Objective: To examine among trauma survivors several potential suicide risk factors, some of which have never been studied in this population (eg, DSM-5 posttraumatic stress disorder [PTSD] symptoms, benzodiazepines).
Methods: Using a cross-sectional self-report survey methodology in a consecutive sample of adult outpatients with trauma (N = 480), we examined relationships between suicide attempts and demographics, trauma types, PTSD symptoms, substance-related problems, and benzodiazepine prescriptions. The study was conducted from October 2014 to February 2015.
Results: PTSD diagnosis was significantly correlated with suicide attempt prevalence (adjusted odds ratio [AOR] = 2.6) and was the variable most strongly associated with the number of attempts among participants with at least 1 suicide attempt. PTSD symptom severities (total, cluster, and all but 3 individual symptoms) significantly correlated with attempted suicide; recklessness (AOR = 1.7), anhedonia (AOR = 1.7), and negative beliefs (AOR = 1.6) were most strongly correlated. Mood/cognitive alterations—a cluster new to the DSM-5—were particularly associated with suicide attempts (AOR = 3.2). Childhood maltreatment was strongly associated with attempted suicide; childhood physical abuse (AOR = 2.9) was the only trauma type significantly correlated with suicide attempts after adjustment for multiple testing. Attempted suicide was significantly correlated with substance-related problems in general (AOR = 2.6) and alcohol specifically (AOR = 2.9).
Conclusions: As predicted, suicide attempts correlated with PTSD symptom severity, childhood maltreatment, and substance-related problems. Our hypothesized correlation between suicide and benzodiazepine prescriptions was in part explained by PTSD symptom severity.
Which Posttraumatic Stress Disorder Symptoms,
Trauma Types, and Substances Correlate
With Suicide Attempts in Trauma Survivors?
ABSTRACT
Objective: To examine among trauma survivors several potential suicide risk factors, some of which have never been studied in this population (eg, DSM-5 posttraumatic stress disorder [PTSD] symptoms, benzodiazepines).
Methods: Using a cross-sectional self-report survey methodology in a consecutive sample of adult outpatients with trauma (N = 480), we examined relationships between suicide attempts and demographics, trauma types, PTSD symptoms, substance-related problems, and benzodiazepine prescriptions. The study was conducted from October 2014 to February 2015.
Results: PTSD diagnosis was significantly correlated with suicide attempt prevalence (adjusted odds ratio [AOR] = 2.6) and was the variable most strongly associated with the number of attempts among participants with at least 1 suicide attempt. PTSD symptom severities (total, cluster, and all but 3 individual symptoms) significantly correlated with attempted suicide; recklessness (AOR = 1.7), anhedonia (AOR = 1.7), and negative beliefs (AOR = 1.6) were most strongly correlated. Mood/cognitive alterations—a cluster new to the DSM-5—were particularly associated with suicide attempts (AOR = 3.2). Childhood maltreatment was strongly associated with attempted suicide; childhood physical abuse (AOR = 2.9) was the only trauma type significantly correlated with suicide attempts after adjustment for multiple testing. Attempted suicide was significantly correlated with substance-related problems in general (AOR = 2.6) and alcohol specifically (AOR = 2.9).
Conclusions: As predicted, suicide attempts correlated with PTSD symptom severity, childhood maltreatment, and substance-related problems. Our hypothesized correlation between suicide and benzodiazepine prescriptions was in part explained by PTSD symptom severity.
Prim Care Companion CNS Disord 2017;19(5):17m02177
https://doi.org/10.4088/PCC.17m02177
© Copyright 2017 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Wright State University, Dayton, Ohio
bBoonshoft School of Medicine, Wright State University, Dayton, Ohio
cSchool of Medicine, Case Western Reserve University, Cleveland, Ohio
d35th Mental Health Flight, Misawa Air Base, Misawa, Aomori, Japan
*Corresponding author: Jeffrey Guina, MD, Department of Psychiatry, Wright State University, 627 S Edwin C. Moses Blvd, Dayton, OH 45417 ([email protected]).
