Background: Psoriasis is an immune-mediated, chronic disease with a genetic background that involves skin, nails, and joints. The incidence of psoriasis varies from 2.0% to 4.0% depending on the geographical location, ethnic background, and environmental conditions. Recent research has proved that psoriasis is a systemic inflammatory disease with extensive systemic implications. Objectives of the study were to explore the severity of psoriasis, dermatology-related quality of life, and psychiatric health of the patients with reference to sociodemographic, lifestyle, and clinical characteristics.
Method: Consecutive patients with psoriasis (ICD-10 criteria) from skin outpatient clinics of 3 tertiary care hospitals in Lahore, Pakistan, between November 1, 2012, and December 31, 2012, were assessed in this prospective cross-sectional study. The final sample includes 87 patients who were evaluated for severity of psoriasis (Psoriasis Area Severity Index [PASI]), dermatology-related quality of life (Dermatology Life Quality Index [DLQI]), and psychiatric morbidity (12-item General Health Questionnaire [GHQ-12]) and were assessed on 23 sociodemographic, lifestyle, and clinical variables.
Results: Of the 23 variables, the PASI was significantly associated with education and habit of drinking alcohol (P < .05), the DLQI was significantly associated with disturbed eating (P < .05), and the GHQ-12 score was significantly associated with hair disease (P < .05), current income (P < .05), and disturbed eating and sleeping (P < .01). The PASI, DLQI, and GHQ-12 were not usually affected by sociodemographic, lifestyle, and clinical factors, except for some variables such as education of the patient, alcohol intake, eating and sleeping disturbance, and income status. A statistically significant correlation (P < .01) was found between all 3 scores (ie, PASI, DLQI, and GHQ-12). The correlation coefficients of the PASI with the DLQI and GHQ-12 are 0.345 and 0.460, respectively, and that of the DLQI with the GHQ-12 is 0.635. A moderating effect of the DLQI score was found on the relationship between the PASI and GHQ-12 scores.
Conclusions: Psoriasis has an immense impact on the life of patients and common comorbidities in psoriasis including coronary heart disease, depression, cerebrovascular disease, and metabolic syndrome. Screening for these comorbidities in psoriasis patients is essential. Impaired quality of life negatively affects the psyche of patients and initiates coping mechanisms, which may lead to depression and anxiety, social dysfunction, and loss of confidence, and the psychosocial burden of the disease may become more than the physical burden. The dermatologist usually manages physical disease and fails to address the social, emotional, and psychological aspects. Quality of life improves if these psychological aspects are also properly dealt with.
Disease Severity, Quality of Life, and Psychiatric
Morbidity in Patients With Psoriasis With Reference to Sociodemographic, Lifestyle, and Clinical Variables:
A Prospective, Cross-Sectional Study From Lahore, Pakistan
ABSTRACT
Background: Psoriasis is an immune-mediated, chronic disease with a genetic background that involves skin, nails, and joints. The incidence of psoriasis varies from 2.0% to 4.0% depending on the geographical location, ethnic background, and environmental conditions. Recent research has proved that psoriasis is a systemic inflammatory disease with extensive systemic implications. Objectives of the study were to explore the severity of psoriasis, dermatology-related quality of life, and psychiatric health of the patients with reference to sociodemographic, lifestyle, and clinical characteristics.
Method: Consecutive patients with psoriasis (ICD-10 criteria) from skin outpatient clinics of 3 tertiary care hospitals in Lahore, Pakistan, between November 1, 2012, and December 31, 2012, were assessed in this prospective cross-sectional study. The final sample includes 87 patients who were evaluated for severity of psoriasis (Psoriasis Area Severity Index [PASI]), dermatology-related quality of life (Dermatology Life Quality Index [DLQI]), and psychiatric morbidity (12-item General Health Questionnaire [GHQ-12]) and were assessed on 23 sociodemographic, lifestyle, and clinical variables.
Results: Of the 23 variables, the PASI was significantly associated with education and habit of drinking alcohol (P < .05), the DLQI was significantly associated with disturbed eating (P < .05), and the GHQ-12 score was significantly associated with hair disease (P < .05), current income (P < .05), and disturbed eating and sleeping (P < .01). The PASI, DLQI, and GHQ-12 were not usually affected by sociodemographic, lifestyle, and clinical factors, except for some variables such as education of the patient, alcohol intake, eating and sleeping disturbance, and income status. A statistically significant correlation (P < .01) was found between all 3 scores (ie, PASI, DLQI, and GHQ-12). The correlation coefficients of the PASI with the DLQI and GHQ-12 are 0.345 and 0.460, respectively, and that of the DLQI with the GHQ-12 is 0.635. A moderating effect of the DLQI score was found on the relationship between the PASI and GHQ-12 scores.
Conclusions: Psoriasis has an immense impact on the life of patients and common comorbidities in psoriasis including coronary heart disease, depression, cerebrovascular disease, and metabolic syndrome. Screening for these comorbidities in psoriasis patients is essential. Impaired quality of life negatively affects the psyche of patients and initiates coping mechanisms, which may lead to depression and anxiety, social dysfunction, and loss of confidence, and the psychosocial burden of the disease may become more than the physical burden. The dermatologist usually manages physical disease and fails to address the social, emotional, and psychological aspects. Quality of life improves if these psychological aspects are also properly dealt with.
Prim Care Companion CNS Disord 2015;17(3):doi:10.4088/PCC.14m01629
© Copyright 2015 Physicians Postgraduate Press, Inc.
Submitted: January 19, 2014; accepted November 11, 2014.
Published online: June 25, 2015.
Corresponding author: Mohammad Jafferany, MD, FAPA, Psychiatry and Behavioral Sciences, Central Michigan University College of Medicine, 3215 Hallmark Ct, Saginaw, MI 48603 ([email protected]).
