ABSTRACT
Posttraumatic stress disorder (PTSD) is an uncomfortable response that can follow exposure to 1 or more dangerous or frighteningly traumatic circumstances. Symptoms often include intrusive thoughts, insomnia, nightmares, flashbacks, avoidance behaviors, and hypervigilance or related emotionally troubling experiences. When overtly present, PTSD induces considerable emotional, social, occupational, and interpersonal dysfunctions. Psychotherapy is a commonly recommended initial intervention. There are a wide variety of techniques available. Psychotherapy can also be utilized as a preventative measure when intervention is available in the immediate aftermath of exposure to a potentially precipitating event. Most combat veterans with PTSD at Veterans Administration medical centers in the United States are prescribed pharmacotherapy. Different antidepressant, antipsychotic, adrenergic, and anticonvulsant medications are most commonly utilized. Optimal intervention for patients experiencing PTSD often includes prolonged follow-up that applies both talk and drug therapies in a supportive environment. This narrative review describes psychotherapeutic and pharmacologic approaches to treat PTSD.
Prim Care Companion CNS Disord 2021;23(1):19nr02572
To cite: Pary R, Micchelli AN, Lippmann S. How we treat posttraumatic stress disorder. Prim Care Companion CNS Disord. 2021;23(1):19nr02572.
To share: https://doi.org/10.4088/PCC.19nr02572
© Copyright 2021 Physicians Postgraduate Press, Inc.
aVeterans Administration Medical Center, Louisville, Kentucky
bDepartment of Psychiatry, University of Louisville School of Medicine, Louisville, Kentucky
*Corresponding author: Steven Lippmann, MD, 410 East Chestnut St #610, Louisville, KY 40202 ([email protected]).
Exposure to 1 or more traumatic events is an essential feature of posttraumatic stress disorder (PTSD).1 An individual’s reaction to such circumstances typically meets criteria for an acute stress disorder in the immediate aftermath of the trauma. Characteristic symptoms include intrusive thoughts, nightmares, and flashbacks of the traumatic events; sleep difficulties; avoidance behaviors; and hypervigilance. When these manifestations do not resolve in a month, PTSD may clinically emerge. Negative social, occupational, and interpersonal dysfunctions are often consequences of the offending experiences. Determination of a diagnosis is complicated by various details about the trauma, depressive or anxiety symptoms, and the heterogeneity of presentations.
A variety of pharmacologic treatments and psychotherapeutic strategies are recommended by different providers. Interventions should occur soon after the trauma and provide a supportive and safe environment.2 Therapeutic determinants include patient preference, their access to treatment, and their readiness to participate.
At Veterans Administration (VA) medical centers, psychotherapy with exposure to the traumatic memories is administered by nurses, social workers, and psychologists. Medication management is provided by advanced nurse practitioners or psychiatrists. Primary care and specialty physicians attend to most of the patients’ medical needs. This narrative review describes psychotherapeutic and pharmacologic approaches to treat PTSD.
PSYCHOTHERAPY
Psychotherapies are documented with good efficacy for subjects with diagnoses of PTSD.3,4 These interventions include cognitive-processing therapy, cognitive-behavioral therapy (CBT), eye movement desensitization, and reprocessing or narrative exposure therapy.3,4 These interventions generally improve the clinical status of many patients. Meta-analytic reviews5,6 indicate that trauma-focused PTSD psychotherapies yield more sustained benefit than pharmaceutical treatments.
