Objective: Bright light therapy is a noninvasive biological intervention for disorders with nonnormative circadian features. Eating disorders, particularly those with binge-eating and night-eating features, have documented nonnormative circadian eating and mood patterns, suggesting that bright light therapy may be an efficacious stand-alone or adjunctive intervention. The purpose of this systematic literature review, using PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines, was (1) to evaluate the state of the empirical treatment outcome literature on bright light therapy for eating disorders and (2) to explore the timing of eating behavior, mood, and sleep-related symptom change so as to understand potential mechanisms of bright light therapy action in the context of eating disorder treatment.
Data Sources: A comprehensive literature search using PsycInfo and PubMed/MEDLINE was conducted in April 2016 with no date restrictions to identify studies published using bright light therapy as a treatment for eating disorders. Keywords included combinations of terms describing disordered eating (eating disorder, anorexia nervosa, bulimia nervosa, binge eating, binge, eating behavior, eating, and night eating) and the use of bright light therapy (bright light therapy, light therapy, phototherapy). After excluding duplicates, 34 articles were reviewed for inclusion.
Study Selection and Data Extraction: 14 published studies of bright light therapy for eating disorders met inclusion criteria (included participants with an eating disorder/disordered-eating behaviors; presented as a case study, case series, open-label clinical trial, or randomized/nonrandomized controlled trial; written in English; and published and available by the time of manuscript review).
Results: Results suggest that bright light therapy is potentially effective at improving both disordered-eating behavior and mood acutely, although the timing of symptom response and the duration of treatment effects remain unknown.
Conclusions: Future research should systematically control for placebo response, assess symptom change frequently and across a broad range of systems, and evaluate the longer-term efficacy of bright light therapy for eating disorders.
A Systematic Review of
Bright Light Therapy for Eating Disorders
ABSTRACT
Objective: Bright light therapy is a noninvasive biological intervention for disorders with nonnormative circadian features. Eating disorders, particularly those with binge-eating and night-eating features, have documented nonnormative circadian eating and mood patterns, suggesting that bright light therapy may be an efficacious stand-alone or adjunctive intervention. The purpose of this systematic literature review, using PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines, was (1) to evaluate the state of the empirical treatment outcome literature on bright light therapy for eating disorders and (2) to explore the timing of eating behavior, mood, and sleep-related symptom change so as to understand potential mechanisms of bright light therapy action in the context of eating disorder treatment.
Data Sources: A comprehensive literature search using PsycInfo and PubMed/MEDLINE was conducted in April 2016 with no date restrictions to identify studies published using bright light therapy as a treatment for eating disorders. Keywords included combinations of terms describing disordered eating (eating disorder, anorexia nervosa, bulimia nervosa, binge eating, binge, eating behavior, eating, and night eating) and the use of bright light therapy (bright light therapy, light therapy, phototherapy). After excluding duplicates, 34 articles were reviewed for inclusion.
Study Selection and Data Extraction: 14 published studies of bright light therapy for eating disorders met inclusion criteria (included participants with an eating disorder/disordered-eating behaviors; presented as a case study, case series, open-label clinical trial, or randomized/nonrandomized controlled trial; written in English; and published and available by the time of manuscript review).
Results: Results suggest that bright light therapy is potentially effective at improving both disordered-eating behavior and mood acutely, although the timing of symptom response and the duration of treatment effects remain unknown.
Conclusions: Future research should systematically control for placebo response, assess symptom change frequently and across a broad range of systems, and evaluate the longer-term efficacy of bright light therapy for eating disorders.
Prim Care Companion CNS Disord
2016;18(5):doi:10.4088/PCC.16r02008
© Copyright 2016 Physicians Postgraduate Press, Inc.
aDepartment of Psychology, University of Missouri–Kansas City, Kansas City
*Corresponding author: Jennifer D. Lundgren, PhD, Department of Psychology, University of Missouri–Kansas City, 5030 Cherry St, Kansas City, Missouri, 64116 ([email protected]).
Circadian rhythm, or the variation in physiology and behavior that corresponds approximately to a 24-hour cycle,1 is disrupted in a variety of behavioral health conditions including mood disorders,2,3 sleep-wake disorders,4,5 and eating disorders.6–8 Circadian rhythm is regulated by biological clocks located both centrally, in the suprachiasmatic nuclei of the anterior hypothalamus, and peripherally in the organs such as the liver, gut, pancreas, fat, and muscle.9 The central circadian clock is synchronized (entrained) by cues, primarily light exposure and food intake. Other types of stimuli, however, can serve as synchronizing agents in the cellular circadian clocks throughout the body, including temperature, exercise, and even social cues.1,10
The eating disorder with the most prominent circadian dyssynchrony is night eating syndrome,11 characterized by a circadian delay of food intake manifested by evening hyperphagia and/or nocturnal awakening and ingestion of food.7,12 Neuroendocrine hormones associated with ingestive behavior, including leptin and insulin, have been found to mirror the phase-delayed food-intake pattern of individuals diagnosed with night eating syndrome.6 In this same study,6 ghrelin was phase advanced nearly 5 hours and glucose circadian rhythm was inverted. The authors6 cautioned that cause and effect between the nonnormative hormonal patterns and the circadian-delayed eating patterns cannot be established in their study, and it is plausible that eating behavior was entraining physiology in their sample. In addition to the prominent feature of circadian-delayed ingestive behavior and associated nonnormative hormonal circadian phase shifts found in persons with night eating syndrome, there is evidence of a unique circadian pattern of mood that worsens in the latter half of the day in many individuals diagnosed with night eating syndrome.7 This circadian mood pattern is reflected in the research diagnostic criterion that mood disturbance worsens in the evening.11 Although there is no evidence of a circadian phase delay or advance in the sleep patterns of individuals diagnosed with night eating syndrome, sleep architecture and quality is disrupted, particularly in people who regularly wake at night and consume food.13 Sleep disruption is an important aspect of circadian rhythm in individuals with night eating syndrome because light is involved in the entrainment of the central circadian clock.