Psoriasis is an immune-mediated chronic inflammatory skin disease with an unpredictable course and unknown cause.1–3 It is estimated that 1%–3% of the world population have psoriasis.4,5 Psoriasis waxes and wanes in the form of episodes.6 Triggers/exacerbating factors or alleviating factors may be identified.7 Psoriasis affects nails and skin and may affect joints.8,9 Race, geographic location, and ethnic backgrounds are some of the important factors influencing the prevalence of psoriasis.10 Onset of the disease may be sudden or gradual.11 Psoriasis can start at any age11–13; however, the late teens and late fifth decade may be the most common ages at onset.13 Psoriasis may require lifelong management.14,15
Social rejection and alienation are forms of discrimination that patients with psoriasis experience and may result in their feeling stigmatized.16,17 Visible disfigurement impairs the self-image of the patient, which influences all aspects of his/her life,18 and is accompanied by embarrassment, shame, guilt, and anger.19–21 These patients abhor public parks, sports, and social gatherings, and they become the center of attention when they try to hide their skin with inappropriate clothing. They also may avoid intimate relationships.22,23 Reduced opportunities at work, school, or university are the direct result of damaged self-image and reduced self-confidence.24–26 Social interplay between the patient and society is very complex and multifaceted24; it is not unidirectional and leads to initiation of many coping mechanisms, which include anticipation of discrimination and fear of social rejection. This fear causes isolation, social anxiety, and social disability.17,27 Issues of maladjustment arise when people stare and pity, particularly if they think the disease is infectious.28 Intimacy seems impossible, and close relationships become complicated.22,23
Psoriasis is experienced over the course of a patient’s lifetime, as there is no cure and it is not life threatening.29, The patient may develop coping strategies to meet the demands of everyday life and try to adapt to the new paradigm.26,31–33 For the patient, it is an effort to cope on cognitive and behavioral levels to solve personal and social problems by neutralizing conflict and reducing stress.29,30,34 Positive and optimistic self-management can help inner anxieties and outer strains. When these demands exceed the capacity and resources of the patient, coping mechanisms fail, and he/she experiences stress.18,35–37
Social support, attention, confiding relationships, companionship, comprehension of the whole situation, easily understandable explanations, thought sharing, and self-management are strategies used in different forms of psychotherapy.38–40 These nonpharmacologic strategies may be beneficial when incorporated into treatment regimens for patients with psoriasis. If patients change their behavior and attitudes, they can reduce stress and improve quality of life.41,42 Salutogenesis is a term used to explain this phenomenon.43 When patients with psoriasis are the victims of adverse situations, several personal factors help them to develop a sense of coherence and view the situation more realistically. Hope and a sense of wellness fill the mind, and the patient faces all types of stress readily and confidently.43,44 Joy, intimacy, love, relaxation, and a sense of safety can defeat stress, disgust, fear, anger, and anguish in the thoughts of psoriasis patients.38,45
Kurd and colleagues46 found a higher frequency of anxiety and depression in patients with psoriasis in a population-based cohort study in the United Kingdom. Psychiatric morbidity has an association with psoriasis; depression and anxiety are the main psychiatric disorders in these patients.47–49 Depression has a 3-pronged response: autonomic, neuroendocrine, and immunologic; so, effects of depression may be 3-fold if it occurs as a comorbidity in psoriasis.50
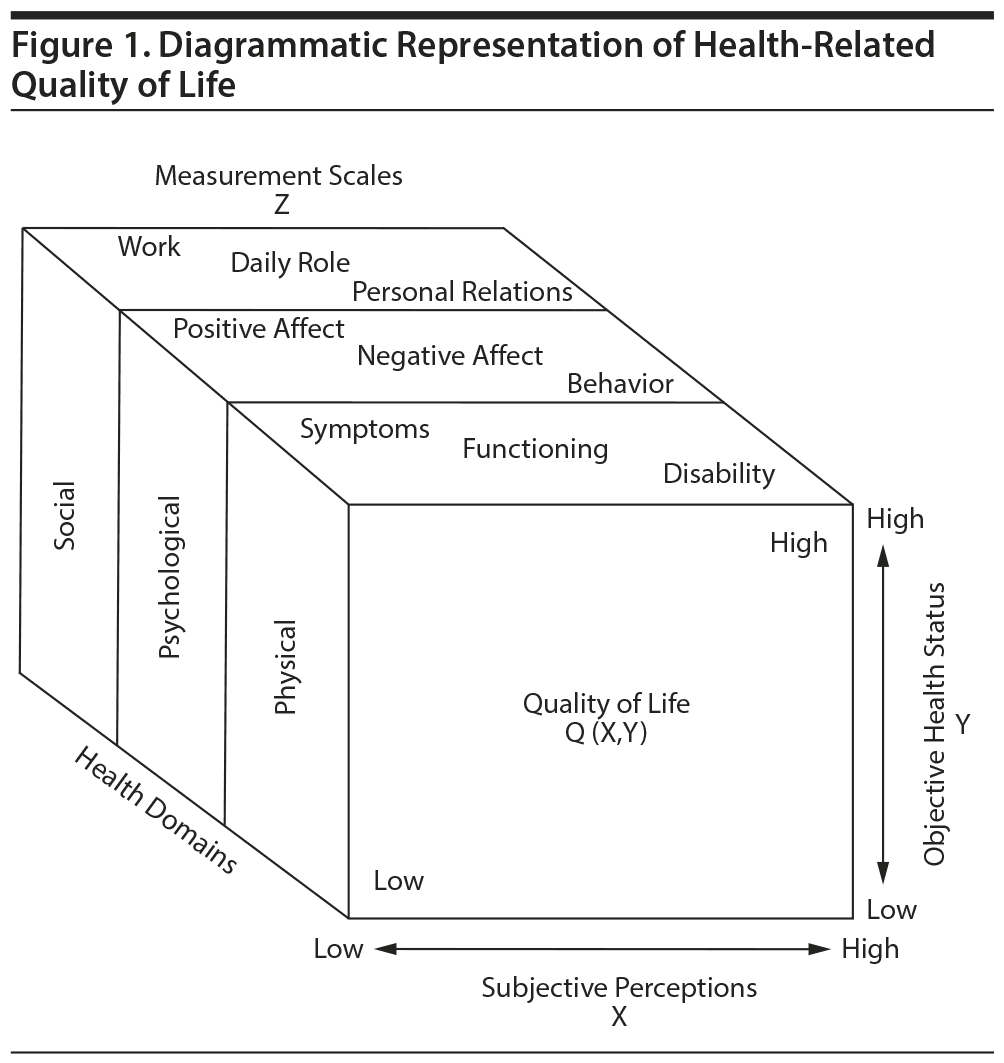
Emotional agony takes the shape of anger, which may become unpredictable.51 A holistic approach to treatment has been recommended for patients with skin diseases.52,53 Quality of life includes subjective emotional, intellectual, and physical facets of a person.54 Life at work along with family and friends cannot be ignored.54,55 Intelligent physicians actively listen to their patients and consider their concerns about treatment and prognosis. Thus, periodic assessment of “health-related” quality of life is needed (Figure 1).55,56 Quality of life has a very important role in the activities of daily living and social survival of psoriasis patients.57,58 Finlay and Coles59 conducted a survey to identify handicaps faced by psoriasis patients and resultant impairment. Results showed loss of workdays in working patients. Those who did not work said that it was due to psoriasis.59 The impairment results in disability, with the patient consequently unable to perform a role or activity. This disability changes the status of a person in society.60–63
The severity of psoriasis frequently changes, as does the psychiatric and clinical profile of the patient, and both may affect quality of life.24,27,57 Demographic characteristics and lifestyle have a definite bearing on the manner in which the disease behaves and its treatment and prognosis.64 Therefore, we undertook this study to investigate results of the Psoriasis Area Severity Index (PASI), Dermatology Life Quality Index (DLQI), and 12-item General Health Questionnaire (GHQ-12) in various groups of psoriasis patients, with reference to sociodemographic, lifestyle, and clinical characteristics. The interrelationship between the PASI, DLQI, and GHQ-12 were also studied, as well as the moderating effect of the DLQI on the relationship between the PASI and GHQ-12.
METHOD
This study uses a cross-sectional, prospective and observational design. The setting was the dermatology departments of 3 tertiary care hospitals in Lahore, Pakistan. Eligible patients were informed about the study and its objectives. After signing the consent forms, they were asked about sociodemographic details, and the first part of the questionnaire was completed by the researcher or other trained colleagues. Afterward, history of psoriasis and clinical information were taken by a qualified dermatologist. Family history, associated complaints, treatment history, and comorbidities were also included in the second part of the questionnaire. The questionnaire was followed by a detailed dermatologic examination, during which severity of disease was documented by using the PASI.
Sampling
The sampling technique was nonprobability, convenient, and purposive. Consecutive psoriasis patients from skin outpatient clinics of 3 tertiary care hospitals in Lahore between November 1, 2012, and December 31, 2012, were included in the sample. Patients with plaque psoriasis (ICD-10 criteria) aged ≥ 14 years were included in the study. Patients were excluded from the study if they had non–plaque variety psoriasis, had severe systemic disease, were receiving systemic steroids or methotrexate, and were aged < 14 years.
Data and Instruments
The 7 sociodemographic variables in this study included gender, employment status, residence, age, marriage years, current income, and education level. The 3 lifestyle-related variables included hobby or sport, smoking, and drinking alcohol. The 13 clinical profile variables included onset of disease, any incident (like death of a close relative or divorce) associated with disease, hair disease, nail disease, other skin disease, psoriasis in first-degree relatives, psoriasis in second-degree relatives, psoriasis in other family members, hypertension, diabetes, other disease, eating disturbance, and sleeping disturbance.
Three scores, the PASI, DLQI and GHQ-12, were used to measure demographic, lifestyle, and clinical characteristics. The severity and extent of psoriasis was measured using the PASI.65 Researchers use this tool to gauge the severity of psoriasis in the form of a score. The whole body is divided into 4 regions: head (10% of the person’s skin), upper limbs (20% of the person’s skin), trunk (30% of the person’s skin), and lower limbs (40% of the person’s skin). Erythema, scaling, and thickness are 3 important clinically discernible features easily visible to and assessable by the clinician. Each feature is observed by the clinician, and a number is assigned that ranges between 0 and 4, with 4 being the worst. Erythema means redness, scaling means desquamation, and thickness means in duration. The sum of the erythema, scaling, and thickness scores constitutes the summary measure of severity of psoriasis for each region. Regional scores were then added to calculate a single score for overall patient severity.
