Psychogenic movement disorders (PMDs) are common, associated with significant psychosocial impairments, and frequently comorbid with other physical and psychiatric conditions. However, treatment of PMDs has been largely unsuccessful. Recently, treatments focused on conditions comorbid with PMDs have been hypothesized as a possible improvement to PMD-focused treatments. This case report describes a patient initially diagnosed with a PMD and referred for psychotherapy after appointments with neurologic and psychiatric providers. Upon referral to psychotherapy, the patient received a diagnosis of comorbid obsessive-compulsive disorder (OCD) and treatment with exposure and response prevention (ERP), an evidence-based psychotherapy for OCD. The patient demonstrated reliable improvements in all self-report measures as well as remission of PMD and OCD symptoms via behavioral observation at the end of therapy and at a 1-month follow-up. This case presents initial support for the treatment of comorbid and overlapping conditions in patients with PMDs, providing a pilot demonstration to support future large investigations.

Exposure and Response Prevention for Comorbid Symptoms of Obsessive-Compulsive Disorder and Psychogenic Movement Disorder

ABSTRACT
Psychogenic movement disorders (PMDs) are common, associated with significant psychosocial impairments, and frequently comorbid with other physical and psychiatric conditions. However, treatment of PMDs has been largely unsuccessful. Recently, treatments focused on conditions comorbid with PMDs have been hypothesized as a possible improvement to PMD-focused treatments. This case report describes a patient initially diagnosed with a PMD and referred for psychotherapy after appointments with neurologic and psychiatric providers. Upon referral to psychotherapy, the patient received a diagnosis of comorbid obsessive-compulsive disorder (OCD) and treatment with exposure and response prevention (ERP), an evidence-based psychotherapy for OCD. The patient demonstrated reliable improvements in all self-report measures as well as remission of PMD and OCD symptoms via behavioral observation at the end of therapy and at a 1-month follow-up. This case presents initial support for the treatment of comorbid and overlapping conditions in patients with PMDs, providing a pilot demonstration to support future large investigations.
Prim Care Companion CNS Disord 2018;20(4):18br02314
To cite: Gros DF, Allan NP, Haren WB. Exposure with response prevention for comorbid symptoms of obsessive-compulsive disorder and psychogenic movement disorder. Prim Care Companion CNS Disord. 2018;20(4):18br02314.
To share: https://doi.org/10.4088/PCC.18br02314
© Copyright 2018 Physicians Postgraduate Press, Inc.
aMental Health Service, Ralph H. Johnson Veterans Affairs Medical Center, Charleston, South Carolina
bDepartment of Psychiatry and Behavioral Sciences, Medical University of South Carolina, Charleston, South Carolina
cDepartment of Psychology, Ohio University, Athens, Ohio
*Corresponding author: Daniel F. Gros, PhD, Mental Health Service 116, Ralph H. Johnson VAMC, 109 Bee St, Charleston, SC 29401 ([email protected]).
