The Transdermal Delivery System of Monoamine Oxidase Inhibitors
Monoamine oxidase inhibitors (MAOIs) were once widely used as effective treatments for major depressive disorder, particularly for patients with atypical or treatment-resistant depression. Today, MAOIs have largely been replaced by newer antidepressants because of concerns over potential serious side effects due to their mechanism of action. Monoamine oxidase (MAO) is an enzyme that metabolizes serotonin, norepinephrine, and dopamine, the neurotransmitters that are most associated with depression; inhibiting MAO, therefore, makes more of these neurotransmitters available for synaptic action. However, MAO also metabolizes tyramine, a trace amine found in some foods that acts as a sympathomimetic. Allowing excess tyramine to accumulate via MAO inhibition can result in hypertensive crisis due to the release of norepinephrine; therefore, patients taking an MAOI have had to follow dietary restrictions to avoid tyramine-rich foods. Hypertensive crisis may also be precipitated by using MAOIs in conjunction with other drugs that have vasoconstrictive properties, that act as sympathomimetics, or that inhibit the reuptake of norepinephrine. Serotonin syndrome is another serious adverse effect that can potentially occur when using an MAOI with another drug that inhibits the reuptake of serotonin. In this article, the mechanism of action of MAOIs is reviewed, along with that of a newer MAOI formulation that lessens the need for dietary restrictions and has a greater safety and tolerability profile than the older oral formulations.
(J Clin Psychiatry 2012;73[suppl 1]:25-30)
From the Department of Pharmacy Practice and the Center for Clinical Research, Mercer University College of Pharmacy and Health Sciences, Atlanta, Georgia.
This article is derived from the planning teleconference series “A Fresh Look at Monoamine Oxidase Inhibitors for Depression,” which was held December 2011 through February 2012 and supported by an educational grant from Mylan Specialty L.P. (formerly known as Dey Pharma, L.P.).
Dr VanDenBerg has received grant/research support from Eli Lilly and Cognitive Research Corporation.
Corresponding author: Chad M. VanDenBerg, PharmD, BCPP, 3001 Mercer University Drive, DV-129, Atlanta, GA 30341 ([email protected]).
doi:10.4088/JCP.11096su1c.04
© Copyright 2012 Physicians Postgraduate Press, Inc.
Beginning with their introduction in the 1950s, and for several decades thereafter, monoamine oxidase inhibitors (MAOIs) were widely used as an effective treatment for major depressive disorder, particularly for atypical depression1 and treatment-resistant depression.2 Today, MAOIs have largely been replaced by newer antidepressants due to concerns regarding potential side effects from drug and food interactions and the resulting need for dietary restrictions and careful medical management. Understanding the mechanism of action of MAOIs, however, can help clinicians to prevent these interactions. Additionally, a newer MAOI formulation that is easier to administer and has a better safety and tolerability profile is available.
MAOI Mechanism of Action
The pathophysiology of depression has yet to be fully understood, but all pharmacotherapies for the disorder are based on increasing the synaptic action of one or more of the monoamine neurotransmitters serotonin, norepinephrine, and dopamine.3 The MAOIs inhibit monoamine oxidase (MAO), a mitochondrial enzyme that acts as a catalyst for converting biogenic amines to their corresponding aldehydes. The MAO enzyme oxidatively deaminates and inactivates excess neurotransmitter molecules; therefore, inhibiting MAO activity by deactivating the enzyme allows serotonin, norepinephrine, and dopamine to accumulate, increasing their availability for synaptic action.4 Originally, this action was thought to be the basis for the antidepressant action of MAOIs, but one hypothesis proposes secondary adaptive mechanisms, such as downregulation of monoamine receptors and the elevation of other trace amines, as possible factors in the antidepressant effect.5 Although MAOIs increase the availability of monoamines almost immediately, the secondary effects occur after chronic administration of the medication over several weeks, which coincides with the delayed onset of antidepressant effect.
- MAO is an enzyme that metabolizes serotonin, norepinephrine, and dopamine; inhibiting MAO allows these neurotransmitters to accumulate in the synaptic cleft.
- MAOIs have potentially serious side effects, such as hypertensive crisis and serotonin syndrome, due to diet and drug interactions.
- To avoid these adverse effects, patients should be educated regarding dietary restrictions and drug interactions.