Dermatology-specific and health-related quality of life was measured by the DLQI, which includes fitness, efficiency, illness, self-image, self-esteem, anxiety and depression, work, leisure time, rejection, social support, and stigma.16,66–69 The Urdu version of the DLQI was used to assess the dermatology-specific life quality index.70
The GHQ-12 was chosen as an instrument to gauge depression, anxiety, psychological distress, loss of confidence, and social dysfunction.70–72 It is used as a unitary measure.71 The GHQ-12 has been used in primary care and nonpsychiatric settings worldwide.73 This 12-item questionnaire is easy to understand, uncomplicated, and short and requires very little time to be completed.74 The Urdu version of the GHQ-12 is a validated tool for detection of psychiatric illness in the Pakistani population.70,72 The GHQ-12 was administered by a psychologist at the end of the interview.
Analysis
Descriptive and clinical statistics were first calculated. The association of these variables with the PASI, DLQI, and GHQ-12 was examined using the Student t test, analysis of variance, Kruskal-Wallis, and Mann-Whitney test. Interrelation between the 3 scores was also studied, and a correlation matrix was deduced. The moderating role of the DLQI in the relationship between the PASI and GHQ-12 was calculated through hierarchical regression analysis. The data were analyzed using SPSS version 20 (SPSS Inc, Chicago, Illinois).
RESULTS
The sample consisted of 87 patients. Age was distributed in 3 groups: ≤ 25 = 21 (25.3%), 26–45 = 37 (44.6%), and ≥ 46 = 25 (30.1%). The sample included 56 males (64.4%) and 31 females (35.6%). The majority of patients (n = 52) had an urban background (61.9%), and 32 had a rural background (38.1%); 38 of the patients were employed (54.3%), and 32 were unemployed (45.7%). The majority of the patients (n = 53) had gradual onset of disease (63.1%), and only 31 had a sudden onset (36.9%). Fifty-six patients had no hobby or sport (64.4%), whereas 31 had a hobby or sport (35%).
Psoriasis Severity and Clinical Impact
The PASI, DLQI, and GHQ-12 scores were studied with respect to sociodemographic, lifestyle, and clinical variables. The mean score of the PASI for males was 10.1 and for females was 6.6; the standard deviation was 10.0 for males and 7.1 for females. The mean score of the GHQ-12 for males was 15.2 and for females was 13.7; the standard deviation was 8.5 for males and 7.6 for females. The mean score of the DLQI for males was 10.6 and for females was 8.4; the standard deviation was 7.7 for males and 6.6 for females.
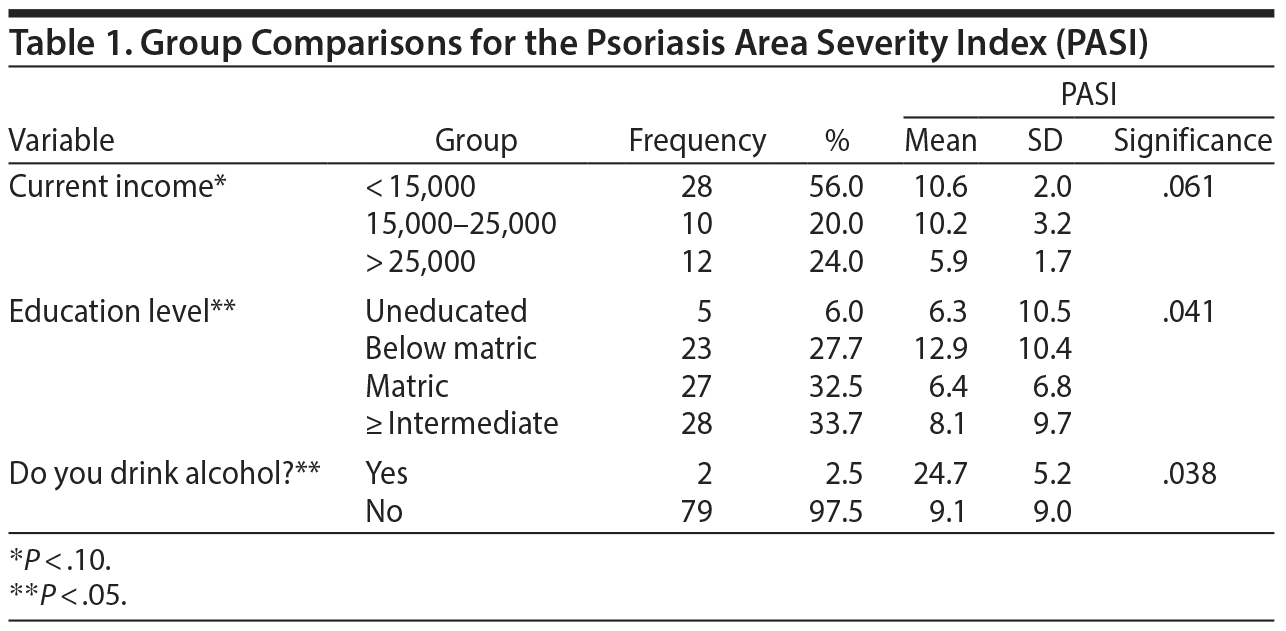
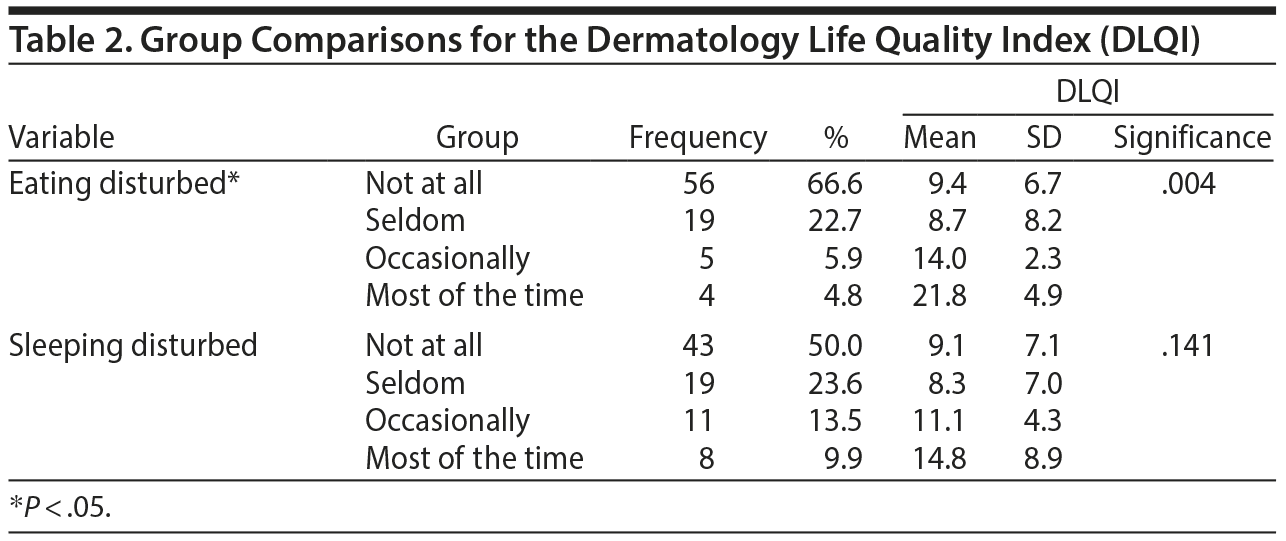
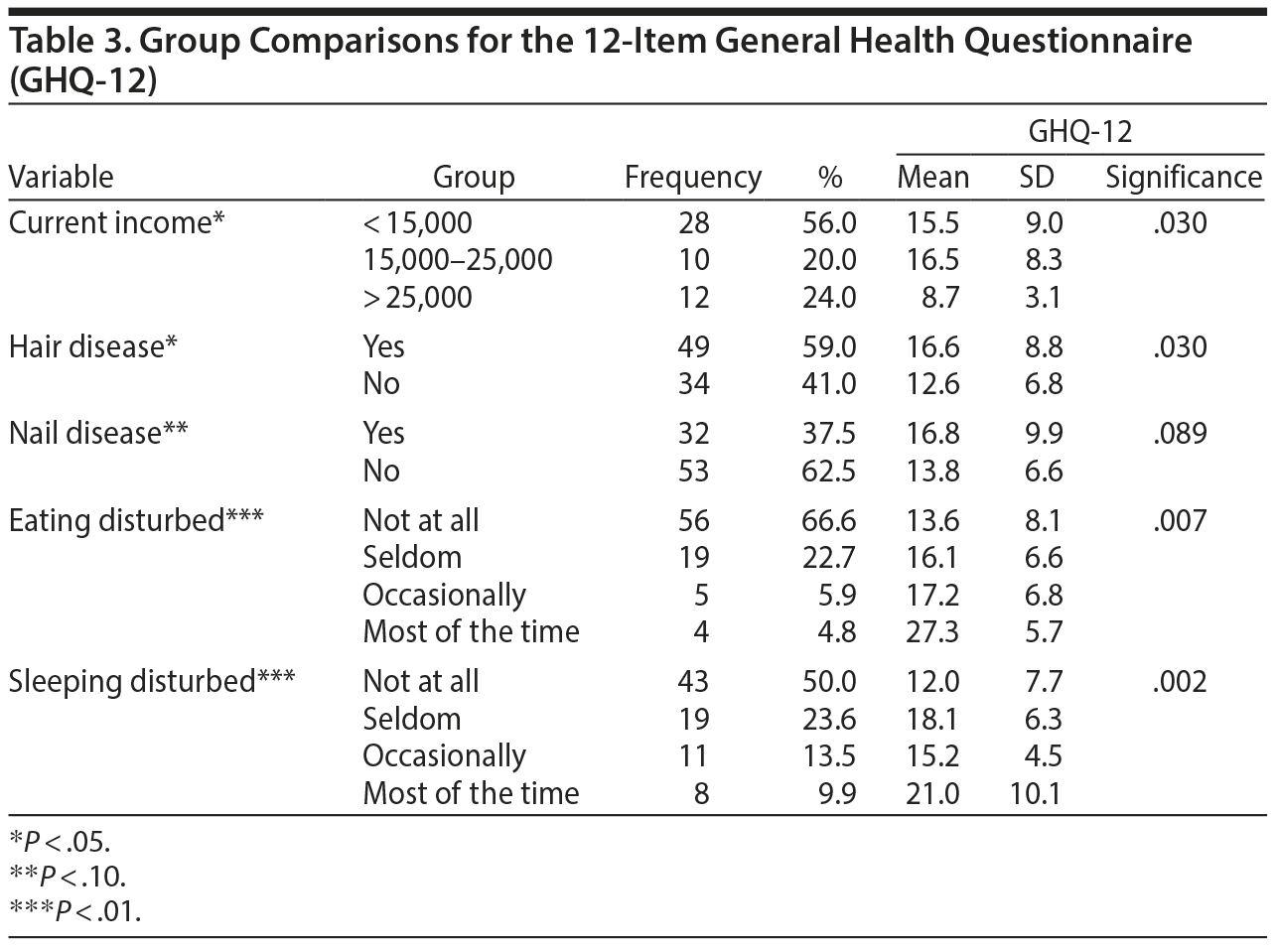
