Increased Use of Antidepressants in Women Decreases Suicides in Men: An Ecological Study

ABSTRACT
Objective: The suicide rate has decreased in many countries, while the use of antidepressants has increased. In our previous study, the decrease in suicide rate between 1994 and 2001 was greater in men than in women, but the increase in use of antidepressants was greater in women than in men. We hypothesized that the increase in the use of antidepressants in women associates with the decrease in suicide rate in men.
Method: Population-based suicide rate and reimbursed antidepressant prescriptions, an indicator of antidepressant use, between 1994 and 2001 in Finland were analyzed in the whole population. Variance in the suicide rates in men and women was explained by antidepressant prescriptions for men and women, age, time period, and geographical region in Poisson regression analyses.
Results: The decrease in suicide rate in men associated significantly with the increase in antidepressant prescriptions in women even though the model took into account the effect of increased antidepressant prescriptions in men, as well as the effects of age, time, and region (risk ratio [RR] = 0.70, P = .004, in the model without age; RR = 0.89, P = .048 in the complete model). However, the decrease in suicide rate in women did not associate with the increase in antidepressant prescriptions in men.
Conclusions: Increased prescription of antidepressants in women associates with a decreased suicide rate in men. Increased use of antidepressive medication in women may decrease depressiveness in their microsocieties and thereby reduce the risk of suicides also in men.
Prim Care Companion CNS Disord 2012;14(3):doi:10.4088/PCC.11m01256
© Copyright 2012 Physicians Postgraduate Press, Inc.
Submitted: July 19, 2011; accepted November 28, 2011.
Published online: May 10, 2012.
Corresponding author: Raimo K. R. Salokangas, MD, PhD, Department of Psychiatry, Turku University Central Hospital, 20520 Turku, Finland ([email protected]).
Depression is one of the most important clinical risk factors for suicide.1 In the general population, depression is more prevalent in women than in men,2 but men commit suicide much more often than women.3 In the 1990s, concurrently with the increased use of new-generation antidepressants, the suicide rate decreased in many countries.4 In our previous study,5 the decline in suicide rate in men associated with increased use of antidepressants (measured by reimbursed prescriptions) in men, and, correspondingly, the decline in suicide rate in women associated with increased use of antidepressants in women. However, the suicide rate declined more in men than in women, while use of antidepressants increased more in women than in men. How can this discrepancy be explained?
Mental problems accumulate in social networks. Suicide and depression tend to spread in a peer-to-peer fashion,6 and people’s happiness seems to depend on the happiness of others with whom they are connected.7 Thus, it is possible that effective treatment of a depressive person may decrease the depressiveness of another person who is not treated but who belongs to the same social network, ie, microsociety. It is possible that this indirect treatment effect could also prevent suicide candidates from committing suicide.
Our hypothesis was that the increase in use of antidepressants, indicated by reimbursed antidepressant prescriptions, in women associates significantly with the decline in suicide rate in men. This hypothesis was tested using the nationwide data on completed suicides and antidepressant prescriptions between 1994 and 2001 in Finland.
METHOD
The causes of death8 were obtained from the death certificates issued by physicians and collected annually by Statistics Finland. In the case of suicide, the certificate is based on a forensic autopsy. The data filed in Statistics Finland also comprise information on sex, age, and region in which the deceased lived, as well as various other demographic data.
Statistics Finland provided the data on the annual number of completed suicides in the 22 health care districts of Finland and the corresponding number of inhabitants from 1994 to 2001. The data for the 22 health care districts, comprising separate information for men and women and for 5 age-group categories, were grouped into 5 regional social security areas. In 1994, the populations for the regional social security areas were 1,845,847 (South Finland), 1,131,443 (Southwest Finland), 708,247 (West Finland), 751,554 (East Finland), 655,059 (North Finland), and 5,092,150 (all). The corresponding rates for suicides per 100,000 people were 28.60 (South Finland), 26.22 (Southwest Finland), 32.58 (West Finland), 19.46 (East Finland), 26.79 (North Finland), and 27.26 (all).
