reported being prescribed increasing numbers of antidepressants and mood stabilizers over the last decade as her depression and suicidal ideation worsened—medications were added each time she had a complaint; however, ineffective agents were rarely, if ever, discontinued. Table 1 provides a listing of her medications, dosing, and indications at admission.
TREATMENT AND PROGRESS
In light of significant suicidal ideation at admission, treatment initially focused on developing a working alliance that included a safety plan to turn to staff and peers in times of distress, with a focus on improving emotion regulation and exploring and understanding the factors that contributed to her deterioration and hospitalization. During her hospitalization, Ms A’s treatment included (1) twice-weekly rounds/medication management meetings with as-needed contacts to reduce adverse polypharmacy with a psychiatrist, (2) twice-weekly individual cognitive-behavioral therapy with a psychologist, (3) once-weekly family therapy via phone conference with a social worker, (4) 2-4 sessions of rehabilitation therapy groups (eg, readiness to change, barriers to change, dialectical behavior therapy skills), (5) milieu therapy, and (6) 24-hour nursing care. In sum, though she was not prescribed a manualized, borderline personality disorder-specific psychotherapy protocol, the eclectic combination of supportive-expressive therapy, cognitive-behavioral therapy, and dialectical behavior therapy techniques all within a therapeutic milieu and 24-hour nursing support allowed for greater recognition and acceptance of emotional distress and learning skills to better manage emotional regulation capacities. Additional details are outside the scope of this case discussion.
Initially, Ms A was fearful and expressed outrage at the idea of discontinuing medications. Several sessions were spent discussing her fears and sharing the diagnostic concerns and the risks to her health. She reluctantly agreed to a gradual taper when assured that staff was monitoring her physical and psychiatric symptoms and was willing to negotiate if she experienced an exacerbation of symptoms.
Systematic taper of multiple medications to reduce adverse polypharmacy was instituted because Ms A was overly sedated (slurring of speech, unsteady gate, and concerns of adequate diabetic control). Sedating medications (clonazepam, zolpidem) and stimulants (amphetamine/dextroamphetamine) were reduced given her self-reported noncompliance, significant somnolence, and suicide-related behaviors. There were no signs of withdrawal, anxiety, problems with concentration, or problems with insomnia with these changes. With a presumed diagnosis of bipolar disorder not otherwise specified, Ms A was subsequently tapered off venlafaxine with no ill effect. Little change was made to the mood stabilizers. As medications were tapered, staff interventions focused on effective emotion regulation management and health-promoting exercise and diet to better manage chronic medical conditions. Ms A eventually came to appreciate clearer thinking and improved functioning without anxiolytics and stimulants. In fact, she requested additional decreases in her medication regimen. With improving physical health status, she was better able to appreciate her tendency to express emotional distress as somatic complaints. Over time, she developed more effective coping strategies including turning to others during times of distress. These behaviors were reinforced in individual, group, and family therapy sessions.
Some psychiatric symptoms were exacerbated by her poor physical health, and her poor health status impacted the severity of psychiatric distress. During the course of her hospitalization, Ms A’s insulin was increased (see Table 1), and she met weekly with a dietitian to learn and implement improved eating behaviors. Work with the dietitian also addressed a history of disordered eating, which greatly impacted her diabetes. Her fasting glucose levels improved, and by discharge, she had lost 10 lb. She was able to demonstrate better portion control, carbohydrate counting, and no binge-eating behavior. Of note, her poor diabetic control was thought to be contributing to paresthesias, for which she was prescribed pregabalin.
An undersuppressed thyroid was thought to contribute to Ms A’s lethargy, so her levothyroxine dose was increased. A relative iron deficiency anemia also may have caused lethargy and was addressed with iron supplementation. Her liver function tests returned to normal levels with discontinuation of atorvastatin calcium. The importance of dietary compliance and exercise were reinforced throughout her treatment. Ms A presented with a history of irritable bowel syndrome and regular use of diphenoxylate/atropine. It became clear throughout treatment that her gastrointestinal symptoms seemed to correlate with her interpersonal distress. As she progressed in treatment, her symptoms decreased, and diphenoxylate/atropine was no longer utilized.
Several elements of the plan were not implemented due to time limitations. At discharge, it was recommended that Ms A’s next level of care provider consider tapering lamotrigine, discontinuing buspirone (prior tapers resulted in increased gastrointestinal distress), and tapering hydroxyzine hydrochloride (which was added as an as-needed agent for periodic spikes in anxiety).
RESULTS
During the course of her 56-day hospitalization, Ms A tolerated the taper in her pharmacologic regimen from admission (no. = 21) to discharge (no. = 12), representing a 43% reduction in absolute medication burden. The reduction in the complexity of her medication regimen (Medication Regimen Complexity Index score18 [MRCI]) was just as dramatic from admission (MRCI = 46) to discharge (MRCI = 27.5), representing a 40% decrease in complexity. Reduced polypharmacy occurred within the context of symptomatic improvement, including reduced depressive and anxious and somatic complaints, as well as improved general well-being at discharge. Of note, Ms A was able to maintain these treatment gains up to 24 weeks after her hospitalization, though not without spikes in depressive symptoms at 2 weeks and 12 weeks posthospitalization (see Figures 1 and 2).
