Objective: Congestive heart failure (CHF) and hypertension are prevalent diseases with high mortality and morbidity rates. Depression and anxiety are frequently associated with cardiovascular diseases. This observational cross-sectional study assessed depression, anxiety, suicidality, and quality of life in 240 patients with CHF (with or without hypertension) or hypertension (without CHF).
Method: Subjects were evaluated between June 2005 and June 2007 using the Hamilton Anxiety Rating Scale (HARS), Hamilton Depression Rating Scale, Montgomery-Asberg Depression Rating Scale, Medical Outcomes Study 36-item Short-Form Health Survey (both physical component score and mental component score), and Satisfaction With Life Scale (SWLS). Patients with CHF were assigned a New York Heart Association functional classification.
Results: The CHF patients had higher scores on the depressive factor and the HARS and higher suicidality. Furthermore, they had lower scores on the physical component score, higher scores on the mental component score, and lower scores on the SWLS. Depressive symptom level was a significant predictor of lower physical health (P = .012), whereas anxiety was a significant predictor of satisfaction with life (P = .002). CHF compared to hypertension was a predictor of higher mental health as measured with the mental component score and lower satisfaction with life. Higher anxiety predicted lower satisfaction with life both in patients with CHF and with hypertension.
Conclusions: Anxiety and depressive symptoms and cardiovascular disease were frequently associated. Screening for anxiety and depression in cardiovascular patients may be crucial.
Prim Care Companion J Clin Psychiatry 2010;12(6):e1-e9
Submitted: October 16, 2009; accepted February 16, 2010.
Published online: November 25, 2010 (doi:10.4088/PCC.09m00916gry).
Corresponding author: Gianluca Serafini, MD, Department of Neuroscience, Sapienza University of Rome, Sant’ Andrea Hospital, Via di Grottarossa 1035-1039, 00189 Rome, Italy ([email protected]).
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
CME Background
Articles are selected for credit designation based on an assessment of the educational needs of CME participants, with the purpose of providing readers with a curriculum of CME articles on a variety of topics throughout each volume. Activities are planned using a process that links identified needs with desired results.
To obtain credit, read the material and go to PSYCHIATRIST.COM to complete the Posttest and Evaluation online.
CME Objective
After studying this article, you should be able to:
- Screen for anxiety and depression in patients with cardiovascular disease because of the impact that these comorbidities have on quality of life and functional status
Accreditation Statement
The CME Institute of Physicians Postgraduate Press, Inc., is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians.
Credit Designation
The CME Institute of Physicians Postgraduate Press, Inc., designates this educational activity for a maximum of 1.5 AMA PRA Category 1 Creditsâ„¢. Physicians should only claim credit commensurate with the extent of their participation in the activity.
Date of Original Release/Review
This educational activity is eligible for AMA PRA Category 1 Credit through December 31, 2013. The latest review of this material was October 2010.
Financial Disclosure
All individuals in a position to influence the content of this activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past 3 years, Larry Culpepper, MD, MPH, Editor in Chief, has been a consultant and a member of the advisory boards for AstraZeneca, Cephalon, Forest, Pfizer, Wyeth, Eli Lilly, Takeda, Merck, Neurocrine, sanofi, Bristol-Myers Squibb, and Otsuka and has been a member of the speakers panels for Forest, Wyeth, and Pfizer. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure appears at the end of the article.
Objective: Congestive heart failure (CHF) and hypertension are prevalent diseases with high mortality and morbidity rates. Depression and anxiety are frequently associated with cardiovascular diseases. This observational cross-sectional study assessed depression, anxiety, suicidality, and quality of life in 240 patients with CHF (with or without hypertension) or hypertension (without CHF).
Method: Subjects were evaluated between June 2005 and June 2007 using the Hamilton Anxiety Rating Scale (HARS), Hamilton Depression Rating Scale, Montgomery-Asberg Depression Rating Scale, Medical Outcomes Study 36-item Short-Form Health Survey (both physical component score and mental component score), and Satisfaction With Life Scale (SWLS). Patients with CHF were assigned a New York Heart Association functional classification.
Results: The CHF patients had higher scores on the depressive factor and the HARS and higher suicidality. Furthermore, they had lower scores on the physical component score, higher scores on the mental component score, and lower scores on the SWLS. Depressive symptom level was a significant predictor of lower physical health (P = .012), whereas anxiety was a significant predictor of satisfaction with life (P = .002). CHF compared to hypertension was a predictor of higher mental health as measured with the mental component score and lower satisfaction with life. Higher anxiety predicted lower satisfaction with life both in patients with CHF and with hypertension.
Conclusions: Anxiety and depressive symptoms and cardiovascular disease were frequently associated. Screening for anxiety and depression in cardiovascular patients may be crucial.
Prim Care Companion J Clin Psychiatry 2010;12(6):e1-e9
© Copyright 2010 Physicians Postgraduate Press, Inc.
Submitted: October 16, 2009; accepted February 16, 2010.
Published online: November 25, 2010 (doi:10.4088/PCC.09m00916gry).
Corresponding author: Gianluca Serafini, MD, Department of Neuroscience, Sapienza University of Rome, Sant’ Andrea Hospital, Via di Grottarossa 1035-1039, 00189 Rome, Italy ([email protected]).
Congestive heart failure (CHF), often punctuated by acute exacerbation, is the most common form of heart failure. Over 20 million people are affected by CHF worldwide,1 almost 5 million in the United States2 and 10 million in Europe.3,4 The incidence and prevalence increases with age,5,6 and in subjects over the age of 65 years, CHF is the main cause of hospitalization and disability.7 Mortality among patients with CHF is 6-7 times higher than in the general population.8 In past studies, sudden death was a greater problem in patients with New York Heart Association (NYHA) functional classification IV and in those with advanced CHF.9,10
Hypertension is considered one of the leading causes of death and disability, and its prevalence is rapidly increasing in developing countries.11 Hypertension is reported to be the fourth most common cause of premature death in developed countries and the seventh in developing countries.12 Recent reports indicate that nearly 1 billion adults (roughly a quarter of the world’s population) have hypertension, and this rate is predicted to increase to 1.56 billion by the year 2025.13 Hypertension is a major risk factor for cardiovascular morbidity, including CHF,14 although the association between high arterial and incident hypertension has not been well studied.15
Several studies have reported that approximately 1 in 4 patients treated in primary care settings shows psychological problems, predominantly anxiety and/or depression.16,17 Runkewitz et al18 reported that approximately 22.1% of nonpsychiatric patients show clinically relevant psychological symptoms. Depression and anxiety are common conditions in primary care settings, affecting at least 10% of primary care patients. Depression in primary care is associated with an increasing risk of cardiovascular disease, diabetes, hypertension, stroke, and several symptoms increasing health service costs.19,20 General practitioners are considered to be gatekeepers who have a specific responsibility for the assessment, recognition, and treatment of psychiatric disorders.21 However, the recognition and diagnosis of psychological problems by primary care physicians remain poor and inadequate.22 The identification rate of depressive or anxiety disorders is reported to be only 50%-60%,23 and physicians do not take into account over 50% of psychiatric conditions.24
Clinical Points
- Adequate screening for anxiety, depression, and suicide risk in patients with cardiovascular diseases may be crucial.
