Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
To the Editor: In the United States, there are approximately 3.2 million people—1.2% of the population—with a diagnosis of schizophrenia. While this percentage only represents a small fraction of the total population, it is estimated that one-third of these individuals have treatment-resistant schizophrenia. Although clozapine is the only US Food and Drug Administration (FDA)-approved antipsychotic for treatment-resistant schizophrenia, its use is limited by its unique and rather intimidating side effect profile, including agranulocytosis (incidence of approximately 1%) and myocarditis (incidence of approximately 3%).
Clozapine-Induced Myocarditis: The Heartfelt Silent Assassin
To the Editor: In the United States, there are approximately 3.2 million people—1.2% of the population—with a diagnosis of schizophrenia.1 While this percentage only represents a small fraction of the total population, it is estimated that one-third of these individuals have treatment-resistant schizophrenia.2 Although clozapine is the only US Food and Drug Administration (FDA)-approved antipsychotic for treatment-resistant schizophrenia,3 its use is limited by its unique and rather intimidating side effect profile, including agranulocytosis (incidence of approximately 1%)4 and myocarditis (incidence of approximately 3%).5 Clozapine labeling provides rigorous hematology monitoring recommendations for frequency and clinical decisions on the basis of absolute neutrophil count but does not provide the same type of guidance for the early detection of myocarditis.6 While incidence of clozapine-induced myocarditis has been estimated at 3%,5 mortality rates have been reported as high as 50% when undetected.5,7 Since 83% of myocarditis cases develop within 2 to 3 weeks of clozapine initiation,5 the high mortality rates may reflect difficulty in differentiating symptoms of clozapine dose titration from nonspecific symptoms (tachycardia, fever, and fatigue) of myocarditis.8 In the majority of cases, clozapine-induced myocarditis occurs at standard dosing ranges of 100-450 mg daily, which suggests a non-dose-dependent effect.7
Many health care providers have the misconception that eosinophilia can serve as the primary marker for the onset of clozapine-induced myocarditis. In a case series by Ronaldson et al,9 66% of nonfatal cases did not develop eosinophilia until up to 7 days after peak troponin I/T levels, indicating eosinophilia is not useful in the early detection of myocarditis. Two other markers, C-reactive protein (CRP) and troponin, are more consistent in providing earlier detection of myocarditis.7 CRP elevation occurs around the same time as symptom onset and is followed by an elevation in troponin that may not be detectable for 3 days or more.10 In symptomatic patients, studies have shown that a combination of troponin 2 times the upper limit of normal and CRP > 100 mg/L is diagnostic of clozapine-induced myocarditis with 100% sensitivity.11 A monitoring protocol described by Ronaldson et al11 recommends immediate discontinuation of clozapine following these laboratory findings. Determination to rechallenge should be made on a case-by-case basis after stratifying the patient’s risks and benefits.
The Clozapine Review Committee (CRC) at our hospital implemented a clozapine-induced myocarditis monitoring protocol to improve patient safety, in part, because clozapine utilization more than doubled in the previous couple of years. The CRC decided that adding CRP and troponin T testing at baseline and weekly with complete blood counts (CBCs) for the first month of clozapine treatment placed little extra burden on patients and hospital staff. The testing was also considered to be a very favorable venture from an economic perspective, since the total cost of monitoring weekly CRP and troponin T levels for 1 month was $164.24 per patient. The hospital’s clozapine titration protocol was officially updated to include a prepopulated laboratory order for baseline and weekly CRP and troponin T levels for 1 month with weekly CBCs.
