Objective: To identify key mood, social, and functional correlates of current participation in mental health treatment and barriers to participation in mental health treatment among older HIV infected (HIV+) veterans.
Methods: HIV+ veterans (N = 150) aged ≥ 50 years receiving HIV-related medical care at the VA San Diego Healthcare System, San Diego, California, anonymously completed a survey assessing current self-reported mood, social support, daily functioning problems, mental health service utilization, and barriers to participating in mental health services. Veterans also completed the 2-item Patient Health Questionnaire (PHQ-2), a validated depression screening instrument frequently used in primary care settings. Data were collected from February 2014 to May 2014.
Results: Overall, 44% of participants screened positive for depressive symptomatology on the PHQ-2; 55% of those who screened positive were participating in mental health treatment. Of the 45% of veterans who screened positive on the PHQ-2 and were not in treatment, two-thirds (66%) stated they had been offered services; however, they were not engaging in or accepting the services. Regardless of PHQ-2 status, current self-reported depressive symptoms emerged as an independent, significant positive predictor of participation in mental health treatment (odds ratio = 5.98; 95% CI, 1.16-30.72; P = .03), whereas anxiety, HIV-related stigma, sufficiency of social support, and daily functioning problems were not associated with mental health treatment utilization. Primary reported barriers to mental health treatment included scheduling/availability, travel time and transportation, and discomfort with group settings.
Conclusions: Results of this study suggest there may be a need to better engage older HIV+ veterans in depression-related treatment. The use of telehealth technology, such as teletherapy, electronic devices, and cell phone-based programs, may be beneficial in helping older HIV+ veterans overcome many barriers that restrict their participation in mental health treatment.
Predictors and Barriers to Mental Health Treatment
Utilization Among Older Veterans Living With HIV
ABSTRACT
Objective: To identify key mood, social, and functional correlates of current participation in mental health treatment and barriers to participation in mental health treatment among older HIV infected (HIV+) veterans.
Methods: HIV+ veterans (N = 150) aged ≥ 50 years receiving HIV-related medical care at the VA San Diego Healthcare System, San Diego, California, anonymously completed a survey assessing current self-reported mood, social support, daily functioning problems, mental health service utilization, and barriers to participating in mental health services. Veterans also completed the 2-item Patient Health Questionnaire (PHQ-2), a validated depression screening instrument frequently used in primary care settings. Data were collected from February 2014 to May 2014.
Results: Overall, 44% of participants screened positive for depressive symptomatology on the PHQ-2; 55% of those who screened positive were participating in mental health treatment. Of the 45% of veterans who screened positive on the PHQ-2 and were not in treatment, two-thirds (66%) stated they had been offered services; however, they were not engaging in or accepting the services. Regardless of PHQ-2 status, current self-reported depressive symptoms emerged as an independent, significant positive predictor of participation in mental health treatment (odds ratio = 5.98; 95% CI, 1.16–30.72; P = .03), whereas anxiety, HIV-related stigma, sufficiency of social support, and daily functioning problems were not associated with mental health treatment utilization. Primary reported barriers to mental health treatment included scheduling/availability, travel time and transportation, and discomfort with group settings.
Conclusions: Results of this study suggest there may be a need to better engage older HIV+ veterans in depression-related treatment. The use of telehealth technology, such as teletherapy, electronic devices, and cell phone–based programs, may be beneficial in helping older HIV+ veterans overcome many barriers that restrict their participation in mental health treatment.
Prim Care Companion CNS Disord 2017;19(1):16m02059
https://doi.org/10.4088/PCC.16m02059
© Copyright 2017 Physicians Postgraduate Press, Inc.
aVA San Diego Healthcare System, San Diego, California
bDepartment of Psychiatry, University of California San Diego, La Jolla, California
cThe Sam and Rose Stein Institute for Research on Aging, University of California San Diego, La Jolla, California
dCalifornia School of Professional Psychology, Alliant International University, San Diego, California
*Corresponding author: Raeanne C. Moore, PhD, Department of Psychiatry, University of California, San Diego, 220 Dickinson Drive, St B (8231), San Diego, CA 92103-8231 ([email protected]).