The Finnish Social Insurance Institution9 provides nationwide social insurance for the whole population of Finland and pays a refund for the purchase of prescription drugs to everyone in Finland. The prescription register also includes information on the gender, residence, and age (in 5 categories) of the person purchasing the drug. Annual data, comprising only reimbursed antidepressant prescriptions in outpatient care, but not hospital care, were calculated as defined daily doses.

- Depression is not limited to individuals. It is also contagious and may extend to people who are close to the patient.
- Effective interventions for a patient’s depression may also reduce stress, depressiveness, and suicidality in the patient’s close interpersonal network.
- In addition to the individual patient, clinicians should take into account the patient’s interpersonal network when treating depression.
Statistical analyses were performed using Poisson regression.10 In multivariate analyses, variation in suicide rate (as dependent variable) was explained by the course of time (1 year = 1 unit), age group, region (confounding variables), and number of prescriptions of antidepressive drugs per population (multiplied by 10) (independent variables and indicators of use of antidepressants). In these analyses, variation in suicide rate in men was explained by age and region, as well as by antidepressant prescriptions in men and women. Correspondingly, the variation in suicide rate in women was explained by age group and region, as well as by antidepressant prescriptions in women and men. A P value less than .05 was regarded as significant. Statistical analyses were carried out using SAS System software, version 8.2 (SAS Institute, Cary, North Carolina). The study method is described in detail in our previous article.5
RESULTS
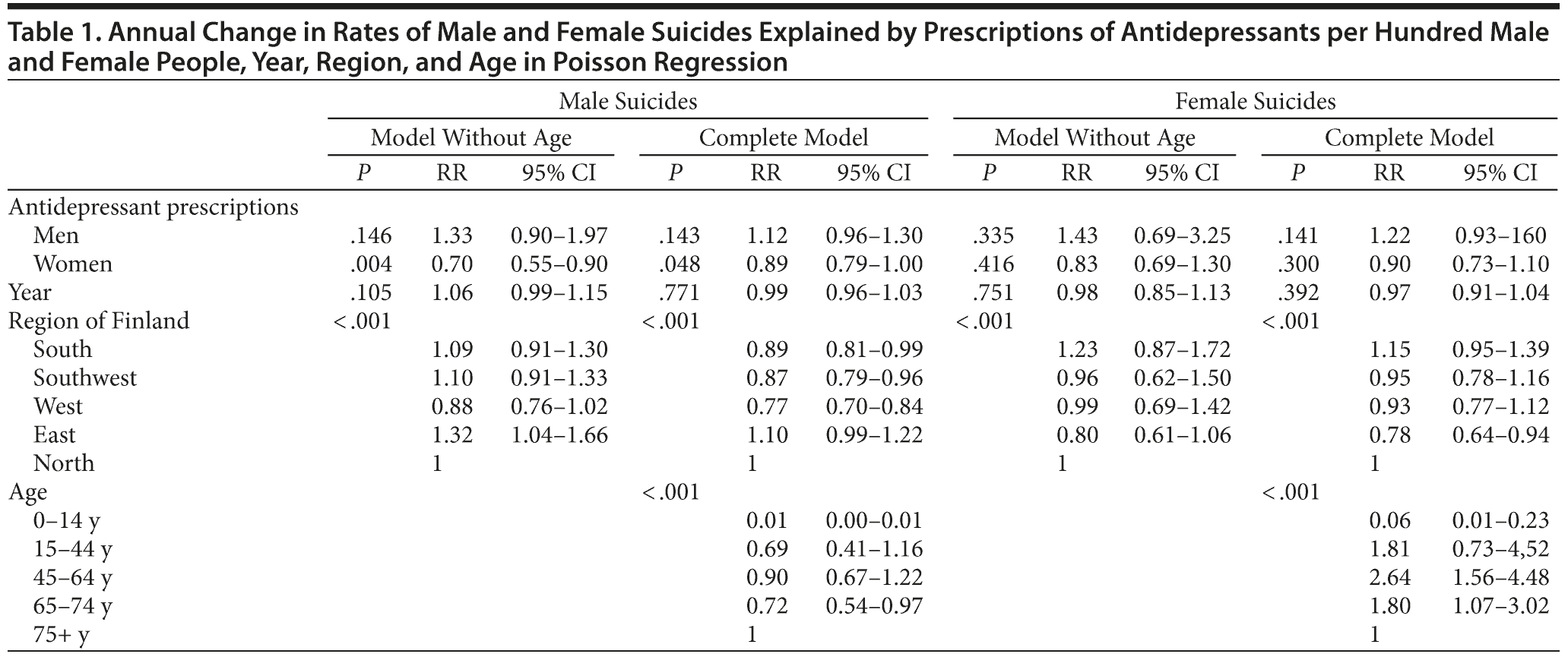
In the model without age, annual change in suicide rate in men was explained significantly by antidepressant prescriptions in women (risk ratio = 0.70, P = .004) and region. In the complete model, antidepressant prescriptions in women significantly explained suicide rate in men (risk ratio = 0.89, P = .048) even though the effects of antidepressant prescriptions in men and confounding variables were taken into account (Table 1). The suicide rate in women was significantly explained only by region and age, as shown in Table 1.