- A transdermal MAOI formulation with a greater tolerability and safety profile than oral MAOIs is available, which, at the minimum effective dosage, avoids the need for dietary restrictions.
MAO Subtypes
Two isoenzymes of MAO have been identified: MAO-A and MAO-B. Both are found in the central nervous system (CNS) and in the intestine and liver, but they have different substrates and different relative distributions. MAO-A is mainly found in the brain and intestine and is present in serotonin, dopamine, and norepinephrine neurons. In the brain, MAO-A preferentially metabolizes serotonin and norepinephrine, and in the intestine, MAO-A catabolizes amines absorbed into the gastrointestinal (GI) tract, including tyramine. The main substrates for MAO-B, which is found in brain regions rich in serotonergic neurons and in platelets and other tissues, are β-phenylethylamine, dopamine, and tyramine. MAO-B preferentially metabolizes trace amines such as 2-phenylethylamine. Both MAO-A and MAO-B metabolize dopamine.4,6
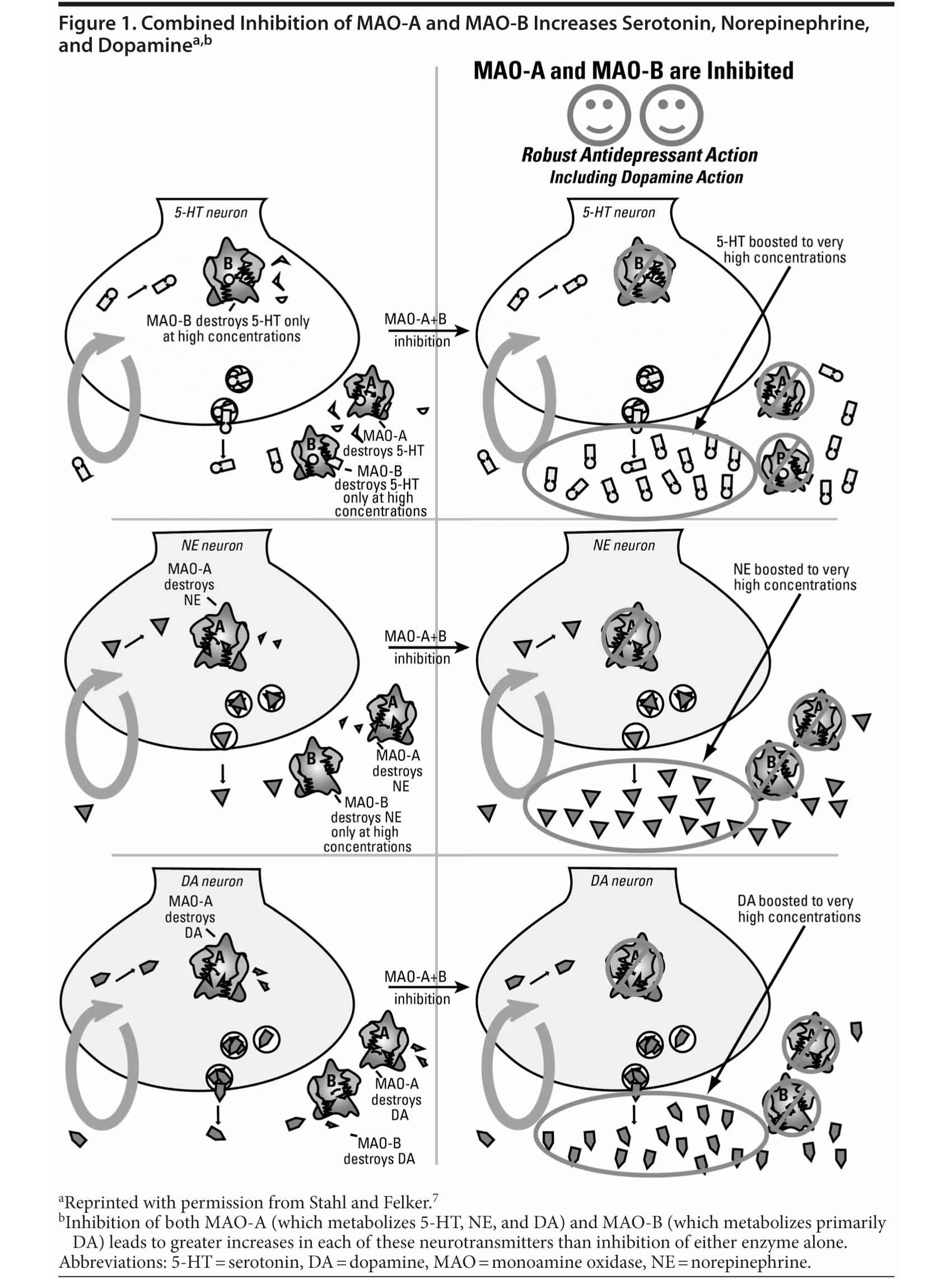
Inhibition of MAO-A increases the levels of serotonin and norepinephrine and, to a lesser extent, dopamine, as dopamine will still be metabolized by MAO-B (Figure 1).7 Inhibiting MAO-B has little effect on serotonin and norepinephrine levels, and dopamine levels will not rise substantially due to continued metabolism by MAO-A. MAO-A preferentially metabolizes all 3 of the monoamines most associated with depression, and inhibition of MAO-A in the brain is needed for an antidepressant effect. However, inhibiting both MAO-A and MAO-B leads to a greater increase in all 3 neurotransmitters than inhibition of either alone.7
MAOIs can be either nonselective or selective. Nonselective MAOIs inhibit both isoenzymes, whereas selective MAOIs inhibit either MAO-A or MAO-B. The classic oral MAOIs approved to treat depression in the United States (isocarboxazid, phenelzine, and tranylcypromine) are all nonselective. Oral selegiline is a selective inhibitor of MAO-B and is approved at low doses (10 mg/d) as an adjunct to carbidopa/levodopa to treat Parkinson’s disease. However, at doses high enough to induce an antidepressant effect (30 to 60 mg/d), oral selegiline loses its selectivity and inhibits both MAO-A and MAO-B.8-10