An unfortunately common sequela of trauma, suicide is more prevalent in posttraumatic stress disorder (PTSD) than in other anxiety disorders,1 and PTSD diagnosis predicts suicide attempts among ideators.2 PTSD compounds the effect of depression-related suicidality,3 but PTSD also predicts suicidality independent of comorbidities.4,5 Although some suicide studies5–11 evaluate PTSD symptom clusters, only one known study12 has investigated associations between each individual PTSD symptom and suicidality. While these previous studies used DSM-IV criteria, to the authors’ knowledge, ours is the first to examine DSM-513 PTSD symptoms. We hypothesized (H1) that suicide attempts are associated with worse PTSD symptom severity, particularly mood/cognitive symptoms, recklessness, avoidance, and flashbacks. These symptoms each include a quality of escape (eg, conscious avoidance, reckless reward-seeking to escape distress, dissociative symptoms such as flashbacks, amnesia, emotional numbness, and detachment), consistent with the escape theory of suicide in which symptoms and behaviors are used to avoid negative effects.14,15 Furthermore, mood/cognitive symptoms may indicate comorbid depression, guilt, shame, hopelessness, and a sense of foreshortened future, which have been shown to mediate the association of PTSD with suicidality.12,16–18 Suicidality may function to self-treat dissociative symptoms or punish one’s self due to guilt.19 Finally, recklessness may indicate impulsive reward-seeking or a disregard for one’s own safety similar to or predictive of suicidality,20–22 suggestive of the reward deficiency theory of suicide in which reward and pleasure dysfunctions lead to seeking unnatural and unhealthy rewards.23
Among trauma types, child abuse and assaults have been associated with the highest suicide attempt rates among PTSD patients.10,24,25 Sexual traumas are generally associated with higher rates of PTSD and suicide attempts than other trauma types,26,27 particularly childhood sexual abuse.2,28 We hypothesized (H2) that interpersonal traumas such as child abuse and sexual trauma are particularly associated with suicide attempts. That interpersonal traumas increase suicide risk is consistent with the interpersonal theory of suicide,29 which posits that traumatic experiences (particularly in childhood) can lead to fearlessness and pain insensitivity (which may correspond with the PTSD symptom recklessness) and thwarted belongingness (which may correspond with mood/cognitive symptoms such as detachment and anhedonia) that can contribute to suicidality.
Several studies2 have examined substance use as a risk factor for suicidality. Substance use is particularly concerning in trauma patients (with and without PTSD) in whom substance use disorders are commonly comorbid30 and have been found to increase suicide risk.8 We hypothesized (H3) that substance-related problems correlate with suicide attempts in trauma patients. Use of the numbing, sedating, or euphoric effects of substances to avoid trauma-related distress is consistent with both the escape theory and reward deficiency theory, and the disinhibiting and fear- and pain-reducing effects of many substances are consistent with the interpersonal theory of suicide. Due to their similar effects (ie, numbing, sedating, disinhibiting, fear-reducing), we also hypothesize (H4) that benzodiazepine prescriptions correlate with suicide attempts. This theory is consistent with preliminary findings that benzodiazepines can cause or worsen depression and suicidality,31,32 although the latter has never before been studied specifically in trauma patients.
METHODS
Participants