The Veterans Health Administration is the largest single provider of HIV treatment in the United States, providing care for approximately 24,000 HIV-infected (HIV+) veterans annually.1 One of every 250 veterans receiving services at the Veterans Health Administration is living with HIV/AIDS.1 Due to advances in highly active antiretroviral therapy and high late-life infection rates, a substantial portion of these HIV+ veterans are 50 years of age or older, and this number of older HIV+ veterans continues to rise.2,3 While HIV+ veterans of all ages face additional challenges beyond their HIV+ status, older veterans with HIV face numerous behavioral health problems.4–7
There is a pressing need for increased knowledge about the behavioral health needs of older HIV+ veterans. Prevalence rates of mood and substance use disorders are elevated in older HIV+ adults compared to older HIV uninfected (HIV–) adults and have been reported to be as high as 50%.8 In addition to heightened risk for clinical depression, those aging with HIV are at increased risk for negative mood and apathy compared to those without HIV.9 Moreover, the expected declines in diagnoses of major depressive disorder associated with older HIV– adults are not generally apparent in those with HIV.10–13 This co-occurrence of mental illness and HIV results in poor health outcomes, including decreased CD4 T-lymphocytes, increased viral loads, and high health care costs.14 In terms of psychosocial functioning, the Veterans Aging Cohort Study15 found that social isolation is related to greater risk of hospitalization and death in HIV+ veterans compared with HIV– veterans. Moreover, this population faces additional burden from HIV-related stigma and disability, which is frequently compounded by ageism, and psychosocial challenges such as availability of social support. Despite the considerable risks associated with this population, studies16 estimate 40%–90% of mental health concerns remain undetected in primary care settings. This lack of adequate detection results in mental health problems going untreated among older HIV+ adults. If these problems could be readily identified, more patients would potentially be offered treatment. Whether they engage in treatment is another important question, and this study aims to discover predictors of engagement and potential barriers to mental health service utilization.
This study’s first aim was to identify key mood, social, and daily functioning correlates of current participation in mental health treatment in an older HIV+ veteran sample. The 2-item Patient Health Questionnaire (PHQ-2)17 was utilized to identify patients in need of mental health services. The PHQ-2 is commonly used as a depression screener in primary care and infectious disease clinics, and positive screens often prompt mental health service referrals. Next, predictors of treatment utilization were explored among participants with positive PHQ-2 screens. Predictors of treatment engagement were also evaluated on the basis of endorsement of current self-reported depressive symptoms.
The second aim of this study was to examine barriers to participating in mental health treatment. Treatment barriers have not been formally evaluated, despite the substantial portion of veterans living with HIV and comorbid diagnoses not accessing Veterans Administration (VA) services. Potential obstacles most likely include identifying patients with the greatest need for treatment, scheduling difficulties, time and travel to treatment, and privacy concerns. The examination of factors relating to barriers and engagement in mental health treatment may lead to targeted solutions for this growing and vulnerable population.
METHODS
Participants and Design
Participants included 150 older (age range, 50–81 years) HIV+ veterans receiving HIV-related medical care at the VA San Diego Healthcare System, San Diego, California. Data were collected from February 2014 to May 2014. Potential HIV+ participants were identified and approached by clinical staff at the VA special infectious diseases (SPID) clinic during their routine medical visit and asked to complete an anonymous survey. Surveys were completed in the waiting area and sealed in an envelope by the participant. Surveys were completed by 265 unique veterans; however, only those aged ≥ 50 years were included in the analysis. Of the patients approached, 9% refused to complete the survey, 10% did not return it, and 6% began the survey and discontinued. The study was approved by the VA San Diego Healthcare System Institutional Review Board. All participants received a copy of a stamped informed consent and the California Experimental Subject’s Bill of Rights.
Measures
Demographic characteristics. To ensure anonymity, age was the only demographic characteristic collected. There are a very small number of HIV+ women who receive care at the SPID clinic, so we did not collect sex as a demographic as it would have been considered identifying information.
Mental Health Needs Assessment Survey. We developed a self-report Mental Health Needs Assessment Survey to evaluate mental health, psychosocial, and daily functioning problems of HIV+ veterans and mental health utilization. Survey questions were developed through a literature review and vetted through a consensus process with experts in the field and with VA SPID clinical staff. Depressive symptomatology was measured by the PHQ-217 and a yes/no item (“Are you currently suffering from depression?”). The PHQ-2 and yes/no depression items were highly correlated (r = 0.69, P < .001). Dichotomous (yes/no) items were used to assess anxiety, stress, HIV-related stigma, and daily functioning problems in the following areas: activities of daily living, instrumental activities of daily living, antiretroviral adherence, and driving problems. A dichotomous variable was created by collapsing endorsement of 1 or more of the daily functioning problems into “yes” and no endorsement of any problems into “no.” The survey also included the following yes/no questions: (1) “Do you feel you have sufficient support to address your mental health needs at this time?” (2) “Do you feel the San Diego VA is adequately addressing your mental health needs as a person living with HIV/AIDS?” (3) “Have you been offered mental health treatment at the San Diego VA?” We wanted to assess mental health needs and not burden the participants or staff with long measures, which is why we chose to use these brief, dichotomous questions instead of validated instruments of anxiety, stress, stigma, and daily functioning. Additionally, the participants completed our survey in the waiting area prior to their clinic appointment, so we needed to ensure the survey could be completed in a short time and would not disrupt the flow of the clinic.