Night eating syndrome is not the only eating disorder to display nonnormative circadian features. For example, Lavender and colleagues14 found that dietary restriction among individuals diagnosed with anorexia nervosa is more likely to occur in the first half of the day and that binge and purge episodes are more likely to occur in the evening. Mood disturbance that co-occurs with eating disorders also displays circadian features (eg, mood that worsens throughout the day)8 or seasonal worsening of mood.15 Ecological momentary assessment demonstrates that many individuals who struggle with binge eating experience the highest frequency of binge eating on days characterized by a circadian pattern of worsening affect throughout the day.16 Although the circadian timing of sleep does not appear to have phase advances or delays, disordered-eating behaviors are often associated with disruptions in the sleep-wake cycle.17 Binge-eating behavior has been associated with lifetime histories of sleep disturbance,18 with some evidence that disordered-eating behaviors precede difficulty initiating and maintaining sleep over time in young adults.19 As noted previously, the fact that sleep is so frequently disrupted in eating disorders is important from the perspective of circadian rhythm health because the sleep-wake and light-dark cycles are important central circadian rhythm synchronizers.1
Because light exposure is a central circadian synchronizer, bright light therapy is increasingly being used as a noninvasive biological intervention to treat disorders with circadian rhythm disruption. Administration of bright light therapy generally involves daily exposure to a specialized fluorescent light box designed to give off light at a much brighter intensity to that of indoor lighting, typically around 5,000 to 10,000 lux, for a minimum of 1 week in order to see therapeutic effects.20 Lux is a unit of light intensity measured at a specific distance from a light source (differing from lumens, which is the total light output measured at the source and not taking into account area or spread of the light). Examples of common lux ranges encountered include 100–500 lux (residential indoor lighting), 500–700 lux (well-lit office buildings), 10,000 lux (sunrise on a clear spring day), and 100,000 lux (noontime on a summer day).21 Mårtensson and colleagues22 documented significant variability in the length of bright light therapy among treatment outcome studies for both seasonal and nonseasonal depression (range, 1 week–6 weeks). The nature of the circadian disruption (eg, jet lag vs seasonal affective disorder) dictates the timing of bright light therapy exposure, but early morning exposure is more effective than evening exposure for mood disorders.23 The hypothesized mechanisms of action of bright light therapy, particularly for seasonal affective disorder, is the central realignment of circadian phase as the result of ocular light exposure, as well as increased alertness and arousal.20,24
Bright light therapy has been evaluated as an intervention for the treatment of disordered-eating behavior, particularly disorders involving binge-eating and night-eating behavior. To our knowledge, no systematic review has been conducted to summarize the state of the literature or explore patterns of treatment outcome. Therefore, the purpose of this review, using PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines,25 is (1) to evaluate the state of the empirical treatment outcome literature on bright light therapy for eating disorders, while being inclusive of multiple intervention methodologies and eating-disordered populations and (2) to explore the timing of eating behavior, mood, and sleep-related symptom change with bright light therapy so as to understand better potential mechanisms of bright light therapy action in the context of eating disorder treatment. Notably, we have focused our review on the specific behaviors of eating, mood, and sleep because of the well-established relationship between mood and eating behavior across eating disorders6,7 and the substantial empirical support for bright light therapy as an intervention for mood disorders, particularly those with a seasonal pattern.22 Additionally, sleep is an important outcome given the documented sleep disturbances associated with eating disorders13,18,19 and the role of the light-dark (sleep-wake) cycle in maintaining circadian rhythm. It is important to critically evaluate the state of the literature in order to inform future treatment outcome research using bright light therapy, particularly as the role of circadian rhythm disruption on behavioral health is increasingly being recognized.26
METHODS
Literature Search
A comprehensive literature search using PsycInfo and PubMed/MEDLINE was conducted to identify published studies indicating the use of bright light therapy as a treatment for eating disorders. The search was performed in April 2016 with no date restrictions using combinations of keywords describing disordered eating (eating disorder, anorexia nervosa, bulimia nervosa, binge eating, binge, eating behavior, eating, and night eating) and the use of bright light therapy (bright light therapy, light therapy, phototherapy). We searched the reference lists of other previously published studies to find additional articles. After excluding duplicates, the search resulted in 33 studies. During the manuscript review process, 1 additional study was published and included, yielding a total of 34 articles to be reviewed
Inclusion and Systematic Review Methods
Each of the 34 articles was screened by the first author (M.T.B.) using review inclusion criteria. Studies were deemed eligible if they (1) included participants diagnosed with an eating disorder or disordered-eating behaviors (eg, subthreshold eating disorder diagnosis, weight restricting, binge-purge episodes, compensatory behaviors, night eating), regardless of comorbid diagnoses (eg, mood disorders); (2) were presented as a case study, case series, open-label clinical trial, or a randomized or nonrandomized controlled clinical trial; (3) were reported in English; and (4) were published and available as of April 1, 2016. Additionally, articles were included if bright light therapy was the primary treatment or if it was adjunctive to another primary intervention, as long as the primary intervention did not change or was controlled for the duration of the bright light therapy. Because of the relatively low number of articles found, there were no methods used to assess risk of bias of individual studies.
For all included studies, the first author (M.T.B.) systematically reviewed the report and documented (1) the study design (eg, case study, case series, open-label clinical trial, or randomized/nonrandomized clinical trial; status of bright light therapy as a primary treatment) and methodology: bright light therapy intensity of light, session length and times per day, and duration of treatment; (2) the study and participant characteristics: participant mean age, gender composition, study sample size, diagnoses (eg, eating disorder and any comorbidity with seasonal affective disorder or major depression); and (3) outcome assessment and results of the study: measures used and follow-up outcomes if present. For studies that included assessments across multiple time points, the timing of change in eating disorder symptoms, mood, and sleep was documented in order to evaluate the timing of symptom change in relation to one another. The second author (J.D.L.) verified this process.