This study was approved by the Wright-Patterson Medical Center Institutional Review Board. Participants were nonemergent outpatients at a military medical center treating active duty and retired service members and dependents. During clinic hours, investigators approached consecutive incoming patients following registration and informally assessed exclusion criteria (ie, under 18 years old or in apparent physical or psychological distress). Participants were asked to complete anonymous surveys and place them into sealed envelopes in a collection box in the lobby. Consent was implied by survey completion as explained on a cover page containing the purpose and risks of the study as well as institutional review board contact information, which participants were encouraged to keep.
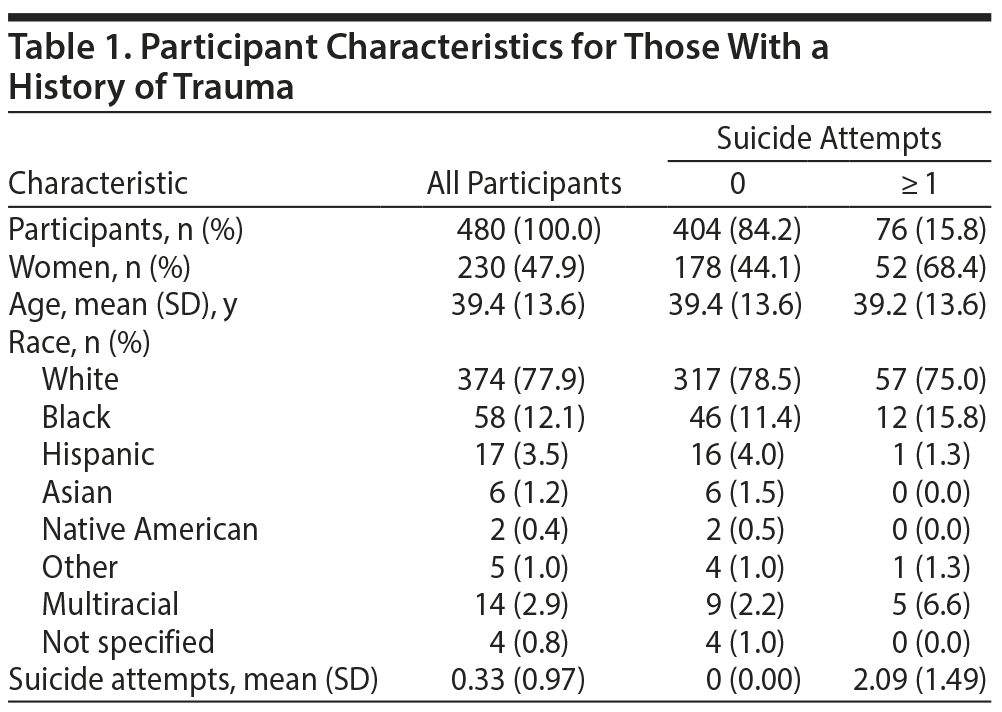
Of 1,000 surveys distributed, 768 (76.8%) were returned with sections completed about suicide attempts and PTSD symptoms. Of these, 480 (62.5%) reported a trauma history and were included in the study. Participant characteristics are described in Table 1. Between those with at least 1 suicide attempt and those with none, there were no significant differences in age (P = .9129) or race (P = .3201), but women were significantly more likely to attempt suicide than men (P = .0001). Regarding military status, 46.2% were active duty, 24.0% were dependents, 21.9% were retired, 5.8% marked “other” (eg, nonactive reserves, nonretired separated), and 2.1% did not respond. Regarding trauma type, participants reported witnessed violence (37.3%), life-threatening injury or illness (34.6%), combat (29.6%), physical assault (24.2%), sexual assault (23.1%), childhood sexual abuse (18.3%), severe motor vehicle collision (17.9%), childhood physical abuse (17.7%), natural disaster (14.0%), childhood neglect (13.1%), violent death of a loved one (13.1%), and terrorism (11.9%).
Measures
The survey assessed PTSD symptoms using the PTSD Checklist for the DSM-5 (PCL-5),33 a commonly used 20-item self-report measure with strong reliability and validity. The rest of the survey contained questions based on the DSM-513 inquiring about demographics; suicide attempts (measured by a single yes/no item that asked “Have you ever attempted suicide?” followed by “If yes, how many times?”); the DSM-5 trauma definition with 12 trauma types (listed in Table 2) and a write-in section; difficulty in controlling use of or social/occupational/legal/medical problems due to alcohol, tobacco, or illicit drugs; and current and past benzodiazepine prescriptions (with a list of those available in the United States). Participants were considered to meet DSM-5 PTSD criteria (n = 164, 34.2%) if reporting a trauma history and at least moderate severity (2–4 on a 0–4 scale) of ≥ 1 intrusive, ≥ 1 avoidance, ≥ 2 mood/cognitive, and ≥ 2 hyperarousal symptoms.
Statistical Analysis
We tested for associations between the explanatory variables described above and having ever attempted suicide using logistic regression, adjusted for sex, age, and race. We tested for associations between explanatory variables and “number of suicide attempts – 1” among those with at least 1 suicide attempt using Poisson regression. Strengths of association are presented as adjusted odds ratios (AORs) for logistic and adjusted ratios of mean outcomes (RADJ) for Poisson regression: for dichotomous variables, comparing those with and without explanatory variables; for total/cluster PTSD symptom severities, comparing predicted prevalence and means at the 75th and 25th severity percentiles (the choice of percentiles is for presentation purposes and does not impact significance tests); and for individual PTSD symptom severities, corresponding to a 1-unit increase in severity (0–4).
Analyses were performed in R 3.1.2.34 Significance tests were 2-sided, and the Hommel method in SAS 9.4 PROC MULTTEST was used to adjust for multiple testing across all analyses to preserve a familywise α = .05 level of significance. P values presented below are Hommel-adjusted.
