Stress-Induced Cardiomyopathy and Possible Link to Cerebral Executive Function: A Case Report
To the Editor: A complex and poorly understood relationship exists between cerebral and cardiac function.1 Stress produces a range of physiological responses that are relevant to cardiovascular and cerebrovascular disease. Upon stress perception, the hypothalamic-pituitary-adrenocortical (HPA) and sympatho-adrenomedullary axes are activated, increasing bioavailability of cortisol, epinephrine, and norepinephrine.2 Given the reliance of both cardiac and cerebral function on the integrity of this system, any impairment in the form of overstimulation or understimulation may manifest as cardiac and cerebrovascular pathology as illustrated in the case report below.
Case report. Ms A, a 56-year-old woman with known hypertension and hypercholesterolemia, was admitted with chest pain following an argument with a family member. She had no history of ischemic heart or neurologic disease. On presentation, she was noted to be confused.
Physical examination was unremarkable with no focal neurologic or cardiac abnormality identified. Further investigations revealed troponin T and creatine kinase peak concentrations of 1.15 μg/L (reference range, < 0.03 μg/L) and 614 U/L (reference range, < 180 U/L), respectively. Admission electrocardiogram (ECG) demonstrated sinus rhythm without ischemic changes (Figure 1). Computed tomography scan of the brain was unremarkable. She continued to experience amnesia over the first 12 hours after her admission; amnesia had resolved by the following day. An urgent neurology consultation was sought, and the diagnosis of transient global amnesia was made on the basis of the patient’s clinical features.
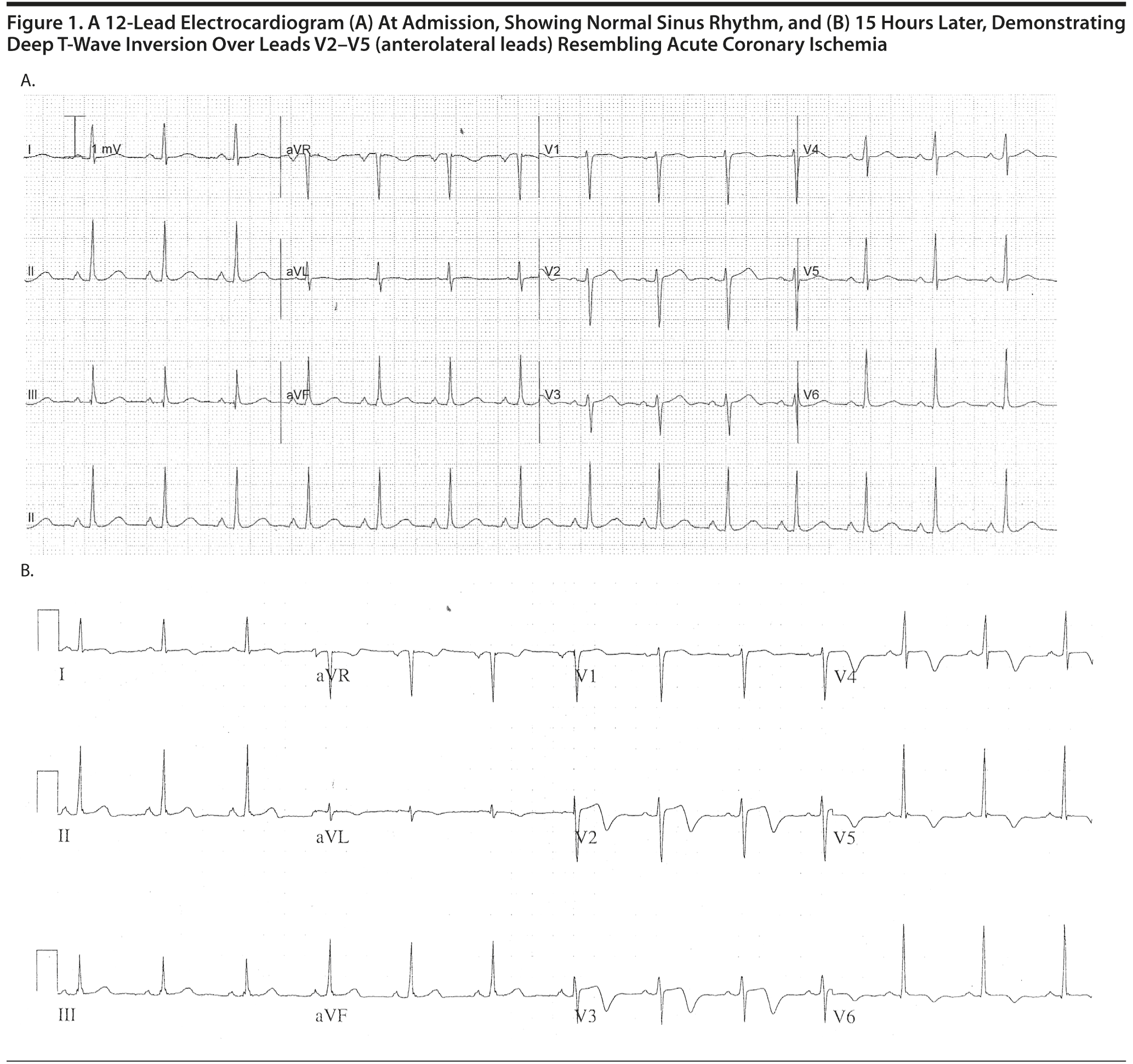
Ms A was admitted to the coronary care unit; serial ECG monitoring showed biphasic and deep T-wave inversion over the anterolateral leads (see Figure 1). She underwent coronary angiography, which showed “smooth” coronary arteries and apical “ballooning” on left ventriculography consistent with takotsubo cardiomyopathy. Magnetic resonance imaging of the brain identified an incidental 6-mm left middle cerebral artery aneurysm with no associated hemorrhage or ischemia. Her final diagnoses were stress-induced (takotsubo) cardiomyopathy and transient global amnesia.