- Patients with severe chronic pain may see suicide as the only way of escaping their suffering.
- Clinicians should teach patients how to recognize the cues for anxiety, depression, and suicidal behavior and encourage them to seek help.
Patients at higher risk for increased anxiety and depression are generally female, single or divorced, and complaining of fatigue and/or cardiovascular symptoms.18 Both anxiety and depression are associated with CHF and hypertension. There is evidence that links depression,25 anxiety,25,26 and both anxiety and depression26,27 to CHF mortality and sudden cardiac death. Additionally, depression is associated with a higher mortality in both outpatients28,29 and inpatients with CHF.30 The presence of depression in patients with existing coronary artery disease confers a relative risk between 1.5 and 2.5 for cardiac morbidity and mortality.31 Several authors have suggested that patients with CHF, anxiety, and depression have a worse quality of life, greater disability, and an increased rate of hospitalization,30,32,33 but other studies have not replicated these findings.28,32
Also, several studies have hypothesized that there is a link between CHF, hypertension, and suicide.34,35 This link, however, has typically been inferred from uncontrolled case series, and few rigorous studies have been published.25,36-38
Suicidal ideation is associated with functional disability, anxiety, depression, increased health service use, and subjective distress in primary care patients39,40 but frequently remains undetected by primary care physicians. It is well known that major depressive and anxiety disorders have also been shown to play significant roles in the increased risk of suicidal ideation among primary care patients.41,42
Although most guidelines recommend improving the quality of life and helping patients comply with the treatment for cardiovascular diseases, particularly among elderly individuals with severe disability and functional impairment,43 the exact role of psychological factors has not been evaluated.44 The present study was designed to evaluate the impact of anxiety, depression, and several risk factors for suicide on the quality of life and functional status of patients with CHF and hypertension.
METHOD
Study Design
This study involves the cross-sectional analysis of enrollment data for subjects with CHF and hypertension. The study protocol was reviewed and approved by the Rome Public Health Department Institutional Review Board, and all study participants signed an informed consent.
Subjects. Study entry criteria were determined through several stages. At the beginning of the study, 256 patients at least 18 years old with a diagnosis of CHF (with or without hypertension) or hypertension (without CHF) were screened. Some CHF patients had hypertension, but none of the hypertension patients had CHF.
The diagnoses of hypertension and CHF were assigned by a cardiologist and confirmed by a second cardiologist blind to the first diagnosis. The NYHA functional classification12 was used to assess the degree to which heart failure limited physical activities corresponding to disease severity. As functional abilities decrease, NYHA classification increases from class I to class IV. In the current study, NYHA classification was determined using a semistructured clinical interview completed by trained research assistants. We considered hypertension to be present when a person’s blood pressure was consistently ≥ 140 mm Hg systolic or ≥ 90 mm Hg diastolic.45
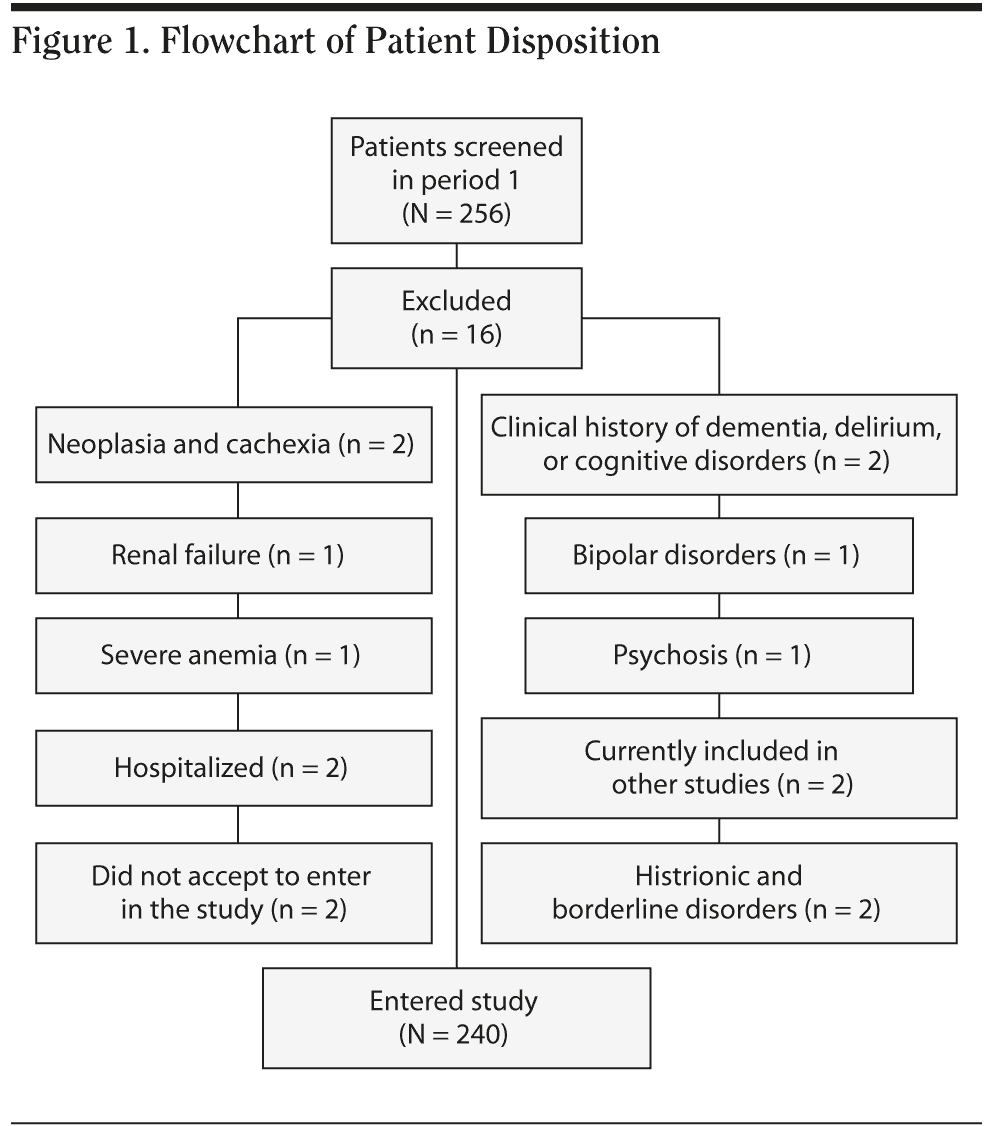
Sixteen subjects were excluded from the study for the following reasons. Four subjects with CHF were excluded because they were affected by severe medical conditions (2 with neoplasia and cachexia, 1 with renal failure, and 1 with severe anemia), 4 subjects with hypertension did not sign the informed consent, 2 subjects had been recently hospitalized, 2 reported over 6 hospitalizations in the last 2 years (and so had a greater functional impairment due to the severity of the illness), and 6 with CHF were excluded because they had a DSM-IV Axis I diagnosis (2 patients had a clinical history of dementia and delirium, 1 had a bipolar disorder type I, 1 had a psychosis, and 2 had a histrionic and a borderline personality disorder). We also excluded 2 individuals with hypertension because they were currently included in other studies (Figure 1).