RESULTS
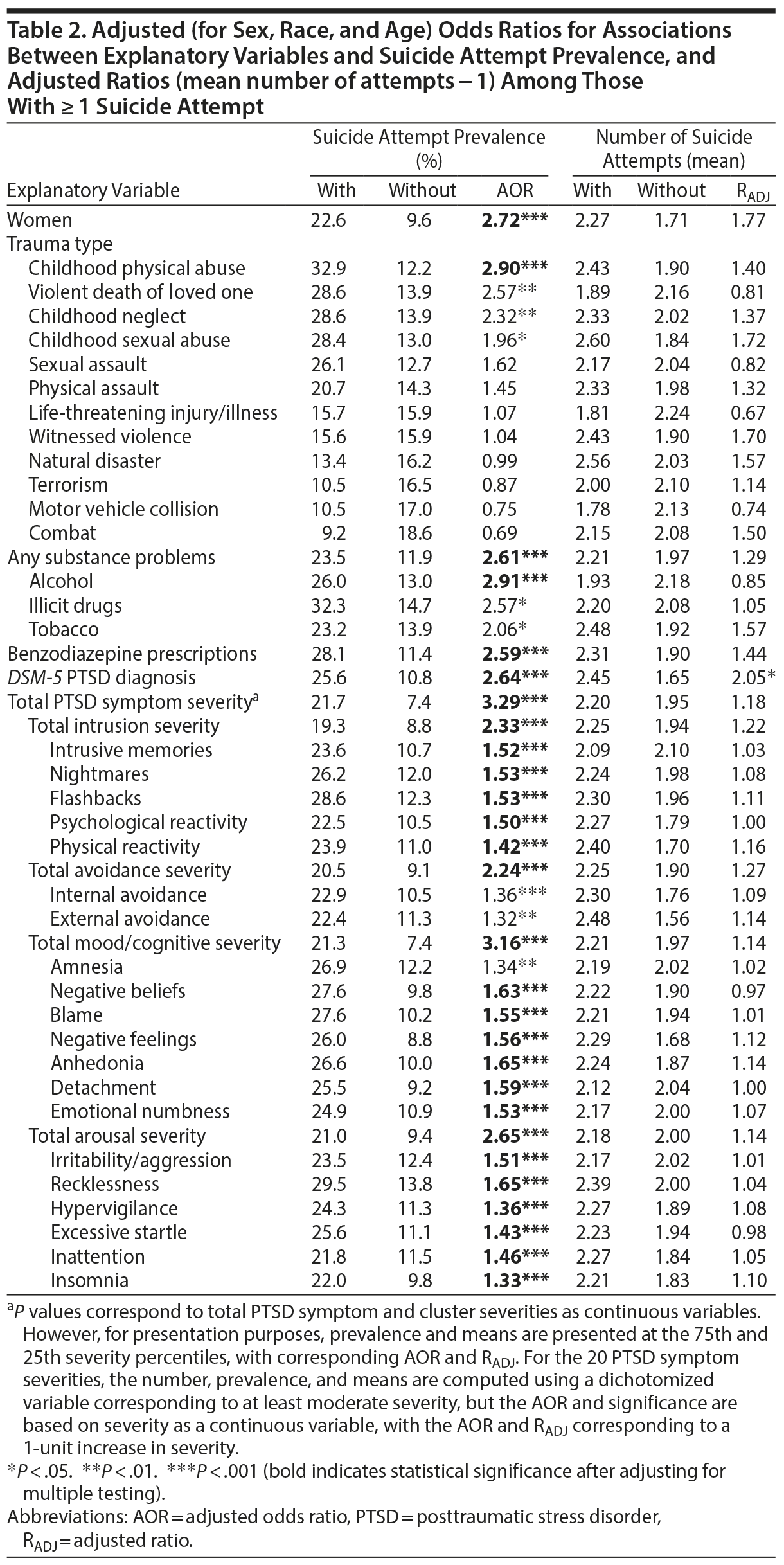
Table 2 summarizes associations between explanatory variables and suicide attempts.
PTSD Symptoms (H1)
Suicide attempts were significantly associated with worse total PTSD symptom severity (AOR = 3.29, P < .0001), DSM-5 PTSD diagnosis (AOR = 2.64, P = .0128), each PTSD symptom cluster, and all but 3 individual PTSD symptoms (amnesia, internal avoidance, and external avoidance were significant before but not after adjusting for multiple testing). Among those with at least 1 attempt, PTSD diagnosis (RADJ = 2.45) was the only variable significantly correlated with number of attempts before adjusting for multiple testing (P = .0309), but it was not significant after adjustment.
Trauma Type (H2)
Four trauma types significantly correlated with attempted suicide before adjusting for multiple testing: childhood physical abuse (AOR = 2.90, P = .0002), violent death of a loved one (AOR = 2.57, P = .0037), childhood neglect (AOR = 2.32, P = .0099), and childhood sexual abuse (AOR = 1.96, P = .0246). Childhood physical abuse (P = .0128) continued to be significantly associated with attempted suicide after multiple-testing adjustment. Sexual assault and combat correlated with suicide attempts positively and negatively, respectively, but not significantly after adjusting for sex, age, and race.
Substance-Related Problems (H3)
Suicide attempts significantly correlated with substance-related problems (AOR = 2.6, P = .0003; 2.9 for alcohol, 2.6 for illicit drugs, 2.1 for tobacco), but only with any substance problem (AOR = 2.61, P = .0189) and alcohol problems (AOR = 2.91, P = .0128) after adjusting for multiple testing.