Additionally, participants were asked an open-ended question regarding barriers to participating in mental health treatment: “What do you feel would keep you from attending group sessions designed specifically to support mental health needs for veterans living with HIV?” Group therapy was selected as a prompt given that it was a service we would be interested in implementing. Two authors (R.C.M. and E.S.) independently categorized responses to the open-ended question into 5 categories: travel time to the VA and transportation costs (eg, “distance and time to VA”), group settings (eg, “I do not do well in group settings,” “I don’t want to be outed”), time constraints (eg, “my busy schedule,” “time off from work”), not needed (eg, “not necessary at this time”), and other (eg, “HIV stigma,” “health-related problems”). Interrater reliability of coding of the open-ended responses was excellent, with κ = 0.90, P < .001. Discrepancies were discussed by the 2 authors and resolved.
Statistical Analyses
IBM SPSS Statistics version 2118 was used to conduct all analyses. A PHQ-2 cut point of ≥ 2 was used on the basis of improved sensitivity over more conservative cut points.19 Participants with a positive PHQ-2 screening result were compared on the basis of whether they were or were not participating in mental health treatment. We conducted χ2 tests to examine differences in rate of mood (ie, depression, anxiety, and stress), social support, and functional problems between the 2 groups. Logistic regression was used to identify independent correlates of participation in mental health treatment.
RESULTS
Mood, Social, and Functional Correlates of Mental Health Service Utilization
Six participants did not complete the PHQ-2 questions, which left 144 participants for analyses. Of the participants, 44% screened positive for depressive symptomatology (PHQ-2 score ≥ 2). Of those screening positive, 55% reported participation in mental health treatment. A majority of these services were obtained at the VA (89%). Our survey did not specify if community services were obtained through the VA’s Choice Act20 or independently. Sixty-six percent of veterans who screened positive on the PHQ-2 and were not in mental health treatment stated they had been offered services; however, they were not engaging in or accepting the services they were offered. Among those with positive PHQ-2 screens, participants who reported they were suffering from HIV-related stigma were more likely to be in treatment (χ2 = 4.22, P = .04) compared to those who did not report HIV-related stigma, whereas current self-reported depressed mood, anxiety, stress, functional problems, and insufficient social support were unrelated to treatment utilization.
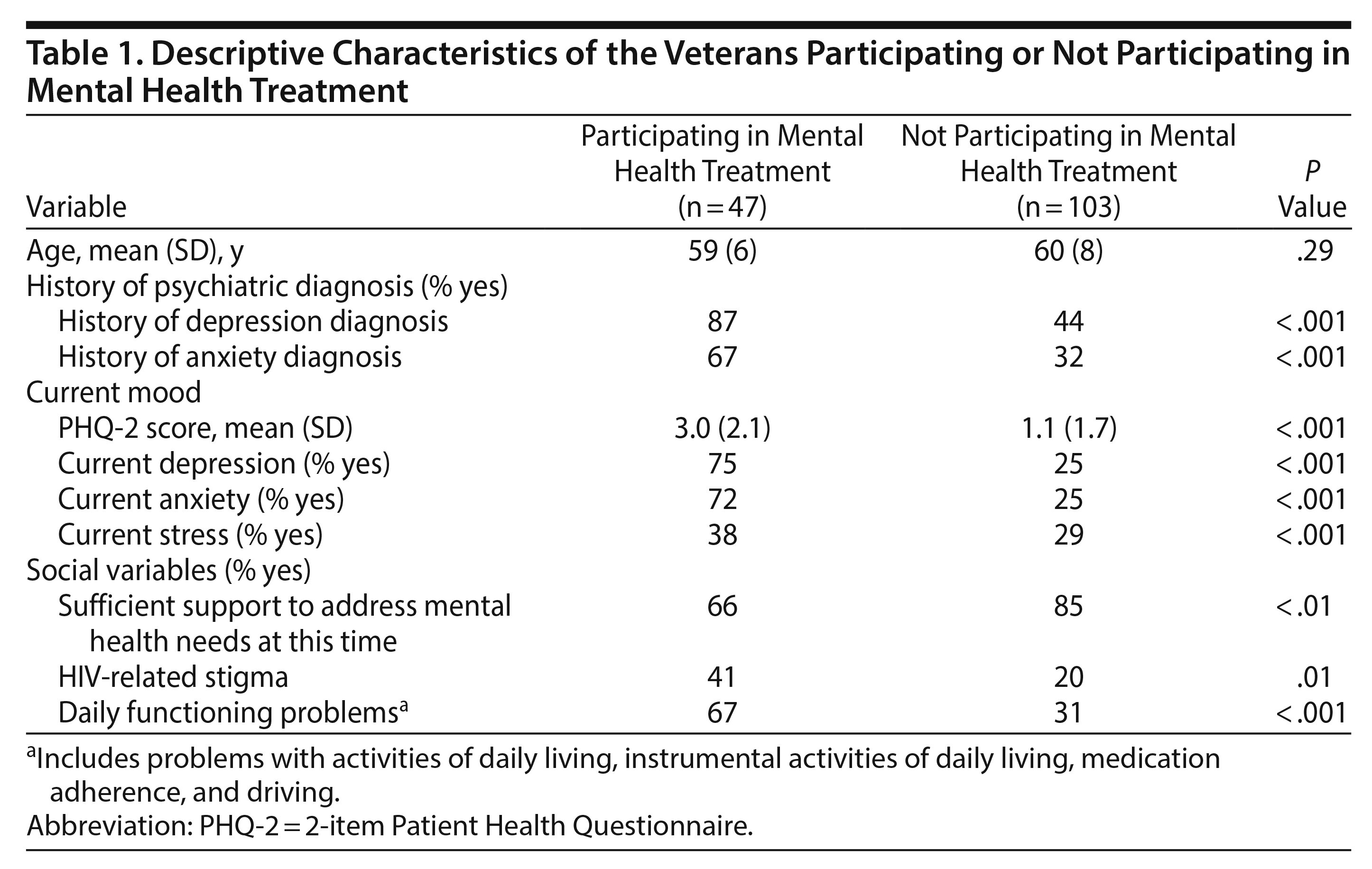