CBT is most commonly recommended for treating people with PTSD, especially when utilized within 6 months following traumatic incident exposures.7 For those who benefit from CBT, effectiveness can endure for years. However, some patients do not respond well to CBT.8 Prolonged exposure therapy incorporates imaginal and in vivo exposures, psychoeducation, and breathing relaxation.9
Patients with PTSD who received exposure or sertraline therapies evidenced improvements that were sustained for 24 months.10 Reportedly, these therapies are more effective than sertraline for patients with PTSD.10
Cognitive-processing therapy is a manual-based intervention that is applied to aid recovery from PTSD.11 Cognitive-processing therapy is effective for many military combat veterans.9 Through writing, individuals exposed to trauma and negative emotions can better process troublesome memories.4 Maladaptive thinking is identified and reshaped.4,11
During eye movement desensitization and reprocessing therapy, patients recall distressing traumatic images while a therapist directs them to perform side-to-side eye movements.12 Eye movement desensitization and reprocessing therapy is reportedly as effective as trauma-focused CBT and better than non–trauma-focused CBT.13
Narrative exposure therapy is a short-term therapy for patients with PTSD symptoms, especially those who have experienced multiple traumas over long periods as a result of war.14 The treatment involves emotional exposure to the memories of traumatic events and the reorganization of these memories into a coherent chronological narrative. In contrast, present-centered therapy is not trauma focused and does not include disclosure discussion or exposure of traumatic events.15 Present-centered therapy is time limited and targets daily challenges that individuals with PTSD encounter that may be related to their trauma.15 Present-centered therapy includes psychoeducation to help patients understand how symptoms disrupt their day-to-day functioning. A comparative analysis16 was conducted between narrative exposure therapy and present-centered therapy in adults over age 55 years seeking treatment for PTSD. Both interventions benefited older PTSD survivors, with differences not significant enough to recommend one therapy over the other.16
PREVENTION
There are some immediate interventions recommended to immediately follow a traumatic event. Stress management techniques involve a single-session review of circumstances after a trauma; however, psychological debriefing for PTSD is less effective and can even be harmful.17
A collaborative approach often helps acutely traumatized victims, focusing on problem solving and support via CBT.18 Early exposure and cognitive therapies accelerate long-term reductions in PTSD symptoms, and benefit is prolonged.8 Yet, there are survivors with PTSD who remain refractory.8
PHARMACOTHERAPY
About 80% of combat veterans with PTSD concerns treated at VA medical centers or clinics are prescribed pharmacotherapy.19 Of patients involved, 89% receive antidepressants, 61% anxiolytics, and 34% antipsychotics.19
Selective Serotonin Reuptake Inhibitors
Selective serotonin reuptake inhibitors (SSRIs) block the presynaptic reuptake of serotonin. They are effective for a variety of PTSD symptoms, such as trauma reexperiencing, avoidance, numbing, and hyperarousal.20 Fluoxetine, paroxetine, and sertraline have efficacy for diminishing PTSD symptoms and depression.20,21 Quality of life is also improved.20 Paroxetine, sertraline, and fluoxetine as PTSD treatments were found to be superior to placebo.21 PTSD symptoms declined to a 30% remission rate in a brief sertraline trial17; however, extending sertraline therapy to 36 weeks increased the benefits.22–25 In subjects with a partial response to sertraline, adding prolonged exposure therapies increased the response.26,27 Similar research with paroxetine was less helpful.28 Sertraline and paroxetine are specifically approved treatments for people with PTSD.23 Fixed and flexible dosage paroxetine regimens are suggested.25,29 Improved memory, fewer symptoms, and an increase in hippocampal volume were documented among participants in a paroxetine trial29; the measurements by magnetic resonance imaging documented 4% larger volumes.
Serotonin-Norepinephrine Reuptake Inhibitors
Serotonin-norepinephrine reuptake inhibitors block presynaptic reuptake of serotonin and norepinephrine. Venlafaxine diminished PTSD symptoms during a 6-month trial.30 This drug was associated with better stress management; however, many subjects did not quickly achieve remission.30,31
Tricyclic Antidepressants
Tricyclic antidepressants block presynaptic reuptake of serotonin and norepinephrine. Imipramine, amitriptyline, and desipramine have demonstrated effectiveness for patients with PTSD symptoms.31–33 Currently, these medications are less commonly utilized.
Monoamine Oxidase Inhibitors
Monoamine oxidase inhibitors block the intraneuronal catabolism of monoamines including serotonin, norepinephrine, and dopamine. Vietnam War combat veterans with PTSD indicated that phenelzine reduces arousal and reexperiencing phenomena, but it is currently infrequently prescribed.32
Adrenergic Antagonists
Prazosin, an a1-adrenergic antagonist, decreases military trauma–related nightmares.34 Prazosin can induce significant hypotension but otherwise is well tolerated. Prazosin reduces sleep disruptions and might diminish nightmares. These dreams contain threatening past combat content, while dreams of people in domestic settings often feel less realistic.34 PTSD-related fear memories are diminished by β-adrenergic blockade at the amygdala.35 In animals, noradrenergic blockade in the lateral amygdala hampers memory consolidation.