Benzodiazepine Prescriptions (H4)
Benzodiazepine prescriptions (AOR = 2.59, P = .0006) significantly correlated with suicide attempts.
DISCUSSION
PTSD Symptom Severity Correlates
With Suicide Attempts (H1)
DSM-5 PTSD diagnosis and most PTSD symptom severities were associated with attempted suicide, and the former was the strongest correlate of number of attempts. Anhedonia, recklessness, and negative beliefs were the PTSD symptoms most strongly associated with suicide attempts—2 mood/cognitive symptoms, and the latter 2 new to DSM-5. These 3 symptom correlations may support the interpersonal theory of suicide,29,35 since recklessness can indicate fearlessness and pain insensitivity, and anhedonia (eg, decreased social interest) and negative beliefs (eg, “The world is dangerous,” “I am broken,” and “Life will never get better” resulting in social isolation) can lead to thwarted belongingness and perceived burdensomeness. Correlations with anhedonia (lack of reward) and recklessness (risky reward-seeking) may also support the reward deficiency theory of suicide.23 Our finding about negative beliefs is consistent with the only previous study12 of individual PTSD symptoms, which correlated suicidality with a sense of foreshortened future—a DSM-IV PTSD symptom subsumed by the DSM-5 symptom negative beliefs.
While previous studies found reexperiencing,6,9,11,12 avoidance/numbing,9,10 and arousal7,11 to be the DSM-IV clusters most associated with suicidality, our study found all DSM-5 clusters to be significantly correlated but especially highlighted mood/cognitive symptoms as a major risk factor for suicide (ie, the largest discrepancy among clusters, and 6 of the 7 strongest individual correlations were in this cluster). This is a novel finding, as the mood/cognitive cluster was created by DSM-5. This finding is supported by previous studies that found suicidality in trauma patients was associated with both the PTSD “numbing cluster” (ie, detachment and numbness segregated from the DSM-IV avoidance/numbing cluster)5,8 and the major depressive disorder “cognitive-affective cluster” (ie, depressed mood, guilt),5 which together nearly approximates the DSM-5 mood/cognitive cluster. The importance of mood/cognitive symptoms in suicide risk may support the idea that self-harm—which arguably includes suicidality, recklessness, and substance use—may serve the function of self-treating numbing (such as emotional numbness, detachment, and anhedonia) or punishing one’s self (possibly due to PTSD symptoms such as self-blame and negative feelings or beliefs about one’s self).19
Child Maltreatment Correlates
With Suicide Attempts (H2)
As predicted, child traumas (ie, physical abuse, sexual abuse, neglect) were the trauma types most correlated with attempted suicide; physical abuse was significantly associated after adjusting for multiple testing. While we cannot determine causation based on our study, our data support our hypothesis and previous research24,28,36,37 suggesting that child abuse is a unique predictor of suicidality with child trauma preceding suicidality. Sexual trauma (our other hypothesized predictor) had mixed findings: childhood sexual abuse was strongly associated with suicide attempts, and while sexual assault was significantly associated with suicide attempts when unadjusted, the association was largely explained by gender (just as combat was in the reverse direction). The relationship between child abuse and suicide, which has been found to be only partially mediated by mental disorders, is thought to be explained by the intrusive physical nature of the trauma that increases the survivor’s perception of severity or shared risk factors (eg, genetic, environmental, personality) that may predispose individuals to both trauma and suicidality.24,37 Our findings that child abuse is particularly associated with suicide attempts relative to other trauma types also further supports the interpersonal theory of suicide.29
Substance-Related Problems
Correlate With Suicide Attempts (H3)
Problems with any substance were significantly associated with attempted suicide, with alcohol-related problems being more associated than illicit drugs or tobacco. Substance use is known to have strong associations with suicide in the general population38 and depressed patients,39 and our data highlight the importance in trauma survivors specifically. Potential explanations are most likely bidirectional (eg, suicidal individuals may be more likely to “self-medicate” with substances,40 and substances may cause or worsen depression, disinhibition, and PTSD symptoms that can increase suicidality).31 Nevertheless, substance problems are a well-known suicide risk factor, and these findings support our hypothesis and several possible theories of suicide including escape,14 reward deficiency,23 and the interpersonal theory.29
Benzodiazepine Prescriptions
Correlate With Suicide Attempts (H4)