All MAOIs approved to treat depression in the United States are irreversible, meaning they bind to MAO for the life of the enzyme. Once the medication is stopped, a period of 7 to 10 days is required for new MAO enzyme to be generated and enzymatic activity to resume.4
Adverse Effects and Mechanism of Action
The most common early side effects of oral MAOIs include insomnia, sedation, orthostatic hypotension, dizziness, and nausea. Later side effects reported for MAOIs include weight gain, edema, muscle pain, myoclonus, paresthesia, and sexual dysfunction.11 The most serious adverse effects associated with MAOIs, however, are due to food and drug interactions.
Food interactions. Tyramine is a trace amine, found in many foods, that acts as an indirect sympathomimetic.12 MAO-A metabolizes dietary tyramine in the GI system and liver, which restricts the uptake of tyramine into the circulatory system. Irreversible inhibition of intestinal MAO-A, via oral delivery of an MAOI, can therefore lead to serious interactions with foods containing high levels of tyramine.
Normally, MAO-A in the intestinal wall and in the liver can metabolize up to 400 mg of ingested tyramine.7 When MAO-A is inhibited in the gut, as little as 10 mg of ingested tyramine can cause an excessive amount to enter the bloodstream, where it triggers the release of norepinephrine from sympathetic nerve terminals. Excess norepinephrine causes a rapid and sometimes severe increase in blood pressure that can lead to hypertensive crisis, possibly resulting in stroke or even death. Thus, patients taking irreversible, nonselective MAO inhibitors must follow dietary restrictions that limit tyramine intake.13
Reversible inhibitors of MAO-A (RIMAs) have been developed in an effort to avoid the tyramine reaction. With these medications, when tyramine is ingested and absorbed in the gut in large enough amounts to increase the release of norepinephrine, the accumulation of norepinephrine displaces the RIMA from the active site on the MAO-A enzyme, allowing the norepinephrine to be metabolized.14 Dietary restrictions are unnecessary with RIMAs. As tyramine does not cross the blood-brain barrier, MAO-A in the brain will continue to be inhibited, maintaining the antidepressant effect.15 The MAO-A selective RIMA moclobemide is available throughout much of the world but is not approved in the United States.
