Circadian Synchronization Linked to a Successful Treatment in a Severely Depressed Adolescent
To the Editor: Circadian rhythm abnormalities have recently been considered a key factor to the onset and outcome of affective disorders.1,2 Circadian rhythm irregularities in depressed adults and adolescents have been reported by several authors.3,4 Blunted circadian amplitude or decreases of the 24-hour spectral power expressing weak entrainment to the 24-hour day are the main circadian rhythm dysfunctions observed in major depressive disorder (MDD) patients.4 MDD patients may also show reduced exposure to light and irregularity of daily social activity, also known as social rhythms, which are important cues for the synchronization to a 24-hour environmental cycle. Depressed adolescents spend less time in bright light and show low light exposure compared to healthy controls.5 Disruptions of social rhythms have also been associated with affective episodes.6
As the social rhythm theory predicts, any significant life event will disrupt social and biological rhythms and may lead to a depressive state or disorder in vulnerable individuals.7 Adolescents are more vulnerable to social rhythm disruptions due to a conflict between early morning school schedules and a tendency of the body to phase delay its biological rhythms. This tendency is attributed to an ontogenetic trend and is influenced by social activities such as late night social events.8
On the other hand, several strategies based on chronobiological principles such as strengthening temporal cues, or zeitgebers, by increasing exposure to light and stimulating social rhythm regularity are effective in synchronizing circadian rhythms and improving affective states. Moreover, agomelatine, a new antidepressant drug, has been considered effective due to its effects on circadian rhythms.9
Here, we describe a successful treatment of a severely depressed adolescent using antidepressants associated with strengthening of time cues. After we obtained signed informed consent forms from the parents, the patient’s current depression diagnosis was assessed through a face-to-face clinical interview with the patient and his parents separately and combined with the Brazilian version of the Schedule for Affective Disorders and Schizophrenia for School Aged Children: Present and Lifetime Version (K-SADS-PL).10 His depressive symptoms were evaluated with the Children’s Depression Rating Scale-Revised (CDRS-R)11 to assess clinical improvement and treatment response; the CDRS-R was administered weekly in the first 13 weeks and monthly until the end of the study. Data were collected for 51 consecutive weeks, from April 14, 2002, to April 5, 2003. The patient’s motor activity was recorded with a wrist actimeter, which is a small programmable activity monitor with a digital memory worn on the nondominant wrist. The time series were formed by 10-min periods and weeks beginning on Sundays. The data were submitted to Sokolov and Bushell’s periodogram algorithm using El Temps software (A. D×ez-Noguera, Barcelona, Spain; 1999) for the detection of the 24-hour spectral power. The patient’s motor activity was evaluated without any medication in the beginning of the study for 2 weeks and again at the end of the study from the 47th through the 51st week.