DISCUSSION
Ms A’s case is an all-too-common consequence of 15 to 30-minute outpatient medication checks and 3 to 5-day hospital stays, especially among individuals with borderline personality disorder. This cycle often perpetuates with subsequent brief hospitalizations, during which multiple medications are again added and further multiplied when the patient resumes outpatient care. Ms A presented to the hospital in acute psychiatric crisis with an extensive medication regimen that was of limited benefit. Over the years, she most likely was prescribed a different medication to treat each and every symptom that she experienced. This pattern of prescribing is a common occurrence in the context of borderline personality disorder in which a large range of fluctuating symptoms is a common clinical course. While additions were routinely made to Ms A’s medication list, few appear to have been discontinued. Drugs very likely were initiated over time to counteract the side effects of other drugs, such as adding sedatives/hypnotics when there is also stimulant use.
Polypharmacy also very likely contributes to reduced sense of efficacy in patients with borderline personality disorder, constituting further iatrogenic harm in light of the fact that 1 of the goals of first-line psychotherapeutic treatment frequently includes efforts to increase patients’ self-responsibility and self-efficacy. Together, a reduction in polypharmacy could be conceptualized as a high priority in the treatment of borderline personality disorder, though relatively few intervention trials include this construct in demonstrations of clinical effectiveness.19 Perhaps 1 of the reasons that few have embraced the potential merits of reduction in polypharmacy as a treatment outcome may be the consequence of the variable definitions of polypharmacy and methods of quantifying it.1 There is a need for measures that quantify more than just reduction in absolute number or complexity of a medication regimen, such as measures that capture the reduction in potential harm/risk associated with a changed medication regimen.
Of note, improved medical management most likely contributed to an improvement in many of Ms A’s psychiatric/somatic complaints, reducing the need for inappropriately prescribed psychotropic medications, which have little efficacy or utility. For example, she evidenced considerably improved diabetic control via changes to and compliance with her medications and diet and exercise regimens (including a 10-lb weight loss by discharge), as well as better control of her thyroid functioning. Both of these changes most likely contributed to improvement in her somatic complaints. Given the high prevalence of comorbid medical conditions and medical service utilization among individuals with borderline personality disorder,20 a thorough medical evaluation will not only improve patients’ overall quality of life but will also likely identify medical symptoms that have been masquerading as psychiatric symptoms and contributing to polypharmacy.
CONCLUSION
Despite good intentions to provide symptomatic relief, polypharmacy can be associated with iatrogenic harm and contribute to functional impairment, especially in the context of borderline personality disorder, in which symptomatic fluctuations are part of the illness itself. A thorough medical and psychiatric evaluation and management during an extended hospitalization allowed Ms A to experience a significant reduction in her medication burden—both in absolute numbers and complexity. A reduction in polypharmacy was associated with symptomatic improvement that was sustained 6 months postdischarge. Unfortunately, it is unknown whether treatment gains were maintained with the reduced medication regimen given that clinicians outside of her inpatient treatment team provided ongoing mental health care in her home community. Future efforts should collect data related to quantifying postdischarge mental health treatment. Nonetheless, with sustained symptomatic improvement over time, the patient is very likely to comply with a cheaper, less-complex medication regimen. Extended hospitalization may be clinically indicated for select patients and may be cost-efficient in the long run, especially in terms of reduced medical and pharmaceutical costs. Additional measures of medication risk and liability have the potential to become markers of treatment effectiveness.
Drug names: amphetamine/dextroamphetamine (Adderall and others), atorvastatin (Lipitor), atropine/diphenoxylate (Lomotil, Lonox, and others), buspirone (BuSpar and others), cetirizine (Zyrtec, Xyzal, and others), clonazepam (Klonopin and others), esomeprazole (Nexium, Vimovo, and others), lamotrigine (Lamictal and others), levothyroxine (Synthroid, Tirosint, and others), lithium (Lithobid and others), metformin (Glucophage and others), mirtazapine (Remeron and others), pregabalin (Lyrica), venlafaxine (Effexor and others), ziprasidone (Geodon), zolpidem (Ambien, Edluar, and others).
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Author affiliations: The Menninger Clinic and Menninger Department of Psychiatry and Behavioral Sciences, Baylor College of Medicine, Houston, Texas.
Financial disclosure: Drs Madan, Oldham, Gonzalez, and Fowler have no personal affiliations or financial relationships with any commercial interest to disclose relevant to the article.
Funding/support: This research was partially supported by The Menninger Clinic Foundation and McNair Medical Institute. Dr Madan is a McNair Scholar.