Procedure. The final sample (N = 240) was enrolled in the study between June 2005 and June 2007 at the Department of Cardiology, Sant’ Andrea Hospital (Rome, Italy) and “Riuniti” Hospital (Foggia, Apulia, Italy); those participants who completed all study measures were consecutively included as outpatients. All patients were approached by a research assistant after checking in for their appointment for CHF and hypertension and were asked to complete a brief questionnaire in which they were asked to indicate their age in years, gender, race, years of education, and marital status and whether or not they had been diagnosed with different health conditions, including asthma, cancer, coronary artery disease, diabetes, emphysema or chronic obstructive pulmonary disorder (COPD), heart attack, hearing loss, osteoarthritis, osteoporosis, rheumatoid arthritis, or stroke. Participation was voluntary.
Data
All participants were evaluated using the Semistructured Clinical Interview for DSM-IV Axis I and Axis II Disorders (SCID-I and SCID-II),46 the 17-item Hamilton Depression Rating Scale (HDRS17)47 and the Montgomery-Asberg Depression Rating Scale (MADRS)48 for the assessment of depressive symptoms, the Hamilton Anxiety Rating Scale (HARS)49 for the assessment of anxiety symptoms, the Satisfaction With Life Scale (SWLS),50 and the Medical Outcomes Study 36-Item Short-Form Health Survey (SF-36)51 for the health-related quality-of-life measurements. Subjects were investigated only for anxiety and depressive symptoms, not using an interview, to classify individuals as meeting criteria for major depressive disorder or an anxiety disorder.
Assessment of Depression
HDRS17. The HDRS17,47 a 17-item clinician-rated scale, was used to evaluate depressive symptom severity. It includes confounding items (eg, pain complaints with fatigue or irritability and anxiety), weights some items over others (eg, 0-3 vs 0-5 scored items), and possesses other psychometric flaws. However, Iannuzzo et al,52 using Cicchetti and Sparrow’s 53 guidelines for evaluating reliability coefficients, obtained excellent total score reliability for the HDRS17 (intraclass correlation coefficient = 0.98).
MADRS. The MADRS was developed in response to some of the limitations of the HDRS and other approaches to measuring depression.48 Neither the HDRS17 nor the MADRS cover all 9 symptom domains needed to diagnose a major depressive episode according to the DMS-IV-TR. The MADRS, designed to be sensitive to treatment changes, is briefer and more uniform than the HDRS. A limitation of the MADRS is the lack of a structured interview, which may affect its reliability. However, the internal consistency of the MADRS is satisfactory, with a Cronbach α of 0.84. The deletion of any of the 9 items would not increase the internal consistency of the total score.48
SF-36. The SF-36 is a generic measure of health status and is widely used across the world. The SF-36 is a multi-item scale that assesses 8 health areas: physical functioning, role limitations due to physical problems, social functioning, bodily pain, general mental health, role limitations due to emotional problems, vitality, and general health perceptions. The SF-36 identifies functional problems coexisting with mood disorder symptoms and other common health problems in primary care patients. Its psychometric properties are well documented.51 Reliability estimates for physical and mental summary scores usually exceed 0.90.54
SWLS. The SWLS50 is a 5-item self-report measure of satisfaction with one’s life (ie, a measure of global life satisfaction). It measures life satisfaction as a cognitive-judgmental process rather than focusing on affect. The Cronbach α reliability for the scale is 0.87, and the test-retest reliability for a 2-month period is 0.82. The advantage of the SWLS is that it is less correlated with affect than other life satisfaction measures, and the respondents are free to judge various domains (eg, health or material wealth) and several feeling states (eg, loneliness) according to their own preferences. The scale’s Cronbach α is 0.75.55
Assessment of Suicidality
Suicidality was measured using the 3 following dimensions: suicide attempts, suicidal ideation, and suicidal lethality. Suicide attempts were classified as self-injurious behaviors considered clinically significant or requiring emergency medical assessment. Violent suicidal acts were those involving grave bodily injury that may well have resulted in death but for timely medical or surgical interventions and included use of firearms, hanging, jumping, and automobile wrecks. Suicidal ideation was patient-reported thoughts of wishing to be dead, and not merely preoccupation with death or potential ill health.
Suicidal lethality was evaluated using 3 levels of severity (level 1: vague to moderate suicidal ideation, no organized plan, and no expressed intent; level 2: moderate to intense ideation, vague plan, some intent, and no specific time frame; and level 3: intense ideation, organized plan, particularly if lethal such as shooting or hanging, and strong intent). Lethality was considered higher if there was a past history of suicide attempts. Other factors considered as potentially increasing lethality were a drug/alcohol abuse history, a history of suicide by family members, recent significant losses, and the presence of numerous stressors.
Statistical Analysis
Depressive symptom measure. One item of the MADRS and 1 item of the HDRS measure suicidal risk and ideation; these items were used to assess current suicidality. To avoid the strong correlation between measures of depression and suicide risk, we calculated the depression scores omitting the items measuring suicidal risk. The 1-tailed Pearson correlation coefficient between the HDRS and the MADRS scores was 0.76 (P < .001) (MADRS9 and HDRS16 Pearson r = 0.70, P < .001), indicating a strong convergence between these measures.
We performed 2 factor analyses (using a principal components extraction) on the measures of depression and suicidality to seek common factors explaining the variance. In the first factor analysis, only 1 factor had eigenvalues of 1 or higher (F1 initial eigenvalues = 1.70), explaining almost 85% of the variance. The factor loading was 0.833 for each measure. In the second factor analysis, only 1 factor had eigenvalues of 1 or higher (F1 initial eigenvalues = 1.82), explaining almost 91% of the variance of the suicidality measures. The factor loading was 0.907 for each measure. Depressive and suicidality factors are then used in all the bivariate and multivariate analyses.
