Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
To the Editor: Myasthenia gravis (MG) is a chronic autoimmune disease characterized by neuromuscular transmission dysfunction. Depression and anxiety disorders are frequent in MG patients, and pharmacologic treatment may be compromised by adverse effects on neuromuscular transmission or respiratory depression. Cognitive-behavioral therapy (CBT) is an evidence-based form of psychotherapy for treatment of depression, anxiety disorders, and insomnia with the benefit of having no adverse effects on MG.
Cognitive-Behavioral Therapy for Psychiatric Comorbidity in a Case of Muscle-Specific Kinase-Positive Myasthenia Gravis
To the Editor: Myasthenia gravis (MG) is a chronic autoimmune disease characterized by neuromuscular transmission dysfunction. Depression and anxiety disorders are frequent in MG patients, and pharmacologic treatment may be compromised by adverse effects on neuromuscular transmission or respiratory depression.1-4 Cognitive-behavioral therapy (CBT) is an evidence-based form of psychotherapy for treatment of depression, anxiety disorders, and insomnia5 with the benefit of having no adverse effects on MG. We report the case of a patient with severe MG and comorbid adjustment disorder with mixed anxiety, depression, and insomnia that were effectively treated with CBT.
Case report. A 59-year-old woman presented to a neurology clinic with ocular symptoms and a previous diagnosis of MG. Electromyography indicated normal nerve conduction velocities and amplitudes in the ulnar nerve. Repetitive stimulation of the spinal accessory nerve at 2 Hz pre- and postexercise for 1 minute showed a decremental response in the trapezius muscle. Acetylcholine receptor antibodies were negative, but her muscle-specific kinase antibody level was 2,560 nmol/L. A CT scan of the chest was within normal limits. Within 2 months of her MG diagnosis, she developed an acute exacerbation with dysphagia and breathing difficulties. Examination revealed anxiety, dysarthria, and bilateral ptosis. She was treated with a course of intravenous immunoglobulin (IVIg), pyridostigmine 60 mg qid, and prednisone 60 mg/d in the hospital, which improved the MG symptoms, but she became extremely anxious and fearful of dying in her sleep from breathing difficulties. She developed severe insomnia, which was unresponsive to medications. She was referred for CBT and continued treatment for MG including IVIg.
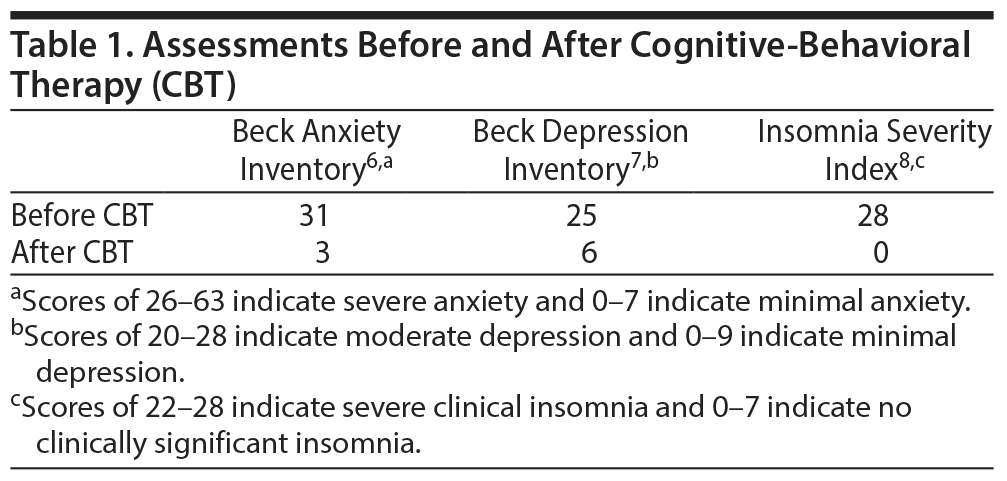
At the first CBT session, her nightly sleep averaged 2 hours. Her mood was anxious and sad, and she had daily headaches. She worried that insomnia would worsen the MG, damage her health irreparably, and result in death. She worried about burdening her husband and was frustrated by the excessive fatigue from MG. She was diagnosed with adjustment disorder with mixed anxiety, depressed mood with comorbid insomnia (DSM-IV criteria). Sleep hygiene education, relaxation, and stimulus-control strategies were used to address the insomnia. Behavioral strategies and cognitive restructuring were utilized to target the anxiety and depressive symptoms. By the fourth CBT session, her anxiety level, panic attacks, and insomnia improved even though she still had MG symptoms of fatigue, chewing difficulties, dysarthria, and jaw weakness. She subsequently had another exacerbation of MG with facial weakness, dysphagia, and