Adrenergic receptors are abundant throughout the brain,3 myocardium,4 and coronary arteries.5 It is well established that catecholamine signaling through β-adrenergic receptors mediates endogenous regulation of complex central nervous system processes such as attention, arousal, learning, and memory3,6–8 as well as important cardiac functions such as chronotropy, inotropy, and lusitropy. There is general consensus that this “cerebro-cardiac” process occurs via the β-adrenoceptor–mediated cyclic-AMP (cAMP)–dependent protein kinase pathway.9–11
A growing body of evidence suggests that cortisone and epinephrine may also impair memory retrieval and therefore contribute to the mechanism of peritraumatic amnesia. de Quervain and colleagues reported that stress and infusion of cortisone impair memory retrieval in rats12 and humans.13 Sadowski et al10 demonstrated that infusion of epinephrine resulted in impairment of place and response learning. Furthermore, detrimental effects of cortisone on hippocampal function during memory retrieval have been shown to require concurrent norepinephrine-dependent activation of the basolateral part of the amygdala,14,15 which may be via an inhibitory G protein–coupled suppression of cAMP signaling.16,17 Altogether, memory formation, consolidation, and retrieval seem to be a function of β1-adrenergic receptor function, and stress impairs memory retrieval by exerting its action on the β2-adrenergic receptor.
Catecholamine overstimulation has been suggested as the key pathogenetic factor in takotsubo cardiomyopathy. This cardiac syndrome is now increasingly recognized by the mental health practitioner as either a disease association18,19 or a complication of a psychiatric treatment, such as electroconvulsive therapy.20,21 Although the exact pathogenesis has not been fully elucidated, data from animal,22 imaging,23 and myocardial histologic24 studies indicate that overactive β-adrenergic signaling, in the presence of supraphysiological catecholamine concentrations, plays a significant role in mediating this phenomenon. Given the density of β-adrenergic receptors are greatest25 in the apical segments of the myocardium, Lyon and colleagues4 suggest these receptors are important in this disease phenomenon, which explains the apical propensity of transient myocardial stunning seen in takotsubo cardiomyopathy.
Our case report provides a collection of cardiac and cerebral clinical findings that would support the common mechanistic link described in our review. Further understanding of this complex, dynamic relationship is required to formulate a more targeted preventive and therapeutic management strategy.
References
1. Samuels MA. The brain-heart connection. Circulation. 2007;116(1):77–84. doi:10.1161/CIRCULATIONAHA.106.678995 PubMed
2. Steptoe A, Kivimäki M. Stress and cardiovascular disease. Nat Rev Cardiol. 2012;9(6):360–370. doi:10.1038/nrcardio.2012.45 PubMed
3. Roozendaal B, McEwen BS, Chattarji S. Stress, memory and the amygdala. Nat Rev Neurosci. 2009;10(6):423–433. doi:10.1038/nrn2651 PubMed
4. Lyon AR, Rees PS, Prasad S, et al. Stress (Takotsubo) cardiomyopathy—a novel pathophysiological hypothesis to explain catecholamine-induced acute myocardial stunning. Nat Clin Pract Cardiovasc Med. 2008;5(1):22–29. doi:10.1038/ncpcardio1066 PubMed
5. Jensen BC, Swigart PM, Laden ME, et al. The alpha-1D: is the predominant alpha-1-adrenergic receptor subtype in human epicardial coronary arteries. J Am Coll Cardiol. 2009;54(13):1137–1145. doi:10.1016/j.jacc.2009.05.056 PubMed
6. Hurlemann R. Noradrenergic-glucocorticoid mechanisms in emotion-induced amnesia: from adaptation to disease. Psychopharmacology (Berl). 2008;197(1):13–23. doi:10.1007/s00213-007-1002-x PubMed
7. Hurlemann R, Hawellek B, Matusch A, et al. Noradrenergic modulation of emotion-induced forgetting and remembering. J Neurosci. 2005;25(27):6343–6349. PubMed
8. Hagena H, Manahan-Vaughan D. Learning-facilitated long-term depression and long-term potentiation at mossy fiber-CA3 synapses requires activation of β-adrenergic receptors. Front Integr Neurosci. 2012;6:23. doi:10.3389/fnint.2012.00023 PubMed