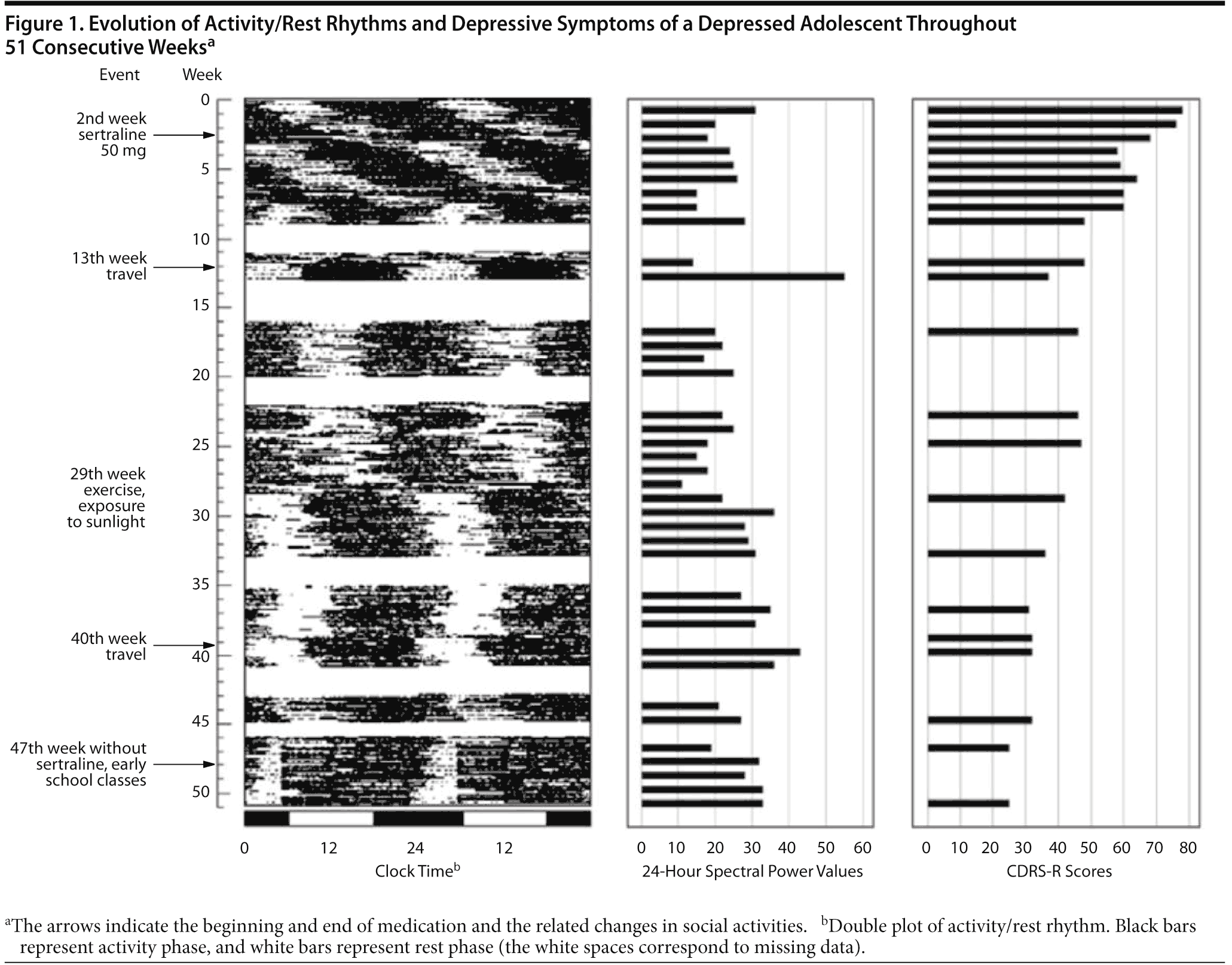
Case report. John, a 17-year-old white adolescent boy, was evaluated in April 2002; he presented with a family history of major depression and schizophrenia and with sleep problems since the age of 9 months. His depressive symptoms began when he was 15 years old after he did not seem well adjusted in a new school after moving to a new house. The symptoms worsened in the beginning of 2002 when his mother received a breast carcinoma diagnosis and he failed entrance exams to the university. At the index time, he presented with severe depressive symptoms: anhedonia, lack of energy, sleep complaints, irritability and morbid ideation, lack of interest in school, and social withdrawal behavior that resulted in his dropping out of school. He spent his nights playing computer games and slept during the day. His social interaction was therefore reduced to family contacts and remote computer playmates at night. He also reported left-eye diplopia, related to an idiopathic and transitory VI pair paresis causing visual difficulty, which was an additional factor causing isolation at home all the time (Figure 1).
In the first 12 weeks, he was severely depressed (DSM-IV major depressive disorder; CDRS-R score = 78) and his activity/rest rhythms showed a longer than 24-hour pattern with low 24-hour spectral power (SP) value of 20. Although he had taken an antidepressant (sertraline 50 mg) since the second week and his left-eye diplopia improved markedly, his depressive symptoms (CDRS-R score = 37) improved significantly only at the 13th week when his rhythms were strongly entrained (24-hour SP = 54) after traveling with his family to a nearby sea resort and exposing himself to sunlight and to physical exercise. When he returned, he became depressed again from the 16th to the 28th week (CDRS-R score = 46) and his activity/rest rhythms were less adjusted (24-hour SP = 11-24), with a phase delay of about 12 hours (concentrated activity at night). Since the 29th week, he has improved his affective state when he has exposed himself to sunlight and exercised after learning about the importance of these changes for synchronizing his rhythms. At the 40th week, when he traveled again with his family, his rhythms were better adjusted to the light/dark cycle, with a 24-hour SP of 43. As he had greatly improved, his medication was discontinued at the 47th week. Although from the 29th until the 51st week his depressive symptoms remitted (CDRS-R score < 40) and we observed an increase of 24-hour SP (26-36), his activity/rest rhythm showed an unstable pattern with a tendency to be active at night and large phase delays (up to 4 hours) on weekends after starting school early in the morning at the 47th week.