RESULTS
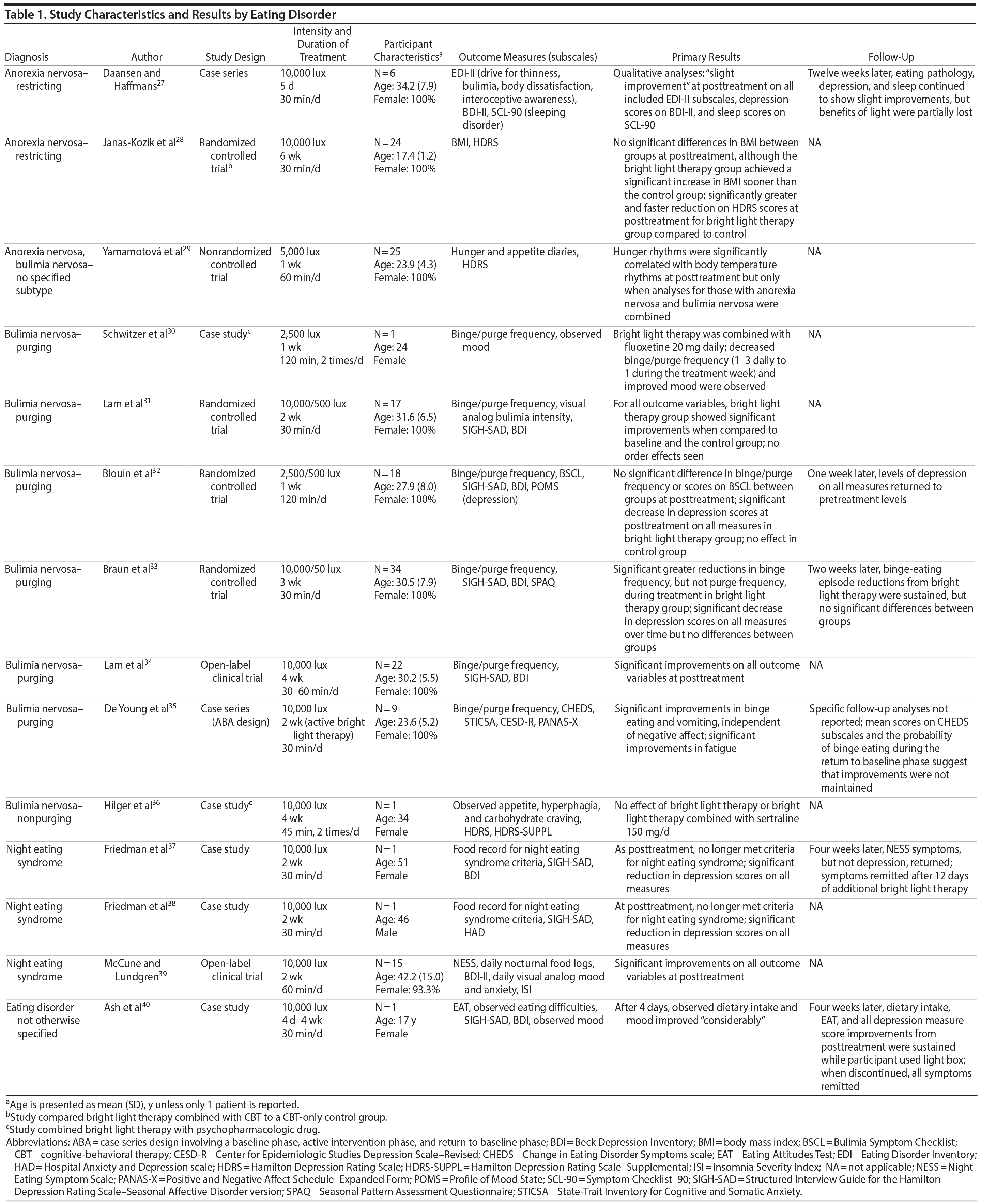
Of the 34 articles identified, 14 studies27–40 were eligible for inclusion in the review. Details about each of these 14 studies can be found in Table 1.
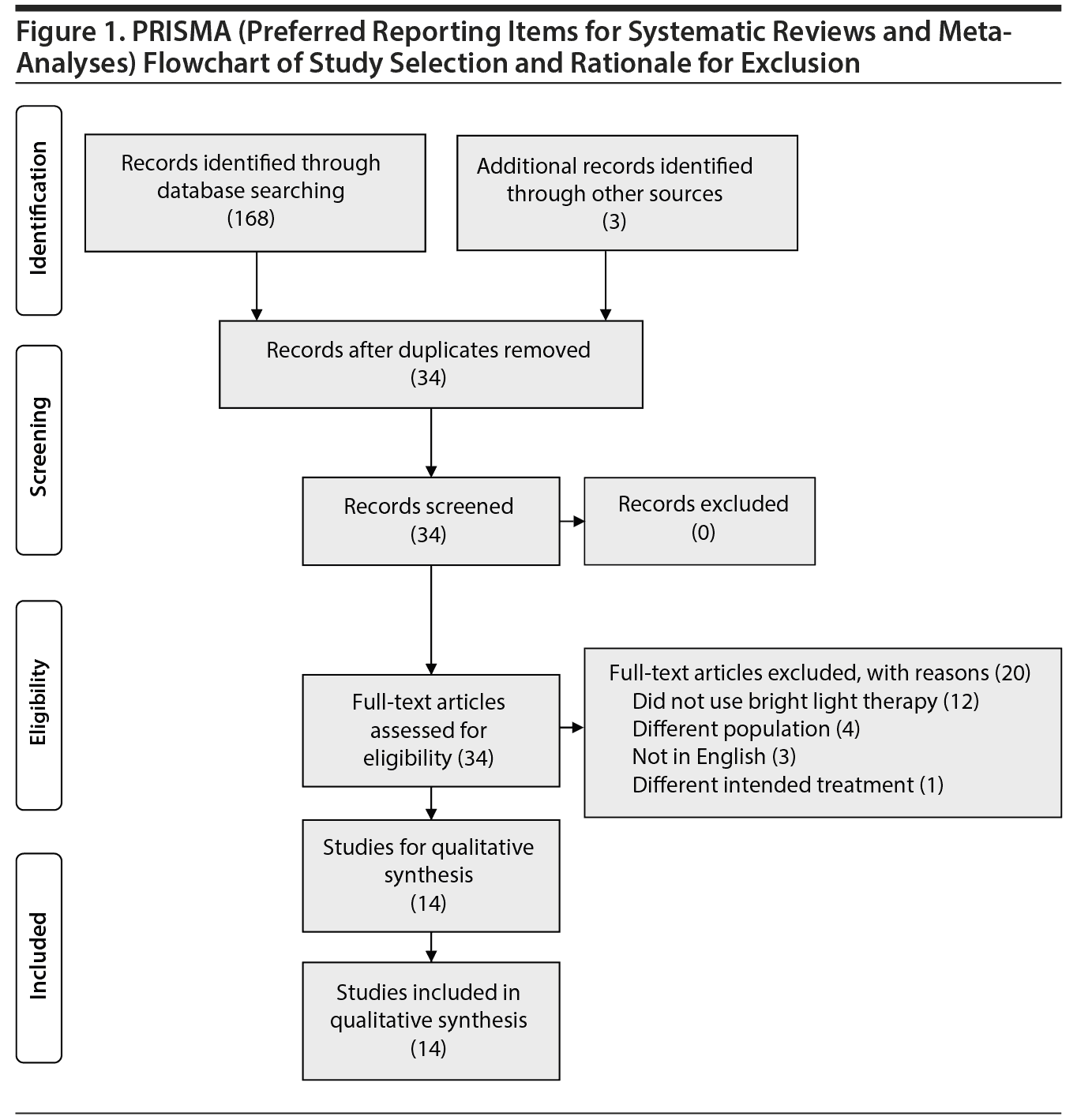
The remaining 20 articles were excluded on the basis of the following reasons: 12 studies did not actually use bright light therapy for disordered-eating behavior or were reports on treatment approaches for eating disorders; 3 studies used bright light therapy in a population with seasonal affective disorder, but recorded eating and dietary preferences; 3 studies were not reported in English; 1 study used bright light therapy in a population with Alzheimer’s disease; and 1 study used bright light therapy for weight reduction in an obese population. A PRISMA flow diagram25 depicting the phases of article identification, inclusion, and exclusion can be found in Figure 1.
Study Methodology and Characteristics
Design. As Table 1 illustrates, case studies (those following 1 participant over time) were the most frequently used study design (5 studies30,36–38,40). Three of those used bright light therapy in conjunction with pharmacotherapy. Randomized controlled trials (in which participants were randomly assigned to different groups) were the next most frequently used design (4 studies28,31–33). Three of those compared bright light therapy to a dim red light placebo condition; 1 compared bright light therapy in conjunction with cognitive-behavioral therapy (CBT) to CBT alone. These randomized controlled trials varied in their methodological designs (eg, crossover vs parallel, double-blind vs single-blind). The remaining 5 studies were open-label clinical trials (in which all participants received bright light therapy, 2 studies34,39), a case series (similar to the case study design but following multiple participants, 2 studies27,35), or a nonrandomized controlled trial against healthy participants (1 study29). Five studies27,32,33,37,40 included a follow-up period, which is the interval between the last bright light therapy session and the outcome measure, that ranged from 1-week to 12-week periods.