As predicted, current or past benzodiazepine prescriptions were strongly associated with suicide attempts. Sedatives have been found to be a suicide risk factor in general populations,32,41,42 even when adjusting for mental disorders.43 Proposed mechanisms for benzodiazepine-induced suicidality include depressogenic effects, disinhibition, confusion, amnesia, hallucinations, paranoia, and parasomnias.31,42 In trauma patients specifically, benzodiazepines have been linked with worse PTSD severity, depression, substance use, and disinhibition,31 which could all potentially contribute to suicidality. We hypothesize that prescribed benzodiazepines—even when not misused—can increase suicide risk. Alcohol (which had the strongest association with suicide attempts relative to other substance categories and a strong evidence base as a suicide risk factor in previous research38,39) has similar effects as benzodiazepines, which supports benzodiazepines as a suicide risk factor due to their similar mechanism of action (directly increasing suicide risk) and cross-tolerance (indirectly increasing risk by leading some benzodiazepine users to supplement use with the more available alcohol and some alcohol users to be prescribed benzodiazepines to treat alcohol-induced symptoms such as anxiety and insomnia).44 The correlation between benzodiazepines and suicide attempts may be bidirectional (eg, use could result in depressogenic effects, disinhibition, avoidance, disrupted sleep architecture, or iatrogenic addiction, and suicidal individuals may seek prescriptions for intentional overdose) or confounded (eg, benzodiazepines are more likely to be prescribed for more severe PTSD symptoms, which correlate with suicidality, and prescriptions are more likely to be sought by substance users who are more likely to attempt suicide). To this end, we performed a post hoc analysis: after adjusting for total PTSD symptom severity, benzodiazepine prescriptions were positively associated with attempted suicide (AOR = 1.72) but not significantly so. While this finding may indicate benzodiazepines are simply a marker of PTSD symptom severity, it may be explained by benzodiazepines also or instead being a contributor to PTSD symptom severity (ie, benzodiazepines could cause or worsen some symptoms in some individuals which, in turn, increases suicide risk). Since this is the first study to evaluate the association between benzodiazepines and suicide in trauma patients, we recommend future studies try to elucidate these findings. Nevertheless, benzodiazepines should be avoided or used with caution in PTSD patients, especially because they have little to no evidence of efficacy and the potential to worsen PTSD.31
Suicide Attempts Are More
Common in Traumatized Women
Women were significantly more likely to have attempted suicide than men among those with trauma, consistent with several previous studies45 in the general population. This finding may relate to the higher likelihood for women to have stress-related internalizing symptoms (eg, depression, anxiety, self-harm) than men (who are more likely to externalize, eg, recklessness, irritability, substance use) or sexual traumas46; however, in our sample this gender difference remained after adjusting for sexual trauma.
Limitations
Potential limitations of this study include a cross-sectional approach, self-report reliability, generalizability (our sample is a military and clinical population), investigator-designed questions (besides the PCL-5), and survivor bias (ie, men are more likely to complete suicide than women). We attempted to improve self-report reliability with anonymous surveys and, because of inconsistencies in how participants determine what constitutes a trauma,46 by providing the DSM-5 definition of trauma in the survey. Additionally, the cross-sectional nature of the study limits us from determining the relative timing of suicide attempts and variables (eg, if trauma preceded attempts, if substance use was contemporaneous with attempts). Strengths of this study include use of current diagnostic criteria, large total sample size, and identification of trauma survivors from a larger clinical sample (rather than starting with a sample of self-identified trauma or PTSD patients). We believe our findings—particularly novel findings about DSM-5 symptoms and benzodiazepines (both of which have never been studied before in relationship to suicide in trauma survivors)—warrant further research for generalizability to other populations, for determination of causation, for assessment of ideations and completions as well as attempts,2 and to examine if screening particular symptoms and specifically targeting them with treatment can reduce suicide risk.
CONCLUSIONS
In conclusion, this study supports our hypotheses that suicide attempts correlate with worse PTSD symptom severities (particularly mood/cognitive alterations and recklessness), childhood maltreatment (particularly physical abuse), and substance-related problems (particularly alcohol). Our hypothesized correlation between suicide and benzodiazepine prescriptions was in part explained by PTSD symptom severity.
Submitted: June 10, 2017; accepted July 28, 2017.
Published online: October 26, 2017.
Potential conflicts of interest: None.
Funding/support: None.