Drug interactions. The amount of norepinephrine potentiated by MAOIs alone is not great enough to elevate blood pressure in the absence of tyramine ingestion. However, MAOIs should not be used in combination with other adrenergic medications, including some decongestants, stimulants such as methylphenidate and amphetamines, opioids or pain medications that contain sympathomimetic vasoconstrictors, and antidepressants or appetite suppressants with norepinephrine uptake inhibition, as hypertensive crisis can result.
Combining MAOIs with medications that inhibit serotonin reuptake (including other antidepressants, certain analgesic agents, and the antitussive agent dextromethorphan) can cause serotonin syndrome, a potentially lethal condition caused by the accumulation of excessive serotonin.14 When switching a patient to or from an MAOI, a washout period of about 2 weeks is recommended; switching from fluoxetine, however, requires a washout period of 5 weeks due to its long half-life.
Transdermal Delivery System for Selegiline
Although simplified over the years, the dietary restrictions that accompany MAOI use have been perceived by patients and clinicians as difficult to manage. One effort to improve the safety of MAOIs and limit or avoid the need for dietary restrictions was the development of the selegiline transdermal system (STS). With the STS, the drug is delivered in a controlled manner over 24 hours via the once-daily application of a matrix-type patch. By bypassing the GI tract, the transdermal preparation of selegiline avoids the complete inhibition of MAO-A in the gut that occurs with oral MAOIs.
Pharmacokinetics
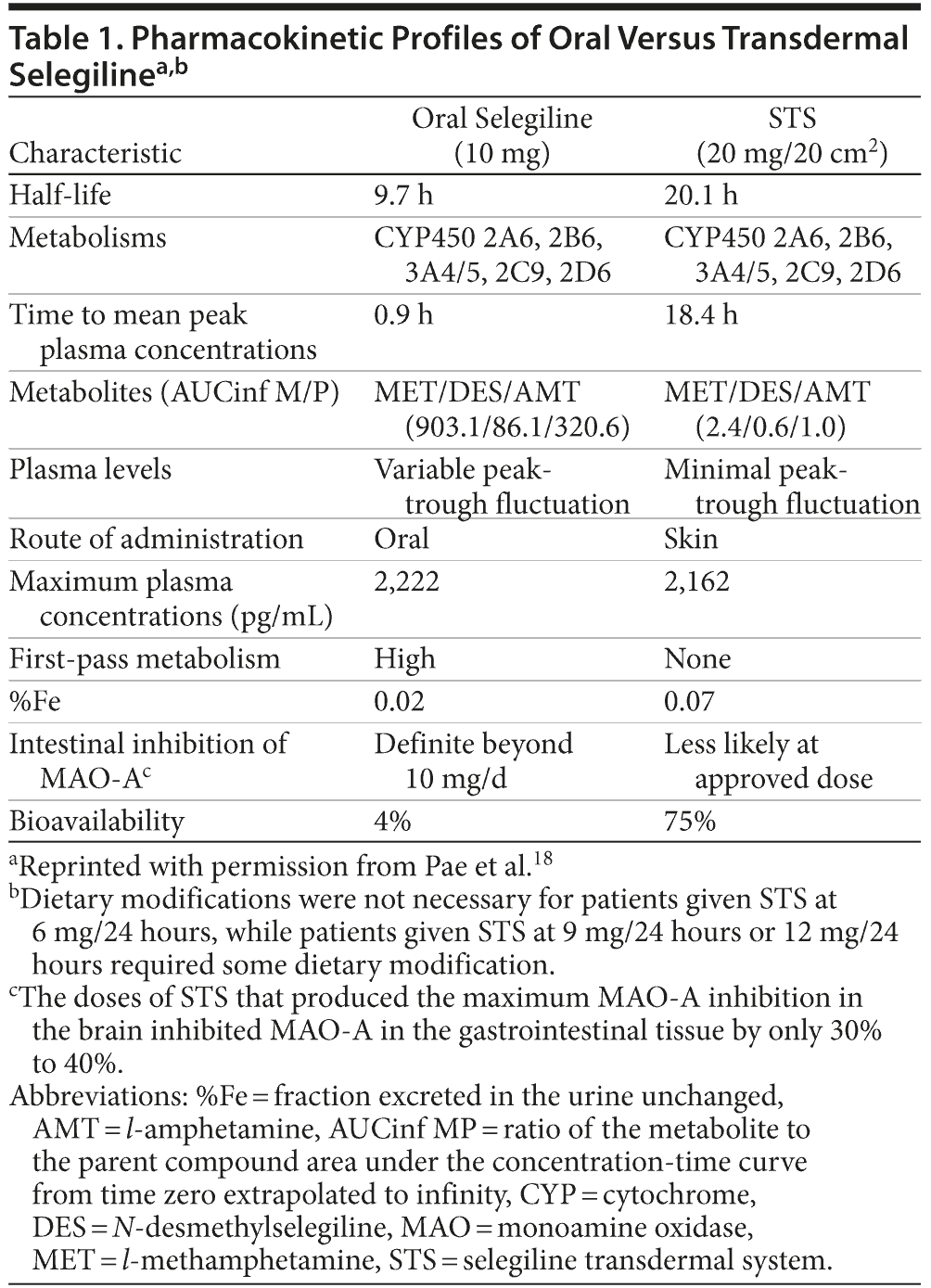
The physiochemical properties of selegiline (eg, low molecular weight, high lipid solubility) make it well-suited for transdermal delivery. Selegiline is a weak base with a molecular weight of 187.3, a pKa of 7.5, and a calculated octanol/water partition coefficient of 3.4.16 Delivering a highly lipid-soluble compound such as selegiline transdermally allows it to rapidly penetrate cell membranes and quickly reach target sites in the CNS. Upon application of the patch, about 25% to 30%, on average, of the selegiline content is delivered systemically over 24 hours, and steady-state plasma concentrations are achieved within 5 days of daily dosing.17 Gender does not affect the pharmacokinetics or metabolism of transdermally delivered selegiline. Table 1 summarizes the pharmacokinetics of oral selegiline and the STS.18