Light box methodology. Studies varied in their methodological use of light box treatment. The majority (11 studies) used 10,000 lux as their standard light intensity for active treatment, with 1 study29 using 5,000 lux and 2 studies30,32 using 2,500 lux. When dim red light was used as a control or comparison condition, 2 studies31,32 used 500 lux as the intensity and 1 study33 used 50 lux.
As seen in Table 1, session length was quite variable (30 minutes once a day to 120 minutes twice a day). However, the majority (8 studies27,28,31,33,35,37,38,40) reported a treatment duration of 30 minutes once a day. Duration of active treatment varied (4 days to 6 weeks). The 2 most common active treatment duration lengths were 2 weeks (5 studies31,35,37–39) and 1 week (3 studies29,30,32), with all other studies using unique treatment durations. Time of day for light box usage varied, with most study protocols prescribing light box exposure during the morning (11 studies27–29,31,33–35,37–40; either generally during the morning hours or at an exact time), although the others prescribed light box usage in the late afternoon and early evening (from 5:00–7:00 pm),32 both morning and evening (7:00–9:00 am and 6:00–8:00 pm),30 or not specified.36
Participant characteristics and diagnoses. Excluding case studies with 1 participant (5 studies30,36,37,38,40), the average number of participants in each of the 9 remaining studies was 18.89 (SD = 8.55), with a range of 6–34 participants. The mean age for participants across all studies (n = 175 individuals) was 30.96 years old (SD = 10.06). The majority of participants were female (98.9%, n = 173), and the vast majority of studies did not report participant ethnicity. Almost half of all participants (49.3%, n = 82 individuals) had a comorbid mood diagnosis.
All 14 studies included participants with full-threshold eating disorder diagnosis or disordered-eating behavior. Of the included studies, 227,28 included individuals with anorexia nervosa (restricting subtype), 630–35 included individuals with bulimia nervosa (purging type), 136 included an individual with bulimia nervosa (nonpurging type), 337–39 included individuals with night eating syndrome, 140 included an individual with a diagnosis of eating disorder not otherwise specified (DSM-III-R41 criteria) used at the time of the study, and 129 included a mix of individuals with either anorexia nervosa or bulimia nervosa (subtypes were not specified). See Table 1 for the listing of eating disorder diagnosis by study.