Next, we evaluated predictors of mental health utilization regardless of PHQ-2 status to further understand treatment engagement. Overall, approximately one-third (n = 47) of the sample was participating in mental health treatment. Of these participants, 77% received mental health care at the VA and 23% in the community. Table 1 shows age, mood, social, and functional characteristics by group (participating in mental health treatment: yes/no). Results from univariable analyses indicated HIV+ veterans in mental health treatment were significantly more likely to report current depression (χ2 = 30.75, P < .001), anxiety (χ2 = 27.30, P < .001), stress (χ2 = 15.90, P < .001), HIV-related stigma (χ2 = 6.24, P = .01), and functional problems (χ2 = 13.02, P < .001) and less likely to report having social support to address their mental health needs (χ2 = 7.13, P < .01, Table 1) compared to those not in mental health treatment. These factors were entered into a logistic regression model. Results indicated current depressive symptom reporting (odds ratio [OR] = 5.98; 95% CI, 1.16–30.72; P = .03) was the only independent significant predictor of current mental health treatment participation.
Mental Health Service Utilization at the VA San Diego
As shown in Table 2, participants in mental health treatment (either VA or community) were less likely to feel the VA was adequately addressing their mental health needs (χ2 = 8.14, P < .01) compared to those not in treatment, although a majority of those in treatment still felt the VA was adequately addressing their needs (71% vs 90%, respectively). Participants in treatment were also significantly more likely to have been offered mental health treatment at the VA San Diego compared to those not participating in mental health treatment (χ2=14.79, P < .001). Current mood problems (depressed mood, anxiety, and stress) were reported by approximately one-quarter of veterans not participating in mental health treatment. Of those veterans reporting current mental health problems and not in treatment, 78% stated they had been offered services, while 22% had not.

Barriers to older HIV+ veterans’ participating in mental health treatment. Seventy-one participants responded to an open-ended question regarding barriers to participating in VA mental health treatment (ie, group therapy). Five participants reported more than 1 treatment barrier. The following descriptive categories emerged: (1) scheduling/availability (28%), (2) travel time and transportation to and from the VA (27%), (3) dislike of group settings (23%), and (4) not needed (10%). Additional patient-reported barriers included HIV-associated stigma, shame, disinterest, and health-related problems (< 18% frequency).