Psychogenic movement disorders (PMDs) are characterized by abnormal movements or absence of normal movement that result from a psychiatric, rather than organic neurologic, disturbance. Community estimates of PMDs are 5.3% in movement disorder clinics and 1%-9% in neurologic units.1,2 Although no single clinical symptom is indicative of the disorder from a neurology perspective, there are several historical (eg, abrupt onset, static course, spontaneous remissions and cures, paroxysmal symptoms, and psychiatric comorbidities) and clinical (eg, inconsistencies in movement, incongruence with organic disorders) cues that suggest the diagnosis of a PMD.3 From a psychiatric perspective, PMDs are most consistent with a conversion disorder (functional neurologic symptom disorder) and are defined as 1 symptom or more of altered voluntary motor or sensory function that is incompatible with recognized neurologic or medical conditions and causes clinically significant distress or impairment. However, despite these overlapping perspectives between neurology and psychiatry, PMDs have been described as a "crisis for neurology" due to resistance from patients regarding the diagnosis and limited treatments and as a "borderland" between neurology and psychiatry, as the roles of providers are not well defined in the treatment of PMDs.2,4
As a result of PMDs aligning with the broader psychiatric categories of conversion disorders, somatoform disorders, illness anxiety disorder, body dysmorphic disorder, and pain disorder as well as the limited effective psychiatric treatments for PMDs, their psychiatric comorbidity has received increasing attention in the literature.1-4 The rates of comorbid disorders range from 19% to 57% in the literature, with depressive and anxiety disorders found to be among the most common.4,5 Due to the challenges in directly treating PMDs, it has been suggested that evaluating for and treating psychiatric comorbidity may be an effective means to approach PMDs.2 Currently, research is limited on this approach to treatment. The authors present the case of a patient with comorbid obsessive-compulsive disorder (OCD) and PMDs involving psychogenic tremor and deliberate slowness of movement who received an empirically validated psychotherapy for OCD, exposure and response prevention (ERP).6
CASE REPORT
Mr A was a 40-year-old, married, white male veteran who presented to a large Veterans Affairs Medical Center (VAMC) with freezing of movements and benign tremor and past diagnoses of OCD, unspecified personality disorder, and alcohol use disorder. All psychiatric conditions were diagnosed at his previous treatment facility. Mr A also reported a series of past neck injuries from various physical activities (eg, high school football). At the time of his initial visit to primary care, Mr A had been receiving chiropractic treatment for his physical concerns (eg, neck pain and tremor) for years, although no physical cause for said symptoms was identified by his provider. He also had been given bupropion (150 mg once daily) and aripiprazole (10 mg as needed) for his symptoms of depression and anxiety, but he had discontinued both medications due to concerns that they were contributing to his episodes of freezing and tremor. Mr A received a consult to the neurology department and the mental health service at the completion of his primary care visit. Mr A completed 8 visits with a psychiatrist and 2 visits with a neurologist over 6 months to assess for the appropriate diagnosis and course of treatment.
Neurologic Assessment
Mr A completed a neurologic examination, which was unremarkable despite reports of a tremor in his hand that was postural and a rotatory tremor toward the right. Mr A also reported episodes of freezing of movement that were not positional; occurred while standing, lying, and sitting; and were described as a cataplexy-type state. These freezing periods involved "self-talk" during which he coached himself through motor initiation and planning, often resulting in efforts to repeat movements several times in a row until the movement felt right. Treatment was deferred by his neurologist to his psychiatrist.

- Interplay between neurology and psychiatry is critical for diagnosis of and treatment planning for psychogenic movement disorder.
- Medication treatments for movement disorder provide limited, sustained improvements.
- Psychotherapy for comorbid obsessive-compulsive disorder (OCD) may result in remission of OCD and PMD symptoms.
Psychiatric Assessment and Treatment
During his visits with a psychiatrist, differential diagnoses of catatonic-type schizophrenia, early parkinsonism, and OCD with PMDs were further assessed and informed treatment recommendations. Mr A was prescribed fluoxetine (10 mg once daily) and lorazepam (1 mg as needed) to address baseline symptoms of anxiety and depression reported at his first visit. Gains were witnessed in Mr A’s mood, freezing periods, and tremors at the second visit, further supporting the diagnosis of an affective disorder. Diagnostic imaging also was employed through the neurology department to successfully rule out parkinsonian tremor. Fluoxetine was further adjusted during this phase of treatment to target additional symptom improvement (ranging from 10-40 mg daily). However, a relapse of tremor and development of delays and pausing in speech were experienced 4 months into treatment. The relapse occurred during and worsened after a stressful weekend trip with his wife when neck pain was experienced during a long car ride. The observation of symptoms of PMDs and affective disorders as well as the brief improvements and then return of symptoms associated with psychosocial stressors and physical cues resulted in a referral to the psychology department for further assessment and consideration for psychotherapy. Of note, fluoxetine (10 mg 3 times daily) was maintained during the course of psychotherapy.
