aDepartment of Psychiatry, Iqraa International Hospital and Research Centre, Calicut, Kerala, India
*Corresponding author: N. A. Uvais, MBBS, DPM, Department of Psychiatry, Iqraa International Hospital and Research Centre, Calicut, Kerala, India ([email protected]).
Prim Care Companion CNS Disord 2021;23(3):20br02898
To cite: Uvais NA. Profile of patients attending a general hospital psychiatric clinic during lockdown in India: a retrospective study. Prim Care Companion CNS Disord. 2021;23(3):20br02898.
To share: https://doi.org/10.4088/PCC.20br02898
© Copyright 2021 Physicians Postgraduate Press, Inc.
The 2019 severe acute respiratory syndrome coronavirus 2 pandemic originated in Wuhan, China and spread to most countries across the world, with more than 73 million confirmed cases and 1.64 million deaths at the time of this writing.1 The first confirmed case of coronavirus disease 2019 (COVID-19) in India was documented on January 30, 2020 in the South Indian state of Kerala in an Indian national evacuated from China.2 At the time of this writing, there are more than 9.9 million confirmed cases in India.1 However, the Indian government took various measures to stop the spread of infection from the beginning of the pandemic. The control measures started with airport screening for COVID-19 infection among travelers, especially from China.3 The control measures culminated in a nationwide lockdown for 21 days starting on March 24, 2020.4 During the lockdown period, most of the government and private psychiatry outpatient services were closed to reduce the spread of the infection, making it difficult for patients with psychiatric illnesses to access psychiatric services. Considering the potential of the COVID-19 pandemic to induce psychiatric illness among the general population and the risk of deterioration of the mental states of patients already receiving treatment from the psychiatry department, our hospital continued outpatient psychiatry clinics and consultations after proper screening and taking adequate precautions. Very little is known regarding the impact of the strict nationwide lockdown on mental health and the reasons for which patients accessed mental health services during the lockdown, which required special permission from government authorities for travel. The purpose of this study was to explore the sociodemographic and clinical details of patients who attended an outpatient psychiatric clinic in our hospital to shed light on the impact of the pandemic and the needs of psychiatric patients during lockdown in South India.
Methods
In this retrospective study, digital records of psychiatric patients who attended the psychiatry outpatient department of a tertiary care hospital in South India during lockdown from March 24, 2020, to April 14, 2020 were analyzed. The sociodemographic and clinical details were retrieved from the digital records using a structured performa. The sociodemographic details included age, sex, and marital status. The clinical details collected were the psychiatric diagnosis made by the treating psychiatrist, any medical comorbidities, reason for consultation, and any documentation of COVID-19–related stress.
The collected data were evaluated in the SPSS 20.0 program. Descriptive statistics (mean, SD, frequency distribution) were computed for all demographic and clinical variables. A χ2 test was employed to assess if there was a significant association between categorical variables. A P value < .05 was considered statistically significant.
Results
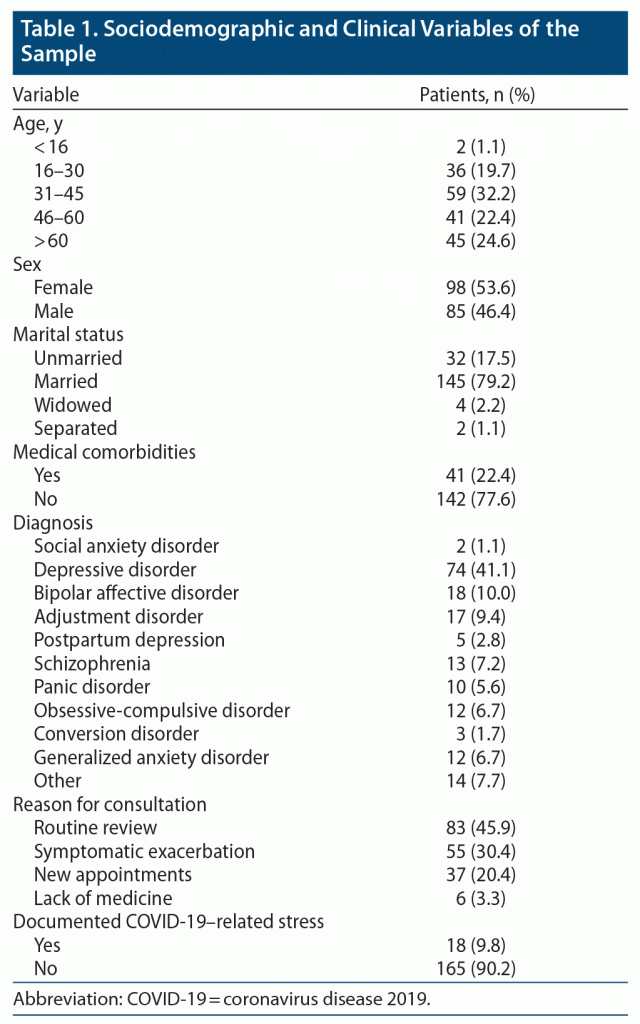
The analysis showed that 183 patients attended the psychiatric outpatient department during the lockdown period. The mean age of the patients was 45.97 years (SD = 17.24). Ninety-eight patients (53.6%) were women, 145 (79.2%) were married, and 41 (22.4%) had comorbid medical illness. The most common psychiatric diagnoses were depressive disorder (41.1%), bipolar affective disorder (10.0%), adjustment disorder (9.4%), and schizophrenia (7.2%). Eighty-three patients (45.9%) visited the clinic for routine review, 55 (30.4%) visited due to exacerbations in psychiatric symptoms, and 37 (20.4%) were new appointments. Significant COVID-19 pandemic–related stress was documented in 18 patients (9.8%). The sociodemographic and clinical details of the sample are summarized in Table 1.