DISCUSSION
Depression and other mental health problems, such as anxiety, stress, and HIV-related stigma, are common among older HIV+ veterans, yet the unique needs of this group warrant additional investigation given that a majority of HIV+ veterans are aged ≥ 50 years.3 In the present study, we found that all of the aforementioned factors, along with social support and functional problems, were significant correlates of participation in mental health treatment among older HIV+ veterans. One explanation for these findings is that veterans receiving treatment are in greater need of services, and it is precisely because of these increased mental health needs that they are receiving services. We also found current mental health problems (depressed mood, anxiety, and stress) in approximately one-quarter of veterans currently not participating in mental health treatment. A majority of these veterans had been offered services (78%) but for unknown reasons chose not to engage. An additional one-fifth of those identified as potentially in need of services denied they had been offered such services. It may be that these participants did not recognize the offered mental health services as such an offer. It may also be that the numerous medical and psychosocial comorbidities faced by this relatively “new” veteran population necessitate a coordinated care, team-based approach similar to care models that exist for other chronic illnesses (eg, diabetes). These findings are consistent with prior work by Zanjani et al,13 who found that despite evidence of need, older HIV+ adults were less likely to receive care for mental health and substance abuse than their younger counterparts.
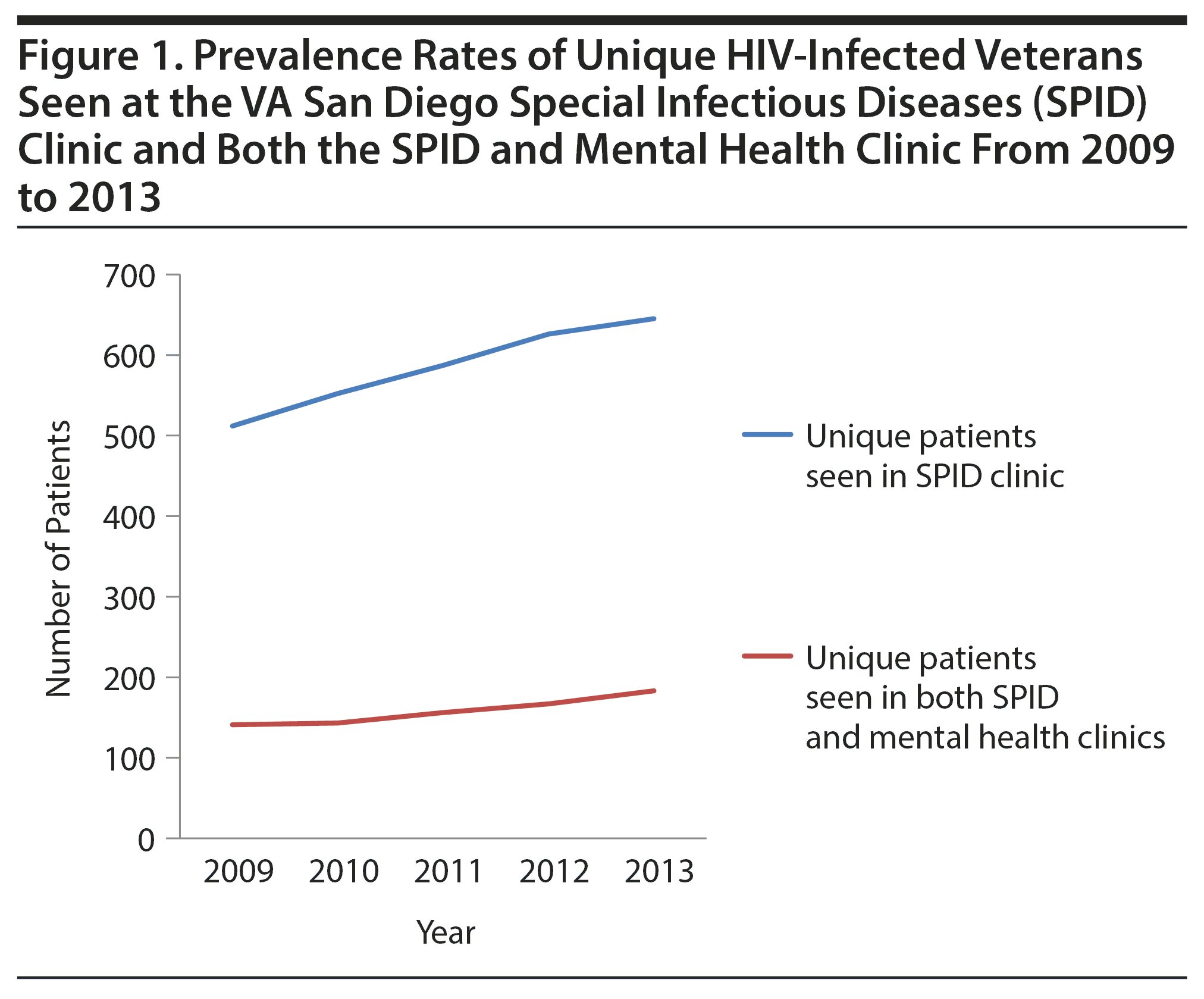
As a whole, the VA has made tremendous strides in increasing mental health treatment access in recent years, as evidenced by a 500,000 increase in veterans receiving specialized mental health treatment at the VA from 2006 to 2013.21 As seen in Figure 1, the number of VA San Diego SPID clinic patients has steadily increased, and the rates of veterans coenrolled in the SPID and mental health clinics have increased at a comparable rate. Additionally, the VA has played a leading role in recognition of potential improvements in both access efficiency and treatment efficacy through provision of mental health care within primary care clinics rather than specialized mental health clinics.22,23 The successful integration of many mental health services into primary care clinics significantly improved both access and quality of mental health care provided.24 Our findings suggest that many HIV+ veterans do not feel the mental health clinic is meeting their needs, and further expansion of the existing integrated model to include specialized mental health services for these veterans within primary care clinics may be warranted.
It is important to note that the most commonly reported barriers to mental health treatment were issues such as scheduling/availability, travel time, and transportation costs. The use of telehealth technology to address mental health needs, such as teletherapy, electronic devices, and cell phone–based programs, can help overcome many of these common barriers to treatment. To increase access to care, the VA has implemented telemental health in many clinics.21 Leveraging this technology in infectious disease clinics would help increase the flexibility of appointment times to synchronize with the schedules of older HIV+ veterans, reduce travel time and distance, and, ultimately, may improve quality of life in these veterans. Another notable barrier to treatment was dislike of group settings. While our survey specifically asked about interest and barriers to group therapy, thereby priming participants to think about group treatment, it nonetheless is an important barrier within this population, especially considering the high reported rates of HIV-related stigma. Telehealth technology may address this barrier, and there