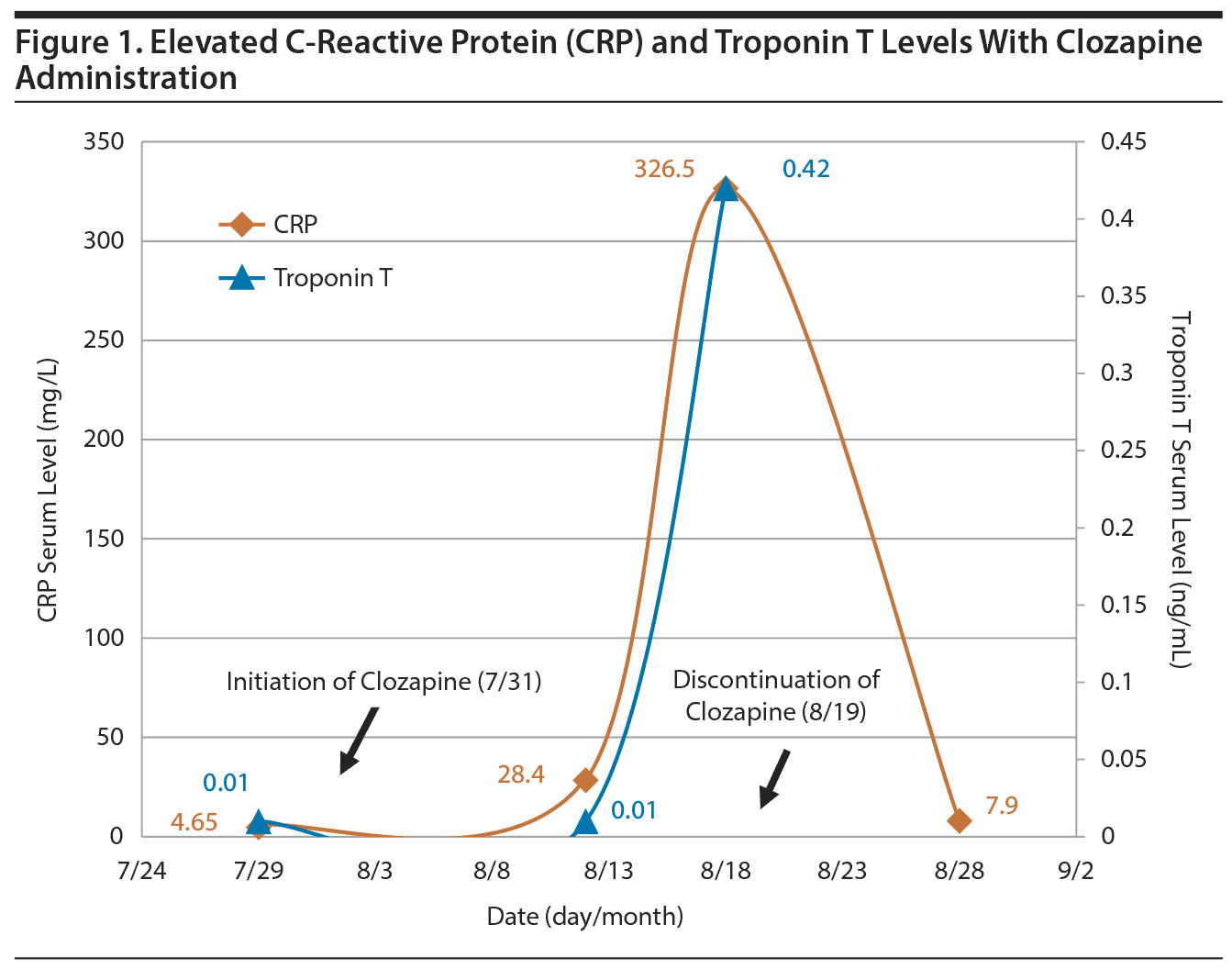
Case report. Mr A, a 30-year-old black male resident of a long-term care facility, was started on clozapine for management of treatment-refractory schizophrenia. Past medical history included hypertension, type 2 diabetes mellitus, hyperlipidemia, allergic rhinitis, nutcracker esophagus, and extrapyramidal side effects. Per medical records, there was no history of cardiovascular disease. At the time of clozapine initiation, Mr A’s medications included amlodipine 5 mg/d, metformin 1,000 mg/d, pravastatin 20 mg/d, montelukast 10 mg/d, loratadine 20 mg/d, omeprazole 80 mg/d, benztropine 1 mg/d, haloperidol 40 mg/d, iloperidone 16 mg/d, and olanzapine 15 mg/d. Haloperidol and iloperidone were discontinued by day 4 of clozapine treatment, and olanzapine was discontinued by day 13. Two days prior to initiating clozapine, baseline CRP, troponin T, and eosinophil were measured and determined to be within normal limits (4.65 mg/L, < 0.010 ng/mL, and 0.12 cells/mm3, respectively). Per hospital protocol, clozapine was initiated and slowly titrated over 17 days to 300 mg/d.
Twelve days after clozapine initiation, the CRP level (28.4 mg/L) was moderately elevated, while the troponin T level (< 0.01 ng/mL) and eosinophil count (0.10 ח 109/L) remained within normal limits. During this time, Mr A complained of a headache, nausea, and anorexia. He developed a fever of 101.3°F (38.5°C) on day 15, which peaked 3 days later to 102°F (38.9°C) and was accompanied by tachycardia (120 bpm). On day 18, the CRP (326.5 mg/L) and troponin T (0.42 ng/mL) levels had risen substantially (Figure 1); however, his eosinophil count remained within normal limits (0.10 ח 109/L). Because Mr A demonstrated signs and symptoms consistent with myocarditis, immediate discontinuation of clozapine treatment was warranted. Mr A became afebrile the day after clozapine was discontinued on day 19, while his CRP level was almost within normal limits by day 28. On day 20, a 12-lead electrocardiogram revealed sinus tachycardia, nonspecific T wave abnormalities, a normal QTc interval, and no ST-segment abnormalities. On day 21, a transthoracic echocardiogram was unremarkable, with left ventricular ejection fraction of 55%.