Propranolol, a β-blocker, may attenuate unwanted PTSD memories among patients.36 Symptoms decreased in those prescribed propranolol 40 mg shortly after a traumatic exposure.36 Subsequent studies,37 however, have not supported propranolol in the prevention or treatment of PTSD.
Antipsychotics
Studies38,39 have shown quetiapine or olanzapine to be helpful for veterans with PTSD. Patients experienced improvement in rating scores, reductions in reexperiencing phenomena, and less hyperarousal.38,39 Olanzapine augmentation to an SSRI regimen was found to diminish PTSD stress measures, sleep symptoms, and depression.21 In a trial40 of military-related PTSD with SSRI-resistant symptoms, treatment outcomes at 23 VA outpatient medical centers after 6 months of risperidone treatment were no better than placebo. In women with PTSD randomized to risperidone or placebo after washout from other psychotropic medications, risperidone monotherapy was more beneficial for anxiety, depression, and PTSD ratings.41 Low-dose risperidone is a safe and effective treatment for intrusive and hyperarousal symptoms in adult women with chronic PTSD from childhood physical, sexual, verbal, and emotional abuse.42
Anticonvulsants
There are inconsistent results of efficacy from topiramate in PTSD cases. Improvement occurred with topiramate compared to placebo in reexperiencing, avoidance, and numbing symptoms among PTSD patients.43 Yet, another topiramate monotherapy trial resulted in a decrease in PTSD symptoms that was not statistically significant.44 Male veterans in a residential treatment program for combat-related PTSD were randomized to flexible-dose topiramate or placebo.45 Results for patients taking topiramate failed to show benefit over placebo.45
Similar results were noted with divalproex. In a randomized controlled trial, divalproex was not effective for treating chronic PTSD in older male military combat veterans.46 Divalproex also failed to surpass placebo in a preliminary trial for people with PTSD.47
Ketamine
Ketamine, an N-methyl-D-aspartate receptor antagonist, was found to reduce PTSD symptoms.48 The trial randomly assigned patients to receive a single infusion of intravenous ketamine or midazolam. After 24 hours, ketamine diminished PTSD and depressive symptoms more than midazolam. Ketamine was tolerated with no significant side effects.48
D-Cycloserine
In a meta-analysis49 of anxiety disorders, obsessive-compulsive disorder, and PTSD, D-cycloserine, an N-methyl-D-aspartate receptor partial agonist, was associated with a small augmentation effect on exposure therapy, which was not moderated by concurrent antidepressants. However, in a study50 in which subjects were limited to only PTSD patients, D-cycloserine in conjunction with exposure therapy failed to demonstrate a benefit.
PHARMACEUTICAL EFFICACY