Student t tests and Fisher exact tests were used to determine if there were mean differences between the groups. The Benjamin-Hochberg procedure was used to control for type 1 errors. Sequential regression analyses were used to test the impact of depressive symptoms, anxiety symptoms, suicidality, and other variables on the quality of life. To enter the suicidality factor in the sequential regression analysis, we dichotomized the variable: scores of 0 = lower suicidality and scores > 0 = higher suicidality.
RESULTS
Patient Characteristics
Two hundred forty patients with no history of psychopathology were consecutively admitted and included in the current study. Patients had not taken psychotropic drugs before recruitment into the present study and had no history of previous psychotropic medication. They were divided into 2 groups: 120 outpatients with CHF and 120 outpatients with hypertension. The CHF conditions included ischemic heart disease (57%), hypertension (19%), diabetes (12%), valvular heart disease (8%), and cardiomyopathy (4%). Subjects with CHF had a mean age of 59.7 years (range, 38-78 years; SD = 12.0); 79 (66%) were men, and 41 (34%) were women. Of the patients with CHF, 18 (15%) were in NYHA class I (no limitation of physical activity), 36 (30%) in NYHA class II (slight limitation of physical activity), 36 (30%) in NYHA class III (marked limitation of physical activity), and 30 (25%) in NYHA class IV (unable to carry out any physical activity without discomfort and symptoms of cardiac insufficiency at rest). Ninety-two (76.7%) CHF patients also had hypertension, 10 (12%) patients had diabetes, 6 (7.2%) had peripheral vascular disease, and 2 (2.4%) had COPD. The CHF patients had a mean duration of illness of 6.5 years (SD = 1), and a mean of 6.3 (SD = 2) previous hospitalizations because of hypertension (52%), paroxysmal nocturnal dyspnea and orthopnea (40%), and dizziness and confusion (8%).
Subjects with hypertension had a mean age of 60.8 years (range, 40 to 82 years; SD = 11); 62 (52%) were men and 58 (48%) were women. They had a mean duration of illness of 6.6 years (SD = 2) and a mean of 1.8 (SD = 1) previous hospitalizations. Ten (8.4%) patients were affected by secondary hypertension due to medical conditions (80% renal artery stenosis, 15% Cushing syndrome, and 5% hyperparathyroidism). None of the hypertension patients also had CHF. Five (6%) patients had diabetes, 1 (1.2%) had peripheral vascular disease, and 3 (3.6%) had COPD.
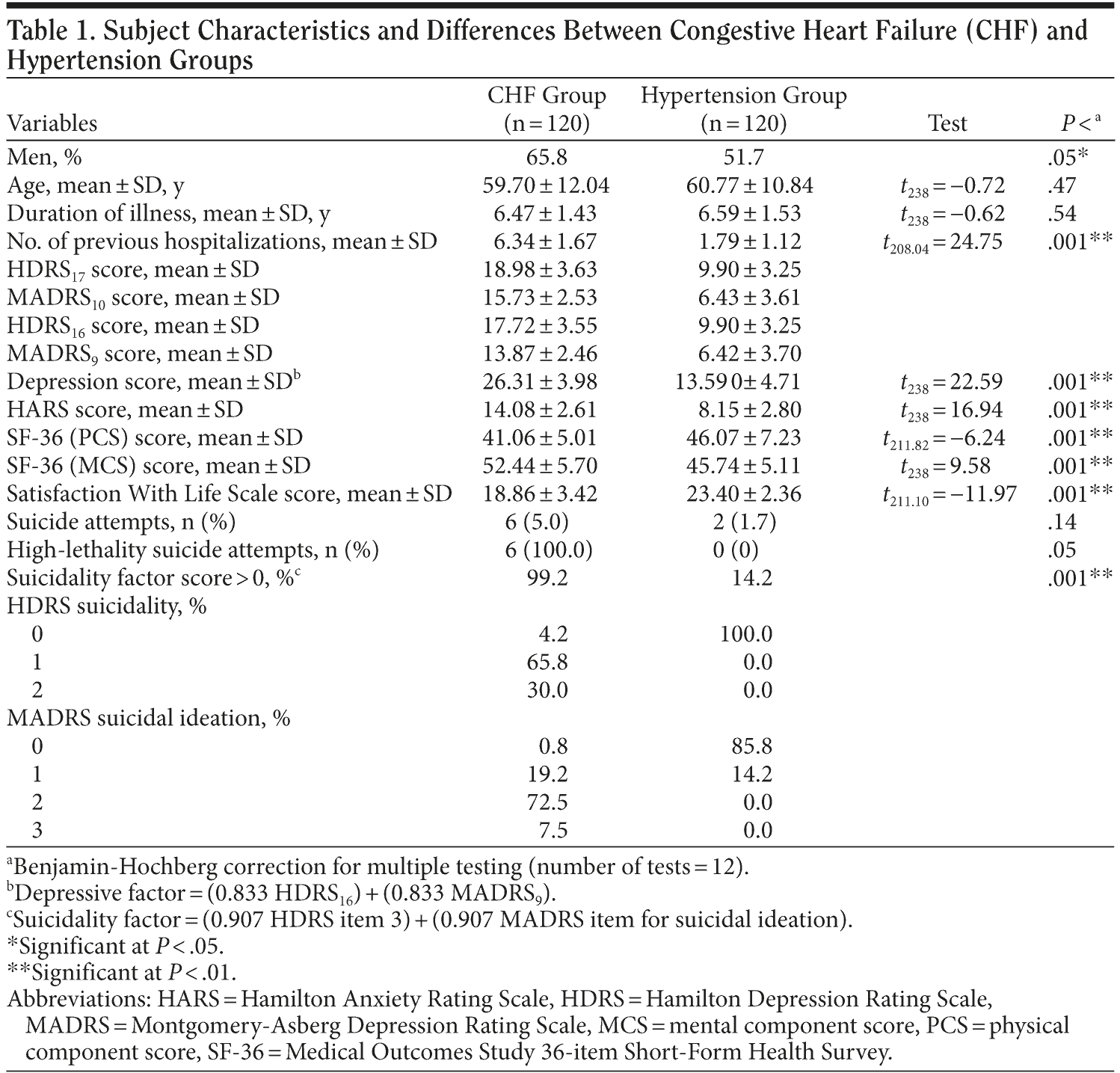
Differences between subjects with CHF and hypertension. The differences between patients with CHF (with or without hypertension) and hypertension (without CHF) are listed in Table 1. The 2 groups differed on several variables even after controlling for multiple testing. The CHF patients were more likely to be men (65.8% vs 51.7%; P < .02), had more previous hospitalizations (6.34 ± 1.67 vs 1.79 ± 1.12; t208.04 = 24.75; P < .001), had higher scores on the depressive factor (26.31 ± 3.98 vs 13.59 ± 4.71; t238 = 22.59; P < .001) and the HARS (14.08 ± 2.61 vs 8.15 ± 2.80; t238 = 16.94; P < .001), and had scores higher than 0 on the suicidality factor and higher suicidality (99.2% vs 14.2%; P < .001) than patients with hypertension.