Assessments. The full list of measures used in the studies can be found in Table 1. Each study assessed eating pathology and mood. Food diaries and binge/purge logs were the most frequently used assessments for disordered eating, including the number of binge and purge episodes (10 studies29–35,37–39). Three studies used a self-report symptom assessment to measure disordered-eating behavior (Change in Eating Disorder Symptoms Scale,35 Eating Disorder Inventory-II [EDI-II],42 or Bulimia Symptoms Checklist43). The original Beck Depression Inventory44 and the Structured Interview Guide for the Hamilton Depression Rating Scale, Seasonal Affective Version45 were the most frequently used assessments of mood. Sleep/wake diaries were used to assess sleep in 4 studies, although only 227,39 reported sleep as an outcome variable; they used the Symptom Checklist-90 (SCL-90)46 and the Insomnia Severity Index (ISI),47 respectively, as their measures for sleep.
Summary of Results by Eating Disorder Diagnosis
Anorexia nervosa. Two studies27,28 examined participants with anorexia nervosa–restricting subtype, with 1 additional study29 including participants with anorexia nervosa, although subtype was not specified. Daansen and Haffmans27 reported that after bright light therapy and at a 12-week follow-up, they found “slight improvement” on core eating pathology as assessed by the drive for thinness, bulimia, body dissatisfaction, and interoceptive awareness subscales on the EDI-II. However, due to small sample size, these analyses were examined qualitatively. Janas-Kozik and colleagues28 used body mass index (BMI) as a proxy for eating behavior and found no significant differences at posttreatment for the bright light therapy + CBT group compared to a CBT-only control. They reported, however, that the group with bright light therapy achieved a significant increase in BMI compared to baseline much sooner than the control group (3 weeks compared to 6 weeks). Yamamotová and colleagues29 found that after bright light therapy, hunger rhythms were significantly correlated with body temperature rhythms. They stipulated, however, that this effect was evident only after participants with anorexia nervosa were pooled with those with bulimia nervosa.29
All 3 studies reported significant (or in the case of Daansen and Haffmans,27 moderate qualitative) reductions in depressive symptoms at posttreatment. Janas-Kozik et al28 found a significantly greater reduction in symptoms, faster reduction of symptoms (third week compared to fourth week), and lower intensity of symptoms at posttreatment from baseline for the bright light therapy + CBT group when compared to the control. The Daansen and Haffmans27 study was the only one to include a follow-up for this population, and they reported that “benefits were partly lost” after 3 months.(p295) Daansen and Haffmans27 reported having slight improvement from average to below average scores for sleep on the SCL-90 at both posttreatment and follow-up. They stated that this was verified with reports from the participants’ sleep diaries.
Bulimia nervosa. Seven studies30–36 examined participants with bulimia nervosa (6 with bulimia nervosa, purging subtype, and 1 with bulimia nervosa, nonpurging subtype). Results for disordered-eating behavior symptoms were mixed. Four studies30,31,34,35 found significant decreases in binge-eating episodes and purge frequency at posttreatment. Of the remaining studies, both Blouin and colleagues32 and Hilger and colleagues36 found no effect of bright light therapy on binge eating or purge frequency. Conversely, Braun and colleagues33 found significantly greater reductions in binge-eating episodes in the bright light therapy group during treatment compared to control but no effects on purge frequency. When assessing disordered-eating symptoms at a 2-week follow-up, Braun et al33 reported that binge-eating episode reductions were sustained, but there were no significant differences between groups.
All but 1 study36 reported significant reductions in depressive symptoms or negative affect. Braun and colleagues,33 however, reported that depressive symptoms decreased for both the bright light therapy and dim red light control groups over time, and there were no significant differences between groups. Blouin and colleagues32 also reported that depressive symptoms returned to pretreatment levels at a 1-week follow up. De Young and colleagues35 noted that fatigue was the only specific facet of negative affect to improve with bright light therapy in their sample.
The Hilger et al36 case study was the only article in this review to report no effects on both eating pathology and mood with either bright light therapy or bright light therapy in addition to sertraline 150 mg. Symptom reduction was eventually found after administering reboxetine 8 mg per day for 2 weeks. While this study36 used 4 weeks of bright light therapy twice daily for 45 minutes, there was no specification on prescribed time of day (morning, evening, or a specific time) for treatment administration.
Night eating syndrome. Three studies37–39 examined participants with night eating syndrome. All 3 studies found significant reductions in night eating syndrome symptoms (eg, morning anorexia, evening hyperphagia, awakenings during the nighttime that include snacking in order to restore sleep), with both case studies37,38 reporting that the participant no longer met criteria for night eating syndrome, although specific symptom reductions or presence of any remaining subthreshold symptoms were not reported in these studies. In the case of Friedman and colleagues,37 at a 4-week follow-up, the participant’s night eating syndrome symptoms returned but remitted after an additional 12 days of bright light therapy. No specifics on symptoms were reported.
All 3 studies37–39 also reported significant reductions in depressive symptoms. As mentioned previously, in the Friedman et al37 study, the participant’s night eating syndrome symptoms returned after 4 weeks. However, depressive symptoms remained in remission.
As stated previously, while other articles assessed for sleep, only 2 included sleep as outcome variables. For those with night eating syndrome, the McCune and Lundgren39 study assessed for sleep as an outcome measure. Decreased ISI scores reflected significant improvements in sleep at posttreatment.
Other. One study40 included a participant with eating disorder not otherwise specified (presented with DSM-III-R symptoms of anorexia nervosa but did not meet the criteria of low body weight). This study found that after 4 days of bright light therapy in an inpatient setting, the participant’s eating “improved considerably” and her dietary intake continually improved after 1 month of outpatient light box usage. However, the authors40 report that after discontinuing bright light therapy for a week, she was “unable to maintain adequate dietary intake.”(p96) The participant was administered bright light therapy immediately, her dietary intake was re-established, and bright light therapy was subsequently used over time as a prophylactic against further seasonal development of symptoms.40 Her depressive symptoms followed a similar pattern to her disordered-eating behaviors and were likewise as affected by the presence and absence of bright light therapy.