For patients with sleep disturbances, prazosin, mirtazapine, and trazodone have been prescribed effectively.33 Antidepressant medications commonly utilized for PTSD rarely result in complete symptom remission, but they offer some relief.34 Once a patient improves, tapering antidepressant pharmaceuticals gradually over several months reduces relapse risk upon discontinuation.34
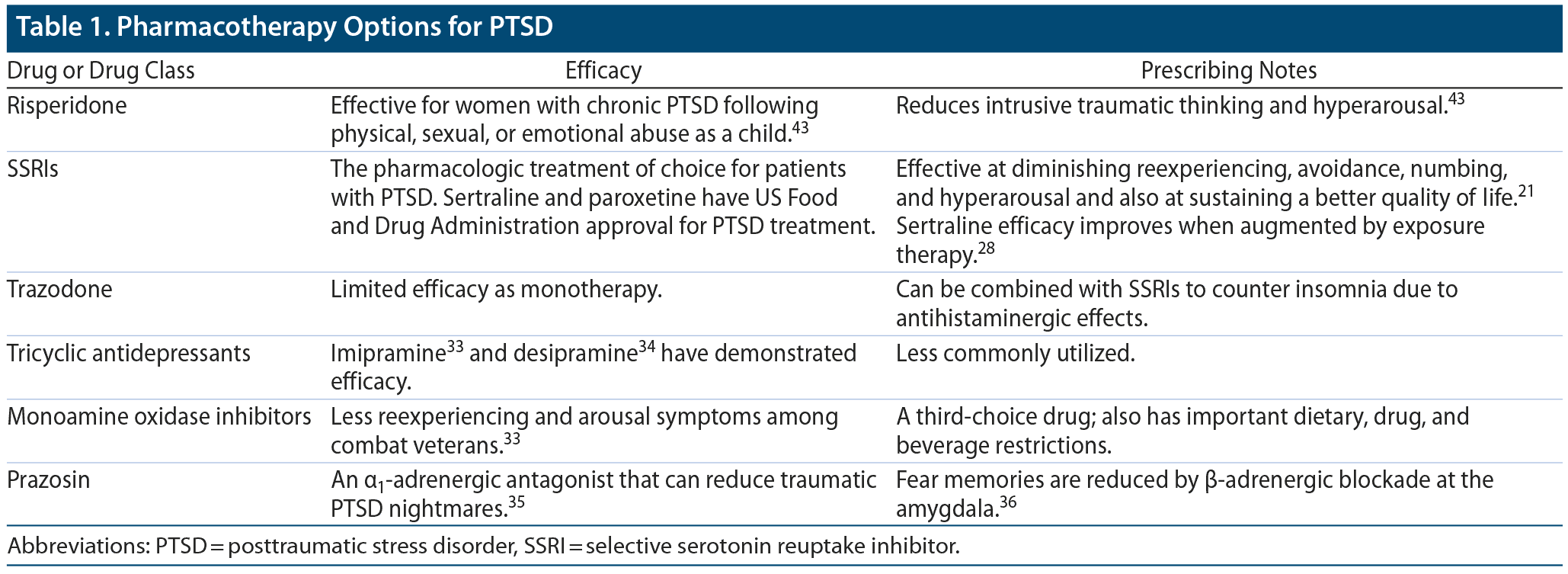
Prevention of PTSD has not been effective with escitalopram, gabapentin, temazepam, or propranolol.5 Benzodiazepines may actually increase PTSD symptoms in some people.5 Pharmacotherapy options for PTSD are included in Table 1, and a list of treatment guidelines is included in Table 2.
CONCLUSION
A first-line treatment for PTSD is trauma-focused exposure-based psychotherapy. When psychotherapy is not available, or if the patient prefers medication, an SSRI is a prudent option. It is important that the patient understand that psychotherapy will require close and frequent appointments and will probably be more time consuming and costly than a medication management approach.
Also, and especially in older men, the likelihood of SSRI-induced sexual dysfunction and other potential SSRI side effects should be discussed. Practitioners who provide therapies can be from multiple disciplines such as social work, psychology, or psychiatry, but specific therapy training is necessary to treat PTSD. If the clinician is not versed in a PTSD-specific therapy, a referral source is necessary.
In the VA, patients with PTSD sometimes receive the combination of medication management and psychotherapy, but the evidence base for the effectiveness of a medication plus therapy approach is insufficient. For example, combat-related PTSD patients were randomized to receive prolonged exposure plus placebo, sertraline with enhanced medication management, or the combination of prolonged exposure and sertraline. No difference was noted in change in enhanced medication management, prolonged exposure therapy plus placebo, and prolonged exposure therapy plus sertraline.55 In summary, close collaboration and communication between health care providers and the patient is necessary to effectively treat PTSD.
Submitted: November 25, 2019; accepted February 22, 2020.
Published online: February 18, 2021.
Potential conflicts of interest: None.
Funding/support: None.
Clinical Points
- Psychotherapy is a commonly recommended initial intervention for posttraumatic stress disorder (PTSD).
- Different antidepressant, antipsychotic, adrenergic, and anticonvulsant medications are most commonly utilized in pharmacologic treatment of PTSD.
- Optimal intervention for patients experiencing PTSD often includes prolonged follow-up that applies both talk and drug therapies in a supportive environment.
References (55)

- American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
- Stein MB, Rothbaum BO. 175 years of progress in PTSD therapeutics: learning from the past. Am J Psychiatry. 2018;175(6):508–516. PubMed CrossRef NLM
- Jonas DE, Cusack K, Forneris CA, et al. Psychological and Pharmacological Treatments for Adults With Posttraumatic Stress Disorder. Rockville, MD: PTSD; 2013.