Furthermore, patients with CHF had lower scores on the physical component score (PCS) (41.06 ± 5.01 vs 46.07 ± 7.23; t211.82 = −6.24; P < .001), higher scores on the mental component score (MCS) (52.44 ± 5.70 vs 45.74 ± 5.11; t238 = 9.58; P < .001), and lower scores on the SWLS (18.86 ± 3.42 vs 23.40 ± 2.36; t211.10 = −11.97; P < .001) than patients with hypertension. The 2 groups did not significantly differ in the number of suicide attempts after the diagnosis of CHF or hypertension (5.0% vs 1.7%), but the suicide attempts in CHF patients were more likely to have high lethality than those in hypertension patients (100.0% vs 0%; P < .04).
Correlation of SF-36 and SWLS measures. The 1-tailed Pearson correlation between the PCS and MCS scores was −0.49 (P = .0008), between PCS and the SWLS scores was 0.10 (P = .06), and between MCS and SWLS scores was −0.21 (P = .001).
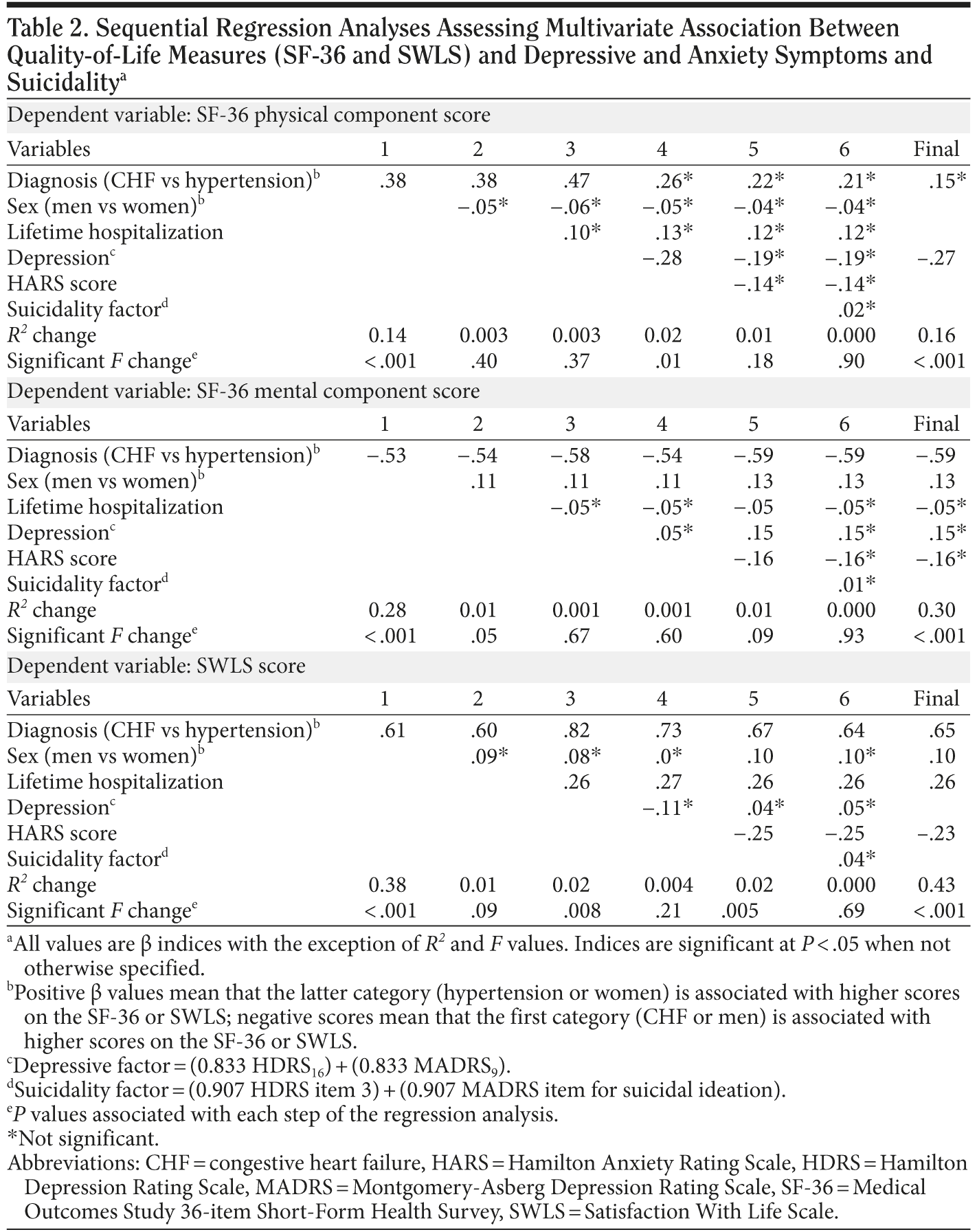
Relationship between depressive and anxiety symptoms, suicidality, and quality of life. To test the association between depressive symptoms, anxiety symptoms, and suicidality with the quality of life of the patients, 3 sequential regression analyses were performed (Table 2). For the PCS, only the diagnosis (CHF vs hypertension) and the depressive factor were significant predictors and, when combined, only the depressive factor predicted higher scores on the PCS (standardized β coefficient = −0.27; P = .012). For the MCS, diagnosis (CHF vs hypertension), sex (men vs women), lifetime hospitalizations, depressive factor, and HARS score were significant correlates, and, in the final model, CHF (standardized β coefficient = −0.59; P < .001) and sex (women) (standardized β coefficient = 0.13; P = .03) were significant predictors of higher scores on the MCS. For SLWS, diagnosis (CHF vs hypertension), sex (men vs women), lifetime hospitalizations, and HARS score were significant correlates and also significant predictors of the SWLS score in the final model. Hypertension (standardized β coefficient = 0.65; P < .001), sex (women) (standardized β coefficient = 0.10; P = .05), higher lifetime hospitalizations (standardized β coefficient = 0.26; P = .005), and higher HARS score (standardized β coefficient = −0.23; P = .002) were associated with higher scores on the SWLS.
DISCUSSION
Patients with CHF were more often hospitalized and showed more anxiety and higher suicidality than patients with hypertension. They were more physically ill and showed less satisfaction with life than patients with hypertension. Additionally, they had made more lethal suicide attempts than hypertension patients. In CHF patients, depressive symptom level was the only significant predictor of physical health, while diagnosis and sex were significant predictors of mental health. Satisfaction with life was predicted by group, lifetime hospitalizations, and HARS score.