9. Murchison CF, Schutsky K, Jin SH, et al. Norepinephrine and β1-adrenergic signaling facilitate activation of hippocampal CA1 pyramidal neurons during contextual memory retrieval. Neuroscience. 2011;181:109–116. doi:10.1016/j.neuroscience.2011.02.049 PubMed
10. Sadowski RN, Jackson GR, Wieczorek L, et al. Effects of stress, corticosterone, and epinephrine administration on learning in place and response tasks. Behav Brain Res. 2009;205(1):19–25. doi:10.1016/j.bbr.2009.06.027 PubMed
11. McGaugh JL, Roozendaal B. Role of adrenal stress hormones in forming lasting memories in the brain. Curr Opin Neurobiol. 2002;12(2):205–210. doi:10.1016/S0959-4388(02)00306-9 PubMed
12. de Quervain DJ, Roozendaal B, McGaugh JL. Stress and glucocorticoids impair retrieval of long-term spatial memory. Nature. 1998;394(6695):787–790. doi:10.1038/29542 PubMed
13. de Quervain DJ, Roozendaal B, Nitsch RM, et al. Acute cortisone administration impairs retrieval of long-term declarative memory in humans. Nat Neurosci. 2000;3(4):313–314. doi:10.1038/73873 PubMed
14. Roozendaal B, Hahn EL, Nathan SV, et al. Glucocorticoid effects on memory retrieval require concurrent noradrenergic activity in the hippocampus and basolateral amygdala. J Neurosci. 2004;24(37):8161–8169. doi:10.1523/JNEUROSCI.2574-04.2004 PubMed
15. Roozendaal B, Okuda S, Van der Zee EA, et al. Glucocorticoid enhancement of memory requires arousal-induced noradrenergic activation in the basolateral amygdala. Proc Natl Acad Sci U S A. 2006;103(17):6741–6746. doi:10.1073/pnas.0601874103 PubMed
16. Schutsky K, Ouyang M, Castelino CB, et al. Stress and glucocorticoids impair memory retrieval via beta2-adrenergic, Gi/o-coupled suppression of cAMP signaling. J Neurosci. 2011;31(40):14172–14181.
17. Schutsky K, Ouyang M, Thomas SA. Xamoterol impairs hippocampus-dependent emotional memory retrieval via Gi/o-coupled β2-adrenergic signaling. Learn Mem. 2011;18(9):598–604. doi:10.1101/lm.2302811 PubMed
18. Maldonado JR, Pajouhi P, Witteles R. Broken heart syndrome (Takotsubo cardiomyopathy) triggered by acute mania: a review and case report. Psychosomatics. 2013;54(1):74–79. doi:10.1016/j.psym.2012.03.009 PubMed
19. Summers MR, Lennon RJ, Prasad A. Pre-morbid psychiatric and cardiovascular diseases in apical ballooning syndrome (tako-tsubo/stress-induced cardiomyopathy): potential pre-disposing factors? J Am Coll Cardiol. 2010;55(7):700–701. doi:10.1016/j.jacc.2009.10.031 PubMed
20. Serby MJ, Lantz M, Chabus BI, et al. Takotsubo cardiomyopathy and electroconvulsive treatments: a case study and review. Int J Psychiatry Med. 2010;40(1):93–96. doi:10.2190/PM.40.1.g PubMed
21. Sharp RP, Welch EB. Takotsubo cardiomyopathy as a complication of electroconvulsive therapy. Ann Pharmacother. 2011;45(12):1559–1565. doi:10.1345/aph.1Q393 PubMed
22. Ueyama T, Kasamatsu K, Hano T, et al. Catecholamines and estrogen are involved in the pathogenesis of emotional stress-induced acute heart attack. Ann N Y Acad Sci. 2008;1148(1):479–485. doi:10.1196/annals.1410.079 PubMed
23. Prasad A, Madhavan M, Chareonthaitawee P. Cardiac sympathetic activity in stress-induced (Takotsubo) cardiomyopathy. Nat Rev Cardiol. 2009;6(6):430–434. doi:10.1038/nrcardio.2009.51 PubMed
24. Wittstein IS. Stress cardiomyopathy: a syndrome of catecholamine-mediated myocardial stunning? Cell Mol Neurobiol. 2012;32(5):847–857. doi:10.1007/s10571-012-9804-8 PubMed
25. Mori H, Ishikawa S, Kojima S, et al. Increased responsiveness of left ventricular apical myocardium to adrenergic stimuli. Cardiovasc Res. 1993;27(2):192–198. doi:10.1093/cvr/27.2.192 PubMed
Author affiliations: Cardiovascular Research Centre, Department of Medicine, University of Adelaide, Adelaide (Drs Sidharta, Nelson, and Worthley); and Eastern Health, Department of Cardiology, Box Hill Hospital, Victoria (Drs Sajeev and Cooke), Australia.
Potential conflicts of interest: None reported.
Funding/support: None reported.
Published online: December 5, 2013.
Prim Care Companion CNS Disord 2013;15(6):doi:10.4088/PCC.13l01557
© Copyright 2013 Physicians Postgraduate Press, Inc.
Enjoy this premium PDF as part of your membership benefits!