- Monson CM, Schnurr PP, Resick PA, et al. Cognitive processing therapy for veterans with military-related posttraumatic stress disorder. J Consult Clin Psychol. 2006;74(5):898–907. PubMed CrossRef NLM
- Lee DJ, Schnitzlein CW, Wolf JP, et al. Psychotherapy versus pharmacotherapy for posttraumatic stress disorder: systemic review and meta-analyses to determine first-line treatments. Depress Anxiety. 2016;33(9):792–806. PubMed CrossRef NLM
- Merz J, Schwarzer G, Gerger H. Comparative efficacy and acceptability of pharmacological, psychotherapeutic, and combination treatments in adults with posttraumatic stress disorder: a network meta-analysis. JAMA Psychiatry. 2019;76(9):904–913. PubMed CrossRef NLM
- Shalev AY, Ankri Y, Israeli-Shalev Y, et al. Prevention of posttraumatic stress disorder by early treatment: results from the Jerusalem Trauma Outreach And Prevention Study. Arch Gen Psychiatry. 2012;69(2):166–176. PubMed CrossRef NLM
- Shalev AY, Ankri Y, Gilad M, et al. Long-term outcome of early interventions to prevent posttraumatic stress disorder. J Clin Psychiatry. 2016;77(5):e580–e587. PubMed CrossRef NLM
- Foa EBHE, Rothbaum BO. Treatments that Work. Prolonged Exposure Therapy for PTSD: Emotional Processing of Traumatic Experiences. Therapist Guide. New York, NY: Oxford University Press; 2007.
- Zoellner LA, Roy-Byrne PP, Mavissakalian M, et al. Doubly randomized preference trial of prolonged exposure versus sertraline for treatment of PTSD. Am J Psychiatry. 2019;176(4):287–296. PubMed CrossRef NLM
- Resick PA, Schnicke MK. Cognitive Processing for Rape Victims: A Treatment Manual. Newbury Park, CA: Sage; 1993.
- Feske U. Eye movement desensitization and reprocessing treatment for posttraumatic stress disorder. Clin Psychol (New York). 1998;5(2):171–181. CrossRef
- Bisson JI, Roberts NP, Andrew M, et al. Psychological therapies for chronic post-traumatic stress disorder (PTSD) in adults. Cochrane Database Syst Rev. 2013;(12):CD003388. PubMed NLM
- Robjant K, Fazel M. The emerging evidence for narrative exposure therapy: a review. Clin Psychol Rev. 2010;30(8):1030–1039. PubMed CrossRef PubMed CrossRef NLM
- Belsher BE, Beech E, Evatt D, et al. Present-centered therapy (PCT) for post-traumatic stress disorder (PTSD) in adults. Cochrane Database Syst Rev. 2019;2019(11):CD012898. PubMed NLM
- Lely JCG, Knipscheer JW, Moerbeek M, et al. Randomized controlled trial comparing narrative exposure therapy with present-centred therapy for older patients with post-traumatic stress disorder. Br J Psychiatry. 2019;214(6):369–377. PubMed CrossRef NLM
- Rose S, Bisson J, Churchill R, et al. Psychological debriefing for preventing posttraumatic stress disorder (PTSD). Cochrane Database Syst Rev. 2002;(2):CD000560. PubMed NLM
- Zatzick D, Roy-Byrne P, Russo J, et al. A randomized effectiveness trial of stepped collaborative care for acutely injured trauma survivors. Arch Gen Psychiatry. 2004;61(5):498–506. PubMed CrossRef NLM
- Mohamed S, Rosenheck RA. Pharmacotherapy of PTSD in the US Department of Veterans Affairs: diagnostic- and symptom-guided drug selection. J Clin Psychiatry. 2008;69(6):959–965. PubMed CrossRef NLM
- Rapaport MH, Endicott J, Clary CM. Posttraumatic stress disorder and quality of life: results across 64 weeks of sertraline treatment. J Clin Psychiatry. 2002;63(1):59–65. PubMed CrossRef NLM
- Stein DJIJ, Ipser JC, Seedat S. Pharmacotherapy for posttraumatic stress disorder (PTSD). Cochrane Database Syst Rev. 2006;(1):CD002795. PubMed NLM
- Brady K, Pearlstein T, Asnis GM, et al. Efficacy and safety of sertraline treatment of posttraumatic stress disorder: a randomized controlled trial. JAMA. 2000;283(14):1837–1844. PubMed CrossRef NLM