Role of the sponsors: This study follows the guidelines on good publication practices. The study sponsors were not involved in any aspect of the research activities and did not approve the specific protocol or manuscript. Thus, the authors were independent from study sponsors in the context of the research.
REFERENCES
1. Medical Directors Council and State Medicaid Directors. NASMHPD Medical Directors’ Technical Report on Psychiatric Polypharmacy. Alexandria, VA: National Association of State Mental Health Program Directors (NASMHPD); 2001.
2. Bender DS, Dolan RT, Skodol AE, et al. Treatment utilization by patients with personality disorders. Am J Psychiatry. 2001;158(2):295-302. PubMed doi:10.1176/appi.ajp.158.2.295
3. Frye MA, Ketter TA, Leverich GS, et al. The increasing use of polypharmacotherapy for refractory mood disorders: 22 years of study. J Clin Psychiatry. 2000;61(1):9-15. PubMed doi:10.4088/JCP.v61n0104
4. Centorrino F, Goren JL, Hennen J, et al. Multiple versus single antipsychotic agents for hospitalized psychiatric patients: case-control study of risks versus benefits. Am J Psychiatry. 2004;161(4):700-706. PubMed doi:10.1176/appi.ajp.161.4.700
5. Hospital-Based Inpatient Psychiatric Services. The Joint Commission website. http://www.jointcommission.org/hospital-based_inpatient_psychiatric_services/. Updated: May 5, 2014. Accessed June 11, 2014.
6. American Psychiatric Association Practice Guidelines. Practice guideline for the treatment of patients with borderline personality disorder. Am J Psychiatry. 2001;158(suppl 10):1-52. PubMed
7. Oldham JM. Guideline watch: practice guideline for the treatment of patients with borderline personality disorder. Focus. 2005;3(3):396-400. doi:10.1176/foc.3.3.396
8. National Health and Medical Research Council. Clinical Practice Guidelines for the Management of Borderline Personality Disorder. Melbourne, Australia: National Health and Medical Research Council; 2012.
9. National Institute of Health and Clinical Excellence. NICE Clinical Guideline 78. Borderline Personality Disorder: Treatment and Management. London, UK: National Institute of Health and Clinical Excellence; 2009.
10. Stoffers JM, Völlm BA, R×¼cker G, et al. Psychological therapies for people with borderline personality disorder. Cochrane Database Syst Rev. 2012;8:CD005652. PubMed doi:10.1002/14651858.cd005652.pub2
11. Lieb K, Zanarini MC, Schmahl C, et al. Borderline personality disorder. Lancet. 2004;364(9432):453-461. PubMed doi:10.1016/S0140-6736(04)16770-6
12. Tannenbaum C, Sheehan NL. Understanding and preventing drug-drug and drug-gene interactions. Expert Rev Clin Pharmacol. 2014;7(4):533-544. PubMed doi:10.1586/17512433.2014.910111
13. First MB, Spitzer RL, Gibbon M, et al. Structured Clinical Interview for DSM-IV-TR Axis I Disorders, Research Version, Nonpatient Edition. New York, NY: Biometrics Research, New York State Psychiatric Institute; 2002.
14. First MB, Gibbon M, Spitzer RL, et al. Structured Clinical Interview for DSM-IV Axis II Personality Disorders, (SCID-II). Washington, DC: American Psychiatric Press, Inc; 1997.
15. Madan A, Fowler JC. Consistency and coherence in treatment outcome measures for borderline personality disorder. Borderline Personal Disord Emoti Dysregul. 2015;2(1):1-4. doi:10.1186/s40479-014-0022-5
16. Kroenke K, Spitzer RL, Williams JB, et al. The Patient Health Questionnaire Somatic, Anxiety, and Depressive Symptom Scales: a systematic review. Gen Hosp Psychiatry. 2010;32(4):345-359. PubMed doi:10.1016/j.genhosppsych.2010.03.006
17. World Health Organization. Wellbeing Measures in Primary Care/The DEPCARE Project. Stockholm, Sweden: WHO Regional Office for Europe; 1998.
18. George J, Phun YT, Bailey MJ, et al. Development and validation of the Medication Regimen Complexity Index. Ann Pharmacother. 2004;38(9):1369-1376. PubMed doi:10.1345/aph.1D479
19. Zanarini MC, Frankenburg FR, Reich DB, et al. Attainment and stability of sustained symptomatic remission and recovery among patients with borderline personality disorder and Axis II comparison subjects: a 16-year prospective follow-up study. Am J Psychiatry. 2012;169(5):476-483. PubMed doi:10.1176/appi.ajp.2011.11101550
20. Keuroghlian AS, Frankenburg FR, Zanarini MC. The relationship of chronic medical illnesses, poor health-related lifestyle choices, and health care utilization to recovery status in borderline patients over a decade of prospective follow-up. J Psychiatr Res. 2013;47(10):1499-1506. PubMed doi:10.1016/j.jpsychires.2013.06.012
Enjoy this premium PDF as part of your membership benefits!