are several emerging mental health cell phone–based programs that may provide personalized, individualized treatment with reduced staff burden.25 Other reported treatment barriers included shame, disinterest, and health-related problems. The diversity of reported treatment obstacles suggests assessment of these barriers should occur during initial treatment planning sessions. This assessment may result in increased mental health utilization and foster active treatment engagement among veterans. Findings from open-ended questions in the present study can help develop a structured measure of treatment barriers for this population.
In the present study, the PHQ-2 appears to be an adequate screening instrument to identify those in need of mental health services. When PHQ-2 scores were not taken into consideration, current self-report of depressive symptoms was the only independent correlate of mental health treatment participation. Both methods therefore indicated depressive symptomatology was the most potent predictor of mental health service utilization. This finding may be because reporting depressive symptoms results in the provision of mental health services. It may also be that the SPID clinic screens depressive symptoms more routinely than other mental health symptoms. It is worth noting that over a quarter of older HIV+ veterans not engaged in treatment still endorsed depressive symptoms, as well as anxiety and stress, and a proportion had yet to be offered services. These findings highlight the need to screen for mental health symptoms in this veteran group with high health care needs. The inclusion of mental health screenings at infectious disease and primary care clinics may ensure that the psychological needs of HIV+ older adults are identified and treated. According to the American Psychological Association,26 4 of 5 individuals with HIV do not receive effective mental health treatment, largely due to “one size fits all” systems of health care, which is inadequate in meeting the complex needs of those aging with HIV. Our data indicate a larger proportion of HIV+ veterans are receiving treatment than this national average, and of those not receiving treatment, the majority feel the VA has the resources necessary. The VA’s integrated health care model is a strong environment in which to advance this issue, and continued efforts to integrate primary health care, geriatricians, HIV providers, and mental health treatment may address the complex needs of this growing population.26 Comprehensive assessment and integrated health care planning in this population are necessary and have already been identified as priority areas by the VA.27
The present study had several limitations. As our survey was administered anonymously, age was the only demographic characteristic collected. Thus, we cannot characterize our sample in terms of other important factors, such as sex, education level, socioeconomic status, and race/ethnicity. There might be important differences among subgroups of older veterans that are yet to be discerned. Additionally, substance abuse was not evaluated despite the high rates of abuse within this population. While we used a validated measure to assess depressive symptomatology, we did not include validated measures of anxiety and stress, to keep the burden on the participants and SPID clinic staff low. Nonetheless, we found some useful information that could be followed up with a more thorough set of measures (eg, Beck Anxiety Inventory,28 Perceived Stress Scale29). Another limitation is that the survey did not assess the modality of mental health treatment that veterans were offered or participated in (eg, whether participants were receiving psychotherapy, psychopharmacology, or a combination of both). Lastly, all data were collected via participants’ self-report. Future studies should also include objective assessments, such as chart reviews, to better understand the mental health needs of this population.