Group comparisons of the PASI score showed a significant difference with respect to education level (P = .041) and use of alcohol (P = .038). The other 21 variables showed no significant difference (Table 1). Group comparisons of the DLQI score showed a significant difference with respect to disturbed eating (P = .004). The other 22 variables showed no significant difference (Table 2). Group comparisons of the GHQ-12 score showed a significant difference with respect to current income (P = .030), hair disease (P = .030), disturbed eating (P = .007), and disturbed sleeping (P = .002). The other 19 variables showed no significant difference (Table 3).
Relationships Between Scales
The DLQI score was correlated with the PASI score (0.345, P < .01). Similarly, a positive correlation (0.635, P < .01) between the DLQI score and GHQ-12 score was found. The PASI score was also correlated with the GHQ-12 score (0.460, P < .01) (Table 4).
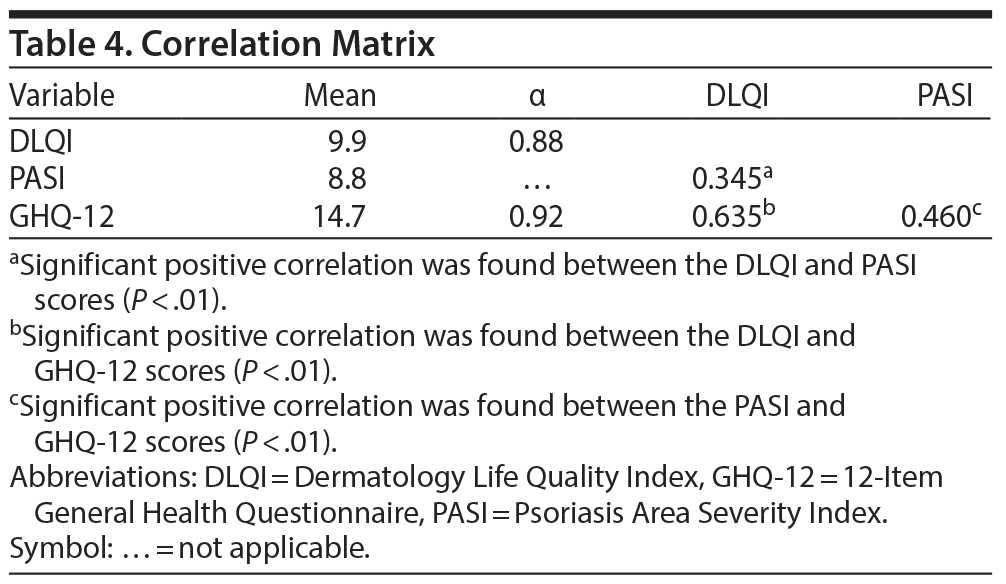
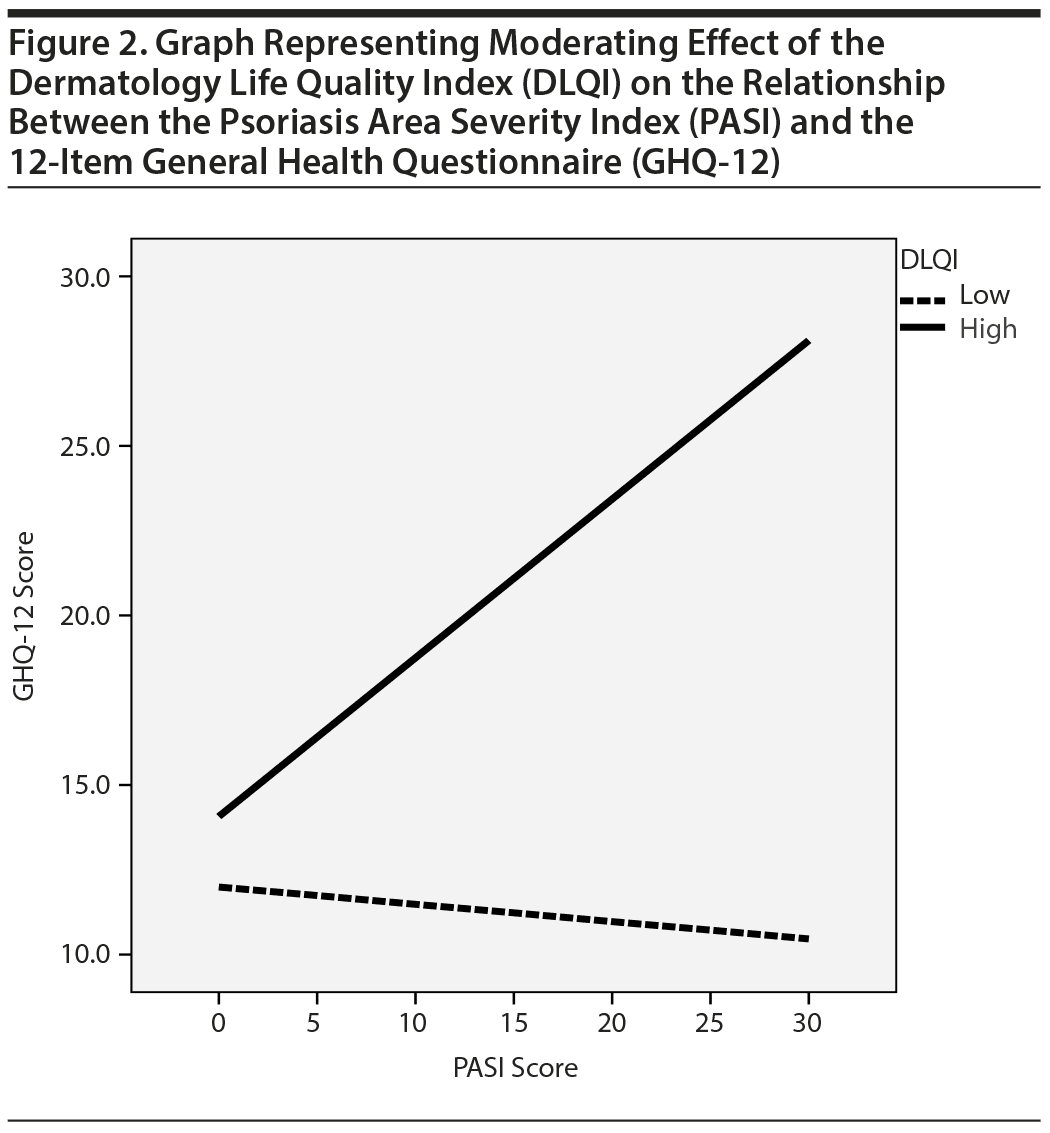
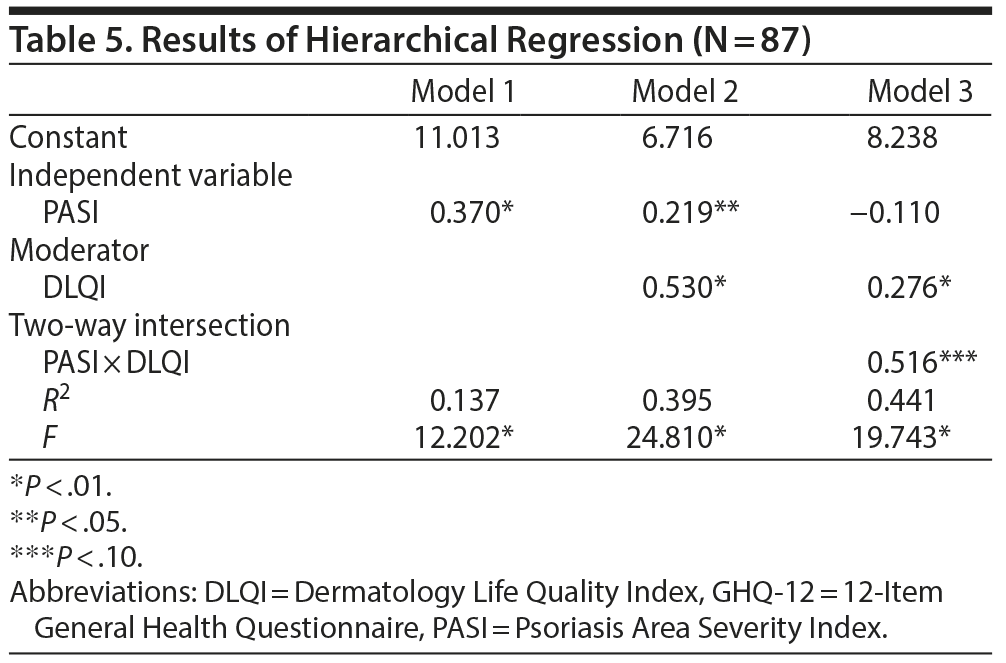
The relationships between all 3 scales were evaluated using 3 regression models. In Table 5, model 1 examines the primary effect of the PASI on the GHQ-12. Results show that the PASI score has a significant and positive influence on the GHQ-12 score (0.37, P < .01). Model 2 further includes the DLQI as the moderator in the model. The β value of the moderator is also significant (0.53, P < .01). Model 2 shows an increase in R2 by about 26%. In model 3, the intersection term (ie, PASI × DLQI) is also added in the model. The regression for the intersection term is also significant. This result confirms the moderating effect of the DLQI on the relationship between the PASI and GHQ-12 (Figure 2).
DISCUSSION
We found that at one point in time, severity of psoriasis and dermatologic and health-related quality of life and depression, anxiety, and psychological distress interact and influence each other. In addition, a number of patient characteristics influence disease severity, quality of life, and psychological status. In our study, educational background was associated with severity of disease; higher education helped the patients and they had less impairment of quality of life, a finding shared by others.16,75 As we found, alcohol may make psoriasis worse; and others have reported its association with psoriasis that is more severe and refractory to treatment.76 While we found no significant relationship, others have reported that income has a modest influence on severity of disease.77
Disturbed eating was shown to significantly alter quality of life as measured by the DLQI in this research. Sleep and appetite are affected in patients with psoriasis depending on the location of the lesions on exposed parts of the skin.78 In a study by Gaikwad et al,79 more than half of the patients complained of loss of sleep. This loss of sleep may be very disturbing. Loss of sleep is due to physical symptoms and discomfort but affects quality of life to a great extent.80 Disturbed sleep, disturbed eating, income of the patient, and involvement of hair were significantly related to the GHQ-12 in this research. Quality of sleep may also be reported due to subjective emotional experience.81,82 Dietary intake and sleep are disturbed in older patients with psoriasis. These changes may cause worsening of the disease.83 Pruritis has been shown to cause disturbed sleep.83,84 Suicidal contemplation may also be associated with sleep disturbance.82,85