This report is the first published case evaluating changes in circadian rhythms, life events, and depressive symptoms during 1 year of a severely depressed adolescent with successful treatment. This case reinforces the relationship between life events, social and biological rhythm disturbances, and affective disorders.6 Moreover, these results suggested the importance of strengthening temporal cues to synchronize the rhythms and to improve depressive symptoms.3,9
Negative life events observed prior to onset of his symptoms might be considered important factors to trigger social and circadian rhythm irregularities and depressive state. Since John’s rhythms were monitored after the onset of symptoms, we could evaluate an association only between his activity/rest rhythm patterns and his depressive outcome. The unstable rhythm pattern with desynchronized, delayed phases and a 12-hour phase shift observed during his depressive state suggest a relationship between circadian dysfunctions and depressive symptoms. The late-night computer use might be an additional factor in his delays and approximate 12-hour phase shift.8 We are using the term desynchronized to qualify the longer-than-24-hour rest/activity rhythm instead of the expression free-running rhythm, which applies to controlled studies in which time cues have been abolished.12 In this case, time cues were also reduced, since he was more socially withdrawn and probably experienced reduced sunlight exposure as he slept during the day. Some researchers have postulated that depressive symptoms may lead to circadian dysfunction by reducing exposures to time cues.3. To date, the relationship between circadian dysfunction and a depressive state may be a bidirectional pathway.
The patient’s unstable rhythm patterns also might be considered a risk or a vulnerability factor for triggering depression. As he had sleep problems since 9 months of age and presented with highly unstable rhythmic patterns almost all the time, even when he was not depressed, we can suppose that he had a circadian disturbance prior to the depression onset. Probably, his later bed and wake times might express an extreme evening tendency noticed even in the early months of life that may have grown in adolescence.8 There is some evidence in the literature about a relationship between eveningness and affective disorders.13 Furthermore, extreme evening tendency was also associated with rhythm instability.14 His sleep phase delays on weekends observed when he began school early in the morning could be the result of a conflict between his evening tendency and early morning social demands. We may also observe that the adolescent sleep phase cycle shows an irregular pattern characterized by increased delays on weekends as a result of sleep deprivation during the week.15
A delay to improve depressive symptoms was reported by Teicher and colleagues16 in depressed children with circadian disturbance. Our patient became markedly better only when his rhythms were entrained after strengthening temporal cues such as sunlight exposure, physical exercise, and social relationships. In addition, antidepressant drugs also affect the circadian period, phase relationships, and enhanced circadian amplitude and sensitivity to zeitgebers.3,9 Psychotherapy might also help to improve his social relationships.17 In this respect, strengthening temporal cues should be a chronobiological strategy for successful depressive treatment in patients with circadian disturbance.18 Furthermore, therapies based on stimulating regularity of social rhythms, light/dark exposure, and sleep modifications have been reported to improve treatment of affective disorders.3,9
This case report suggests the importance of considering the interrelationship between circadian rhythms and affective disorders to amplify the underlying mechanisms involved in both rhythmic and affective disorders in order to support accurate diagnosis and successful treatments. Some limitations of this study should be considered: (1) the lack of other circadian rhythm analysis and ambient light profiles limits the discussion on synchronization mechanisms; (2) some activity data were not recorded when he took off the actimeter; and (3) as this was his first depressive episode, we can not exclude a bipolar outcome.