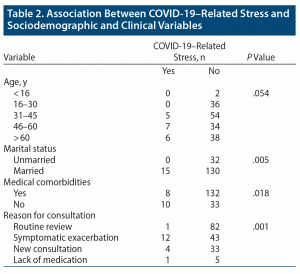
Among the new appointments, 4 patients (10.81%) had COVID-19–related stress as a precipitating factor for their psychiatric morbidity. Statistically significant higher COVID-19–related stress was found among the age group aged 46–60 years (P = .054), married patients (P = .005), and those with medical comorbidities (P = .018). There was a statistically significant association between symptomatic exacerbation as a reason for consultation and COVID-19–related stress (P = .001). The correlation between COVID-19–related stress and other variables is summarized in Table 2.
Discussion
The COVID-19 pandemic and related lockdown disrupted mental health care delivery in most countries. A recent survey5 by the World Health Organization found that significant disruption in critical mental health services occurred in 93% of countries worldwide. Although there was a clear warning from health authorities that a pandemic like COVID-19 could significantly increase demand for mental health services as isolation, bereavement, and financial crisis can trigger psychiatric illnesses or exacerbate existing ones, very few interventions were done to address this challenge, especially in developing countries. The current study results show that there was a real need for outpatient psychiatric services even during lockdown, as around 10 patients visited our clinic each working day after obtaining special permissions from government authorities.
The study findings show that 20.4% of the patients who attended the clinic during lockdown had new-onset psychiatric disorders. If there had been no functioning psychiatric outpatient clinic taking proper safety precautions against the virus during lockdown, it would have been difficult to help patients with new-onset psychiatric disorders during that time. Although the government legalized the practice of telepsychiatric services to mitigate the mental health crisis associated with COVID-19, such a rapid shift in care-seeking behavior is difficult for many patients. Those suffering from psychotic illnesses, belonging to a lower socioeconomic class, or living in a remote location may not utilize such telepsychiatric services due to clinical and logistic barriers.6
COVID-19–related stress was well documented in 18 patients (9.8%). Moreover, COVID-19–related stress was significantly higher among patients aged 46–60 years, those who were married, and those with medical comorbidities. Even from the beginning of the pandemic, it was known that COVID-19 infection has higher mortality among older patients with medical comorbidities.7 The older patients in our sample with medical comorbidities might have perceived COVID-19 as more dangerous than did the younger patients. Moreover, lockdown-related changes in lifestyle, especially closing of religious spaces, might have precipitated or exacerbated mental health problems in this population as reported in a previous case series8 from India.
Findings also showed a statistically significant association between consultation for exacerbation of existing mental health problems and COVID-19 pandemic–related stress, which is an expected finding. However, in the absence of regular psychiatric services, it would have been difficult for this group of patients to obtain proper psychiatric attention and treatment.
In conclusion, this study highlights the impact of the pandemic on patients with mental illness and the pattern and needs of patients attending a psychiatric clinic during the lockdown in India. In the absence of proper psychiatric services during the lockdown, it would have been difficult for patients to access mental health services, especially at a time when their mental health needs were expected to increase. In similar situations in the future, better strategies should be adopted to continue psychiatric services, while taking proper precautions to mitigate the associated mental health challenge and support vulnerable populations with psychiatric illnesses.
Received: December 17, 2020.
Published online: May 20, 2021.
Potential conflicts of interest: None.
Funding/support: None.
References (8)

- COVID-19 Coronavirus Pandemic. Worldometer. 2020. Accessed May 6, 2021. https://www.worldometers.info/coronavirus/#countries
- Andrews MA, Areekal B, Rajesh KR, et al. First confirmed case of COVID-19 infection in India: a case report. Indian J Med Res. 2020;151(5):490–492. PubMed CrossRef
- Responding to COVID-19—Learnings from Kerala. World Health Organization. Published July 2, 2020. Accessed May 6, 2021. https://www.who.int/india/news/feature-stories/detail/responding-to-covid-19---learnings-from-kerala
- Hebbar N. PM Modi announces 21-day lockdown as COVID-19 toll touches 12. The Hindu. Published March 24, 2020. Updated March 25, 2020. Accessed May 6, 2021. https://www.thehindu.com/news/national/pm-announces-21-day-lockdown-as-covid-19-toll-touches-10/article31156691.ece
- COVID-19 disrupting mental health services in most countries, WHO survey. World Health Organization. Published October 5, 2020. Accessed May 6, 2021. https://www.who.int/news/item/05-10-2020-covid-19-disrupting-mental-health-services-in-most-countries-who-survey
- Triana AJ, Gusdorf RE, Shah KP, et al. Technology literacy as a barrier to telehealth during COVID-19. Telemed J E Health. 2020;26(9):1118–1119. PubMed CrossRef
- Zhou F, Yu T, Du R, et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet. 2020;395(10229):1054–1062. PubMed CrossRef
- Uvais NA. Psychological impact of the COVID-19 pandemic among the elderly: a case series from India. Prim Care Companion CNS Disord. 2020;22(4):20com02675. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!