respiratory distress, which required intubation. Plasmapheresis was instituted along with mycophenolate, and she recovered quickly. Despite the MG exacerbation, she maintained improvements in insomnia, anxiety, and depression. She continued CBT and received a total of 7 hourly sessions. By her last session, insomnia was resolved and sleep time averaged 7 hours 42 minutes with 2 brief awakenings. She no longer met diagnostic criteria for adjustment disorder with anxious and depressed mood (Table 1). She continued plasmapheresis and rituximab treatment for another 3 years. Muscle-specific kinase antibody titers decreased from 1,280 nmol/L to 20 nmol/L. All medications for MG were discontinued. She remained in complete stable remission for 2 years. At follow-up, 19 months after CBT treatment, she continued to do well and to apply the CBT strategies to cope with occasional compromised sleep or negative mood changes.
Despite the ongoing manifestations of MG in the initial stages, the comorbid anxiety, depression, and severe insomnia improved with CBT in a relatively brief time, and the improvements were sustained for 19 months after CBT was completed. At a later stage, the effective treatment and improvement of MG symptoms also could have contributed to the improved insomnia and psychological status. Considering its safety and efficacy, CBT could be a first-line treatment for comorbid anxiety, depression, or insomnia disorders in MG patients and thus warrants increased awareness of this treatment modality.
References
1. Ybarra MI, Kummer A, Frota ER, et al. Psychiatric disorders in myasthenia gravis. Arq Neuropsiquiatr. 2011;69(2A):176-179. PubMed CrossRef
2. Paradis C, Friedman S, Lazar RM, et al. Anxiety disorders in a neuromuscular clinic. Am J Psychiatry. 1993;150(7):1102-1104. PubMed CrossRef
3. Magni G, Micaglio GF, Lalli R, et al. Psychiatric disturbances associated with myasthenia gravis. Acta Psychiatr Scand. 1988;77(4):443-445. PubMed CrossRef
4. Kulaksizoglu IB. Mood and anxiety disorders in patients with myasthenia gravis. CNS Drugs. 2007;21(6):473-481. PubMed CrossRef
5. Chambless DL, Ollendick TH. Empirically supported psychological interventions: controversies and evidence. Annu Rev Psychol. 2001;52(1):685-716. PubMed CrossRef
6. Beck AT, Ward CH, Mendelson M, et al. An inventory for measuring depression. Arch Gen Psychiatry. 1961;4(6):561-571. PubMed CrossRef
7. Beck AT, Epstein N, Brown G, et al. An inventory for measuring clinical anxiety: psychometric properties. J Consult Clin Psychol. 1988;56(6):893-897. PubMed CrossRef
8. Morin CM, Belleville G, Bélanger L, et al. The Insomnia Severity Index: psychometric indicators to detect insomnia cases and evaluate treatment response. Sleep. 2011;34(5):601-608. PubMed CrossRef
aDepartment of Psychiatry and Behavioral Neuroscience, St Louis University School of Medicine, St Louis, Missouri
bDepartment of Neurology, George Washington University, Washington, DC
Potential conflicts of interest: None.
Funding/support: None.
Patient consent: Permission was received from the patient to publish the case, and the case has been de-identified to protect anonymity.
Published online: October 26, 2017.
Prim Care Companion CNS Disord 2017;19(5):17l02103
https://doi.org/10.4088/PCC.17l02103
© Copyright 2017 Physicians Postgraduate Press, Inc.
Enjoy this premium PDF as part of your membership benefits!