DISCUSSION
The results of the present study supported our hypothesis: the decreased time trend of suicides in men associated with increased use of antidepressants in women even though the study controlled for the effects of use of antidepressants in men and confounding factors. Use of antidepressants was indicated by purchased prescriptions of antidepressive drugs. To our knowledge, this is the first study suggesting that, at the national level, increased use of antidepressive drugs in women may reduce suicides in men. It is possible that increased use of antidepressants in women, in addition to decreasing their own depressiveness and anxiety, also leads to decreased depressiveness in their close social networks, thereby decreasing stress and suicidality in men belonging to this network. Further, decreased depressiveness in microsocieties may be seen as decreased suicidal behavior in men in society as a whole. It is also possible that increased use of antidepressants in women improves depressive men’s willingness to accept antidepressive drug treatment.
Depression is one of the most common psychiatric disorders in society. However, depression is not limited to individuals; it is also contagious. Healthy subjects who conversed on the telephone with a depressed patient became more depressed, anxious, hostile, and rejecting than when they conversed with nondepressive patients or healthy controls.11 In 2 studies, roommates living with depressive students became depressive themselves.12,13 Further, elevation of depressive symptoms in children has been followed by elevation of depressive syndromes in parents,14 and a peer’s depressive symptoms predicted an increase in adolescents’ depressive symptoms.15 In elderly couples, depression in one spouse predicted similar depression in the other spouse.16 It seems, however, that the association between spouses is not symmetric. In a sample of older couples, the husband’s depression was associated with the well-being of his wife, but the wife’s depression was rarely associated with the husband’s well-being.17 Clinical studies suggest that depression and other psychiatric and interpersonal problems are common within the close network of depressive and suicidal subjects.18-21 Additionally, in a random sample of the general population in Finland, the major depressive episode of the study subjects was associated with their spouse’s major depressive episode.22
Like depressiveness, happiness can also spread within a social network. Having a friend who lived within a mile and who became happy greatly increased the probability that a person was happy.7 Similar effects were seen in coresident spouses, siblings who lived within a mile of each other, and next-door neighbors, but not in coworkers.7 The authors concluded that people’s happiness depends on the happiness of others with whom they are connected. It is also possible that effective intervention in an individual with depression reduces depressiveness in her close, as well as her extended, social network. Christakis23 has suggested that the effect of health care on a patient has both positive and negative collateral health effects, health externalities, via the patient’s social ties.
Antidepressants may also have an unwanted effect. There is some evidence that use of antidepressants may induce mania or hypomania in subjects with depression and lead to psychosocial problems in their close networks. In a meta-analysis, the overall risk of mania in patients using antidepressants was 12.7%, while the corresponding risk in patients not using antidepressants was 7.5%.24 However, a beneficial effect of antidepressants on an individual’s depression and possibly on his or her network is more frequent. In children and adolescents, antidepressants may induce suicidal ideas and behavior. Compared to the risk in adults, the increased risk of suicidality in adolescents is weak but consistent. However, epidemiologic studies do not support a relationship between use of antidepressants and suicide rate.25 The present study controlled for the effect of age, and young age associated with decreased, not increased, suicide rate.5
Depression is more prevalent in women than in men.2 Depression is also one of the most important risk factors for suicides, but suicides are more frequent in men than in women.1 Women have larger social networks than men, although the meaning of these networks with regard to their health is not uniform.26 Following the reasoning above, it is expected that when female individuals become depressed, depressiveness also increases in their interpersonal network and leads to increased risk of suicide among male network members. On the other hand, when depressive females have received effective drug and/or psychosocial intervention for their depression, depressiveness decreases in their social network, and the risk of suicide decreases in their male network members. This favorable effect can be seen as decreased numbers of male suicides at the national level.