CONCLUSIONS
Comprehensive and integrated care models are necessary given the large number of veterans with comorbid HIV and mental health needs. Efforts to combat HIV and mental health stigma and to integrate primary health and mental health care at infectious disease or general medicine clinics will most likely improve the overall well-being in persons living and aging with this disease. Additionally, the use of telehealth and mobile health technology may decrease the barriers associated with mental health treatment.
Submitted: September 28, 2016; accepted
November 3, 2016.
Published online: February 2, 2017.
Potential conflicts of interest: Dr D. J. Moore has received grant support from Gillead Sciences.
Funding/support: Salary support for this research was provided, in part, by the National Institute of Mental Health grants K23 MH107260 (Dr R. C. Moore), K23 MH105297 (Dr Marquine), and T32 MH019934 (Dr R. C. Moore). Salary support for Dr Schiehser was provided by VA RR&D MERIT 1 I01 RX001691-01A1.
Role of the sponsor: The funder provided salary support.
Previous presentation: These data were presented at the 18th Annual United States Conference on AIDS; October 2–5, 2014; San Diego, California.
Disclaimer: The views expressed in this article are those of the authors and do not necessarily reflect the position or policy of the Department of Veterans Affairs.
REFERENCES
1. Department of Veterans Affairs. National HIV/AIDS Strategy Operational Plan 2011. AIDS.gov website. https://www.aids.gov/federal-resources/national-hiv-aids-strategy/nhas-operational-plan-va.pdf. Accessed January 4, 2017.
2. HIV/AIDS among persons 50 and older. 2008. CDC website.https://www.cdc.gov/hiv/group/age/olderamericans/. Accessed January 8, 2013.
3. Vance DE, Cody SL. Predictions of geriatric HIV in 2030. Lancet Infect Dis. 2015;15(7):753–754. PubMed doi:10.1016/S1473-3099(15)00063-8
4. Justice AC. HIV and aging: time for a new paradigm. Curr HIV/AIDS Rep. 2010;7(2):69–76. PubMed doi:10.1007/s11904-010-0041-9
5. Moore RC, Moore DJ, Thompson WK, et al. A case-controlled study of successful aging in older HIV-infected adults. J Clin Psychiatry. 2013;74(5):e417–e423. PubMed doi:10.4088/JCP.12m08100
6. Stoff DM. Mental health research in HIV/AIDS and aging: problems and prospects. AIDS. 2004;18(suppl 1):S3–S10. PubMed doi:10.1097/00002030-200401001-00002
7. High KP, Brennan-Ing M, Clifford DB, et al; OAR Working Group on HIV and Aging. HIV and aging: state of knowledge and areas of critical need for research: a report to the NIH Office of AIDS Research by the HIV and Aging Working Group. J Acquir Immune Defic Syndr. 2012;60(suppl 1):S1–S18. PubMed doi:10.1097/QAI.0b013e31825a3668
8. Pence BW, Miller WC, Whetten K, et al. Prevalence of DSM-IV-defined mood, anxiety, and substance use disorders in an HIV clinic in the southeastern United States. J Acquir Immune Defic Syndr. 2006;42(3):298–306. PubMed doi:10.1097/01.qai.0000219773.82055.aa
9. Ciesla JA, Roberts JE. Meta-analysis of the relationship between HIV infection and risk for depressive disorders. Am J Psychiatry. 2001;158(5):725–730. PubMed doi:10.1176/appi.ajp.158.5.725
10. Justice AC, McGinnis KA, Atkinson JH, et al; Veterans Aging Cohort 5-Site Study Project Team. Psychiatric and neurocognitive disorders among HIV-positive and negative veterans in care: Veterans Aging Cohort Five-Site Study. AIDS. 2004;18(suppl 1):S49–S59. PubMed doi:10.1097/00002030-200401001-00008
11. Rabkin JG, McElhiney MC, Ferrando SJ. Mood and substance use disorders in older adults with HIV/AIDS: methodological issues and preliminary evidence. AIDS. 2004;18(suppl 1):S43–S48. PubMed doi:10.1097/00002030-200401001-00007
