Use of Face Masks Among Patients With Psychiatric Illnesses During the COVID-19 Pandemic:
A Hospital-Based Cross-Sectional Study
A face mask is a device that covers the nose, mouth, and chin and if used appropriately provides a physical barrier against potentially infectious droplets. During the coronavirus disease 2019 (COVID-19) pandemic, many countries made it mandatory for the general population to wear appropriate face masks when going out in public. It was argued that when people have COVID-19 infection, their respiratory droplets usually contain the virus and thus covering their mouth and nose with a face mask can significantly reduce transmission of the virus.1 Moreover, when people visit hospitals, wearing a face mask can protect other patients with comorbidities from contracting COVID-19 infection. However, incorrect use of face masks may increase the risk of spreading COVID-19. Research has also explored the association between personal characteristics and the practice of using face masks.2 There is emerging evidence to suggest that many patients with psychiatric disorders, especially those suffering from psychotic illness, may not understand the risks of COVID-19 infection or follow instructions, such as wearing face masks while visiting the hospital, and may contract the disease or become superspreaders.3,4 However, at the time of this writing, no studies have examined use of face masks among patients with various psychiatric disorders. The aim of this study was to assess use of face masks among psychiatric patients during the COVID-19 pandemic.
Methods
The objective of this hospital-based cross-sectional study was to examine the practice of using face masks among psychiatric patients in India. The study was conducted from July 20, 2020, to August 6, 2020. The study was approved by the institutional ethics committee. All consecutive patients attending an outpatient psychiatry department in Kerala, India, were enrolled in the study after providing informed consent. Patients were initially observed by a trained social worker as to whether they were wearing a face mask, and if so, if they were wearing it properly. The proper manner of wearing a mask was defined as the face mask covers the nose, mouth, and chin adequately. After documenting the above variable, the trained social worker approached the patient and collected demographic data and details regarding the patients’ practice of using face masks via a structured questionnaire. After collecting the demographic details, the trained social worker provided proper instructions regarding the use of face masks to all patients who did not wear a mask or who were wearing it inappropriately and helped them put the mask on properly before entering the doctors’ consulting room.