Limitations of Study
The prescription register of the Finnish Social Insurance Institution provides an accurate and comprehensive picture of the sale of drugs in Finland. The reliability of the suicide statistics in Finland is high,27 and the number of undetermined deaths is low.28 The major limitation of the study relates to the ecological database. We were not able to couple the data on antidepressant prescriptions and completed suicides individually, and therefore we cannot be sure that the suicide rate decreased only among those who started to use antidepressants. Nor were we able to evaluate the social networks of subjects using antidepressants, or the suicide rate in these networks specifically. Thus, the results and conclusions should be considered preliminary: investigating causal relations requires other kinds of study designs.
CONCLUSIONS
Our study suggests that, at the national population level, increased use of antidepressants in women associates with a decreased suicide rate in men. It is possible that increased use of antidepressive medication in women leads to a decrease in stress and depressiveness in their microsocieties, thereby also reducing the risk of suicides in men belonging to their close social network.
Author affiliations: Departments of Psychiatry (Drs Salokangas and Korkeila) and Biostatistics (Messrs Korpelainen and Helenius), University of Turku, Turku; Population Studies Unit, Department of Chronic Diseases Prevention, National Institute for Health and Welfare, Turku (Dr Salminen); Department of Psychiatry, University Central Hospital, Turku (Dr Salokangas); Psychiatric Clinic, Turku City Hospital, Turku (Dr Salokangas); and Department of Psychiatry, Harjavalta Hospital, Harjavalta (Dr Korkeila), Finland.
Potential conflicts of interest: None reported.
Support/funding: A researcher-applied unrestricted scholarship from the Eli Lilly Foundation, Finland, was received for this study.
Acknowledgment: The authors thank the Chief of Health Research, Research Professor Timo Klaukka, MD, PhD (deceased), from the Research Department, Social Insurance Institution, for help in acquiring the necessary data on antidepressant prescriptions.
REFERENCES
1. Isometsä ET, Henriksson MM, Aro HM, et al. Suicide in major depression. Am J Psychiatry. 1994;151(4):530-536. PubMed
2. Smith AL, Weissman MM. Epidemiology. In: Paykel ES, ed. Handbook of Affective Disorders. 2nd ed. Cambridge, England: Churchill Livingstone, 1992:111-129
3. Heikkinen ME, Isometsä ET, Marttunen MJ, et al. Social factors in suicide. Br J Psychiatry. 1995;167(6):747-753. PubMed doi:10.1192/bjp.167.6.747
4. Isacsson G. Suicide prevention—a medical breakthrough? Acta Psychiatr Scand. 2000;102(2):113-117. PubMed doi:10.1034/j.1600-0447.2000.102002113.x
5. Korkeila J, Salminen JK, Hiekkanen H, et al. Use of antidepressants and suicide rate in Finland: an ecological study. J Clin Psychiatry. 2007;68(4):505-511. PubMed doi:10.4088/JCP.v68n0403
6. Andrews JA, Tildesley E, Hops H, et al. The influence of peers on young adult substance use. Health Psychol. 2002;21(4):349-357. PubMed doi:10.1037/0278-6133.21.4.349
7. Fowler JH, Christakis NA. Dynamic spread of happiness in a large social network: longitudinal analysis over 20 years in the Framingham Heart Study. BMJ. 2008;337:a2338. PubMed doi:10.1136/bmj.a2338
8. Statistics Finland. Causes of Death 2002 [in Finnish]. Helsinki, Finland: Multiprint; 2003. http://www.stat.fi/index_en.html
9. National Agency for Medicines and Social Insurance Institution. Finnish Statistics on Medicines, Reports From 1991 to 2002. Helsinki, Finland: Edita; 1992-2003.
