Prim Care Companion CNS Disord 2021;23(5):20br02996
To cite: Uvais NA, Moideen S, Babu F, et al. Depression and anxiety among patients with active COVID-19 infection: a cross-sectional study. Prim Care Companion CNS Disord. 2021;23(5):20br02996.
To share: https://doi.org/10.4088/PCC.20br02996
© Copyright 2021 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Iqraa International Hospital and Research Centre, Calicut, Kerala, India
bDepartment of Internal Medicine, Iqraa International Hospital and Research Centre, Calicut, Kerala, India
cSchool of Management Studies, Cochin University of Science and Technology, Kerala, India
dDepartment of Physical Medicine and Rehabilitation, Government Medical College, Kozhikode, India
eNandha College of Pharmacy, Erode, India
*Corresponding author: N. A. Uvais, MBBS, DPM, Iqraa International Hospital and Research Centre, Calicut, Kerala, India ([email protected]).
Coronavirus disease 2019 (COVID-19) caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) virus, initially diagnosed among a cluster of unexplained cases of pneumonia in Wuhan, China in late December 2019, has changed all aspects of human life drastically across the world.1 Apart from the morbidity and mortality associated with the virus, the infection control measures such as lockdown, travel restrictions, and social distancing also disrupted the social and economic lives of most of the world population. The rapid spread of the infection resulted in the collapse of the health care systems of many countries, and many patients died due to the lack of availability of medical support including hospital beds, oxygen, and ventilators.2 Studies3,4 have well documented a significant increase in the level of psychological distress among the general population as well as frontline workers during the COVID-19 pandemic. Research5 among the COVID-19 patient population also showed significant rates of psychological distress, probably due to biological as well as psychosocial factors. Neurotropism of SARS-CoV-2, isolation, quarantine, steroid exposure, medical complications during hospital stay, and stigma can be some of the causal factors for the higher psychological morbidity among patients with COVID-19.6 Currently, there are only a few epidemiologic studies7–9 exploring psychiatric morbidity among patients diagnosed with COVID-19. Moreover, most of the existing research employed an online survey design to study psychiatric morbidities among active as well as recovered patients with COVID-19 due to the social-distancing protocols in place to prevent the spread of infection. COVID-19–related mental health research is scarce in lower middle-income countries of Asia. In the present cross-sectional study, we explored the prevalence of anxiety and depression and its correlates in a COVID-19 patient population in south India.
Methods
This was a cross-sectional study conducted at a COVID-19 treatment facility managed by public-private partnership in south India. The study was approved by the hospital ethics committee. The study period was August 1, 2020, to September 30, 2020. Purposive sampling was used to recruit participants. Inclusion criteria were COVID-19–positive patients > 18 years of age who were clinically stable for the interview. Informed consent was taken from all participants. Sociodemographic and clinical details were collected according to a structured form. Medical records were reviewed to collect information about medical backgrounds, overall medical parameters of COVID-19, laboratory values, and treatment details.
The 7-item Generalized Anxiety Disorder Scale (GAD-7)10 is a scale used to assess anxiety symptoms. Total scores range from 0 to 21, with higher scores reflecting higher severity levels of anxiety. Cutoff points of 5, 10, and 15 are interpreted as representing mild, moderate, and severe levels of anxiety, respectively, on the GAD-7.
Depressive symptoms were measured using the 9-item Patient Health Questionnaire (PHQ-9),11 which includes 9 items with scores between 0 and 27. For the PHQ-9, scores of 5 to 9, 10 to 14, 15 to 19, and 20 to 27 corresponded to mild, moderate, moderately severe, and severe depression symptoms, respectively.
Data were analyzed with SPSS version 23.0 (IBM, Armonk, New York). Continuous variables were expressed as mean ± SD. Categorical variables were expressed as frequencies and percentages. An independent-sample t test was used to test for differences in continuous variables. χ2 was used to compare categorical variables. Differences were considered statistically significant if the P value was < .05.
Results
Among 154 participants, 45 (29.2%) were in the age group 18–30 years and 31–50 years, and 64 (41.6%) were > 50 years. Eighty (51.9%) participants were female. Fifteen (9.7%) and 38 (24.7%) patients had hospital and family exposure, respectively, and 101 patients (65.6%) had unknown exposure. Seventy-four (61.2%) participants were having symptoms of COVID-19, and 92 (59.7%) had comorbid medical illness. Also, 94.2% of the participants had no travel history, and 3.9% were working in the health care sector. Only 2 patients had any adverse clinical events during their hospital stay, and the majority of the patients (96.7%) were discharged after treatment. Of the patients, 9.7% had clinically significant depression, while 7.8% had mild, 1.3% had moderate, and 0.6% had severe depression. Also, 5.8% of the sample had clinically significant anxiety, while 5.2% had mild, and 0.6% had severe anxiety. The sociodemographic and clinical details are summarized in Table 1. There was a statistically significant association between clinically significant depression and being > 45 years of age (P = .032). There was a statistically significant association between clinically significant anxiety and a positive travel history (P = .006).
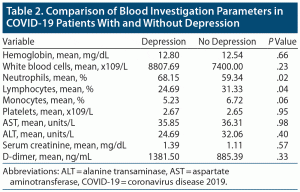
After comparing the white blood cell counts between COVID-19 patients with and without depression, results showed that the neutrophil count was higher in the depression group (mean=68.15%) than in the nondepression group (mean=59.34%) (P = .02). The lymphocyte count was significantly lower in the depression group (mean=24.69%) compared with the nondepression group (mean=31.33%) (P = .04). The details are summarized in Table 2. No statistically significant association was seen between clinically significant anxiety and blood parameters.