Order of symptom change. Only 132 of the 14 studies presented enough assessment data to examine the order of symptom change. Blouin and colleagues32 collected daily Profile of Mood State assessments and binge behavior diaries, allowing for an analysis of the covariance between depressed mood and disordered-eating behavior. They found that depressive symptoms assessed by the Beck Depression Inventory and Hamilton Depression Rating Scale significantly decreased after exposure to bright light therapy, but this was not seen in the dim red light control group. They also saw that the depressive symptoms returned to baseline levels after the withdrawal of bright light therapy at the 1-week follow-up. They saw a similar trend in the daily Profile of Mood State ratings for depression but noted that the group × time interaction was not significant. According to the daily binge diaries, the authors32 found no effect of group or time on binge/purge frequencies, but they noted a reduction of binge frequency over the last 2 days in the intervention group during the bright light therapy period, which was not seen at any other time or in the control group. This reduction, however, was not statistically significant. On the basis of these data, it is difficult to conclude whether decreases in binge episodes were secondary to improvement in depressive symptoms or vice versa. De Young and colleagues35 collected daily eating behavior and affect assessments but did not report on the order of symptom change across time. Their analyses did demonstrate that binge-eating frequency improved independent of changes in affect.
DISCUSSION
The purpose of this review was 2-fold: (1) to summarize the current state of the literature of bright light therapy with regard to its effect among individuals diagnosed with eating disorders and (2) to explore the relatively sparse outcome data for clues about potential mechanisms of symptom change, particularly in relation to eating behavior, mood, and sleep. While we were able to present a thorough review of the treatment outcome literature, our goal of understanding the relationship of mood, sleep, and eating behavior symptom change in relation to one another was not achieved due to the dearth of empirical data. Nevertheless, in order to further the state of the literature, we offer our suggestions for future research in the use of bright light therapy for eating disorders to include designs capable of collecting sufficient and necessary data to clarify the resulting mechanisms of action.
Overall, the majority of studies that have examined bright light therapy for disordered eating have demonstrated significant improvements in both depressed mood and eating pathology for the duration of the treatment period, with only a select few studies exhibiting null results in 1 or both of these primary outcomes. These improvements were found regardless of the type of eating disorder present. Sleep, unfortunately, was rarely assessed. Study design, light box methodology, and treatment duration varied among studies, with the majority being case studies utilizing 10,000 lux as the active treatment dose and using the light in the morning for at least 30 minutes daily for 2 weeks.
These findings are consistent with other studies highlighting the potential use of bright light therapy for disordered eating.48,49 Aigner and colleagues48 briefly noted the outcomes of the Lam et al31 and Braun et al33 studies in their report on pharmacologic interventions for eating disorders. Krysta and colleagues49 included the results from 6 studies, as well as a discussion on the overlapping role of depression and disordered eating, in their review of treatments for depression in adolescent populations. The current report, however, is the first to systematically review the use of bright light therapy on all forms of disordered-eating behavior. Furthermore, this report also included uncontrolled studies and case studies to provide the only comprehensive review across all ages in the present literature. Importantly, because the studies included in this review varied significantly in methodological quality, the results should be interpreted with significant caution.
Authors have continually suggested that bright light therapy is a potential stand-alone or adjunctive intervention for individuals with disordered eating, especially those with a seasonal component to their symptoms. Relatively few studies, however, are well controlled, and researchers have not attempted to examine the mechanisms of symptom change when using bright light therapy in populations with disordered eating (ie, Why is bright light therapy effective in this population? Is it due to improvement in mood or sleep or is there a mechanism specific to the regulation of food intake?). We suggest that future studies include designs and assessment methods capable of examining these specific parameters.
Table 2 provides a list of suggested assessment techniques across a range of behavioral and physiologic domains relevant to disordered-eating behavior. It is important to assess changes across multiple domains (eg, eating behavior, hunger and satiety hormones, and neural response to food cues) to evaluate potential mechanisms of action in bright light therapy for disordered eating. The inclusion of a dim red light control group via a randomized controlled trial or other similar design would also benefit the literature by controlling for placebo effects and the improvement of depressive symptoms spontaneously over time.

Alongside these suggestions, we also propose that future studies explore an alternative conceptualization of bright light therapy on disordered eating in light of the data on circadian rhythm and sleep disruption in such disorders. Previous studies29,31 have sought to understand the effect of bright light therapy on disordered eating through the framework of its use in seasonal affective disorder (ie, improvements in mood may lead to improvements in binge/purge episodes, restrictive eating, etc). These studies29,31 suggest that symptoms of disordered eating, as well as mood, hormone and temperature regulation, and sleep, are the result of an increased metabolism of melatonin and lower levels of serotonin due to circadian rhythm disturbances, commonly seen in winter months with decreased exposure to light. As such, studies examining bright light therapy in this population also assess mood symptoms.
While this effect may exist, no studies to our knowledge have experimentally examined sleep within the bright light therapy/disordered-eating literature. Only 4 of the 14 studies in this review mentioned sleep, and 2 assessed sleep improvements alongside disordered eating. Given the role of sleep disturbance in both mood disorders50 and disordered eating, as well as its potential to disrupt circadian rhythm, it may be possible that individuals are seeing improvements in their disordered eating because they have improved sleep. Notably, De Young and colleagues35 found that fatigue, as assessed by the Positive and Negative Affect Schedule–Expanded Form, was the only facet of negative affect to improve with bright light therapy administration in women with bulimia nervosa. They did not assess sleep specifically, so it is unknown if changes in fatigue correlated with changes in sleep in their sample. Also, the relationship between circadian rhythm and mood disturbances may suggest a potential mediation effect when conceptualizing sleep within a bright light therapy/disordered-eating framework (ie, Is this an intervention that improves sleep that acts as a mediator between mood and disordered eating?). For example, Blouin and colleagues32 found decreases in depressive symptoms but no initial effect on binge/purge episodes between groups. Their bright light therapy design was the only one to specify that participants receive the intervention in the early evening, which has been shown to have a different effect on circadian rhythm synchronization compared to early morning exposure.23 Indeed, it is possible that sleep was unaffected by the intervention in this particular study and may explain why the effect was not present on disordered eating.