A randomized, open-label study16 demonstrated that transdermal selegiline delivers a higher plasma concentration of drug to the CNS over a longer period of time, and with a lower dosage, than does oral selegiline. The greater bioavailability of 6 mg of transdermal selegiline (73.4%) versus 10 mg of oral selegiline (4.4%) is due to the avoidance of the extremely high first-pass metabolism that occurs with the oral medication in the GI system and liver before entering the circulatory system.16 In addition, transdermal selegiline maintains a sustained plasma concentration during the 24-hour application period, whereas the oral medication plasma concentration peaks within 1 hour and then declines rapidly. Because MAO-A is largely unaffected in the gut by the STS, patient sensitivity to dietary tyramine is more than 20 times less with the selegiline transdermal patch than with oral tranylcypromine.19
Both oral and transdermal selegiline are metabolized through multiple CYP450 isoenzymes and form, in order, the metabolites N-desmethylselegiline, l-methamphetamine, and l-amphetamine; l-methamphetamine is the major metabolite formed.16 However, metabolite levels, which may be associated with neurotoxicity, are greatly reduced with transdermal delivery (see Table 1).18,20
Pharmacodynamics
Transdermal selegiline must be administered at doses high enough to lose its selectivity for MAO-B in order to have an antidepressant effect. While oral selegiline inhibits MAO-A activity in the brain and duodenum to a similar extent, to avoid reactions to dietary tyramine, the transdermal delivery system preferentially targets MAO-A activity in the brain over peripheral activity. Transdermal selegiline ID50 values for inhibition of brain MAO-A activity are 7.5 times lower than ID50 values for inhibition of intestinal MAO-A activity.21 This means that the antidepressant effect, via inhibition of MAO-A in the brain, can occur with a significantly lower potential for tyramine reactions due to inhibition of MAO-A in the gut. Based on route of delivery and avoidance of the first-pass effect, transdermally delivered selegiline is 6 to 8 times more potent for inhibiting brain MAO-A activity than orally delivered selegiline. Therefore, a lower dose is needed to produce an antidepressant effect.
Animal studies18 show that STS doses that inhibit more than 90% of the activity of both MAO-A and MAO-B in the brain have a maximal inhibition of 40% of MAO-A and 70% to 75% of MAO-B activity in GI tissue. Doses that inhibit brain MAO-A by 55% to 60% and brain MAO-B by 85% to 90% show no inhibition of GI MAO-A activity and show only 40% to 60% inhibition of GI MAO-B activity. In these studies, higher doses lost their selectivity for inhibiting MAO-B in the brain but not in GI tissue.
