Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
To the Editor: Neuroleptic malignant syndrome (NMS) is a rare but potentially serious reaction to antipsychotic medications. The incidence of NMS is around 0.9%, with an estimated mortality of 5.6%-12%. Early recognition is key and a low index of suspicion is required as the presentation shares symptoms with other disorders, which is further compounded by a lack of definitive diagnostic criteria.
Neuroleptic Malignant Syndrome: The Value of Diagnostic Criteria
To the Editor: Neuroleptic malignant syndrome (NMS) is a rare but potentially serious reaction to antipsychotic medications. The incidence of NMS is around 0.9%,1 with an estimated mortality of 5.6%-12%.2,3 Early recognition is key and a low index of suspicion is required as the presentation shares symptoms with other disorders,1,4,5 which is further compounded by a lack of definitive diagnostic criteria.
Case report. Mr A, an African man in his mid-20s, was admitted to an inpatient mental health unit in January 2017 with first-episode psychosis and was compulsorily detained under Section 2 of the UK Mental Health Act 1983. He appeared thought disordered, with derailment, tangentiality, thought blocking, and poverty of speech. He had no previous psychiatric history and no medical comorbidities. There was no family history of mental illness and no history of illicit drug use. Routine blood test results were unremarkable, and a urine drug screen was negative for all substances.
After admission to the ward, he began hitting his head against windows and was started on lorazepam 1 mg oral and haloperidol 5 mg oral on an as-required basis up to a maximum dosage of 20 mg/d. On day 3, following his third dose of haloperidol 5 mg, he began to show a marked improvement, being able to speak fluently and provide a good history of events. The haloperidol prescription remained on an as-required basis while monitoring for side effects in line with national guidance for management of first-episode psychosis,6 and the patient received a maximum of 10 mg of haloperidol within a 24-hour period.
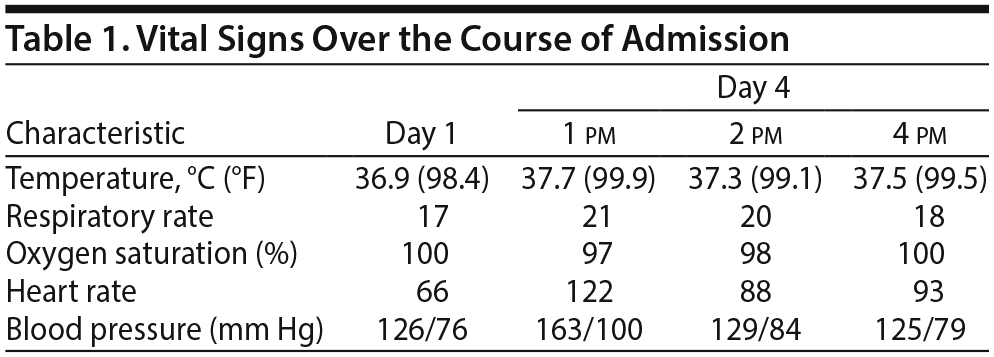
On day 4 of his admission, he began to experience upper limb stiffness following a fifth dose of haloperidol and became drowsy and disoriented. His physical examination showed an aural temperature of 37.7°C (99.9°F), tachycardia, and hypertension (Table 1). Haloperidol was discontinued immediately. After 1 hour, his symptoms appeared to improve and his vital signs were normalizing. However, 2 hours later, a clinical examination revealed marked upper and lower limb rigidity, and laboratory studies demonstrated a high creatine kinase (CK) level of 2,694 U/L (laboratory reference range, 30-175 U/L).
He was transferred to the medical ward for supportive management of NMS. He received fluids and lorazepam intravenously, and following improvement, he returned to the psychiatric ward 4 days later. He continued to improve, and aripiprazole was initiated 14 days after resolution of NMS to treat his psychotic symptoms. Aripiprazole was introduced from a low dose of 5 mg and slowly increased over 4 weeks to 15 mg at discharge. He experienced no recurrence of NMS and remains in remission under the care of the early intervention team in the community.
Multiple criteria for NMS have been reported,7-13 each with differing critical values required to confirm the diagnosis. Gurrera et al14 developed international consensus on criteria and critical values required to diagnose NMS. While this is a welcome attempt to achieve uniformity in diagnosis, difficulties remain in identifying how many criteria are required for a confident diagnosis.
In the case presented here, the patient met all criteria for NMS defined by Gurerra et al14 except temperature over 38°C (100.4°F). He would not have reached the threshold for diagnosis using several other criteria,9,10,12 while those requiring temperature over 37.5°C (99.5°F) would have supported a diagnosis of NMS.7,8,11 This case highlights the need for clinicians to be vigilant even when the full criteria are not met, as patients may not present with hyperthermia until later in the development of NMS1,15 and cases of atypical NMS have been reported without hyperthermia.16
It has been suggested that due to inaccuracy of temperature measurements, it is difficult to tell if NMS truly is a "hyperthermic syndrome" and what level of hyperthermia is necessary to reach diagnostic threshold.17 In this scenario, NMS was identified only 4 days after starting antipsychotics, possibly before the development of true hyperthermia, and therefore failed to reach full diagnostic criteria.
Additionally, guidelines on antipsychotic rechallenge following NMS are lacking, in part because most antipsychotics, including atypicals, have been associated with NMS.18 While the choice of antipsychotic does not appear to affect the success of a rechallenge following NMS,19 there are reports20 that aripiprazole can be used with success in recurrent NMS, possibly due to partial agonism at D2 receptors, and this case demonstrates a further instance of its successful use.