Psychological Assessment and Treatment
Mr A completed a series of assessments with a psychologist focused on diagnostic clarity. Mr A’s wife accompanied him during the intake and treatment sessions. The assessment included the Mini-International Neuropsychiatric Interview 5.0 (MINI),7 Depression Anxiety Stress Scales (DASS),8 and Illness Intrusiveness Rating Scale (IIRS).9 The MINI is a structured diagnostic interview designed to provide a brief, but accurate, assessment of a wide range of DSM-IV psychiatric disorders,10 including mood disorders, anxiety disorders, and substance use disorders.7 The DASS is a 21-item self-reported measure with 3 subscales designed to assess dysphoric mood (depression subscale), symptoms of fear and autonomic arousal (anxiety subscale), and symptoms of tension and agitation (stress subscale).8 The DASS items are rated on a 4-point Likert scale, ranging from 0-3, and summed to compute the 3 subscales. The scores are doubled to be consistent with the 42-item version of the DASS. The IIRS is a 13-item self-reported measure that assesses the extent to which a disease interferes with important domains of life, including health, diet, work, and several others.9 Each item is rated on a 7-point Likert scale, ranging from 1-7.
Mr A endorsed symptoms consistent with OCD on the MINI. His reported symptoms included obsessions regarding his likelihood of reinjury of his neck and his related severe impairment, despite no physically identified symptoms or problems that put him at risk for further injury. For example, Mr A reported obsessing that "I am going to hurt my neck if I’ m not careful and then be in constant pain," and over images of himself in a neck brace and being "disabled" (eg, seated in a wheelchair). Mr A reported using a number of compulsions to reduce the distress associated with his obsessions. These compulsions were those identified by the neurologist and psychiatrist, namely stopping or freezing, slowing of movements and speech, and repeating movements. For example, Mr A made very slow and deliberate movements when met in the waiting room by his psychologist. Mr A slowly moved his head upward, paused 3 seconds, said "I’ ¦am’ ¦here’ ¦," paused 3 seconds, lifted himself from his chair with his legs while keeping his back and neck from bending or moving, paused 3 seconds, and then walked toward the psychologist again without his back or neck bending or moving. Mr A also was silently mouthing self-talk related to his movements (eg, "I am standing up now. I will not hurt my neck.") and frequently took long, deep breaths while moving. During the interview, Mr A’s wife reported these behaviors occurred during all situations (eg, "It takes him like 5 minutes to get a can of soda from the fridge."). Mr A reported significant impairment associated with these symptoms, including job loss, financial difficulties, and a previous divorce (since remarried). Mr A also reported symptoms consistent with comorbid, recurrent major depressive disorder, involving depressed mood, anhedonia, poor sleep, fatigue, concentration difficulties, and feelings of worthlessness (he denied suicidal ideation).
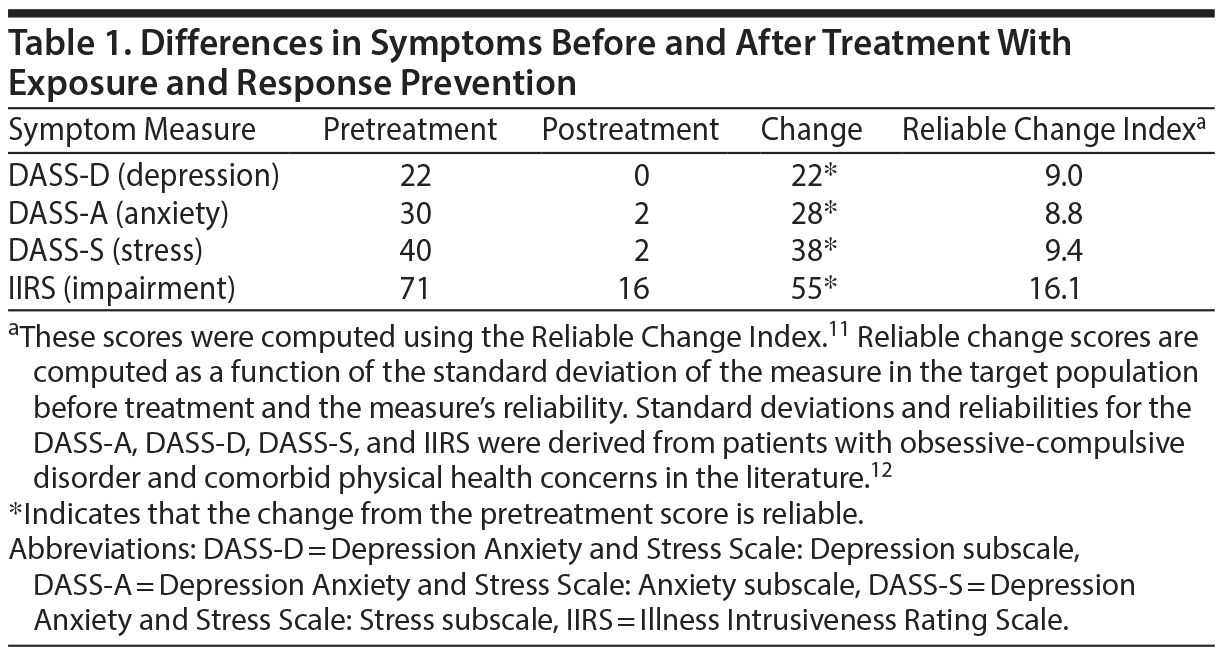