Safety Profile
In placebo-controlled trials22,23 of STS for treatment of acute depression, the tolerability profile of STS was similar to that of placebo except for application site reactions. No significant differences between the treatment groups and the placebo groups were noted for adverse effects for cardiovascular, nervous, digestive, respiratory, urogenital, or musculoskeletal systems or for sexual function. A 52-week study24 that assessed maintenance treatment with STS also reported a safety profile similar to that of placebo except for application site reactions.
Transdermal selegiline is classified as a nonallergen; application site reactions are similar to those of other transdermally delivered medications and probably due to the adhesive used in the patch.25 Application site reactions are generally a form of irritant contact dermatitis (rather than allergic contact dermatitis) and are mild to moderate, transient in nature, and resolve spontaneously after patch removal.26 Skin reactions can be minimized by rotating the patch site, carefully removing the patch and then washing the site with warm soapy water, and using moisturizers and topical corticosteroids.
The available STS patches deliver 6 mg, 9 mg, or 12 mg of medication per 24 hours, and no hypertensive crises have been reported at any dose of the patch. A study19 of tyramine pressor sensitivity found no significant effects for the minimum effective dose (6 mg/24 h) after 33 days of treatment. Dietary restrictions are not necessary at the 6 mg/24 hours dose but are recommended at higher doses due to a lack of safety data.
Although the STS reduces the risk of food interactions, it does not protect against potential hypertensive crisis and serotonin syndrome due to drug interactions. The same precautions against drug interactions should be taken when using STS as when using other MAOIs.
Efficacy for Major Depressive Disorder
Three placebo-controlled trials demonstrated efficacy for STS over placebo for the acute treatment of depression (Table 2).18 In the first trial,23 patients were randomly assigned to take either 6 mg/24 hours STS (n = 89) or placebo (n = 88) for 6 weeks. Patients in the STS group experienced significantly better outcomes on all outcome measures. In the second trial,22 145 patients received STS 6 mg/24 hours and 144 patients received the placebo patch for 8 weeks. This trial showed a modest but significant benefit for the STS over placebo. A third placebo-controlled study27 investigated the efficacy of STS administered in a dose range (6 mg/24 h to 12 mg/24 h) for 8 weeks and showed antidepressant efficacy over placebo across the dose range for both primary and secondary outcome measures.
A 52-week trial24 investigated relapse rates for patients randomly assigned to take STS (n = 149) or placebo (n = 163) after responding to 10 weeks of acute treatment with STS 6 mg/24 hours. Compared with patients receiving placebo, significantly fewer patients receiving STS experienced relapse (P = .0025), and patients receiving STS experienced a significantly longer time to relapse (P = .0048).
Advantages of Transdermal Delivery
Skin patches have become fairly familiar to patients over the past few decades, as they have been used in the treatment of various illnesses including motion sickness, Alzheimer’s disease, restless legs syndrome, Parkinson’s disease, pain from postherpetic neuralgia, smoking addiction, attention-deficit/hyperactivity disorder, and angina.28,29 Patches are also used for contraception and hormone replacement.29 The STS uses a matrix-type patch, which has several advantages over the older reservoir-type patch. With many reservoir patches, the drug is contained in an alcohol solution, which irritates the skin. Matrix patches are smaller and thinner, adhere better to the skin, and are generally better tolerated than reservoir patches.28
With a transdermal patch, some of the side effects that occur when the same drug is delivered orally can be avoided because the drug is delivered directly into the circulatory system. The transdermal patch avoids certain side effects created due to first-pass metabolism in the intestine and liver. The patch also maintains steady plasma drug levels, thereby reducing tolerability problems that are associated with fluctuations in plasma concentrations.29 The reduction in adverse effects may help patients to more easily reach and maintain therapeutic levels of the drug, which should provide greater efficacy and, in turn, increase treatment adherence.
Another advantage of the patch delivery system is ease of use; patches are applied once a day, simplifying the treatment regimen for those taking multiple daily doses of oral formulations, and are a visual reminder that treatment has been administered.29 Transdermal delivery can also be helpful for patients with certain medical conditions, such as swallowing difficulties.
