Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
To the Editor: Electroconvulsive therapy (ECT) is an effective method of treatment for numerous psychiatric disorders, but it also precipitates distinct effects on intraocular pressure (IOP). Administration of propofol and succinylcholine cause, respectively, a decrease and increase in IOP. During convulsions, IOP further rises before returning to baseline after approximately 10 minutes.
Successful Use of Electroconvulsive Therapy in the Setting of Multiple Risk Factors for Retinal Detachment
To the Editor: Electroconvulsive therapy (ECT) is an effective method of treatment for numerous psychiatric disorders, but it also precipitates distinct effects on intraocular pressure (IOP).1 Administration of propofol and succinylcholine cause, respectively, a decrease and increase in IOP.1 During convulsions, IOP further rises before returning to baseline after approximately 10 minutes.1 The significance of these transient pressure changes remains unknown.
Changes in IOP co-occur with retinal detachment.2 A majority of patients with unilateral retinal detachment possess relative hypotony in the affected eye.2 How a change in IOP might cause retinal detachment remains uncertain; a competition between IOP and choroidal pressure might induce exudative detachment.2 When choroidal pressure exceeds IOP, fluid accumulates behind the retina and delamination ensues.
A patient subjected to ECT might, therefore, be at risk for retinal detachment.3 If a patient possesses additional risk factors for retinal detachment, one must ask, "Is ECT contraindicated?"
Here, we describe the case of a depressed patient with lattice degeneration of the retina, which predisposes to retinal detachment. The patient underwent ECT for psychotic depression, to which she responded well with no ophthalmologic complications.
Case report. Ms A, a 70-year-old white woman, was hospitalized for worsening psychotic depression. In addition to depressive signs and symptoms, she exhibited a preoccupation with having multiple neurologic and cardiovascular diseases; assessments by neurologists and a cardiologist were inconclusive. Ms A met DSM-5 criteria for major depressive disorder with psychotic features.
Prior to admission, Ms A was treated for depression with escitalopram 20 mg, olanzapine 10 mg, and psychotherapy. Her outpatient psychiatrist noted that her symptoms had not improved, and she was unable to function in her role as a teacher. Of note, Ms A’s past medical history was significant for essential hypertension, hypercholesterolemia, osteoporosis, lattice degeneration of the retina in her left eye, and repair of a retinal detachment in her right eye 30 years prior. She was additionally treated with gabapentin, amlodipine, hydrochlorothiazide, enalapril, and aspirin for various medical ailments.
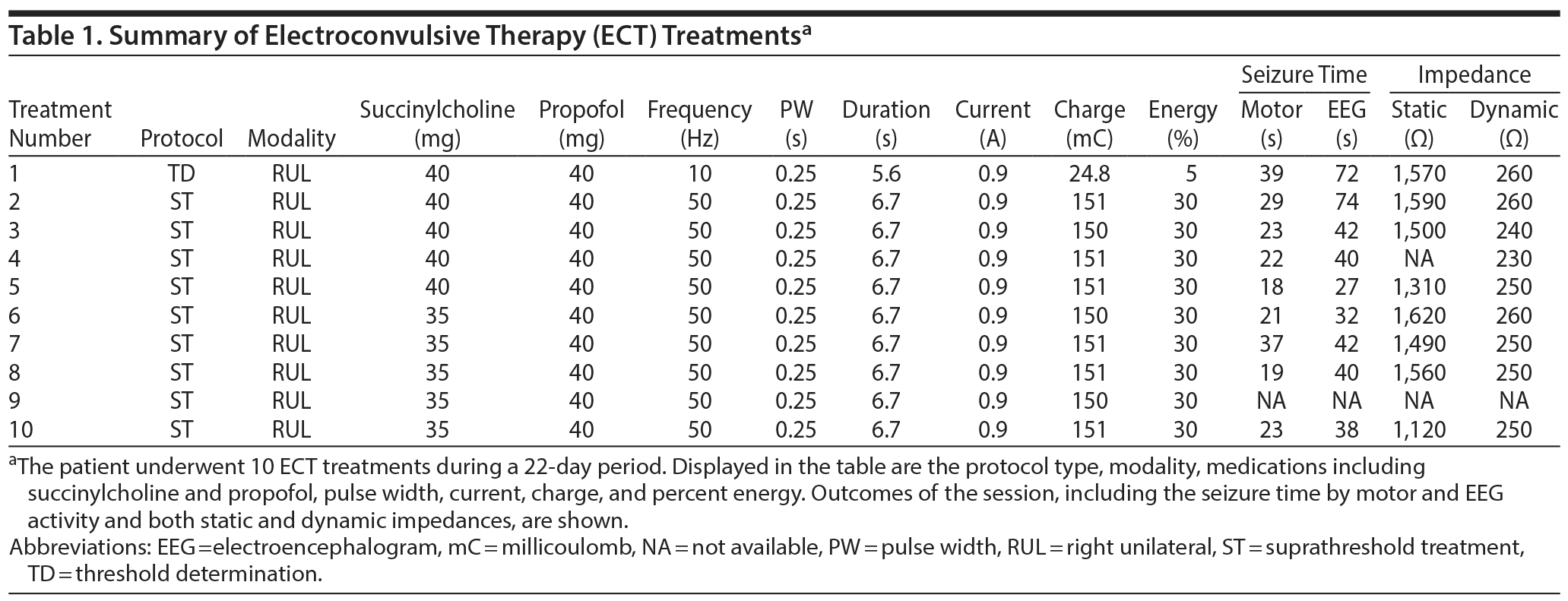
Clinical assessment revealed a Hamilton Depression Rating Scale (HDRS)4 score of 32 and a Montreal Cognitive Assessment (MoCA)5 score of 23. Brain magnetic resonance imaging revealed no pathology. On our unit, Ms A’s olanzapine dose was titrated to 20 mg, and her escitalopram was cross-tapered to sertraline 200 mg, but she exhibited no response. Given the severity of symptoms and lack of clinical response, the treatment team recommended ECT. Ms A was provided a daily antihypertensive (lisinopril 10 mg) prior to each treatment, and blood pressures were measured both before and after each session. She underwent 10 ECT treatments with no complication (Table 1).