Mr A endorsed symptoms on the self-report measures that were consistent with the structured clinical interview (MINI). He reported severe symptoms of depression (DASS-D), anxiety (DASS-A), and stress (DASS-S) and very severe functional impairment associated with his symptoms. Of note, it took Mr A nearly 1 hour to complete the self-report measures (eg, typically completed in 10-15 minutes by patients). All baseline scores are reported in Table 1.
Mr A’s symptoms were conceptualized within an OCD framework in which his past neck injuries and short-term disability served as a significant stressor that promoted obsessions (eg, "I am going to reinjure my neck and become disabled.") and related compulsions to reduce the anxiety associated with the obsessions (eg, rigidly controlled and slowed movements, repeated self-talk prior to movements, repeating movements until they felt correct). On the basis of these symptoms, the psychologists selected ERP as the evidence-based psychotherapy of choice to address Mr A’s symptoms. Brief psychoeducation was provided for OCD and ERP. Mr A agreed to begin ERP.
Treatment began with a more in-depth explanation of ERP, which involves treating the symptoms of OCD by repeatedly exposing the patient to feared stimuli or situations, while preventing the use of compulsions.6 The exposure process includes identifying the patient-specific feared stimuli or situations for future exposure practice, ordering exposures by difficulty, and engaging in varied activities to improve learning and generalization. In ERP, the exposures themselves include a response prevention component to delay or completely prevent the use of compulsions. Within this framework, ERP was used to expose Mr A to quick, unpredictable movements without the use of self-talk or repeating movements. One early example involved the psychologist’s quickly giving verbal instructions for Mr A to complete during the session without using compulsions (eg, stand up, sit, jump, look right, look left, look down). Within this example, Mr A’s expectation was that quick movements, lacking self-talk and freezing, would result in a neck injury and related disability. By repeating quick movements that lacked said compulsions, Mr A was able to violate or disprove his negative expectations and learn the more correct or accurate outcome of his movements without compulsions. Mr A and his wife were instructed to repeat these practices at home together (eg, wife quickly calling out movements for Mr A to complete without compulsions) or for Mr A to complete on his own (eg, use his smartphone’s timer to practice retrieving drinks from the refrigerator in less than 30 seconds). Mr A’s progress was tested during each session, as well as naturally observed by the psychologist (eg, leaving the waiting room), with the types of assignments increasing in difficulty each week (eg, reducing time to complete tasks and movements directly targeting neck movements, rather than the whole body). Mr A demonstrated dramatic improvements after only 4 weeks of ERP treatment due largely to daily practice and homework completion. Mr A no longer displayed any abnormal movements or speech patterns, and his tremor was no longer visible at the completion of ERP. Mr A’s use of self-talk also had stopped. As presented in Table 1, Mr A endorsed significant improvements from severe symptoms at pretreatment to minimal symptoms at posttreatment in his self-reported symptoms of depression, anxiety, and stress on the DASS and related impairment on the IIRS.