Clinicians need to remain vigilant and pragmatic regarding the multiple diagnostic criteria for NMS. In a condition with a high mortality rate predominantly affecting young people, prompt treatment in suspected NMS should be prioritized. In the case described, treatment with aripiprazole achieved remission of psychotic symptoms without a recurrence of NMS.
References
1. Pileggi DJ, Cook AM. Neuroleptic malignant syndrome. Ann Pharmacother. 2016;50(11):973-981. PubMed CrossRef
2. Modi S, Dharaiya D, Schultz L, et al. Neuroleptic malignant syndrome: complications, outcomes, and mortality. Neurocrit Care. 2016;24(1):97-103. PubMed CrossRef
3. Tse L, Barr AM, Scarapicchia V, et al. Neuroleptic malignant syndrome: a review from a clinically oriented perspective. Curr Neuropharmacol. 2015;13(3):395-406. PubMed CrossRef
4. Dosi R, Ambaliya A, Joshi H, et al. Serotonin syndrome versus neuroleptic malignant syndrome: a challenging clinical quandary. BMJ Case Rep. 2014;2014(2):bcr2014204154. PubMed CrossRef
5. Lang FU, Lang S, Becker T, et al. Neuroleptic malignant syndrome or catatonia? trying to solve the catatonic dilemma. Psychopharmacology (Berl). 2015;232(1):1-5. PubMed CrossRef
6. National Institute for Health and Care Excellence (NICE). Psychosis and schizophrenia in adults: prevention and management. Clinical guideline [CG178]. https://www.nice.org.uk/guidance/cg178/chapter/recommendations#first-episode-psychosis-2. Published February 2014. Updated March 2014. Accessed September 2017.
7. Levenson JL. Neuroleptic malignant syndrome. Am J Psychiatry. 1985;142(10):1137-1145. PubMed CrossRef
8. Addonizio G, Susman VL, Roth SD. Symptoms of neuroleptic malignant syndrome in 82 consecutive inpatients. Am J Psychiatry. 1986;143(12):1587-1590. PubMed CrossRef
9. Mathews T, Aderibigbe YA. Proposed research diagnostic criteria for neuroleptic malignant syndrome. Int J Neuropsychopharmacol. 1999;2(2):129-144. PubMed CrossRef
10. Caroff SN, Mann SC. Neuroleptic malignant syndrome. Med Clin North Am. 1993;77(1):185-202. PubMed CrossRef
11. Pope HG Jr, Keck PE Jr, McElroy SL. Frequency and presentation of neuroleptic malignant syndrome in a large psychiatric hospital. Am J Psychiatry. 1986;143(10):1227-1233. PubMed CrossRef
12. Friedman JH, Davis R, Wagner RL. Neuroleptic malignant syndrome: the results of a 6-month prospective study of incidence in a state psychiatric hospital. Clin Neuropharmacol. 1988;11(4):373-377. PubMed CrossRef
13. American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
14. Gurrera RJ, Caroff SN, Cohen A, et al. An international consensus study of neuroleptic malignant syndrome diagnostic criteria using the Delphi method. J Clin Psychiatry. 2011;72(9):1222-1228. PubMed CrossRef
15. Norris B, Angeles V, Eisenstein R, et al. Neuroleptic malignant syndrome with delayed onset of fever following risperidone administration. Ann Pharmacother. 2006;40(12):2260-2264. PubMed CrossRef
16. Rodriguez OP, Dowell MS. A case report of neuroleptic malignant syndrome without fever in a patient given aripiprazole. J Okla State Med Assoc. 2006;99(7):435-438. PubMed
17. Gillman PK. Neuroleptic malignant syndrome, poor science and inaccurate measurements. J Psychopharmacol. 2011;25(6):850. PubMed CrossRef
18. Belvederi Murri M, Guaglianone A, Bugliani M, et al. Second-generation antipsychotics and neuroleptic malignant syndrome: systematic review and case report analysis. Drugs R D. 2015;15(1):45-62. PubMed CrossRef
19. Wells AJ, Sommi RW, Crismon ML. Neuroleptic rechallenge after neuroleptic malignant syndrome: case report and literature review. Drug Intell Clin Pharm. 1988;22(6):475-480. PubMed CrossRef
20. Trutia A, Bledowski J, Pandurangi A, et al. Neuroleptic rechallenge with aripiprazole in a patient with previously documented neuroleptic malignant syndrome. J Psychiatr Pract. 2008;14(6):398-402. PubMed CrossRef
aCoventry and Warwickshire Partnership Trust, The Caludon Centre, Coventry, United Kingdom
Potential conflicts of interest: None.
Funding/support: None
Previous presentation: Conference abstract at Royal College of Psychiatrists International Congress 2017; June 29, 2017; Edinburgh, Scotland;.
Patient consent: Informed consent was obtained from the patient to publish this case report, and information has been deidentified to protect anonymity.
Published online: August 2, 2018.
Prim Care Companion CNS Disord 2018;20(4):17l02218
To cite: Rowland TA, Banga A, Ayadurai N. Neuroleptic malignant syndrome: the value of diagnostic criteria. Prim Care Companion CNS Disord. 2018;20(4):17l02218.
To share: https://doi.org/10.4088/PCC.17l02218
© Copyright 2018 Physicians Postgraduate Press, Inc.
Enjoy this premium PDF as part of your membership benefits!