- Alexander W. Pharmacotherapy for post-traumatic stress disorder in combat veterans: focus on antidepressants and atypical antipsychotic agents. P&T. 2012;37(1):32–38. PubMed NLM
- Londborg PD, Hegel MT, Goldstein S, et al. Sertraline treatment of posttraumatic stress disorder: results of 24 weeks of open-label continuation treatment. J Clin Psychiatry. 2001;62(5):325–331. PubMed CrossRef NLM
- Tucker P, Zaninelli R, Yehuda R, et al. Paroxetine in the treatment of chronic posttraumatic stress disorder: results of a placebo-controlled, flexible-dosage trial. J Clin Psychiatry. 2001;62(11):860–868. PubMed CrossRef NLM
- Otto MW, Hinton D, Korbly NB, et al. Treatment of pharmacotherapy-refractory posttraumatic stress disorder among Cambodian refugees: a pilot study of combination treatment with cognitive-behavior therapy vs sertraline alone. Behav Res Ther. 2003;41(11):1271–1276. PubMed CrossRef NLM
- Rothbaum BO, Cahill SP, Foa EB, et al. Augmentation of sertraline with prolonged exposure in the treatment of posttraumatic stress disorder. J Trauma Stress. 2006;19(5):625–638. PubMed CrossRef NLM
- Simon NM, Connor KM, Lang AJ, et al. Paroxetine CR augmentation for posttraumatic stress disorder refractory to prolonged exposure therapy. J Clin Psychiatry. 2008;69(3):400–405. PubMed CrossRef NLM
- Marshall RD, Beebe KL, Oldham M, et al. Efficacy and safety of paroxetine treatment for chronic PTSD: a fixed-dose, placebo-controlled study. Am J Psychiatry. 2001;158(12):1982–1988. PubMed CrossRef NLM
- Davidson JR, Rothbaum BO, van der Kolk BA, et al. Multicenter, double-blind comparison of sertraline and placebo in the treatment of posttraumatic stress disorder. Arch Gen Psychiatry. 2001;58(5):485–492. PubMed CrossRef NLM
- Davidson J, Rothbaum BO, Tucker P, et al. Venlafaxine extended release in posttraumatic stress disorder: a sertraline- and placebo-controlled study. J Clin Psychopharmacol. 2006;26(3):259–267. PubMed CrossRef NLM
- Kosten TR, Frank JB, Dan E, et al. Pharmacotherapy for posttraumatic stress disorder using phenelzine or imipramine. J Nerv Ment Dis. 1991;179(6):366–370. PubMed CrossRef NLM
- Petrakis IL, Ralevski E, Desai N, et al. Noradrenergic vs serotonergic antidepressant with or without naltrexone for veterans with PTSD and comorbid alcohol dependence. Neuropsychopharmacology. 2012;37(4):996–1004. PubMed CrossRef NLM
- Raskind MA, Peskind ER, Kanter ED, et al. Reduction of nightmares and other PTSD symptoms in combat veterans by prazosin: a placebo-controlled study. Am J Psychiatry. 2003;160(2):371–373. PubMed CrossRef NLM
- Debiec J, LeDoux JE. Noradrenergic signaling in the amygdala contributes to the reconsolidation of fear memory: treatment implications for PTSD. Ann N Y Acad Sci. 2006;1071(1):521–524. PubMed CrossRef NLM
- Vaiva G, Ducrocq F, Jezequel K, et al. Immediate treatment with propranolol decreases posttraumatic stress disorder two months after trauma. Biol Psychiatry. 2003;54(9):947–949. PubMed CrossRef NLM
- Steenen SA, van Wijk AJ, van der Heijden GJ, et al. Propranolol for the treatment of anxiety disorders: systematic review and meta-analysis. J Psychopharmacol. 2016;30(2):128–139. PubMed CrossRef NLM
- Villarreal G, Hamner MB, Cañive JM, et al. Efficacy of quetiapine monotherapy in posttraumatic stress disorder: a randomized, placebo-controlled trial. Am J Psychiatry. 2016;173(12):1205–1212. PubMed CrossRef NLM
- Carey P, Suliman S, Ganesan K, et al. Olanzapine monotherapy in posttraumatic stress disorder: efficacy in a randomized, double-blind, placebo-controlled study. Hum Psychopharmacol. 2012;27(4):386–391. PubMed CrossRef NLM
- Krystal JH, Rosenheck RA, Cramer JA, et al; Veterans Affairs Cooperative Study No. 504 Group. Adjunctive risperidone treatment for antidepressant-resistant symptoms of chronic military service-related PTSD: a randomized trial. JAMA. 2011;306(5):493–502. PubMed CrossRef NLM