10. McCullagh P, Nelder JA. Generalized Linear Models. 2nd ed. London, England: Chapman and Hall; 1989.
11. Coyne JC. Depression and the response of others. J Abnorm Psychol. 1976;85(2):186-193. PubMed doi:10.1037/0021-843X.85.2.186
12. Howes MJ, Hokanson JE, Loewenstein DA. Induction of depressive affect after prolonged exposure to a mildly depressed individual. J Pers Soc Psychol. 1985;49(4):1110-1113. PubMed doi:10.1037/0022-3514.49.4.1110
13. Joiner TE Jr. Contagious depression: existence, specificity to depressed symptoms, and the role of reassurance seeking. J Pers Soc Psychol. 1994;67(2):287-296. PubMed doi:10.1037/0022-3514.67.2.287
14. Abela JR, Zinck S, Kryger S, et al. Contagious depression: negative attachment cognitions as a moderator of the temporal association between parental depression and child depression. J Clin Child Adolesc Psychol. 2009;38(1):16-26. PubMed doi:10.1080/15374410802575305
15. van Zalk MH, Kerr M, Branje SJ, et al. Peer contagion and adolescent depression: the role of failure anticipation. J Clin Child Adolesc Psychol. 2010;39(6):837-848. PubMed doi:10.1080/15374416.2010.517164
16. Goodman CR, Shippy RA. Is it contagious? affect similarity among spouses. Aging Ment Health. 2002;6(3):266-274. PubMed doi:10.1080/13607860220142431
17. Stimpson JP, Peek MK, Markides KS. Depression and mental health among older Mexican American spouses. Aging Ment Health. 2006;10(4):386-393. PubMed doi:10.1080/13607860500410060
18. Zweig RA, Hinrichsen GA. Factors associated with suicide attempts by depressed older adults: a prospective study. Am J Psychiatry. 1993;150(11):1687-1692. PubMed
19. Levkovitz V, Fennig S, Horesh N, et al. Perception of ill spouse and dyadic relationship in couples with affective disorder and those without. J Affect Disord. 2000;58(3):237-240. PubMed doi:10.1016/S0165-0327(99)00118-4
20. Hecht H, Genzw×¼rker S, Helle M, et al. Social functioning and personality of subjects at familial risk for affective disorder. J Affect Disord. 2005;84(1):33-42. PubMed doi:10.1016/j.jad.2004.09.002
21. Johnson JG, Cohen P, Gould MS, et al. Childhood adversities, interpersonal difficulties, and risk for suicide attempts during late adolescence and early adulthood. Arch Gen Psychiatry. 2002;59(8):741-749. PubMed doi:10.1001/archpsyc.59.8.741
22. Lindeman SM, Hirvonen JI, Hakko HH, et al. Use of the National Register of medico-legal autopsies in epidemiological suicide research. Int J Legal Med. 1995;107(6):306-309. PubMed doi:10.1007/BF01246878
23. Christakis NA. Social networks and collateral health effects. BMJ. 2004;329(7459):184-185. PubMed doi:10.1136/bmj.329.7459.184
24. Tondo L, Vסzquez G, Baldessarini RJ. Mania associated with antidepressant treatment: comprehensive meta-analytic review. Acta Psychiatr Scand. 2010;121(6):404-414. PubMed doi:10.1111/j.1600-0447.2009.01514.x
25. Masi G, Liboni F, Brovedani P. Pharmacotherapy of major depressive disorder in adolescents. Expert Opin Pharmacother. 2010;11(3):375-386. PubMed doi:10.1517/14656560903527226
26. Kawachi I, Berkman LF. Social ties and mental health. J Urban Health. 2001;78(3):458-467. PubMed doi:10.1093/jurban/78.3.458
27. Lindeman S, Kaprio J, Isometsä E, et al. Spousal resemblance for history of major depressive episode in the previous year. Psychol Med. 2002;32(2):363-367. PubMed doi:10.1017/S0033291701004780
28. ×–hberg A, Lönnqvist J. Suicides hidden among undetermined deaths. Acta Psychiatr Scand. 1998;98(3):214-218. PubMed doi:10.1111/j.1600-0447.1998.tb10069.x