Mr A met with his psychiatrist for a 1-month follow-up after completion of brief ERP and reported that he was "doing great." He denied any relapses of tremor, freezing of movements, disruptions in speech, or self-talk despite having a few episodes of shoulder blade and neck stiffness (previously identified triggers for obsessions and compulsions). Mr A added that he had begun to titrate himself off of his medication, as he felt that it was no longer needed to address his symptoms. No additional medications were prescribed due to Mr A’s noted symptom improvements.
DISCUSSION
This case report details the assessment and treatment of a patient with comorbid symptoms of OCD and PMDs that initially mimicked other more serious neurologic and psychiatric disorders (catatonic-type schizophrenia and early parkinsonism). The evaluation, collaboration, and communication between primary care, neurology with imaging, and psychiatry were successful in developing an accurate diagnosis and determining treatment recommendations. Ultimately, evidence-based psychotherapy targeting the comorbid symptoms of OCD was found to be most effective in addressing both disorders and achieving symptom remission. There are several implications of the case report that merit further discussion.
As recommended elsewhere,4 the interplay between neurology and psychiatry was vital in the correct diagnosis and treatment planning of this case. This process can be especially challenging, as patient-perceived organic-disordered movement is labeled as psychogenic symptoms by neurologists and, therefore, a referral to psychiatry is initiated. The key to the present case was the speed and frequency of these appointments. Mr A obtained appointments within primary care, neurology, and then psychiatry all in a period of 4 days. In addition, all providers were included in the documentation of these visits to further facilitate communication. This process allowed Mr A to receive a quick diagnosis and initial feedback on treatment options that were shared across each of his providers. This process highlights the strength of providing care within the multidisciplinary/multiservice facility, as is the case at VAMCs, and very likely contributed to the positive outcome in this case. Although direct research is needed, this level of collaboration and frequency of care could be comparable to more intensive programs for conversion disorder offered in Canada and the United Kingdom.4
Another implication of the present case was the success of the treatment approach. Rather than focusing on the initial diagnosis of a PMD, the secondary or comorbid symptoms of OCD were successfully targeted. Although there has been some research in the treatment of the symptoms of PMD and conversion disorder via brief psychodynamic psychotherapy,13,14 the findings for those practices and other similar approaches (eg, hypnosis therapy) have not been particularly impressive.4,14 The present case example used a largely successful, empirically validated psychotherapy for the comorbid or overlapping symptoms of OCD and evidenced significant improvements across 4 weeks of therapy that were sustained at 1-month follow-up. Of note, treatment of OCD through ERP resulted not only in reductions of Mr A’s obsessive and compulsive symptoms, but also in his PMD symptoms (ie, trembling). Although a follow-up visit to his neurologist would have been necessary to confirm, it seems very likely that Mr A would no longer have received a PMD diagnosis. Although preliminary, these findings support previous suggestions4 that treating psychiatric comorbidity may be an effective approach to treating PMDs. Alternatively, it also is possible that ERP had a direct effect on the PMD symptoms themselves, independent of its effect on OCD symptoms. Further research is needed to better understand the relations among ERP and the symptoms of OCD and PMDs.
There are a few limitations of this case report. For example, Mr A was treated as part of standard clinical care within a VAMC, thus specialized disorder-specific assessments, such as the Yale-Brown Obsessive Compulsive Scale (Y-BOCS),15 were not completed to more fully support symptom improvements. Future research should include semistructured diagnostic interviews for the affective disorders, such as the Anxiety and Related Disorders Interview Schedule for DSM-516 or Y-BOCS, to confirm their diagnosis. Measures specifically designed to assess PMDs also would be helpful in tracking these symptoms.17 Additional follow-up assessments might have been useful in plotting the long-term outcomes associated with the treatment.
CONCLUSIONS
PMDs are challenging to diagnose and even more challenging to treat. Best practice should involve a strong collaboration between neurology and psychiatry. However, even when these recommendations are followed, psychiatric/psychological treatment outcomes for PMDs are not promising.4,12 The present case study provides preliminary support for using a well-established therapeutic practice, ERP, to treat the comorbid or overlapping symptoms of OCD to reduce the associated or manifested symptoms of PMDs. Future research should further explore this finding in larger samples and in other related and commonly comorbid conditions (eg, depressive and anxiety disorders).