REFERENCES
1. Sareen J, Houlahan T, Cox BJ, et al. Anxiety disorders associated with suicidal ideation and suicide attempts in the National Comorbidity Survey. J Nerv Ment Dis. 2005;193(7):450–454. PubMed CrossRef
2. May AM, Klonsky ED. What distinguishes suicide attempters from suicide ideators? a meta-analysis of potential factors. Clin Psychol Sci Pract. 2016;23(1):5–20. CrossRef
3. Oquendo MA, Friend JM, Halberstam B, et al. Association of comorbid posttraumatic stress disorder and major depression with greater risk for suicidal behavior. Am J Psychiatry. 2003;160(3):580–582. PubMed CrossRef
4. Sareen J, Cox BJ, Stein MB, et al. Physical and mental comorbidity, disability, and suicidal behavior associated with posttraumatic stress disorder in a large community sample. Psychosom Med. 2007;69(3):242–248. PubMed CrossRef
5. Guerra VS, Calhoun PS, Mid-Atlantic Mental Illness Research Education and Clinical Center Workgroup. Examining the relation between posttraumatic stress disorder and suicidal ideation in an OEF/OIF veteran sample. J Anxiety Disord. 2011;25(1):12–18. PubMed CrossRef
6. Bell JB, Nye EC. Specific symptoms predict suicidal ideation in Vietnam combat veterans with chronic post-traumatic stress disorder. Mil Med. 2007;172(11):1144–1147. PubMed CrossRef
7. Ben-Ya’acov Y, Amir M. Posttraumatic symptoms and suicide risk. Pers Individ Dif. 2004;36(6):1257–1264. CrossRef
8. Hellmuth JC, Stappenbeck CA, Hoerster KD, et al. Modeling PTSD symptom clusters, alcohol misuse, anger, and depression as they relate to aggression and suicidality in returning US veterans. J Trauma Stress. 2012;25(5):527–534. PubMed CrossRef
9. Kotler M, Iancu I, Efroni R, et al. Anger, impulsivity, social support, and suicide risk in patients with posttraumatic stress disorder. J Nerv Ment Dis. 2001;189(3):162–167. PubMed CrossRef
10. Lemaire CM, Graham DP. Factors associated with suicidal ideation in OEF/OIF veterans. J Affect Disord. 2011;130(1–2):231–238. PubMed CrossRef
11. Tarrier N, Gregg L. Suicide risk in civilian PTSD patients—predictors of suicidal ideation, planning and attempts. Soc Psychiatry Psychiatr Epidemiol. 2004;39(8):655–661. PubMed CrossRef
12. Selaman ZM, Chartrand HK, Bolton JM, et al. Which symptoms of post-traumatic stress disorder are associated with suicide attempts? J Anxiety Disord. 2014;28(2):246–251. PubMed CrossRef
13. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. Fifth Edition. Arlington, VA: American Psychiatric Association; 2013:271–280.
14. Baumeister RF. Suicide as escape from self. Psychol Rev. 1990;97(1):90–113. PubMed CrossRef
15. Chatard A, Selimbegovic L. When self-destructive thoughts flash through the mind: failure to meet standards affects the accessibility of suicide-related thoughts. J Pers Soc Psychol. 2011;100(4):587–605. PubMed CrossRef
16. Bryan CJ, Morrow CE, Etienne N, et al. Guilt, shame, and suicidal ideation in a military outpatient clinical sample. Depress Anxiety. 2013;30(1):55–60. PubMed CrossRef
17. Hendin H, Haas AP. Suicide and guilt as manifestations of PTSD in Vietnam combat veterans. Am J Psychiatry. 1991;148(5):586–591. PubMed CrossRef
18. Panagioti M, Gooding PA, Pratt D, et al. An empirical investigation of suicide schemas in individuals with posttraumatic stress disorder. Psychiatry Res. 2015;227(2–3):302–308. PubMed CrossRef
19. Briere J, Gil E. Self-mutilation in clinical and general population samples: prevalence, correlates and functions. Am J Orthopsychiatry. 1998;68(4):609–620. PubMed CrossRef
20. Cheung YT, Wong PW, Lee AM, et al. Non-suicidal self-injury and suicidal behavior: prevalence, co-occurrence, and correlates of suicide among adolescents in Hong Kong. Soc Psychiatry Psychiatr Epidemiol. 2013;48(7):1133–1144. PubMed CrossRef
21. Guertin T, Lloyd-Richardson E, Spirito A, et al. Self-mutilative behavior in adolescents who attempt suicide by overdose. J Am Acad Child Adolesc Psychiatry. 2001;40(9):1062–1069. PubMed CrossRef
22. Sharhabani-Arzy R, Amir M, Ben-Ya’acov Y. Suicide risk, posttraumatic stress disorder symptoms, and personality style among battered women in Israel. Family Violence & Sexual Assault. 2002;18(1):15–22.