This review has several limitations. Although results suggest that bright light therapy is likely efficacious for individuals regardless of eating disorder, binge-eating disorder was not included because no study assessed this particular eating disorder. Likewise, several articles included in this review were case studies, and the bulk of the remaining articles had a mean of 19 participants, an overwhelming majority of which were female. These relatively small and homogenous samples, coupled with the small number of studies, varying light box methodologies, and the presence of studies with null findings in 1 or more outcome variables, cast doubt on the internal validity of many of the studies and the generalizability validity of the conclusions in this review. More thorough and methodologically rigorous outcome studies are needed to evaluate the efficacy and durability of bright light therapy for the treatment of eating disorders. Future studies that address these methodological limitations, as well as assess a much broader range of behavioral and physiologic systems, are necessary to advance this literature and further evaluate the empirical foundation of bright light therapy for disordered-eating behavior.
Submitted: June 24, 2016; accepted September 8, 2016.
Published online: October 27, 2016.
Drug names: fluoxetine (Prozac and others), sertraline (Zoloft and others).
Potential conflicts of interest: None.
Funding/support: None.
REFERENCES
1. Vitaterna MH, Takahashi JS, Turek FW. Overview of circadian rhythms. Alcohol Res Health. 2001;25(2):85–93. PubMed
2. Turek FW. From circadian rhythms to clock genes in depression. Int Clin Psychopharmacol. 2007;22(suppl 2):S1–S8. PubMed doi:10.1097/01.yic.0000277956.93777.6a
3. Kripke DF, Elliott JA, Welsh DK, et al. Photoperiodic and circadian bifurcation theories of depression and mania. F1000 Res. 2015;4:107. PubMed doi:10.12688/f1000research.6444.1
4. Bjorvatn B, Pallesen S. A practical approach to circadian rhythm sleep disorders. Sleep Med Rev. 2009;13(1):47–60. PubMed doi:10.1016/j.smrv.2008.04.009
5. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Publishing; 2013.
6. Goel N, Stunkard AJ, Rogers NL, et al. Circadian rhythm profiles in women with night eating syndrome. J Biol Rhythms. 2009;24(1):85–94. PubMed doi:10.1177/0748730408328914
7. O’Reardon JP, Ringel BL, Dinges DF, et al. Circadian eating and sleeping patterns in the night eating syndrome. Obes Res. 2004;12(11):1789–1796. PubMed doi:10.1038/oby.2004.222
8. Crosby RD, Wonderlich SA, Engel SG, et al. Daily mood patterns and bulimic behaviors in the natural environment. Behav Res Ther. 2009;47(3):181–188. PubMed doi:10.1016/j.brat.2008.11.006
9. Silva CM, Sato S, Margolis RN. No time to lose: workshop on circadian rhythms and metabolic disease. Genes Dev. 2010;24(14):1456–1464. PubMed doi:10.1101/gad.1948310
10. Mistlberger RE, Skene DJ. Social influences on mammalian circadian rhythms: animal and human studies. Biol Rev Camb Philos Soc. 2004;79(3):533–556. PubMed doi:10.1017/S1464793103006353
11. Allison KC, Lundgren JD, O’Reardon JP, et al. Proposed diagnostic criteria for night eating syndrome. Int J Eat Disord. 2010;43(3):241–247. PubMed
12. Lundgren JD, Shapiro JR, Bulik CM. Night eating patterns of patients with bulimia nervosa: a preliminary report. Eat Weight Disord. 2008;13(4):171–175. PubMed doi:10.1007/BF03327503
13. Rogers NL, Dinges DF, Allison KC, et al. Assessment of sleep in women with night eating syndrome. Sleep. 2006;29(6):814–819. PubMed
14. Lavender JM, Utzinger LM, Crosby RD, et al. A naturalistic examination of the temporal patterns of affect and eating disorder behaviors in anorexia nervosa. Int J Eat Disord. 2016;49(1):77–83. PubMed doi:10.1002/eat.22447
15. Donofry SD, Roecklein KA, Rohan KJ, et al. Prevalence and correlates of binge eating in seasonal affective disorder. Psychiatry Res. 2014;217(1–2):47–53. PubMed doi:10.1016/j.psychres.2014.03.012
16. Berg KC, Peterson CB, Crosby RD, et al. Relationship between daily affect and overeating-only, loss of control eating-only, and binge eating episodes in obese adults. Psychiatry Res. 2014;215(1):185–191. PubMed doi:10.1016/j.psychres.2013.08.023
17. Kim KR, Jung YC, Shin MY, et al. Sleep disturbance in women with eating disorder: prevalence and clinical characteristics. Psychiatry Res. 2010;176(1):88–90. PubMed doi:10.1016/j.psychres.2009.03.021
18. Trace SE, Thornton LM, Runfola CD, et al. Sleep problems are associated with binge eating in women. Int J Eat Disord. 2012;45(5):695–703. PubMed doi:10.1002/eat.22003
19. Bos SC, Soares MJ, Marques M, et al. Disordered eating behaviors and sleep disturbances. Eat Behav. 2013;14(2):192–198. PubMed doi:10.1016/j.eatbeh.2013.01.012
20. Pail G, Huf W, Pjrek E, et al. Bright-light therapy in the treatment of mood disorders. Neuropsychobiology. 2011;64(3):152–162. PubMed doi:10.1159/000328950
21. Rosenthal NE. Winter Blues: Everything You Need to Know to Beat Seasonal Affective Disorder. 4th ed. New York, NY: Guilford Publications; 2012.