We found significant positive correlation between the DLQI and PASI scores (0.345, P < .01). Mattei et al86 previously reported a positive correlation between severity of disease and quality of life; in their study, psychological symptoms were also improved by clearing of psoriatic skin lesions (75%), especially in patients treated with biologics. We found significant positive correlation between the DLQI and GHQ-12 scores (0.635, P < .01). Impaired quality of life negatively affects the psyche of patients and initiates coping mechanisms, which have long-lasting implications on the psyche of patients.87 Impaired quality of life may lead to depression and anxiety, social dysfunction, and loss of confidence. These indicators are measured by the GHQ-12.21,88,89
Depression, anxiety, social dysfunction, and loss of confidence are all psychiatric and psychological disorders, which can be treated only if they are identified and evaluated by a clinician who knows about them. If they go unidentified and untreated, the life of the psoriasis patient may be miserable, and the psychosocial burden of the disease may become more than the physical burden.90–92 The skin, neuroendocrine system, and immune system are interconnected and communicative.93–95 Psoriasis patients mostly visit dermatologists, who diagnose and treat patients with psoriasis. As dermatologists have limited knowledge of psychiatry, related needs of these patients go unmet. Medical needs may be met, but functioning and disability are not addressed. Physical needs are partially addressed, ignoring functioning and disability, whereas psychosocial needs are not addressed at all. It can be deduced that only 10% of the patients’ needs are addressed, whereas 90% of the needs of patients are unmet.56,96 Psychological stress affects epidermal permeability barrier homeostasis and may aggravate psoriasis.97,98 Patients with psychocutaneous disorders often do not like to be referred to psychiatrists, so liaison among primary care physicians, psychiatrists, and dermatologists may be very beneficial.90,92,99–101
Limitations
This study has limitations. The study design was cross-sectional and, therefore, while associations may be identified, the results do not imply causality. Temporal associations were not evaluated. Selection bias is also possible, as sampling was time based and was not a probability sampling. Due to smaller sample size, sampling method, and the tertiary clinic setting of the study, generalizations to other groups of patients are unwarranted. Only plaque psoriasis was included in this study; other varieties of psoriasis may have different clinical and psychiatric correlates.