Submitted: April 13, 2018; accepted June 7, 2018.
Published online: August 16, 2018.
Potential conflicts of interest: None.
Funding/support: This study is supported by Department of Veteran Affairs Clinical Sciences Research and Development Career Development Award CX000845 (principal investigator: Dr Gros).
Role of the sponsor: Veterans Affairs Clinical Sciences Research and Development and Ralph H. Johnson VAMC had no further role in study design; in the collection, analysis and interpretation of data; in the writing of the report; or in the decision to submit the paper for publication.
Disclaimer: The views expressed in this article are those of the authors and do not necessarily reflect the position or policy of the Department of Veterans Affairs or the United States government.
Patient consent: Consent was received from the patient to publish this case report, and data were de-identified to protect anonymity.
REFERENCES
1. Bhatia KP, Schneider SA. Psychogenic tremor and related disorders. J Neurol. 2007;254(5):569-574. PubMed CrossRef
2. Kranick SM, Gorrindo T, Hallett M. Psychogenic movement disorders and motor conversion: a roadmap for collaboration between neurology and psychiatry. Psychosomatics. 2011;52(2):109-116. PubMed CrossRef
3. Gupta A, Lang AE. Psychogenic movement disorders. Curr Opin Neurol. 2009;22(4):430-436. PubMed CrossRef
4. Kranick SM, Ellenstein A, Hallett M. Psychiatric comorbidities and risk factors in psychogenic movement disorders: a biopsychosocial approach. Eur Neurol J. 2010;2:1-7.
5. American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
6. Foa EB, Yadin E, Lichner TK. Exposure and Response (Ritual) Prevention for Obsessive-Compulsive Disorder: Therapist Guide (Treatments That Work). New York, NY: Oxford University Press; 2012.
7. Sheehan DV, Lecrubier Y, Sheehan KH, et al. The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry. 1998;59(suppl 20):22-33, quiz 34-57. PubMed
8. Lovibond SH, Lovibond PF. Manual for the Depression Anxiety Stress Scales. 2nd ed. Sydney, Australia: Psychology Foundation of Australia; 1995.
9. Devins GM, Binik YM, Hutchinson TA, et al. The emotional impact of end-stage renal disease: importance of patients’ perception of intrusiveness and control. Int J Psychiatry Med. 1983-1984;13(4):327-343. PubMed CrossRef
10. American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fourth Edition. Washington, DC: American Psychiatric Association; 1994.
11. Jacobson NS, Truax P. Clinical significance: a statistical approach to defining meaningful change in psychotherapy research. J Consult Clin Psychol. 1991;59(1):12-19. PubMed CrossRef
12. Gros DF, Antony MM, McCabe RE, et al. Frequency and severity of the symptoms of irritable bowel syndrome across the anxiety disorders and depression. J Anxiety Disord. 2009;23(2):290-296. PubMed CrossRef
13. Hinson VK, Weinstein S, Bernard B, et al. Single-blind clinical trial of psychotherapy for treatment of psychogenic movement disorders. Parkinsonism Relat Disord. 2006;12(3):177-180. PubMed CrossRef
14. Kompoliti K, Wilson B, Stebbins G, et al. Immediate vs delayed treatment of psychogenic movement disorders with short term psychodynamic psychotherapy: randomized clinical trial. Parkinsonism Relat Disord. 2014;20(1):60-63. PubMed CrossRef
15. Goodman WK, Price LH, Rasmussen SA, et al. The Yale-Brown Obsessive Compulsive Scale, I: development, use, and reliability. Arch Gen Psychiatry. 1989;46(11):1006-1011. PubMed CrossRef
16. Brown TA, Barlow DH. Anxiety and Related Disorders Interview Schedule for DSM-5 (ADIS-5): Clinician Manual. New York, NY: Oxford; 2014.
17. Hinson VK, Cubo E, Comella CL, et al. Rating scale for psychogenic movement disorders: scale development and clinimetric testing. Mov Disord. 2005;20(12):1592-1597. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!