Data were analyzed using Statistical Package for Social Sciences version 14 (SPSS Inc, Chicago, Illinois). Frequencies and percentages were used to describe the data. Chi-square was applied to determine statistical differences between groups. The resulting P values were considered significant if < .05.
Results
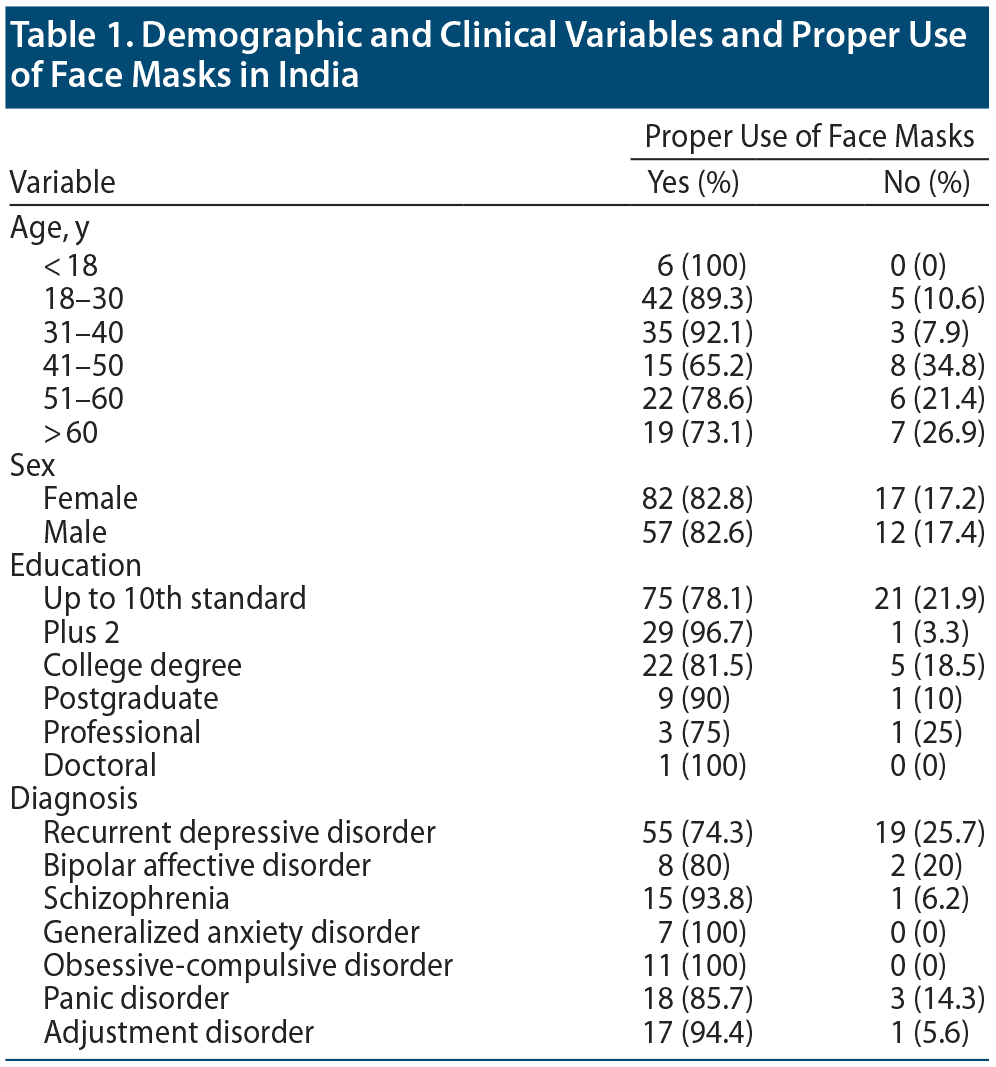
During the study period from July 20, 2020, to August 6, 2020, 168 psychiatric patients attending the psychiatry outpatient department were observed and interviewed. Half of the participants were aged 18-40 years, 58.9% were female, 57.1% had studied up to the 10th standard, and 64.9% were not working. The most common psychiatric diagnosis was depressive disorder (44%), followed by panic disorder (12.5%) and adjustment disorder (10.7%); 17.3% were suffering from psychotic illness. Results showed that 99.4% of patients were wearing face masks, but 17.4% were not wearing them properly. Demographic and clinical details regarding face mask use are summarized in Table 1. Cloth masks were most commonly used (87.5%), while 9.5% of patients were wearing surgical masks and 1.8% N95 masks. Reuse of masks was reported by 90.5%, and 90.5% said they cleaned the masks. Washing was the most common cleaning modality (89.9%). There was no significant difference between men and women regarding frequency of use or proper use of face masks. No significant difference in frequency of use or proper use of face masks was found between patients with a psychotic illness and those without such a diagnosis. A significant association was found between education level and face mask type (P = .053) and reuse of face masks (P = .058). Patients with postgraduate and doctoral education used surgical and N95 masks significantly more often and reused face masks significantly less compared to those with lower levels of education.
Discussion
At the time of this writing, real-life data on face mask use among psychiatric outpatients have not been reported. Control of respiratory infection at the source using a face mask is a well-established preventive strategy. Severe acute respiratory virus coronavirus 2 spreads person to person through close contact. With no effective treatment or vaccine available, reducing the rate of infection by such prevention methods is the only option.1 With evidence suggesting that face masks protect against COVID-19 infection, many governments across the globe instructed citizens to wear face masks when leaving their homes.1 The government of India made use of face masks mandatory in many major Indian cities in April 2020, and not wearing a face mask was declared punishable by up to 6 months in prison. In the Indian state of Kerala, where this study was conducted, face masks and social distancing are mandatory until 2021.