After completion of her ECT course, Ms A displayed significant improvement in all symptoms, and her HDRS and MoCA scores improved to 6 and 28, respectively. Sertraline and olanzapine were cross-tapered to venlafaxine (225 mg/d) and lithium (600 mg/d). One month postdischarge, her psychiatric symptoms remained in remission with no ophthalmologic complications.
Prior to this report, no evidence has been published describing successful use of ECT in a patient with lattice degeneration. Because ECT induces transient changes in both IOP and blood pressure, it remains unclear whether ECT precipitates retinal tearing in a patient with ophthalmologic comorbidities.1,2,6 Our patient displayed no complications. This finding is consistent with prior reports6,7 of successful ECT treatment in patients who had undergone ophthalmologic surgeries.
Further studies must elucidate the risk of ophthalmologic complications from ECT for different ophthalmologic comorbidities. Per this report, however, we can conclude that those patients suffering from treatment-resistant major depressive disorder in the setting of lattice degeneration should not be dissuaded from treatment with ECT.
References
1. Boroojeny SB, Tabatabai NH, Babakhani B, et al. The effect of electroconvulsive therapy using propofol and succinylcholine on the intraocular pressure. Middle East J Anaesthesiol. 2012;21:713-717. PubMed
2. Bottega WJ, Bishay PL, Prenner JL, et al. On the mechanics of a detaching retina. Math Med Biol. 2013;30(4):287-310. PubMed CrossRef
3. Mart×nez-Amorós E, Real Barrero E, Fuste Fusares C, et al. Bilateral posterior vitreous detachment after electroconvulsive therapy. Gen Hosp Psychiatry. 2009;31(4):385-387. PubMed CrossRef
4. Hamilton M. A rating scale for depression. J Neurol Neurosurg Psychiatry. 1960;23(1):56-62. PubMed CrossRef
5. Nasreddine ZS, Phillips NA, Bédirian V, et al. The Montreal Cognitive Assessment, MoCA: a brief screening tool for mild cognitive impairment. J Am Geriatr Soc. 2005;53(4):695-699. PubMed CrossRef
6. Sienaert PA, Vanholst C. Electroconvulsive therapy after eye surgery. J ECT. 2013;29(2):139-141. PubMed CrossRef
7. Saad DA, Black JL, Krahn LE, et al. ECT post eye surgery: two cases and a review of the literature. J ECT. 2000;16(4):409-414. PubMed CrossRef
aWeill Cornell/Rockefeller/Sloan-Kettering Tri-Institutional MD-PhD Program, New York, New York
bWeill Cornell Medical College, Westchester Division, White Plains, New York
Potential conflicts of interest: None.
Funding/support: None.
Patient consent: The authors obtained consent from the patient to publish this case report, and information has been de-identified to protect anonymity.
Published online: April 5, 2018.
Prim Care Companion CNS Disord 2018;20(2):17l02190
To cite: Salvi JD, Iqbal M, Kotbi N, et al. Successful use of electroconvulsive therapy in the setting of multiple risk factors for retinal detatchment. Prim Care Companion CNS Disord. 2018;20(2):17l02190.
To share: https://doi.org/10.4088/PCC.17l02190
© Copyright 2018 Physicians Postgraduate Press, Inc.
Enjoy this premium PDF as part of your membership benefits!