Conclusion
Classic MAOIs are effective for depression but have serious potential side effects, including hypertensive crisis due to either ingestion of dietary tyramine or drug interactions and serotonin syndrome due to drug interactions. A modified diet that restricts tyramine intake is necessary with the oral MAOIs that are available in the United States; however, a transdermal formulation for selegiline has lessened the need for these restrictions. Avoiding other medications that boost norepinephrine or serotonin levels can prevent hypertensive crisis and serotonin syndrome due to drug interactions. With a better safety and tolerability profile than that of oral MAOIs, STS offers another option for treating depression, particularly for patients with atypical or treatment-resistant depression.
Drug names: carbidopa/levodopa (Parcopa, Sinemet, and others), fluoxetine (Prozac and others), isocarboxazid (Marplan), methylphenidate (Focalin, Daytrana, and others), phenelzine (Nardil and others), selegiline oral formulation (Eldepryl, Zelapar, and others), selegiline transdermal system (EMSAM), tranylcypromine (Parnate and others).
Disclosure of off-label usage: The author has determined that, to the best of his knowledge, oral selegiline and moclobemide are not approved by the US Food and Drug Administration for the treatment of depression.
References
1. Henkel V, Mergl R, Allgaier AK, et al. Treatment of depression with atypical features: a meta-analytic approach. Psychiatry Res. 2006;141(1):89-101. PubMed doi:10.1016/j.psychres.2005.07.012
2. Amsterdam JD, Shults J. MAOI efficacy and safety in advanced stage treatment-resistant depression—a retrospective study. J Affect Disord. 2005;89(1-3):183-188. PubMed doi:10.1016/j.jad.2005.06.011
3. Owens MJ. Selectivity of antidepressants: from the monoamine hypothesis of depression to the SSRI revolution and beyond. J Clin Psychiatry. 2004;65(suppl 4):5-10. PubMed
4. Krishnan KR. Revisiting monoamine oxidase inhibitors. J Clin Psychiatry. 2007;68(suppl 8):35-41. PubMed
5. Baker GB, Coutts RT, McKenna KF, et al. Insights into the mechanisms of action of the MAO inhibitors phenelzine and tranylcypromine: a review. J Psychiatry Neurosci. 1992;17(5):206-214. PubMed
6. Schatzberg AF, Nemeroff CB. The American Psychiatric Press Textbook of Psychopharmacology. 2nd ed. Washington, DC: American Psychiatric Press; 1998.
7. Stahl SM, Felker A. Monoamine oxidase inhibitors: a modern guide to an unrequited class of antidepressants. CNS Spectr. 2008;13(10):855-870. PubMed
8. Mann JJ, Aarons SF, Wilner PJ, et al. A controlled study of the antidepressant efficacy and side effects of (-)-deprenyl. A selective monoamine oxidase inhibitor. Arch Gen Psychiatry. 1989;46(1):45-50. PubMed doi:10.1001/archpsyc.1989.01810010047007
9. Schulz R, Antonin KH, Hoffmann E, et al. Tyramine kinetics and pressor sensitivity during monoamine oxidase inhibition by selegiline. Clin Pharmacol Ther. 1989;46(5):528-536. PubMed doi:10.1038/clpt.1989.181
10. Heinonen EH, Anttila MI, Lammintausta RA. Pharmacokinetic aspects of l-deprenyl (selegiline) and its metabolites. Clin Pharmacol Ther. 1994;56(6 pt 2):742-749. PubMed doi:10.1038/clpt.1994.204
11. Fiedorowicz JG, Swartz KL. The role of monoamine oxidase inhibitors in current psychiatric practice. J Psychiatr Pract. 2004;10(4):239-248. PubMed doi:10.1097/00131746-200407000-00005
12. Culpepper L, Kovalick LJ. A review of the literature on the selegiline transdermal system: an effective and well-tolerated monoamine oxidase inhibitor for the treatment of depression. Prim Care Companion J Clin Psychiatry. 2008;10(1):25-30. PubMed doi:10.4088/PCC.v10n0105
13. Gardner DM, Shulman KI, Walker SE, et al. The making of a user friendly MAOI diet. J Clin Psychiatry. 1996;57(3):99-104. PubMed
14. Stahl MS. Stahl’s Essential Psychopharmacology: Neuroscientific Basis and Practical Applications. 3rd ed. New York, NY: Cambridge University Press; 2008.