12. Vance DE, Mugavero M, Willig J, et al. Aging with HIV: a cross-sectional study of comorbidity prevalence and clinical characteristics across decades of life. J Assoc Nurses AIDS Care. 2011;22(1):17–25. PubMed doi:10.1016/j.jana.2010.04.002
13. Zanjani F, Saboe K, Oslin D. Age difference in rates of mental health/substance abuse and behavioral care in HIV-positive adults. AIDS Patient Care STDS. 2007;21(5):347–355. PubMed doi:10.1089/apc.2006.0043
14. Rothbard AB, Miller K, Lee S, et al. Revised cost estimates of Medicaid recipients with serious mental illness and HIV-AIDS. Psychiatr Serv. 2009;60(7):974–977. PubMed doi:10.1176/ps.2009.60.7.974
15. Greysen SR, Horwitz LI, Covinsky KE, et al. Does social isolation predict hospitalization and mortality among HIV+ and uninfected older veterans? J Am Geriatr Soc. 2013;61(9):1456–1463. PubMed doi:10.1111/jgs.12410
16. US Department of Health and Human Services. Impact of mental illness on people living with HIV 2015. https://hab.hrsa.gov/sites/default/files/hab/Publications/careactionnewsletter/mentalhealth.pdf. Accessed January 4, 2017.
17. Kroenke K, Spitzer RL, Williams JB. The Patient Health Questionnaire-2: validity of a two-item depression screener. Med Care. 2003;41:1284–1292. PubMed doi:10.1046/j.1525-1497.2001.016009606.x
18. IBM SPSS Statistics for Windows, Version 21.0. Armonk, NY: IBM Corporation; 2012.
19. Corson K, Gerrity MS, Dobscha SK. Screening for depression and suicidality in a VA primary care setting: 2 items are better than 1 item. Am J Manag Care. 2004;10(11 pt 2):839–845. PubMed
20. US Department of Veterans Affairs. Veterans Access, Choice and Accountability Act of 2014 (“Choice Act”). VA.gov website. http://www.va.gov/opa/choiceact/documents/choice-act-summary.pdf. Accessed January 4, 2017.
21. US Department of Veterans Affairs. VA Mental Health Care Fact Sheet 2015. https://commissiononcare.sites.usa.gov/files/2015/12/20151019-04-VA_Fact_Sheet-VA_Mental_Health_Care_SEP15.pdf .
22. Rubenstein L, Chaney E, Kearney L, et al. Report on Integrating Mental Health Into PACT (IMHIP) in the VA. September 2013. http://www.hsrd.research.va.gov/publications/internal/IMHIP-Report.pdf. Accessed January 4, 2017.
23. Pomerantz A, Cole BH, Watts BV, et al. Improving efficiency and access to mental health care: combining integrated care and advanced access. Gen Hosp Psychiatry. 2008;30(6):546–551. PubMed doi:10.1016/j.genhosppsych.2008.09.004
24. Watts BV, Shiner B, Pomerantz A, et al. Outcomes of a quality improvement project integrating mental health into primary care. Qual Saf Health Care. 2007;16(5):378–381. PubMed doi:10.1136/qshc.2007.022418
25. Depp CA, Ceglowski J, Wang VC, et al. Augmenting psychoeducation with a mobile intervention for bipolar disorder: a randomized controlled trial. J Affect Disord. 2015;174:23–30. PubMed doi:10.1016/j.jad.2014.10.053
26. American Psychological Association. Resolution on psychologists in integrated primary care and specialty health settings. 2016. APA website. http://www.apa.org/about/policy/integrated-primary-care.aspx
27. US Department of Veterans Affairs. HIV/AIDS for health care providers: integrated mental health care. 2015. VA.gov Web site. http://www.hiv.va.gov/provider/integrated-mental-health.asp. Accessed November 6, 2015.
28. Creamer M, Foran J, Bell R. The Beck Anxiety Inventory in a non-clinical sample. Behav Res Ther. 1995;33(4):477–485. PubMed doi:10.1016/0005-7967(94)00082-U
29. Cohen S, Kamarck T, Mermelstein R. A global measure of perceived stress. J Health Soc Behav. 1983;24(4):385–396. PubMed doi:10.2307/2136404
Enjoy this premium PDF as part of your membership benefits!