- Padala PR, Madison J, Monnahan M, et al. Risperidone monotherapy for post-traumatic stress disorder related to sexual assault and domestic abuse in women. Int Clin Psychopharmacol. 2006;21(5):275–280. PubMed CrossRef NLM
- Reich DB, Winternitz S, Hennen J, et al. A preliminary study of risperidone in the treatment of posttraumatic stress disorder related to childhood abuse in women. J Clin Psychiatry. 2004;65(12):1601–1606. PubMed CrossRef NLM
- Yeh MS, Mari JJ, Costa MC, et al. A double-blind randomized controlled trial to study the efficacy of topiramate in a civilian sample of PTSD. CNS Neurosci Ther. 2011;17(5):305–310. PubMed CrossRef NLM
- Tucker P, Trautman RP, Wyatt DB, et al. Efficacy and safety of topiramate monotherapy in civilian posttraumatic stress disorder: a randomized, double-blind, placebo-controlled study. J Clin Psychiatry. 2007;68(2):201–206. PubMed CrossRef NLM
- Lindley SE, Carlson EB, Hill K. A randomized, double-blind, placebo-controlled trial of augmentation topiramate for chronic combat-related posttraumatic stress disorder. J Clin Psychopharmacol. 2007;27(6):677–681. PubMed CrossRef NLM
- Davis LL, Davidson JR, Ward LC, et al. Divalproex in the treatment of posttraumatic stress disorder: a randomized, double-blind, placebo-controlled trial in a veteran population. J Clin Psychopharmacol. 2008;28(1):84–88. PubMed CrossRef NLM
- Hamner MB, Faldowski RA, Robert S, et al. A preliminary controlled trial of divalproex in posttraumatic stress disorder. Ann Clin Psychiatry. 2009;21(2):89–94. PubMed NLM
- Feder A, Parides MK, Murrough JW, et al. Efficacy of intravenous ketamine for treatment of chronic posttraumatic stress disorder: a randomized clinical trial. JAMA Psychiatry. 2014;71(6):681–688. PubMed CrossRef NLM
- Mataix-Cols D, Fernández de la Cruz L, Monzani B, et al; the DCS Anxiety Consortium. D-Cycloserine augmentation of exposure-based cognitive behavior therapy for anxiety, obsessive-compulsive, and posttraumatic stress disorders: a systematic review and meta-analysis of individual participant data. JAMA Psychiatry. 2017;74(5):501–510. PubMed CrossRef NLM
- Rothbaum BO, Price M, Jovanovic T, et al. A randomized, double-blind evaluation of D-cycloserine or alprazolam combined with virtual reality exposure therapy for posttraumatic stress disorder in Iraq and Afghanistan War veterans. Am J Psychiatry. 2014;171(6):640–648. PubMed CrossRef NLM
- Ursano RJ, Bell C, Eth S, et al; Work Group on ASD and PTSD; Steering Committee on Practice Guidelines. Practice Guideline for the Treatment of Patients With Acute Stress Disorder and Posttraumatic Stress Disorder. Am J Psychiatry. 2004;161(Suppl):3–31. PubMed NLM
- Benedek DM, Friedman MJ, Zatzick D, et al. Guideline Watch (March 2009): Practice Guideline for the Treatment of Patients With Acute Stress Disorder and Posttraumatic Stress Disorder. Washington, DC: American Psychiatric Association; 2009.
- Clinical Practice Guideline for the Treatment of Posttraumatic Stress Disorder (PTSD) in Adults. Washington, DC: American Psychological Association; 2017.
- VA/DoD Clinical Practice Guidelines. Management of Posttraumatic Stress Disorder and Acute Stress Reaction 2017. Washington, DC: US Department of Veterans Affairs/Department of Defense; 2017.
- Rauch SAM, Kim HM, Powell C, et al. Efficacy of prolonged exposure therapy, sertraline hydrochloride, and their combination among combat veterans with posttraumatic stress disorder: a randomized clinical trial. JAMA Psychiatry. 2019;76(2):117–126. PubMed CrossRef NLM
Enjoy this premium PDF as part of your membership benefits!