The findings of the present study indicate that anxiety and depressive symptoms represent relevant predictors of poor quality of life in patients with chronic illnesses such as cardiovascular diseases. Additionally, we found that anxiety and depression symptoms were rarely detected or correctly treated by physicians. Only 2 (0.01%) of the patients of the present sample had had previous contact with psychiatric services. This finding should encourage physicians and psychiatrists to work together to correctly approach and manage complex and chronic diseases such as CHF and hypertension.
In our sample, the CHF patients had a higher level of disability than the hypertension patients. They experienced a higher level of physical disability and reported a worse quality of life, with impairment in movement and conducting ordinary activities. The CHF patients were more likely to be men, to have more previous hospitalizations, and to have made more high-lethality suicide attempts, although they had the same duration of illness.
Those individuals making highly lethal suicide attempts and having a greater injury burden could have had a bipolar disorder. In another study,56 high-lethality attempters reported greater suicidal intent and required inpatient medical treatment. Also, individuals with bipolar disorder who have made high-lethality attempts in the past more often make high-lethality attempts later and represent a subgroup of subjects at higher risk, so their identification and management are critical.56 In the present sample, the CHF patients were more anxious than the hypertension patients, and a higher anxiety symptom level was associated with both more suicide attempts and more lethal suicide attempts. In accord with these findings, the severity of anxiety does not appear to protect against the likelihood of suicide attempts or the lethality of suicide attempts as reported by a recent study.57 However, the sample size of suicide attempters did not allow definitive conclusions.
The role of anxiety in this subgroup appears to be critical. Anxiety was a significant predictor of lower satisfaction with life and was found to be associated with somatic phobias, death wishes, and somatic pain. CHF patients may view suicide as a reasonable solution for their somatic pain and disability. Only 2 (1.6%) subjects of both groups had had previous contact with psychiatric services. Most people who commit suicide have visited a physician in the month before the suicide, and these visits represent an opportunity to save people.58 None of the patients in the study by Faris et al58 committed suicide on the same day that they saw a psychiatrist. The 5 most common symptoms listed in the week before the suicide were anxiety, unspecified gastrointestinal symptoms, depression, unspecified cardiac symptoms, and hypertension. These symptoms could be considered to be early warning signs of unrecognized psychiatric disorders such as affective or anxiety disorders, which may increase the risk of suicide.
Juurlink et al59 observed a strong association between the cumulative number of illnesses and symptoms and the estimated risk of suicide. Compared with patients with no identified illness, for example, patients with 3 illnesses had about a 3-fold increase in the estimated risk of suicide, and patients with 5 illnesses had about a 5-fold increase in risk. Frierson60 noted that attempted suicide in elderly individuals with several coexisting medical problems is a major psychiatric problem. In their study, major depression was the most common psychiatric diagnosis in the CHF patients and COPD the most frequently noted physical ailment. Klein-Schwartz and Oderda61 found that patients with preexisting cardiovascular disease and severe somatic pains are at particular risk of worsening ischemic heart disease, congestive heart failure, and suicide attempts.
Relevant psychosocial factors may be important in developing anxiety, depression, and cardiovascular diseases. For example, patients’ beliefs about their illness should be adequately explored. Family stress, family coping, health stress, and the patient’s personality should be evaluated in order to predict life satisfaction. These variables taken together may produce an “at risk mental state” in which individuals may not be able to mobilize resources and coping abilities. This state may increase the patients’ suffering and lead them to perceive their illness as intolerable; therefore, suicide may appear as the only solution to their suffering and pain.
Similar to Juurlink et al,59 in the present study, the CHF patients who experienced a more chronic condition were more likely to attempt suicide with lethal methods than the hypertension patients.59 Physicians therefore should be aware of the risk of suicide among patients experiencing severe pain because patients may see suicide as the only way of escaping their suffering.
Study Limitations
The limitations of this study include its nonblinded design and lack of control groups. Also, the sample size was too small for a cross-sectional observational study. An additional limitation is the lack of follow-up. It would be interesting to monitor anxiety, depression, and risk of suicide in patients with cardiovascular diseases 12 or 24 months after baseline. However, the strength of the present study was that it was not based on spontaneous clinician reports about anxiety, depression, and quality of life but on reliable and valid psychometric assessments. As a result, the findings may be considered valid. Depressive symptoms were assessed using both the HDRS, designed to assess the severity of depression, and the MADRS, developed in response to some of the limitations of the HDRS. The 1-tailed Pearson correlation index between the HDRS and the MADRS was 0.76 (P < .001) (MADRS-9 by HDRS16 Pearson r = 0.70; P < .001), indicating a strong convergence among the measures of depression.
It was not possible to screen patients according to a classification of hypertension (grade 1 or mild hypertension ≥ 140 and/or ≥ 90-99; grade 2 or moderate hypertension 160-179 and/or 100-109; and grade 3 or severe hypertension ≥ 180 and/or ≥ 110; isolated systolic hypertension ≥ 140 and 90),45 and the distribution of CHF severity (NYHA classification) was heterogeneous.
Finally, in the present study, we could not investigate hopelessness and psychache as additional variables involved in increasing suicide risk. Furthermore, we did not assess suicide lethality.
CONCLUSION
Anxiety and depression frequently coexist with cardiovascular diseases and may have complex relationships. Our findings have important implications for prevention. Physicians, nurses, and other health care professionals should be alert to the quality of life related to patients with chronic illnesses who may have symptoms of depression and anxiety and a high risk for suicide. Our findings suggest the need for health professionals to screen patients with chronic illnesses in order to promote psychosocial rehabilitation and decrease the caregivers’ and patients’ stress.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration−approved labeling has been presented in this article.
Author affiliations: Department of Psychiatry (Drs Serafini, Pompili, Iacorossi, Cuomo, Vista, Girardi, and Tatarelli) and Department of Cardiology (Dr De Biase), Sant’ Andrea Hospital, Sapienza University of Rome (Drs Serafini, Pompili, Iacorossi, Cuomo, Vista, Girardi, De Biase, and Tatarelli); Universit× Europea di Roma (Dr Innamorati), Italy; McLean Hospital, Harvard Medical School, Boston, Massachusetts (Dr Pompili); and The Richard Stockton College of New Jersey, Pomona (Dr Lester).
Financial disclosure: Dr Serafini has served as a consultant to or received grant/research support from Bristol-Myers Squibb, Janssen-Cilag, Eli Lilly, and GlaxoSmithKline. Dr Pompili has served as a consultant to or received grant/research support from Eli Lilly and Organon. Dr Girardi has served as a consultant to or received grant/research support from AstraZeneca, Bristol-Myers Squibb, Eli Lilly, Janssen-Cilag, and Organon. Dr Tatarelli has served as a consultant to or received grant/research support from Bristol-Myers Squibb, Eli Lilly, Janssen-Cilag, Merck, and Servier. Drs Innamorati, Iacorossi, Cuomo, Vista, Lester, and De Biase have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: None reported.