CONCLUSIONS
After patients with psoriasis are examined and treated by dermatologists, they should be screened for psychiatric, cardiac, and metabolic comorbidities. Health-related quality of life should also be estimated in all psoriasis patients. Liaison clinics should be set up in all dermatology departments. Dermatologists should be made aware of the psychiatric complications of psoriasis during their training. A system of active integrated management of psoriasis and comorbidities, both medical and psychiatric, should be developed and evaluated.
Author affiliations: AIMC Research Cell, Allama Iqbal Medical College, Jinnah Hospital, Lahore (Dr Khawaja); Department of Dermatology Services, Institute of Medical Sciences Services Hospital, Lahore (Dr Bokhari); Department of Dermatology, Fatima Jinnah Medical College, Sir Ganga Ram Hospital, Lahore (Dr Rasheed); Department of Dermatology, Postgraduate Medical Institute, Lahore General Hospital, Lahore (Dr Shahzad); Department of Statistics, National College of Business Administration and Economics, Lahore (Dr Hanif); Lahore Business School, The University of Lahore, Lahore (Dr Qadeer), Pakistan; and Department of Psychiatry, College of Medicine, Central Michigan University, East Campus, Saginaw (Dr Jafferany).
Potential conflicts of interest: None reported.
Funding/support: None reported.
REFERENCES
1. Gelfand JM, Dommasch ED, Shin DB, et al. The risk of stroke in patients with psoriasis. J Invest Dermatol. 2009;129(10):2411–2418. doi:10.1038/jid.2009.112 PubMed
2. Griffiths CE, Barker JN. Pathogenesis and clinical features of psoriasis. Lancet. 2007;370(9583):263–271. doi:10.1016/S0140-6736(07)61128-3 PubMed
3. Nestle FO, Kaplan DH, Barker J. Psoriasis. N Engl J Med. 2009;361(5):496–509. doi:10.1056/NEJMra0804595 PubMed
4. Kaur I, Dogra S, Jain R, et al. Comparative study of calcipotriol (0.005%) ointment and tazarotene (0.05% and 0.1%) gel in the treatment of stable plaque psoriasis. Indian J Dermatol Venereol Leprol. 2008;74(5):471–474. doi:10.4103/0378-6323.44302 PubMed
5. Nickoloff BJ, Nestle FO. Recent insights into the immunopathogenesis of psoriasis provide new therapeutic opportunities. J Clin Invest. 2004;113(12):1664–1675. doi:10.1172/JCI200422147 PubMed
6. Campalani E, Barker JNWN. The clinical genetics of psoriasis. Curr Genomics. 2005;6(1):51–60. doi:10.2174/1389202053202157
7. Meier M, Sheth PB. Clinical spectrum and severity of psoriasis. Curr Probl Dermatol. 2009;38:1–20. doi:10.1159/000232301 PubMed
8. Radtke MA, Langenbruch AK, Schäfer I, et al. Nail psoriasis as a severity indicator: results from the PsoReal study. Patient Relat Outcome Meas. 2011;2:1–6. PubMed
9. Chang CC, Gangaram HB, Hussein SH. Malaysian Psoriasis Registry: preliminary report of a pilot study using a newly revised registry form. Med J Malaysia. 2008;63(suppl C):68–71. PubMed
10. Neimann AL, Porter SB, Gelfand JM. The epidemiology of psoriasis. Expert Rev Dermatol. 2006;1(1):63–75. doi:10.1586/17469872.1.1.63
11. Naldi L, Gambini D. The clinical spectrum of psoriasis. Clin Dermatol. 2007;25(6):510–518. doi:10.1016/j.clindermatol.2007.08.003 PubMed
12. Lebwohl M. Psoriasis. Lancet. 2003;361(9364):1197–1204. doi:10.1016/S0140-6736(03)12954-6 PubMed
13. Langley RG, Krueger GG, Griffiths CE. Psoriasis: epidemiology, clinical features, and quality of life. Ann Rheum Dis. 2005;64(suppl 2):ii18–ii23, discussion ii24–ii25. doi:10.1136/ard.2004.033217 PubMed
14. Colombo G, Altomare G, Peris K, et al. Moderate and severe plaque psoriasis: cost-of-illness study in Italy. Ther Clin Risk Manag. 2008;4(2):559–568. PubMed
15. Dehkharghani S, Bible J, Chen JG, et al. The economic burden of skin disease in the United States. J Am Acad Dermatol. 2003;48(4):592–599. doi:10.1067/mjd.2003.178 PubMed
16. Hrehorów E, Salomon J, Matusiak L, et al. Patients with psoriasis feel stigmatized. Acta Derm Venereol. 2012;92(1):67–72. doi:10.2340/00015555-1193 PubMed
17. Kimball AB, Jacobson C, Weiss S, et al. The psychosocial burden of psoriasis. Am J Clin Dermatol. 2005;6(6):383–392. doi:10.2165/00128071-200506060-00005 PubMed
18. Vardy D, Besser A, Amir M, et al. Experiences of stigmatization play a role in mediating the impact of disease severity on quality of life in psoriasis patients. Br J Dermatol. 2002;147(4):736–742. doi:10.1046/j.1365-2133.2002.04899.x PubMed
19. Schmid-Ott G. Future trends in psychodermatological psoriasis research: somatopsychic or psychosomatic focus? Dermatol Psychosom. 2003;4(3):129–130. doi:10.1159/000073988
20. Schmid-Ott G, Schallmayer S, Calliess IT. Quality of life in patients with psoriasis and psoriasis arthritis with a special focus on stigmatization experience. Clin Dermatol. 2007;25(6):547–554. doi:10.1016/j.clindermatol.2007.08.008 PubMed
21. Schmid-Ott G, Künsebeck HW, Jäger B, et al. Significance of the stigmatization experience of psoriasis patients: a 1-year follow-up of the illness and its psychosocial consequences in men and women. Acta Derm Venereol. 2005;85(1):27–32. doi:10.1080/000155550410021583 PubMed
22. Ginsburg IH, Link BG. Feelings of stigmatization in patients with psoriasis. J Am Acad Dermatol. 1989;20(1):53–63. doi:10.1016/S0190-9622(89)70007-4 PubMed
23. Ginsburg IH, Link BG. Psychosocial consequences of rejection and stigma feelings in psoriasis patients. Int J Dermatol. 1993;32(8):587–591. doi:10.1111/j.1365-4362.1993.tb05031.x PubMed
24. Barankin B, DeKoven J. Psychosocial effect of common skin diseases. Can Fam Physician. 2002;48:712–716. PubMed
25. Magin P, Adams J, Heading G, et al. The psychological sequelae of psoriasis: results of a qualitative study. Psychol Health Med. 2009;14(2):150–161. doi:10.1080/13548500802512294 PubMed
26. Sampogna F, Tabolli S, Abeni D; IDI Multipurpose Psoriasis Research on Vital Experiences (IMPROVE) investigators. Living with psoriasis: prevalence of shame, anger, worry, and problems in daily activities and social life. Acta Derm Venereol. 2012;92(3):299–303. doi:10.2340/00015555-1273 PubMed
27. Basavaraj KH, Navya MA, Rashmi R. Relevance of psychiatry in dermatology: present concepts. Indian J Psychiatry. 2010;52(3):270–275. doi:10.4103/0019-5545.70992 PubMed
28. Rumsey N, Harcourt D. Body image and disfigurement: issues and interventions. Body Image. 2004;1(1):83–97. doi:10.1016/S1740-1445(03)00005-6 PubMed
29. Choi J, Koo JY. Quality of life issues in psoriasis. J Am Acad Dermatol. 2003;49(suppl 2 ):S57–S61. doi:10.1016/S0190-9622(03)01136-8 PubMed
30. Mukhtar R, Choi J, Koo JY. Quality-of-life issues in psoriasis. Dermatol Clin. 2004;22(4):389–395, viii. doi:10.1016/j.det.2004.03.016 PubMed
31. Fortune DG, Richards HL, Main CJ, et al. Patients’ strategies for coping with psoriasis. Clin Exp Dermatol. 2002;27(3):177–184. doi:10.1046/j.1365-2230.2002.01055.x PubMed
32. Wahl AK, Gjengedal E, Hanestad BR. The bodily suffering of living with severe psoriasis: in-depth interviews with 22 hospitalized patients with psoriasis. Qual Health Res. 2002;12(2):250–261. doi:10.1177/104973202129119874 PubMed
33. Zaher HAEM, Amin ME, Rakhawy MY. Coping with depression and anxiety in patients with psoriasis. Egypt J Psychiatry. 2010;31(2):57–63.