As the only FDA-approved antipsychotic for patients with treatment-resistant schizophrenia, treatment with clozapine cannot be ruled out due to fear of adverse effects. When monitored appropriately, clozapine is a safe and very effective antipsychotic. In a study by Tiihonen et al,12 clozapine was associated with significantly lower mortality compared to other antipsychotics. As clozapine remains underutilized in many patients with treatment-resistant schizophrenia, practitioners should strive to find ways to further improve patient safety by focusing on the reduction of myocarditis incidence. On the basis of these data, a more stringent monitoring protocol, including CRP and troponin I/T, should be recommended during the first month of clozapine therapy.
References
1. Rashmi N, Mark D. Schizophrenia symptoms, patterns and statistics and patterns. MentalHelp.net website. https://www.mentalhelp.net/articles/schizophrenia-symptoms-patterns-and-statistics-and-patterns/. Accessed August 29, 2018.
2. Caspi A, Davidson M, Tamminga CA. Treatment-refractory schizophrenia. Dialogues Clin Neurosci. 2004;6(1):61-70. PubMed
3. Chakos M, Lieberman J, Hoffman E, et al. Effectiveness of second-generation antipsychotics in patients with treatment-resistant schizophrenia: a review and meta-analysis of randomized trials. Am J Psychiatry. 2001;158(4):518-526. PubMed CrossRef
4. Alvir JMJ, Lieberman JA, Safferman AZ, et al. Clozapine-induced agranulocytosis. Incidence and risk factors in the United States. N Engl J Med. 1993;329(3):162-167. PubMed CrossRef
5. Ronaldson KJ, Fitzgerald PB, McNeil JJ. Clozapine-induced myocarditis, a widely overlooked adverse reaction. Acta Psychiatr Scand. 2015;132(4):231-240. PubMed CrossRef
6. Clozapine [package insert]. East Hanover, NJ: Novartis Pharmaceuticals Corporation; 2015.
7. De Berardis D, Serroni N, Campanella D, et al. Update on the adverse effects of clozapine: focus on myocarditis. Curr Drug Saf. 2012;7(1):55-62. PubMed CrossRef
8. Miller LJ, Grande RE. Clozapine-induced myocarditis may warrant cardiac monitoring protocol. Ment Health Clin [Internet]. 2015;5(2):82-87. CrossRef
9. Ronaldson KJ, Taylor AJ, Fitzgerald PB, et al. Diagnostic characteristics of clozapine-induced myocarditis identified by an analysis of 38 cases and 47 controls. J Clin Psychiatry. 2010;71(8):976-981. PubMed CrossRef
10. Ronaldson KJ, Fitzgerald PB, McNeil JJ. Evolution of troponin, C-reactive protein and eosinophil count with the onset of clozapine-induced myocarditis. Aust N Z J Psychiatry. 2015;49(5):486-487. PubMed CrossRef
11. Ronaldson KJ, Fitzgerald PB, Taylor AJ, et al. A new monitoring protocol for clozapine-induced myocarditis based on an analysis of 75 cases and 94 controls. Aust N Z J Psychiatry. 2011;45(6):458-465. PubMed CrossRef
12. Tiihonen J, Lönnqvist J, Wahlbeck K, et al. 11-year follow-up of mortality in patients with schizophrenia: a population-based cohort study (FIN11 study). Lancet. 2009;374(9690):620-627. PubMed CrossRef
aFulton State Hospital Pharmacy, Fulton, Missouri
Potential conflicts of interest: None.
Funding/support: None.
Patient consent: Consent was obtained from the patient to publish this report, and information has been de-identified to protect anonymity.
Published online: October 11, 2018.
Prim Care Companion CNS Disord 2018;20(5):17l02256
To cite: Deardorff OG, Conklin TM, Hopkins TM, et al. Clozapine-induced myocarditis: the heartfelt silent assassin. Prim Care Companion CNS Disord. 2018;20(5):17l02256.
To share: https://doi.org/10.4088/PCC.17l02256
© Copyright 2018 Physicians Postgraduate Press, Inc.
Enjoy this premium PDF as part of your membership benefits!