This CME activity is expired. For more CME activities, visit cme.psychiatrist.com.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
REFERENCES
1. Congestive Heart Failure Worldwide Markets, Clinical Status and Product Development Opportunities. Lake Forest, CA: New Medicine, Inc; 1997:1-40.
2. American Heart Association. Heart and Stroke Statistical Update: 2001. Dallas, TX: American Heart Association; 2001.
3. Ho KKL, Pinsky JL, Kannel WB, et al. The epidemiology of heart failure: the Framingham Study. J Am Coll Cardiol. 1993;22(suppl A):6A-13A. PubMed
4. Redfield MM. Heart failure—an epidemic of uncertain proportions. N Engl J Med. 2002;347(18):1442-1444. PubMed doi:10.1056/NEJMe020115
5. Senni M, Tribouilloy CM, Rodeheffer RJ, et al. Congestive heart failure in the community: a study of all incident cases in Olmsted County, Minnesota, in 1991. Circulation. 1998;98(21):2282-2289. PubMed
6. Rich MW. Heart failure in the 21st century: a cardiogeriatric syndrome. J Gerontol A Biol Sci Med Sci. 2001;56(2):M88-M96. PubMed
7. Harwood D, Hawton K, Hope T, et al. Psychiatric disorder and personality factors associated with suicide in older people: a descriptive and case-control study. Int J Geriatr Psychiatry. 2001;16(2):155-165. PubMed doi:10.1002/1099-1166(200102)16:2<155::AID-GPS289>3.0.CO;2-0
8. SEOSI Investigators. Survey on heart failure in Italian hospital cardiology units: results of the SEOSI study. Eur Heart J. 1997;18(9):1457-1464. PubMed
9. McCarthy M, Lay M, Addington-Hall J. Dying from heart disease. J R Coll Physicians Lond. 1996;30(4):325-328. PubMed
10. McMurray JJV, Petrie MC, Murdoch DR, et al. Clinical epidemiology of heart failure: public and private health burden. Eur Heart J. 1998;19(suppl P):9-16. PubMed
11. Reddy KS. Hypertension control in developing countries: generic issues. J Hum Hypertens. 1996;10(suppl 1):S33-S38. PubMed
12. Criteria Committee of the New York Heart Association. Nomenclature and Criteria for Diagnosis of Diseases of the Heart and Great Vessels. 9th ed. Boston, MA: Little, Brown; 1994.
13. Kearney PM, Whelton M, Reynolds K, et al. Global burden of hypertension: analysis of worldwide data. Lancet. 2005;365(9455):217-223. PubMed
14. Mancia G, De Backer G, Dominiczak A, et al, The Task Force for the Management of Arterial Hypertension of the European Society of Hypertension, The Task Force for the Management of Arterial Hypertension of the European Society of Cardiology. 2007 Guidelines for the Management of Arterial Hypertension: The Task Force for the Management of Arterial Hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). Eur Heart J. 2007;28(12):1462-1536. PubMed
15. O’ Donnell CJ, Ridker PM, Glynn RJ, et al. Hypertension and borderline isolated systolic hypertension increase risks of cardiovascular disease and mortality in male physicians. Circulation. 1997;95(5):1132-1137. PubMed
16. Jacobi F, Höfler M, Meister W, et al. Prevalence, detection and prescribing behavior in depressive syndromes: a German federal family physician study. Nervenarzt. 2002;73(7):651-658. PubMed doi:10.1007/s00115-002-1299-y
17. Ansseau M, Dierick M, Buntinkx F, et al. High prevalence of mental disorders in primary care. J Affect Disord. 2004;78(1):49-55. PubMed doi:10.1016/S0165-0327(02)00219-7
18. Runkewitz K, Kirchmann H, Strauss B. Anxiety and depression in primary care patients: predictors of symptom severity and developmental correlates. J Psychosom Res. 2006;60(5):445-453. PubMed doi:10.1016/j.jpsychores.2005.09.003
19. Saravay SM, Lavin M. Psychiatric comorbidity and length of stay in the general hospital: a critical review of outcome studies. Psychosomatics. 1994;35(3):233-252. PubMed
20. Robinson WD, Geske JA, Prest LA, et al. Depression treatment in primary care. J Am Board Fam Pract. 2005;18(2):79-86. PubMed doi:10.3122/jabfm.18.2.79
21. Andersson SJ, Troein M, Lindberg G. General practitioners’ conceptions about treatment of depression and factors that may influence their practice in this area: a postal survey. BMC Fam Pract. 2005;6(1):21. PubMed doi:10.1186/1471-2296-6-21
22. Elliott RL. Depression in primary care. Ethn Dis. 2007;17(suppl 2):S2-S28, S33. PubMed
23. Hoyer J, Wittchen HU. Generalized anxiety disorders in primary medical care. Versicherungsmedizin. 2003;55(3):127-135. PubMed
24. Meyer T, Klemme H, Herrmann C. Depression but not anxiety is a significant predictor of physicians’ assessments of medical status in physically ill patients. Psychother Psychosom. 2000;69(3):147-154. PubMed doi:10.1159/000012383
25. Rozanski A, Blumenthal JA, Kaplan J. Impact of psychological factors on the pathogenesis of cardiovascular disease and implications for therapy. Circulation. 1999;99(16):2192-2217. PubMed
26. Deepa R, Shanthirani CS, Pradeepa R, et al. Is the ‘ rule of halves’ in hypertension still valid?—evidence from the Chennai Urban Population Study. J Assoc Physicians India. 2003;51:153-157. PubMed