22. Mårtensson B, Pettersson A, Berglund L, et al. Bright white light therapy in depression: a critical review of the evidence. J Affect Disord. 2015;182:1–7. PubMed doi:10.1016/j.jad.2015.04.013
23. Terman M, Terman JS, Ross DC. A controlled trial of timed bright light and negative air ionization for treatment of winter depression. Arch Gen Psychiatry. 1998;55(10):875–882. PubMed doi:10.1001/archpsyc.55.10.875
24. Cajochen C. Alerting effects of light. Sleep Med Rev. 2007;11(6):453–464. PubMed doi:10.1016/j.smrv.2007.07.009
25. Moher D, Liberati A, Tetzlaff J, et al; PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med. 2009;151(4):264–269, W64. PubMed doi:10.7326/0003-4819-151-4-200908180-00135
26. Jagannath A, Peirson SN, Foster RG. Sleep and circadian rhythm disruption in neuropsychiatric illness. Curr Opin Neurobiol. 2013;23(5):888–894. PubMed doi:10.1016/j.conb.2013.03.008
27. Daansen PJ, Haffmans J. Reducing symptoms in women with chronic anorexia nervosa: a pilot study on the effects of bright light therapy. Neuroendocrinol Lett. 2010;31(3):290–296. PubMed
28. Janas-Kozik M, Krzystanek M, Stachowicz M, et al. Bright light treatment of depressive symptoms in patients with restrictive type of anorexia nervosa. J Affect Disord. 2011;130(3):462–465. PubMed doi:10.1016/j.jad.2010.10.014
29. Yamamotová A, Papezová H, Vevera J. Normalizing effect of bright light therapy on temperature circadian rhythm in patients with eating disorders. Neuroendocrinol Lett. 2008;29(1):168–172. PubMed
30. Schwitzer J, Neudorfer C, Fleischhacker WW. Seasonal bulimia treated with fluoxetine and phototherapy. Am J Psychiatry. 1993;150(11):1752. PubMed doi:10.1176/ajp.150.11.1752a
31. Lam RW, Goldner EM, Solyom L, et al. A controlled study of light therapy for bulimia nervosa. Am J Psychiatry. 1994;151(5):744–750. PubMed doi:10.1176/ajp.151.5.744
32. Blouin AG, Blouin JH, Iversen H, et al. Light therapy in bulimia nervosa: a double-blind, placebo-controlled study. Psychiatry Res. 1996;60(1):1–9. PubMed doi:10.1016/0165-1781(95)02532-4
33. Braun DL, Sunday SR, Fornari VM, et al. Bright light therapy decreases winter binge frequency in women with bulimia nervosa: a double-blind, placebo-controlled study. Compr Psychiatry. 1999;40(6):442–448. PubMed doi:10.1016/S0010-440X(99)90088-3
34. Lam RW, Lee SK, Tam EM, et al. An open trial of light therapy for women with seasonal affective disorder and comorbid bulimia nervosa. J Clin Psychiatry. 2001;62(3):164–168. PubMed doi:10.4088/JCP.v62n0305
35. De Young KP, Thiel A, Goodman EL, et al. A preliminary mechanistic test of the effects of light therapy in bulimia nervosa. Adv Eat Disord. 2016;4(3):237–249. doi:10.1080/21662630.2016.1198980.
36. Hilger E, Willeit M, Praschak-Rieder N, et al. Reboxetine in seasonal affective disorder: an open trial. Eur Neuropsychopharmacol. 2001;11(1):1–5. PubMed doi:10.1016/S0924-977X(00)00114-0
37. Friedman S, Even C, Dardennes R, et al. Light therapy, obesity, and night-eating syndrome. Am J Psychiatry. 2002;159(5):875–876. PubMed doi:10.1176/appi.ajp.159.5.875
38. Friedman S, Even C, Dardennes R, et al. Light therapy, nonseasonal depression, and night eating syndrome. Can J Psychiatry. 2004;49(11):790. PubMed
39. McCune AM, Lundgren JD. Bright light therapy for the treatment of night eating syndrome: a pilot study. Psychiatry Res. 2015;229(1–2):577–579. PubMed doi:10.1016/j.psychres.2015.07.079
40. Ash JB, Piazza E, Anderson JL. Light therapy in the clinical management of an eating-disordered adolescent with winter exacerbation. Int J Eat Disord.
1998;23(1):93–97. PubMed doi:10.1002/(SICI)1098-108X(199801)23:1<93::AID-EAT12>3.0.CO;2-O
41. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. Third Edition, Revised. Washington, DC: American Psychiatric Publishing; 1987.
42. Garner DM. Eating Disorder Inventory-II. Odessa, FL: Psychological Assessment Resources; 1991.
43. Blouin AG, Blouin JH, Perez EL, et al. Treatment of bulimia with fenfluramine and desipramine. J Clin Psychopharmacol. 1988;8(4):261–269. PubMed doi:10.1097/00004714-198808000-00005
44. Beck AT, Ward CH, Mendelson M, et al. An inventory for measuring depression. Arch Gen Psychiatry. 1961;4:561–571. PubMed doi:10.1001/archpsyc.1961.01710120031004
45. Williams JB. Structured Interview Guides for the Hamilton Rating Scales. Psychopharmacol Ser. 1990;9:48–63. PubMed
46. Derogatis LR. The SCL-90 Manual I: Scoring, Administration, and Procedures for the SCL-90. Baltimore, MD: Clinical Psychometric Research; 1977.
47. Bastien CH, Vallières A, Morin CM. Validation of the Insomnia Severity Index as an outcome measure for insomnia research. Sleep Med. 2001;2(4):297–307. PubMed doi:10.1016/S1389-9457(00)00065-4
48. Aigner M, Treasure J, Kaye W, et al; WFSBP Task Force On Eating Disorders. World Federation of Societies of Biological Psychiatry (WFSBP) guidelines for the pharmacological treatment of eating disorders. World J Biol Psychiatry. 2011;12(6):400–443. PubMed doi:10.3109/15622975.2011.602720
49. Krysta K, Krzystanek M, Janas-Kozik M, et al. Bright light therapy in the treatment of childhood and adolescence depression, antepartum depression, and eating disorders. J Neural Transm (Vienna). 2012;119(10):1167–1172. PubMed doi:10.1007/s00702-012-0863-2
50. Breslau N, Roth T, Rosenthal L, et al. Sleep disturbance and psychiatric disorders: a longitudinal epidemiological study of young adults. Biol Psychiatry. 1996;39(6):411–418. PubMed doi:10.1016/0006-3223(95)00188-3
Enjoy this premium PDF as part of your membership benefits!