34. Folkman S, Lazarus RS, Dunkel-Schetter C, et al. Dynamics of a stressful encounter: cognitive appraisal, coping, and encounter outcomes. J Pers Soc Psychol. 1986;50(5):992–1003. doi:10.1037/0022-3514.50.5.992 PubMed
35. Fortune DG, Richards HL, Griffiths CE, et al. Psychological stress, distress and disability in patients with psoriasis: consensus and variation in the contribution of illness perceptions, coping and alexithymia. Br J Clin Psychol. 2002;41(2):157–174. doi:10.1348/014466502163949 PubMed
36. Richards HL, Fortune DG, Griffiths CE, et al. The contribution of perceptions of stigmatization to disability in patients with psoriasis. J Psychosom Res. 2001;50(1):11–15. doi:10.1016/S0022-3999(00)00210-5 PubMed
37. Scharloo M, Kaptein AA, Weinman J, et al. Patients’ illness perceptions and coping as predictors of functional status in psoriasis: a 1-year follow-up. Br J Dermatol. 2000;142(5):899–907. doi:10.1046/j.1365-2133.2000.03469.x PubMed
38. Picardi A, Mazzotti E, Gaetano P, et al. Stress, social support, emotional regulation, and exacerbation of diffuse plaque psoriasis. Psychosomatics. 2005;46(6):556–564. doi:10.1176/appi.psy.46.6.556 PubMed
39. Janković S, Raznatović M, Marinković J, et al. Relevance of psychosomatic factors in psoriasis: a case-control study. Acta Derm Venereol. 2009;89(4):364–368. doi:10.2340/00015555-0669 PubMed
40. Chuh A, Wong W, Zawar V. The skin and the mind. Aust Fam Physician. 2006;35(9):723–725. PubMed
41. Fava GA, Sonino N. The clinical domains of psychosomatic medicine. J Clin Psychiatry. 2005;66(7):849–858. doi:10.4088/JCP.v66n0707 PubMed
42. Hrehorów E, Reich A, Szepietowski J. Quality of life in patients with psoriasis: relationship with pruritus, stress and symptoms of depression. Dermatol Klin. 2007;9:19–23.
43. Antonovsky A. Health, Stress and Coping. San Francisco, CA: Jossey-Bass; 1979.
44. Antonovsky A. Unraveling the Mystery of Health. How People Manage Stress and Stay Well. San Francisco, CA: Jossey-Bass; 1987.
45. Basińska MA, Drozdowska M. Emotional intelligence as an indicator of satisfaction with life of patients with psoriasis. Postepy Dermatol Alergol. 2013;30(6):365–372. doi:10.5114/pdia.2013.39435 PubMed
46. Kurd SK, Troxel AB, Crits-Christoph P, et al. The risk of depression, anxiety, and suicidality in patients with psoriasis: a population-based cohort study. Arch Dermatol. 2010;146(8):891–895. PubMed
47. Mattoo SK, Handa S, Kaur I, et al. Psychiatric morbidity in psoriasis: prevalence and correlates in India. Ger J Psychiatry. 2005;8:17–22.
48. Russo PA, Ilchef R, Cooper AJ. Psychiatric morbidity in psoriasis: a review. Australas J Dermatol. 2004;45(3):155–159, quiz 160–161. doi:10.1111/j.1440-0960.2004.00078.x PubMed
49. Sharma S, Bassi R, Singh A. A comparative study of depression and anxiety in psoriasis and other chronic skin diseases. J Pakistan Assoc Dermatologists. 2011;21(4):235–240.
50. Schmitt JM, Ford DE. Role of depression in quality of life for patients with psoriasis. Dermatology. 2007;215(1):17–27. doi:10.1159/000102029 PubMed
51. Kossakowska MM, Cieścińska C, Jaszewska J, et al. Control of negative emotions and its implication for illness perception among psoriasis and vitiligo patients. J Eur Acad Dermatol Venereol. 2010;24(4):429–433. doi:10.1111/j.1468-3083.2009.03432.x PubMed
52. Koblenzer CS. Psychosomatic concepts in dermatology: a dermatologist-psychoanalyst’s viewpoint. Arch Dermatol. 1983;119(6):501–512. doi:10.1001/archderm.1983.01650300055017 PubMed
53. Wittkower E, Russell B. Emotional factors in skin disease. JAMA. 1953;153(12):1133. doi:10.1001/jama.1953.02940290065029
54. Gill TM, Feinstein AR. A critical appraisal of the quality of quality-of-life measurements. JAMA. 1994;272(8):619–626. doi:10.1001/jama.1994.03520080061045 PubMed
55. Gill TM. Quality of life assessment: values and pitfalls. J R Soc Med. 1995;88(12):680–682. PubMed
56. Testa MA, Simonson DC. Assessment of quality-of-life outcomes. N Engl J Med. 1996;334(13):835–840. doi:10.1056/NEJM199603283341306 PubMed
57. Bhosle MJ, Kulkarni A, Feldman SR, et al. Quality of life in patients with psoriasis. Health Qual Life Outcomes. 2006;4(1):35. doi:10.1186/1477-7525-4-35 PubMed
58. de Korte J, Sprangers MA, Mombers FM, et al. Quality of life in patients with psoriasis: a systematic literature review. J Investig Dermatol Symp Proc. 2004;9(2):140–147. doi:10.1046/j.1087-0024.2003.09110.x PubMed
59. Finlay AY, Coles EC. The effect of severe psoriasis on the quality of life of 369 patients. Br J Dermatol. 1995;132(2):236–244. doi:10.1111/j.1365-2133.1995.tb05019.x PubMed
60. World Health Organization. Constitution of the World Health Organization. Handbook of Basic Documents. 5th ed. Geneva, Switzerland: Palais des Nations, World Health Organization; 1952:3–20.
61. World Health Organization. International Classification of Impairments, Disabilities and Handicaps. Geneva, Switzerland: World Health Organization; 1980:27–29.