This study found that 99.4% of patients were wearing face masks while visiting the psychiatry outpatient department, but 17.4% were not covering the mouth, nose, and chin properly. However, improper use of face masks was not significantly associated with age, sex, or education. Past research2 among the general population has shown higher education and female sex to be positively associated with face mask-wearing behavior, and younger age was negatively associated with face mask-wearing behavior.
There was a prevailing argument after detection of a cluster of 50 cases of COVID-19 among inpatients in 1 psychiatric hospital in Wuhan, China, that it may be difficult to enforce standard recommendations to prevent spread of infection like using face masks among psychiatric patients due to their illness-related factors.3,4 No significant difference in face mask use between psychotic and nonpsychotic patients was found in the current study. However, this finding has the limitation that the severity of psychiatric symptoms was not assessed with standardized scales in either group.
This study also found higher frequency of use of surgical masks and N95 masks among highly educated study participants. Considering the prevailing confusion regarding the spread of infection by aerosols, it can be argued that educated patients might have selected surgical and N95 masks while visiting the hospital to prevent the risk of spread of infection by aerosols.5 However, the shortage of surgical and N95 masks is a serious concern in a developing country like India, and excessive use of such face masks, ideally recommended for health care personnel, might exacerbate the shortage and lead to infection and death among these workers. There is a need to educate these individuals as well as the general public that use of cloth masks is an effective and sustainable alternative to surgical masks as a means of infection control for general community use.5
In conclusion, the findings of this study suggest that although the majority of the study participants used face masks, mostly cloth masks, while visiting the hospital, many used face masks inappropriately, which might lead to spread of COVID-19 infection. Therefore, these results might be of value in the creation of education campaigns on the proper use of face masks to reduce the spread of COVID-19 infection among the psychiatric patient population.
Received: August 13, 2020.
Published online: November 25, 2020.
Potential conflicts of interest: None.
Funding/support: None.
REFERENCES
1.Chu DK, Akl EA, Duda S, et al; COVID-19 Systematic Urgent Review Group Effort (SURGE) study authors. Physical distancing, face masks, and eye protection to prevent person-to-person transmission of SARS-CoV-2 and COVID-19: a systematic review and meta-analysis. Lancet. 2020;395(10242):1973-1987. PubMed CrossRef
2.Sim SW, Moey KS, Tan NC. The use of facemasks to prevent respiratory infection: a literature review in the context of the health belief model. Singapore Med J. 2014;55(3):160-167. PubMed CrossRef
3.Yao H, Chen JH, Xu YF. Patients with mental health disorders in the COVID-19 epidemic. Lancet Psychiatry. 2020;7(4):e21. PubMed CrossRef
4.Kavoor AR. COVID-19 in people with mental illness: challenges and vulnerabilities. Asian J Psychiatr. 2020;51:102051. PubMed CrossRef
5.Esposito S, Principi N, Leung CC, et al. Universal use of face masks for success against COVID-19: evidence and implications for prevention policies. Eur Respir J. 2020;55(6):2001260. PubMed CrossRef
aDepartment of Psychiatry, Iqraa International Hospital and Research Centre, Calicut, Kerala, India
*Corresponding author: N. A. Uvais, MBBS, DPM, Iqraa International Hospital and Research Centre, Calicut, Kerala, India ([email protected]).
Prim Care Companion CNS Disord 2020;22(6):20br02789
To cite: Uvais NA. Use of face masks among patients with psychiatric illnesses during the COVID-19 pandemic: a hospital-based cross-sectional study. Prim Care Companion CNS Disord. 2020;22(6):20br02789.
To share: https://doi.org/10.4088/PCC.20br02789
© Copyright 2020 Physicians Postgraduate Press, Inc.
Enjoy this premium PDF as part of your membership benefits!