References
1. Harvey AG. Sleep and circadian functioning: critical mechanisms in the mood disorders? Annu Rev Clin Psychol. 2011;7(1):297-319. PubMed doi:10.1146/annurev-clinpsy-032210-104550
2. Kapczinski F, Frey BN, Vieta E. Sleep and circadian disturbances in bipolar disorders: an urgent need for objective assessment and systematic follow up. J Clin Psychiatry. 2011;72(5):724. doi:10.4088/JCP.11l06850
3. Wirz-Justice A. Chronobiology and mood disorders. Dialogues Clin Neurosci. 2003;5(4):315-325. PubMed
4. Teicher MH, Glod CA, Harper D, et al. Locomotor activity in depressed children and adolescents, 1: circadian dysregulation. J Am Acad Child Adolesc Psychiatry. 1993;32(4):760-769. PubMed doi:10.1097/00004583-199307000-00009
5. Armitage R, Hoffmann R, Emslie G, et al. Rest-activity cycles in childhood and adolescent depression. J Am Acad Child Adolesc Psychiatry. 2004;43(6):761-769. PubMed doi:10.1097/01.chi.0000122731.72597.4e
6. Grandin LD, Alloy LB, Abramson LY. The social zeitgeber theory, circadian rhythms, and mood disorders: review and evaluation. Clin Psychol Rev. 2006;26(6):679-694. PubMed doi:10.1016/j.cpr.2006.07.001
7. Ehlers CL, Kupfer DJ, Frank E. Biological rhythms and depression: the role of zeitgebers and zeitstöres. Depression. 1993;1(6):285-293. doi:10.1002/depr.3050010602
8. Louzada FM, Silva AGT, Peixoto CAT, et al. The adolescence sleep phase delay: causes, consequences and possible interventions. Sleep Science. 2008;1:49-53.
9. Kronfeld-Schor N, Einat H. Circadian rhythms and depression: human psychopathology and animal models. Neuropharmacology. 2012;62(1):101-114. Epub 2011 Aug 18. PubMed
10. Brasil HH. Desenvolvimento da Vers×£o Brasileira da Schedule for Affective Disorders and Schizophrenia for School Aged Children Present and Lifetime Version (K-SADS-PL) e Estudo de suas Propriedades Psicométricas [thesis]. São Paulo, Brazil: Federal University of São Paulo, Paulista School of Medicine; 2003.
11. Poznanski EO, Mokros HB. Children’s Depression Rating Scale-Revised (CDRS-R). Los Angeles, CA: Western Psychological Services; 1996.
12. Wever RA. The Circadian System of Man: Results From Experiments Under Temporal Isolation. New York, NY: Springer Verlag; 1979.
13. Hasler BP, Allen JJ, Sbarra DA, et al. Morningness-eveningness and depression: preliminary evidence for the role of the behavioral activation system and positive affect. Psychiatry Res. 2010;176(2-3):166-173. PubMed doi:10.1016/j.psychres.2009.06.006
14. Kerkhof GA, Van Dongen HP. Morning-type and evening-type individuals differ in the phase position of their endogenous circadian oscillator. Neurosci Lett. 1996;218(3):153-156. PubMed doi:10.1016/S0304-3940(96)13140-2
15. Valdez P, Ram×rez C, Garc×a A. Delaying and extending sleep during weekends: sleep recovery or circadian effect? Chronobiol Int. 1996;13(3):191-198. PubMed doi:10.3109/07420529609012652
16. Teicher MH, Glod CA, Pahlavan K, et al. Circadian Activity Dysregulation and Antidepressant Response in Children and Adolescents. In: Scientific Proceedings of the 37th Meeting of the American Academy of Child and Adolescent Psychiatry; Chicago, Illinois; vol 6; 1990:58.
17. Frank E, Swartz HA, Mallinger AG, et al. Adjunctive psychotherapy for bipolar disorder: effects of changing treatment modality. J Abnorm Psychol. 1999;108(4):579-587. PubMed doi:10.1037/0021-843X.108.4.579
18. Salgado-Delgado R, Osorio AT, Saderi N, et al. Disruption of circadian rhythms: a crucial factor in the etiology of depression. Depress Res Treat. 2011; 839743. Epub 2011 PubMed.doi:10.1155/2011/839743.
Author affiliations: Department of Psychiatry, Paulista School of Medicine, Federal University of São Paulo (Drs Mesquita and Del-Porto); Central University of São Camilo, São Paulo (Dr Finazzi); Center for Health Sciences, Federal University of Bahia Rec×´ncavo, Bahia (Dr Duarte); and Department of Psychiatry, Faculty of Medicine (Dr Fu-I); and School of Arts, Sciences, and Humanities, University of São Paulo, São Paulo (Dr Menna-Barreto), Brazil.
Potential conflicts of interest: None reported.
Funding/support: None reported.
Published online: June 14, 2012.
Prim Care Companion CNS Disord 2012;14(3):doi:10.4088/PCC.11l01330
© Copyright 2012 Physicians Postgraduate Press, Inc.