62. Renzi C, Picardi A, Abeni D, et al. Association of dissatisfaction with care and psychiatric morbidity with poor treatment compliance. Arch Dermatol. 2002;138(3):337–342. doi:10.1001/archderm.138.3.337 PubMed
63. Stern RS, Nijsten T, Feldman SR, et al. Psoriasis is common, carries a substantial burden even when not extensive, and is associated with widespread treatment dissatisfaction. J Investig Dermatol Symp Proc. 2004;9(2):136–139. doi:10.1046/j.1087-0024.2003.09102.x PubMed
64. Kimball AB, Leonardi C, Stahle M, et al; The PSOLAR investigators and Steering Committee. Demography, baseline disease characteristics, and treatment history of patients with psoriasis enrolled in a multicenter, prospective, disease-based registry (PSOLAR). Br J Dermatol. 2014;171(1):137–147. doi:10.1111/bjd.13013
65. Fredriksson T, Pettersson U. Severe psoriasis: oral therapy with a new retinoid. Dermatologica. 1978;157(4):238–244. doi:10.1159/000250839 PubMed
66. Basra MKA, Fenech R, Gatt RM, et al. The Dermatology Life Quality Index 1994–2007: a comprehensive review of validation data and clinical results. Br J Dermatol. 2008;159(5):997–1035. PubMed
67. Finlay AY. Quality of life indices. Indian J Dermatol Venereol Leprol. 2004;70(3):143–148. PubMed
68. Finlay AY, Khan GK. Dermatology Life Quality Index (DLQI): a simple practical measure for routine clinical use. Clin Exp Dermatol. 1994;19(3):210–216. doi:10.1111/j.1365-2230.1994.tb01167.x PubMed
69. Pakran J, Riyaz N, Nandakumar G. Determinants of quality of life in psoriasis patients: a cluster analysis of 50 patients. Indian J Dermatol. 2011;56(6):689–693. doi:10.4103/0019-5154.91830 PubMed
70. Ahmer S, Faruqui RA, Aijaz A. Psychiatric rating scales in Urdu: a systematic review. BMC Psychiatry. 2007;7(1):59. doi:10.1186/1471-244X-7-59 PubMed
71. Goldberg, DP. The Detection of Psychiatric Illness by Questionnaire. London, UK: Oxford University Press; 1972.
72. Minhas FA, Iqbal K, Mubbashar MH. Validation of Self-Rating Questionnaire in primary care settings of Pakistan. Pak J Clin Psychiatr. 1995;5:60–69.
73. Goldberg DP, Blackwell B. Psychiatric illness in general practice: a detailed study using a new method of case identification. BMJ. 1970;1(5707):439–443. doi:10.1136/bmj.2.5707.439 PubMed
74. Goldberg DP, Steele JJ, Smith C, et al. Training family doctors to recognize psychiatric illness with increased accuracy. Lancet. 1980;316(8193):521–523. doi:10.1016/S0140-6736(80)91843-7 PubMed
75. Zachariae R, Zachariae H, Blomqvist K, et al. Quality of life in 6,497 Nordic patients with psoriasis. Br J Dermatol. 2002;146(6):1006–1016. doi:10.1046/j.1365-2133.2002.04742.x PubMed
76. Kazakevich N, Moody MN, Landau JM, et al. Alcohol and skin disorders: with a focus on psoriasis. Skin Therapy Lett. 2011;16(4):5–6. PubMed
77. Horn EJ, Fox KM, Patel V, et al. Association of patient-reported psoriasis severity with income and employment. J Am Acad Dermatol. 2007;57(6):963–971. doi:10.1016/j.jaad.2007.07.023 PubMed
78. Lee E. Dermatology and psychiatry. Hong Kong J Dermatol Venereol. 2009;17:67–68.
79. Gaikwad R, Deshpande S, Raje S, et al. Evaluation of functional impairment in psoriasis. Indian J Dermatol Venereol Leprol. 2006;72(1):37–40. doi:10.4103/0378-6323.19716 PubMed
80. Schmid-Ott G, Böhm D, Stock Gissendanner S. Patient considerations in the management of mental stress in psoriasis. Patient Intelligence. 2012;4:41–50.
81. Janowski K, Steuden S, Pietrzak A, et al. Social support and adaptation to the disease in men and women with psoriasis. Arch Dermatol Res. 2012;304(6):421–432. doi:10.1007/s00403-012-1235-3 PubMed
82. Vladut CI, Kallay E. Psychosocial implications of psoriasis: theoretical review. Cogn Brain Behav. 2010;14:23–35.
83. Farage MA, Miller KW, Sherman SN, et al. Assessing quality of life in older adult patients with skin disorders. Glob J Health Sci. 2012;4(2):119–131. PubMed
84. Gupta MA, Gupta AK, Kirkby S, et al. Pruritus in psoriasis: a prospective study of some psychiatric and dermatologic correlates. Arch Dermatol. 1988;124(7):1052–1057. doi:10.1001/archderm.1988.01670070040016 PubMed
85. Gupta MA, Schork NJ, Gupta AK, et al. Suicidal ideation in psoriasis. Int J Dermatol. 1993;32(3):188–190. doi:10.1111/j.1365-4362.1993.tb02790.x PubMed
86. Mattei PL, Corey KC, Kimball AB. Psoriasis Area Severity Index (PASI) and the Dermatology Life Quality Index (DLQI): the correlation between disease severity and psychological burden in patients treated with biological therapies. J Eur Acad Dermatol Venereol. 2014;28(3):333–337. doi:10.1111/jdv.12106 PubMed
87. Rieder E, Tausk F. Psoriasis, a model of dermatologic psychosomatic disease: psychiatric implications and treatments. Int J Dermatol. 2012;51(1):12–26. doi:10.1111/j.1365-4632.2011.05071.x PubMed
88. Quek KF, Low WY, Razack AH, et al. Reliability and validity of the General Health Questionnaire (GHQ-12) among urological patients: a Malaysian study. Psychiatry Clin Neurosci. 2001;55(5):509–513. doi:10.1046/j.1440-1819.2001.00897.x PubMed
89. Toyabe S, Shioiri T, Kobayashi K, et al. Factor structure of the General Health Questionnaire (GHQ-12) in subjects who had suffered from the 2004 Niigata-Chuetsu earthquake in Japan: a community-based study. BMC Public Health. 2007;7(1):175. doi:10.1186/1471-2458-7-175 PubMed
90. Jafferany M. Psychodermatology: a guide to understanding common psychocutaneous disorders. Prim Care Companion J Clin Psychiatry. 2007;9(3):203–213. doi:10.4088/PCC.v09n0306 PubMed
91. Jafferany M, Vander Stoep A, Dumitrescu A, et al. The knowledge, awareness, and practice patterns of dermatologists toward psychocutaneous disorders: results of a survey study. Int J Dermatol. 2010;49(7):784–789. PubMed
92. Jafferany M. Psychodermatology: when the mind and skin interact. Psychiatric Times. 2011;28(12):1–2.
93. Dhabhar FS. A hassle a day may keep the doctor away: stress and the augmentation of immune function. Integr Comp Biol. 2002;42(3):556–564. doi:10.1093/icb/42.3.556 PubMed
94. Dhabhar FS, Satoskar AR, Bluethmann H, et al. Stress-induced enhancement of skin immune function: a role for gamma interferon. Proc Natl Acad Sci U S A. 2000;97(6):2846–2851. doi:10.1073/pnas.050569397 PubMed
95. Zmijewski MA, Slominski AT. Neuroendocrinology of the skin: an overview and selective analysis. Dermatoendocrinol. 2011;3(1):3–10. doi:10.4161/derm.3.1.14617 PubMed
96. Feldman SR, Ravis S, Moran WP, et al. Patients seen in a dermatology clinic have unmet preventive health care needs. J Am Acad Dermatol. 2001;44(4):706–709. doi:10.1067/mjd.2001.112914 PubMed
97. Robles TF. Stress, social support, and delayed skin barrier recovery. Psychosom Med. 2007;69(8):807–815. doi:10.1097/PSY.0b013e318157b12e PubMed
98. Kimball AB, Gladman D, Gelfand JM, et al; National Psoriasis Foundation. National Psoriasis Foundation clinical consensus on psoriasis comorbidities and recommendations for screening. J Am Acad Dermatol. 2008;58(6):1031–1042. doi:10.1016/j.jaad.2008.01.006 PubMed
99. Choi EH, Brown BE, Crumrine D, et al. Mechanisms by which psychologic stress alters cutaneous permeability barrier homeostasis and stratum corneum integrity. J Invest Dermatol. 2005;124(3):587–595. doi:10.1111/j.0022-202X.2005.23589.x PubMed
100. de Zoysa P. Psychological interventions in dermatology. Indian J Dermatol. 2013;58(1):56–60. doi:10.4103/0019-5154.105312 PubMed
101. Shenoi SD, Prabhu S, Nirmal B, et al. Our experience in a psychodermatology liaison clinic at Manipal, India. Indian J Dermatol. 2013;58(1):53–55. doi:10.4103/0019-5154.105310 PubMed
Enjoy this premium PDF as part of your membership benefits!