27. Coryell C. Fraser- Smith N. Panic disorders and cardiac disease. Circulation. 2000;347:3456-3467.
28. Murberg TA, Bru E, Svebak S, et al. Depressed mood and subjective health symptoms as predictors of mortality in patients with congestive heart failure: a two-years follow-up study. Int J Psychiatry Med. 1999;29(3):311-326. PubMed doi:10.2190/0C1C-A63U-V5XQ-1DAL
29. Murberg TA, Bru E. Social relationships and mortality in patients with congestive heart failure. J Psychosom Res. 2001;51(3):521-527. PubMed doi:10.1016/S0022-3999(01)00226-4
30. Jiang W, Alexander J, Christopher E, et al. Relationship of depression to increased risk of mortality and rehospitalization in patients with congestive heart failure. Arch Intern Med. 2001;161(15):1849-1856. PubMed doi:10.1001/archinte.161.15.1849
31. Lett HS, Blumenthal JA, Babyak MA, et al. Depression as a risk factor for coronary artery disease: evidence, mechanisms, and treatment. Psychosom Med. 2004;66(3):305-315. PubMed doi:10.1097/01.psy.0000126207.43307.c0
32. Jiang W, Kuchibhatla M, Cuffe MS, et al. Prognostic value of anxiety and depression in patients with chronic heart failure. Circulation. 2004;110(22):3452-3456. PubMed doi:10.1161/01.CIR.0000148138.25157.F9
33. Moser DK. Psychosocial factors and their association with clinical outcomes in patients with heart failure: why clinicians do not seem to care. Eur J Cardiovasc Nurs. 2002;1(3):183-188. PubMed doi:10.1016/S1474-5151(02)00033-6
34. Opasich C, De Feo S, Barbieri M, et al. Health care quality in terminal cardiac decompensation: a “multidisciplinary” reflexion. Ital Heart J suppl. 2003;4(2):112-118. PubMed
35. Conwell Y, Duberstein PR, Caine ED. Risk factors for suicide in later life. Biol Psychiatry. 2002;52(3):193-204. PubMed doi:10.1016/S0006-3223(02)01347-1
36. Beautrais AL. A case control study of suicide and attempted suicide in older adults. Suicide Life Threat Behav. 2002;32(1):1-9. PubMed doi:10.1521/suli.32.1.1.22184
37. Waern M, Rubenowitz E, Runeson B, et al. Burden of illness and suicide in elderly people: case-control study. BMJ. 2002a;324(7350):1355. PubMed doi:10.1136/bmj.324.7350.1355
38. Waern M, Runeson BS, Allebeck P, et al. Mental disorder in elderly suicides: a case-control study. Am J Psychiatry. 2002b;159(3):450-455. PubMed doi:10.1176/appi.ajp.159.3.450
39. Welch SS. A review of the literature on the epidemiology of parasuicide in the general population. Psychiatr Serv. 2001;52(3):368-375. PubMed doi:10.1176/appi.ps.52.3.368
40. King RA, Schwab-Stone M, Flisher AJ, et al. Psychosocial and risk behavior correlates of youth suicide attempts and suicidal ideation. J Am Acad Child Adolesc Psychiatry. 2001;40(7):837-846. PubMed doi:10.1097/00004583-200107000-00019
41. Goldney RD, Wilson D, Dal Grande E, et al. Suicidal ideation in a random community sample: attributable risk due to depression and psychosocial and traumatic events. Aust N Z J Psychiatry. 2000;34(1):98-106. PubMed doi:10.1046/j.1440-1614.2000.00646.x
42. Rost K, Zhang M, Fortney J, et al. Persistently poor outcomes of undetected major depression in primary care. Gen Hosp Psychiatry. 1998;20(1):12-20. PubMed doi:10.1016/S0163-8343(97)00095-9
43. Artinian NT, Magnan M, Christian W, et al. What do patients know about their heart failure? Appl Nurs Res. 2002;15(4):200-208. PubMed doi:10.1053/apnr.2002.35959
44. Rector TS, Cohn JN; Pimobendan Multicenter Research Group. Assessment of patient outcome with the Minnesota Living with Heart Failure Questionnaire: reliability and validity during a randomized, double-blind, placebo-controlled trial of pimobendan. Am Heart J. 1992;124(4):1017-1025. PubMed doi:10.1016/0002-8703(92)90986-6
45. European Society of Hypertension-European Society of Cardiology Guidelines Committee. 2003 European Society of Hypertension-European Society of Cardiology guidelines for the management of arterial hypertension. J Hypertens. 2003;21(6):1011-1053. PubMed doi:10.1097/00004872-200306000-00001
46. Williams JB, Gibbon M, First MB, et al. The Structured Clinical Interview for DSM-III-R (SCID): II. multisite test-retest reliability. Arch Gen Psychiatry. 1992;49(8):630-636. PubMed
47. Hamilton M. A rating scale for depression. J Neurol Neurosurg Psychiatry 1960;23:56-62. PubMed
48. Fantino B, Moore N. The self-reported Montgomery-Åsberg Depression Rating Scale is a useful evaluative tool in major depressive disorder. BMC Psychiatry. 2009;9(1):26. PubMed doi:10.1186/1471-244X-9-26
49. Hamilton M. The assessment of anxiety states by rating. Br J Med Psychol. 1959;32(1):50-55. PubMed
50. Diener E, Emmons RA, Larsen RJ, et al. The Satisfaction With Life Scale. J Pers Assess. 1985;49(1):71-75. PubMed doi:10.1207/s15327752jpa4901_13
51. Ware JE Jr, Sherbourne CD. The MOS 36-item Short-Form health survey (SF-36). I: conceptual framework and item selection. Med Care. 1992;30(6):473-483. PubMed doi:10.1097/00005650-199206000-00002
52. Iannuzzo RW, Jaeger J, Goldberg JF, et al. Development and reliability of the HAM-D/MADRS interview: an integrated depression symptom rating scale. Psychiatry Res. 2006;145(1):21-37. PubMed doi:10.1016/j.psychres.2005.10.009
53. Cicchetti DV, Sparrow SA. Developing criteria for establishing interrater reliability of specific items: applications to assessment of adaptive behavior. Am J Ment Defic. 1981;86(2):127-137. PubMed
54. McHorney CA, Ware JE Jr, Lu JF, et al. The MOS 36-item Short-Form Health Survey (SF-36): III. tests of data quality, scaling assumptions, and reliability across diverse patient groups. Med Care. 1994;32(1):40-66. PubMed doi:10.1097/00005650-199401000-00004
55. Requena Hernסndez C, López Fernסndez V, Gonzסlez Boto R, et al. Psychometric properties of the satisfaction with life scale in active elderly women. Rev Esp Geriatr Gerontol. 2009;44(3):146-148. PubMed
56. Oquendo MA, Carballo JJ, Rajouria N, et al. Are high-lethality suicide attempters with bipolar disorder a distinct phenotype? Arch Suicide Res. 2009;13(3):247-256. PubMed doi:10.1080/13811110903044385
57. Nakagawa A, Grunebaum MF, Oquendo MA, et al. Clinical correlates of planned, more lethal suicide attempts in major depressive disorder. J Affect Disord. 2009;112(1-3):237-242. PubMed doi:10.1016/j.jad.2008.03.021
58. Faris R, Purcell H, Henein MY, et al. Clinical depression is common and significantly associated with reduced survival in patients with non-ischaemic heart failure. Eur J Heart Fail. 2002;4(4):541-551. PubMed doi:10.1016/S1388-9842(02)00101-0
59. Juurlink DN, Herrmann N, Szalai JP, et al. Medical illness and the risk of suicide in the elderly. Arch Intern Med. 2004;164(11):1179-1184. PubMed doi:10.1001/archinte.164.11.1179
60. Frierson RL. Suicide attempts by the old and the very old. Arch Intern Med. 1991;151(1):141-144. PubMed doi:10.1001/archinte.151.1.141
61. Klein-Schwartz W, Oderda GM. Poisoning in the elderly: epidemiological, clinical and management considerations. Drugs Aging. 1991;1(1):67-89. PubMed doi:10.2165/00002512-199101010-00008