23. Elman I, Borsook D, Volkow ND. Pain and suicidality: insights from reward and addiction neuroscience. Prog Neurobiol. 2013;109:1–27. PubMed CrossRef
24. Belik S, Cox BJ, Stein MB, et al. Traumatic events and suicidal behavior: results from a national mental health survey. J Nerv Ment Dis. 2007;195(4):342–349. PubMed CrossRef
25. LeBouthillier DM, McMillan KA, Thibodeau MA, et al. Types and number of traumas associated with suicidal ideation and suicide attempts in PTSD: findings from a US nationally representative sample. J Trauma Stress. 2015;28(3):183–190. PubMed CrossRef
26. Darves-Bornoz JM, Choquet M, Ledoux S, et al. Gender differences in symptoms of adolescents reporting sexual assault. Soc Psychiatry Psychiatr Epidemiol. 1998;33(3):111–117. PubMed CrossRef
27. Kimerling R, Ouimette P, Wolfe J. Gender and PTSD. New York, NY: Guildford Press; 2002.
28. Ystgaard M, Hestetun I, Loeb M, et al. Is there a specific relationship between childhood sexual and physical abuse and repeated suicidal behavior? Child Abuse Negl. 2004;28(8):863–875. PubMed CrossRef
29. Van Orden K, Witte T, Cukrowicz KC. The interpersonal theory of suicide. Psychol Rev. 2010;117(2):575–600. PubMed CrossRef
30. Bailey KM, Stewart S. Relations among trauma, PTSD, and substance misuse: the scope of the problem. In: Ouimette P, Read JP, eds. Trauma and Substance Abuse: Causes, Consequences, and Treatment of Comorbid Disorders. 2nd ed. Washington, DC: American Psychological Association; 2014:11–34.
31. Guina J, Rossetter SR, DeRhodes BJ, et al. Benzodiazepines for PTSD: a systematic review and meta-analysis. J Psychiatr Pract. 2015;21(4):281–303. PubMed CrossRef
32. Dodds TJ. Prescribed benzodiazepines and suicide risk: a review of the literature. Prim Care Companion CNS Disord. 2017;19(2):16r02037. PubMed CrossRef
33. Blevins CA, Weathers FW, Davis MT, et al. The Posttraumatic Stress Disorder Checklist for DSM-5 (PCL-5): development and initial psychometric evaluation. J Trauma Stress. 2015;28(6):489–498. PubMed CrossRef
34. The R Foundation. The R Project for Statistical Computing. R Project website. http://www.R-project.org. Updated March 6, 2017. Accessed September 29, 2017.
35. Silva C, Hagan CR, Rogers ML, et al. Evidence for propositions of the interpersonal theory of suicide among a military sample. J Clin Psychol. 2016;73(6):1–6. PubMed CrossRef
36. Maniglio R. The role of child sexual abuse in the etiology of suicide and non-suicidal self-injury. Acta Psychiatr Scand. 2011;124(1):30–41. PubMed CrossRef
37. Wiederman MW, Sansone RA, Sansone LA. History of trauma and attempted suicide among women in a primary care setting. Violence Vict. 1998;13(1):3–9. PubMed
38. Miller NS, Mahler JC, Gold MS. Suicide risk associated with drug and alcohol dependence. J Addict Dis. 1991;10(3):49–61. PubMed CrossRef
39. Davis L, Uezato A, Newell JM, et al. Major depression and comorbid substance use disorders. Curr Opin Psychiatry. 2008;21(1):14–18. PubMed CrossRef
40. Lee J, Lee SW, Choi K, et al. Differential mediating effects of PTSD symptom clusters on alcohol use and sleep in university students with trauma experiences: a multi-group analysis. Pers Individ Dif. 2015;85:1–6. CrossRef
41. Pigeon WR, Woosley JA, Lichstein KL. Insomnia and hypnotic medications are associated with suicidal ideation in a community population. Arch Suicide Res. 2014;18(2):170–180. PubMed CrossRef
42. McCall WV, Benca RM, Rosenquist PB, et al. Hypnotic medications and suicide: risk, mechanisms, mitigation, and the FDA. Am J Psychiatry. 2016;174(1):18–25. PubMed CrossRef
43. Carlsten A, Waern M. Are sedatives and hypnotics associated with increased suicide risk of suicide in the elderly? BioMed Central Geriatrics. 2009;9:20. PubMed CrossRef
44. Pary R, Lewis S. Prescribing benzodiazepines in clinical practice. Resid Staff Physician. 2008;54(1):8–17.
45. Kessler RC, Borges G, Walters EE. Prevalence of and risk factors for lifetime suicide attempts in the National Comorbidity Survey. Arch Gen Psychiatry. 1999;56(7):617–626. PubMed CrossRef
46. Tolin DF, Foa EB. Sex differences in trauma and posttraumatic stress disorder: a quantitative review of 25 years of research. Psychol Trauma. 2008;S(1):37–85. CrossRef
Enjoy this premium PDF as part of your membership benefits!