15. Lotufo-Neto F, Trivedi M, Thase ME. Meta-analysis of the reversible inhibitors of monoamine oxidase type A moclobemide and brofaromine for the treatment of depression. Neuropsychopharmacology. 1999;20(3):226-247. PubMed doi:10.1016/S0893-133X(98)00075-X
16. Azzaro AJ, Ziemniak J, Kemper E, et al. Pharmacokinetics and absolute bioavailability of selegiline following treatment of healthy subjects with the selegiline transdermal system (6 mg/24 h): a comparison with oral selegiline capsules. J Clin Pharmacol. 2007;47(10):1256-1267. PubMed doi:10.1177/0091270007304779
17. EMSAM (selegiline patch) [package insert]. Napa, CA: Dey Pharma LP; 2010. http://dailymed.nlm.nih.gov/dailymed/lookup.cfm?setid=b891bd9f-fdb8-4862-89c5-ecdd700398a3. Accessed April 20, 2012.
18. Pae CU, Lim HK, Han C, et al. Selegiline transdermal system: current awareness and promise. Prog Neuropsychopharmacol Biol Psychiatry. 2007;31(6):1153-1163. PubMed doi:10.1016/j.pnpbp.2007.04.020
19. Azzaro AJ, Vandenberg CM, Blob LF, et al. Tyramine pressor sensitivity during treatment with the selegiline transdermal system 6 mg/24 h in healthy subjects [published correction appears in J Clin Psychopharmacol. 2006;46(10):1225-1226]. J Clin Pharmacol. 2006;46(8):933-944. PubMed doi:10.1177/0091270006289852
20. Wagner GC, Walsh SL. Evaluation of the effects of inhibition of monoamine oxidase and senescence on methamphetamine-induced neuronal damage. Int J Dev Neurosci. 1991;9(2):171-174. PubMed doi:10.1016/0736-5748(91)90008-A
21. Mawhinney M, Cole D, Azzaro AJ. Daily transdermal administration of selegiline to guinea-pigs preferentially inhibits monoamine oxidase activity in brain when compared with intestinal and hepatic tissues. J Pharm Pharmacol. 2003;55(1):27-34. PubMed doi:10.1111/j.2042-7158.2003.tb02430.x
22. Amsterdam JD. A double-blind, placebo-controlled trial of the safety and efficacy of selegiline transdermal system without dietary restrictions in patients with major depressive disorder. J Clin Psychiatry. 2003;64(2):208-214. PubMed doi:10.4088/JCP.v64n0216
23. Bodkin JA, Amsterdam JD. Transdermal selegiline in major depression: a double-blind, placebo-controlled, parallel-group study in outpatients. Am J Psychiatry. 2002;159(11):1869-1875. PubMed doi:10.1176/appi.ajp.159.11.1869
24. Amsterdam JD, Bodkin JA. Selegiline transdermal system in the prevention of relapse of major depressive disorder: a 52-week, double-blind, placebo-substitution, parallel-group clinical trial. J Clin Psychopharmacol. 2006;26(6):579-586. PubMed doi:10.1097/01.jcp.0000239794.37073.70
25. Pauporte M, Goodhead M, Azzaro AJ, et al. Selegiline transdermal system (STS): preclinical assays of dermal safety. Cutan Ocul Toxicol. 2005;23(3):173-178. doi:10.1081/CUS-200035363
26. Ale I, Lachapelle JM, Maibach HI. Skin tolerability associated with transdermal drug delivery systems: an overview. Adv Ther. 2009;26(10):920-935. PubMed doi:10.1007/s12325-009-0075-9
27. Feiger AD, Rickels K, Rynn MA, et al. Selegiline transdermal system for the treatment of major depressive disorder: an 8-week, double-blind, placebo-controlled, flexible-dose titration trial. J Clin Psychiatry. 2006;67(9):1354-1361. PubMed doi:10.4088/JCP.v67n0905
28. Farlow MR, Somogyi M. Transdermal patches for the treatment of neurologic conditions in elderly patients: a review. Prim Care Companion CNS Disord. 2011;13(6):doi:10.4088/PCC.11r01149. doi:10.4088/PCC.11r01149
29. Oertel W, Ross JS, Eggert K, et al. Rationale for transdermal drug administration in Alzheimer disease. Neurology. 2007;69(suppl 1):S4-S9. PubMed doi:10.1212/01.wnl.0000281845.40390.8b