Discussion
This cross-sectional study explored the prevalence of anxiety and depression among 154 patients admitted to a COVID-19–designated hospital in south India. The questionnaire was applied face to face by trained staff after taking proper safety precautions. The results showed that 9.7% had clinically significant depression and 5.8% had clinically significant anxiety. The rates of depression and anxiety found in our study are significantly lower than those of previous published studies. Dai et al7 conducted a cross-sectional study of depression and anxiety among COVID-19–positive patients in Wuhan, China and found that the prevalence of anxiety and depressive symptoms was 18.6% and 13.4%, respectively. Another study from China by Chen et al8 also found that the prevalence of depression and anxiety was 21.0 and 16.4%, respectively. However, another study9 from Iran found that 97.2% of patients with COVID-19 had some degree of depression. The lower prevalence of depression and anxiety in our sample could be due to the following. Most of the previous studies employed an online survey design to study the prevalence of anxiety and depression among active patients with COVID-19 due to the pandemic disease prevention and control measures. Online survey studies were found to have serious methodological limitations, and respondents with biases may select themselves into the sample resulting in higher prevalence.12 A recent meta-analysis13 exploring the prevalence of anxiety and depression in South Asia during the COVID-19 pandemic among the general population reported that the pooled prevalence of anxiety and depression was relatively lower in India compared to other South Asian countries. Moreover, 38.8% of our study sample was asymptomatic, and they were admitted according to the government protocol at that point in time. The hospital where the study was conducted was set up in a public-private partnership in the district of Calicut by converting a running psychiatric hospital into a COVID-19 treatment facility. The hospital was well known in the district for its high-quality medical care at an affordable rate. Thus, admission to a trusted hospital setting might also have reduced the stress levels of the patients. The dedicated staff as well as the fully functioning communication facilities (mobile/landline), which patients can use freely to communicate with their loved ones, might also have played a role in reducing the psychiatric morbidities.
In conclusion, our study assessed the prevalence rates of clinically significant depression and anxiety among active hospitalized COVID-19 patients in India. The prevalence rates of depression and anxiety in our study are significantly less than previous studies from various parts of the world. Our findings show that a significant portion of patients with active COVID-19 infection has clinically significant depression and anxiety, which can persist or aggravate during the course of the illness. There is an urgent need to address the psychological needs of the COVID-19 patient population from the active phase of the illness itself.
Received: April 23, 2021.
Published online: September 16, 2021.
Potential conflicts of interest: None.
Funding/support: None.
References (13)

- Singhal T. A review of coronavirus disease-2019 (COVID-19). Indian J Pediatr. 2020;87(4):281–286. PubMed CrossRef
- Vincent JL, Taccone FS. Understanding pathways to death in patients with COVID-19. Lancet Respir Med. 2020;8(5):430–432. PubMed CrossRef
- Necho M, Tsehay M, Birkie M, et al. Prevalence of anxiety, depression, and psychological distress among the general population during the COVID-19 pandemic: a systematic review and meta-analysis [published online ahead of print April 1, 2021]. Int J Soc Psychiatry. PubMed CrossRef
- Sirois FM, Owens J. Factors associated with psychological distress in health-care workers during an infectious disease outbreak: a rapid systematic review of the evidence. Front Psychiatry. 2021;11:589545. PubMed CrossRef
- Banerjee D, Viswanath B. Neuropsychiatric manifestations of COVID-19 and possible pathogenic mechanisms: insights from other coronaviruses. Asian J Psychiatr. 2020;54:102350. PubMed CrossRef
- Szcześniak D, Gładka A, Misiak B, et al. The SARS-CoV-2 and mental health: from biological mechanisms to social consequences. Prog Neuropsychopharmacol Biol Psychiatry. 2021;104:110046. PubMed CrossRef
- Dai L-L, Wang X, Jiang T-C, et al. Anxiety and depressive symptoms among COVID-19 patients in Jianghan Fangcang Shelter Hospital in Wuhan, China. PLoS One. 2020;15(8):e0238416. PubMed CrossRef
- Chen Y, Huang X, Zhang C, et al. Prevalence and predictors of posttraumatic stress disorder, depression and anxiety among hospitalized patients with coronavirus disease 2019 in China. BMC Psychiatry. 2021;21(1):80. PubMed CrossRef
- Zandifar A, Badrfam R, Yazdani S, et al. Prevalence and severity of depression, anxiety, stress and perceived stress in hospitalized patients with COVID-19. J Diabetes Metab Disord. 2020;19(2):1–8. PubMed CrossRef
- Spitzer RL, Kroenke K, Williams JB, et al. A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med. 2006;166(10):1092–1097. PubMed CrossRef
- Kroenke K, Spitzer RL, Williams JB. The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med. 2001;16(9):606–613. PubMed CrossRef
- Andrade C. The limitations of online surveys. Indian J Psychol Med. 2020;42(6):575–576. PubMed CrossRef
- Li Y, Scherer N, Felix L, et al. Prevalence of depression, anxiety and post-traumatic stress disorder in health care workers during the COVID-19 pandemic: a systematic review and meta-analysis. PLoS One. 2021;16(3):e0246454. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!